Here is the direct answer: gums do not truly "grow back" after osseous surgery the way skin heals over a cut. What you see in the weeks and months after periodontal or implant-related surgery is a combination of swelling resolution, flap repositioning, and soft-tissue remodeling, not true regeneration of lost gum tissue. Some coronal rebound (the gum margin creeping back upward) does happen, and it can be significant. But whether the gum returns to its exact pre-surgery height depends heavily on the type of procedure, your individual tissue, and how well the healing goes. Let's break down exactly what's happening and what you should realistically expect.
Do Gums Grow Back After Osseous Surgery? Timelines and What to Expect
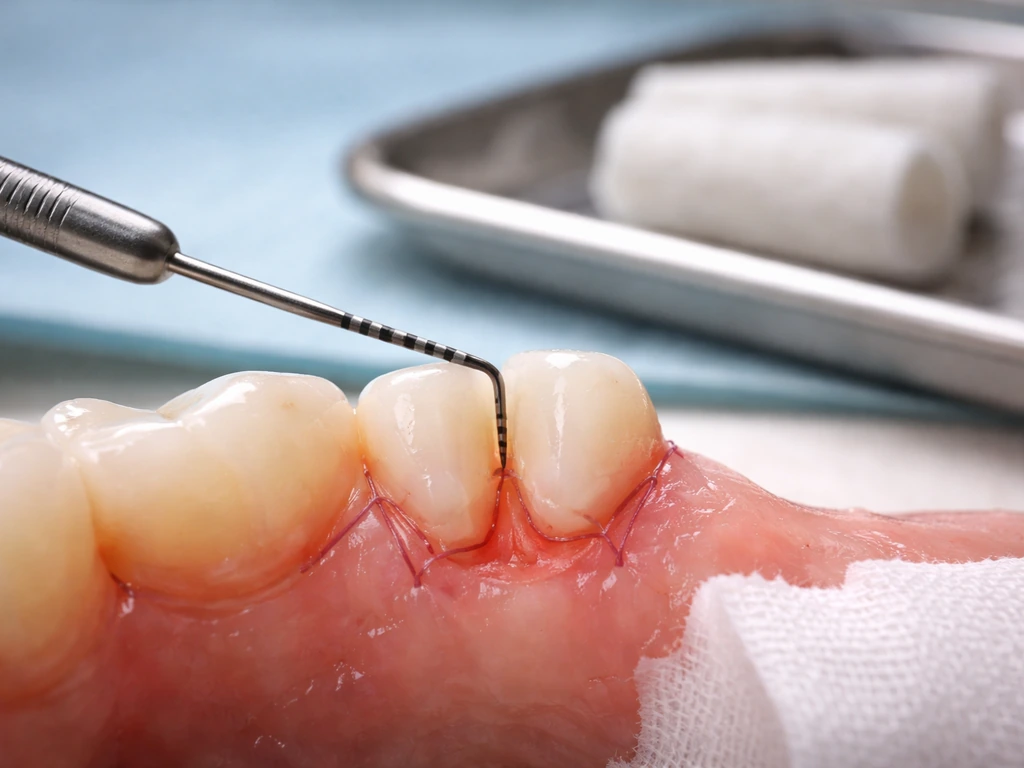
What "gum regrowth" actually means after osseous surgery
When people ask if gums grow back, they usually picture the gum line moving back up to where it was before surgery. That's understandable, but it conflates a few different biological processes. True gum regeneration would mean new periodontal attachment, new bone, and new soft tissue all forming in the space where disease destroyed them. That only happens in specific regenerative procedures using barrier membranes, bone grafts, or growth factors. Osseous surgery, particularly osseous resective surgery, is actually designed to reshape the bone and reposition the gum to eliminate diseased pockets. The goal isn't to restore the original anatomy; it's to create a healthy, stable, maintainable one. So when the gum appears to "come back" after osseous surgery, what's really happening is tissue remodeling and, in some cases, coronal migration of the gingival margin over time, not regeneration.
This matters because patients often walk in expecting their gums to look like they did before surgery, and that expectation gap causes a lot of anxiety. It also explains why gum changes after procedures like scaling or tartar removal follow a similar logic: do gums grow back after tartar removal is a question rooted in the same misconception, that tissue removed or displaced by a procedure will simply regenerate. The honest answer, across almost all of these scenarios, is that healing and regeneration are not the same thing.
Do gums grow back after flap surgery
Osseous resective surgery (ORS) involves lifting a flap of gum tissue, reshaping the underlying bone to eliminate the bony defects that harbor bacteria, and then suturing the flap back down, often at a slightly more apical (lower) position than before. This is where the perception of "gum loss" comes from, since the tissue is intentionally placed lower to reduce pocket depth. After that, there is genuine coronal migration over time, meaning the gum margin does creep upward to some degree.
Research using a fiber retention osseous resective technique found that over six months, the gingival margin moved coronally by an average of around 2.0 mm in apically positioned flap cases and about 1.3 mm in crestal flap cases. That's measurable and clinically meaningful. However, this rebound is not complete restoration to the original position. Longer-term data shows that sites treated with fiber retention ORS tend to complete most of their coronal rebound within the first 12 months, while conventional ORS sites can continue rebounding for up to about 48 months before stabilizing. So the gum does move back somewhat, but how much depends on where the flap was placed, the bone level beneath it, and the surgical technique used.
One important concept here is the distance between the sutured flap margin and the alveolar crest. When that distance is 2 mm or less, gingival margin stability is less predictable, and you tend to see more unpredictable rebound or recession. When there's adequate distance, outcomes are more stable. This is the kind of detail your periodontist is factoring in during surgery, even if they don't always explain it this way post-op.
Do gums grow back after implant surgery
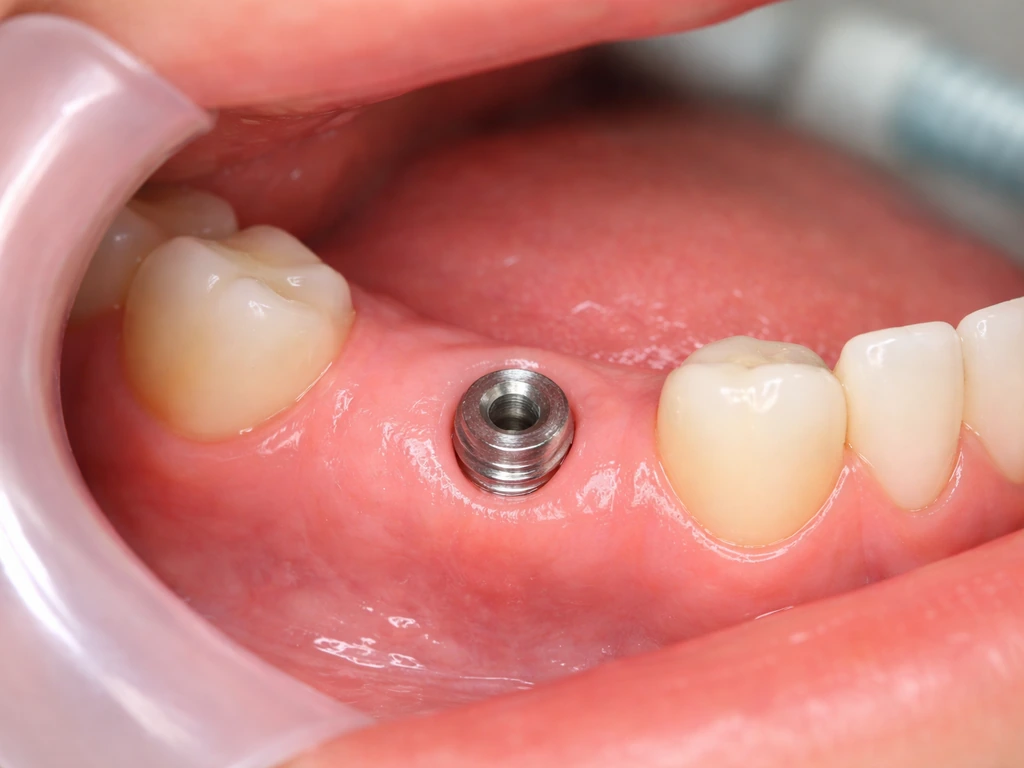
Implant-related gum changes follow a different path than flap surgery for natural teeth, and it's worth treating them separately. With implants, the soft tissue that forms around the implant (called peri-implant mucosa) is biologically different from the attached gingiva around natural teeth. It doesn't have the same fibrous attachment, and it's more vulnerable to recession over time.
Studies tracking patients for one year after implant-supported fixed prostheses found that peri-implant mucosal recession does occur during that first year, and it's more common in the maxilla (upper jaw) than the mandible. When guided bone regeneration (GBR) is also involved, long-term data from studies with at least five years of loading shows that marginal soft tissue recession is a common feature, not an exception. This isn't a surgical failure. It's the expected biology of peri-implant tissue as it matures and adapts to function.
Even when keratinized tissue augmentation is done around implants to try to stabilize the soft tissue zone, reduction in the augmented tissue volume continues for years. Case series tracking patients for up to 20 years show meaningful reduction between the immediate post-augmentation result and the three-year and beyond measurements. So when someone asks whether gums grow back after implant surgery, the short answer is: some healing and initial tissue fill does occur, but the long-term trajectory for peri-implant tissue often involves gradual recession rather than restoration of original soft-tissue dimensions.
This is distinct from what happens after tooth extractions. If you've ever wondered about whether gums grow back after wisdom teeth removal, the answer involves similar principles: the socket fills with granulation tissue and eventually bone, and the overlying gum heals closed, but the anatomy is permanently changed from what it was before extraction.
How long soft tissue takes to heal vs what's actually stable long-term
This is where a lot of the confusion lives. Early healing (the first two to three weeks) involves granulation tissue formation, re-epithelialization, and vascular changes. The tissue looks puffy, red, and different from what it will eventually be. By weeks two and three, the main soft-tissue wound healing events are largely completed. After that comes the maturation and remodeling phase, which takes much longer.
For conventional flap surgery, complete soft-tissue healing in terms of the tissue appearing clinically healed occurs around five to six weeks on average. Flapless implant placement heals faster, around four to four-and-a-half weeks. But "healed" doesn't mean "stable." The gum margin continues shifting for months to years after that initial closure. Here is a rough timeline to set realistic expectations:
| Timeframe | What's happening | What you should expect |
|---|---|---|
| 0–2 weeks | Granulation tissue forming, sutures in place, swelling present | Tissue looks puffy and different; this is normal |
| 2–6 weeks | Re-epithelialization mostly complete, sutures removed | Tissue looks more settled; still not final position |
| 3–6 months | Significant coronal rebound occurring (especially after ORS) | Gum margin moving upward; gum appearance actively changing |
| 6–12 months | Tissue largely stabilizing for fiber retention ORS cases | Most of the rebound you'll see has happened |
| 12–48 months | Continued slow rebound in some conventional ORS cases; recession possible with implants | Long-term stable state emerging; implant tissue may still recede |
The takeaway: don't judge your final result at six weeks. The tissue is still moving. But also don't assume that time alone will bring everything back to where it was. For many patients, the three-to-six-month mark is when you can have a realistic conversation with your periodontist about whether the outcome is what was planned.
What actually determines how much gum comes back
Not all osseous surgery outcomes are equal, and several factors meaningfully affect how much coronal rebound happens and whether soft tissue stays stable long-term.
Surgical technique and flap design
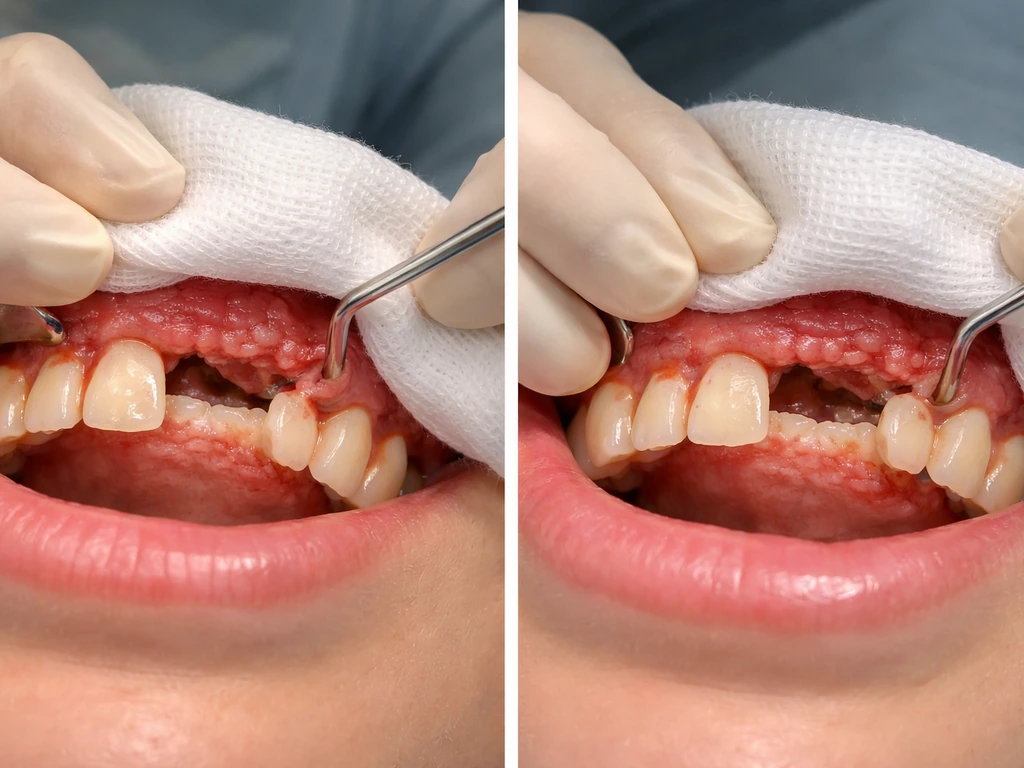
Where the surgeon positions the flap margin relative to the alveolar crest matters enormously. An apically positioned flap placed further from the crest allows more predictable rebound. A crestal position gives less. The use of fiber retention techniques (where supracrestal fibers are preserved) also appears to support more coronal migration than conventional ORS. Your periodontist's training and technique aren't just stylistic choices; they directly affect how your tissue behaves afterward.
Whether a soft-tissue graft was used
If a connective tissue graft or free gingival graft was added during or alongside the osseous procedure, there's more tissue volume to work with, and outcomes tend to be more favorable in terms of coverage and keratinized tissue width. Without grafting, the available tissue is only what was already there, and if that was thin to begin with, results are more limited. This is particularly relevant for implant sites, where the baseline tissue phenotype around the implant heavily predicts long-term stability.
Your baseline gum phenotype
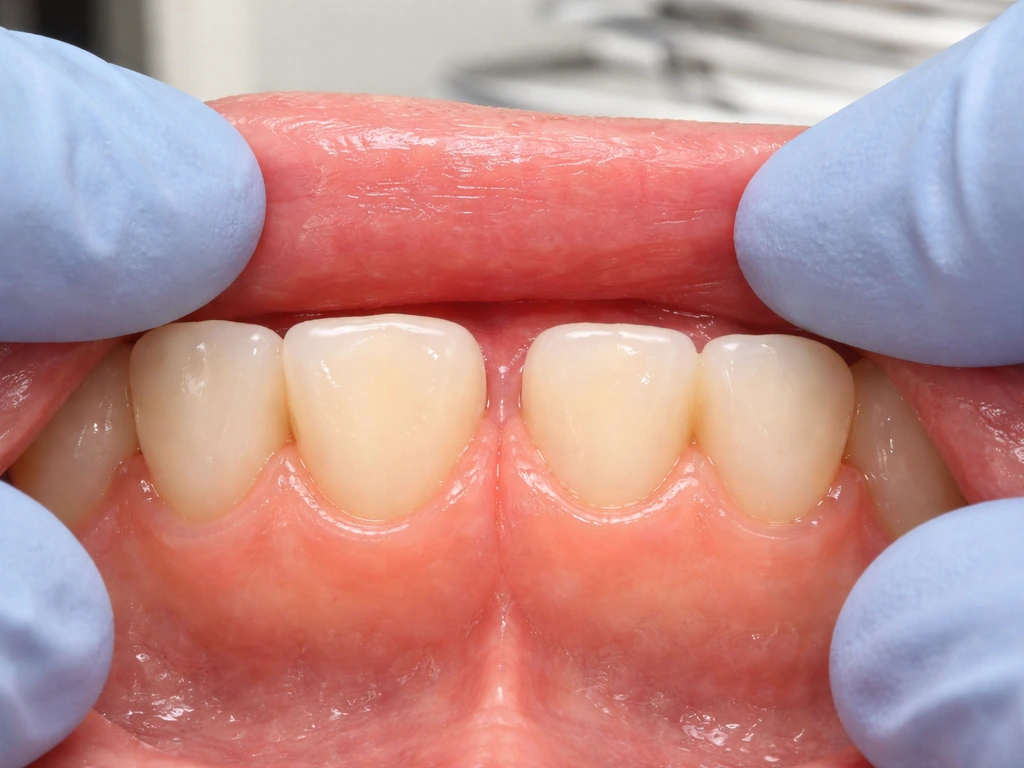
Gum tissue comes in two broad phenotypes: thick and flat, or thin and scalloped. Thick-phenotype patients tend to heal with more volume and show better coronal rebound. Thin-phenotype patients are more susceptible to recession post-surgery and see less rebound. This isn't something you can change, but it's something your surgeon should be accounting for in the treatment plan.
Bone levels beneath the tissue
The gum follows the bone. If significant bone loss was present before surgery and bone recontouring removed more, the soft tissue has less bony support to rest on. This limits how far coronally the gum can realistically migrate. Conversely, if the bone levels are relatively maintained and the procedure was conservative, the tissue has more structural support for rebound.
Patient-level factors
Smoking is probably the single biggest modifiable factor. It impairs vascularization, slows healing, and increases the risk of infection and attachment loss after periodontal surgery. Even one day of not smoking post-op is encouraged in surgical aftercare protocols, but honestly, stopping for the full healing period (and beyond) makes a real difference. Diabetes, particularly uncontrolled diabetes, similarly impairs wound healing and compromises the collagen maturation that's essential for stable soft tissue. Plaque control post-surgery is critical too. Inflammation from plaque disrupts the remodeling phase and can push the tissue margin apically rather than coronally. These aren't abstract risks; they directly determine whether you're in the group that sees good rebound or the group that sees recession.
When gums won't fully come back and signs something's wrong
Some degree of gum position change after osseous surgery is expected and permanent. That's not necessarily a problem if the pockets are gone and the tissue is healthy. But there are situations where the lack of regrowth signals a real issue rather than just expected remodeling.
Progressive recession (the gum line continues moving downward weeks or months after the initial healing phase), increasing tooth sensitivity that wasn't there before, persistent swelling or redness that doesn't improve, and visible bone or implant threads at the gum line are all signs that something more than routine remodeling is happening. For implant patients especially, these could be early signs of peri-implantitis, a destructive inflammatory condition that the European Federation of Periodontology has published detailed clinical guidelines on managing. Catching this early matters; the guidelines emphasize that progressive peri-implant bone loss requires intervention, not watchful waiting.
Contact your surgeon promptly if you experience any of the following:
- Severe pain that keeps you from sleeping or functioning normally and isn't responding to prescribed pain relief
- Persistent fever, especially if you're already on antibiotics
- Significant swelling that is getting worse rather than better after day three
- Swelling or tightness extending into your throat or difficulty swallowing
- Continued heavy bleeding more than two days after surgery
- Gum line that appears to be actively and progressively pulling away from teeth or implants after the initial six-week healing window
- Any visible loose sutures or tissue flap that seems to have separated
Don't minimize these symptoms or wait to see if they resolve on their own. The window for catching and correcting early complications is narrow, and acting quickly protects the investment you've made in your periodontal health.
Practical steps to support healing right now
What you do in the first few weeks post-surgery has a direct effect on how much rebound you get and how stable your tissue ends up. Here is the practical guidance based on what post-surgical protocols actually recommend.
- Do not brush or floss the surgical site on the day of surgery. The morning after, you can brush and floss other areas of your mouth, but stay away from the surgical site until your periodontist clears you. Disrupting the early clot or sutures undoes the repair.
- Use ice packs on the outside of your face for the first 24–48 hours to reduce swelling. Apply in 20-minute on/off cycles.
- Take prescribed antibiotics for the full course, even if you feel fine. Stopping early allows bacterial regrowth that can compromise healing.
- Don't smoke. Not on day one, not on day three, not for the healing period. This is the highest-impact thing you can do.
- Eat soft foods and avoid anything hard, crunchy, or that requires heavy chewing near the surgical site. Think scrambled eggs, yogurt, soft pasta, and smoothies.
- Rinse gently with chlorhexidine or prescribed rinse as directed, but don't swish aggressively. You're trying to keep the area clean without mechanically disturbing the flap.
- Keep your head elevated when sleeping for the first few nights to reduce swelling and bleeding.
- Manage blood sugar if you have diabetes. Hyperglycemia directly impairs the collagen formation needed for stable tissue remodeling.
- Attend all follow-up appointments. The six-week, three-month, and six-month visits aren't optional check-ins; they're when your surgeon is evaluating whether the tissue is tracking as expected or needs intervention.
Plaque control once you're cleared to clean the surgical site is equally important. Inflammation from bacterial biofilm is a direct antagonist to coronal rebound and tissue stability. This is true whether you're healing after osseous surgery, after crown lengthening (the gum dynamics are closely related, and whether gums grow back after crown lengthening follows the same biological principles), or after any other soft-tissue procedure.
Questions to ask your periodontist at your follow-up
Going into follow-up appointments with specific questions gets you much better information than a general "how does it look?" conversation. Here are questions worth asking:
- Where did you position the flap relative to the alveolar crest, and how much coronal rebound should I realistically expect over the next six months?
- Was a connective tissue graft used, and if not, would one have been appropriate for my tissue type?
- What's my gingival phenotype, and how does that affect my prognosis for tissue stability?
- At what point will the gum position be considered stable and what will you be measuring to assess that?
- For implant patients: what's my keratinized tissue width around the implant, and is it adequate for long-term health?
- What are the early signs of peri-implantitis I should watch for between appointments?
- How frequently do I need professional cleaning around this site going forward?
The bigger picture on gum regrowth myths
A lot of the "do gums grow back" anxiety online is driven by a real misunderstanding of gum biology. Gum tissue doesn't regenerate the way the internet sometimes implies. Questions like whether gums can grow back after brushing too hard or whether gums grow back after plaque removal all hit the same wall: gum tissue that is lost to recession or destroyed by disease does not spontaneously regenerate. What can happen is that remaining tissue heals, the tissue volume can be surgically augmented, and inflammation-driven pseudo-pocketing can resolve to reveal healthier tissue beneath. But that is not the same as regrowing what was lost.
Orthodontic treatment is another area where gum changes are often misunderstood. People wonder whether gums grow back after Invisalign when they notice recession during or after treatment. Again, the answer depends on the mechanism: if the recession is from appliance trauma or excessive tooth movement, that tissue doesn't regenerate without intervention. If it's from inflammatory gum disease that gets better with hygiene, you may see some apparent recovery as swelling resolves.
Similarly, when patients get dental work like veneers and notice their gum line looks different afterward, the question of whether gums grow back after veneers points to the same concept: any true recession around the preparation margin is permanent without grafting, though inflammation-related swelling that resolves can make gums appear to "grow back" when in reality they're just returning to their healthy baseline.
For deeper cleanings like scaling and root planing, the question of whether gums grow back after scaling is especially common because patients often see their gums look much lower after a deep clean. That's usually the swelling going down rather than tissue being removed. The gum wasn't destroyed by the cleaning; it just looks more receded once the inflammatory puffiness resolves. That's an important distinction, and one worth understanding before you worry too much about what you see in the mirror after any periodontal procedure.
The bottom line on osseous surgery specifically: some gum height does come back over months through coronal rebound, but it won't be a full restoration of your pre-disease anatomy. A well-executed osseous procedure with good post-op care should leave you with healthier tissue at a more apical position, stable pockets, and a gum line you can maintain. That is a successful outcome, even if it looks different than what you started with. Focus on whether the tissue is healthy, stable, and manageable, not on whether it's back to where it was before disease changed it.
FAQ
If gums “grow back” after osseous surgery, will my gumline return to the exact pre-surgery height?
Not always. After osseous resective surgery, the gum margin may move coronally, but the amount is limited by how far the flap was placed apically and how much bone support remains under it. If your margin is still moving downward after the first early healing phase, that pattern suggests an issue like inflammation, flap position problems, or inadequate plaque control rather than normal rebound.
How can I tell the difference between normal healing and gum recession that I should worry about?
Yes, sensitivity and tightness can happen without true recession. During remodeling, the gum tissue may feel different because the flap is healing and the surface is reorganizing, even if the margin looks stable. Persistent or worsening sensitivity after you have fully stopped the immediate post-op pain period is a reason to contact your surgeon.
When is the best time to judge the final gum position after osseous surgery?
Follow-up timing matters. Many surgeons reassess tissue position and pocket stability around 3 to 6 months, because that is when most planned coronal rebound should be largely evident. A cosmetic change at 2 to 6 weeks can be misleading, since the gum margin continues shifting afterward.
What if my gums seem to stop moving or look the same after a few months?
Healing can look “stalled” if there is ongoing inflammation or trauma. Common causes include not cleaning the surgical area as instructed, eating hard or sticky foods that irritate the site, or smoking resuming early. If you are maintaining good plaque control and still see no improvement over several months, ask your periodontist whether there is a biologic or mechanical blocker (for example, pocket persistence or unfavorable flap/bone relationship).
Does getting a graft during osseous surgery change whether gums can rebound?
If you also received a graft, ask what type it was and where it was placed. Connective tissue or free gingival grafts can increase tissue thickness and keratinized tissue, which often improves stability. Without grafting, thin or scalloped tissue tends to rebound less and recession risk can be higher, especially on thinner biotypes.
Can brushing help gums grow back after osseous surgery, or can it make things worse?
Possibly, but there are caveats. Over aggressive home pressure with a toothbrush, frequent scrubbing along the margin, or using a hard brush too early can irritate the tissue and slow favorable remodeling. Gentle, technique-specific brushing usually matters more than trying to “treat” the gumline at home by pushing it upward.
Are gumline changes after osseous surgery around teeth different from gum changes after implant surgery?
It depends on the implant procedure. For natural teeth, osseous surgery mainly aims to reshape bone and reposition tissue. For implants, the soft tissue behaves differently and may gradually thin or migrate even with good surgery, so “regrowth” expectations should be lower unless grafting and tissue augmentation were part of the plan.
How does the amount of bone recontouring affect whether the gum margin rebounds?
Yes. If the surgical plan included recontouring bone away from the tooth or implant platform, the tissue has to adapt to that new bone foundation. Less bone support can limit how far coronally the gum margin can migrate, even if healing is otherwise successful.
Which symptoms should prompt an earlier call rather than waiting for the next follow-up?
Contact your clinician sooner if symptoms include pus, foul taste, increasing swelling after it should be settling, or gumline recession that continues to worsen beyond the early remodeling window. These are more concerning for infection or progressive peri-implant disease than for normal coronal rebound.
Do conditions like diabetes or medications affect gum rebound after osseous surgery?
Yes, medication can play a role indirectly. If a patient has uncontrolled diabetes, poor healing can limit stable remodeling. Some medications can also change bleeding or inflammation behavior, which may mask early problems, so tell your surgeon about all meds and changes since surgery.
What specific measurements should I ask my periodontist to track during follow-ups?
Ask for a measurement plan. Request to know the baseline distance between the flap margin and alveolar crest (or the clinical estimate of margin position and bone level), and ask how it will be rechecked over time. That helps you interpret whether your result is tracking toward expected stability.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

