Yes, a real tooth can appear in the roof of your mouth, but it is almost never a sign that you are growing a new tooth. What you are most likely dealing with is an extra tooth (called a supernumerary tooth), an impacted canine or incisor that erupted in the wrong place, or a non-tooth growth like a bony lump or a cyst that just feels like a tooth. True tooth regrowth from scratch does not happen in adults, and enamel does not naturally regenerate once it is gone. True tooth regrowth from scratch does not happen in adults, and enamel does not naturally regenerate once it is gone, which is also why it is not typical to wonder can a tooth grow in your ear without an underlying issue. So if you feel something new and hard on your palate, the question is not whether you are magically growing a third set of teeth. The question is what is actually there and whether you need to get it looked at, which in most cases you do.
Can Teeth Grow in the Roof of Your Mouth? What to Know

Teeth on the palate vs the tooth regrowth myth
The internet is full of people convinced that humans can grow teeth in random places if conditions are just right. That is not how it works. Teeth develop from specialized cells called tooth buds, and those buds are laid down very early in development. They do not spontaneously appear in adulthood. However, a tooth bud that already exists can end up in the wrong place. Trauma to a baby tooth, crowding, or a structural anomaly can displace a developing tooth so that it tries to erupt somewhere unexpected, including the roof of the mouth. That is not new growth. That is misdirected development from a structure that was always there.
Enamel, the outer coating of your teeth, cannot grow back at all once it is lost. A 2025 editorial in the British Dental Journal confirmed there is currently no clinically available solution that can effectively regrow lost enamel. Dentin regeneration is being actively researched, and pulp regeneration techniques exist in clinical practice, but none of this means teeth can sprout in new locations. Those are repair strategies for existing teeth, not mechanisms for producing new ones.
What a "roof of mouth tooth" could actually be
When someone notices something hard or tooth-like on their palate, there are several real possibilities. Some are genuinely dental, others are not.
Actual extra or misdirected teeth
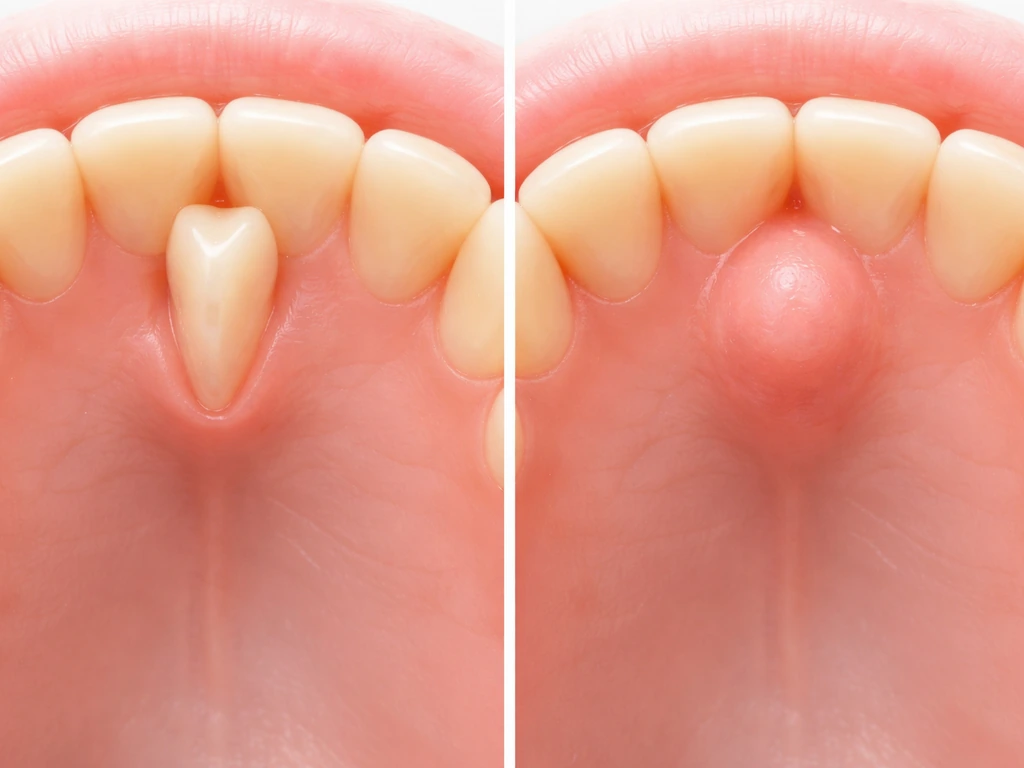
Supernumerary teeth are extra teeth that form beyond the normal 20 baby teeth or 32 adult teeth. They occur in roughly 1 to 3 percent of the population and can erupt into unusual locations, including the palate. Palatally impacted canines are another well-documented scenario: instead of erupting down into the arch where they belong, the upper canine gets stuck in the palate. Case reports document these canines being surgically exposed and then guided into their correct position. Ectopic eruption, where a tooth tries to come in at the wrong angle or location, has an estimated prevalence of around 5.6 percent. Maxillary incisors, the front upper teeth, are among those most commonly affected.
Non-tooth growths that mimic teeth
A hard midline bump on the roof of your mouth that has been there for years is very likely a torus palatinus, a benign bony overgrowth that Cleveland Clinic estimates is present in a meaningful portion of the adult population. It is not a tooth, it contains no enamel, and it usually requires no treatment unless it causes problems with speech, swallowing, or denture fit. A nasopalatine duct cyst, by contrast, is a fluid-filled lesion that forms near the incisive canal just behind your upper front teeth. It can cause swelling, drainage, and pain in the front palate and can look alarming on imaging even though it is benign. Distinguishing it from a tooth-related (periapical) cyst requires clinical exam, X-rays, and sometimes a biopsy. Minor salivary gland tumors can also appear on the palate, and while many are benign, studies show malignancy rates in palatal salivary gland lesions ranging from 35 to 82 percent depending on the series, which is exactly why a new palatal lump should not be ignored.
How tooth development and eruption normally works
Understanding the normal timeline makes it easier to recognize when something is off.
| Age Range | What's Happening |
|---|---|
| 5 to 10 months | First baby teeth erupt (lower central incisors, then upper central incisors) |
| 6 to 12 years | Baby teeth fall out and permanent teeth replace them in a predictable sequence |
| 7 to 9 years | Upper permanent central incisors typically erupt |
| 11 to 13 years | Upper canines typically erupt; this is the most common time palatal impaction is noticed |
| 17 to 25 years | Wisdom teeth (third molars) erupt, often with complications |
| After age 25 | No new teeth should be developing or erupting in a typical adult |
Tooth buds can be displaced by trauma to a baby tooth, by crowding, or by the presence of a supernumerary tooth blocking the normal path. When that happens, the affected tooth may erupt ectopically, meaning it comes in at the wrong angle or in the wrong location entirely. In children and adolescents this is the most common reason a tooth-like structure appears somewhere unexpected on the palate. In adults, if a new hard bump appears, it is almost certainly not a tooth erupting for the first time. That same idea comes up in questions like can a tooth grow in your nose, but the biology is different and usually not true regrowth. It is more likely a bony growth, a cyst, or a lesion that needs evaluation.
Can teeth or enamel actually regenerate in adults?
This is one of the most common misconceptions in dentistry, and the short answer is no, not in any natural or currently available clinical way. Enamel is produced by cells called ameloblasts, and those cells die off after a tooth fully erupts. Once enamel is gone, your body has no mechanism to replace it. Researchers are exploring stem cell approaches to recreate ameloblast-like cells, and a 2024 paper showed it is possible to induce human stem cells toward an ameloblast pathway in the lab, but this is nowhere near a clinical treatment you can receive today.
Dentin is a different story. The pulp tissue inside a tooth can deposit secondary dentin over time, and clinical trials using growth factors like rhPDGF-BB have demonstrated some ability to stimulate this process. Regenerative endodontic therapy (revascularization) is an established protocol for immature permanent teeth in children with pulp necrosis. But none of this means a whole tooth can regrow, or that a new tooth can form somewhere it was never supposed to be. The biology simply does not support that.
Symptoms to watch for when a new palatal bump appears
Not every bump on the roof of your mouth is an emergency, but paying attention to the specific characteristics helps you decide how urgently to act. Here is what to look for:
- Hard versus soft: a tooth or bone is hard and immovable; a cyst or salivary gland lesion may feel firm but slightly compressible
- Location: bumps right at the midline near the back of the front teeth are more likely tori or nasopalatine cysts; bumps off to the side near where canines should sit are more suspicious for an impacted tooth
- How long it has been there: a bump that has been stable for years is more likely a torus; something that appeared recently and is growing should be evaluated promptly
- Pain or pressure: pain can suggest infection, cyst expansion, or a tooth under tension trying to erupt
- Drainage or taste: a foul or salty taste can mean an infected cyst or abscess is draining
- Swelling of the face or gums around the area
- Numbness in the roof of the mouth, lip, or tongue
- Any associated loosening of nearby teeth
In children, a hard bump on the palate near the front teeth during the canine eruption years (roughly age 11 to 13) is worth bringing up at the next dental visit. If there is any pain or a tooth in the arch appears to be missing, do not wait.
When to see a dentist or oral surgeon, and red flags that can not wait
Most palatal bumps warrant at least a dental visit within a few weeks. Some need to be seen much sooner. The American Dental Association recommends that any white or red patch or lesion that does not resolve within two weeks be re-evaluated and considered for biopsy. The American Cancer Society lists unexplained numbness in the mouth, a lump or mass in the mouth or throat, and difficulty swallowing or opening the mouth as warning signs that require prompt evaluation. Mayo Clinic notes that oral cancer can present as a growth or lump that does not heal, and AAOMS emphasizes that persistent pain or sores lasting more than two to three weeks are concerning.
Get seen urgently, meaning within one to two weeks, if you notice any of these:
- A lump that appeared suddenly and is growing
- Numbness in the roof of the mouth, lip, or tongue
- A sore or ulceration on the palate that has not healed in two weeks
- Difficulty swallowing, speaking, or opening your mouth
- Swollen lymph nodes in the neck alongside a palatal bump
- Bleeding from the area without an obvious cause
- Fever or signs of spreading infection (swelling of the face, difficulty breathing)
For a stable, painless, long-standing hard bump with none of these features, a routine dental appointment is fine. Your general dentist can evaluate many of these findings directly. If imaging suggests an impacted tooth, a significant cyst, or anything that looks surgically complex, they will refer you to an oral and maxillofacial surgeon. If there is any concern about a potentially malignant lesion, you want that referral to happen quickly.
It is worth noting that unusual tooth-like structures do not only appear in the mouth. If you’re wondering can a tooth grow in your nose, it’s helpful to know that new tooth formation in adulthood generally does not happen. If you are also wondering whether teeth can grow in your throat, the short answer is that new tooth formation in adulthood is extremely unlikely can teeth grow in your throat. Similar ectopic or odontogenic anomalies have been documented in other head and neck locations, which speaks to how varied the developmental paths of dental tissue can be, though those cases are distinctly rare.
How diagnosis works and what treatment looks like
The diagnostic process
Diagnosis starts with a clinical exam. Your dentist will palpate the area to assess hardness, size, and mobility, and will check the surrounding teeth for vitality (are they alive or dead at the nerve level?) and proper positioning. Periapical or panoramic X-rays are usually the next step. These can identify impacted teeth, cysts, bony abnormalities, and the relationship of any lesion to adjacent tooth roots. For anything complex, especially suspected impacted teeth or large cysts, a cone-beam CT (CBCT) scan gives a three-dimensional picture that is far more useful for surgical planning. Case reports of familial impacted supernumerary teeth consistently rely on CBCT to map out exactly where each tooth is sitting.
For nasopalatine duct cysts and other soft tissue lesions, the definitive diagnosis requires histopathology. That means a tissue sample has to be examined under a microscope. No imaging alone can rule in or rule out a nasopalatine duct cyst versus a radicular cyst versus something more serious. If your clinician wants to biopsy a palatal lump, that is not an overreaction. It is the only way to be certain.
Typical treatment paths
- Impacted or ectopic tooth: surgical exposure by an oral surgeon, followed by orthodontic traction to guide the tooth into its correct position. In some cases, if the tooth is not salvageable or there is no space for it, extraction is the right call.
- Supernumerary tooth: usually extraction, especially if it is blocking normal eruption or causing crowding. Timing depends on the child's age and the position of the extra tooth.
- Torus palatinus: no treatment needed in most cases. If it interferes with a denture or causes trauma from hard foods, surgical removal under local anesthesia is straightforward.
- Nasopalatine duct cyst: surgical enucleation (removal of the entire cyst lining) is the standard treatment. Recurrence rates are low when the cyst is fully removed.
- Palatal salivary gland lesion: surgical excision followed by pathology review. Treatment and prognosis depend entirely on the histologic result.
- Monitoring: for very small, asymptomatic, and clearly benign findings (like a small stable torus), watchful waiting with periodic re-evaluation is appropriate.
The bottom line is that something new and hard on the roof of your mouth deserves a proper look. It is very unlikely to be a spontaneously regenerating tooth, because that is not something human biology does. What it could be ranges from completely harmless to something that genuinely needs treatment. A dental exam with the right imaging will almost always give you a clear answer, and in the rare cases where imaging is not enough, a biopsy will. Do not sit on it for months hoping it goes away on its own, especially if it is growing, painful, or comes with any of the red-flag symptoms listed above.
FAQ
How can I tell if the hard spot on my palate is actually a tooth versus a bony bump?
A tooth-like lump is more likely if it is associated with the surrounding teeth (for example, a nearby tooth looks absent or ectopic) and if imaging shows a tooth structure or a lesion near tooth roots. If the bump is long-standing, firm, and perfectly stable in size, it may be a torus palatinus or other benign bone growth, which typically has no enamel. The quickest way to sort this out is an exam plus a dental X-ray; plain inspection alone cannot reliably distinguish enamel-bearing structures from bone or cysts.
If I had braces or dental trauma before, could that cause a tooth to appear in the wrong place on the roof of my mouth?
Yes. Trauma to a baby tooth, crowding, or a supernumerary tooth can redirect the eruption path of an existing tooth bud so it comes in ectopically, including toward the palate. If you notice a new hard spot alongside signs like delayed eruption of an upper front tooth or shifting of nearby teeth, mention your orthodontic history, since it can change what your dentist looks for first.
Is it ever possible that enamel is “growing back” over a new bump?
No. Your body does not regenerate enamel once it is formed and later lost, and enamel-producing cells stop functioning after eruption. If something looks like a tooth surface, it is more likely an actual tooth (or calcified lesion) rather than new enamel appearing over time. If you suspect this, do not rely on the appearance alone, ask whether imaging shows tooth material.
What imaging should I expect, and when is a CBCT scan needed?
Many cases start with periapical films or a panoramic X-ray to look for impacted teeth, cystic changes, and how close a lesion is to roots. A cone-beam CT is more appropriate when the finding is complex, when surgical planning may be needed, or when standard X-rays cannot clearly show the exact location and angulation of a suspected impacted tooth or supernumerary tooth. If your clinician is considering an oral surgery approach, ask whether CBCT is indicated for 3D mapping.
Do nasopalatine duct cysts always require a biopsy?
Not always, but diagnosis often cannot be confirmed confidently with imaging alone when symptoms and appearance overlap with other cysts. If the lesion looks cystic near the incisive canal and the diagnosis would change management, biopsy or histopathology may be recommended. In practice, clinicians biopsy palatal lumps to avoid missing less common but more serious causes.
What are the red flags that mean I should seek urgent care rather than waiting for a routine appointment?
Seek evaluation promptly (often within one to two weeks) if the lump is accompanied by unexplained numbness, rapidly changing size, persistent pain, recurrent drainage, difficulty swallowing, trouble opening your mouth, or ulceration that does not heal. Also seek prompt care if you feel a mass in the mouth or throat region, since some non-dental causes can mimic “tooth-like” growths.
If it’s painless and it’s been there a long time, could I just monitor it?
Sometimes, especially if it is clearly stable and the exam suggests a benign bony finding like torus palatinus. However, you still need at least one proper evaluation to establish what it is, because cysts and some tumors can start quietly. A practical approach is to book a dental visit soon, take note of size and symptoms, and update your clinician if it changes.
Should I try to remove or pick at the lump at home?
No. Trying to scrape, drill, or squeeze a palatal lump can lead to infection, bleeding, and delayed diagnosis, especially if it is a cyst or salivary lesion. If it is a tooth eruption issue, attempts to “clean it out” can also damage adjacent tissues. Let your dentist determine whether it needs imaging, referral, or a biopsy.
If imaging suggests an impacted tooth, what determines whether it gets extracted or exposed and moved?
The decision depends on the tooth involved, its orientation, the presence of symptoms, and whether it threatens nearby roots or prevents normal eruption. If it is a supernumerary tooth, removal is often considered to clear space. For impacted canines or incisors, clinicians may recommend surgical exposure and orthodontic traction to bring the tooth into the correct position, but the exact plan depends on 3D imaging and surrounding anatomy.
Which clinician should I see first for a new palatal lump?
Start with your dentist or general dentist, since they can do an oral exam, check nearby tooth vitality and positioning, and order initial X-rays. If imaging suggests surgical complexity, an impacted tooth, a large cyst, or something that needs specialized management, an oral and maxillofacial surgeon is often the right next step. If malignancy is a concern, prompt referral to the appropriate specialist is important.

Can a tooth grow in your nose? Learn what’s possible, what it likely is, and next steps for ENT and dental care.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn
Learn which teeth seem to grow twice: primary replaced by permanent, plus wisdom teeth timing and limits on regrowth

