The mandible grows through a combination of endochondral ossification at the condyles (the rounded knobs that connect your lower jaw to your skull) and intramembranous bone remodeling along the body and ramus of the jaw. In plain terms: specialized cartilage at the back of your lower jaw gets replaced by bone, while osteoblasts and osteoclasts continuously add and remove bone tissue along the jaw's surface to reshape it. This process starts before birth and continues actively through your late teens, with a major acceleration during puberty. After that, fine-scale remodeling continues into adulthood, but the dramatic size changes are done.
How Does the Mandible Grow and Affect Tooth Development
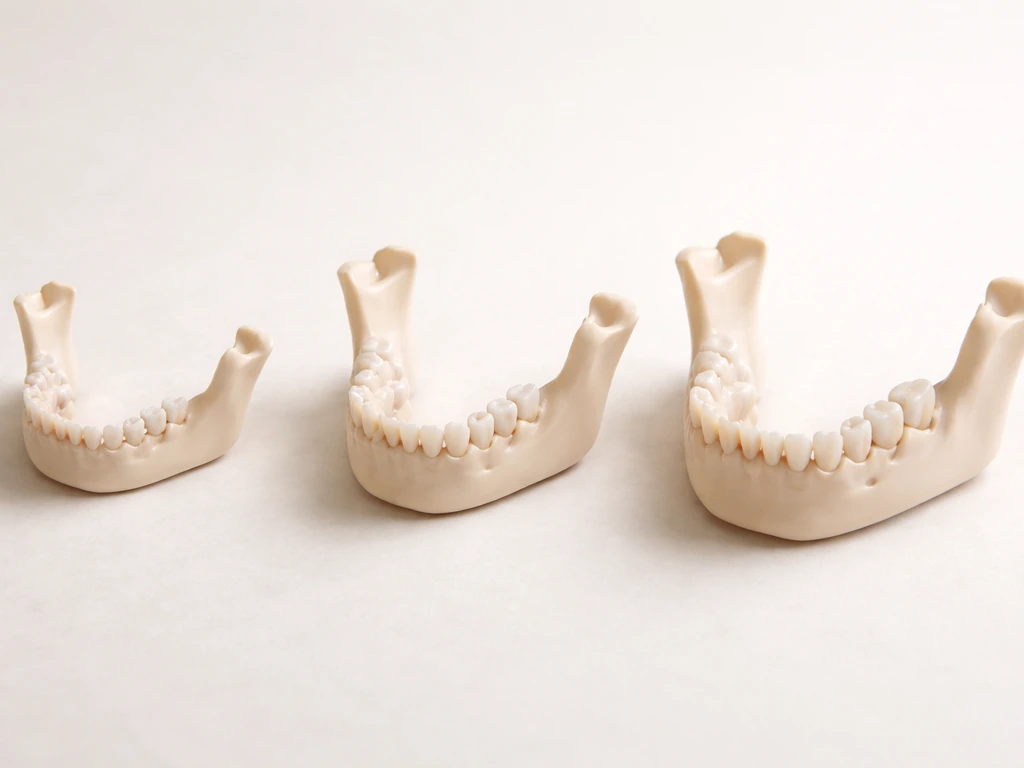
Mandible growth basics: what changes and when
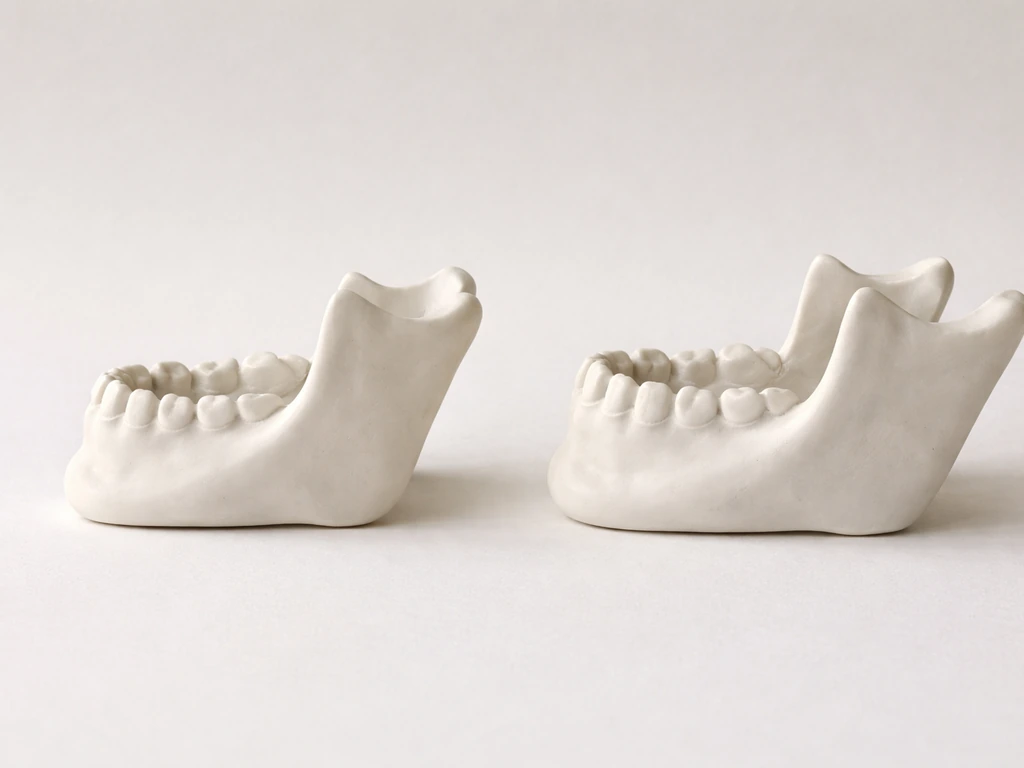
From infancy through early childhood, the mandible changes fast. Longitudinal research tracking babies from birth to age five found that total mandibular length shows the greatest growth changes of any jaw dimension, followed by ramus height (the vertical part of the jaw) and corpus length (the horizontal part you feel when you touch your chin). Put simply, the jaw is getting both longer and taller at the same time during those early years.
Growth then continues more gradually through middle childhood, setting the stage for the pubescent push. During adolescence, mandibular growth accelerates in a pattern called the pubertal growth spurt. Critically, this spurt is tied to pubertal stage, not just calendar age. Girls typically hit peak mandibular growth velocity earlier than boys, while boys experience a longer, more intense growth period that produces greater overall jaw size. By the late teens (often 17 to 19 in females, sometimes into the early 20s in males), active condylar growth winds down and the jaw approaches its final adult dimensions.
One thing that surprises a lot of people: even after your jaw stops visibly growing, it never completely stops changing. Bone remodeling continues throughout your life for maintenance and repair. The shape of the mandible can shift subtly in your 30s, 40s, and beyond, especially along the lower border. But this is slow surface-level adaptation, not the kind of growth that adds jaw length or height the way puberty does.
The main growth mechanisms driving jaw size changes
Condylar cartilage: the engine of mandibular growth
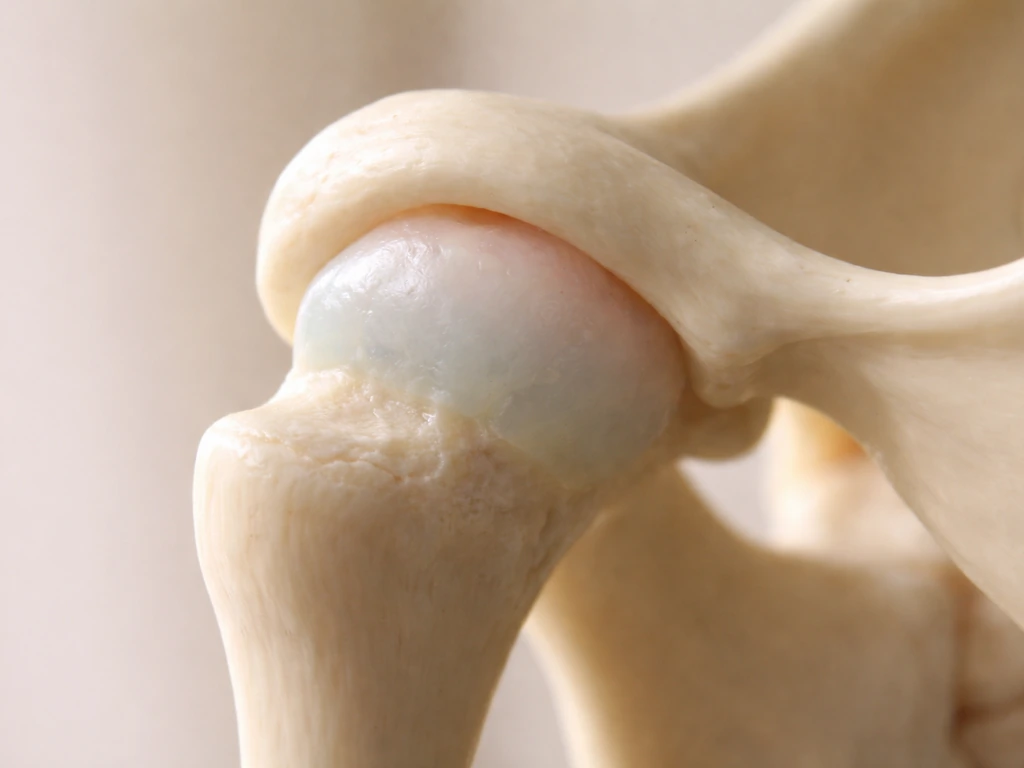
The condylar cartilage is the most important growth site in the lower jaw. The mandibular condyle is classified as a secondary cartilage, meaning it has different biological characteristics than the growth plates in your long bones, but it works on the same general principle: cartilage cells proliferate and then get replaced by bone tissue through endochondral ossification. This is what lengthens and repositions the jaw over time. The condyle is also mechanosensitive, meaning it responds to mechanical loading. Research on the condyle shows that physical forces acting on the jaw can influence local growth factor expression and metabolic activity in the cartilage. That is part of why functional jaw habits (like how you bite, chew, or whether you breathe through your mouth) can subtly affect the direction and amount of jaw growth.
Bone remodeling along the body and ramus
Away from the condyle, the jaw grows and reshapes through intramembranous ossification and surface remodeling. Osteoblasts deposit new bone on the outer surface of the jaw while osteoclasts resorb bone on inner surfaces. This coupled process reshapes the entire mandible as it grows, adjusting the angle, thickness, and contours of the jaw body. Even mature bone undergoes this cycle to repair microdamage and maintain structural integrity. What it cannot do is regenerate a jaw that stopped growing decades ago back to a new growth phase.
What controls how the jaw grows: genetics, hormones, nutrition, and habits
Genetics sets the blueprint for your jaw's size and shape. But that blueprint gets modified significantly by biological signals and environmental inputs during the growth window.
- Hormones: Growth hormone (GH) and insulin-like growth factor 1 (IGF-1) are the primary drivers of skeletal growth, including the mandible. Sex steroids (estrogen and testosterone) regulate the timing and intensity of the pubertal spurt, with estrogen eventually signaling the growth plates to close. Children with growth hormone deficiency show measurable craniofacial differences, and GH therapy can influence jaw development when started early enough.
- Nutrition: Adequate protein, calcium, vitamin D, and overall caloric intake are necessary for bone formation. Chronic malnutrition during childhood can blunt jaw growth, just as it stunts overall skeletal growth.
- Mechanical loading and habits: Chewing forces stimulate condylar cartilage activity. Mouth breathing is associated with a more vertical, downward-rotated jaw growth pattern (sometimes called a clockwise rotation), which can affect facial proportions and bite relationships. This is a functional influence, not a genetic one, but it is real.
- Sleep and overall health: Growth hormone is primarily secreted during deep sleep, so chronic sleep disruption in children can theoretically affect skeletal growth rates.
The key takeaway is that while you cannot choose your genetic jaw template, the growth process that fills in that template is genuinely responsive to biological and environmental factors, especially during childhood and early adolescence. That is the window where intervention matters most.
How jaw growth connects to tooth eruption, spacing, and wisdom teeth
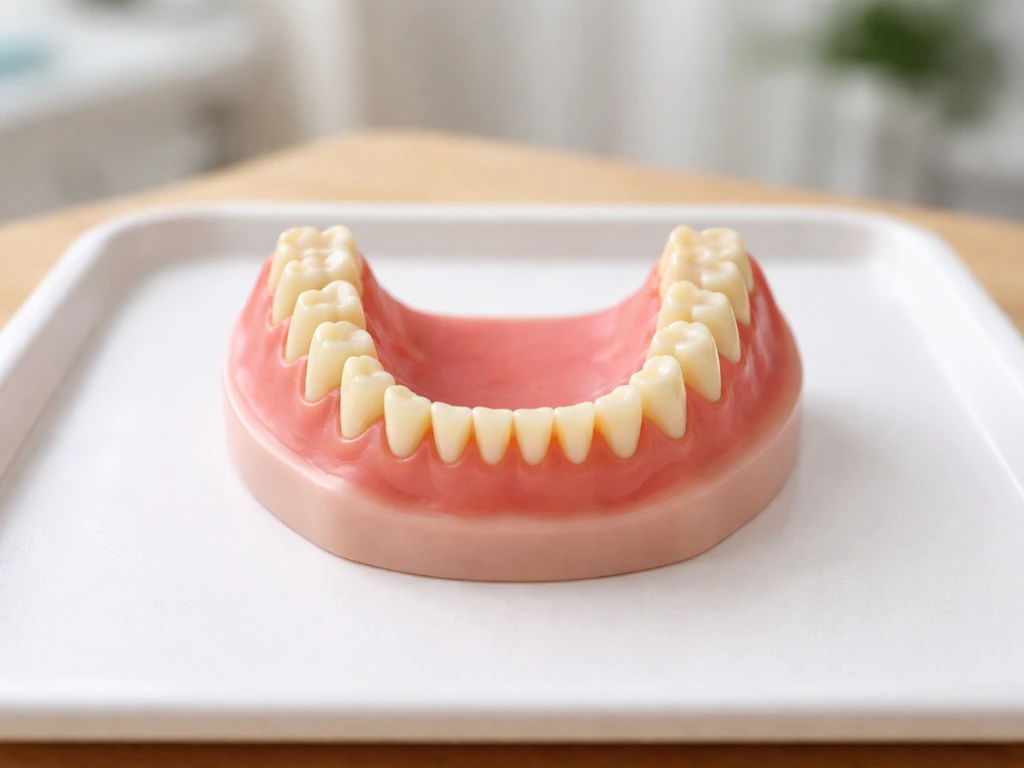
Jaw growth and tooth eruption are deeply linked. As the mandible lengthens and the alveolar bone (the tooth-bearing ridge) develops, it creates the physical space that teeth erupt into. When jaw growth keeps pace with dental development, teeth tend to align reasonably well. When the jaw falls short, you get crowding, tipping, and impaction.
The most familiar example of this mismatch is wisdom teeth. Mandibular third molars typically begin attempting to erupt between ages 17 and 25. Whether they come in cleanly depends heavily on how much space remains at the back of the jaw after the other molars have erupted. Research using panoramic radiographs confirms that complete wisdom tooth eruption (what researchers call stage D) rarely occurs before age 17. The exact timing varies by individual growth rates, jaw morphology, and jaw length. When there is not enough room, impaction results, and this is extremely common because the modern human mandible frequently does not grow long enough to accommodate all four third molars.
The connection between jaw length and molar eruption also applies to the permanent molars that come in earlier. Molars grow in at specific developmental windows, and the jaw needs to be at the right stage of development to receive them properly. When molar teeth grow in, the timing of jaw growth needs to keep pace to reduce the risk of crowding and misalignment. Your molars grow in during childhood and early adolescence, but the exact age varies by tooth and individual development Molars grow in at specific developmental windows. When jaw growth is slow or the timing is off, early crowding signals can appear well before wisdom teeth are even a concern.
When jaw growth goes off track: signs to watch for
Abnormal mandibular growth typically shows up as a mismatch between the upper and lower jaws, leading to bite problems called malocclusions. Orthodontists classify these using measurements taken from skull X-rays (cephalometric analysis), including angles like SNB (which measures the lower jaw's position relative to the skull base, with a reference value around 80 degrees in adults, and values around 72 degrees or lower suggesting a retruded lower jaw) and ANB (the angle difference between upper and lower jaw positions).
Common presentations of mandibular growth problems include:
- Class II malocclusion: Upper teeth significantly overlap the lower, often because the lower jaw is underdeveloped or retruded. This creates the 'overbite' appearance many people associate with needing braces.
- Class III malocclusion: Lower teeth sit in front of upper teeth, often because the lower jaw has grown excessively or the upper jaw is underdeveloped.
- Crowding: Teeth overlap or twist because there is not enough jaw length to accommodate them.
- Open bite: Upper and lower front teeth do not touch when the back teeth are together, sometimes related to vertical jaw growth patterns or habits like thumb-sucking.
- Asymmetry: One side of the jaw grows more than the other, which can result from differences in condylar activity or early trauma.
Parents often notice these patterns when children start losing baby teeth and the permanent teeth come in crowded or at odd angles. An early evaluation, usually recommended around age 7 by most orthodontic guidelines, can catch growth discrepancies while there is still active growth to work with.
Can the mandible or teeth actually 'grow back'? Realistic limits explained
Here is where it is important to be direct and honest, especially on a site that spends a lot of time busting dental regeneration myths. The mandible does not regenerate in the way that, say, a lizard regenerates a tail. Once active growth ends (typically by the late teens for most people), the jaw will not spontaneously resume growing to fix a deficiency. That is also why do molars fall out and grow back is usually the wrong expectation: most adult molars do not fall out and then regrow Once active growth ends (typically by the late teens for most people). Similarly, tooth enamel cannot regenerate itself once teeth have erupted because the cells that form enamel (ameloblasts) are lost at eruption and never return. These are hard biological limits.
That said, there is a meaningful distinction between natural regeneration (which is not happening in an adult jaw) and treatment-supported change, which is very real and works with the biology that still exists.
| What you're asking about | Can it 'grow back' naturally? | What actually can be done |
|---|---|---|
| Mandible length in a growing child | Yes, within the normal growth window | Functional appliances, jaw expanders, orthopedic devices during active growth |
| Mandible length in an adult | No, condylar growth is complete | Orthognathic (jaw) surgery to reposition bone; orthodontics to compensate |
| Alveolar bone around teeth | Limited self-repair only | Bone grafting, guided regeneration procedures prior to implants |
| Tooth enamel | No, enamel-forming cells are gone after eruption | Remineralization for early lesions; fillings, crowns, or veneers for structural loss |
| Impacted wisdom teeth erupting on their own | Possible if space develops, but often does not | Monitoring, surgical exposure, or extraction depending on angulation and space |
Orthodontic tooth movement is also worth understanding here. Braces and aligners do not make the jaw grow back, but they use the fact that living bone continuously remodels to move teeth through bone. Pressure on one side of a tooth root causes resorption; tension on the other side causes new bone formation. The periodontal ligament (the tissue connecting root to bone) is the key player in this process. It is a clever use of existing biology, but it is fundamentally different from regeneration.
What to do next: age-based guidance and when to get evaluated
Where you are in the growth timeline determines what your realistic options are. Here is practical guidance by life stage:
Children ages 6 to 10
This is when mixed dentition (baby teeth alongside incoming permanent teeth) creates your first clear look at how the jaw and teeth are coordinating. If you notice significant crowding, a noticeable overbite or underbite, or a child who consistently breathes through their mouth, a first orthodontic evaluation is worthwhile. Many orthodontists use this window for interceptive treatment, meaning they try to guide jaw growth before the pubertal spurt locks things in.
Tweens and teenagers ages 11 to 17
This is the most active and important window for mandibular growth intervention. Because the pubertal spurt drives a significant acceleration in jaw size changes, functional appliances and orthopedic devices are most effective here. Orthodontists can use cervical vertebral maturation (visible on a lateral X-ray) to estimate where a patient is in their growth spurt rather than guessing based on age alone. If jaw surgery might eventually be needed, starting orthodontic preparation during this window can make a significant difference in outcomes. Wisdom teeth (third molars) also begin developing in this period, and panoramic X-rays around age 16 to 17 give a good first look at whether they are likely to erupt cleanly or become impacted.
Adults ages 18 and up
Active mandibular growth is done for most adults. If you have a significant jaw discrepancy that affects your bite, breathing, or facial appearance, orthognathic surgery combined with orthodontics is the established route. This is genuine repositioning of bone, not regeneration, but it produces reliable functional and aesthetic results. For adults with crowded teeth or impacted wisdom teeth, the evaluation starts with a panoramic X-ray and clinical exam, and treatment options range from orthodontics to extractions depending on what is present. If you have noticed your bite shifting or your jaw feeling different in your 30s or 40s, ongoing bone remodeling and sometimes temporomandibular joint changes are the most likely explanations, and a dentist can sort out which is happening.
The most important practical advice is not to wait. The growth window for meaningful orthopedic jaw intervention is genuinely limited, and it closes faster than most parents expect. An evaluation at age 7 to 8 does not mean your child needs treatment immediately. It means you will know early enough to act during the window that actually matters.
FAQ
If my child’s jaw doesn’t look right early on, can braces make the mandible grow later?
Yes, but only in specific ways. The mandible can continue surface remodeling for maintenance and repair, so you may notice subtle contour changes. It does not restart puberty-style length and height growth, so braces or aligners alone cannot “grow” a stopped jaw back to a new growth phase.
Does crowding always mean the mandible is too small?
Tooth crowding can appear for reasons other than insufficient jaw length, including early loss of baby teeth, tooth size differences, premature loss of space, abnormal eruption paths, and habits that shift tooth position. A clinician should check space, eruption angles, and bite relationships, not just jaw size.
If the lower jaw is growing normally, can there still be an overbite or underbite?
A common pattern is growth mismatch between arches. Even with a normally growing mandible, the upper jaw or dental eruption timing can differ, producing an overall bite problem. That is why evaluation should include both upper and lower jaw relationships, not mandible growth alone.
How strong is the link between mouth breathing and how the mandible grows?
Mouth breathing is associated with changes in orofacial function, posture, and sometimes dental and skeletal patterns. However, it is not automatically the sole cause of mandibular shape differences. The first step is usually identifying and treating the underlying driver (allergies, nasal obstruction), while an orthodontic evaluation addresses bite and growth effects.
Can a single X-ray measurement (like SNB or ANB) tell me what treatment will work?
Cephalometric angles like ANB and SNB help quantify jaw position, but they can be affected by head posture, facial growth stage, and measurement method. Your clinician should interpret these alongside the child’s growth phase, bite measurements, and 3D imaging when needed.
What does “interceptive treatment” usually involve at age 7 to 8?
Interceptive treatment does not necessarily mean immediate braces. Many plans use removable appliances, habit control, or limited corrections to guide eruption and create better conditions during active growth, especially around the mixed dentition period. The goal is to buy time and reduce worsening during the pubertal spurt.
If my teen’s panoramic X-ray looks okay for wisdom teeth, does that mean they will definitely erupt normally?
Wisdom tooth eruption is influenced by both tooth development and available posterior space. Even if a child has an average jaw length, the pattern of growth, molar tipping, and eruption timing can change whether third molars have room. Panoramic X-rays help estimate risk, but they do not guarantee the outcome.
What is the difference between orthopedic appliances and braces in terms of jaw change?
Not exactly. Orthodontic forces move teeth by remodeling around the roots, while orthopedic growth aims to modify jaw position during active growth using functional loading and appliances. Both rely on living biology, but they target different tissues and have different realistic limits.
If my bite seems to change in my 30s or 40s, is it new mandibular growth?
A noticeable jaw shift in the 30s or 40s is often related to dental changes, periodontal status, or temporomandibular joint and muscle factors. Because active mandibular growth is largely finished, persistent changes should be assessed by a dentist or orthodontist to rule out bite collapse, joint issues, or occlusal problems.
At what point is surgery considered instead of waiting for growth?
Yes, but it depends on timing and the type of mismatch. If a discrepancy exists, many surgeons coordinate treatment with orthodontics rather than “waiting until after surgery.” Your planning will usually consider whether orthodontic preparation is needed to position teeth properly for surgery and to work with remaining growth, if applicable.
Why is it better to get evaluated early if my child might not need treatment yet?
If a jaw discrepancy is suspected, earlier evaluation is mainly about creating options, not forcing treatment. Waiting too long can reduce the window for growth-guided strategies, particularly before the pubertal growth spurt, and can increase the chance that tooth extractions or surgery are needed later.

Molars and premolars usually do not regrow. Learn when teeth erupt vs when extraction or decay means permanent loss.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Learn why humans don’t grow back adult teeth, what natural healing can do, and today’s options like implants and bridges

