Humans can't grow new permanent teeth after losing them because once the second set of teeth is fully developed, the biological machinery that built those teeth simply shuts down and doesn't restart. There's no dormant third set waiting in your jaw. The tooth-forming cells that created your adult teeth are gone, the signaling pathways that organized tooth growth are no longer active, and nothing in your body can spontaneously rebuild a lost molar or incisor from scratch. That's the plain truth, and the rest of this article explains exactly why, what can and can't naturally recover, and what you can actually do about it today.
Why Can’t Humans Grow More Teeth and What to Do Now
How your teeth actually form (and why that matters)
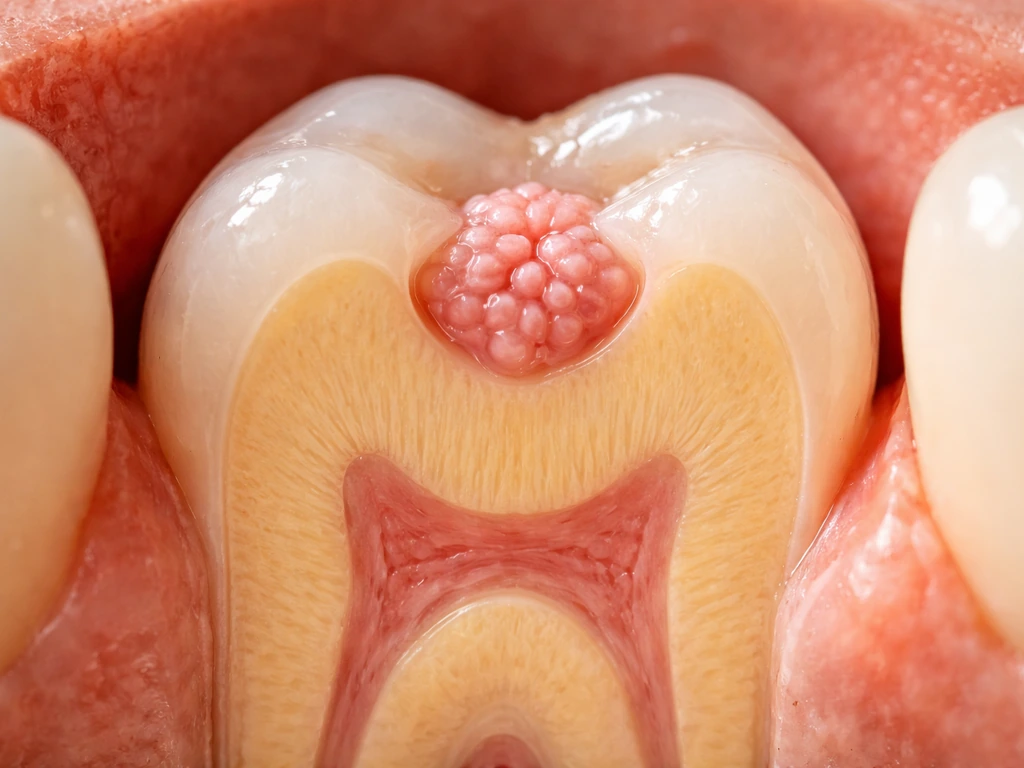
To understand why teeth can't come back, you first have to understand how they're built in the first place. Tooth development is an intricate, tightly timed process driven by conversations between two types of tissue: dental epithelium (which becomes the enamel-producing layer) and dental mesenchyme (which becomes the dentin, pulp, and root-supporting structures). These two tissues exchange chemical signals at very specific stages of development, and that back-and-forth is what builds a tooth with the right shape, hardness, and root structure.
Early in the process, clusters of epithelial cells called enamel knots act as signaling centers that direct cusp formation and overall tooth shape during what dentists call the cap and bell stages of development. A little later, a structure called Hertwig's Epithelial Root Sheath (HERS) forms and grows downward, sending out signals that tell neighboring cells to differentiate into odontoblasts, which then lay down the dentin that forms the tooth's root. It's a beautifully coordinated sequence, and every major tooth structure has a specific cell type that builds it.
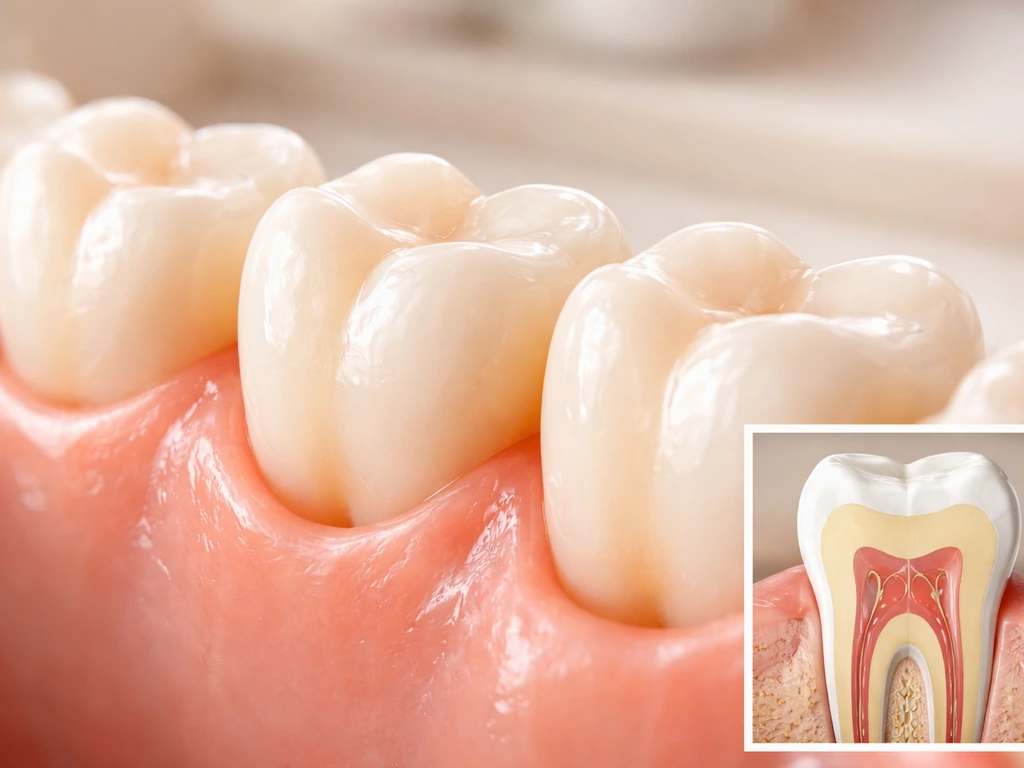
Enamel is made by ameloblasts. Dentin is made by odontoblasts. The pulp (the living nerve and blood vessel core) is built from dental papilla cells. The periodontal ligament, cementum, and surrounding bone that anchor the tooth are formed from the dental follicle. Each of these cell populations appears, does its job during development, and then either disappears or becomes a resting support tissue. Critically, the ameloblasts that build enamel are entirely lost once the tooth erupts. That's why enamel can't regrow, ever. Odontoblasts do persist inside the pulp and can form small amounts of secondary dentin as a defensive response to decay or wear, but they can't build a new tooth or even fully rebuild a large area of lost dentin.
Why permanent teeth don't grow back after they're lost
The biological bottleneck is simple: by the time all your permanent teeth have fully erupted (typically by your early twenties, counting wisdom teeth), the tooth-development program is finished. The epithelial-mesenchymal signaling interactions that are absolutely required to initiate a new tooth germ just don't happen again in adult human jaws. There's no new placode forming, no new enamel knot organizing cusp shape, no HERS migrating downward to signal root formation. The instruction manual closed.
Contrast this with animals like sharks, which have polyphyodonty, meaning continuous tooth replacement throughout life, because their dental epithelium keeps a permanent reserve of stem-like cells cycling through tooth production. Elephants cycle through multiple sets of molars. Crocodiles can replace teeth dozens of times. Humans are diphyodonts: we get exactly two sets and that's it. The evolutionary trade-off is thought to involve the precision and complexity of our teeth. Producing finely shaped, deeply rooted permanent teeth appears to have come at the cost of the continuous replacement ability seen in simpler dentitions.
There's also a physical space argument. Once your permanent teeth erupt and the jaw finishes growing, there's simply no reservoir of tissue primed to produce new tooth germs. Even if you could somehow restart the signaling pathways, there's no organized pool of dental epithelial stem cells in an adult human jaw that could respond to those signals the way embryonic tissue would. A few researchers have found vestigial remnants of dental lamina (the tissue strip that originally seeds tooth formation) in adult human jaws, and these are being studied, but they are not functional tooth factories in any current sense.
Kids versus adults: why losing a tooth means something very different

When a six-year-old loses a tooth, it feels like a big deal, but biologically it's completely routine. Baby teeth (primary teeth) are placeholders. The permanent tooth germ is already forming underneath each one, and the roots of the baby tooth are actually being resorbed by the body as the permanent tooth pushes up. Losing a baby tooth is not tooth loss in the permanent sense; it's just the handoff between set one and set two. Kids get that luxury because the second set of teeth is already in progress.
Adults get no such handoff. When a permanent tooth is lost to decay, trauma, or gum disease, the socket heals over, the surrounding bone gradually resorbs from lack of stimulation, and nothing is coming to fill that gap. The permanent tooth was the last scheduled arrival. This is why adult tooth loss is taken so seriously in dentistry: every lost permanent tooth is permanent. The timeline matters too. Bone loss in the socket where a tooth was extracted can begin within weeks and accelerates over the first year, which affects what treatment options remain available later.
In children, even losing a primary tooth too early (through decay or trauma, before the permanent tooth is ready to erupt) can cause problems, because neighboring teeth may drift into the gap and block the incoming permanent tooth. This is why pediatric dentists sometimes use space maintainers when baby teeth are lost prematurely. The biology is working in a child's favor, but it still requires some management.
What actually can recover naturally (and what absolutely cannot)
This is where a lot of internet misinformation lives, so let's be direct about the line between real recovery and wishful thinking.
What can genuinely recover or improve
- Enamel remineralization: early-stage enamel erosion (white spot lesions, minor surface softening) can be partially reversed with fluoride, calcium phosphate products, and improved oral hygiene. This is not regrowing enamel from scratch; it's redepositing minerals into partially demineralized enamel that still has its structural matrix intact. Once a cavity forms through the enamel layer, remineralization cannot fill it back.
- Gum tissue healing: after a minor injury or a tooth extraction, gum tissue can close over the socket and heal relatively well. Gum tissue is soft tissue and has a reasonable blood supply to support repair.
- Cementum and periodontal ligament: with treatment for periodontal disease, some limited regeneration of the fibers attaching teeth to bone is possible, especially with guided tissue regeneration procedures. This is not regrowth of a whole new support system, but it's meaningful clinical improvement.
- Secondary dentin: the pulp's odontoblasts can lay down small amounts of tertiary (reparative) dentin in response to mild irritation or slow decay, essentially forming a defensive barrier. This is a protective response, not tooth reconstruction.
What cannot grow back under any natural circumstances
- Enamel that has been lost through a cavity, fracture, or severe erosion cannot regrow. Ameloblasts are gone after tooth eruption.
- A lost tooth. Once a permanent tooth is extracted or knocked out and cannot be replanted, no biological process will fill that space with a new tooth.
- Large sections of lost dentin. Small defensive deposits are possible, but if a cavity has progressed deeply, the lost structure needs a filling, crown, or other restoration.
- Significant lost jawbone around a tooth. While bone grafting procedures can rebuild lost bone surgically, the jaw does not regenerate lost bone on its own after tooth loss.
Your real options right now if you've lost a tooth
If you're reading this because you've lost a tooth or are facing tooth loss, the good news is that modern dentistry has excellent ways to restore function and appearance. The right choice depends on your specific situation, how many teeth are involved, your bone density, budget, and timeline.
| Option | How it works | Best for | Key consideration |
|---|---|---|---|
| Dental implant | A titanium post is surgically placed into the jawbone and a crown is attached on top | Single missing teeth or multiple teeth in good bone; most durable long-term solution | Requires adequate bone density; takes 3 to 6+ months total; higher upfront cost |
| Fixed dental bridge | An artificial tooth is anchored to crowns placed over the two adjacent natural teeth | One or two missing teeth with healthy neighboring teeth on each side | Adjacent healthy teeth must be permanently altered; doesn't prevent bone loss in the gap |
| Partial or full denture | A removable appliance that replaces one or several teeth (partial) or all teeth (full) | Multiple missing teeth or full arch replacement; more affordable option | Removable; may feel less natural; bone resorption continues underneath |
| Implant-supported denture | A full denture anchored by two to four implants rather than suction or adhesive | Patients needing full arch replacement who want more stability than conventional dentures | Surgical procedure required; significantly more stable than traditional dentures |
| Orthodontics | Braces or aligners to shift remaining teeth, sometimes to close a gap or prepare for another restoration | Minor gaps, preparation for other treatment, or specific bite corrections | Not a standalone tooth-replacement solution; used alongside or before other options |
If a tooth has been knocked out very recently (within the last hour), there's actually one urgent step: try to replant it yourself by placing it gently back in the socket without scrubbing the root, or store it in milk or saliva and get to an emergency dentist immediately. Reimplantation can work if done fast enough, and the root's periodontal ligament cells can potentially reattach. This window closes quickly, so don't wait.
For everyone else dealing with decay, a cracked tooth, or a recently extracted tooth, the first step is a consultation with a dentist who can take X-rays, assess the bone level, and walk you through the options that actually make sense for your specific situation. There's no universal right answer, but there are definitely better and worse choices depending on your age, overall dental health, and what's happening with the neighboring teeth and bone.
The science of growing new teeth: where research actually stands
Yes, scientists are actively working on bioengineered teeth and stem-cell-based approaches to tooth regeneration. Some of the progress is genuinely exciting. But it's important to understand what stage this research is at, because claims online range from overblown to outright false.
The core challenge for researchers is replicating the embryonic epithelial-mesenchymal signaling environment inside an adult jaw. In lab settings and animal models, scientists have been able to use dental epithelial and mesenchymal cells to grow tooth-like structures that have some enamel and dentin organization. Whole-tooth regeneration has been achieved in mice by implanting engineered tooth germs into the jaw, where the structure then erupted and integrated. That's real and impressive. But mice are not humans, mouse jaws are very different from human jaws, and the jump from a mouse model to a clinically available human treatment is enormous.
Some researchers are investigating small molecule drugs that could potentially reactivate dormant tooth-forming pathways. In 2023 and 2024, a Japanese research team made significant headlines with a drug targeting the USAG-1 protein, which suppresses tooth growth. In animal trials, blocking this protein led to the growth of additional teeth. Human clinical trials were being planned as of early 2025. This is promising, but it's still in early phases, and even if trials succeed, regulatory approval and practical clinical application take years.
The reasons these approaches aren't standard yet come down to a few honest barriers. First, safety: any intervention that reactivates developmental signaling in adult tissue carries risks that have to be characterized very carefully before use in humans. Second, precision: growing a tooth with the right shape, root length, and position in a specific gap in a specific adult patient's jaw is dramatically harder than growing one in a controlled lab environment. Third, scale: even successful techniques need to become reproducible and manufacturable enough to be offered broadly. None of these barriers are impossible, but they are real, and none of them will be solved in the next year or two.
If you see a headline claiming that tooth-regrowing pills or serums are available now, be skeptical. As of 2026, no bioengineered tooth or stem-cell tooth-regeneration treatment has completed human clinical trials and received approval for routine dental use. That said, researchers are still working on tooth-regeneration approaches, but today there is no approved way to grow another adult tooth in a human mouth tooth regeneration. As of 2026, there still isn't a proven clinical treatment that answers when we will be able to grow new teeth As of 2026, no bioengineered tooth or stem-cell tooth-regeneration treatment has completed human clinical trials and received approval for routine dental use.. As of now, can humans grow new teeth is still an active area of research, but it is not something most people can rely on today. The research is moving, but we're still years away from anything a dentist could offer you as a standard appointment. For now, implants remain the closest thing to a "permanent" tooth replacement that modern dentistry offers, and they're genuinely excellent when placed well.
The bottom line on tooth regrowth and what to do next
Humans only get two sets of teeth because our tooth-forming biology runs a finite, tightly sequenced program that ends in early adulthood and cannot restart. Once a permanent tooth is gone, nothing in the body is positioned to replace it naturally. Minor surface-level minerals in enamel can be partially restored with fluoride and good hygiene, gum tissue can heal, and some periodontal support can be partially recovered with treatment, but none of that is the same as growing a new tooth.
If you've lost a tooth or are at risk of losing one, the most useful thing you can do right now is see a dentist promptly. The longer you wait after tooth loss, the more bone resorption occurs, and the fewer straightforward options remain. Implants, bridges, and dentures are all proven, practical solutions available today. Bioengineered teeth and drug-based tooth regeneration are genuinely exciting areas of research, and worth watching, but they're not a reason to delay treatment now.
Understanding why humans only grow two sets of teeth, and why permanent teeth don't grow back after they're lost, helps frame realistic expectations. There's no secret supplement, no oil pulling routine, and no technique that coaxes a new permanent tooth out of an adult jaw. That's not pessimism; it's just biology. Working with what modern dentistry offers today is the most practical, evidence-based path forward.
FAQ
If I lose a permanent tooth, can it grow back naturally if I improve my oral hygiene right away?
Improving hygiene can slow further bone and gum damage, but it does not restart the tooth-forming program in an adult jaw. The main benefit is preventing additional tooth loss and keeping the surrounding tissues in better condition for options like implants or bridges.
What happens if I wait too long after losing a tooth, like months or years?
Bone resorption and soft-tissue shrinkage can make replacement more complex. Longer delays increase the chance you will need procedures to rebuild bone or adjust the gums before you can place an implant or make a stable bridge, whereas earlier treatment often keeps the options simpler.
Can I grow a new tooth by treating an exposed root, like with a filling, crown, or root canal?
Those treatments can save the tooth if enough structure and periodontal support remain, but they do not create a new tooth germ. A root canal addresses the nerve and infection risk, it does not regenerate enamel, dentin, or the periodontal ligament that anchors a whole new tooth.
Are wisdom teeth able to “replace” missing molars later in life?
Wisdom teeth can erupt late, but they are not a biological replacement for a specific missing tooth, and they cannot be relied on for that purpose. Whether they will help depends on spacing, jaw size, angulation, and whether the other teeth have already shifted, which are things an X-ray can show.
If a baby tooth is lost early, will a space maintainer always be needed?
Not always. Some early losses are followed well enough by natural eruption timing, but others lead to drifting that blocks the incoming permanent tooth. A pediatric dentist weighs the child's age, how many teeth are missing, and how far the permanent tooth is from eruption before deciding.
What’s the most important action after a knocked-out tooth (avulsion)?
Time matters, but handling matters too. Do not scrub the root, keep the tooth moist (milk, saline, or saliva), and get emergency dental care as soon as possible so clinicians can assess whether reimplantation or other urgent steps are appropriate.
Do dental implants count as “permanent,” and do they last a lifetime?
Implants are designed to be long-term, but “permanent” depends on maintenance and oral health. Gum disease, poor bite forces, smoking, and inadequate follow-up can threaten implant support, so long-term success requires regular cleaning and checkups.
Are there any legitimate signs that tooth regeneration is actually happening in humans?
As of now, there is no routine, clinically approved method that grows a whole new adult tooth in the mouth. Any claims of a regenerated tooth should be treated as suspect unless they are tied to controlled clinical trials with clear documentation of what tissues formed and whether the tooth integrated normally.
Can minor enamel loss be reversed without growing a new tooth?
You cannot regrow enamel the way a tooth forms in development, but small mineral losses can sometimes be slowed or reversed. Fluoride, remineralizing agents, and stopping active decay can harden early lesions, while cavitated areas typically still require restorative work.
If USAG-1 or stem-cell therapies work someday, would they work for everyone equally?
Not necessarily. Even if a future therapy can stimulate tooth-forming pathways, success will likely depend on factors like the presence of adequate jaw bone, the state of local tissues, age, and how long it has been since tooth loss. These practical constraints are part of why translation from animal models to patients is difficult.
Myth-busting answer on whether adults can regrow teeth, plus real options like implants, crowns, and orthodontics.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Evidence on whether teeth can truly regrow at 30, what can change, and realistic options for missing or damaged teeth.

