Here's the short answer: your gum will not grow back over an exposed crown margin the way skin grows back over a cut. Gum tissue can swell, heal, and stabilize after a crown is placed, but if you're seeing a visible metal or ceramic edge at the gumline weeks or months after the crown was cemented, that's almost always gum recession, not a healing delay. Understanding the difference between normal post-placement healing and true recession is the key to figuring out what to do next. If you're also wondering does gum grow around implant, the same idea applies that normal early healing can stabilize tissue, but true recession still needs evaluation and treatment.
Will My Gum Grow Around My Crown? What to Expect
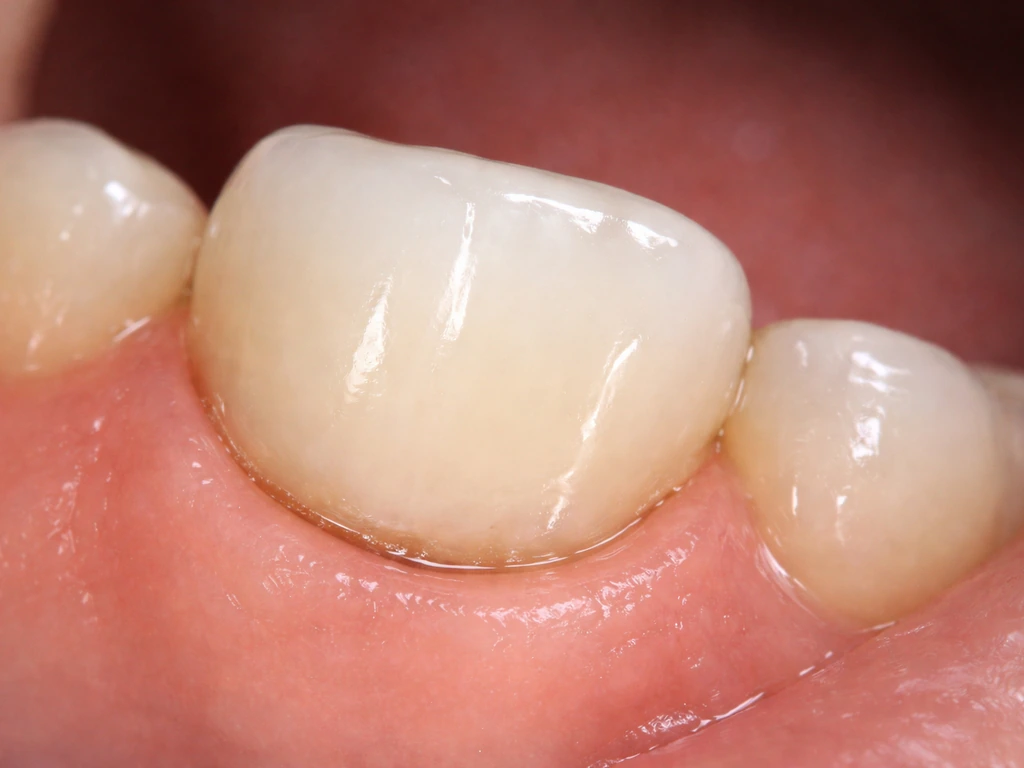
What it actually means when your gumline looks like it's not covering the crown
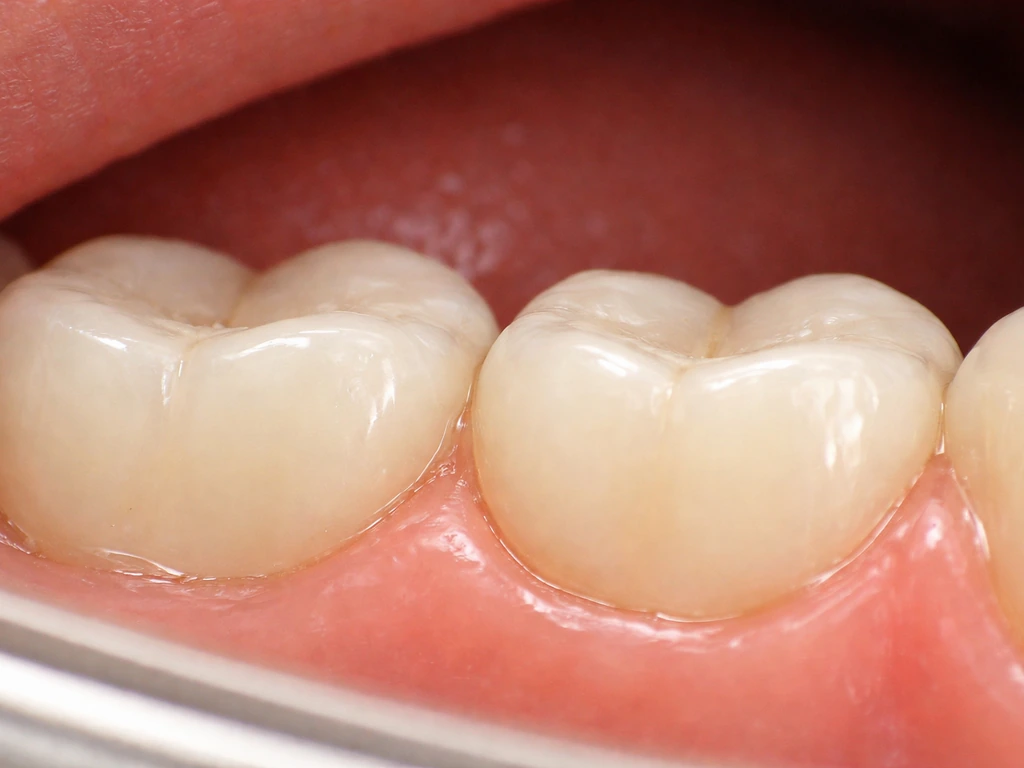
When a crown is made, the dentist takes an impression and the lab fabricates the crown so that its edge, called the margin, sits at or just below your gumline. The goal is for that margin to be hidden by gum tissue and for the crown to blend seamlessly with the tooth. When everything goes well, you never see the margin at all. When something goes wrong, you might notice a dark line at the gumline, a visible metal band, a gap between the crown and the surrounding gum, or tooth sensitivity near the gum edge.
What you're looking at in those cases is an exposed crown margin, and it can happen for a few different reasons. The gum may have receded away from where it was when the crown was made. The crown margin may have been placed incorrectly to begin with. The gum may be inflamed and swollen in a way that hides the problem temporarily, then shrinks back to reveal it. Or the crown simply doesn't fit as well as it should. These are not all the same problem, and they don't all have the same solution.
Do gums naturally grow around crowns? Healing vs. recession
In the first few weeks after a crown is placed, some gum movement is completely normal. The tissue gets irritated during the prep and impression process, and it can swell, pull back slightly, or look uneven. During this early phase, the gum does settle and remodel around the crown. Epithelialization after a gingival procedure takes roughly three to five weeks, and full remodeling of the attachment apparatus takes closer to three months. So if your crown was just placed and the gum looks a little off, some of what you're seeing may genuinely resolve on its own.
But here's the biology limit you need to know: gum tissue does not regenerate lost attachment the way skin heals a scratch. If the gum has receded away from the crown margin, meaning the tissue has moved apically (toward the root tip), it will not creep back up and cover the crown on its own. That kind of recession is a one-way street without intervention. So the question "will my gum grow around my crown" really has two parts: yes, it can adapt and stabilize during normal healing, and no, it cannot reverse actual recession without help.
This is similar to the question of whether gums grow around implants or bridges. In all those cases, gum tissue heals and forms a seal around the restoration, but once true recession has occurred, natural regrowth is not on the table.
Why the crown margin might be exposed: the most common reasons
There are several reasons a crown margin becomes visible, and some of them are more fixable than others. The most important thing is to identify which one you're dealing with.
Poor crown fit or margin adaptation
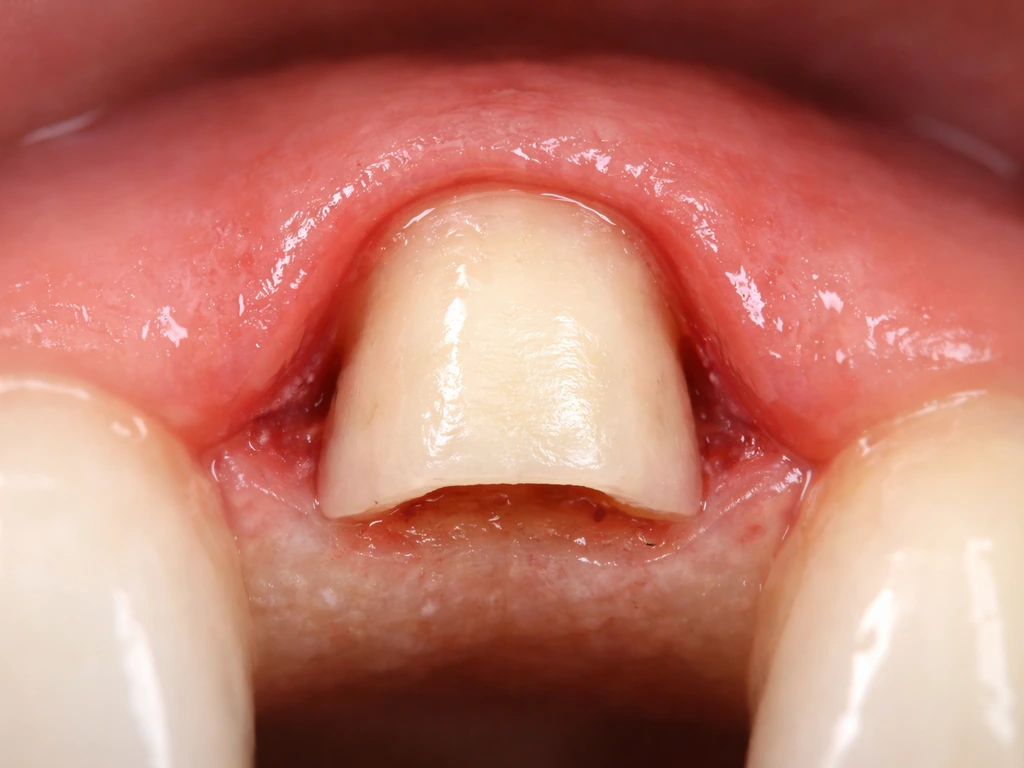
A crown that doesn't fit tightly against the tooth at the margin creates a small ledge or gap. Plaque collects there, triggers chronic inflammation, and that inflammation drives the gum to recede. Research on fixed prosthetic restorations confirms that poor margin adaptation creates a retentive area for plaque and leads to gingival inflammation and, over time, periodontal breakdown. If your crown has always had a rough edge at the gumline or if you feel a shelf with your tongue, poor fit could be the driver.
Margin placed too deep (biologic width violation)
There is a zone below your gumline, called the biologic width, where the gum and bone maintain a protective attachment to the tooth. It's roughly 2 to 3 millimeters from the crest of the bone to the gumline. When a crown margin is placed too far below the gum and encroaches on this zone, the tissue responds by migrating apically to re-establish that space. The junctional epithelium moves down, the gum recedes, and you see the margin. This is a documented cause of recession in crowned teeth and is addressed by re-establishing adequate room for gingival attachment.
Gum disease or chronic inflammation
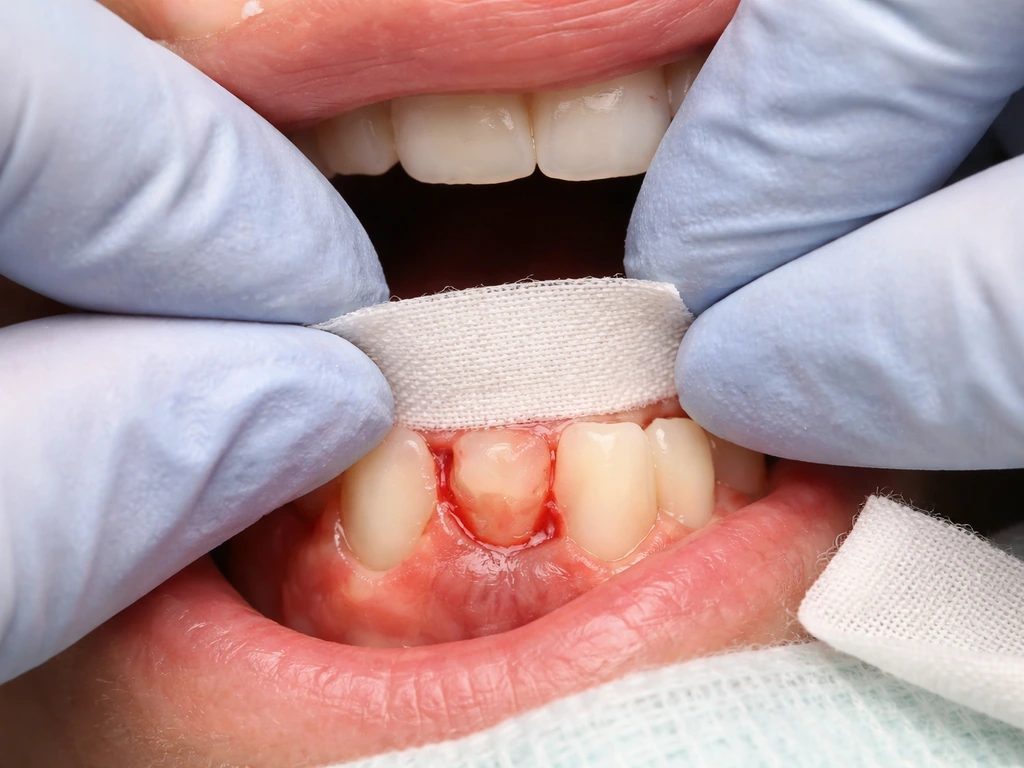
Active periodontal disease causes bone and gum loss independent of any crown. If you already had thin gum tissue or early bone loss when the crown was placed, the gum may recede further over time regardless of crown quality. Crowns don't cause gum disease, but they can harbor plaque at the margin, and any existing inflammation makes recession more likely.
Thin tissue biotype and other risk factors
People with a thin, delicate gum biotype are more prone to recession than people with thick, fibrous tissue. Other factors that increase recession risk around crowns include aggressive tooth brushing (especially with a hard-bristled brush), smoking, and older age. Smokers in particular are at higher risk because nicotine impairs blood flow to gum tissue and masks early signs of inflammation.
How long to wait, and how to tell if things are improving or getting worse
If your crown was placed within the last four to eight weeks, give the tissue time to settle. The gum is still remodeling. As long as you're not seeing active bleeding, pus, increasing sensitivity, or a growing gap at the margin, this can be a watch-and-wait period with good hygiene.
If it's been more than three months since the crown was placed and the margin is still visible, that's not normal healing lag anymore. At that point you're looking at either a fit problem, recession, or both, and you need a professional evaluation. The tissue level at about six weeks post any gingival procedure tends to predict where it will settle at six months, so by the time you're at three months, the picture is fairly clear.
Signs that things are getting worse, not better, include: the dark line or metal edge is growing wider or longer over time, you can see more of the crown than you could a month ago, you're developing sensitivity to cold or touch at the gumline near the crown, or the gum is bleeding regularly when you brush or floss near the crown. Any of these means the situation is progressing and waiting is no longer the right move.
What your dentist can check today
A dentist or periodontist can do a lot in a single visit to tell you exactly what's going on. Here's what a proper exam should include for this kind of concern:
- Periodontal probing: measuring pocket depth around the crown at six points to determine if there's active bone loss or just surface recession
- Margin check: using an explorer to feel whether the crown margin is flush, overcontoured, or has a ledge that's harboring plaque
- Radiograph (X-ray): checking the bone level adjacent to the crowned tooth and confirming where the crown margin sits relative to the bone
- Biologic width assessment: determining whether the margin is encroaching on the attachment zone and whether that's driving the tissue response
- Tissue biotype assessment: visually or with a probe, determining whether you have thin or thick gum tissue, which affects both the prognosis and treatment options
- Gum recession measurement: recording exactly how many millimeters of recession are present so that future visits can track whether it's stable or progressing
When you call to make that appointment, it helps to tell the front desk you're concerned about a visible crown margin and possible gum recession around a crown. That way you're more likely to be scheduled with enough time for a proper periodontal assessment rather than just a quick look.
Treatment options if natural coverage isn't going to happen
The treatment depends entirely on what's causing the problem. Here's how the options stack up from least invasive to most.
Non-surgical options
If the exposed margin is being driven by inflammation from plaque buildup, a professional cleaning and improved home care may stabilize or even slightly improve the tissue position. This isn't the gum growing back, but inflammation reduction can reduce puffiness and allow healthier tissue to sit more consistently around the crown. If the crown itself has an overhanging margin or rough edge, your dentist may be able to smooth and polish it without replacing the crown. If gum disease is a factor, scaling and root planing (a deep cleaning) is typically the starting point before any further decisions are made.
Crown replacement
If the crown fit is poor, the margin is in the wrong place, or biologic width is being violated, the long-term solution often involves replacing the crown. A new crown with a properly placed margin, good adaptation, and the right contour can dramatically reduce the inflammatory driver. On its own, this may not recover lost gum tissue, but it stops the cause and creates conditions where gum health can stabilize.
Crown lengthening (before a new crown)
If the existing margin is too deep and violating biologic width, a periodontist may recommend crown lengthening before replacing the crown. This procedure moves the gum and bone margin to a more apical position, creating room for the restorative margin to sit within the proper zone. After crown lengthening, there is a documented coronal rebound of roughly 1 to 3 millimeters when measured at 6 months to 1 year post-surgery, which dentists account for when planning the final crown margin placement. Healing takes about 3 months before the final crown is made.
Soft tissue grafting
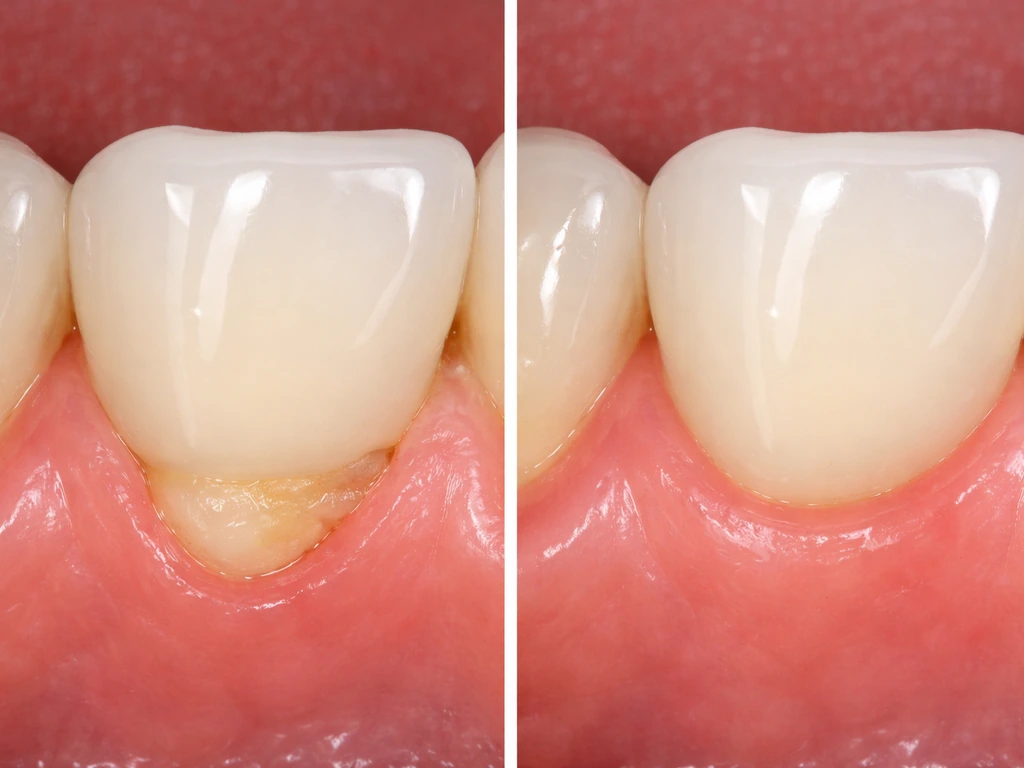
If recession has occurred and the goal is to actually cover the exposed margin with gum tissue again, a soft tissue graft is the surgical option. A connective tissue graft (taken from the palate) or an allograft material is placed over the recession site. This can achieve partial or full coverage of the exposed root and margin, improve aesthetics, and reduce sensitivity. Coverage success depends heavily on tissue biotype, the depth of recession, whether there's adequate blood supply, and the skill of the periodontist. This is not a guaranteed full recovery but in good candidates it works well. The question of whether gum grows over bone grafts, which is relevant when bone loss has accompanied the recession, involves similar tissue healing principles. This is why the same approach to soft tissue healing matters when bone grafting was used as part of recession treatment bone grafts.
| Option | Best suited for | Invasiveness | Can it cover exposed margin? |
|---|---|---|---|
| Professional cleaning + improved hygiene | Inflammation-driven tissue loss, mild cases | Non-surgical | Possibly, if swelling was masking healthy tissue |
| Crown margin smoothing/polishing | Minor overhangs without significant recession | Non-surgical | No, but stops further irritation |
| Crown replacement | Poor-fitting crown, wrong margin placement | Restorative (dental procedure) | No regrowth, but stabilizes tissue |
| Crown lengthening surgery | Biologic width violation before new crown | Surgical | Repositions tissue; does not add coverage |
| Soft tissue graft | True recession with exposed root/margin | Surgical | Yes, partial to full coverage in good candidates |
When to call your dentist urgently, and how to protect what you have
Most exposed crown margins are not dental emergencies, but some situations warrant a prompt call rather than waiting for your next routine visit. Contact your dentist soon if you notice any of the following:
- Pus, swelling, or a bad taste near the crowned tooth (possible infection or abscess)
- Significant pain or throbbing at or below the gumline
- The crown feels loose or your bite has changed suddenly
- You can see an obvious gap opening up between the crown and gum over a matter of days rather than months
- Bleeding that doesn't stop after brushing, or spontaneous bleeding without provocation
For prevention, the most impactful things you can do right now are: switch to a soft-bristled toothbrush and use gentle pressure rather than scrubbing, floss daily including around the crown margin where plaque accumulates most, and get professional cleanings at least every six months (or more frequently if your dentist has already identified gum issues). If you smoke, reducing or stopping is the single most important modifiable factor for gum health around any dental restoration. Ask your dentist whether your specific crown margin placement and tissue type put you in a higher-risk category so you know how closely to monitor things.
The bottom line is that gums do adapt and heal around crowns after placement, but they don't regenerate lost tissue on their own. If the margin is still visible after three months, the gum is not going to cover it without some kind of intervention. If the margin is still visible after three months, the gum is not going to cover it without some kind of intervention why do gums grow over braces. Getting a proper exam now gives you real information rather than guesswork, and many of the treatment options available are straightforward once the cause is identified.
FAQ
If I can still see the crown margin now, will my gum cover it later without treatment?
Usually no. If the margin has been visible for more than about 3 months, that strongly suggests true recession or a margin placement or fit issue, and the gum typically will not creep back up to fully cover it on its own.
What’s the difference between normal healing changes and a problem getting worse?
If you only notice a dark line or slight discoloration right after placement, it may be early healing or mild inflammation. But if the line is becoming wider, you can see more of the edge over time, or you get new cold or brushing sensitivity, treat it as progression and schedule an exam rather than waiting.
Can my gum shrink after crown placement and make the margin show even if the crown didn’t change?
Yes, because irritation and plaque can mask the margin temporarily, then reveal it as swelling goes down. A professional check for crown fit, inflammation, and probing depth at the gumline helps confirm whether you are seeing recession versus a short-term “hidden” margin.
Should I stop flossing around the crown if my gums bleed or the margin looks exposed?
Avoid scrubbing the area, but don’t skip cleaning. Use a soft-bristled brush with gentle pressure and floss once daily, then ask your dentist whether a water flosser or an interdental brush size is appropriate for the space at your margin.
Is it possible to have gum recession around a crown without noticeable pain?
You can have recession without pain. The most useful signs are what you see and what the dentist measures, for example bleeding with probing, changes in pocket depth, and how far the margin is from the gumline. If you’re unsure, ask for a periodontal exam rather than relying only on symptoms.
How does smoking change my risk of gum recession around a crown?
Smoking affects healing and also makes it harder to detect inflammation early. If you smoke, tell your clinician, ask about a cessation plan, and expect you may need closer monitoring or earlier intervention if a visible margin persists.
If the crown feels rough near the gumline, can it be fixed without replacing it?
Not necessarily, but roughness and overhangs can worsen plaque retention and drive inflammation. If your dentist can feel a shelf with a tool or you notice food trapping, ask whether a margin smoothing and polishing attempt is appropriate versus replacement.
Could this be biologic width, and how would I know?
Yes. If the crown margin is placed too deep and violates biologic width, tissue migrates to re-establish the needed space. In that scenario, simply cleaning may calm inflammation, but the margin may keep staying visible unless the restorative position and biologic width are addressed.
If I get a deep cleaning, will that make the gum grow back over the exposed crown margin?
Sometimes. A deep cleaning can reduce inflammation, but it will not rebuild lost attachment when recession has already occurred. Ask whether your main goal is stabilizing gum health, eliminating a plaque source, or covering the exposed margin.
How can I tell whether I’m a good candidate for a soft tissue graft to cover the margin?
Coverage procedures have best results with certain conditions, like adequate blood supply and favorable tissue biotype. Your periodontist can estimate expectations based on recession depth, the amount of keratinized tissue, and whether there is enough support for graft integration.
When should I contact my dentist urgently instead of waiting?
Act sooner if you have pus, increasing swelling, an enlarging gap, or ongoing bleeding around the crown. New or worsening sensitivity plus a margin that is expanding over weeks is also a reason to call promptly rather than waiting for a routine visit.
What should I ask for during the exam so I get a clear answer about the cause?
Get your crown checked for both fit and surface adaptation, and ask for probing measurements around the crown, not just a visual look. Request that the dentist evaluate inflammation, biologic width concerns, and whether the margin is acting as a plaque trap.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn
Learn which teeth seem to grow twice: primary replaced by permanent, plus wisdom teeth timing and limits on regrowth
Milk teeth eruption timeline by age: first tooth, full primary set, what’s normal, and when to see a pediatric dentist.

