Yes, wisdom teeth can absolutely start coming in at 16. It's on the early side of the typical range, but it's not unusual at all. Some people notice their first signs of third molar activity in their mid-teens, while others don't experience anything until their early twenties or even later. If you or your teenager is feeling pressure, soreness, or swelling at the very back of the mouth at 16, those third molars are a completely reasonable explanation.
Can Wisdom Teeth Grow at 16? Eruption Timeline and Next Steps
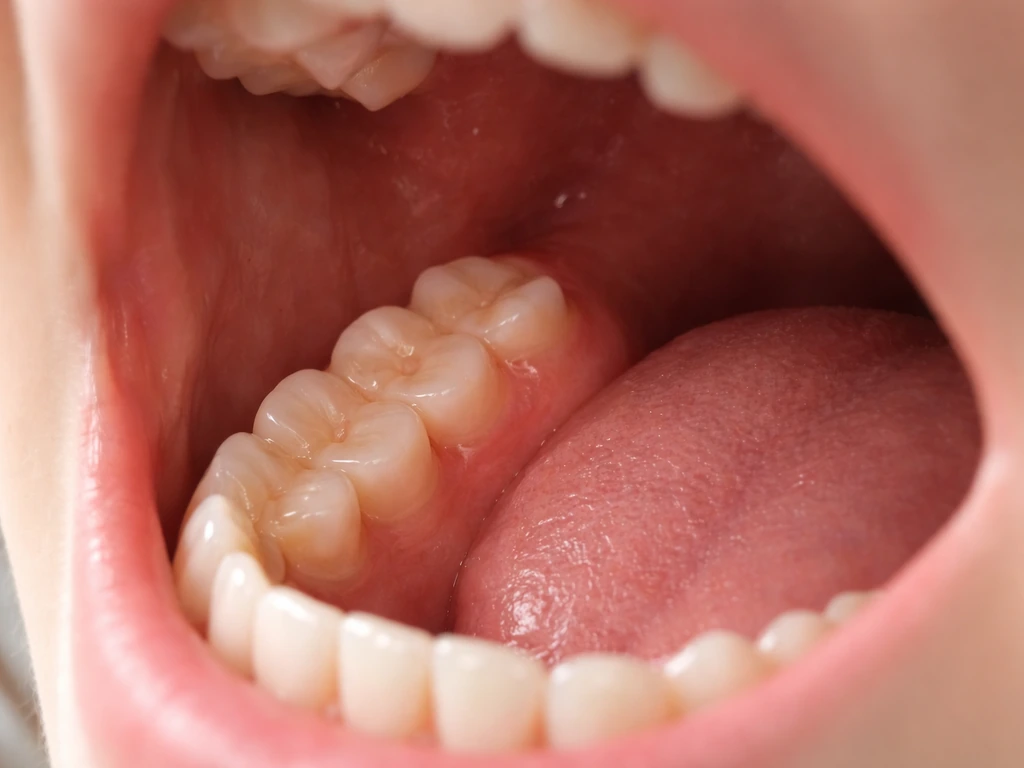
What 'grow' actually means here: eruption vs. regrowth
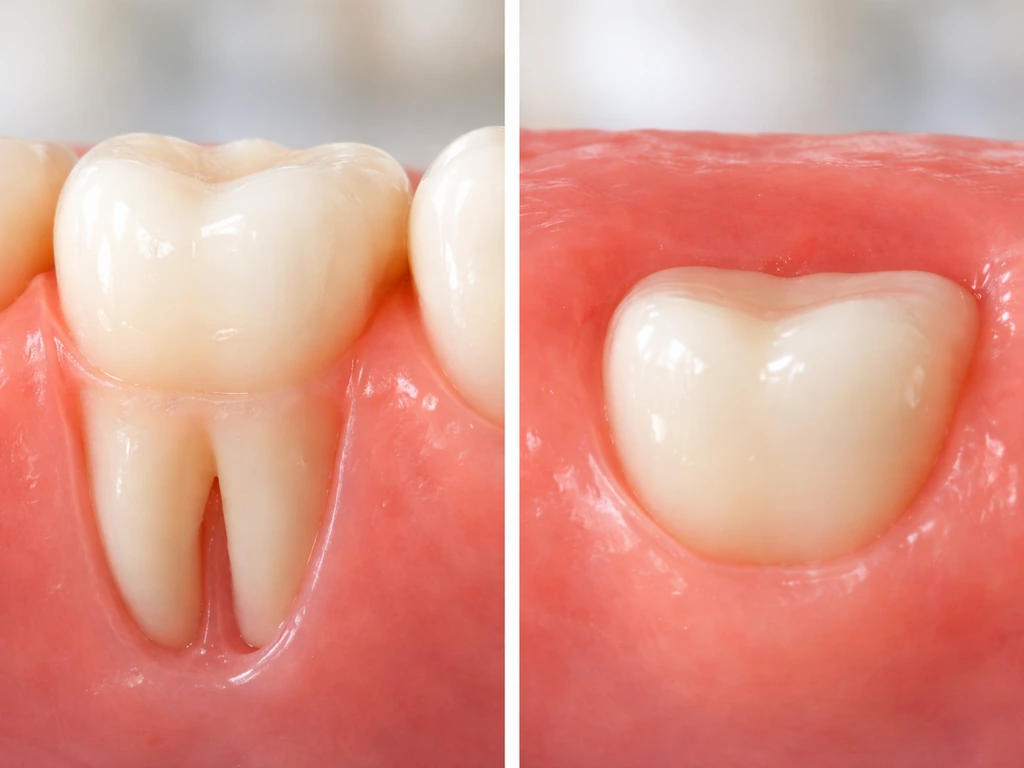
Before going further, it's worth clearing up a common point of confusion. When people ask whether wisdom teeth can 'grow' at 16, they usually mean eruption, which is the process of a tooth that already exists inside your jaw pushing up through the gum and becoming visible. That's very different from true tooth regrowth, which would mean a brand new tooth forming from scratch. Humans cannot regrow teeth. Once a wisdom tooth is removed, it does not grow back. Full stop.
Your wisdom teeth (third molars) have been developing inside your jaw since childhood. Crown formation is typically complete by around age 12, with root development continuing through the mid to late teens. If you're asking specifically about wisdom teeth at 12, the key idea is that age 12 is usually too early for true eruption, though development inside the jaw can be underway. Eruption, where the tooth physically pushes through the gum, comes later. So at 16, the tooth itself isn't 'growing' in the way a seed sprouts. It's been there all along, and it's now making its move toward the surface. That distinction matters because it means no supplement, no food, and no home remedy can make a wisdom tooth 'grow' if it isn't already there developmentally.
Where age 16 fits in the normal eruption timeline
The standard range cited by most dental sources is 17 to 25 years for wisdom tooth eruption. MedlinePlus narrows it to 17 to 21, and the Cleveland Clinic similarly puts it in the 17 to 25 window. So technically, 16 is just before the most common range. But research using panoramic X-rays has found that the alveolar emergence (the point where the tooth starts breaking through bone) can begin as early as 14.6 to 16.2 years in females and 15.1 to 18.3 years in males. In practical terms, the biology backs up what many dentists see clinically: some 16-year-olds are genuinely starting to erupt their third molars, particularly girls.
A helpful way to think about it is in stages. By ages 15 to 16, the roots of wisdom teeth are typically about one-third of their final length. By 17 to 18, roots are approaching two-thirds and the crown begins its push toward the gum. Full root formation usually completes around 19 to 20. So at 16, you're right at the edge of when early eruption activity can realistically begin, especially if development has been running a bit ahead of schedule.
For context, this is part of a broader pattern of variation in the teen years. Questions about whether wisdom teeth can erupt at 13, 14, or 15 reflect the same biological reality: there's a range, genetics plays a big role, and individual timelines vary considerably. For some teens, that same variation can mean wisdom tooth eruption at 13, even though it is earlier than the typical range wisdom teeth erupt at 13. If you're wondering can wisdom teeth grow at 14, the answer follows the same idea: eruption timing varies widely, and genetics plays a big role wisdom teeth can erupt at 14. At 16, the odds of genuine eruption activity are meaningfully higher than at younger ages.
Signs that wisdom teeth might be coming in at 16
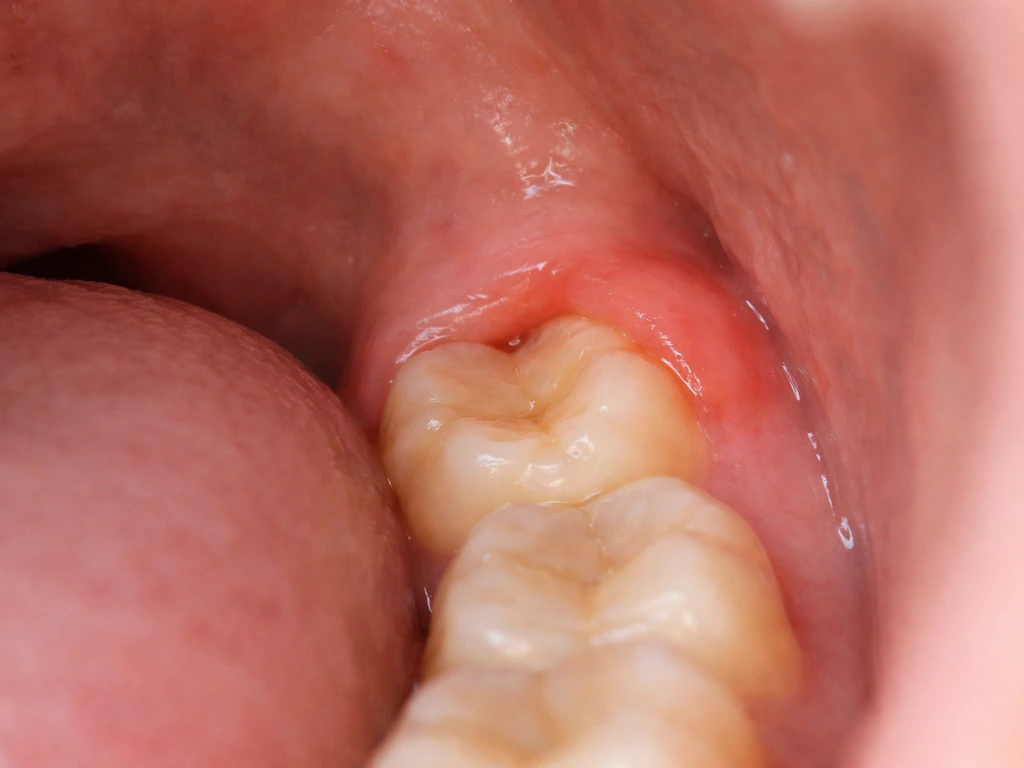
The symptoms of early wisdom tooth eruption can be subtle or pretty hard to ignore. Some people feel a general achiness at the very back of the jaw. Others notice a specific pressure or soreness behind the last molar. The gum tissue in that area may look slightly swollen, or feel tender when touched. Occasionally, a small bump or flap of gum tissue becomes visible as the tooth starts pushing through.
One condition worth knowing about is pericoronitis, which is inflammation of the gum tissue around a partially erupted or erupting wisdom tooth. A flap of gum tissue (called an operculum) can form over the emerging tooth, trapping food and bacteria underneath. Symptoms of pericoronitis can range from mild, like a dull ache near the back teeth and bad breath or a bad taste in the mouth, to more severe, like facial swelling, pus, and significant pain that makes it hard to open your mouth comfortably. If any of the more serious symptoms appear, that's not a 'wait and see' situation. Get to a dentist promptly.
- Dull aching or pressure deep behind the last molar
- Swollen, red, or tender gum tissue at the very back of the mouth
- A visible bump or ridge of gum starting to show
- Mild jaw stiffness or discomfort when chewing
- Bad breath or an unusual taste not explained by other causes
- Headache or earache on the same side as the back-tooth discomfort
- In more serious cases: visible swelling of the face, pus, or difficulty opening the mouth
How a dentist evaluates wisdom teeth at 16
If you bring a 16-year-old in with back-of-mouth symptoms, a dentist's evaluation is pretty straightforward. First, there's a clinical exam: the dentist looks directly at the gum tissue, checks for swelling, probes for tenderness, and asks about symptoms like pain, stiffness, and timing. That clinical picture tells them a lot, but it doesn't tell the whole story.
The key diagnostic tool is X-rays. A panoramic X-ray (one that captures the entire jaw in a single image) is typically the starting point. It lets the dentist assess how many wisdom teeth are present, where they're positioned, what angle they're sitting at, how developed the roots are, and whether there's enough space for them to erupt normally. From there, if impaction is suspected or more detail is needed, additional imaging like cone-beam CT (CBCT) may be recommended, especially if surgical removal is being considered. The panoramic X-ray gives a good overview; the more detailed imaging helps plan next steps.
At 16, a dentist may also be watching orthodontic concerns in parallel. If braces have been involved, or the jaw is still actively developing, wisdom tooth position becomes part of the bigger picture. Don't be surprised if the dentist coordinates with an orthodontist or refers to an oral and maxillofacial surgeon for a specialist opinion.
What impaction means and why it matters
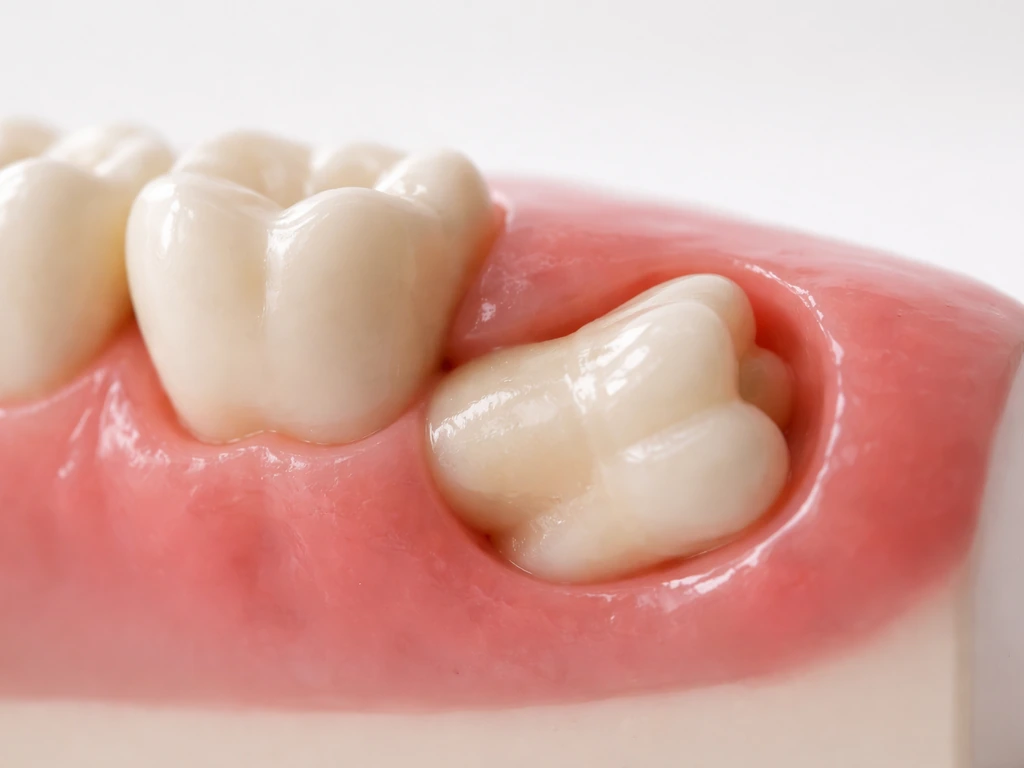
Not every wisdom tooth that starts to move makes it out cleanly. Many wisdom teeth become impacted, meaning they get stuck, either fully under the gum and bone or only partially erupted. This happens because the jaw doesn't always have enough room, or because the tooth is angled in a direction that blocks its path. Cleveland Clinic notes that impaction is common: plenty of people have wisdom teeth that stay trapped under gum or jaw tissue indefinitely.
Impacted teeth aren't always painful right away, but they carry real risks over time. The list includes pericoronitis (that gum inflammation discussed above), decay in the neighboring second molar because the tight space is impossible to clean properly, periodontal disease around the back of the mouth, cyst formation around the impacted tooth, and in rarer cases, damage to the jawbone or nearby nerve structures. Research has documented that the inferior alveolar nerve (the main nerve running through the lower jaw) can sit quite close to lower impacted wisdom teeth, which is one reason extraction at this level requires careful imaging and planning.
The severity and pattern of symptoms matter a lot when deciding whether to act. A single mild episode of discomfort might warrant monitoring. Repeated episodes of pericoronitis, signs of decay in neighboring teeth, or a developing cyst shift the calculus firmly toward intervention. Guidelines from organizations like NICE and the AAOMS are consistent on this: removal is indicated when there's evidence of pathology or disease, not just because a wisdom tooth exists.
What to actually do next
Right now, at home
If the discomfort is mild, a few things help in the short term. Rinsing with warm salt water can reduce gum inflammation and flush debris from around a partially erupted tooth. Over-the-counter pain relievers like ibuprofen (if appropriate for the person's age and health) can take the edge off. Avoid pressing on the area or trying to dislodge anything yourself. Keeping the area as clean as possible, using a soft-bristled toothbrush carefully extended to the back of the mouth, reduces the chance of bacteria accumulating under a gum flap. These are bridge measures, not solutions. They buy time and comfort while you get proper evaluation.
Watch and wait, or plan for extraction?
This is the core decision, and the honest answer is: it depends on what the X-rays show and what symptoms are present. If wisdom teeth at 16 are developing normally, aren't causing any problems, appear to have adequate space, and are in a clean, maintainable position, watchful waiting with periodic X-rays is a perfectly reasonable approach. The AAOMS is clear that wisdom teeth don't need to come out just because they exist. If they're functional, pain-free, cavity-free, and in a position you can actually keep clean, monitoring is appropriate.
On the other hand, if X-rays show impaction, a bad angle, insufficient space, early signs of damage to neighboring teeth, or if symptoms are recurring and significant, an extraction consultation makes sense. Many oral surgeons will see a 16-year-old for this evaluation. Some prefer to wait until the roots are more developed before operating; others may recommend proactive removal before complications develop, particularly if the positioning is clearly problematic. There's no single universal answer, and the Cochrane evidence base actually reflects genuine uncertainty about prophylactic removal of truly asymptomatic, disease-free impacted wisdom teeth. Your specific case matters more than a blanket rule.
The next concrete steps
- Schedule a dental appointment and specifically mention back-of-mouth pain or pressure, so the dentist knows to prioritize a wisdom tooth assessment.
- Ask for a panoramic X-ray if one hasn't been taken in the last year or two. At 16, this gives a current snapshot of exactly where those third molars sit.
- Get a clear picture of what the X-rays show: are the teeth impacted, angled, or positioned normally? Is there adequate space?
- If impaction or significant risk is identified, ask for a referral to an oral and maxillofacial surgeon for a specialist consultation.
- If everything looks manageable for now, establish a monitoring plan with periodic X-rays (typically annually) to track any changes.
- Don't skip cleanings. The back of the mouth near partially erupted wisdom teeth is a high-risk zone for decay and gum disease, and professional cleaning is part of keeping things stable.
The bottom line is that wisdom teeth coming in at 16 is biologically plausible and not something to panic about, but it's also not something to ignore. Get eyes (and imaging) on the situation now, understand what's actually happening in that jaw, and then make decisions based on real data rather than guessing. That's the most useful thing you can do today.
FAQ
If my 16-year-old has no pain, should we still get checked for wisdom teeth?
It can happen at 16, but “silent eruption” is common, meaning symptoms may be minimal at first. If there is no pain, no gum flap irritation, and no cavities or gum inflammation on exams, dentists often monitor rather than rush to remove teeth. A panoramic X-ray is typically the first step to confirm position and whether there is space for normal eruption.
How can we tell if symptoms at the back are truly from wisdom teeth?
Sometimes the discomfort is not from wisdom teeth at all, common lookalikes include a molar cavity, gum infection around the second molar, teething of the first permanent molars (less likely at 16), jaw joint soreness, or sinus-related facial pressure. Because the back of the mouth overlaps with several causes, dentists use an exam and X-rays to avoid treating the wrong problem.
Can supplements or special foods make wisdom teeth erupt faster at 16?
Home remedies cannot make a tooth that is still deep in bone erupt. What you can do is manage secondary inflammation if a gum flap is irritated, salt-water rinses can help flush trapped debris, and keeping the area clean reduces bacterial buildup. If pain is escalating, swelling occurs, or there is bad taste or pus, you should be seen urgently.
When should we stop waiting and seek urgent care for possible pericoronitis?
If there is swelling, fever, pus, trouble swallowing, rapidly worsening pain, or difficulty opening the mouth, those are red flags for more significant infection. In those cases, do not wait for a routine appointment, contact a dentist or urgent care promptly to assess for conditions like pericoronitis and determine whether antibiotics or urgent treatment is needed.
Does being in braces affect whether wisdom teeth at 16 should be extracted or monitored?
Braces can change the story, because wisdom tooth space and angulation interact with orthodontic tooth movement and jaw growth timing. Even if orthodontic treatment is ongoing, most dentists coordinate the wisdom tooth plan with the orthodontist and decide timing based on X-ray findings and how the eruption could affect neighboring teeth or crowding.
What specific X-ray findings usually change the decision from monitoring to extraction?
A dentist generally looks for how much of the tooth is erupted, whether it is angled, the amount of surrounding bone and space, and signs of harm to the second molar or nearby gum tissue. If the wisdom tooth is mostly still inside the jaw but close to a nerve pathway in the lower jaw, the discussion often includes whether to wait for more root development or plan careful surgical timing.
What if a wisdom tooth is only half out at 16, does that always mean it will come in fully?
Sometimes, what looks like “partial eruption” can actually be a gum flap over an impacted tooth, which is where food and bacteria get trapped. Even if the tooth does not fully come out, the gum issue can still recur. The management may involve observation, improved cleaning strategies, or extraction depending on repeated inflammation or evidence of damage.
Is it normal for symptoms to come and go, or does recurrence mean extraction is more likely?
If symptoms keep returning, monitoring still might be reasonable, but the pattern matters. Recurrent pericoronitis episodes, recurring bad breath or taste, new decay on the neighboring second molar, or gum pocketing near the back teeth typically pushes clinicians toward intervention rather than indefinite watchful waiting.
If we choose watchful waiting at 16, how often should we follow up?
For many people, waiting is done with periodic imaging and oral exams, but the interval should be individualized. If a tooth is early erupting at 16, the next check may be scheduled sooner than for a tooth that is clearly fully impacted and symptom-free. Ask the dentist what “watch period” they recommend and what symptoms should trigger an earlier visit.
Can wisdom teeth erupt at 14? Learn eruption vs development, signs, timelines, and when to see a dentist.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Learn why humans don’t grow back adult teeth, what natural healing can do, and today’s options like implants and bridges

