What tartar removal actually does to your gums
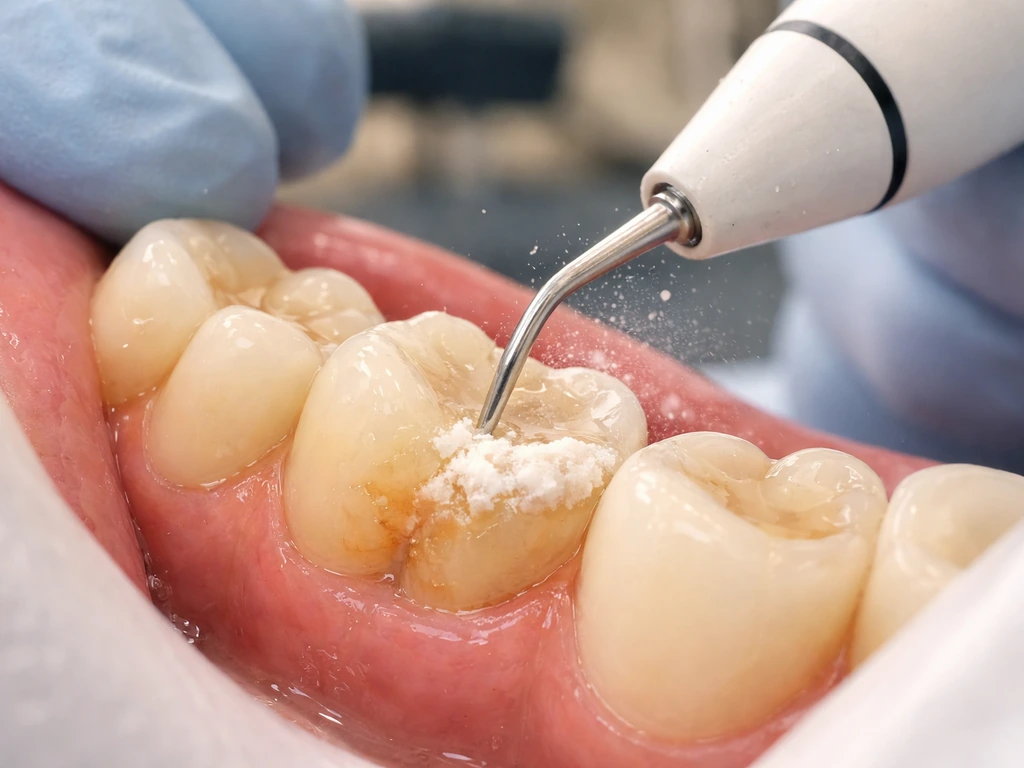
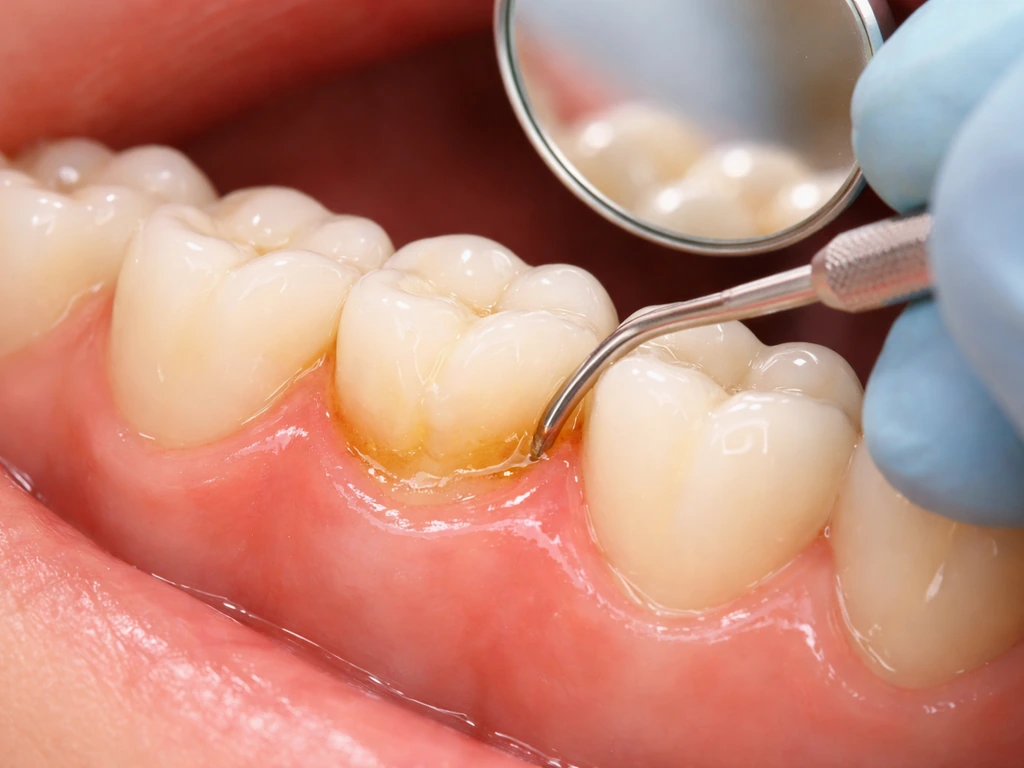
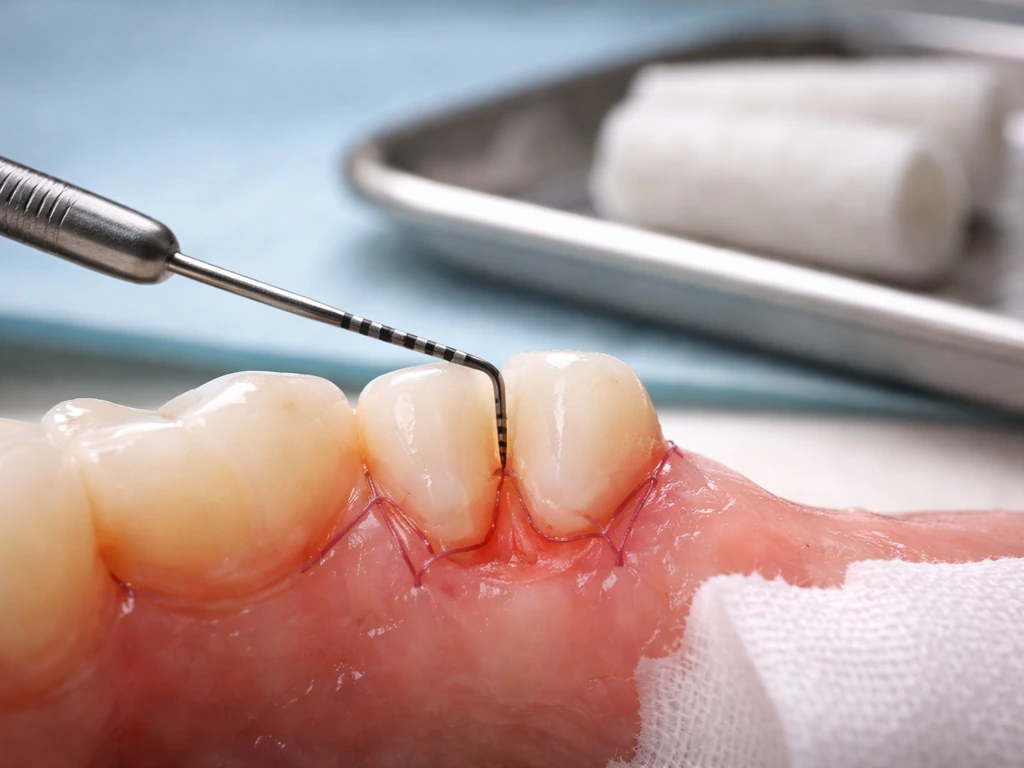
Tartar (dental calculus) is hardened bacterial plaque that your toothbrush cannot remove. It acts like a chronic irritant glued to your teeth at and below the gumline. The longer it sits there, the more your gum tissue responds with inflammation, swelling, and eventually destruction of the structures that hold your teeth in place. Professional tartar removal, called scaling (and scaling and root planing, or SRP, when it goes deeper under the gumline), physically removes that calculus. The American Dental Association classifies this as non-surgical periodontal treatment targeting both supragingival (above the gumline) and subgingival (below the gumline) deposits.
Here is the important distinction most people miss: scaling removes the irritant, but it does not directly rebuild tissue. What happens next is that your immune system stops fighting an active bacterial assault, inflammation subsides, and the tissue can stabilize and, in some cases, partially reattach. The ADA notes that periodontal tissues need about four weeks after non-surgical treatment to show their optimal response, which is why your dentist or hygienist will typically schedule a re-evaluation around that time rather than judging results immediately.
Scaling is fundamentally different from more aggressive periodontal surgery like osseous surgery. With SRP, you are in the non-surgical lane, trying to control infection and allow natural tissue stabilization. That matters when setting your expectations for recovery.
Why your gums may look like they receded after a cleaning
This confuses a lot of people, and understandably so. You go in for a cleaning, and when you look in the mirror a few days later, your teeth look longer or your gums look lower. That feels backwards. What actually happened is that before the cleaning, inflamed gum tissue was swollen and puffed up around your teeth, covering more of the tooth surface than it should. That puffiness made your gums look full or even normal. Once the tartar was removed and the inflammation started to resolve, the tissue tightened and returned closer to its true, healthy position, which is higher on the tooth. The gums did not actually recede further. They deflated from their swollen state.
A published review on gingival changes after scaling and root planing confirms this directly, noting that gingival recession can appear during healing after SRP because swollen tissue contracts as it heals. This is normal and expected. However, if your gums were already dealing with true bone and attachment loss before the cleaning, that deflation can also unmask recession that was always there but hidden under puffy tissue. The cleaning did not cause it; it revealed it.
What can improve vs. what usually cannot
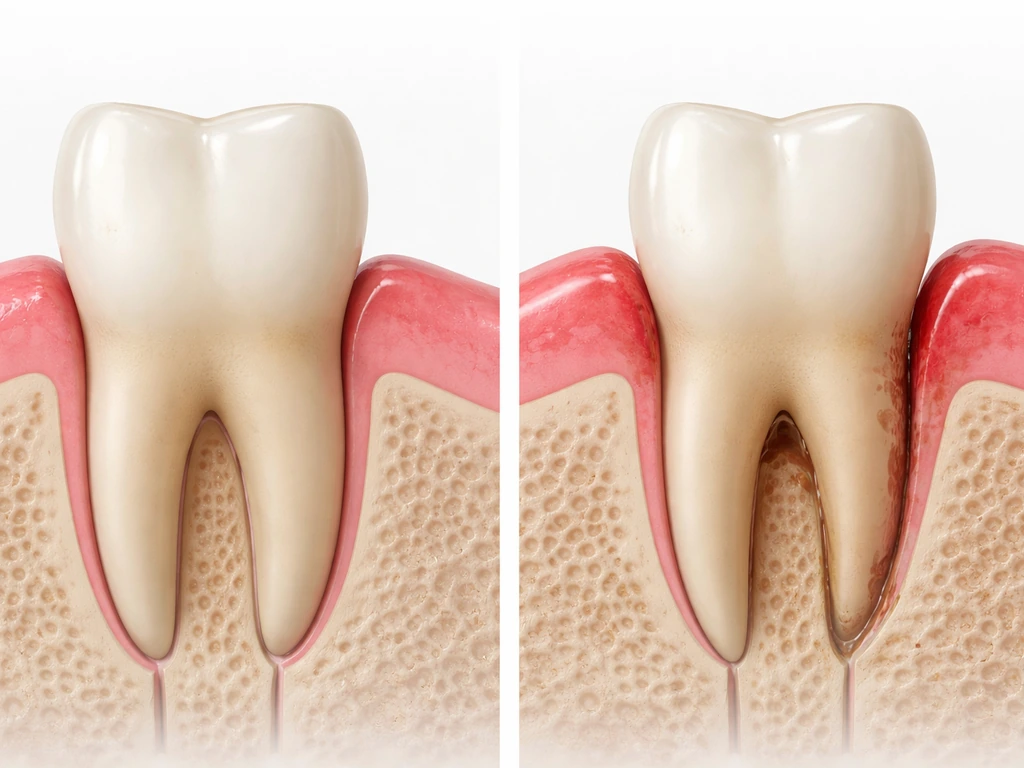
There are two different structures involved here, and they behave very differently after tartar removal. Understanding them changes how you interpret what you see and feel.
What can genuinely improve
Free gingiva, the soft tissue that forms the collar around your tooth, responds well to eliminating infection. When the bacterial load is reduced through scaling and then kept low through your daily brushing and flossing, inflamed gingiva can tighten, firm up, and stop bleeding. Shallow periodontal pockets (up to about 3mm) can reduce in depth after SRP as the inflamed tissue contracts and firms up. In early gum disease (gingivitis or mild periodontitis), this improvement can be substantial and genuinely look like the gums have 'grown back. If you are wondering about Invisalign and whether gums will grow back after aligner-related irritation, the same idea applies: inflammation may improve, but true attachment loss does not regenerate on its own. ' Technically, what happened is that the inflammation resolved and the tissue rebounded to its healthy baseline.
What usually does not come back without intervention
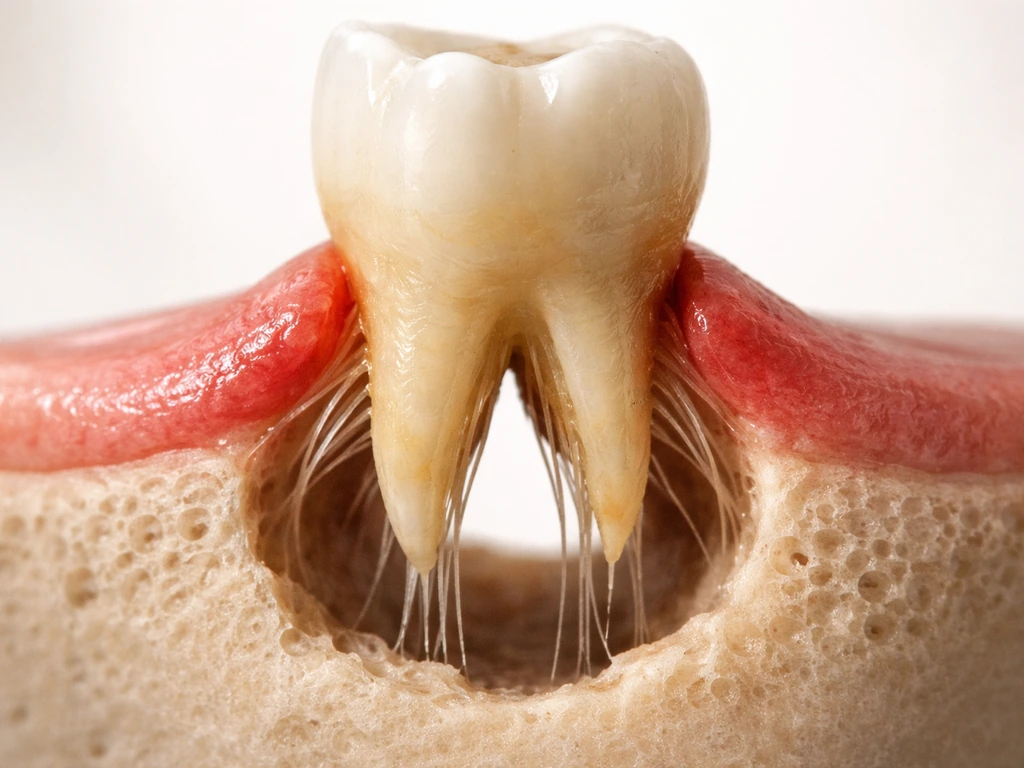
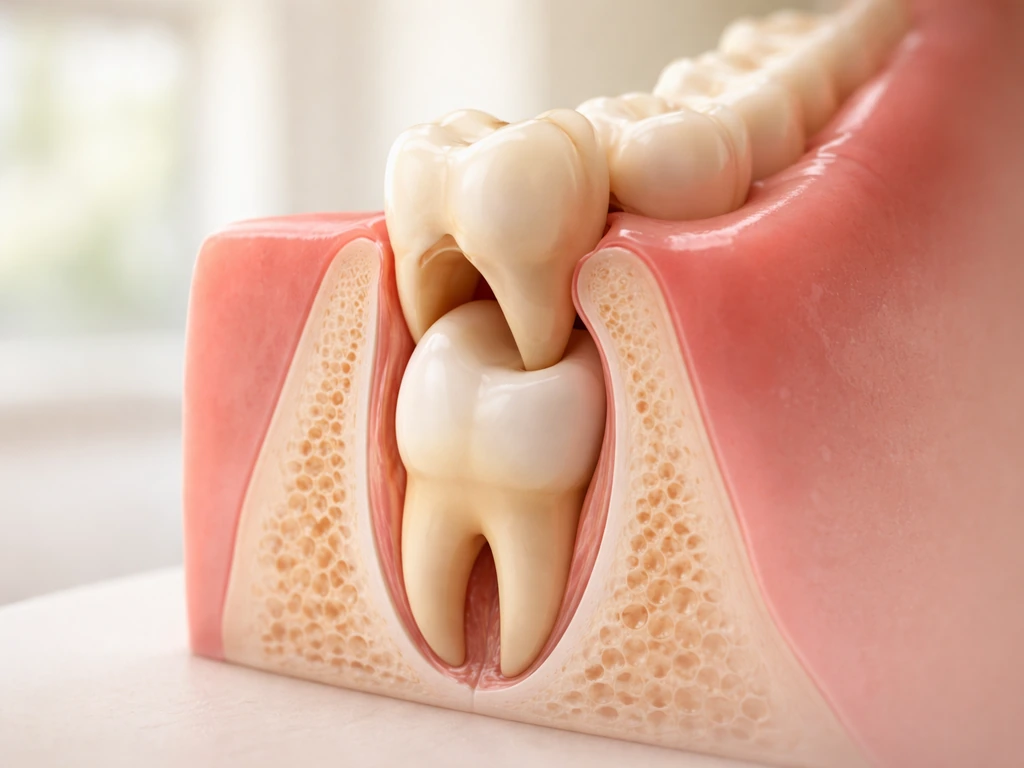
The periodontal attachment, meaning the connective tissue fibers and the alveolar bone that anchor your tooth in the socket, does not regenerate on its own once it has been destroyed. If you are considering crown lengthening, ask whether the issue is inflammation that can settle or true gum recession that would need a graft because it does not naturally regrow do gums grow back after crown lengthening. That is why true gum recession from attachment and bone loss usually does not grow back after plaque or tartar removal without a graft or other periodontal treatment do your gums grow back after plaque removal. Porcelain veneers can improve how teeth look, but they do not cause true gum recession to regrow do gums grow back after veneers. This is the hard biological reality. When a dentist measures clinical attachment level (CAL), they are measuring from a fixed anatomical reference point called the cementoenamel junction (CEJ) to the bottom of the pocket, combining pocket depth and gum recession. True attachment loss shows up as a permanently elevated CAL measurement that does not normalize after scaling, even when pocket depths shrink and gum inflammation resolves. Exposed root surfaces stay exposed. Bone that has been resorbed does not grow back with scaling alone. Those changes require surgical options like gum grafting or, in some cases, regenerative procedures, and even those have limits depending on how much damage exists.
| Tissue or change | Can improve after tartar removal? | Notes |
|---|
| Gingival inflammation and swelling | Yes, often fully | Resolves as infection is controlled |
| Bleeding on probing | Yes, significantly | A sign of active disease; improves with hygiene |
| Shallow pocket depths (1-3mm) | Yes | Tissue tightening can normalize shallow pockets |
| Deeper pocket depths (4mm+) | Partially | SRP can reduce depth; deeper pockets may need surgery |
| True gingival recession (root exposed) | No, not without surgery | Gum grafting needed to cover exposed root |
| Bone loss (alveolar bone) | No, not with SRP alone | Regenerative surgery may help in select cases |
| Clinical attachment level (CAL) loss | Minimal to none with SRP alone | Surgical/regenerative procedures needed for significant gain |
Normal healing timeline vs. signs something is wrong
The first week after a deep cleaning is typically the roughest. Expect some sensitivity, especially to cold, because tartar was shielding the root surface and now it is exposed. Mild soreness and bleeding when brushing gently are both normal. Your gums may look slightly lower on your teeth as the swelling goes down, and that is the inflammation resolving, not new recession happening. If you are dealing with gum changes after a dental procedure like wisdom teeth removal, the same idea applies: inflammation can settle and tissue may look different while true recession and bone loss still do not regrow on their own will my gums grow back after wisdom teeth removal.
By weeks two to four, sensitivity usually decreases noticeably, gums should look pinker and tighter rather than red and puffy, and bleeding should be reducing. The ADA's four-week re-evaluation benchmark exists precisely because this is when your dentist can measure whether pocket depths have improved and whether the tissue is responding as expected.
Get back to your dentist sooner if you notice any of the following after your cleaning:
- Increasing pain, not decreasing, after the first few days
- Swelling that is getting worse or spreading to your face or jaw
- A bad taste or smell that persists beyond the first week, which may suggest infection
- Teeth feeling looser than before the cleaning
- Gums that are still bright red and bleeding heavily at three to four weeks post-cleaning
- Visible pus around the gumline
These are not normal healing signs. They suggest either an active infection that needs treatment or periodontitis that is not responding to non-surgical care alone.
What affects how well your gums recover
Not everyone heals the same way after tartar removal, and the difference is not random. Several factors meaningfully affect outcomes.
Severity of periodontitis is probably the biggest factor. If your pockets were mostly at 4mm or less and bone loss was minimal or absent, your tissue response after SRP will likely be very good. If you have deep pockets of 6mm or more, significant bone loss, or furcation involvement (where the disease has reached the area between tooth roots), SRP alone may not be enough to fully resolve the problem, and surgical options become more relevant.
Smoking dramatically undermines healing. It reduces blood flow to gum tissue, impairs the immune response, and masks clinical signs of disease like bleeding (smokers often have less bleeding even with active disease because smoking constricts blood vessels). If you smoke, your gum tissue simply does not heal as well, and your periodontitis is more likely to progress even after treatment.
Diabetes, particularly uncontrolled diabetes, is consistently recognized as a major risk factor for periodontitis and for poor healing. The relationship goes both ways: gum disease makes blood sugar harder to control, and high blood sugar impairs the tissue repair process.
Your brushing and flossing technique after the cleaning matters enormously. Brushing too hard is one of the most common causes of gum recession, and doing it after a cleaning (when tissue is already sensitive and slightly vulnerable) can worsen recession rather than help it. Brushing too hard is one of the most common causes of gum recession, and if you are wondering whether the damage can reverse, related guidance on can gums grow back after brushing too hard is a useful comparison. Genetics also play a role in how susceptible your tissue is to recession and how well it responds to treatment.
Finally, how well you maintain your teeth going forward is arguably as important as the cleaning itself. The ADA is explicit that periodontitis patients need lifelong supportive care and regular monitoring because the condition can recur. Skipping follow-up appointments and returning to poor home care habits essentially undoes the work of the cleaning over time.
What to do right now: aftercare, monitoring, and questions to ask your dentist
For the first 24 to 48 hours after scaling, avoid very hot or very cold foods and drinks if you are sensitive. Eat soft foods if your gums are sore. Do not skip brushing and flossing, but be gentle. Use a soft-bristle toothbrush and hold it at a 45-degree angle to the gumline, using light pressure in small circular or gentle back-and-forth strokes. You are not trying to scrub; you are trying to disrupt plaque without traumatizing the tissue. If your dentist or hygienist prescribed or recommended an antiseptic rinse (like chlorhexidine), use it exactly as directed and for the duration recommended, not just when you feel like it. Antiseptic rinses are a clinical adjunct, not a substitute for mechanical cleaning.
How to monitor your own healing

- Check your gums in good light every few days. Healthy healing gums should look progressively pinker, firmer, and less puffy over two to four weeks.
- Note whether bleeding on brushing is decreasing over time. Some initial bleeding is normal, but it should trend down, not stay constant or worsen.
- Be aware of sensitivity changes. Sensitivity often peaks in the first week and then fades. Sensitivity that is getting worse, not better, after week one is worth flagging.
- Watch for the gum margin position. Some apparent recession as swelling resolves is expected. Significant further changes after the first two weeks should be discussed with your dentist.
- Keep a simple log if you want: note which areas are sensitive, whether there is bleeding, and whether gums look healthier or the same at each check.
Questions to bring to your follow-up appointment
Your four-week re-evaluation after SRP is not just a routine check. It is when your dentist re-probes your pockets and compares measurements to the baseline. Come prepared with specific questions:
- What are my periodontal probing depths now compared to before the cleaning, and which areas improved?
- Has my clinical attachment level (CAL) changed, or is the improvement mainly from gum shrinkage?
- Are there any pockets that did not respond well to scaling that might need a different approach?
- Do I have any genuine gum recession, and if so, am I a candidate for a gum graft or other procedure?
- What does my bone level look like on X-rays, and has it changed?
- Should I be on a more frequent maintenance schedule (every three to four months instead of every six)?
- Are there any areas where I am brushing too hard or missing, that I should change my technique for?
If your gums do not improve after non-surgical treatment or if recession and pocket depth are significant, your dentist may refer you to a periodontist. A periodontist can discuss options including osseous surgery, guided tissue regeneration, or connective tissue grafts, each targeting different aspects of what SRP alone cannot fix. Understanding whether you are dealing with reversible inflammation or true structural loss is the difference between needing better home care and needing surgery, so those probing numbers and CAL measurements are worth asking about by name.
The same biological limits discussed here apply across a range of scenarios, whether the cause of gum changes is scaling, plaque buildup, aggressive brushing, or even dental procedures. The underlying principle is consistent: gingival inflammation can resolve and tissue can rebound, but lost attachment and exposed root surface do not regenerate without specific intervention. Knowing which category you are in after your cleaning is the most practical, actionable thing you can walk away from this article with.