No, a tooth cannot normally grow in your nose. Human teeth develop from specialized cells in the jaw, guided by a tightly controlled process that unfolds in the gums and alveolar bone, not anywhere near the nasal cavity. So if you or your child has something in the nose that looks or feels like a tooth, it is not a product of normal dental development. That said, rare but real cases of ectopic teeth showing up in the nasal cavity do exist in the medical literature, and there are several other conditions that can produce tooth-like lumps or hard masses inside the nose. Let me break all of this down so you know exactly what you are dealing with and what to do next.
Can a Tooth Grow in Your Nose? What’s Possible and Next Steps
Why a tooth can't just grow in your nose
Teeth form through a process called odontogenesis, which starts in the embryonic jaw tissue. Dental stem cells, signals from surrounding tissue, and a highly organized developmental sequence all have to line up correctly for a tooth to form. This entire process is anchored in the maxilla (upper jaw) and mandible (lower jaw). The nasal cavity is anatomically adjacent to the upper jaw, but it is not part of that developmental machinery. There are no tooth buds sitting in your nasal lining waiting to erupt.
Normal human dental development follows a strict schedule. Primary teeth begin forming before birth, and permanent teeth follow a predictable eruption timeline through childhood and adolescence. None of that programming points to the nose. The nasal floor and the hard palate are in close physical proximity to the upper dental arch, but proximity is not the same as developmental origin. Think of it this way: the furnace and the kitchen in a house share walls, but one does not spontaneously generate the functions of the other.
What people actually see when a 'tooth' appears in the nose
This is where it gets genuinely interesting. While a tooth cannot normally grow in your nose, there are several conditions that can produce something that looks very much like a tooth, or at least a hard, calcified, tooth-shaped structure, inside the nasal cavity. Here are the most common culprits.
Ectopic teeth (the real thing, just in the wrong place)
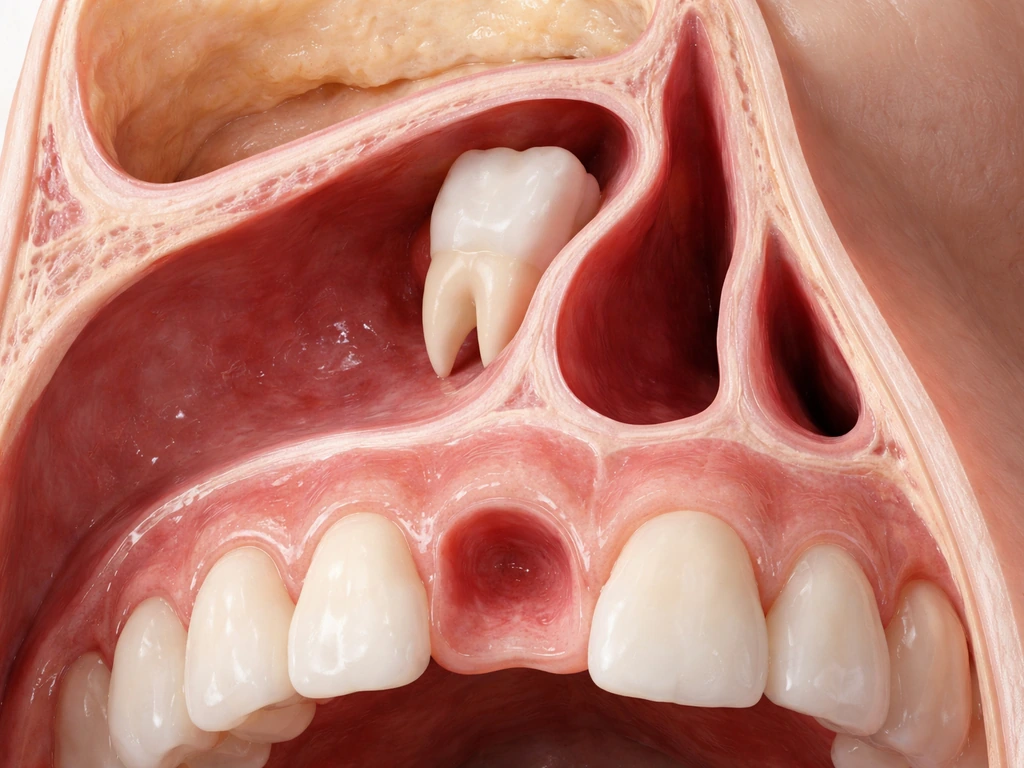
These are genuine documented cases, and yes, they exist. An ectopic tooth is a real tooth that erupted in an abnormal location due to a developmental error. Case reports describe children and adults with actual tooth structures found inside the nasal cavity, usually on the floor of the nose. One pediatric case described unilateral nasal obstruction caused by an intranasal ectopic tooth originating from the inferior turbinate, with no obvious facial deformities or dental abnormalities that would have flagged the issue. Another adult case showed a tooth in the left nasal cavity surrounded by soft tissue on CT. These are rare, not random, and they are not the result of a tooth migrating on its own, but rather a tooth bud that formed and erupted in the wrong place from the start. Symptoms can include recurrent nosebleeds, foul-smelling discharge, and unilateral obstruction.
Rhinoliths (calcified stones, not teeth)
A rhinolith is a hard calcified mass that forms in the nasal cavity when mineral salts slowly deposit around a small nidus, which could be a tiny foreign body, a blood clot, or even retained nasal packing from a prior procedure. Over time it hardens into something that can look remarkably tooth-like on imaging. Symptoms overlap significantly with those of an ectopic tooth: unilateral nasal obstruction, purulent or foul-smelling discharge, facial pain, and headache. On imaging, rhinoliths often show a central radiolucent core surrounded by calcification, which can help distinguish them from actual tooth tissue, though CT is sometimes needed to be sure. Removal is curative in most cases with minimal complications.
Osteomas
Osteomas are benign, slow-growing bony tumors. They are actually the most common benign tumors of the nasal cavity and paranasal sinuses. They grow at roughly 1 mm per year on average, so they can go undetected for a long time before producing symptoms like headache, nasal congestion, or facial pain. On exam or imaging, an osteoma looks like a dense, calcified, well-defined mass, which is easy to mistake for a tooth-like structure if you are not familiar with the difference. Treatment when symptomatic is surgical excision.
Odontogenic cysts and odontomas
Odontogenic cysts (cysts that originate from tooth-forming tissue) can sometimes expand toward or into the nasal cavity. Research has found that a meaningful percentage of such cysts, around 25.8% in one retrospective evaluation, show growth toward the nasal cavity with resulting airway narrowing. Odontomas are a related category, technically odontogenic tumors made up of mature enamel, dentin, cementum, and pulp tissue. They look like small jumbled teeth or calcified masses on imaging and can appear at the nasal floor. A cyst associated with an ectopic supernumerary tooth has also been reported to produce nasal obstruction by expanding into the nasal cavity. These are rare but documented, and they underscore why imaging is essential for a correct diagnosis.
Foreign bodies
In kids especially, a small object pushed into the nose years earlier can calcify over time and look like a tooth on X-ray. This is actually one of the primary items on the differential diagnosis when a child presents with unilateral nasal symptoms and a calcified mass. The differential for a calcified nasal lesion appropriately includes foreign bodies, rhinoliths, ectopic teeth, granulomatous infections, and tumors, which is exactly why a physician cannot just look at it and guess.
Can dental tissue actually regrow or form in the wrong place?
This is a fair question given that this site covers what teeth and dental structures can and cannot regenerate. The short answer is no: dental tissue does not spontaneously regrow in ectopic locations. Mature enamel is incapable of self-regeneration when it sustains mineral loss, a fact well established in biomineralization research. Dentin and cementum have limited reparative capacity, but that repair happens within the tooth structure, not by forming new teeth in random anatomical sites. The dental pulp has some regenerative potential under specific clinical conditions (this is the basis of regenerative endodontics, which the American Association of Endodontists addresses in its 2025 position statement), but even that is about maintaining or partially restoring pulp tissue inside an existing tooth, not growing new dental structures elsewhere.
So when a case report describes a tooth in the nasal cavity, that tooth did not regrow there or migrate there. It formed there from the beginning because of a developmental error in where the tooth bud was positioned. The body cannot create new teeth in the nose any more than it can create new teeth in the ear. Just as you might wonder about whether a tooth can grow in the ear, the answer follows the same logic: normal human anatomy simply does not allow it.
People sometimes ask about teeth appearing in other unusual locations, and the biology is consistent across all of them. Whether someone is curious about teeth growing in the roof of the mouth, teeth appearing in the throat, or even teeth growing out of the toes (which is an entirely different and very rare condition), the underlying point is the same: true ectopic dental tissue requires a developmental origin, not spontaneous regrowth.
Getting a correct diagnosis: who to see and what to ask for
If you or your child has a hard lump in the nose, recurrent nosebleeds from one side, a persistent one-sided nasal blockage, or foul-smelling discharge that doesn't resolve, you need an evaluation, not a wait-and-see approach. Here is how the diagnostic workup typically goes.
Start with an ENT (ear, nose, and throat specialist)
An ENT is the right first call for a nasal mass or persistent unilateral nasal symptoms. They can perform anterior rhinoscopy, which is a direct look into the nasal cavity, and nasal endoscopy, which uses a small camera to get a much better view of the nasal floor, turbinates, and surrounding structures. An ectopic tooth, if present, may actually be visible during endoscopy, appearing as a bony protrusion covered by mucosa on the nasal floor.
Imaging: what to ask for and why
Endoscopy tells you something is there. Imaging tells you what it is and how it relates to surrounding structures. CT (computed tomography) of the sinuses or nasal cavity is the gold standard here. It gives you cross-sectional views that show whether the mass has the density of true tooth tissue (with enamel, dentin, and pulp distinguishable in some cases), whether it looks like a rhinolith with a central nidus, or whether it is a purely bony osteoma. For dental-origin lesions, cone-beam CT (CBCT) and panoramic radiographs are often used in conjunction with sinus CT to evaluate the relationship between the nasal mass and the dental arches. This combination of nasal endoscopy plus CT is consistently how ectopic nasal teeth are confirmed and surgically planned.
Loop in a dentist or oral and maxillofacial surgeon
If the mass appears to have an odontogenic (dental) origin, the ENT should coordinate with a dentist or, ideally, an oral and maxillofacial surgeon (OMFS). The OMFS has the expertise to evaluate whether a supernumerary tooth, an odontoma, or an odontogenic cyst is involved, and to plan removal if needed. For a child, the dentist can also assess whether a normal tooth is missing from the dental arch, which can be a clue that the nasal structure is actually an ectopically located tooth bud from the normal complement.
Questions to ask at your appointment
- Can we do nasal endoscopy today to get a direct look at what's there?
- Do I need a CT scan of the sinuses, and should it include the dental arches?
- Should I also see a dentist or oral surgeon to evaluate whether this has a dental origin?
- Is there any missing tooth in the dental arch that might explain a tooth in this location?
- What is the most likely diagnosis based on what you are seeing, and what are the alternatives?
- If this is a rhinolith, osteoma, or cyst, what does treatment look like?
- If this is an actual ectopic tooth, can it be removed endoscopically?
Urgent vs. routine: how to decide
Not every nasal mass requires a same-day emergency visit, but some symptoms are red flags that mean you should not wait for a routine appointment.
| Symptom or sign | Urgency level | Why it matters |
|---|---|---|
| Uncontrolled or recurrent heavy nosebleeds from one side | Urgent: see ENT or go to urgent care | Persistent unilateral epistaxis can signal pathology requiring endoscopic evaluation |
| Visible nasal mass with facial swelling or skin changes | Urgent: same-day or ER | Could indicate infection, abscess, or aggressive growth |
| High fever (above 39°C / 102.2°F) with severe facial pain | Urgent: ER evaluation | Red flag for complicated sinusitis or spreading infection |
| Double vision, visual changes, or eye swelling | Emergency: go to ER immediately | Suggests orbital involvement, a serious complication |
| One-sided nasal blockage with foul discharge, no fever, no pain | Routine: book ENT within 1-2 weeks | Concerning but not emergency-level; needs evaluation |
| Hard lump noticed incidentally, no symptoms | Routine: book ENT and dentist | Still needs imaging and evaluation but not urgent |
| Child with one-sided stuffy nose and bad smell for weeks | Routine-to-soon: book within days | Classic presentation of nasal foreign body or rhinolith in kids |
Unilateral persistent nosebleeds, facial pain or swelling, reduced sense of smell on one side, and a visible nasal mass are all features that ENT referral guidelines flag as needing prompt evaluation rather than watchful waiting. If in doubt, call your doctor's office and describe the symptoms. They can tell you whether urgent care or a scheduled appointment is appropriate.
Your next-step action plan
Here is what to actually do if you are sitting here today wondering whether you or your child has a tooth in the nose.
- Check for red-flag symptoms first. Go through the table above. If you have any of the urgent or emergency symptoms, stop reading and seek care now.
- Call your primary care doctor or pediatrician (for kids) and describe the symptoms clearly: which side is affected, how long it has been happening, whether there is discharge or bleeding, and whether there is any visible mass.
- Get a referral to an ENT. This is the specialist who can do endoscopy and order appropriate imaging. Ask specifically for nasal endoscopy and CT of the sinuses.
- Bring your dental records or see a dentist around the same time. If the mass turns out to have a dental origin, having a panoramic X-ray from your dentist on hand speeds things up significantly. Your dentist can also check whether any teeth are missing from the arch.
- Once imaging is done, push for a clear differential diagnosis. The CT report and endoscopy findings together should distinguish between an ectopic tooth, rhinolith, osteoma, odontogenic cyst, or other nasal lesion.
- Ask about treatment outcomes specific to the diagnosis. Ectopic nasal teeth are typically removed endoscopically with good outcomes. Rhinoliths are removed and that is usually the end of it. Osteomas are excised surgically when symptomatic. Odontogenic cysts may require more extensive surgery depending on their size and extent.
- Follow up. After treatment, confirm with both the ENT and the dentist that the underlying cause has been fully addressed and that no further monitoring is needed.
The bottom line: a tooth growing in your nose is not a normal biological event, and it is not something the body does spontaneously or through any regenerative process. But a hard, tooth-like structure appearing in or near the nasal cavity is a real clinical finding that deserves a real workup, not guesswork. Rare as true ectopic nasal teeth are, they have been documented, and there are several other conditions that can look almost identical. Get the right specialists involved, get the imaging, and get a clear diagnosis. Once you know what you are dealing with, the treatment path is usually straightforward.
FAQ
How can you tell the difference between an ectopic tooth and a rhinolith if both look like a tooth on X-ray?
Appearance alone is unreliable. CT helps because an ectopic tooth is usually discrete and dental-like, while a rhinolith often has a central nidus (for example, a retained fragment or old packing) with calcification around it. If the lesion’s history fits a prior procedure, foreign body event, or persistent one-sided odor, that shifts suspicion toward rhinolith, but the final call is imaging plus ENT exam.
Is it ever an emergency, or can it wait for a normal ENT appointment?
It can often wait, but not if you have red flags like persistent or heavy one-sided nosebleeding, rapidly worsening obstruction, facial swelling, fever, severe pain, or trouble breathing. If symptoms are significant, call for urgent guidance, because obstruction and infection can become time-sensitive even when the cause is benign.
Can a tooth in the nose be a sign of a genetic syndrome or other systemic problem?
Most cases are isolated and sporadic, especially ectopic teeth found in the nasal cavity. However, odontogenic cysts, multiple supernumerary teeth, or other unusual dental findings may warrant a broader evaluation. An oral and maxillofacial surgeon or dentist can decide whether genetic or syndromic screening is appropriate based on the overall dental and facial pattern.
If it is a foreign body that calcified, will it always be removable and safe to remove?
Often yes, but it depends on size, location, and how embedded it is. The ENT may use endoscopic removal, sometimes after confirming anatomy with CT. The main risk is irritation or bleeding during removal, particularly if the lesion is near vessels or if infection is present, which is why visualization matters.
Do children with unilateral nasal blockage and a calcified spot always need CT?
Not always. Clinicians first balance radiation exposure with urgency and diagnostic uncertainty. If symptoms strongly suggest a foreign body and endoscopic evaluation is likely to be definitive, CT may be avoided. If the lesion’s nature or extent is unclear, or there is concern for tumors or odontogenic lesions, CT becomes more important.
What imaging should I ask for if an ENT suspects a dental-origin lesion in the nose?
Typically sinus or nasal cavity CT is central because it shows density and exact location. If dental origin is suspected, clinicians may add CBCT and/or panoramic radiographs to map relationships to the dental arches and look for missing or supernumerary teeth. Ask whether CBCT is needed in addition to CT for surgical planning.
Could the mass be related to teeth I already had taken out, like a failed root canal or an extraction complication?
Usually not directly. A nasal lesion that is truly tooth-like typically arises from developmental tissue or a calcifying process within the nasal cavity. That said, prior nasal packing or procedures can contribute to rhinolith formation, and chronic infections can mimic masses, so your clinician will want your complete history.
Is it possible for an osteoma or odontogenic lesion to grow without symptoms?
Yes. Osteomas can be slow-growing, and some people only discover them incidentally or after nasal obstruction or headache develops. Odontogenic cysts can also expand gradually toward the nasal airway. That is why consistent unilateral symptoms, even if mild, are worth evaluation rather than dismissal.
If the diagnosis is ectopic tooth, will it always require surgery?
Many cases are treated surgically, especially if symptoms like obstruction, bleeding, foul discharge, or recurrent infection are present. If an asymptomatic lesion is found incidentally and imaging suggests low risk, a clinician may consider observation. The decision depends on location, growth, symptoms, and how close the lesion is to critical structures.
What symptoms should prompt immediate medical care while waiting for evaluation?
Seek prompt care if you develop worsening one-sided obstruction, increasing facial pain or swelling, significant or repeated nosebleeds that do not settle, high fever, worsening foul drainage, or any breathing difficulty. Waiting is more reasonable if symptoms are stable and mild, but escalation is important if they change quickly.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

