Here is the honest answer: gum tissue does not regenerate the way skin does after a cut. Once the gum has receded, that lost tissue does not simply grow back on its own. But that is not the end of the story. Depending on why your gums receded, you can stop further loss, reduce inflammation that makes recession look worse, and in some cases get meaningful root coverage through professional procedures. Knowing exactly what is and is not possible is the first step to actually fixing the problem.
How to Grow Back Gums: What’s Real, What Helps, Next Steps
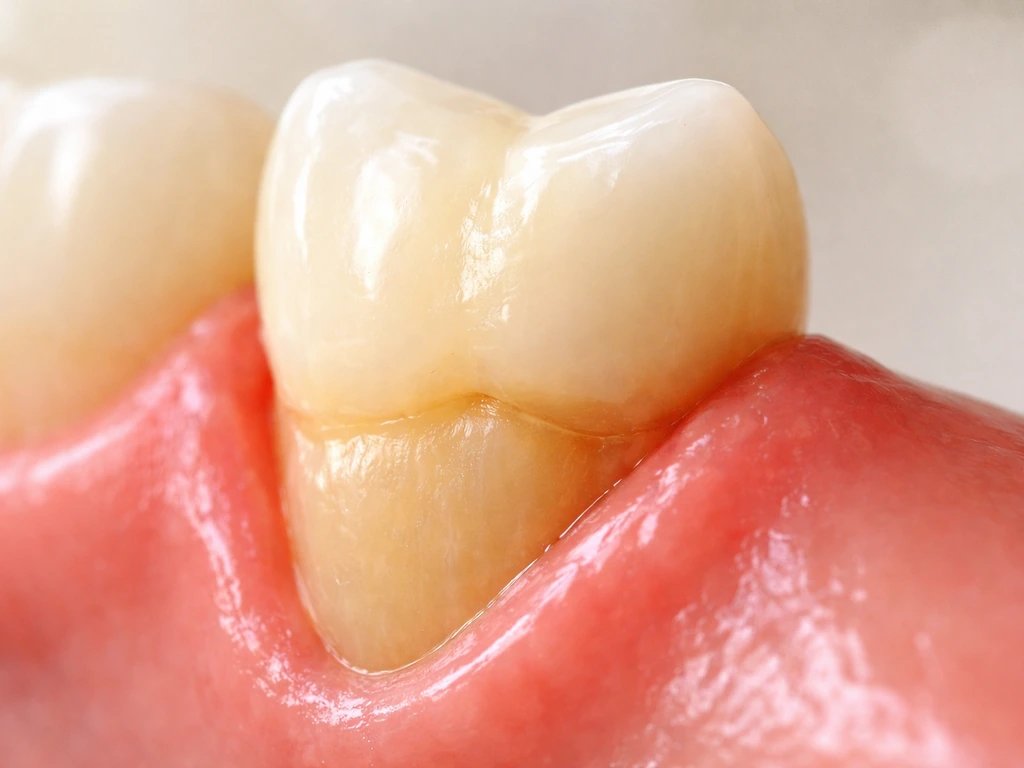
Reality check: can gums truly regrow or is it mostly repair
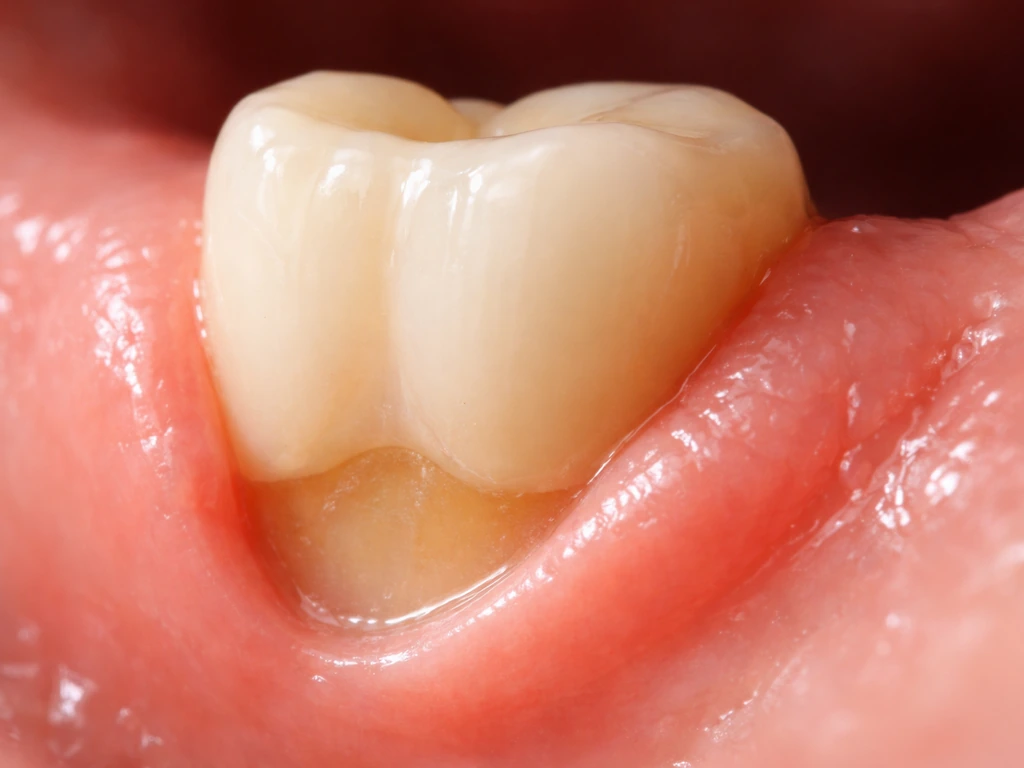
Gum tissue is not like a lizard's tail. The cells that make up your gingiva (the gum tissue around teeth) do not have a built-in instruction set to rebuild lost height after recession has occurred. What can happen, and what most people confuse with 'growing back,' is a reduction in inflammation. When gums are swollen and puffy from gum disease, they can look lower than they actually are in healthy tissue. Treating the disease reduces that swelling and the tissue can look healthier and fuller, but that is inflammation resolution, not regrowth of lost attachment.
True coverage of an exposed root surface requires either preventing further recession or a professional surgical procedure. The good news is that early-stage recession, especially when it is driven by controllable factors like brushing habits or plaque buildup, can often be stabilized very effectively, and surgical options today are genuinely impressive at rebuilding coverage. So while the internet headline 'how to grow back gums naturally' overpromises, there is a real and useful path forward, it just requires being honest about what is in the home-care lane and what needs a periodontist.
Why gums recede and what to identify first
You cannot fix a problem you have not correctly identified. Before trying anything, figure out which category or combination of categories is driving your recession. In one epidemiological study, plaque accumulation (44.1%) and faulty toothbrushing technique (42.7%) were the two most common contributors to gingival recession. That is important because both of those are fixable at home. But recession also comes from periodontal disease, thin gum tissue (a genetic trait), hormonal changes, malocclusion, high frenal attachment, and smoking, each requiring a slightly different approach.
- Periodontal (gum) disease: bacteria under the gumline destroy the attachment between gum and tooth. This is the most serious driver and cannot be reversed by brushing alone.
- Aggressive or incorrect brushing: scrubbing sideways with a medium or hard brush wears gum tissue away mechanically. Technique matters more than brush type.
- Poor plaque control: plaque left at the gumline causes chronic low-grade inflammation that slowly breaks down tissue.
- Smoking and tobacco use: reduces blood flow to gum tissue and masks bleeding, allowing disease to progress silently.
- Thin biotype gum tissue: people with naturally thin gum tissue are more prone to recession, especially during orthodontic treatment.
- Tooth position and malocclusion: teeth pushed outside the arch by braces or natural position put gum tissue under mechanical strain.
- Hormonal changes: pregnancy, menopause, and puberty all affect gum tissue response to plaque.
- High frenal attachment: the soft tissue band connecting lip to gum can pull and cause recession at specific sites.
If you smoke, that deserves a direct mention here. Tobacco use does not just cause recession, it also masks the classic warning signs like bleeding, making you think things are fine when they are not. If you have been wondering if stopping smoking will let your gums grow back, the answer is nuanced: quitting removes a major blocker to healing, but it does not reverse existing structural loss. It does, however, dramatically improve your body's ability to respond to treatment.
What helps gums regrow: evidence-based natural and home supports
Let's be clear about what 'natural' can and cannot do. No home remedy, supplement, or oil creates new gum tissue over an exposed root surface. What natural and home approaches can do is meaningful: reduce inflammation, control the bacteria driving disease, stop further recession, and support your body's healing response when you are also getting professional care. That is not nothing. In fact, it is foundational.
Brushing technique (the biggest lever most people ignore)
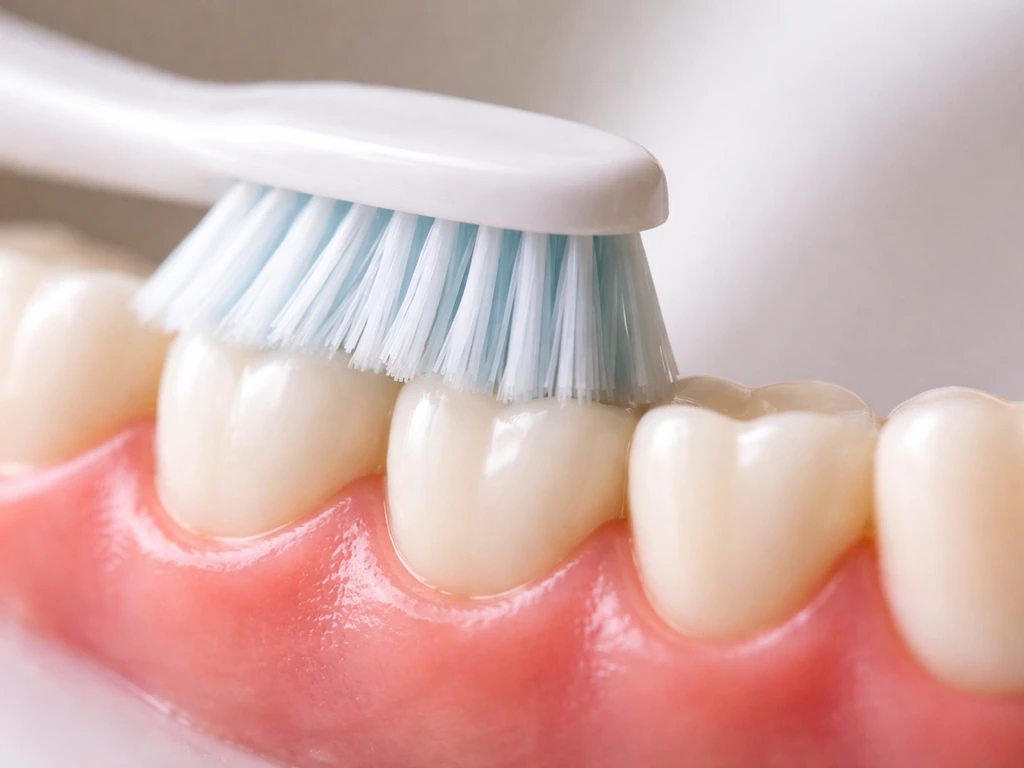
Switch to a soft-bristled brush and use a gentle, small circular or modified Bass technique aimed at a 45-degree angle toward the gumline. Do not scrub. A three-year randomized clinical study found that, when used correctly, neither powered nor manual toothbrushes made pre-existing gingival recession worse, which underscores that technique and consistency are the real variables, not which type of brush you own. If you have been brushing aggressively, correcting that habit alone can stop mechanically driven recession in its tracks.
Flossing and interdental cleaning
Daily interdental cleaning removes plaque from below and between the gumline in areas a brush cannot reach. Use floss, interdental brushes, or a water flosser gently, because improper flossing technique can itself cause localized recession. Wrap floss in a C-shape around each tooth and slide it gently under the gumline, rather than snapping it down repeatedly.
Supplements: vitamin C and what the evidence actually shows

Vitamin C plays a real role in collagen synthesis and gum health. A systematic review found that vitamin C supplementation as an adjunct did not produce clinically significant improvements in pocket depths in periodontitis, but there were some benefit signals for gingival inflammation markers like bleeding. So if you are curious whether vitamin C helps gums grow back, the fair answer is that it supports the tissue environment and may reduce inflammation, but it is not a stand-alone driver of attachment regrowth. Think of it as supportive, not curative.
Oil pulling and coconut oil: what they can and cannot do
Oil pulling has picked up a lot of enthusiasm online as a gum remedy. Randomized controlled trials on oil pulling for plaque-induced gingivitis measured outcomes in plaque and gingivitis indices, not in periodontal attachment regeneration or gum tissue regrowth. The same is true for sesame oil studies that measured plaque and gingival improvements over an eight-week period without measuring tissue-level structural changes. If you want to know more specifically whether oil pulling can grow back gums, the short version is: it may modestly reduce plaque and gingival inflammation as an adjunct to brushing and flossing, but it does not rebuild gum tissue. Similarly, the evidence for coconut oil helping gums grow follows the same pattern: plausible anti-inflammatory and antimicrobial effects at the gingival level, but not tissue regeneration.
Marketed dental products: approach with skepticism
There are various commercial products marketed specifically for gum regrowth or recovery. If you have been looking into whether Dental Pro 7 can grow back gums, apply the same filter: ask whether the evidence supports actual tissue attachment changes, or whether any perceived improvement reflects reduced inflammation and better oral hygiene habits. The biology of gum regrowth means any product claiming to actually regenerate lost gum tissue structurally should be viewed with healthy skepticism unless supported by peer-reviewed clinical outcomes.
Professional options that can regrow or cover exposed root
This is where actual root coverage and something close to true gum rebuilding happens. Professional treatments range from non-surgical deep cleaning to surgical grafting procedures, and the right choice depends on how much recession you have, what caused it, and the health of surrounding tissues.
Scaling and root planing (deep cleaning)
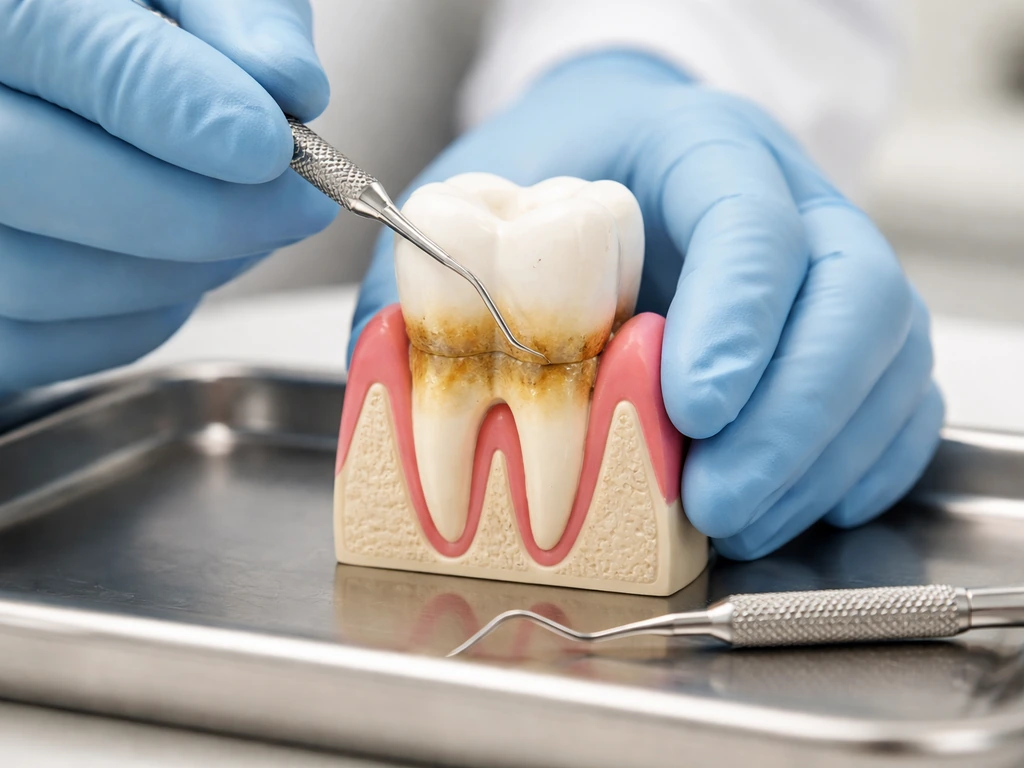
Scaling and root planing (SRP) is the foundational non-surgical treatment for recession driven by periodontal disease. It removes bacterial deposits below the gumline and smooths the root surface so gum tissue can reattach. An RCT found that SRP with chlorhexidine mouthrinse showed significantly less plaque, less bleeding on probing, and greater reductions in pocket depth and attachment level at around 63 days compared to controls. SRP does not rebuild lost gum height, but it controls the disease process that caused the recession, which is a necessary prerequisite for any other treatment to work long-term.
Connective tissue grafts and coronally advanced flap
This is the gold-standard surgical option for root coverage. A subepithelial connective tissue graft (usually taken from the roof of your mouth) is placed under a flap of existing gum tissue that is then moved coronally (toward the crown) to cover the exposed root. A Cochrane review found greater reduction in gingival recession when connective tissue grafts are combined with coronally advanced flaps compared with alternatives. A separate systematic review and meta-analysis confirmed that coronally advanced flap plus connective tissue graft, with or without enamel matrix derivative (EMD), delivers strong root-coverage outcomes. Complete root coverage is achievable in many Miller Class I and II cases.
Laser-assisted periodontal therapy
Laser therapy is increasingly used alongside traditional periodontal treatment. A double-blind split-mouth RCT evaluating Nd:YAG laser-assisted periodontal therapy measured outcomes including gingival recession and clinical attachment level at multiple visits up to around six months. Results support laser as a useful adjunct for managing periodontitis, though it is not a standalone replacement for grafting when structural coverage is the goal.
Guided tissue regeneration and enamel matrix derivative
Guided tissue regeneration uses barrier membranes to encourage the right type of tissue to grow in a specific area. Enamel matrix derivative (EMD), a protein preparation, can be used in combination with surgical flaps to improve the probability of complete root coverage in certain recession classifications. Evidence reviews support CAF with EMD as improving root-coverage probability in single Miller Class I and II recessions relative to flap alone.
Orthodontic considerations
If your recession is tied to tooth position, orthodontic correction can sometimes move teeth back into the arch and reduce the mechanical tension on thin gum tissue. A review on gingival recession specifically noted that orthodontic tooth movement can be associated with recession depending on movement direction and tissue conditions, but it can also sometimes be part of the solution when the tooth is positioned outside the bony arch. This should be assessed by a periodontist and orthodontist together.
| Treatment | What it does | Best for | Realistic outcome |
|---|---|---|---|
| Scaling and root planing | Removes bacterial deposits, controls disease | Recession driven by gum disease | Stops progression, no height regained |
| Connective tissue graft + CAF | Surgically covers exposed root with donor tissue | Moderate to significant recession, Class I/II/III | Significant root coverage, often complete in Class I/II |
| Coronally advanced flap (CAF) alone | Moves existing gum tissue over root | Mild recession with adequate tissue | Partial to complete coverage, less predictable than CTG+CAF |
| CAF + enamel matrix derivative (EMD) | Enhances regeneration potential with proteins | Single recessions, Class I/II | Improved probability of complete root coverage |
| Laser-assisted therapy | Adjunct for periodontitis management | Gum disease component of recession | Improved periodontal parameters; not standalone for coverage |
| Guided tissue regeneration | Barrier membrane guides tissue type | Complex recession with bone involvement | Attachment gain; used with other surgery |
How to make receding gums grow back fast vs realistic timelines
The 'fast' version of this is mostly a myth, and being upfront about that saves you time and money chasing things that will not deliver. Gum tissue heals slowly. After surgical grafting, the initial healing of the wound takes two to four weeks, but final outcomes for root coverage are typically evaluated at six months post-surgery. A practice-based study on deep recession outcomes specifically used a six-month follow-up point to judge surgical results, which is the standard benchmark. Expecting visible coverage results in days or even a few weeks is not realistic for any approach.
On the non-surgical side, reducing inflammation through better oral hygiene can show noticeable improvement in gum appearance (less redness, less swelling, less bleeding) within two to four weeks of consistent behavior change. That is not the same as gum tissue growing back over an exposed root, but it is real, meaningful progress. For professional periodontal therapy, most practices re-evaluate at six to eight weeks after deep cleaning to assess the tissue response before deciding on next steps.
The fastest real route to coverage is surgical grafting performed by a skilled periodontist, combined with excellent ongoing hygiene and periodontal maintenance visits. Even then, you are looking at months, not days. Periodontal maintenance compliance also matters long-term: research shows that patients who regularly attend maintenance visits have significantly better outcomes, including reduced tooth loss, compared to those who skip follow-up care.
Step-by-step at-home plan you can start today
- Switch to a soft-bristled toothbrush immediately. If you are using medium or hard, stop today. Brush twice daily for two minutes using light pressure and a 45-degree angle toward the gumline, moving in small circles or short strokes. Do not scrub.
- Floss or use interdental brushes once daily. Use a gentle C-shape technique, sliding below the gumline on both sides of each tooth without snapping. If your gums bleed consistently after two weeks of gentle flossing, book a dental appointment.
- Rinse with an antimicrobial mouthwash as directed. Chlorhexidine (prescription strength) has the strongest evidence for plaque and gingivitis reduction, but over-the-counter antiseptic rinses used consistently also help reduce bacterial load. Do not use alcohol-based rinses if your gums are already irritated.
- Assess and stop any abrasive habits. This includes whitening toothpastes used daily (high abrasive index can wear gum tissue), teeth grinding without a night guard, chewing on hard objects, and using toothpicks aggressively.
- Quit smoking or tobacco use. This is not optional if you are serious about improving gum health. Smoking impairs blood flow and immune response in gum tissue, and no home remedy or surgery works as well in an active smoker.
- Eat to support gum tissue. Foods rich in vitamin C (citrus, bell peppers, broccoli) support collagen production in gum tissue. Vitamin C supplements may help reduce gingival inflammation as an adjunct, though they are not a standalone fix for recession.
- Stay hydrated and manage dry mouth. Saliva is protective. Medications and mouth breathing can cause dry mouth, which increases bacteria at the gumline. If this applies to you, ask your dentist or pharmacist about saliva substitutes.
- Track your recession with photos. Take consistent photos of affected areas monthly to monitor whether things are stable, improving, or getting worse. This also helps your dentist see changes over time.
When to see a dentist or periodontist and warning signs
Some situations are beyond home care and need professional eyes urgently. Do not wait if you notice any of the following. Gum recession that is visibly worsening week to week, bleeding that does not improve after two weeks of good oral hygiene, pain at the gumline or when touching the tooth root, increased tooth sensitivity to temperature or pressure, loose teeth or teeth that feel like they are shifting, or deep pockets (if you have been told your pocket depths are 5 mm or more). These are signs that active periodontal disease may be progressing, and the window for non-surgical management may be closing.
If you have not seen a dentist or periodontist in the last six months and you have visible recession, that is your cue. A periodontist specifically focuses on the structures supporting teeth, including gum tissue and bone, and is the right specialist to evaluate whether you need deep cleaning, surgery, or monitoring. General dentists can handle early-stage gingivitis and mild recession, but once there are multiple sites of recession, pocket depths over 4 mm, or bone loss visible on X-rays, a periodontist referral is appropriate.
The bottom line is straightforward. You cannot regrow gum tissue at home the way headlines promise. But you can stop things from getting worse, create the best possible environment for healing, and work with a periodontist to get real root coverage through surgical procedures that have solid clinical evidence behind them. Start with the at-home habits today, get a professional evaluation if you have not already, and set realistic expectations: improvement is absolutely achievable, it just takes the right approach and enough time to work.
FAQ
If my gums look like they are “coming back,” how do I tell the difference between true root coverage and just less swelling?
If you truly have exposed root, the only way to get new coverage of that root surface is to stop further recession and, in many cases, use procedures that reposition or regenerate tissue at the gumline. What you can do at home is reduce inflammation and plaque and prevent additional tissue loss, which can make the area look healthier even if the root is not being newly covered yet.
Can my brushing or flossing technique cause gum recession even if I don’t have gum disease? What’s the most common way people mess this up?
Yes, it can. If you brush too hard, use a straight up-and-down scrubbing motion, or aggressively floss in the same spot, you can worsen localized recession even when your underlying disease is controlled. A quick check is whether recession is clustered around specific tooth surfaces that you reliably irritate with technique, then adjust brushing to gentle, targeted motions and floss in a C-shape without snapping.
I don’t bleed when I brush, and I smoke. Does that mean my recession is not serious?
Do not rely on pain or bleeding as your only guide. Smoking can reduce bleeding and make early disease look “quiet,” while still impairing healing and treatment response. If you smoke or vape nicotine, quitting improves your odds of stabilization and surgical success, but it does not restore lost tissue by itself.
At what point should I stop trying home fixes and assume I likely need periodontal treatment?
If you have deep pockets (often 5 mm or more) or recession that is clearly progressing, you should assume the cause is periodontal disease until evaluated. In those situations, “cosmetic-only” approaches are less likely to work because the root surface and surrounding tissues need disease control first, typically through scaling and root planing and then reassessment at a few weeks.
Should I take vitamin C or other supplements to regrow gums, and how do I avoid wasting money?
Be cautious about supplements. Vitamin C might support the tissue environment, but it is not a substitute for removing plaque, controlling inflammation, and treating periodontal disease. If you want to use supplements, do it as an adjunct and discuss dosing with your clinician, especially if you have kidney disease or take blood thinners.
How long should I expect to see results, and when is it reasonable to evaluate whether a treatment worked?
Hairline improvements in redness or swelling within 2 to 4 weeks can happen from better hygiene, but final assessment of root coverage after surgery is typically around 6 months. If you are offered a “fast” claim or want to judge success in days, that is usually unrealistic for structural change.
Can orthodontics fix recession, or could braces make it worse? How is that decision made?
Not exactly. Ortho can help when recession is related to tooth position or thin tissue being pulled into a vulnerable alignment, but it can also worsen recession if the tooth is moved in a way that increases tension or pushes the root toward thinner bone. The safest approach is coordinated planning by a periodontist and orthodontist using gum thickness and bony contour information.
What red flags mean I should not try “natural” approaches first?
If you have recession plus tooth sensitivity, pain, or a visible change that is worsening week to week, or you have loose or shifting teeth, you should seek professional assessment rather than starting multiple home remedies. Those symptoms can indicate active disease, compromised support, or surface/root issues that need examination and targeted treatment.
Once my recession is treated, how do I prevent it from coming back?
Maintenance matters even after successful treatment. Many people feel better and stop follow-up, but consistent periodontal maintenance visits are what help preserve attachment and reduce the chance of recurrence. Plan maintenance based on your clinician’s risk assessment, not on when your gums look fine.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

