What "grow" actually means at age 30
The word "grow" gets used loosely when it comes to teeth, which creates a lot of confusion. There are really four distinct things people could mean. First, eruption: a tooth physically moving through the gum and becoming visible. Second, regeneration: a lost or destroyed tooth structure being rebuilt by the body. Third, remineralization: enamel absorbing minerals from saliva or fluoride to partially repair early surface damage. Fourth, tissue recovery: gum tissue or bone responding to treatment and improving. Each of these is governed by completely different biology, and at 30, not all of them are equally possible.
The myth that needs busting first: your body cannot spontaneously grow a new permanent tooth to replace a missing one. There is no dormant "third set" of teeth waiting to emerge. Once your adult teeth are in, that developmental window is closed. This isn't a dental opinion, it's basic human biology, and understanding that boundary is the starting point for making smart decisions about what actually can be done.
Why adult teeth don't regenerate (the biology, explained simply)
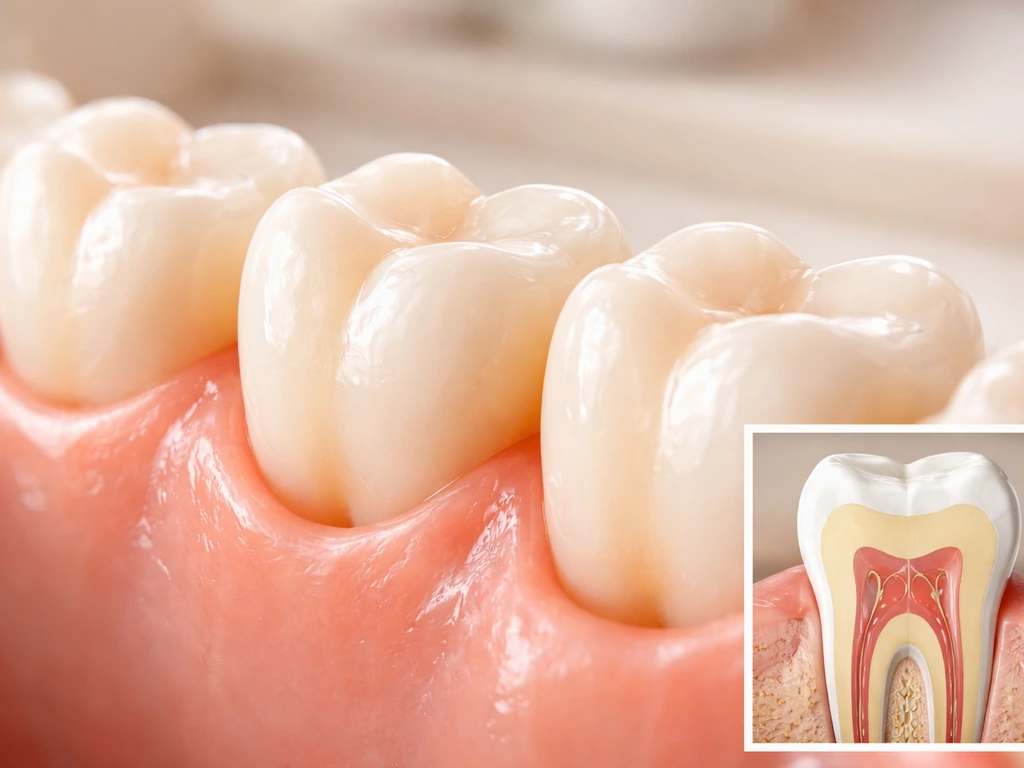
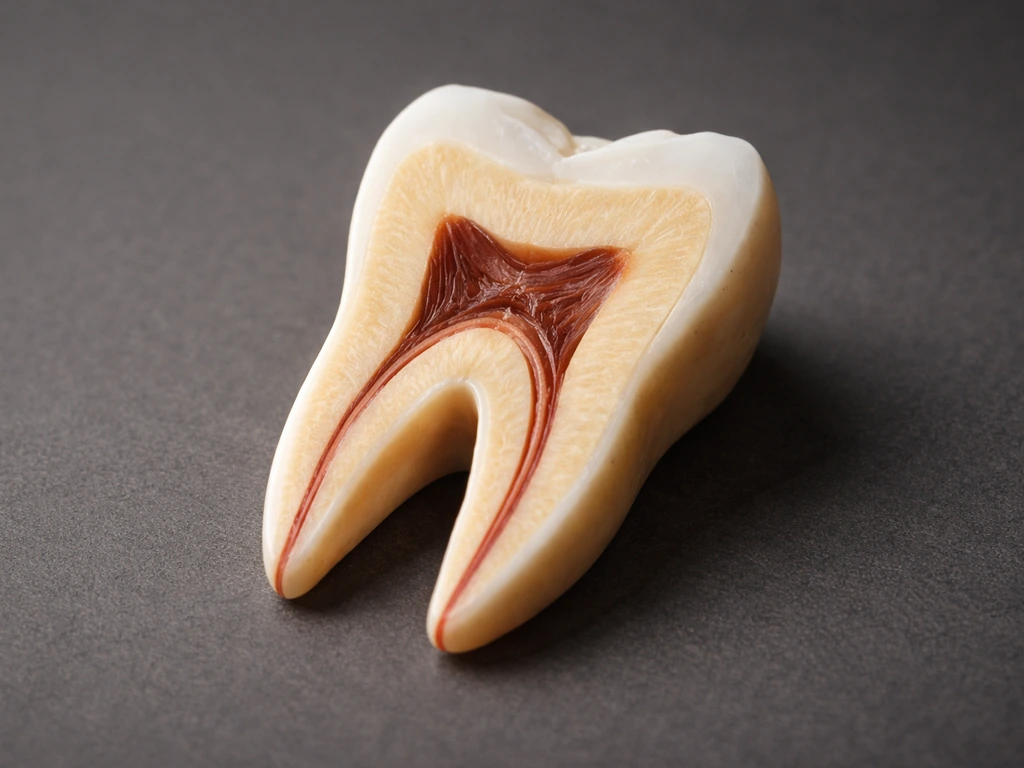
Your teeth develop in stages before and shortly after birth, guided by specialized cells. Enamel, the hard outer layer, is built by cells called ameloblasts. The critical detail: ameloblasts are completely lost when a tooth erupts into the mouth. Once they're gone, they're gone. Research published in the International Journal of Oral Science confirms that adult human teeth cannot regenerate enamel beyond superficial remineralization from saliva, precisely because those enamel-forming cells no longer exist. The same logic extends to the deeper tooth structure. Dentin (the layer beneath enamel) has limited self-repair capacity through a process called tertiary dentin formation, but this is a slow, reactive response to irritation, not true regrowth of lost tooth material.
Regenerative endodontics, a field you might have heard about, is sometimes misunderstood as a way to "regrow" teeth. In reality, the American Association of Endodontists describes these procedures as biologically based treatments specifically for necrotic immature permanent teeth, where the goal is continued root development in younger patients, not replacement of lost enamel or dentin in fully developed adult teeth. The evidence base for this field targets immature tooth biology, not the anatomy of a fully erupted adult molar in a 30-year-old.
So why do people keep asking whether teeth can grow back? Partly because gums can change visibly, partly because teeth can shift position, and partly because the wellness industry is full of products claiming to "remineralize" or "rebuild" teeth. The biology doesn't support the marketing claims, but it does support some genuinely useful, more modest processes, which we'll cover next.
What can still change at 30: remineralization, gum tissue, and eruption
Even though true regrowth is off the table, three things can genuinely change at 30, and they matter a lot clinically.
Enamel remineralization
Early, noncavitated carious lesions (the kind that haven't yet broken through enamel into a cavity) can be arrested and partially remineralized. The ADA's evidence-based clinical guidelines recommend sealants plus 5% sodium fluoride varnish applied every 3 to 6 months as the primary approach for noncavitated active lesions. This isn't enamel growing back, it's minerals from saliva and fluoride filling microscopic gaps in weakened enamel. The moment a lesion becomes cavitated, that window closes and a restoration (filling) is needed. So remineralization is real, but it's a narrow, condition-specific repair process, not tooth regrowth.
Gum tissue changes
Gum tissue responds to treatment more meaningfully than enamel does. The American Academy of Periodontology's regeneration workshop consensus confirms that periodontal regeneration in intrabony defects is achievable, with measurable gains in clinical attachment, decreased probing depth, and radiographic bone height improvement on previously diseased root surfaces. Subepithelial connective tissue grafts (SCTG) are considered the gold standard for covering gum recession. That said, the AAP also notes that regeneration potential is significantly affected by factors like smoking, oral hygiene, tooth mobility, and the specific shape of the bone defect. Gum improvements are generally procedural rather than spontaneous; your gums aren't going to re-cover a receded area on their own.
Ongoing eruption
If you still have wisdom teeth that haven't fully erupted, those can continue to move, though the timeline for that is increasingly unfavorable as you age. More on that in the next section.
Wisdom teeth and late eruption at 30
Maxillary third molars (upper wisdom teeth) typically commence clinical eruption between ages 17 and 21, with root formation potentially extending to around age 25. After 25, spontaneous eruption into a functional position is generally unlikely. So if you're 30 and still have an unerupted or partially erupted wisdom tooth, it's probably not going to come in fully on its own, and that matters for your health.
Some people in their 30s and beyond retain wisdom teeth that are symptomless, and research shows a meaningful percentage of patients have them removed for reasons unrelated to pain. But impacted third molars that stay in place aren't risk-free. The American Association of Oral and Maxillofacial Surgeons notes that untreated impacted wisdom teeth can develop fluid-filled cysts or other complications even when they aren't causing obvious symptoms. If you're 30 and have wisdom teeth that were never evaluated, getting an X-ray and a proper assessment is worth doing now rather than waiting for a problem to develop.
It's worth noting that questions about dental changes across different decades are closely related. If you're curious about what happens slightly later in life, the picture for teeth at age 35 follows similar biological rules, with the same limits on natural regrowth applying just as firmly.
Missing a tooth at 30: your realistic options
This is where the conversation gets very practical. If you're missing a tooth (whether from extraction, trauma, or decay), the body isn't going to fill that gap naturally. But you have several solid clinical options, and the right one depends on your bone density, your budget, your timeline, and which tooth is missing.
| Option | How it works | Timeline | Best for |
|---|
| Dental implant | Titanium post placed in jaw bone, topped with a crown | 6–18 months total depending on protocol | Single missing tooth with adequate bone |
| Fixed bridge | Crowns on adjacent teeth support a false tooth between them | 2–4 weeks after prep | Missing tooth with healthy adjacent teeth |
| Partial denture | Removable appliance replacing one or more teeth | A few weeks to fabricate | Multiple missing teeth or budget constraints |
| Full denture | Removable full arch prosthetic | Weeks to months | Full arch tooth loss |
| Orthodontic space closure | Braces or aligners shift adjacent teeth to close gap | 12–24 months | Certain gaps, usually with younger patients |
Implants are generally considered the closest functional replacement for a natural tooth, but the timing matters. One conventional protocol delays implant placement up to a year after extraction to allow complete alveolar bone healing, followed by a load-free osseointegration period of 3 to 6 months. Immediate placement protocols exist but come with their own considerations around ridge modeling and healing. If you're weighing your options and wondering how your choices now might look in ten years, it helps to think ahead: concerns about teeth at age 40 are often directly shaped by decisions made in your 30s, especially around whether to get an implant early or wait.
Bridges are faster and less invasive than implants but require grinding down healthy adjacent teeth, which is a permanent trade-off. Partial dentures are removable and more affordable but require daily maintenance and don't preserve bone the way implants do. There's no universally correct answer; it depends on your specific clinical picture, which is exactly why a dentist consultation is essential before committing to anything.
Damaged tooth at 30: fillings, crowns, root canals, and what regeneration can and can't do
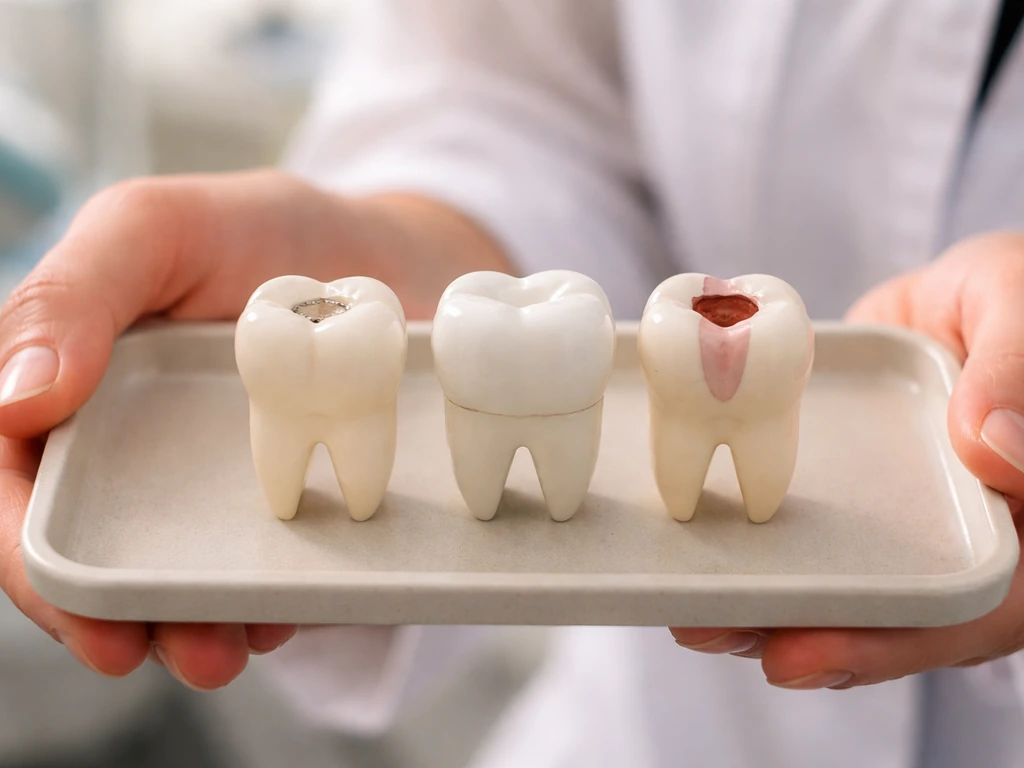
If a tooth is damaged rather than missing, your options are different and often more conservative. The treatment depends on how far the damage has gone.
- Noncavitated lesion (early decay, no visible hole): Fluoride varnish every 3 to 6 months plus sealants can arrest and partially remineralize. No drilling needed.
- Cavitated lesion (actual cavity): A filling is required. The tooth cannot self-repair at this stage.
- Large decay or cracked tooth: A crown is placed over the remaining tooth structure to protect and restore it.
- Decay reaching the pulp (nerve): Root canal therapy removes the infected pulp, the canal is cleaned and sealed, and a crown typically follows.
- Cracked tooth syndrome: Depending on crack depth, treatment ranges from a crown to extraction.
Regenerative approaches like guided tissue regeneration (GTR) are used in periodontal contexts to rebuild bone and attachment around teeth, not to regrow enamel or dentin. Root coverage procedures including GTR and SCTG show measurable gains in clinical studies, but these address gum and bone, not the tooth structure itself. True regeneration of tooth material in a fully adult tooth remains experimental. Cell-based and biomaterial research is ongoing, but nothing is clinically available today that regrows a cavity in a 30-year-old's molar.
It's also worth zooming out on the developmental timeline to understand why this matters. The biology of tooth regrowth is fundamentally different depending on age. The changes that are possible in adolescence, covered in detail for those curious about teeth growing after age 15, simply do not carry forward into your 30s in the same way. By 30, the developmental biology has largely run its course.
What to do right now: your practical next steps
If you landed on this article because something specific is going on with your teeth, here's how to think about your next move.
When to see a dentist (and who)
If you have a missing tooth, see a general dentist or a prosthodontist. If you have gum recession or bone loss, ask for a referral to a periodontist. If a wisdom tooth is still in question, an oral and maxillofacial surgeon or your general dentist can evaluate it. Don't put off an evaluation, especially for wisdom teeth. Complications from impacted third molars can develop silently, and the longer you wait, the fewer options you may have.
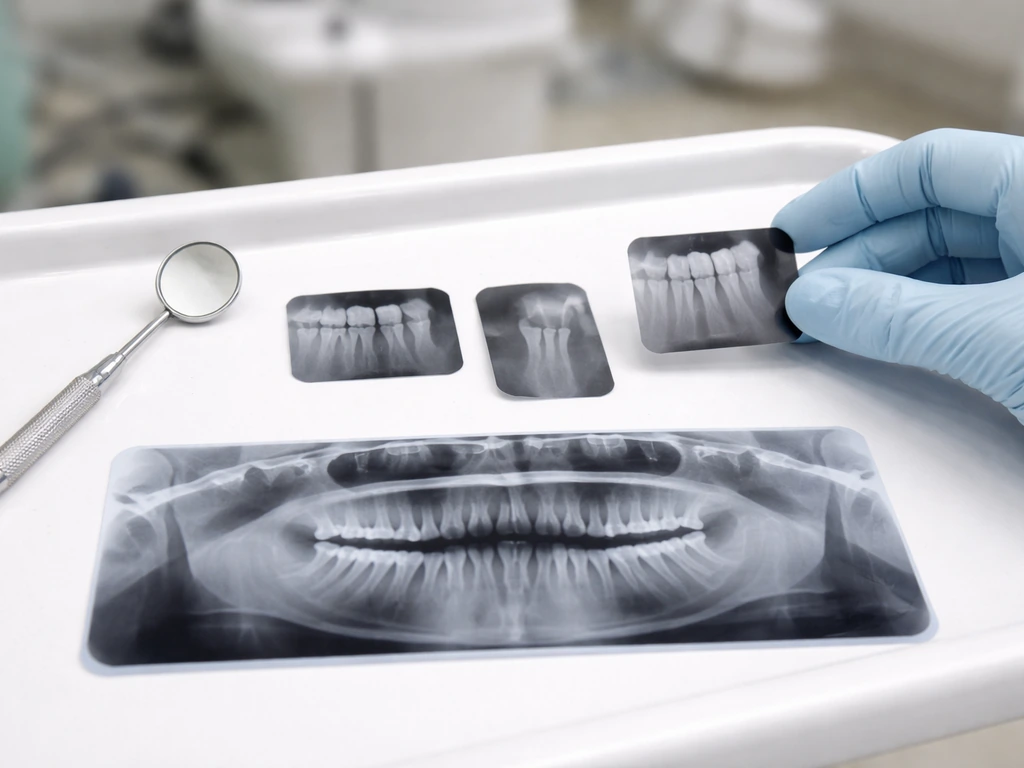
What imaging to expect
Your dentist will likely take bitewing and periapical X-rays to evaluate decay and bone levels. Panoramic radiographs are useful for assessing unerupted teeth and overall jaw anatomy. For more complex cases involving implants or endodontic concerns, cone beam CT (CBCT) may be recommended based on specific clinical indications rather than routine use. The FDA notes that periapical and occlusal views are particularly helpful for detecting unerupted or impacted teeth. Come prepared to have current X-rays taken if you don't already have recent ones.
Questions to ask your dentist
- Is this lesion cavitated or noncavitated? (This determines whether a filling is needed or whether remineralization is still possible.)
- Do I have any signs of periodontal disease, and if so, what's the extent?
- Are my wisdom teeth fully developed and positioned safely, or do they need to be monitored or removed?
- If I need an implant, when should placement happen given my current bone structure?
- Am I a candidate for nonsurgical gum treatment, or would I benefit from a periodontal referral?
Red flags that need prompt attention
- Tooth pain that lingers after eating or drinking hot or cold (possible pulp involvement)
- Swelling in the gum or jaw near a wisdom tooth (possible infection or cyst)
- Spontaneous bleeding when brushing, especially if consistent (a sign of active gum disease)
- A tooth that feels loose (bone loss, periodontal disease, or trauma)
- Visible dark spots or holes in teeth (cavitated lesions that need restoration)
Bleeding on probing is a key clinical marker used during periodontal evaluations to track disease activity, alongside clinical attachment level measurements. These aren't just numbers on a chart; they tell your provider whether your gum situation is stable or actively getting worse.
If you're wondering whether any of this changes much as the years go on, the short answer is that the fundamental biology stays the same. For a deeper look at what the research says about whether teeth grow after age 30, the conclusions are consistent: the window for natural dental development is closed, but the options for restoration, regeneration, and repair through clinical care remain meaningful well into adulthood.
The bottom line: at 30, your teeth aren't going to regrow on their own, but that doesn't mean you're out of options. Early decay can still be arrested. Gum tissue can be restored with the right procedures. Missing teeth can be replaced with implants or prosthetics that function almost as well as natural teeth. The key is getting an accurate picture of your specific situation from a qualified clinician, understanding which category your problem falls into (eruption, damage, or loss), and then choosing the treatment path that fits your biology, timeline, and goals. That's a much more useful frame than hoping something will grow back on its own.