Yes, a cavity can absolutely form and grow under an existing filling. Secondary or recurrent decay is how cavities can grow under an existing filling cavities grow. It's called secondary or recurrent decay, and it's one of the most common reasons dental fillings eventually fail. The filling itself doesn't decay, but the tooth structure around and beneath it can. If there's even a microscopic gap at the edge of your filling, bacteria get in, acid builds up, and the decay process continues just like it would on any unprotected tooth surface. The frustrating part is that you often can't see it or feel it until it's progressed significantly.
Can Cavities Grow on Fillings? Signs, Causes, and Next Steps
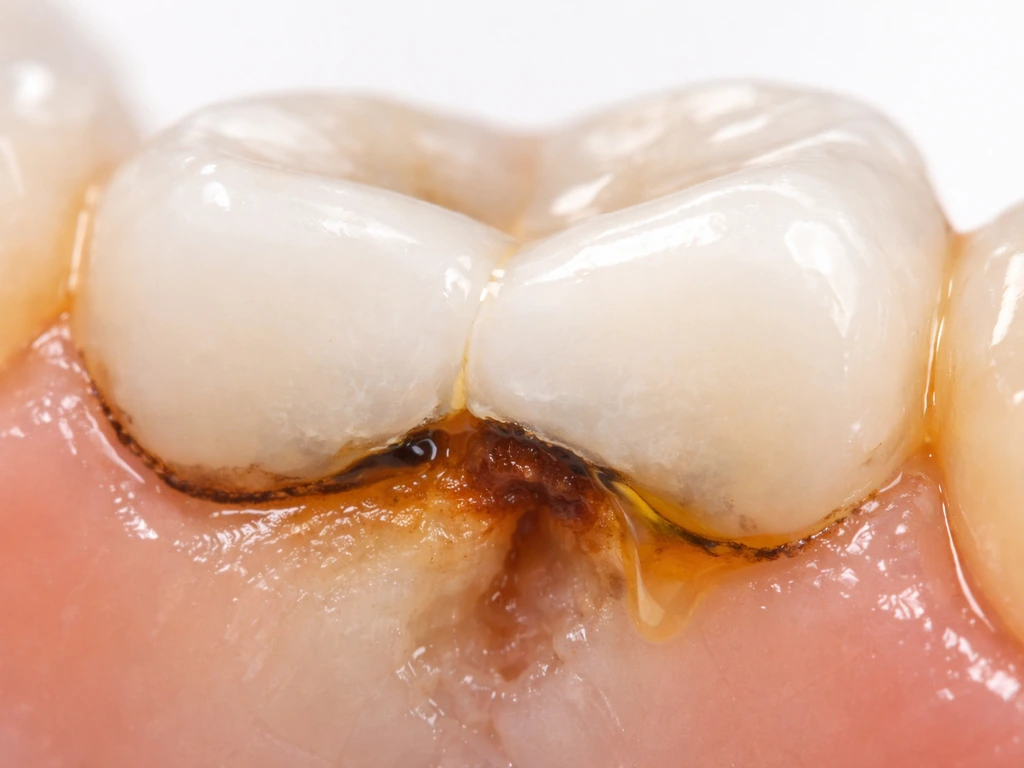
Can a cavity form under an existing filling?
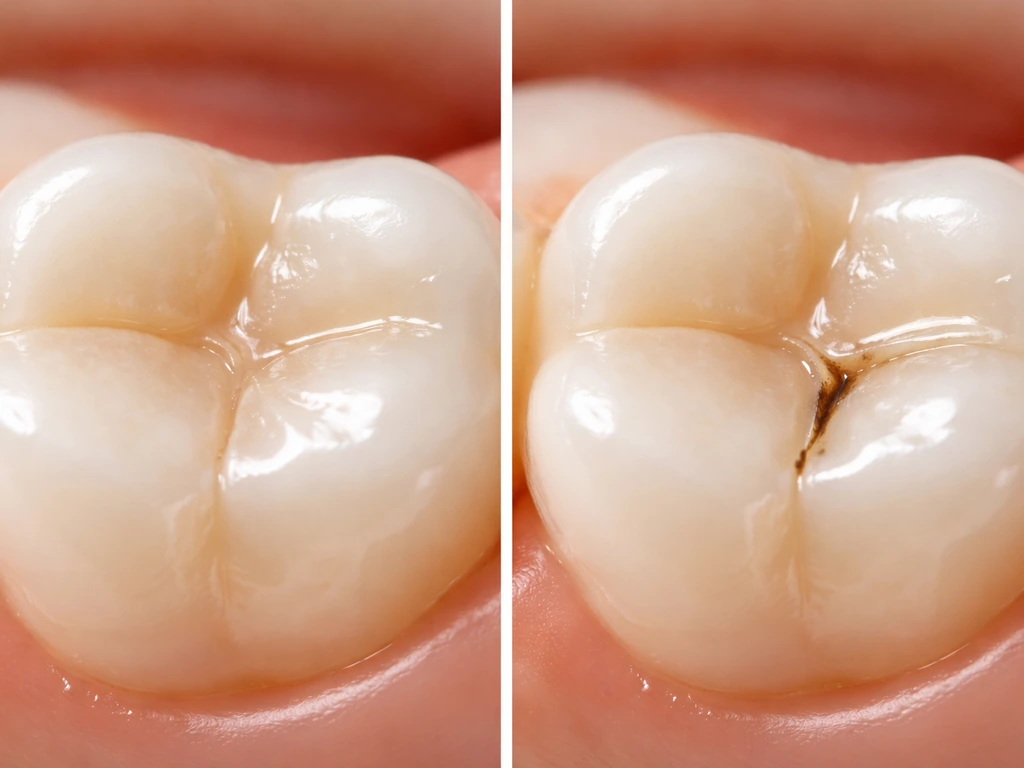
Absolutely, and it happens more often than most people realize. According to the ADA, dental caries is a biofilm-mediated, sugar-driven, dynamic disease that can progress and destroy tooth hard tissues over time, even beneath a restoration. The filling material itself (whether amalgam, composite resin, or porcelain) isn't vulnerable to decay, but the tooth underneath and around it very much is. In fact, secondary caries is one of the leading causes of failure for resin composite restorations, right alongside fracture. So if you've had a filling for a few years and something feels off, your instinct to investigate is correct.
It's also worth being clear about what's happening biologically here. A cavity forming under a filling is not the tooth "growing back" in any sense. Enamel and dentin don't regenerate in adults. What's actually happening is ongoing destruction of the tooth structure that was already there. The decay process never fully stopped, or it restarted at a vulnerable margin. This is a critical distinction: nothing is growing back. Decay is progressing forward.
What secondary (recurrent) decay actually means
The clinical term is secondary caries or recurrent caries, and StatPearls defines it simply as new caries that form at a restoration's margin. Think of the margin as the seam between your filling and the natural tooth. If that seam isn't perfectly sealed, or if it opens up over time, it becomes a pathway for bacteria.
A Clinical Oral Investigations review breaks down secondary caries pathogenesis into three scenarios: decay that is causally linked to a defective restoration (gaps or failed margins), decay that's associated with an intact restoration but driven by the patient's own high-caries risk, or adjacent primary caries that continues to develop right next to the filling. All three can look and feel similar to the patient. From the outside, the tooth might look fine. You might not even have symptoms early on. This is why it's sometimes called "hidden decay" and why regular dental exams matter even when you feel nothing wrong.
Visually, if secondary decay is advanced enough to be visible, you might notice a gray or brown discoloration around the edges of a filling, or the filling might look darker underneath (especially with older amalgam fillings). But in many cases, there's simply nothing visible until a dentist uses instruments or imaging.
Why cavities start under fillings in the first place
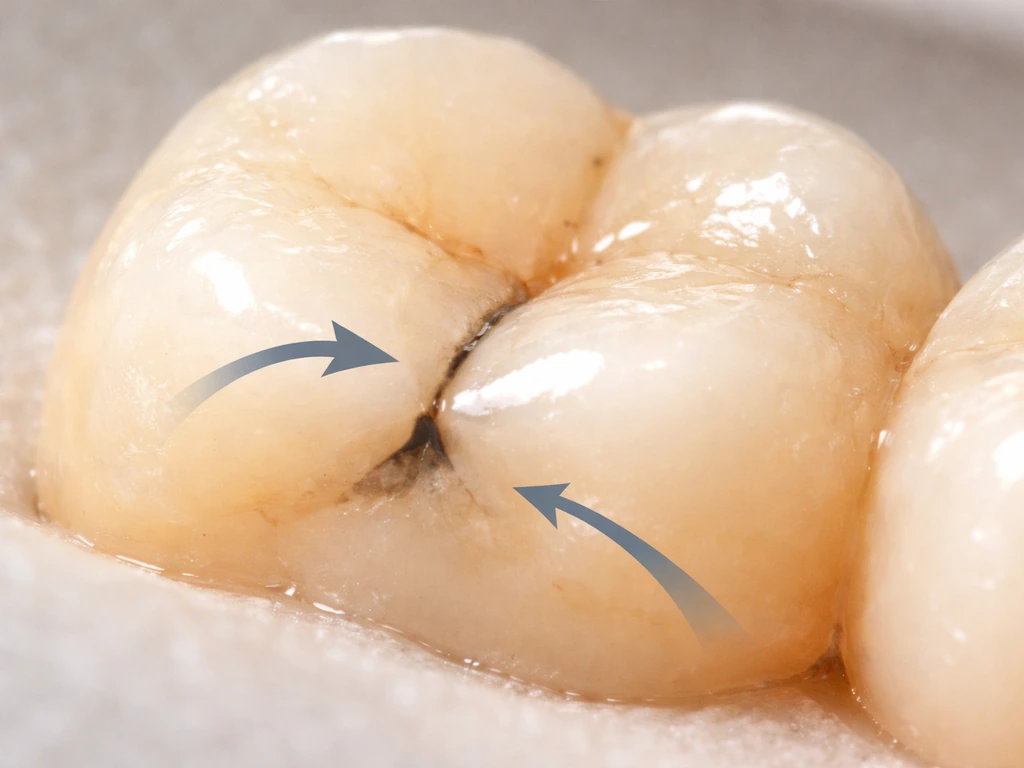
There are a few specific reasons this happens, and understanding them helps you take targeted action to prevent it.
Microleakage and gap formation
This is the big one. Even a filling that looks perfect in your mouth has microscopic gaps at the interface between the restoration and the tooth. Research on composite restorations specifically describes how bacteria and acid by-products leak into these gaps, creating a protected environment where decay can quietly advance. Composite resin fillings contract slightly as they cure, which can widen these gaps over time. Temperature fluctuations from hot and cold foods cause both the filling and the tooth to expand and contract at slightly different rates, gradually loosening the seal further.
Worn or deteriorating margins
Fillings aren't permanent. Most composite fillings last 7 to 10 years on average before they need attention, though some last longer and some fail sooner. Over time, the edges (margins) of a filling can chip, crack, or erode, opening up more surface area for bacteria to colonize. A filling that was placed years ago with a tight seal may no longer have one today.
Diet and oral hygiene
A filling doesn't change your baseline cavity risk. If you have a diet high in sugar and fermentable carbohydrates and you don't brush and floss consistently, you're still feeding the bacteria that cause caries. The margin of a filling is actually a spot where plaque loves to accumulate, especially if the filling sits slightly below or above the surrounding tooth contour. Poor flossing habits leave the proximal (between-tooth) margins particularly exposed.
Dry mouth and age-related changes
Saliva is a natural defense against decay. It buffers acids, rinses away bacteria, and remineralizes early enamel damage. As people age, many medications reduce saliva flow, which raises cavity risk significantly. Older adults with existing fillings are particularly vulnerable to secondary caries for exactly this reason. If you're on medications for blood pressure, allergies, anxiety, or depression, dry mouth may be quietly undermining your older restorations.
Signs and symptoms to watch for
Secondary decay under a filling often has no symptoms at all in the early stages, which is why it can catch people off guard. But as it progresses, there are specific things to pay attention to.
- Tooth sensitivity to cold, heat, or sweet foods that you didn't have before, or that has worsened
- Pain or discomfort when biting down specifically on that tooth
- A lingering ache that doesn't go away quickly after the triggering food or temperature
- A bad taste or smell near the tooth that doesn't resolve with brushing
- Visible discoloration at the edges of the filling (dark brown or gray halo around the restoration)
- A feeling that the filling has shifted, feels loose, or doesn't fit the same way
- Visible chipping or cracking at the margin of the filling
If you experience lingering pain (pain that persists more than 30 seconds after the stimulus is removed), spontaneous throbbing pain, or pain that wakes you up at night, those are signs the decay may have reached or is very close to the dental pulp. That warrants urgent care, not a wait-and-see approach. Don't try to manage that level of pain on your own for more than a day or two without seeing a dentist. This is also the point at which a tooth abscess can develop, which is a serious complication that needs immediate attention. The speed at which a tooth abscess can grow varies, but it can worsen quickly without prompt treatment how fast can a tooth abscess grow.
How dentists check for decay under fillings
Your dentist has several tools for detecting secondary caries, and most appointments involve more than one. Here's what typically happens:
- Visual exam: The dentist looks for discoloration, gaps, chips, or cracks at the filling margins. With composite resin fillings, a transillumination light can sometimes reveal shadows beneath the surface.
- Explorer probing: A sharp dental instrument is used to feel around the margins of the filling. A sticky or soft spot at a margin is a red flag for decay.
- Bitewing X-rays: These are the most common tool for detecting interproximal (between-tooth) decay under fillings. They show a dark shadow in the tooth structure beneath or adjacent to the restoration.
- Periapical X-rays: These give a full view of the root and surrounding bone, helpful when deep decay or possible pulp involvement is suspected.
- Percussion and bite testing: Tapping on the tooth or having you bite on an instrument helps identify whether pain is localized and whether the nerve may be involved.
There are limitations to all of these. X-rays miss decay that's directly beneath a dense metal amalgam filling because the metal blocks the view. Very early or small lesions under composite can also be hard to distinguish on X-ray. If you are wondering how long does it take a small cavity to grow, early or small lesions under composite can still be hard to distinguish on X-ray, so your dentist may rely on other exam methods too. And probing is only as reliable as the access the dentist has to the margins. This is one reason why dentists sometimes recommend replacing an older filling for diagnostic reasons, particularly if symptoms are present but imaging is inconclusive. Removing the old filling lets them see exactly what's underneath.
What treatment looks like if there's decay under a filling
The treatment depends on how much decay is present and how deep it goes. There's no way to treat secondary caries by leaving the filling in place. The old restoration has to come out so the dentist can access and remove all the decayed tissue.
| Situation | Likely Treatment | What to Expect |
|---|---|---|
| Small secondary cavity at the margin | Repair or replacement of the filling | Old filling removed, decay cleaned out, new filling placed in one appointment |
| Moderate decay beneath a larger filling | Full replacement with a larger filling or onlay | May require a bigger restoration if significant tooth structure is lost |
| Decay close to but not into the pulp | Filling replacement, possibly with a protective liner | Higher sensitivity post-treatment; close monitoring for pulp health |
| Decay into the pulp (pulpitis or abscess) | Root canal treatment followed by crown | Multi-appointment process; tooth can usually be saved if treated promptly |
| Extensive structural loss around an old filling | Crown placement after decay removal | Covers and protects what remains of the natural tooth structure |
One thing worth knowing: if your dentist finds decay very close to the pulp but the tooth isn't symptomatic, they may place the new restoration and monitor the tooth over several appointments before committing to a root canal. Not every near-pulp cavity requires immediate root canal therapy. But if symptoms worsen or the pulp becomes irreversibly inflamed, the root canal becomes necessary. Early treatment almost always means a simpler, less expensive outcome, which is the core argument for not delaying when you suspect something is wrong.
How to prevent decay under fillings (and what won't help)
Let's clear up a common misconception first. Enamel and dentin do not regenerate in adult humans. You can slow or even arrest very early-stage decay through remineralization (fluoride, good saliva flow, low acid diet), but once a cavity has formed beneath a filling, that tooth structure is gone. It won't grow back. The filling was placed to replace tooth structure that was destroyed, and if decay forms again around it, more tooth structure is being lost. Nothing is regrowing. This is a fundamental biological limit of human dentition.
Similarly, don't count on oil pulling, special toothpastes, or remineralization supplements to reverse established secondary caries. Remineralization strategies work on the outermost layer of enamel before a cavity has formed, not on decay that's already progressing under a restoration. If you're interested in how cavities progress or the question of whether teeth can regrow from a cavity in different contexts, those are genuinely interesting biology questions, but the answer under a filling is straightforward: the decay needs to be removed and the restoration replaced.
Here's what actually works for prevention:
- Brush twice daily with a fluoride toothpaste, paying close attention to the gumline and margins of existing fillings
- Floss daily, especially at the contact points where fillings meet adjacent teeth
- Get dental X-rays on the schedule your dentist recommends (typically bitewings every 1 to 2 years for adults with a history of cavities)
- Ask your dentist to assess your existing fillings at every checkup, not just look for new cavities
- Stay hydrated and talk to your doctor about alternatives if you're taking medications that cause dry mouth
- Reduce sugar and acid frequency rather than quantity alone (sipping soda all day is worse for margins than drinking it quickly with a meal)
- Ask about fluoride varnish treatments if you're at higher caries risk
- Replace fillings proactively when your dentist flags deteriorating margins, even if you're not in pain yet
Fillings have a lifespan, and treating them like permanent fixes is one of the most common mistakes people make. A filling placed 15 years ago that's never been evaluated is a risk, not a success story. The standard of care is ongoing monitoring, and if your dentist says it's time to replace an older filling, that's the most effective prevention available for secondary decay.
FAQ
If I can’t feel pain, how would I know cavities are growing under my filling?
In early stages secondary decay can be completely symptom-free. Dentists look for changes in the filling margins, use bitewing X-rays and sometimes other imaging or magnification, then probe carefully around the edges. If you notice the filling looks darker at the seam, that can be a useful visual clue even before symptoms appear.
Can a filling itself cause decay, or is it always a gap problem?
A filling material does not “rot,” decay happens where bacteria can access vulnerable tooth tissue, usually at imperfect margins or through microfractures/chipped edges. However, decay can also occur adjacent to the filling if nearby tooth surfaces already have high caries activity, so the problem is not always directly at the exact seam you can see.
Do composite and amalgam fillings behave differently regarding secondary cavities?
Yes. Composite margins can be affected by polymerization shrinkage and slight gap formation over time, while amalgam can still develop recurrent decay at margins if sealing is lost. Also, X-rays can be less reliable directly under metal, so a dentist may depend more on clinical probing and other methods when amalgam is involved.
What does it mean if my dentist “recommends replacing” a filling just for diagnosis?
It usually means imaging and probing do not clearly show whether decay is present, especially with near-margin or near-pulp concerns. By removing the old restoration, the dentist can directly assess the tissue, and sometimes treat early decay before it becomes more invasive.
If I get pain when biting, does that always mean a cavity under the filling?
Not always. Bite pain can be from a cracked tooth, a loose or overcontoured restoration, or gum and periodontal issues. Your dentist will evaluate contact points and may check for fractures, because treatment differs, and you do not want to assume it is always secondary caries.
How often should I have older fillings checked to catch secondary decay early?
A common approach is every 6 months to 1 year depending on your personal caries risk, age, and whether you have multiple restorations. Higher-risk patients (dry mouth, frequent snacking, poor flossing, many past cavities) often need more frequent monitoring than the average patient.
Can dry mouth or medications turn a stable filling into an active cavity risk?
They can. Reduced saliva lowers buffering and remineralization, and it makes plaque at margins more cariogenic. If you are starting new medications or notice worsening dry mouth, tell your dentist, because prevention and monitoring intervals may need to change.
What should I do if I suspect secondary decay and my next dental appointment is weeks away?
Avoid delaying care once you have concerning symptoms. If you have lingering pain after hot or cold lasts more than about 30 seconds, spontaneous throbbing, or pain that wakes you at night, treat it as urgent. Until you are seen, stick to gentle brushing around the area, avoid very sugary snacks, and do not try to “patch” it with OTC sealants or DIY fixes.
Is it ever possible to save the tooth without removing the existing filling if a cavity is found?
For established secondary caries at a restoration margin, the tooth decay must be accessed and removed, which typically requires removing the old filling. Sometimes a close call near the pulp is handled with careful monitoring after placing a new restoration, but leaving the decayed tissue in place is not considered effective treatment.
How can I reduce the chance of secondary decay after my filling is replaced?
Focus on reducing caries risk at the margins: floss daily to keep proximal areas clean, brush with fluoride toothpaste, and if you have dry mouth, discuss saliva support options with your dentist. Also ask your dentist whether you need sealants or more frequent checks based on your diet and past history, since baseline risk drives recurrence.
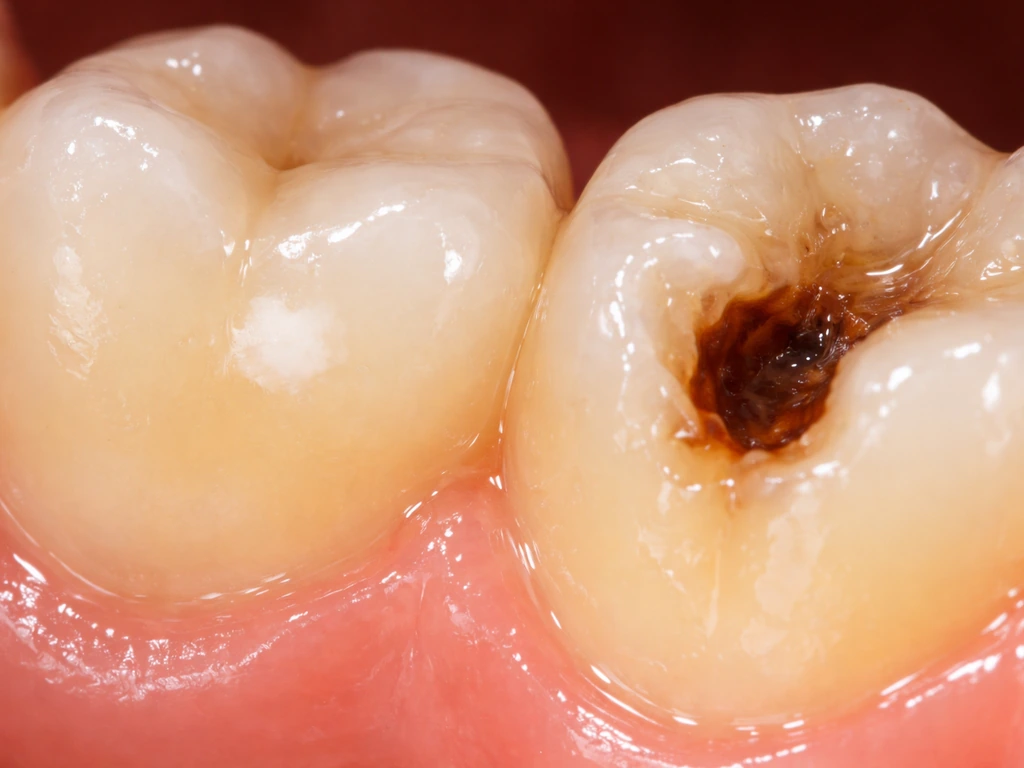
Learn if cavities grow, where decay spreads, how it reaches dentin and pulp, and what stops progression now.
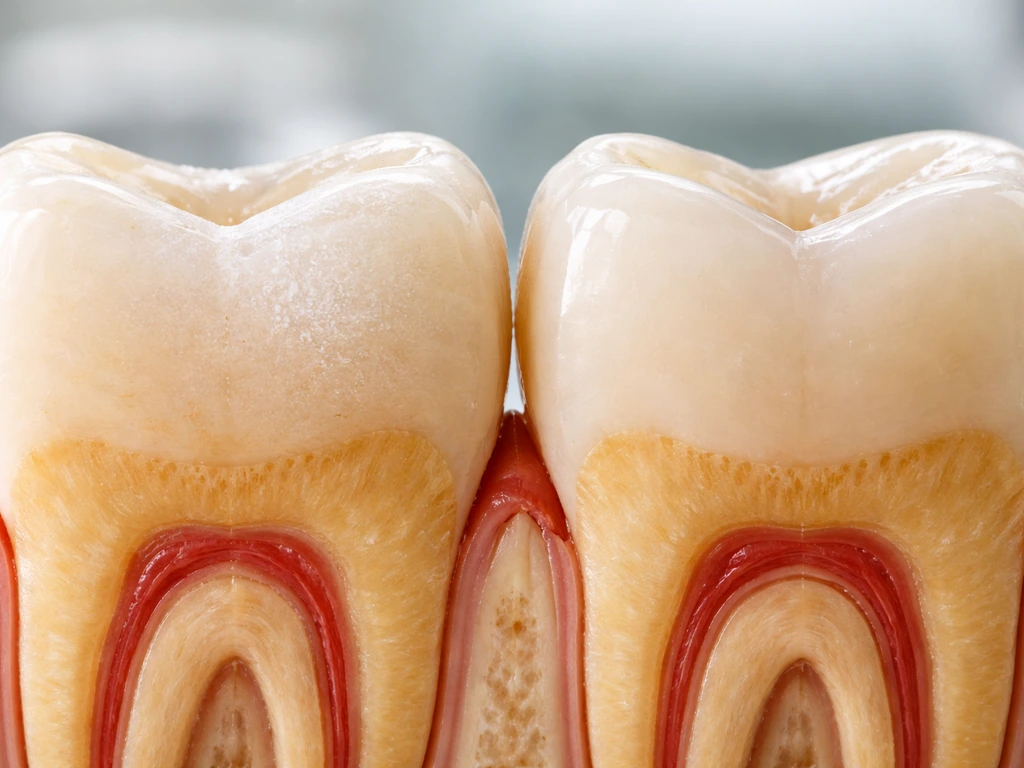
Can teeth regrow from cavities? Learn what can remineralize early, what cannot, warning signs, and next steps.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

