No, humans cannot grow entirely new teeth on demand. You get two natural sets: your 20 primary (baby) teeth and your 32 permanent (adult) teeth, and that's it biologically. Once a permanent tooth is lost, your body has no built-in mechanism to replace it. Humans only grow two sets of teeth because the cells needed to build enamel and the rest of the tooth are effectively lost after eruption why do humans only grow 2 sets of teeth. That's why, after tooth loss, humans typically can't grow more teeth on their own. Researchers are actively working on ways to bioengineer teeth in the lab, and some exciting progress has been made, but as of 2026 there is no clinically available treatment that will grow you a brand-new functional tooth. Even if you still have all your natural permanent teeth, growing a brand-new additional adult tooth is not currently a clinically available option grow another adult tooth. If you're wondering when we will be able to grow new teeth, the answer is that the science is promising but not yet available as a routine treatment when will we be able to grow new teeth. What does exist are excellent tooth-replacement options like implants, bridges, and dentures, and some legitimate (if still experimental) science that may one day change the picture.
Can Humans Grow New Teeth Today? What Science Can Do
How your teeth actually form (and why that matters)
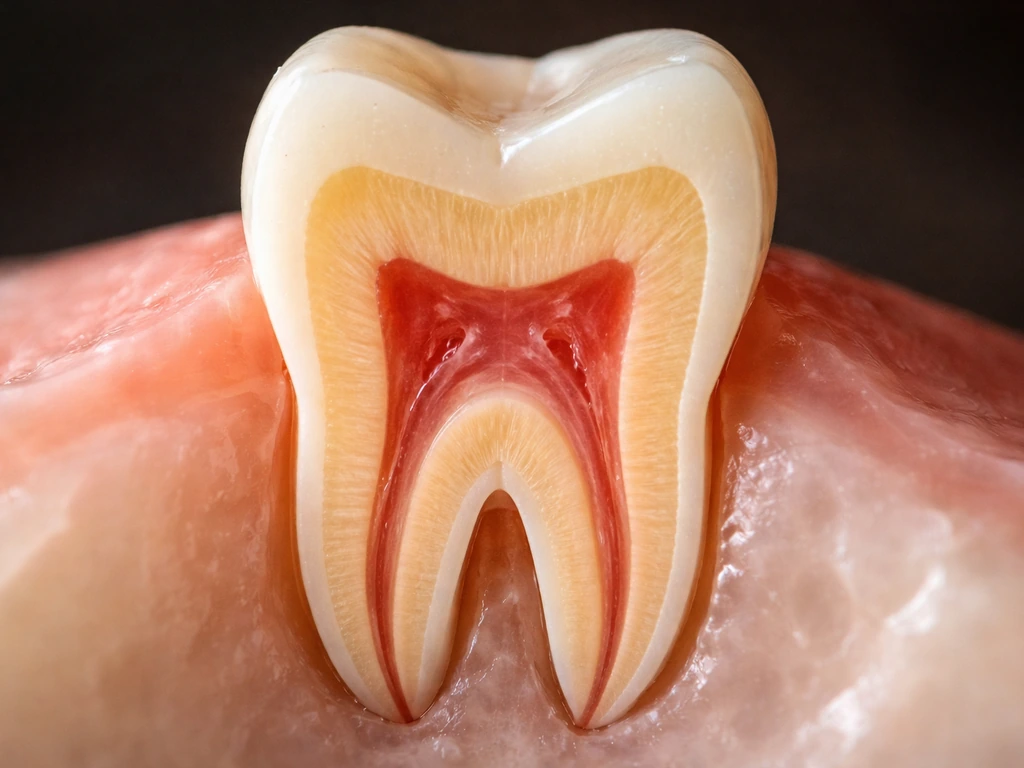
Understanding why teeth can't just regrow starts with knowing how they form in the first place. Tooth development kicks off around the sixth week of embryonic life, when a band of tissue called the primary epithelial band forms from cells lining the developing mouth. From there, a complex back-and-forth conversation happens between two tissue layers: the epithelium (which eventually produces enamel-forming cells called ameloblasts) and the mesenchyme underneath (which produces dentin-forming cells called odontoblasts). These two cell populations signal each other in a tightly coordinated dance that results in the layered structure of a tooth.
Each tooth is built from several distinct compartments. The hard outer shell is enamel, the body's hardest substance, produced entirely by ameloblasts. Just beneath it sits dentin, a slightly softer mineralized tissue made by odontoblasts. In the center is the pulp, the soft living core filled with nerves and blood vessels. Anchoring the whole tooth to your jawbone is the periodontal ligament (PDL), a fibrous tissue that acts like a shock absorber, along with cementum on the root surface and alveolar bone in the jaw. These supporting structures come from a separate tissue compartment called the dental follicle. Every one of these layers requires a unique set of cells that appear at specific developmental windows and are largely gone or exhausted by the time a tooth finishes erupting.
Here's the critical detail: ameloblasts, the only cells that make enamel, are completely lost after a tooth erupts. They don't stick around. That's why enamel cannot repair itself the way a broken bone can. Dentin and pulp have somewhat more regenerative potential because odontoblasts persist inside the living tooth, but even that capacity is limited. The upshot is that the precise cell populations needed to build a tooth from scratch are simply not present in adults.
What researchers are actually working on (and what still doesn't exist)
The science of tooth regeneration is real, it's just much earlier-stage than most news headlines suggest. Researchers broadly fall into a few camps: those working on regrowing specific tooth tissues (like dentin or the periodontal ligament), and those trying to engineer a whole tooth germ in the lab that could be implanted and then erupt naturally. Neither has crossed into routine clinical use.
Partial tissue regeneration: the more advanced work
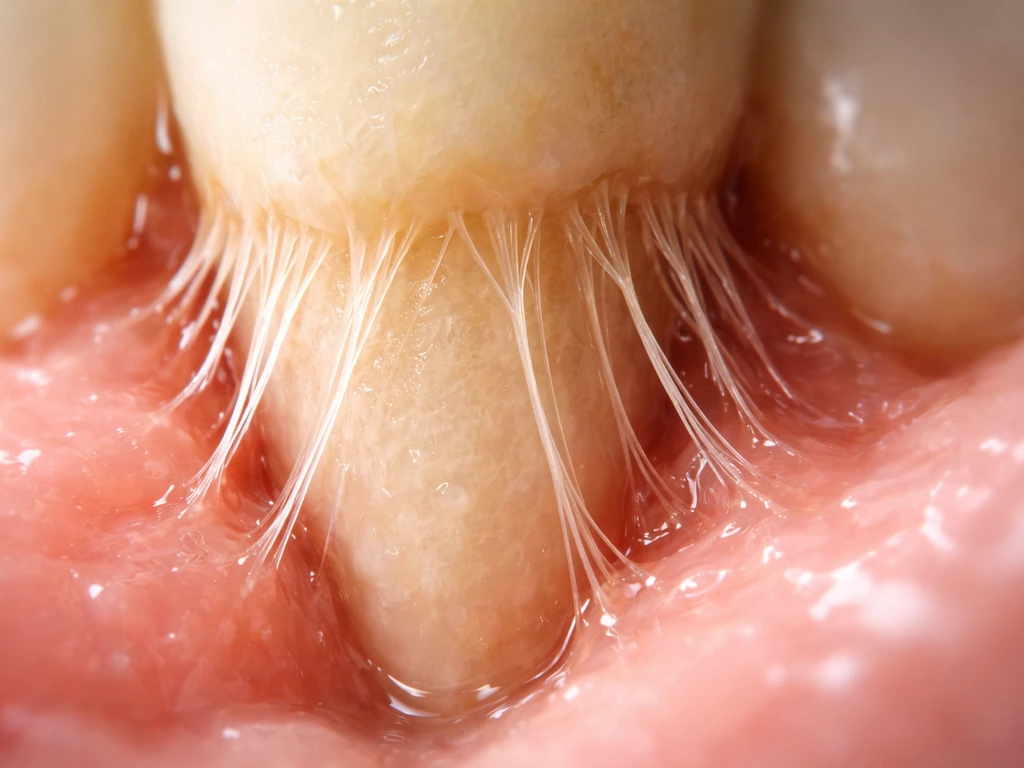
The most clinically relevant progress has been in regenerating parts of the tooth's support system, not the tooth itself. Stem cells derived from the periodontal ligament and dental pulp have been tested in clinical trials for repairing periodontal (gum and bone) defects around existing teeth. A randomized clinical trial published in 2016 showed autologous PDL stem cells could help regenerate bone in periodontal intrabony defects, and a separate trial (NCT02523651) evaluated dental pulp stem cell injections for chronic periodontal disease. These are meaningful advances, but they're about patching damage around a living tooth, not growing a new one.
Regenerative endodontics is another area worth knowing about. This approach, endorsed by the American Association of Endodontists, aims to restore some vitality to a tooth's pulp rather than simply removing it during a root canal. It works best in immature teeth with wide-open root tips, particularly in children and teens, where it can encourage continued root development. In adult teeth, the biology is less forgiving: the root tip is narrower and the capacity for revascularization is reduced. Regenerative endodontics is not creating new enamel or a whole new tooth; it's more about preserving and partially restoring the living tissue inside an existing one.
Whole-tooth bioengineering: promising but not ready
The bigger dream, creating an implantable bioengineered tooth germ that develops into a fully functional tooth in your jaw, is still an unsolved problem. A 2025 comprehensive review of the field described clinical translation as a major ongoing challenge. Researchers have successfully grown tooth-like structures in lab dishes and animal models, but getting a reliable, safe, whole tooth to form in a human jaw remains out of reach. The complexity of coordinating enamel, dentin, pulp, PDL, cementum, and bone, each requiring different cells at different developmental moments, means there's no quick path to a pill or injection that regrows your molar.
| Approach | What it targets | Current clinical status | Whole tooth replacement? |
|---|---|---|---|
| PDL/pulp stem cell therapy | Periodontal bone defects, pulp tissue | Clinical trials (limited), not routine | No |
| Regenerative endodontics | Pulp vitality in existing teeth | Used clinically, mainly for immature teeth | No |
| Bioengineered tooth germ | Full tooth from lab-grown tissue | Animal research, not in human trials | Goal, but not yet |
| Dental implants | Replace a missing tooth root and crown | Established standard of care | Functionally yes, biologically no |
| Bridges | Fill a gap using adjacent teeth | Established standard of care | Functionally yes, biologically no |
| Dentures | Replace multiple or all missing teeth | Established standard of care | Functionally yes, biologically no |
Your real options when you lose a tooth today
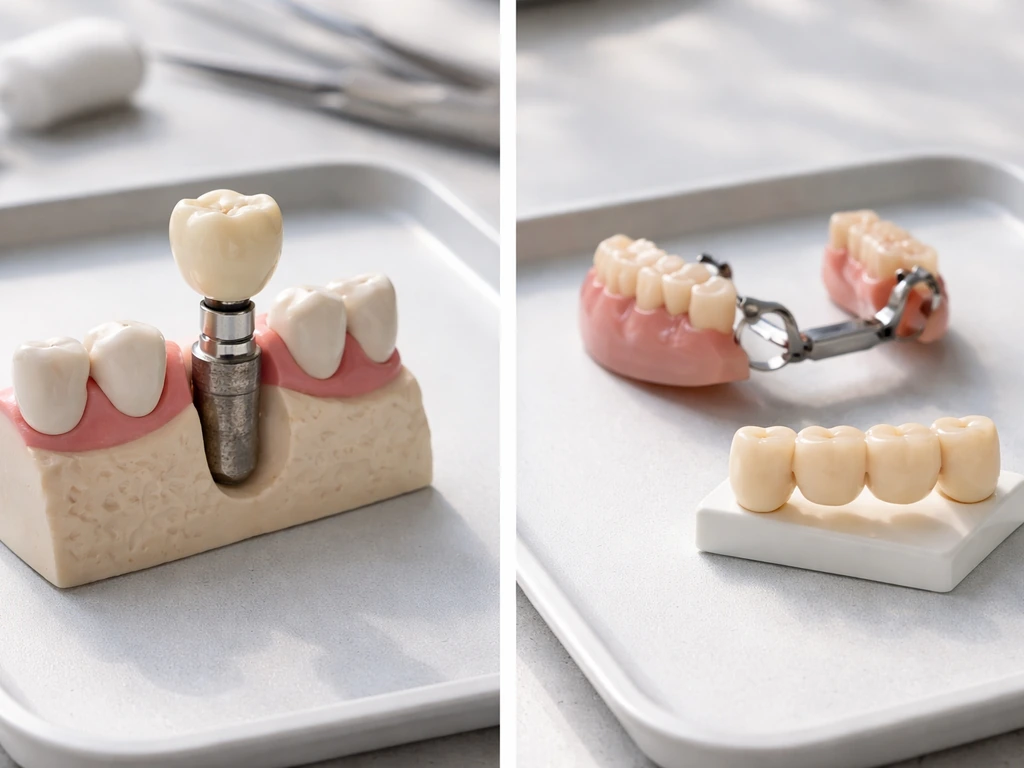
Since biological regrowth isn't on the table, the good news is that modern tooth-replacement options are genuinely excellent. The American College of Prosthodontists frames dental implants as the prosthodontic standard of care for replacing missing teeth, and for most people with adequate bone, they're the closest thing to a natural tooth we have.
- Dental implants: A titanium post is placed into the jawbone and a crown is fitted on top. Implants can replace a single tooth, multiple teeth, or support a full arch. They preserve jawbone, look and function like natural teeth, and can last decades. Eligibility depends on bone density, jaw anatomy, and overall health, so not everyone qualifies right away without additional procedures like bone grafting.
- Fixed bridges: A crown on each side of the gap anchors an artificial tooth in between. No surgery required, faster to complete than an implant, but the neighboring teeth need to be filed down to serve as anchors, which is a permanent change to healthy teeth.
- Partial or full dentures: Removable appliances that replace one, several, or all teeth. Less expensive upfront, but require regular maintenance and refitting as the jaw changes shape over time. The American College of Prosthodontists notes that decisions about relining or replacing dentures are highly case-specific.
- Space management and orthodontics (for kids and teens): In developing dentitions, sometimes the priority is holding space open for a tooth that hasn't erupted yet or planning ahead for an implant once jaw growth finishes. This isn't regeneration, but it's smart biological timing.
- Bonding and crowns: For teeth that are chipped or partially broken rather than fully lost, these restorative options can rebuild structure using composite resin or porcelain, preserving what's left of the natural tooth.
The best option for you depends heavily on your age, the location of the missing tooth, your bone condition, and how many teeth are involved. A prosthodontist or your general dentist can map out which route makes the most sense for your specific situation.
Tooth-regrowth myths vs. what the science actually says
The internet is full of claims about regrowing teeth naturally, so let's go through the most common ones directly.
- Myth: Certain supplements, oils, or diets can regrow lost teeth. Fact: Nothing you eat or apply topically can regenerate a tooth that has been lost. Nutrients like calcium and vitamin D support existing bone and tooth health, but they cannot trigger the formation of new tooth tissue once a tooth is gone.
- Myth: Stem cell treatments can give you a new tooth now. Fact: Current clinical stem cell work focuses on repairing periodontal tissues around existing teeth, not growing new ones. Whole-tooth bioengineering is still in early research stages.
- Myth: A third set of teeth naturally exists in some people. Fact: While there are rare cases of extra (supernumerary) teeth and ongoing research into whether humans have any residual genetic capacity for a third dentition, this is not something that happens reliably or safely in the general population.
- Myth: Wisdom teeth growing in counts as regrowing teeth. Fact: Wisdom teeth (third molars) are part of your original permanent set, just erupting late, usually between ages 17 and 25. Their eruption is development, not regeneration. And as the American Association of Oral and Maxillofacial Surgeons notes, many people need them removed due to decay or crowding risks.
- Myth: Enamel can grow back. Fact: Enamel cannot regenerate. Once it's gone, it's gone, because the cells that make it (ameloblasts) no longer exist in your mouth. Early enamel mineral loss from mild acid attack can be partially reversed through remineralization with fluoride and saliva, but this is not the same as growing new enamel.
- Myth: Japanese researchers already have a tooth-regrowth drug available. Fact: As of May 2026, no tooth-regrowth drug has been approved for clinical use anywhere in the world. Clinical trials are underway in Japan and elsewhere, but these are still investigational.
Who this affects most and what to do next
Your age and the reason for tooth loss change what the smartest next step looks like. Here's how to think about it by life stage.
Children (primary and mixed dentition)
If a child loses a baby tooth early due to decay or injury, the priority is space maintenance, not replacement. The permanent tooth is coming, but losing that space can cause crowding. A pediatric dentist can fit a space maintainer to hold the gap open. If a permanent tooth is lost in childhood (which is uncommon but happens), the focus shifts to protecting the jaw space until growth is complete, typically mid-to-late teens, at which point an implant becomes an option. The American Academy of Pediatric Dentistry's guidelines emphasize that planning for future prostheses is often the right approach when congenital or early tooth loss occurs.
Teens and young adults
Jaw growth typically finishes in the mid-to-late teens for girls and slightly later for boys. Implants placed before growth is complete can end up misaligned as the jaw develops. An orthodontist or oral surgeon can assess whether growth is finished using jaw X-rays. In the meantime, a temporary flipper (a removable appliance with a false tooth) can fill a gap aesthetically. Once growth is confirmed complete, an implant is usually the best long-term solution.
Adults and seniors
For adults, the main variables are bone density (which decreases after tooth loss if an implant isn't placed promptly) and overall health. Implants are the gold standard if bone is sufficient. If not, a bone graft can often create the conditions needed, though it adds time and cost. Bridges are a faster option when adjacent teeth are already compromised. Full or partial dentures remain a practical choice when multiple teeth are missing or when implants aren't feasible.
What to bring to your dental appointment
When you see a dentist or specialist about a missing or damaged tooth, it helps to have a few things ready: your age and any relevant health history, the cause and timing of tooth loss (trauma, decay, extraction, congenital absence), any imaging or X-rays you already have, and a clear sense of your priorities around cost, aesthetics, and how invasive you're willing to go. That combination lets a dentist map out whether implants, a bridge, dentures, or watchful waiting makes the most sense for you right now.
The honest bottom line: true biological tooth regeneration is one of dentistry's most exciting frontiers, and researchers are making real progress on the science. But it's not something you can access today. What you can access, right now, are replacement options that work well and preserve your oral health while that science matures. Don't wait on a future breakthrough to address a missing tooth; losing bone in the meantime makes future options harder and more expensive.
FAQ
If I lose a permanent tooth, is there any way to make it regrow naturally at home (supplements, oils, or home remedies)?
No. There is no at-home approach that can recreate the missing enamel and coordinated tooth-forming tissues. Even when stem cell science is promising in research settings, it has not been translated into a routine “regrow a tooth” therapy you could do yourself.
Why can’t enamel regrow, while some other tissues can heal?
Enamel depends on ameloblasts, and those cells are not retained after a tooth erupts. Because the enamel-making cell population is gone, enamel repair and true regrowth are not comparable to bone healing.
Could regenerative endodontics work for adults who lost a tooth or only damaged the pulp?
Regenerative endodontics is mainly about restoring pulp vitality in a tooth that is already present, and it tends to work best in immature teeth with open root tips (commonly in children and teens). For fully formed adult roots, the procedure is harder to make predictable, and it will not create missing enamel or replace a lost tooth.
Are there any “stem cell” injections available that will grow a new tooth?
Stem cell approaches that have reached clinical testing are focused on repairing tissues around existing teeth, such as periodontal bone and gum-supporting structures. They are not clinically available as a whole-tooth regrowth treatment, so be cautious with marketing claims that suggest otherwise.
If I want the best long-term outcome, how urgent is it to replace a missing tooth?
It matters. Leaving a gap can contribute to bone loss and changes in neighboring teeth over time, which can make future options like implants more difficult and more expensive. A common next step is to book a consultation soon after tooth loss to discuss timelines and preservation strategies.
What should I do immediately after tooth loss to preserve options like implants later?
Ask about maintaining the site and controlling bone loss. Your dentist may recommend a treatment plan that considers timing, imaging, and whether you need a graft or a temporary tooth solution while you heal. The exact recommendation depends on whether the loss was due to extraction trauma, infection, or long-standing decay.
Can orthodontics or spacers replace the need for regeneration?
Sometimes. In children and teens, space maintenance or orthodontic management can preserve the gap until the permanent tooth is ready or until growth is complete. In adults, orthodontics can reposition teeth, but it does not regenerate a lost tooth, so your choice still depends on your health, bite, and jawbone condition.
If I have congenital absence or an early missing permanent tooth, is an implant always the final step?
Often it becomes part of the long-term plan, but timing is different. When growth is ongoing, implants may be delayed to avoid misalignment. Interim solutions (like temporary appliances or other prosthetic approaches) may be used until the jaw has finished developing.
How do dentists decide between implants, bridges, and dentures for my situation?
They typically evaluate age and growth status, the location and number of missing teeth, remaining tooth health, and the condition of the jawbone. Bone sufficiency often determines whether an implant is feasible, while adjacent tooth condition can make bridges more or less practical.
Are there situations where waiting is reasonable instead of replacing right away?
Sometimes, but it depends on the cause and timing of loss. Waiting may be appropriate for short healing windows after extraction or when you need orthodontic coordination. The key caveat is to avoid prolonged gaps that increase bone loss and can shrink the range of future restoration options.
What information should I bring to a consultation to avoid delays or wrong assumptions?
Bring records of the cause and timing of tooth loss (trauma, decay, extraction, infection), any relevant medical conditions and medications (especially those affecting bone healing), and any existing X-rays or scans. Also share your priorities (function, appearance, cost, invasiveness) so the specialist can match options to your goals.
Learn why humans don’t grow back adult teeth, what natural healing can do, and today’s options like implants and bridges
Myth-busting answer on whether adults can regrow teeth, plus real options like implants, crowns, and orthodontics.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

