Gums do not truly "grow around" a dental bridge the way many people hope. There is no biological mechanism that causes gum tissue to expand and seal itself against a bridge the way skin might close over a small cut. What you may see in the first few weeks after bridge placement is minor gum settling or a slight reduction in post-procedure swelling, which can make the fit look a little different over time. But if you are noticing a visible gap, redness, tenderness, or food getting trapped under your bridge, those are signs of a fit issue, gum inflammation, or early periodontal disease, not a gap that gum tissue will simply grow over and fix on its own. This same idea applies to bone graft healing too, so you should not expect gum to grow over a bone graft on its own does gum grow over bone graft.
Do Gums Grow Around Bridge? What’s Normal and What’s Not

What "gums growing around a bridge" actually means

It helps to break this phrase into the three very different things people usually mean when they say it. First, some people are asking whether gums can regenerate lost tissue, essentially regrowing the periodontal attachment that supports teeth. Second, some people are describing normal early settling, where gums that were slightly swollen after the procedure return to a more natural position around the bridge margins. Third, and most commonly, people are describing a gap or space they can see between the bridge and their gumline and hoping the tissue will eventually close it.
The first idea, true periodontal regeneration, refers to the formation of new bone, new cementum, and a new periodontal ligament coronal to an existing defect. This is a specialized clinical goal that requires active treatment, not something that happens passively on its own at home. The second idea, minor settling after placement, is real but modest and usually resolves within a few weeks. The third idea is the most important to understand: a persistent gap between your bridge and your gums is almost never going to close on its own, and waiting for it to do so allows more damage to accumulate.
How dental bridges affect gums and bite over time
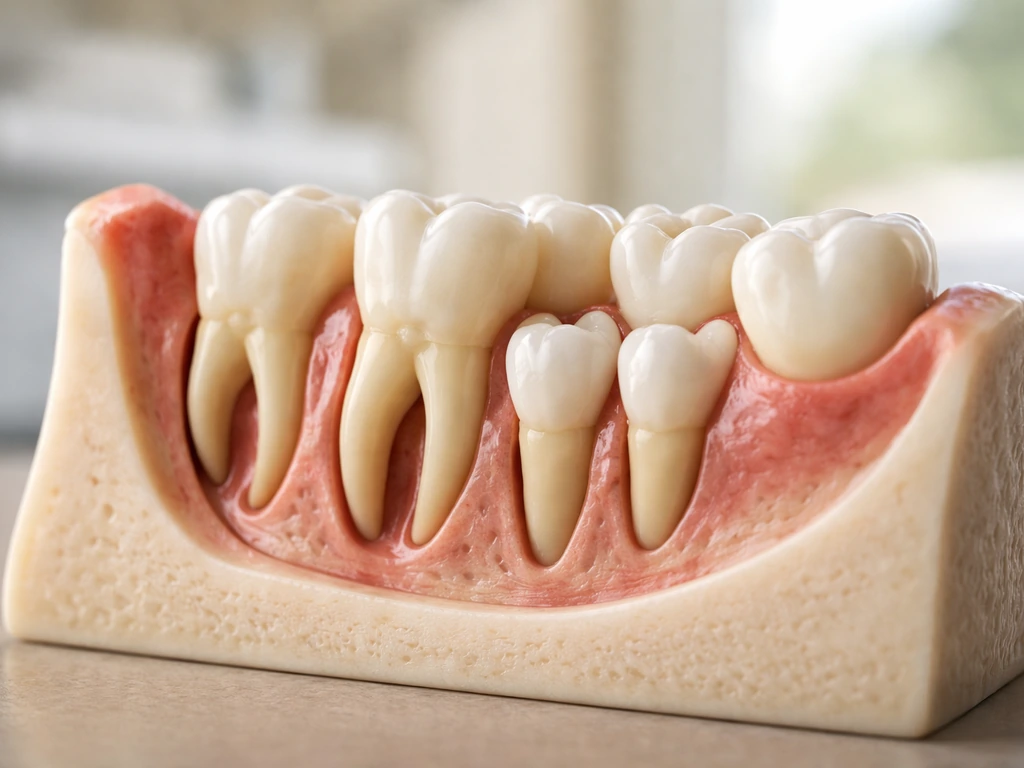
A dental bridge sits on abutment teeth on either side of a gap and includes a false tooth (pontic) suspended between them. The point where the bridge meets the gum is called the margin, and that margin-tissue interface is one of the most biologically sensitive areas in your mouth. When a bridge is well-fitted and well-maintained, the gums around it stay healthy. When something is off, the consequences tend to get worse over time rather than better.
Research consistently shows that subgingival restoration margins (margins that sit at or below the gumline) are associated with increased plaque accumulation, higher gingival inflammation scores, greater pocket depths, and even measurable gingival recession over follow-up periods. Plaque that forms along a poorly fitting margin shifts the bacterial population toward more pathogenic species, which accelerates tissue breakdown. A bridge that was fine at placement can slowly undermine the gums over months and years if the margins aren't perfect, if hygiene slips, or if the design creates plaque traps.
Bite changes matter too. If a bridge is even slightly high or the distribution of bite forces across the abutment teeth is uneven, those teeth can experience excess stress over time, contributing to bone loss and gum recession around them. The pontic also needs a properly designed tissue contact point, because a pontic that presses too firmly against the ridge or traps food underneath it will chronically irritate the gum tissue beneath it.
Can gums actually regenerate around a dental bridge? The real biology
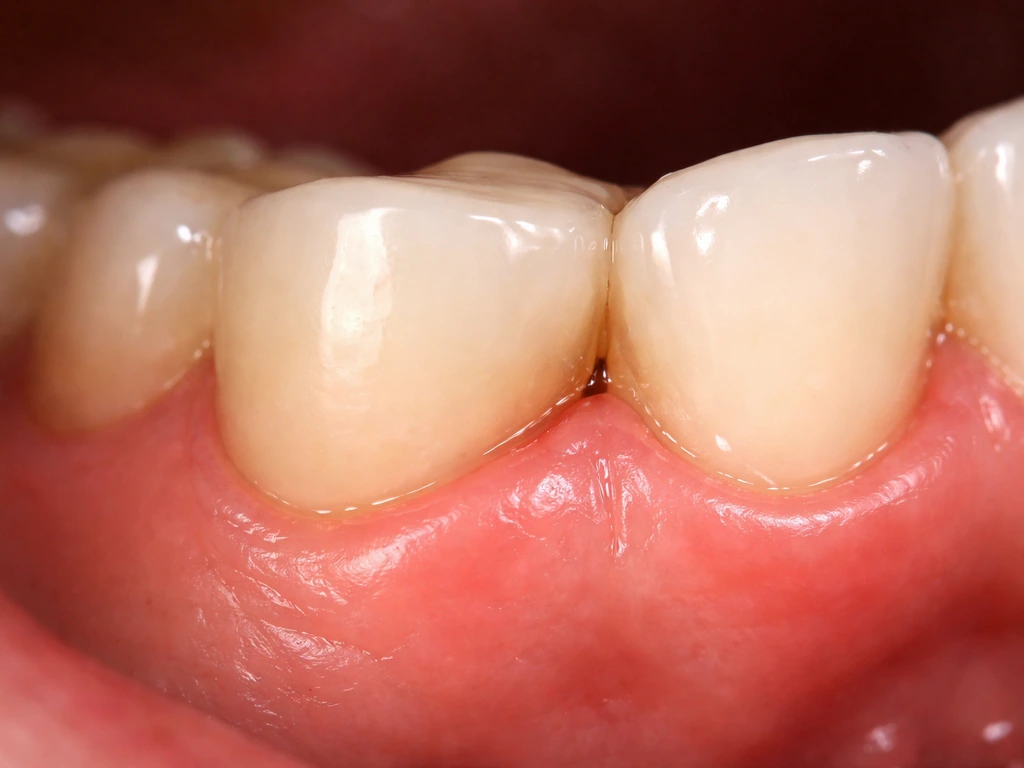
This is where a lot of internet misinformation needs to be addressed directly. Gum tissue does not regenerate to close gaps around dental restorations. The idea that gums will simply "grow back" or "grow around" a bridge is a common misconception, and believing it can delay care until real damage is done.
True periodontal regeneration, as defined by the American Academy of Periodontology, means forming new bone and new periodontal tissue including the ligament and cementum complex. This is distinct from simple reattachment and is a goal of specialized surgical procedures, not spontaneous healing. Research makes clear that the periodontal ligament-cementum attachment destroyed by periodontitis does not reliably self-repair, and human regenerative capacity in this area remains limited even with active clinical treatment.
What gums CAN do is reduce in size when active inflammation is treated. Swollen, inflamed gum tissue looks puffy and red, and once plaque control improves and inflammation resolves, that tissue can firm up and appear to pull back slightly (which is actually a sign of health returning, not growth). People sometimes interpret this as gums "adapting" to the bridge, but it is really just inflammation resolving. This is good news from a tissue health standpoint, but it does not close gaps caused by poor bridge fit or periodontal attachment loss. If you're wondering why gums grow over braces, the same concept applies: gaps from poor fit or attachment loss do not close on their own why do gums grow over braces. Similar questions come up for crowns and implants, where the same biological rules apply: tissue health can improve with treatment, but true regrowth of lost attachment does not happen spontaneously. For implants, the same principle applies: gums can look better when inflammation is treated, but they do not regrow to close persistent gaps from poor fit or lost attachment. If you are asking about crown margins specifically, the same biology applies: gums may improve when inflammation is treated, but they do not regrow to fill persistent gaps the same biological rules apply.
Common reasons for gaps, irritation, and poor fit around bridges
If your bridge looks like it doesn't fit against your gums the way it should, there are several well-established causes to consider:
- Margin misfit: Even a small discrepancy at the bridge margin creates a ledge where plaque accumulates and bacteria thrive. Studies on fixed prostheses consistently link margin discrepancies to periodontal inflammation and progressive tissue breakdown.
- Overcontouring: A bridge that is too bulky at the gumline prevents proper cleaning, promotes plaque buildup, and can displace gum tissue, leading to chronic inflammation.
- Excess cement: Residual cement left beneath the gumline after bridge placement acts as a foreign body that triggers inflammation and bacterial colonization.
- Gum disease (gingivitis or periodontitis): Existing or developing gum disease causes the gum tissue and underlying bone to break down, creating pockets and gaps around abutment teeth.
- Plaque and calculus buildup: Even a well-fitting bridge becomes a problem if cleaning is inadequate. Calculus beneath the bridge pontic or around the abutment margins leads to gingival recession and pocketing.
- Ill-fitting temporary bridges: Temporary restorations with poor margins or excess bulk can damage tissue before the permanent bridge is placed, leaving the gum in a worse state.
- Trauma or bite pressure: Excessive biting force on the bridge can stress the abutment teeth, contributing to bone loss and gum recession over time.
- Normal post-placement swelling resolving: In the first few weeks after bridge placement, gums may look slightly different as procedural swelling resolves. This is the one scenario where a minor change in the gum-bridge relationship is expected and normal.
What you can do today: home care that actually helps
You can't grow new gum tissue at home, but you can significantly reduce inflammation and prevent further damage with meticulous daily cleaning. This is genuinely important because gum health around a bridge is almost entirely dependent on how well you manage plaque at the margins every single day.
Cleaning under and around your bridge
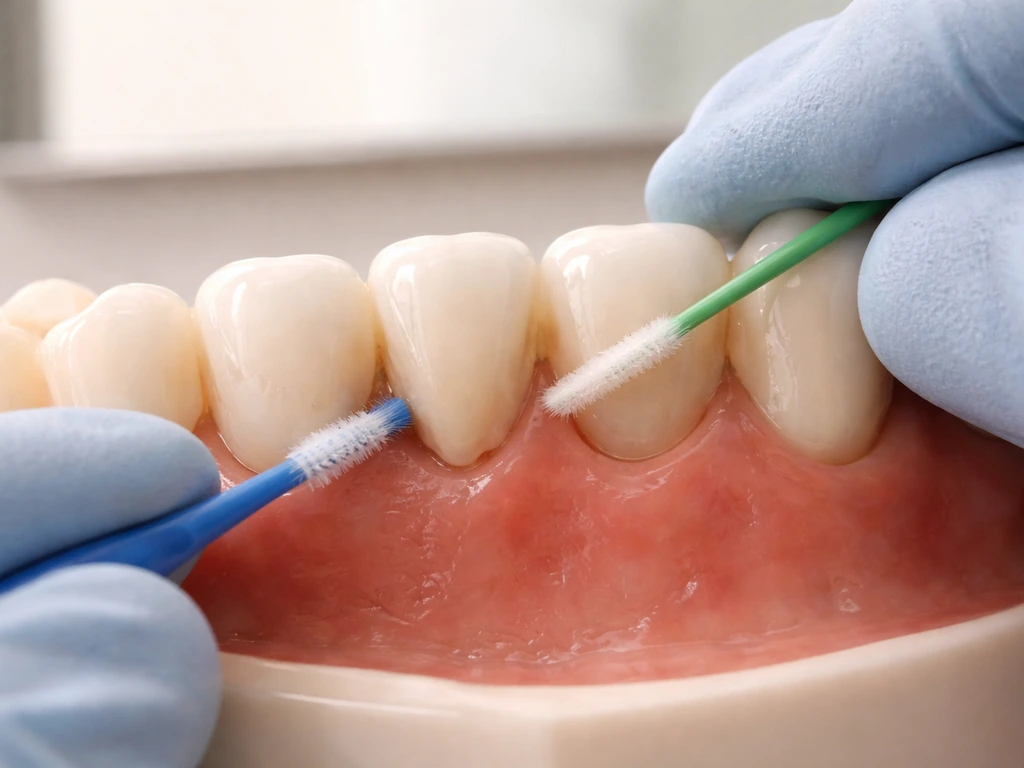
The biggest challenge with bridges is cleaning the underside of the pontic and the margins of the abutment crowns. Standard flossing doesn't work here without a little help. Floss threaders let you pass regular floss beneath the bridge so you can clean the contact areas and the pontic tissue surface with a gentle back-and-forth motion. Superfloss (which has a stiff end, a spongy section, and regular floss) does the same job and some people find it easier to handle.
Interdental brushes (proxy brushes) are excellent for cleaning the space under the pontic and along the sides of the abutment margins, especially if there is any gap or recession that gives them room to work. Choose a size that fits snugly without forcing. Water flossers are a useful addition, particularly for flushing debris and bacteria from beneath the pontic and around tight margins, and clinical trials have shown they can reduce gingival bleeding. That said, a water flosser does not replace mechanical plaque removal at the margins, it supplements it.
What to avoid
- Skipping the pontic area when cleaning. Food and bacteria trapped under the false tooth are a primary cause of gum problems under bridges.
- Using toothpicks aggressively near the gum margins. They can push bacteria deeper and traumatize inflamed tissue.
- Sticky or hard foods that can dislodge or stress the bridge.
- Smoking or tobacco use, which significantly impairs gum healing and promotes bone loss.
- Ignoring sensitivity or a metallic/bad taste thinking it will resolve on its own. These are often early warning signs.
Managing sensitivity while keeping the area clean
If the area is sore or sensitive, the temptation is to avoid cleaning it. This is exactly the wrong response. Gentle cleaning with a soft-bristle brush and a non-abrasive fluoride toothpaste is always better than leaving plaque at an irritated margin. A small amount of sensitivity during brushing is expected when tissue is inflamed; it typically improves as the inflammation resolves with better plaque control. A desensitizing toothpaste can help with temperature sensitivity at the abutment teeth, but it won't address the underlying issue.
When to see a dentist urgently: red flags to watch for
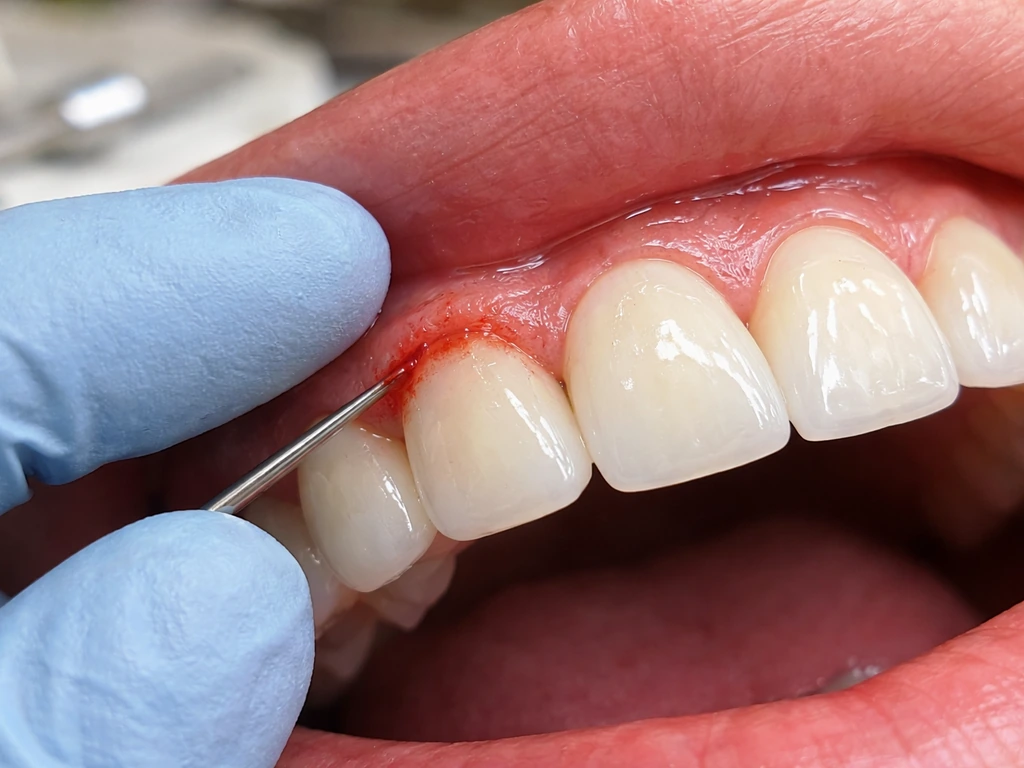
Some changes around a bridge are worth monitoring with your regular dental hygiene and a scheduled appointment. Others need a dentist's attention this week. The following symptoms should prompt you to call your dentist promptly rather than waiting for your next scheduled visit:
- Bleeding that doesn't stop or bleeding that returns every time you clean, even after a week or two of improved hygiene. Bleeding on probing is a key marker of active gum disease.
- Persistent or worsening pain around the bridge, especially deep pain in an abutment tooth.
- A foul taste, bad smell, or visible pus or discharge near the bridge margin. These can indicate a periodontal abscess, which requires prompt treatment. Periodontal abscesses can involve probing depths greater than 6 mm, suppuration, and tooth mobility.
- The bridge feels loose, moves slightly, or sounds different when you bite. This could mean abutment tooth compromise or cement failure.
- Rapidly receding gumline around the abutment teeth, meaning you can visibly see more of the tooth structure than before.
- Swelling of the gum or jaw that appears suddenly or is expanding.
When you go in, your dentist will typically do a periodontal probing exam around all bridge abutments, checking for pocket depths, bleeding on probing, and suppuration. They will also take updated X-rays to assess the bone levels around the abutment teeth and look at the bridge margins for fit and any signs of cement loss or recurrent decay. This gives a complete picture of whether the issue is primarily a hygiene and inflammation problem, a prosthetic fit problem, or a combination of both.
What your dentist can actually do to fix it
The treatment your dentist recommends will depend on what the examination and X-rays reveal. Here are the realistic options:
| Problem Found | Likely Treatment |
|---|---|
| Plaque and calculus at bridge margins, early gingivitis | Professional cleaning and scaling around bridge margins, reinforced home care instructions |
| Periodontitis with pocketing around abutment teeth | Scaling and root planing (deep cleaning) per ADA/AAP nonsurgical periodontitis guidelines, possibly with adjunctive antimicrobials |
| Excess cement beneath the margin | Removal of residual cement, local debridement, reassessment |
| Minor margin misfit or bridge overcontouring | Margin adjustment or recontouring if technically possible, otherwise bridge replacement |
| Cement failure allowing bridge movement | Re-cementing of the bridge after evaluation of abutment tooth condition |
| Ill-fitting bridge with persistent inflammation or bone loss | Bridge replacement with a new restoration that has proper margins, emergence profile, and biologic width compliance |
| Advanced bone loss or abutment tooth failure | Extraction, periodontal surgery, possible implant planning or alternative restorative solution |
| Periodontal abscess | Drainage, debridement, antibiotics if indicated, urgent follow-up |
The most important takeaway is that addressing both the prosthetic cause (if any) and the periodontal condition at the same time produces the best outcomes. Research on fixed prostheses and periodontal health consistently shows that correcting only the restoration without treating the gum disease, or treating only the gum disease while leaving a problematic margin in place, leads to incomplete resolution and recurrence.
If the abutment teeth are still healthy and the problem is caught early, the prognosis is generally very good with appropriate cleaning and possibly a remade bridge. If the underlying bone and attachment are significantly compromised, the discussion becomes more complex and may involve implants as a longer-term solution. Either way, the path forward starts with a proper clinical exam, not watching and waiting for gum tissue to somehow grow into a space it biologically cannot fill.
FAQ
If I can see a small space between my bridge and my gums, will my gums eventually “seal” it?
Usually not. A persistent gap at the bridge margin typically reflects either an imperfect prosthetic fit or periodontal attachment loss, and gum inflammation may temporarily reduce or look different without closing the space. If the gap stays, plaque keeps collecting and the underlying gum support can keep breaking down.
What signs mean the bridge margin issue is more than normal settling?
Normal settling is mild and mainly involves reduced swelling in the first few weeks. Call your dentist if you have ongoing redness, tenderness, bleeding, a visible widening of the margin gap, a distinct bad taste, or food packing under the pontic that persists beyond the early healing window.
My gums looked puffy at first and now look less swollen. Does that mean the bridge is fitting better?
It usually means inflammation is improving, not that tissue has grown into a gap. Even when gums firm up, the bridge can still have an overhang, open margin, or plaque trap. A dentist can confirm fit with an exam and X-rays.
Can I check my bridge fit at home to decide whether I need to be seen urgently?
You can’t reliably measure margin gaps or pocketing at home. Visual gaps plus bleeding on flossing or brushing, persistent sensitivity, or trapped food are practical red flags to schedule an earlier appointment rather than waiting for routine care.
How does “food getting trapped under the pontic” relate to gum problems?
Food and biofilm trapped under the pontic increase plaque exposure at the margin, which can raise inflammation and pocket depth over time. Even if the pontic looks normal from the front, the underside contact area is where many hygiene failures and tissue breakdown start.
What cleaning tools work best under a bridge if floss won’t pass normally?
Floss threaders or Superfloss-type products help you reach beneath the pontic and along abutment margins. If you have room due to recession or a gap, interdental brushes sized to fit snugly can be very effective. A water flosser can supplement but generally should not replace mechanical plaque removal.
Should I stop cleaning if the gum around my bridge bleeds or feels sore?
No. Avoiding cleaning usually worsens plaque accumulation and inflammation. Use gentle technique with a soft brush and non-abrasive fluoride toothpaste, and consider a desensitizing toothpaste if temperature sensitivity is an issue. If bleeding persists after improved plaque control, get evaluated promptly.
How soon after bridge placement should I expect the gums to look “right”?
Minor swelling typically settles within the first few weeks. If you still see progressive gap appearance, continued bleeding, or symptoms are not improving, don’t wait for months. Early adjustment or periodontal treatment is easier than late-stage repair.
Can gum recession around bridge abutment teeth be caused by bite problems?
Yes. If the bridge is slightly high or forces are distributed unevenly, the abutment teeth can experience increased stress, contributing to bone loss and recession around them. Dentists may check occlusion and design, not just the gum tissue.
If my dentist corrects plaque and inflammation, will the gumline rise back to fully cover the bridge margin?
Often the gums can look healthier and appear slightly more “tight” as swelling decreases, but lost attachment or a structural margin problem usually does not fully reverse. Expect visible pocket and fit assessment to guide decisions, not appearance alone.
How do I know whether the problem is mainly hygiene/inflammation or a bridge fit issue?
Your dentist can sort this out with periodontal probing (pocket depth, bleeding), bleeding pattern, exam of the margins, and updated X-rays for bone level and cement loss or recurrent decay. If hygiene alone does not improve the probing or symptoms, a fit adjustment or remake may be needed.
Is it possible to treat the gum disease without fixing the bridge, and still get a good result?
Results are best when both issues are addressed together if they exist. Treating inflammation while leaving a problematic margin often leads to incomplete resolution or recurrence. Your plan should reflect both periodontal status and prosthetic fit.
Could this be related to a bone graft, where gums “cover over” the graft later?
Gums can heal over surgical sites, but that does not mean they will grow over a persistent prosthetic gap. The biological goals are different, and a bridge margin problem typically needs fit correction and periodontal management.
Find out if gums can regrow over crown margins, what affects recession vs stability, and what steps to take now.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn
Learn which teeth seem to grow twice: primary replaced by permanent, plus wisdom teeth timing and limits on regrowth

