Dermoid cysts don't actually grow teeth the way your jaw does. What they do is far stranger: they can contain tooth-like structures that formed during fetal development, built from the same raw biological material that makes real teeth. The cyst itself slowly expands over time, which makes it seem like something is 'growing' inside it. Those tooth-like pieces aren't erupting, they aren't new teeth, and they have nothing to do with dental regeneration. They're developmental leftovers trapped in a cyst that the body never reabsorbed.
How Do Dermoid Cysts Grow Teeth? Causes, Symptoms, Treatment
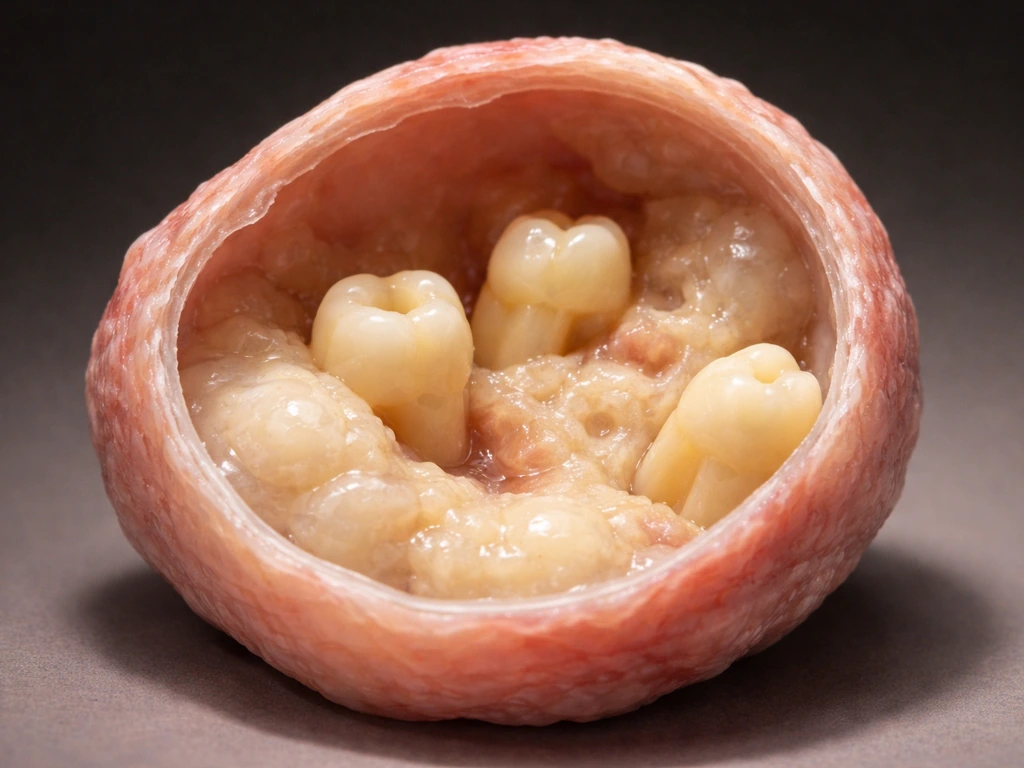
What a dermoid cyst actually is and where it shows up
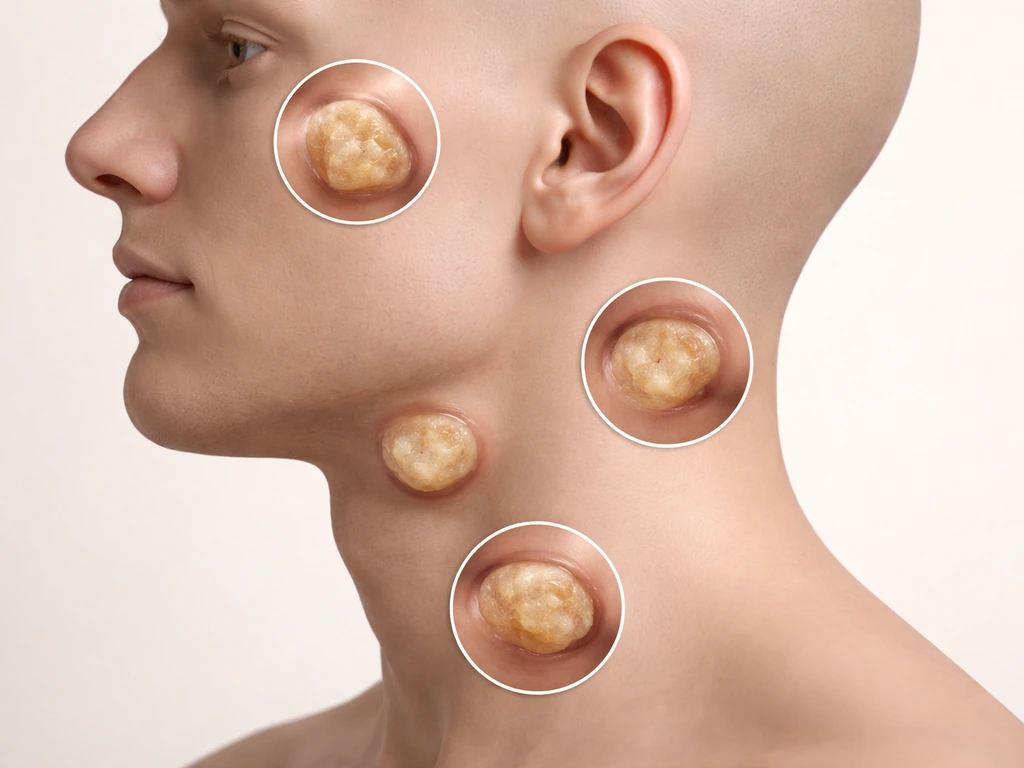
A dermoid cyst is a developmental cyst, meaning it forms during fetal development rather than appearing later due to an infection or injury. It's lined by stratified squamous epithelium (basically skin-like tissue) and its wall can contain mature skin structures like hair follicles, sebaceous glands, and eccrine sweat glands. Inside, you'll often find keratin, hair, and oily sebaceous material. If you are wondering whether tonsil stones can develop overnight, the timeline can feel fast, but it depends on factors like bacteria, debris buildup, and throat dryness can tonsil stones grow overnight. Think of it as a small pocket of skin that got enclosed in the wrong place during embryonic development.
Histologically, doctors distinguish between three types. An epidermoid cyst has only squamous epithelium lining. A true dermoid cyst has skin adnexal structures in the wall. A teratoid cyst contains tissues from all three embryonic germ layers: ectoderm, mesoderm, and endoderm. It's in that teratoid category where you're most likely to see organized dental tissue. For everyday conversation, though, people use 'dermoid cyst' as a loose umbrella term for all three.
In the head and neck, these cysts arise along the lines where embryonic tissue fused together during development. The most common spots are the periorbital area (especially the outer eyebrow region), the midline scalp, the nasal bridge, and the floor of the mouth. For the maxillofacial region specifically, the majority of true oral dermoid cysts appear in the sublingual or submental spaces, right at the midline of the floor of the mouth. They can also appear on the tongue, buccal mucosa, lips, uvula, and in rare cases, within bone itself. Nasal dermoid cysts are actually the most common midline congenital nasal malformation, and roughly 10 to 45 percent of them extend intracranially, which is why they're taken seriously even when they look small.
How tooth-like structures can form inside a dermoid cyst
Here's the part people find hardest to wrap their heads around. Teeth don't just pop up inside a cyst randomly. What happens is that embryonic tissue with the potential to become tooth-forming cells gets enclosed in the cyst during that critical window of fetal fusion. Given the right conditions inside the cyst, that tissue can differentiate into enamel-producing ameloblasts and dentin-producing odontoblasts, the exact same cell types that build your actual teeth. The result is calcified, tooth-like material, sometimes resembling a complete tooth structure, sometimes just fragments of enamel or dentin.
This is only possible in teratoid cysts because they contain tissue from multiple germ layers. Tooth development normally requires coordinated interaction between oral ectoderm and neural crest-derived mesenchyme. When both types of embryonic tissue end up enclosed together in a cyst, that developmental conversation can still happen, just in the wrong location. The resulting structures can look remarkably like real teeth on imaging, which is often how they're first discovered.
Why it looks like teeth are 'growing' from the cyst
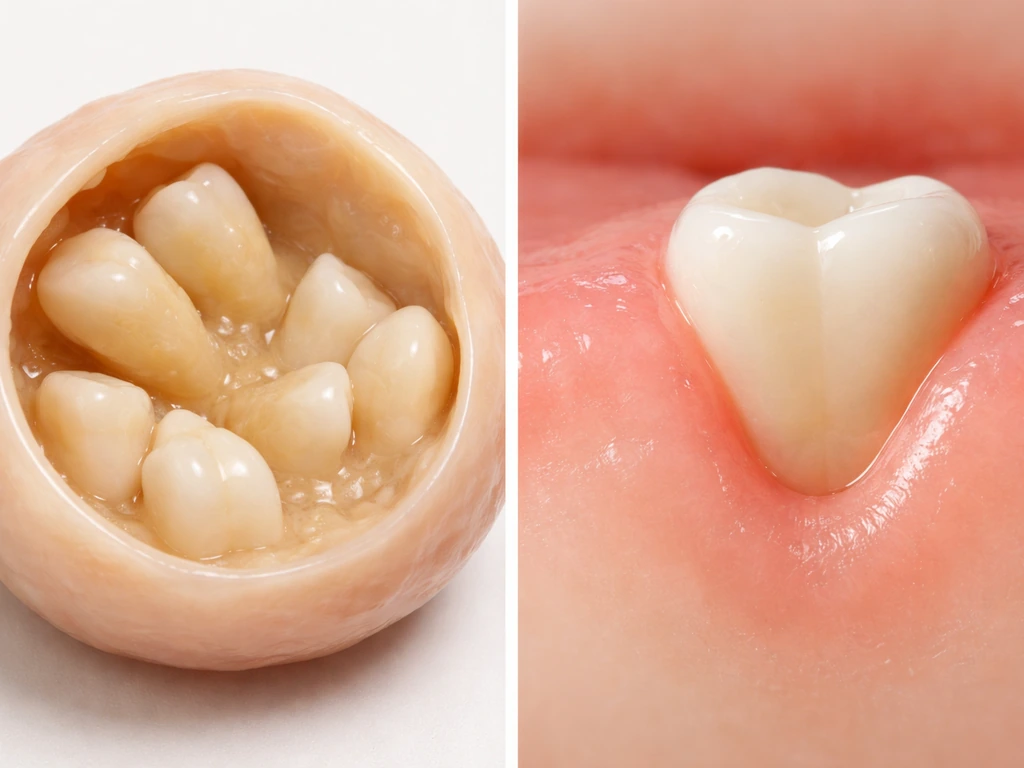
This is the core misconception worth clearing up. The tooth-like structures inside a dermoid cyst are not erupting. They are not regenerating. They formed early in fetal development and have been sitting there ever since. What changes over time is the cyst itself. Dermoid cysts slowly accumulate more keratin and sebaceous secretions as the epithelial lining continues to function like skin. The cyst wall expands. As the cyst grows, it can push tooth-like calcified material in ways that might make it seem like something is emerging or moving. That's the cyst growing, not the tooth growing.
This is fundamentally different from anything happening in your actual mouth. On this site we talk a lot about why dental regeneration is so limited in humans: once adult teeth are lost, they don't grow back, enamel doesn't regrow, and the body has essentially no mechanism for producing a new tooth in your jaw after development is complete. A dermoid cyst exploits a developmental window that closed the moment fetal development finished. It's not a regeneration phenomenon at all. It's closer to what happens with ovarian dermoids, where teeth and hair form from misplaced developmental tissue, a comparison worth noting if you've read about why ovarian cysts sometimes grow teeth.
How common this is and what symptoms you might notice
Dermoid cysts in the head and neck are not as rare as you might think, though ones containing actual tooth-like structures are less common than the basic keratin-filled variety. A Mayo Clinic review of pediatric head-and-neck dermoid cysts covering cases from 1980 to 2002 identified 49 patients, with a median age at diagnosis of just 22 months. That tells you something important: these cysts are often congenital and many are caught in early childhood, though some aren't discovered until adulthood when they've grown large enough to cause noticeable symptoms.
The most typical presentation is a slow-growing, soft, doughy lump, often in the midline of the neck, floor of the mouth, or around the eye. It usually doesn't hurt unless it gets infected. Floor-of-mouth dermoid cysts can cause the tongue to be pushed upward, creating difficulty swallowing or speaking. Nasal dermoids may produce a visible pit or dimple on the nasal bridge, sometimes with hair protruding from it. Signs that something is going wrong, meaning the cyst is infected or has ruptured, include sudden redness, warmth, pain, and drainage of cheesy or foul-smelling material.
- A slow-growing, painless lump in the midline neck, floor of mouth, or periorbital area
- A soft, doughy texture (often described as feeling like a rubber ball)
- Difficulty swallowing or speaking if the cyst is in the floor of the mouth
- A visible pit or small opening on the nose bridge (nasal dermoid)
- Occasional drainage of keratin or sebaceous material
- Sudden pain, redness, or swelling if the cyst becomes infected
What actually causes the cyst to expand over time
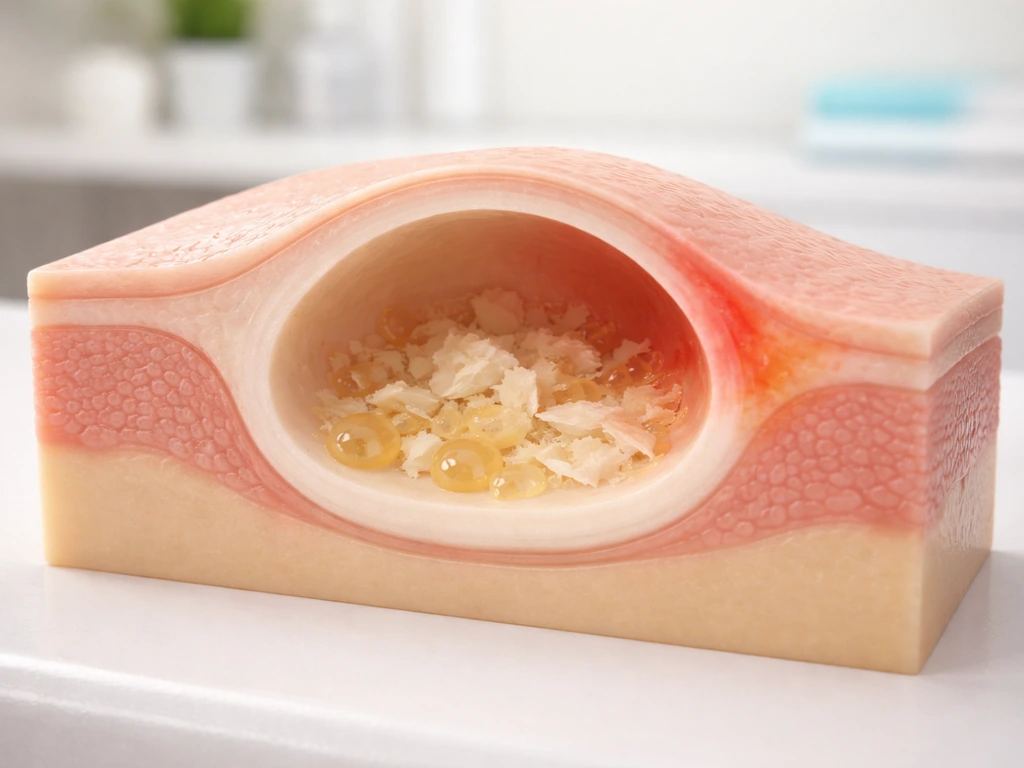
The epithelial lining of a dermoid cyst behaves like skin. It continuously sheds keratin and produces sebaceous secretions into the enclosed space. Since there's nowhere for this material to go, it accumulates and the cyst expands. This is a slow process, often over years or even decades, which is why many dermoid cysts are small at birth or in infancy and only become symptomatic in childhood or early adulthood. The expansion isn't driven by the calcified tooth-like material getting larger. Those structures are already formed. The growth is purely from the accumulating soft contents of the cyst cavity.
Infection dramatically accelerates this timeline. If bacteria enter the cyst (through a sinus tract, skin injury, or rupture), the subsequent inflammation and swelling can cause rapid enlargement in days rather than years. This is when most people suddenly notice a cyst that was previously subtle or undetected.
How doctors diagnose a dermoid cyst and confirm tooth material inside
Physical exam is often the starting point. A skilled clinician can frequently suspect a dermoid cyst just from location, texture, and the patient's age. But imaging is what confirms it, and imaging is also how calcified tooth-like structures get detected. Ultrasound is usually the first-line tool in pediatric cases because it's radiation-free and can characterize the cyst's contents. CT (computed tomography) is the gold standard for identifying calcified material inside the cyst, including tooth-like structures, and it's essential for nasal dermoids where intracranial extension needs to be ruled out. MRI adds detail about soft tissue involvement and is particularly useful when surgery is being planned near critical structures.
On CT, calcified tooth-like structures appear as dense, bright white material within the cyst. The shape can be unmistakably tooth-like. Radiology reports will typically describe 'calcifications' or 'a calcified density consistent with dental tissue.' Final confirmation of what the tissue actually is comes from histopathology: a pathologist examines the surgically removed cyst under a microscope and can identify enamel matrix, dentin, pulp tissue, or other dental structures. That's the definitive answer.
| Imaging Method | What It Shows | Best Used For |
|---|---|---|
| Ultrasound | Cyst size, internal echogenicity, wall characteristics | Initial pediatric evaluation, no radiation |
| CT scan | Calcified material, bone involvement, extent of cyst | Detecting tooth-like structures, nasal dermoids with possible intracranial extension |
| MRI | Soft tissue detail, fat-containing cyst contents, relationship to nearby structures | Surgical planning, complex locations |
Treatment options and what you absolutely should not do at home

Surgical removal is the standard treatment for virtually all dermoid cysts that are symptomatic, growing, or contain tooth-like material. The goal is complete excision of the cyst and its entire lining. If any lining remains, the cyst will come back. For floor-of-mouth cysts, the approach is usually intraoral (through the mouth) if the cyst is small, or extraoral (through a neck incision) for larger ones. Nasal dermoids often require more complex surgery depending on whether there's intracranial involvement. The removed cyst is always sent to pathology for analysis, which is how you get definitive confirmation of the contents.
Timing matters mostly when there's infection. An actively infected cyst is typically treated first with antibiotics and sometimes drainage, then surgically removed once the infection has cleared. Attempting definitive excision through infected tissue significantly increases the risk of incomplete removal and recurrence.
On the home front: do not try to drain, squeeze, or puncture a dermoid cyst yourself. Unlike a garden-variety pimple, a dermoid cyst is deep, has a distinct lining that must be removed surgically, and squeezing it risks rupturing the cyst wall, which causes the contents to spill into surrounding tissue and can provoke a severe inflammatory reaction or introduce infection. This is not a wait-and-see situation if the cyst is growing, causing symptoms, or has any signs of infection.
Dermoid teeth vs. real tooth regeneration: these are completely different things
If you came here from questions about whether teeth can regrow, it's worth being explicit: what happens in a dermoid cyst has nothing to do with tooth regeneration. The tooth-like structures in a dermoid cyst formed during embryonic development, from misplaced tissue, in a completely abnormal location, decades before anyone noticed the cyst. Because these tooth-like pieces are trapped leftovers, you can't tell they are real teeth or expect them to grow like teeth in your mouth can worms grow in your teeth. They are not a sign that the body can generate new teeth. They are a sign of a developmental error that occurred before birth.
True tooth regeneration in the mouth, meaning regrowing a lost tooth, a lost root, or lost enamel from normal dental biology, is something humans essentially cannot do after the adult dentition is established. The dental stem cells and signaling pathways that build teeth during development are no longer active in a functional way in adult jaw tissue. A dermoid cyst is the accidental activation of those pathways in an enclosed developmental remnant, not evidence that the process can be restarted in your mouth. They're related only in that both involve the same original cell types. The context is entirely different.
If you've been reading about structures like tonsil stones or other tissue accumulations that seem to 'grow' in unexpected places, the principle is similar: the body sometimes deposits or accumulates mineralized or structured material in locations that seem surprising, but the mechanism is almost always either developmental misplacement or accumulation of byproducts, not true tissue regeneration. A dermoid cyst with tooth-like material is one of the most dramatic examples of the developmental misplacement category.
Your next steps if you suspect a dermoid cyst
If you or your child has a slow-growing lump in the midline of the neck, floor of the mouth, around the eye, or on the nasal bridge, see a doctor. A general practitioner can do an initial evaluation and refer you to the right specialist, usually an oral and maxillofacial surgeon, an ENT (otolaryngologist), or a pediatric surgeon depending on location. Don't wait for symptoms to worsen. Dermoid cysts that are caught before they become infected are considerably easier to remove completely, which reduces the chance of recurrence. If imaging has already shown calcified material inside the cyst, bring those reports to the surgical consultation. The presence of tooth-like structures doesn't change the fundamental treatment approach, but it does confirm what type of cyst you're dealing with and helps the surgeon know what to expect.
FAQ
Do dermoid cysts ever shed or “move” the tooth-like material into the mouth or skin?
Typically no. The calcified tooth-like pieces usually remain within the cyst cavity. What can look like movement is the cyst expanding and pushing against nearby tissue, or, rarely, rupture or infection causing contents to drain outward.
How can you tell the difference between a dermoid cyst with calcifications and other jaw or neck lumps?
Location and imaging pattern matter. A midline floor-of-mouth or peri-orbital lump plus calcified density on CT raises suspicion, but confirmation requires pathology after excision, especially to rule out different congenital lesions or cyst types.
If imaging shows tooth-like calcifications, does that guarantee it is a teratoid dermoid cyst?
Not always. Calcified dental-like material is most suggestive of teratoid tissue, but the precise subtype depends on microscopic findings (histopathology) of the cyst lining and internal contents after removal.
Can a dermoid cyst go away on its own if it is small?
Most do not fully resolve on their own because the lining continues producing keratin and oil-like secretions. Small cysts may stay quiet for years, but symptomatic or enlarging cysts are usually treated with complete surgical excision.
Is it safe to watch and wait if there is no pain?
Often clinicians can monitor carefully if the cyst is stable and not infected, but it depends on size, location, and whether it is affecting swallowing, breathing, vision, or speech. Floor-of-mouth cysts are especially important to assess promptly because swelling can affect the tongue and airway space.
What are the biggest warning signs that a dermoid cyst is infected or ruptured?
Look for sudden redness, warmth, increasing pain, rapid swelling, fever, or new drainage of thick, cheesy, or foul-smelling material. These signs generally warrant urgent medical evaluation and can change the treatment timeline.
Will antibiotics alone cure a dermoid cyst that has become infected?
Antibiotics may reduce infection and inflammation, but they usually do not eliminate the cyst lining. Definitive management typically involves surgical removal after the infection settles to reduce recurrence risk.
Can pressing on the lump at home make it go away?
No. Squeezing, puncturing, or attempting to drain it can rupture the cyst wall, spill contents into surrounding tissue, intensify inflammation, and increase the chance of spreading infection.
Do tooth-like structures in a dermoid cyst ever cause dental problems like cavities or loose teeth?
They usually do not function like teeth, but they can indirectly affect nearby structures by pressure, causing discomfort, misalignment, or altered movement of the tongue or jaw depending on location. Dental symptoms are often secondary to mass effect rather than true tooth activity.
If my child has a congenital midline lump, what specialist should we see first?
The best starting point is usually the pediatrician or a general practitioner for initial assessment. Based on location, referral is typically to an ENT, an oral and maxillofacial surgeon, or a pediatric surgeon, since surgical approach and imaging priorities differ.
Why is complete excision emphasized, and what happens if the lining is left behind?
Because the lining behaves like skin, it keeps producing keratin and secretions. If any lining remains, the cyst can regrow over time, so surgeons aim for removal of the entire cyst capsule and lining rather than partial debulking.
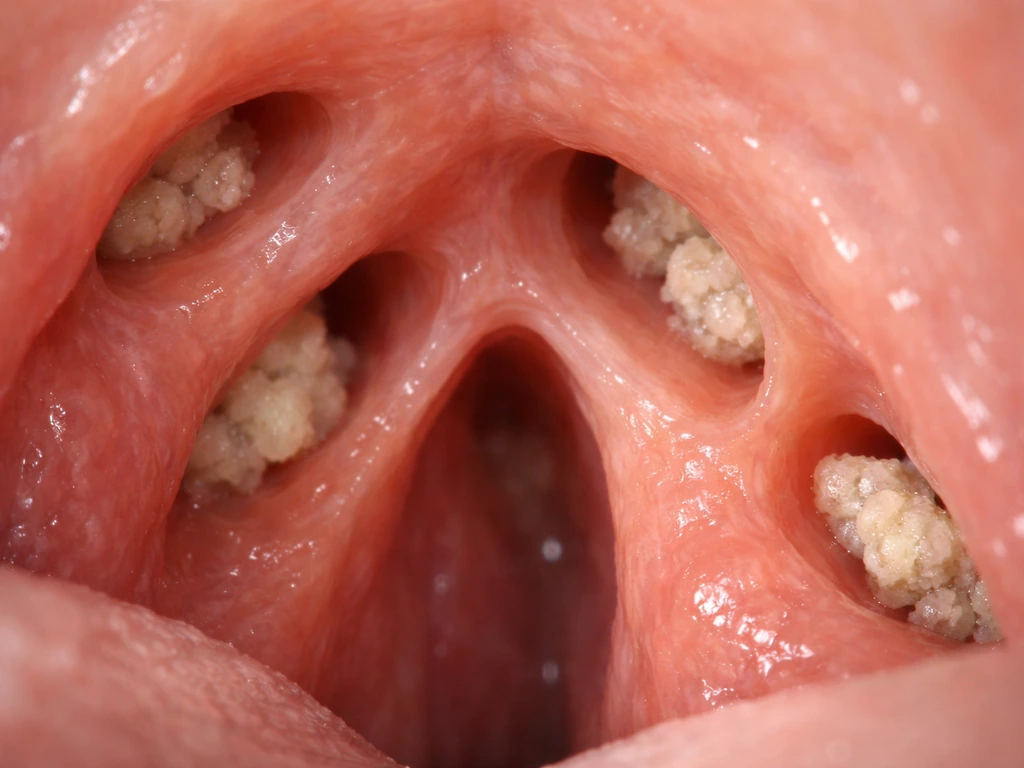
Explains how tonsil stones form in crypts, how long growth takes, why they recur, and what to do for faster relief.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Myth-busting answer on whether adults can regrow teeth, plus real options like implants, crowns, and orthodontics.

