No, enamel cannot grow back. Once tooth enamel is lost, whether from acid erosion, grinding, or physical wear, it is gone permanently. There are no cells left in your adult teeth capable of making new enamel. That is the short answer, and every reputable dental authority, from the Cleveland Clinic to the ADA, agrees on this point. But here is the thing: the full story is more useful than that one sentence. Some early enamel damage can actually be repaired through a process called remineralization, which is not the same as growing new enamel but it does matter a lot for your teeth right now. Understanding the difference is the key to knowing what you should actually do today.
Can Enamel Grow Back? What Helps and What Doesn’t
What's possible and what isn't: enamel vs. other tooth tissues
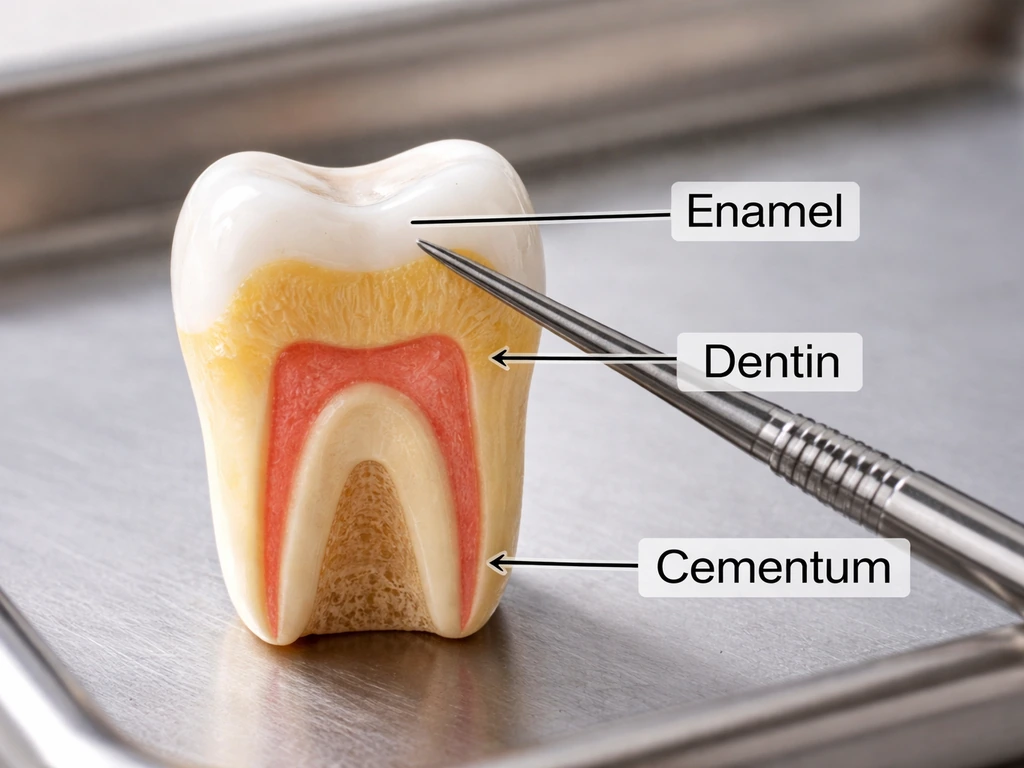
Your tooth is made of several layers, and they do not all behave the same way when damaged. Enamel is the hard outer shell. Dentin sits underneath it. Cementum covers the tooth root. The pulp at the center contains nerves and blood vessels. When people ask whether teeth can regenerate, the answer is different depending on which tissue you are talking about. While teeth tissues like dentin may respond in limited ways, the root tissue and tooth enamel are not truly able to regenerate, so it is important to understand what can and cannot regrow can teeth roots grow back. can bone grow back around teeth
Dentin has a limited repair response. When decay or injury reaches the inner tooth, the pulp can signal the formation of what is called reparative or reactionary dentin, a type of hard tissue that forms as a protective response. It is not a perfect reconstruction, but it is a real biological reaction. The same is not true for enamel. Once enamel is gone, no repair response kicks in. There are no enamel-forming cells left to do anything.
Remineralization is the one process that can genuinely help enamel, but only at an early stage. When enamel starts to demineralize (meaning acid has begun to dissolve the mineral crystals in its structure but has not yet created a cavity), fluoride, calcium, and phosphate can be redeposited into those weakened areas. This is not growing new enamel. It is restoring mineral content to enamel that is already there. Think of it like patching the pores in a brick rather than building a new brick from scratch.
| Tooth Tissue | Can It Regenerate? | What Actually Happens |
|---|---|---|
| Enamel | No | Lost enamel is gone permanently; early demineralization can be remineralized |
| Dentin | Limited | Reparative/reactionary dentin can form in response to injury or decay |
| Cementum | Minimal | Some repair possible but not reliable regeneration |
| Pulp tissue | No (in adults) | Cannot regenerate naturally once significantly damaged |
Why enamel can't grow back (the biology, kept simple)
Enamel is built by specialized cells called ameloblasts. These cells are incredibly active while your teeth are forming, secreting and mineralizing enamel in two stages: a secretory stage where the protein matrix is laid down, and a maturation stage where the mineral content is refined. Here is the critical part: during that maturation process, roughly 25% of ameloblasts undergo apoptosis (programmed cell death), and the rest are lost when the tooth erupts into your mouth. By the time you can see and feel your tooth, the cells that made its enamel are gone.
This is why WebMD, the Cleveland Clinic, and basically every dental biology textbook all say the same thing: mature enamel has no living cells. There is nothing left in the tooth to receive a signal and make new enamel. Researchers are actively studying biomimetic systems and lab-grown enamel-like materials precisely because the body cannot do this on its own. It is not a limitation of medicine or dental care. It is a basic biological fact about how human teeth develop.
This also explains why enamel erosion is taken so seriously. Once you lose it, the only options are to protect what remains or restore the surface with dental materials. There is no waiting for it to come back.
What to do right now based on the signs you have
The right action depends on how far along the damage is. Not all enamel problems look or feel the same, and the treatment path is genuinely different depending on the stage.
Figure out where you stand
Early enamel damage often shows up as white spot lesions, chalky or opaque patches on the tooth surface. These are areas of subsurface demineralization where enamel is weakened but not yet broken through. At this stage, remineralization is genuinely possible. More advanced damage looks like visible thinning, increased translucency at the edges (especially on front teeth), rough or pitted surfaces, or teeth that feel sensitive to cold, sweet, or acidic foods. Full cavities, meaning a hole or breakdown in the tooth surface, are past the point of non-invasive management.
Immediate steps you can take at home
- Switch to a fluoride toothpaste and use it consistently twice a day. Fluoride works by inhibiting demineralization and supporting remineralization of early enamel damage. The CDC and ADA both recommend frequent, small-amount fluoride exposure for exactly this reason.
- If you have sensitivity, try a desensitizing toothpaste with potassium nitrate or stannous fluoride. These do not rebuild enamel but they help manage pain while you address the underlying cause.
- Cut back on acidic foods and drinks: citrus, carbonated drinks, vinegar-based foods, and sports drinks are among the biggest culprits. When you do have them, rinse with water afterward and wait at least 30 minutes before brushing.
- Avoid abrasive toothpastes and hard-bristle brushes. These accelerate enamel wear, especially when enamel is already thinned.
- If you grind your teeth at night, that is an urgent issue. Grinding accelerates enamel loss faster than almost anything else.
When to see a dentist, and what they can do
If you have visible white spots, sensitivity that does not improve, roughness you can feel with your tongue, or any area that looks pitted or translucent, you need a dentist to assess the severity. The treatment path varies significantly depending on the stage.
| Stage of Damage | What It Looks Like | Evidence-Based Treatment Options |
|---|---|---|
| Early (noncavitated white spot) | Chalky/opaque patches, no cavity | Fluoride varnish every 3-6 months, dental sealants, resin infiltration |
| Moderate (enamel erosion, thinning) | Translucent edges, sensitivity, rough texture | Fluoride varnish, desensitizing treatments, sealants, monitoring |
| Advanced (cavitated lesion) | Visible hole, pitting, significant sensitivity | Restorative care: tooth-colored fillings, bonding |
| Severe (extensive loss, exposed dentin) | Brown discoloration, severe sensitivity, visible dentin | Crowns, veneers, or full restorative reconstruction |
The ADA's evidence-based guidelines recommend 5% sodium fluoride varnish applied every 3 to 6 months as a strong, evidence-backed approach to arresting and potentially reversing noncavitated early lesions. Dental sealants can also minimize progression of early lesions on biting surfaces. Resin infiltration is a micro-invasive option where a resin material is applied after conditioning the enamel surface, acting as a barrier to stop progression of white spot lesions. For anything beyond noncavitated lesions, restorative treatment is needed, because remineralization cannot fix a cavity or restore lost tooth structure.
Does enamel grow back after whitening?
This is one of the most common variations of this question, and the anxiety around it is understandable. Whitening treatments, both professional and over-the-counter, use peroxide-based agents that can temporarily increase tooth sensitivity. Some people worry they have damaged their enamel permanently. Here is what actually happens.
Whitening does not remove enamel. What it does is temporarily alter the hydration of enamel and affect the organic components within the tooth structure. The sensitivity you feel after whitening is real, but it is not the same as enamel erosion. The enamel itself has not been dissolved or stripped away by the whitening process when used as directed.
If teeth feel more sensitive after whitening, that sensitivity typically resolves within a few days. Using a remineralizing or desensitizing toothpaste before and after whitening treatments helps. Any apparent improvement in how teeth feel after whitening is not enamel regrowing. It is the tooth rehydrating and minerals being redeposited through saliva contact and fluoride use, which is remineralization, not new enamel growth.
Where it gets more concerning is if you are whitening teeth that already have thinned or eroded enamel. In that case, the underlying sensitivity and damage were there before the whitening. The whitening did not cause the erosion, but it will make existing sensitivity more noticeable. If your teeth look translucent at the edges or feel sensitive even without whitening, see a dentist before starting any whitening treatment.
What Reddit gets wrong (and what the science actually says)
Search for enamel regrowth on Reddit and you will find a mix of genuine personal experiences and some claims that go well beyond what the evidence supports. A few recurring ones are worth addressing directly.
One common claim is that oil pulling, remineralizing toothpaste, or eating certain foods can rebuild or regrow enamel. Remineralizing products like fluoride toothpaste and calcium phosphate preparations can genuinely support remineralization of early lesions. But remineralization means restoring mineral content to already-existing weakened enamel, not generating new enamel tissue. No toothpaste, oil, or diet change will create new enamel where it has been lost.
Another frequent piece of advice is that small cavities can heal themselves if you clean your teeth well enough. This conflates two different things. Noncavitated early lesions (white spots, early demineralization where the surface is still intact) can genuinely be arrested or reversed with fluoride, sealants, and improved oral hygiene. The ADA's own guidelines support this. But an actual cavity, meaning one where the tooth surface has broken down and there is a hole, needs restorative care. Brushing will not fill a cavity.
Some Reddit threads also suggest that switching to a highly alkaline diet or taking specific mineral supplements will stimulate enamel regeneration. There is no clinical evidence that this works. Saliva does play a role in natural remineralization, and diet absolutely affects the rate of enamel erosion, but these are protective and preventive factors, not regenerative ones.
The honest summary: fluoride-based remineralization is real and it works for early damage. Everything else claiming to rebuild or regrow enamel is either repackaging that same remineralization concept or overstating what the evidence shows. Be skeptical of anything promising to regrow what the body structurally cannot regenerate on its own.
Your clearest path forward
If you are reading this because you are worried about your enamel right now, here is the practical takeaway. You cannot grow new enamel. remineralize and strengthen what is there If the damage is more advanced, your dentist has real, effective options from fillings and bonding to veneers and crowns depending on severity. None of these replace enamel biologically, but they do protect the tooth and restore function. can teeth nerves grow back. how long does it take for enamel to grow back
Start with fluoride toothpaste today. Cut acids in your diet. If you grind your teeth, get a night guard. If you have sensitivity, roughness, white spots, or visible thinning, book a dental appointment and be specific about your concerns. The earlier you act, the more options you have, and the more of your natural tooth structure can be preserved.
Enamel is irreplaceable, which means the smartest move is always to protect what you still have rather than wait and hope it comes back. It will not. But with the right approach starting now, you can keep the enamel you have healthy for a long time.
FAQ
If enamel can’t grow back, can the tooth itself “heal” in any other way besides remineralization?
Yes, but it depends on the layer. Enamel cannot regenerate, but dentin can form reactionary or reparative dentin if decay or injury reaches inward. That can help protect the nerve, though it does not recreate the lost enamel layer or restore the original outer hardness.
Do I still need fluoride if I already use a remineralizing toothpaste?
Often, yes. Many “remineralizing” toothpastes contain fluoride, and that matters because fluoride supports redeposition of minerals during early demineralization. The key difference is professional options, like fluoride varnish at intervals, which provide a higher, more sustained fluoride dose for early white spot lesions.
Can enamel be regrown with enzymes or “enamel biomimetic” products sold online?
Most at-home products cannot truly regrow lost enamel, because they cannot recreate the specialized biology that made enamel during tooth development. Even if a product reduces sensitivity or makes teeth look smoother, it’s usually improved surface remineralization or temporary hydration, not new enamel tissue.
How can I tell whether my white spots are reversible or already a cavity?
Look for clues, but get an exam. White spot lesions with an intact surface are commonly noncavitated and may respond to fluoride and sealants, while areas that feel rough, have pitting, or show a defect that catches on the tongue are more likely cavitated and require restorative care.
Does brushing harder or using an abrasive toothpaste make enamel come back?
No. Aggressive brushing and abrasive products can accelerate wear and expose dentin, worsening sensitivity. If you have erosion risk, use a soft brush, gentle technique, and fluoride toothpaste rather than trying to “scrub” enamel back into place.
What’s the fastest way to stop early enamel loss at home?
The most practical sequence is fluoride consistently (twice daily), reduce acid exposure between meals, and consider a desensitizing or remineralizing toothpaste if you’re sensitive. For early lesions, professional fluoride varnish and, when appropriate, sealants can move things faster than home care alone.
Can saliva or drinking water alone reverse enamel demineralization?
Saliva helps, but it is not sufficient for everyone. Saliva buffers acids and provides calcium and phosphate, yet ongoing acid challenges from frequent snacking, reflux, or sugary drinks can outpace natural remineralization. If you repeatedly get white spots, you typically need fluoride-based intervention and behavior changes.
Will a night guard protect enamel even if I grind my teeth?
A night guard protects the tooth surfaces from contact forces and can reduce micro-chipping and wear, but it doesn’t rebuild enamel. If you also have acid reflux or frequent sugary drinks, you still need to address erosion triggers, because grinding and acid can compound the problem.
If whitening doesn’t remove enamel, why do I feel more sensitivity afterward?
Sensitivity after whitening is common and usually reflects temporary fluid shifts and irritation of the tooth’s inner layers rather than true enamel loss. It often improves within a few days. If you have edge translucency or baseline sensitivity, a dentist can check whether you’re starting from already-thinned enamel before whitening.
If I have translucent edges, does that mean enamel is definitely gone?
Not always. Translucency can indicate thinning, enamel wear, developmental hypomineralization, or bonding effects from past dental work. Because treatment differs, a dental exam and, sometimes, imaging helps distinguish “thinning that may respond to protection” from defects that need restorative correction.
Can a cavity really not “heal” if it’s small?
Correct. A true cavity involves breakdown of the tooth surface into a structural defect, and brushing cannot fill it back in. What can “heal” are noncavitated early lesions, where the surface is still intact, typically arrested or reversed with fluoride-based remineralization.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

