There is no single disease where teeth literally sprout up everywhere in your body, but there are real, documented conditions that cause extra tooth-like structures to form in unusual numbers or locations inside the mouth and jaw. The main culprits are supernumerary teeth (extra teeth beyond the normal count), odontomas (tumor-like masses made of disorganized dental tissue), and rarer syndromes like Gardner syndrome that combine multiple dental abnormalities with other systemic findings. None of these mean your body has "gone rogue" and is growing teeth randomly. They are developmental or genetic conditions with clear diagnoses, imaging protocols, and treatment paths.
Disease Where Teeth Grow Everywhere: Causes, Diagnosis, Treatment
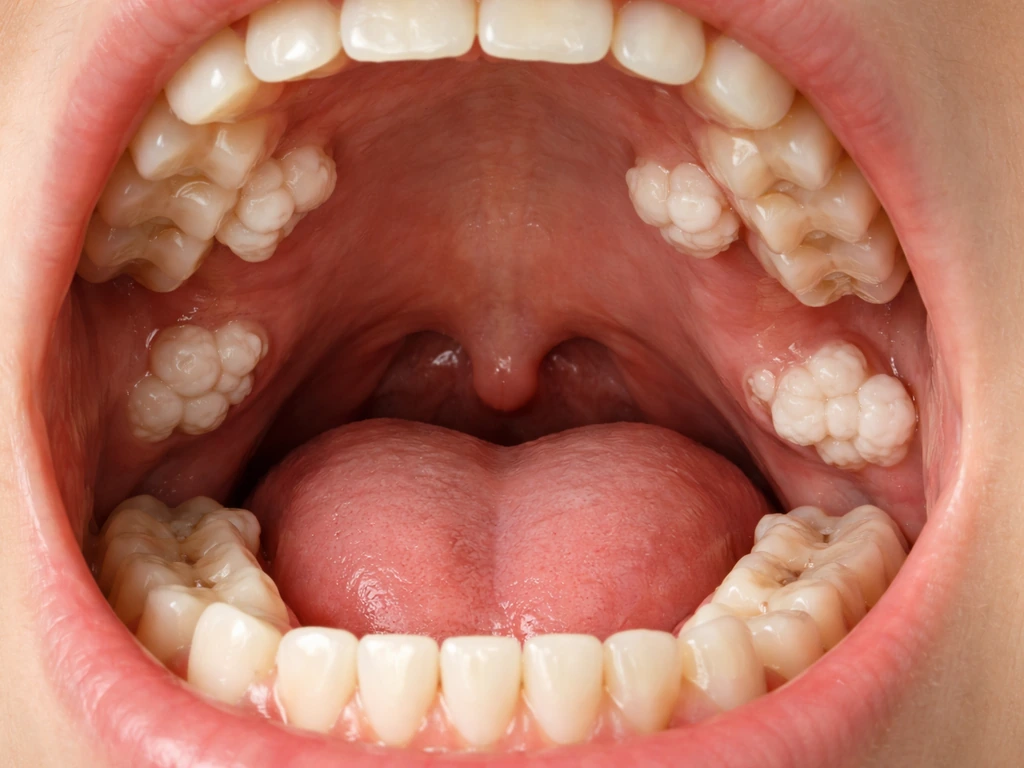
What "teeth growing everywhere" usually means
When people describe teeth or tooth-like lumps appearing in unexpected places, they are almost always talking about one of a handful of specific dental conditions. Getting the terminology straight helps you have a much more productive conversation with your dentist.
Supernumerary teeth
Supernumerary teeth are simply extra teeth. Humans are supposed to develop 20 primary (baby) teeth and 32 permanent teeth. Any tooth beyond that count is called supernumerary. They show up in about 0.3 to 0.8 percent of people with primary dentition and 1.5 to 3.5 percent of people with permanent dentition. A single extra tooth is common enough. Multiple supernumerary teeth in someone without a syndrome, however, are rare and account for roughly 1 percent of supernumerary cases. The most frequent offender is a mesiodens, which is an extra tooth that forms right in the midline between your two upper front teeth. But supernumerary teeth can appear anywhere along the dental arch, and occasionally in genuinely strange spots.
Odontomas
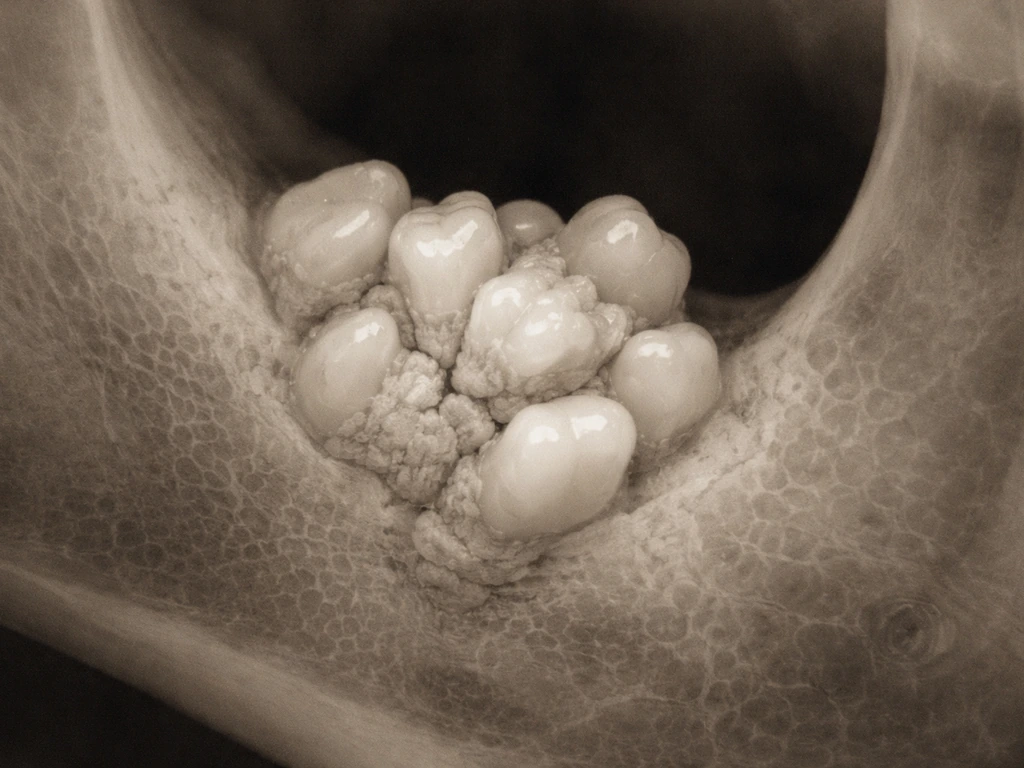
An odontoma is not exactly a tooth and not exactly a tumor. Think of it as a disorganized cluster of dental tissue, including enamel, dentin, and pulp, that formed from the same cells that make teeth but never organized properly. There are two types. A compound odontoma looks like a collection of many small, recognizable tooth-like structures called denticles. A complex odontoma is a dense, disorganized mass of dental hard tissue that does not resemble individual teeth at all. Both types are usually found by accident on X-rays, often because a permanent tooth refused to erupt on schedule.
Syndromic causes: Gardner syndrome and others
Gardner syndrome is a rare genetic condition where multiple dental abnormalities, including supernumerary teeth, impacted or unerupted teeth, and odontomas, appear alongside jaw osteomas (bony growths) and intestinal polyps. About 30 percent of Gardner syndrome patients show dental abnormalities. The key reason dentists need to know about this syndrome is that the dental findings often show up on routine radiographs before the intestinal or other systemic features are identified, which means a dentist can be the first person to flag it. Cleidocranial dysplasia is another developmental condition associated with numerous supernumerary teeth and significant eruption delays.
Ectopic tissue and choristomas
A choristoma is a mass of histologically normal tissue that just shows up in the wrong location. Hard-tissue choristomas can appear on the tongue or in gum tissue and look or feel like calcified or tooth-like lumps. They are not true teeth, but they can absolutely alarm a patient who notices what feels like a hard bony growth somewhere unexpected. Case reports exist of ectopic osseous masses on the tongue, and while these are rare, they illustrate why the phrase "teeth growing everywhere" sometimes comes from real but unusual findings that deserve professional evaluation.
Why it happens: causes and contributing factors
The honest answer is that researchers do not have a single locked-in explanation for why supernumerary teeth or odontomas form. What is clear is that the process starts during tooth development, when the dental lamina, a ribbon of epithelial cells that gives rise to all your teeth, behaves abnormally. The leading theories include:
- Hyperactivity of the dental lamina: the tissue that normally generates a set number of tooth buds keeps producing more than it should.
- Dichotomy of a tooth bud: a single developing tooth bud splits in two, giving rise to an extra tooth alongside the normal one.
- Genetic and environmental contributions: family history matters, and there are likely both inherited gene variants and environmental triggers (such as infection or local trauma during early tooth development) that play a role.
- Atavism theory: a rarely cited but interesting idea that extra teeth represent a reversion to an ancestral trait from ancestors who had more teeth.
- Syndromic gene mutations: in Gardner syndrome, a mutation in the APC tumor suppressor gene drives the whole picture, including dental findings.
- Late-developing supernumerary teeth: a separate category where extra teeth develop obviously later than the teeth they accompany, without any syndromic features, suggesting the dental lamina can remain active longer than expected in some individuals.
For odontomas specifically, most cases are considered developmental in origin rather than truly neoplastic (cancerous). Local trauma, infection during tooth development, or genetic disruption can all theoretically interfere with the orderly differentiation of dental tissue and produce an odontoma.
How to tell if it's a real extra tooth vs. a tooth-like growth
You cannot reliably tell the difference just by looking in the mirror or running your tongue over a lump. That said, there are symptoms and red flags worth knowing about.
Typical presentations
- A permanent tooth that simply never came in when it should have (non-eruption of permanent teeth is reported in roughly 42.5 percent of supernumerary tooth cases found on CBCT imaging).
- A baby tooth that is hanging on way past its expected expiration date while the adult tooth has not appeared.
- A gap or diastema between the upper front teeth that did not close after the baby teeth came out.
- A visible extra tooth or small peg-shaped tooth appearing alongside normal teeth.
- A hard, immovable lump felt under the gum or on the tongue or palate.
- Crowding that does not match the patient's jaw size or orthodontic history.
Red flags that need prompt attention
Most supernumerary teeth and odontomas are surprisingly painless and are found by chance. But certain signs mean you should get to a dentist or oral surgeon soon rather than waiting for your next routine appointment:
- Swelling, redness, or tenderness in the gum or jaw area, which can indicate infection or cyst formation.
- Fever alongside any dental swelling, since this suggests the infection may be spreading.
- Pain or pressure that is getting progressively worse.
- Teeth visibly moving or shifting position in a short period.
- A lump that is growing noticeably over weeks or months.
- A permanent incisor or canine erupting in a very wrong location (in extreme mesiodens cases, teeth have even been reported erupting into the nasal cavity).
- Signs of a dentigerous (follicular) cyst, which can appear as a painless expanding swelling but will show up clearly on imaging.
How dentists diagnose it today
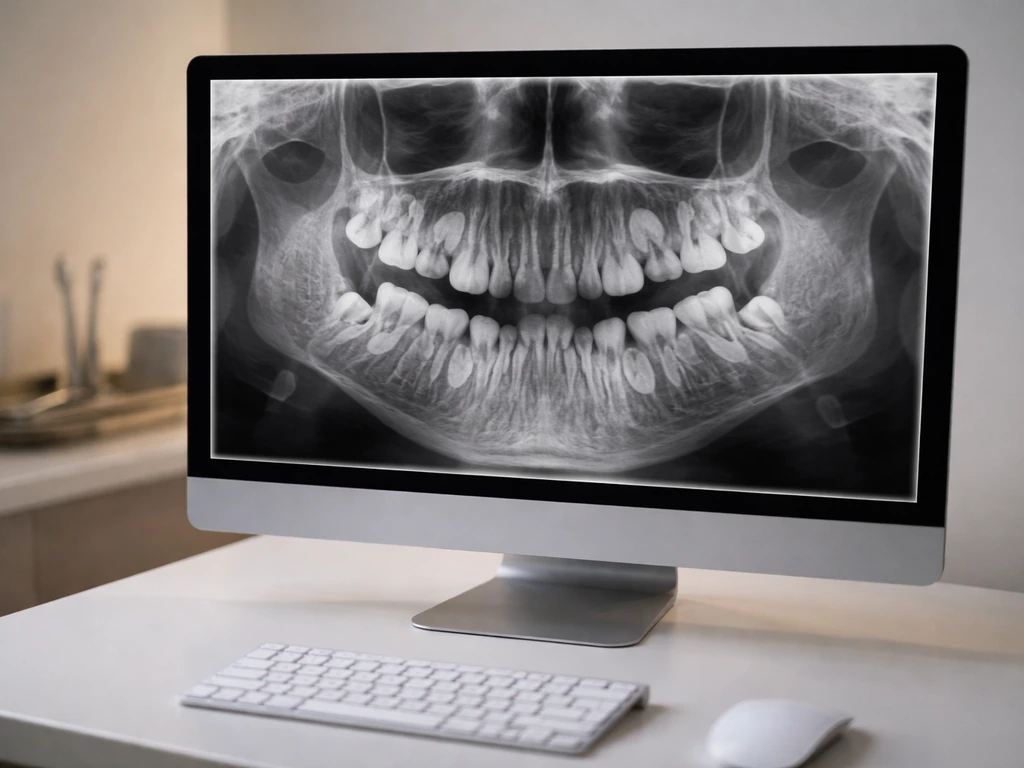
Detection starts with a clinical exam, but almost nothing definitive is confirmed without imaging. A dentist palpating a hard lump under your gum can tell you there is something there, but they cannot tell you if it is a supernumerary tooth, an odontoma, a cyst, or something else. The imaging sequence typically works like this:
- Periapical and bitewing X-rays: these intraoral films give a close-up view of individual teeth and surrounding bone, and they are often where odontomas and extra teeth are first spotted.
- Panoramic radiograph (OPG): a panoramic film shows the full mouth, jaw, and developing teeth in one image and is the standard recommendation for assessing suspected supernumerary teeth, impacted teeth, and third molars. It is the most efficient way to see if there are multiple abnormalities distributed across both jaws.
- Cone beam computed tomography (CBCT): when a panoramic film raises concern about a deep or complex case, CBCT provides precise three-dimensional localization. It is particularly important before surgery when the abnormal tooth or mass is near the inferior alveolar nerve or the maxillary sinus, where knowing exact position prevents nerve or sinus injury during removal. CBCT is also the gold standard for evaluating the full extent and relationship of odontomas to surrounding teeth.
Radiographic appearance alone can usually differentiate compound odontoma (many small identifiable tooth-like structures within a radiolucent border) from complex odontoma (a dense, disorganized radiopaque mass). Supernumerary teeth look like teeth on imaging because they are teeth, though they may be inverted, displaced, or peg-shaped. When the diagnosis is uncertain, especially for soft-tissue lumps or unusual hard-tissue masses, a biopsy and histological examination are the final step. This is particularly true for choristomas and ectopic tissue lesions, where the only way to confirm what the mass is made of is to look at it under a microscope.
If multiple dental abnormalities are found (supernumerary teeth plus osteomas plus odontomas), a referral for medical evaluation to rule out Gardner syndrome or another systemic condition is appropriate. Dental radiographs sometimes detect Gardner syndrome before the gastrointestinal features cause any symptoms, making the dental office an unexpectedly important first line of detection for this condition.
Treatment options and what to expect
Treatment is not one-size-fits-all. It depends on the type of abnormality, where it is, whether it is causing problems, and the patient's age and overall dental development stage. Here is how decisions are typically made:
| Condition | First-Line Treatment | When to Monitor Instead | Key Considerations |
|---|---|---|---|
| Supernumerary tooth (erupted) | Extraction | Rarely; if it is erupted and well-positioned in the arch without crowding, some can be maintained with observation | Orthodontic planning needed for space management after removal |
| Supernumerary tooth (impacted/unerupted) | Surgical removal, usually as soon as the problem is detected | If the patient is very young and the tooth is not yet affecting adjacent teeth, short-term monitoring possible | CBCT recommended before surgery near nerves or sinus |
| Compound odontoma | Surgical excision | Occasionally monitored if very small and asymptomatic in a young child, pending growth | Recurrence after removal is very rare; removal usually allows blocked permanent tooth to erupt |
| Complex odontoma | Surgical excision | Not recommended due to risk of cystic change and bone involvement | Pathology confirmation recommended; recurrence rare |
| Odontoma with cyst or infection | Urgent surgical removal with infection management | Not appropriate | May require antibiotics and hospital-level care if systemic signs present |
| Gardner syndrome (dental component) | Remove odontomas and supernumerary teeth as indicated; refer to gastroenterology | Dental monitoring ongoing | Critical: intestinal polyps require colonoscopic surveillance given malignant potential |
Immediate surgical removal of a supernumerary tooth is generally indicated when it is interfering with the eruption of adjacent permanent teeth, when it has caused crowding or displacement, when it is associated with a cyst or infection, or when it has spontaneously erupted into the mouth. Research supports interceptive treatment as early as possible after detection of abnormal eruption patterns, because delayed eruption of a permanent tooth sometimes self-corrects after the offending supernumerary is removed, particularly if the patient is still in mixed dentition.
After removal, orthodontic treatment is often needed. Creating space, guiding eruption of blocked teeth, and closing gaps are common follow-up needs, especially in adolescents who had significant crowding or midline diastemas from a mesiodens.
Surgery near the jaw carries real risks: damage to the inferior alveolar nerve, perforation of the maxillary sinus, or fracture of surrounding bone are all possible in complex cases. This is why CBCT-informed surgical planning is so important when the mass is deep, close to nerves, or in the posterior jaw.
Can teeth or enamel actually regrow everywhere? Myths vs. science
Let's clear something up directly: the conditions described above are not examples of teeth regrowing. Supernumerary teeth and odontomas form during development, driven by abnormal activity of the dental lamina cells. They are not regenerated teeth. Once your permanent teeth are in and that developmental window closes, the human body does not spontaneously sprout new teeth from gum tissue or bone on its own.
Enamel regeneration is a hot area of dental research right now. Scientists are exploring stem cell approaches, protein-based scaffolds, and smart material delivery systems to engineer enamel tissue. But current research is clear: these approaches involve conditions that are not yet suitable for routine clinical use, and integrating lab-generated enamel with existing tooth structure remains a significant unsolved challenge. As of today, you cannot go to a dentist and have lost enamel biologically regrown. You can have it restored with materials like composite resin or ceramic, but that is a replacement, not regeneration.
Similarly, the internet is full of claims about teeth regrowing in other parts of the body, on fingers, in cysts, or in tumors. People often ask whether can teeth grow in other parts of the body, but those claims usually come from unusual tooth-like masses rather than true tooth regrowth. In real life, cases like this are usually abnormal tissue or a cyst that can include tooth-like material, not true teeth growing on fingers teeth regrowing on fingers. Dermoid cysts can contain hair and sometimes tooth-like structures because they arise from germ cells that carry developmental programming. But this is not your body randomly producing teeth. It is an abnormal growth with a specific pathology. Related questions about whether teeth can grow under other teeth or in entirely unusual locations do have real answers rooted in developmental biology, not magic or random regrowth.
The bottom line: teeth growing in unusual numbers or positions within the jaw is a real developmental condition. Teeth spontaneously regrowing in adults from jaw bone or gum tissue is not biologically possible with current human physiology or available treatments.
Age and timing: when these conditions tend to appear
Timing matters a lot in how these conditions are detected, managed, and interpreted. Here is a practical breakdown by life stage:
Young children (ages 3 to 7)
Supernumerary teeth in primary dentition are relatively rare (0.3 to 0.8 percent prevalence), but they do occur. In young children, these often go unnoticed unless a routine X-ray or a crowding problem prompts investigation. Odontomas are also often caught in this window when a baby tooth lingers well past its expected fall-out date or a permanent tooth fails to start erupting. Watching and waiting is more acceptable here if the child is too young for comfortable surgery, but the situation needs monitoring.
Mixed dentition years (ages 6 to 12)
This is the most common time for problems to become apparent. Permanent teeth erupt on a fairly predictable schedule, and a mesiodens or impacted supernumerary tooth will announce itself by blocking a central incisor or causing a diastema that stubbornly refuses to close. Panoramic X-rays taken around ages 7 to 8 during orthodontic screening routinely catch unerupted supernumerary teeth and odontomas. Early detection and removal during mixed dentition often gives blocked permanent teeth enough room to erupt on their own without needing surgical exposure and orthodontic traction.
Teenagers and young adults
Supernumerary teeth discovered in teenagers have often been present and undetected for years. By adolescence, blocked teeth may need active orthodontic intervention to pull them into position after removal of the obstruction. Late-developing supernumerary teeth are also a recognized category: these are extra teeth that develop noticeably later than their neighbors and may appear on imaging in the early teen years even though they were not visible on earlier X-rays. Wisdom teeth enter the picture here too, and while they are normal third molars rather than supernumeraries, their impaction can cause a similar clinical picture of crowding and failed eruption.
Adults
Adults occasionally discover an extra tooth or odontoma on a routine panoramic film taken for reasons unrelated to abnormal eruption. These are often completely asymptomatic and have been quietly sitting in the jaw for decades. The management question for an adult is more nuanced: if the extra tooth or mass is not causing problems and surgery carries meaningful risk (due to proximity to nerves or sinuses), a monitoring approach with regular imaging is sometimes chosen over removal. But any sign of cyst formation, infection, or neighboring tooth damage tips the decision firmly toward intervention.
FAQ
If I feel a hard, tooth-like lump in my mouth, does that always mean I have an extra tooth?
Yes, but it is usually not “teeth growing” as in new teeth forming. A dentist may see calcified or tooth-like material in benign lesions (for example, dermoid or other developmental cysts, or a hard-tissue choristoma). These are abnormal tissue masses, not true erupted teeth, and they need diagnosis by imaging and sometimes biopsy if the nature of the lump is unclear.
When is a “tooth-like” lump urgent, and when can I wait for my next appointment?
Most lumps do not require emergency care, but you should contact an oral surgeon or dentist promptly if there is rapid growth, significant pain, pus or fever, numbness or tingling (possible nerve involvement), difficulty opening your mouth, or swelling that is spreading. If you have these signs, don’t wait for a routine checkup.
How can I tell whether a midline lump is a mesiodens versus something else?
Do not try to self-diagnose based on where the lump is. Even if a mesiodens is a classic cause of a midline diastema, other conditions can mimic it, including impacted teeth, cysts, odontomas, or ectopic calcified tissue. Reliable identification generally requires dental imaging, often a panoramic X-ray first and CBCT when location is near nerves or the sinus.
When do dentists use CBCT instead of a standard panoramic X-ray?
Only a limited picture is available from plain X-rays. CBCT is especially helpful when the mass is deep, near the inferior alveolar nerve, close to the maxillary sinus, or when the tooth-like structure is displaced. It helps the surgeon plan the safest approach and assess root proximity, which reduces risk compared with relying on 2D images alone.
Do I always need a biopsy to confirm an odontoma or choristoma?
A biopsy is most likely when the lesion does not have classic imaging features, when there is concern for a non-tooth hard-tissue process, or when there is an atypical soft-tissue component. For choristomas and ectopic tissue lesions, histology is often the deciding factor because “tooth-like” appearance alone is not enough.
What clinical pattern should make me ask my dentist about a possible syndrome?
Yes. If you have multiple supernumerary teeth and additional findings like odontomas plus jaw osteomas or a history of intestinal polyps, a medical evaluation is appropriate to rule out syndromes such as Gardner syndrome. The dental team may recommend this even before you have gastrointestinal symptoms, because dental radiographs can show clues earlier.
Why don’t all extra teeth get removed immediately, especially in kids?
In children, dentists often balance removal versus monitoring. If a supernumerary tooth or odontoma is blocking eruption or causing tooth displacement, earlier removal during mixed dentition can allow the permanent teeth to erupt more normally. If it is not causing functional problems and the risks of surgery outweigh the benefits, observation with scheduled imaging may be chosen, especially in very young children.
After removal, will orthodontics be automatic or can it be avoided?
If an impacted tooth is blocked by a supernumerary tooth and the permanent tooth still has a chance to erupt after removal, dentists may delay additional orthodontic procedures to see how eruption responds. Orthodontics becomes more necessary when eruption stalls, when alignment is significantly compromised, or after late-detected cases where years of impaction have already changed positioning.
What determines whether an adult’s incidentally found supernumerary tooth or odontoma should be removed?
Not always. Some adults have an asymptomatic supernumerary tooth or odontoma discovered incidentally. Management often depends on symptoms and risk to adjacent structures. If there are signs of cyst formation, infection, damage to neighboring teeth, or a high likelihood of nerve or sinus complications with surgery, monitoring with periodic imaging may be the safer initial plan.
Why might two people with “extra teeth” get very different surgery plans?
Yes. Surgical planning depends on the lesion type and anatomy. Even when the goal is “remove the obstruction,” the approach differs for an ectopic calcified mass versus a true supernumerary tooth, and for lesions in the posterior jaw versus the anterior region. Surgeons account for proximity to nerves and the sinus and use imaging to reduce the chance of complications.
Are odontomas cancer, and do I need oncology care?
Treatment does not mean cancer treatment. Odontomas are generally considered developmental rather than cancerous, so standard care is evaluation and management of local effects, like eruption failure or crowding. If imaging and clinical findings are atypical, that is when clinicians become more cautious and consider histological confirmation.
Teeth can’t grow anywhere on your body, but true odontogenesis occurs only in specific tissues and sites.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Learn why humans don’t grow back adult teeth, what natural healing can do, and today’s options like implants and bridges

