No, your tooth cannot grow back from a cavity. Once decay destroys enamel or the deeper layers of a tooth, that tissue is gone for good in adults. The only partial exception is a very early-stage cavity, where the enamel has started to lose minerals but the surface hasn't actually broken down yet. At that point, you have a real window to slow or reverse the damage. But once there's a physical hole in the tooth, no amount of toothpaste, oil pulling, or remineralizing diet is going to close it back up. That's the honest, evidence-based answer, and this guide will walk you through exactly what that means for your situation today.
Can Your Tooth Grow Back From a Cavity? What’s Possible
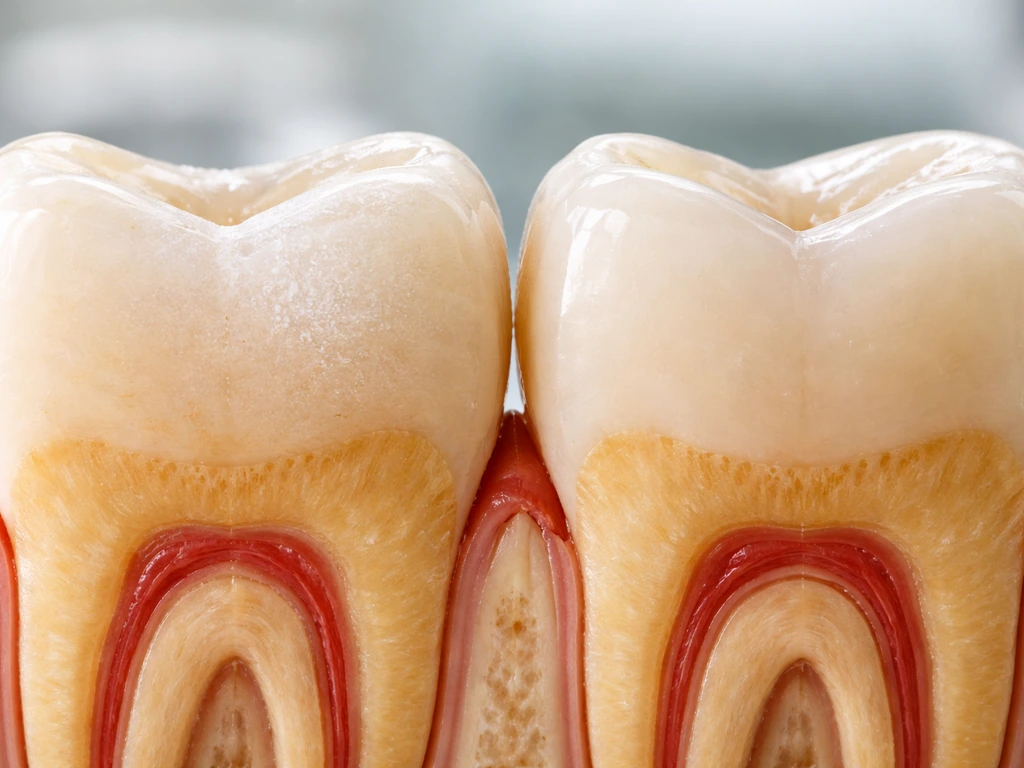
What a cavity actually does to your tooth
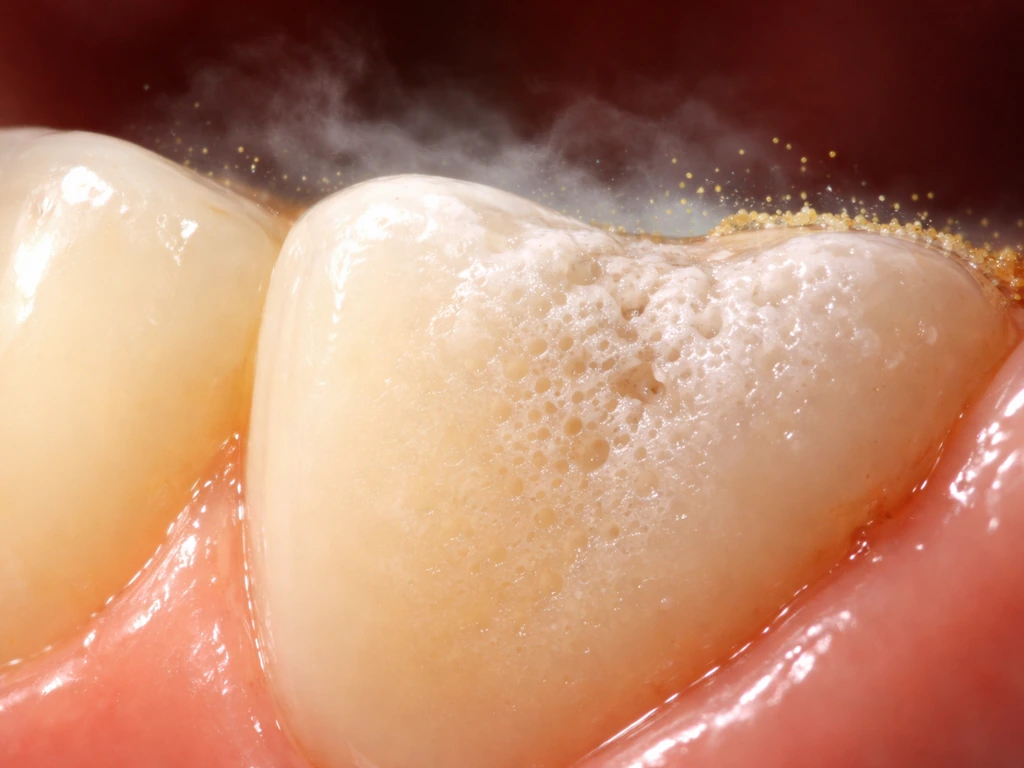
A cavity isn't just a hole that appears out of nowhere. It follows a very predictable progression. Bacteria in your mouth feed on sugars and produce acids. Those acids pull minerals out of your enamel, the hard outer shell of the tooth. At first, this shows up as a chalky white or dull patch on the enamel surface, sometimes called a white spot lesion. The surface is still physically intact at this stage, but the enamel underneath is getting weaker.
If the demineralization continues unchecked, the enamel surface eventually breaks down. That's the point of cavitation, and it's a one-way door. From there, the cavity can move into the dentin, the softer layer beneath the enamel. Dentin has microscopic channels that lead toward the nerve, which is why cavities in dentin often cause sensitivity to temperature and sweetness. As bacteria invade the dentin, the tooth tries to protect itself by laying down what's called tertiary dentin around the pulp chamber. It's a defensive response, but it only buys time. If decay reaches the pulp (the innermost part of the tooth containing the nerve and blood supply), you're looking at infection, significant pain, and a much more involved treatment. how fast a tooth abscess can grow from that point is something a lot of people underestimate, which is why getting ahead of it matters.
Can enamel or the tooth actually regrow after decay
Here's the biology in plain language: enamel is made by cells called ameloblasts, and those cells are only active while the tooth is forming. Once the tooth fully erupts into your mouth, the ameloblasts are gone. There's no mechanism left in your body to produce new enamel. So no, enamel cannot regenerate after it has been physically lost to a cavity. The same goes for dentin that has been destroyed by bacterial invasion, and absolutely for the whole tooth. Nothing that has been eaten away by a cavity grows back.
The nuance, and this is important, is what happens before a true hole forms. A white spot lesion is classified as a noncavitated lesion, meaning the enamel surface is still technically intact even though mineral has been lost beneath it. At this stage, remineralization is genuinely possible. Fluoride and calcium from saliva can deposit back into the weakened enamel and harden it again. This isn't regrowing enamel from scratch, it's repairing the mineral structure that's already there. It's a meaningful distinction: you're rescuing the existing enamel, not creating new tissue.
Can a cavity fill itself in naturally, or does it need repair
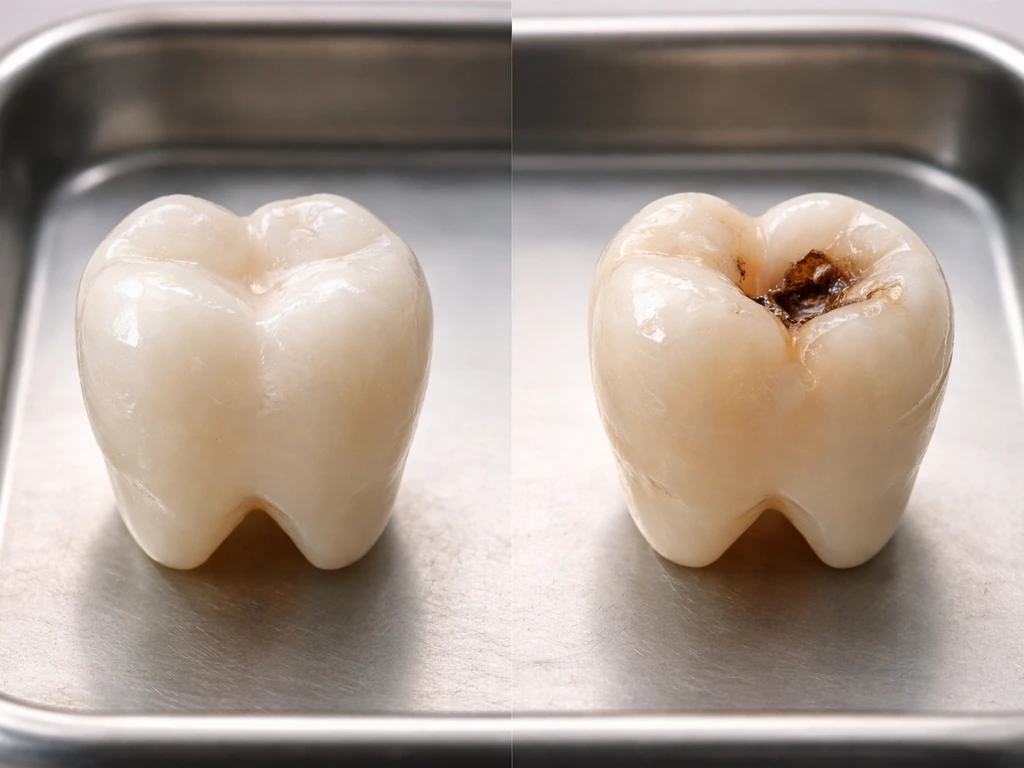
A cavitated lesion, meaning one where the enamel or tooth surface has actually broken down, will not self-fill. Full stop. Once that surface is breached, bacteria and plaque get trapped inside the cavity where your saliva and fluoride can't effectively reach them. The decay continues from the inside, and there's no natural process that closes the hole back up. If you've been told that eating more remineralizing foods or using special toothpaste will fix a cavity you can already feel or see, that's misinformation.
Remineralization strategies, things like fluoride varnish applied every three to six months, fluoridated toothpaste, and diet adjustments, are genuinely useful and evidence-backed. But they're tools for stopping early, noncavitated lesions in their tracks, not for repairing physical holes. It's worth understanding how cavities grow over time, because the difference between a noncavitated lesion and a cavitated one is often just a matter of weeks or months without intervention.
Signs you need a dentist urgently
Not every cavity is a same-week emergency, but some situations absolutely are. Knowing the difference can save you from a much worse outcome. If you're experiencing any of the following, don't wait for a routine appointment:
- Spontaneous, throbbing tooth pain that isn't triggered by anything, especially if it wakes you up at night
- Swelling in your gum, jaw, or face, even if it seems minor right now
- Fever alongside tooth pain or facial swelling, which can signal that infection is spreading
- Pus, a bad taste, or a pimple-like bump on the gum near a tooth
- Difficulty swallowing or breathing (this is a genuine emergency, go to an ER immediately)
- Pain that has recently gotten dramatically worse after a period of quiet
These are the red flags associated with a dental abscess. A tooth abscess will not go away on its own, and if the infection spreads beyond the tooth, it can become life-threatening. Mayo Clinic is explicit that fever with facial swelling, or any trouble breathing or swallowing, means you should not wait. If you can't reach a dentist, go to an emergency room. For less dramatic but still concerning symptoms, like lingering sensitivity to cold or a toothache that comes and goes, call your dentist and get an appointment within a day or two.
Treatment options depending on how deep the decay goes
What a dentist recommends depends almost entirely on how far the cavity has progressed. Here's a practical breakdown:
| Decay Stage | What's Affected | Typical Treatment |
|---|---|---|
| Early / noncavitated (white spot) | Enamel mineral loss, surface intact | Fluoride varnish, remineralization, monitoring |
| Shallow cavity | Enamel into outer dentin | Composite or amalgam filling |
| Moderate cavity | Deeper dentin, near pulp | Filling or crown depending on size |
| Deep cavity / pulp involvement | Pulp infected or inflamed | Root canal treatment, then crown |
| Severe / irreparable | Tooth structure too compromised | Extraction, then implant/bridge/denture |
A filling is the most common fix for a straightforward cavity. The dentist removes the decayed material and fills the hole with composite resin or amalgam. If the decay has spread significantly and weakened the tooth structure, a crown may be needed to protect what's left. If the pulp has become infected, a root canal is necessary. That involves removing the infected tissue from inside the tooth, sealing the root canals, and usually placing a crown on top. Extraction is the last resort, used when the tooth can't be saved. One thing that surprises people: it's also possible to get decay on a tooth that's already been treated, so understanding whether cavities can grow on fillings is useful context if you have older dental work.
What can actually be remineralized, and what can't
Remineralization is real, but it has a hard cutoff. It works on noncavitated lesions where enamel mineral has been lost but the enamel surface is still physically present. The main drivers of remineralization are fluoride and saliva. Fluoride works by inhibiting the demineralization process and making enamel more resistant to acid, while also facilitating the redepositing of calcium and phosphate minerals into weakened enamel. Community water fluoridation alone has been shown to reduce tooth decay by about 25% in children and adults, which gives you a sense of just how significant consistent low-level fluoride exposure really is.
For remineralization at home, using fluoride toothpaste twice daily is the most important thing you can do. Your dentist can apply professional-strength fluoride varnish (typically 5% sodium fluoride) every three to six months for higher-risk patients, or use a 1.23% APF gel application as part of a care plan. Casein phosphopeptide products (like some remineralizing toothpastes) have supporting evidence as well, though fluoride remains the gold standard. What remineralization cannot do is repair physical cavities, regrow enamel that's been physically lost, or repair dentin or pulp damage. If you're wondering how long it takes a small cavity to grow from an early white spot into something that needs a filling, the answer depends on your diet, oral hygiene, and saliva quality, but it can happen faster than most people assume.
Does it matter how fast the cavity is progressing
Yes, a lot. Cavity growth rate varies significantly from person to person and tooth to tooth. How much a cavity can grow in a month is not a fixed number, but in a high-sugar diet with poor oral hygiene, progression from a white spot to a visible cavity can happen in weeks. In someone with good saliva flow, low sugar intake, and regular fluoride exposure, an early lesion might stay noncavitated and stable for months or even longer. This is why your dentist's recall interval matters and why they sometimes recommend more frequent checkups for people with active caries risk.
Kids vs adults: age changes the picture
Children have one advantage that adults don't: baby teeth fall out. If a baby tooth has a cavity that's causing problems, the treatment approach can be more conservative in some cases, since the tooth will eventually be replaced. But this doesn't mean cavities in primary teeth are no big deal. Baby teeth hold space for permanent teeth, help children eat and speak properly, and a badly infected baby tooth can affect the developing adult tooth underneath. If a child's baby tooth reaches the stage of irreversible pulpitis (where the nerve is damaged beyond repair), the options are typically a pulpotomy (removing the infected pulp tissue while preserving the root) or extraction followed by a space maintainer.
For adults, there is no second set of teeth waiting. Every permanent tooth you have is the only one you'll get, with one possible exception: wisdom teeth. If a wisdom tooth hasn't come in yet and you lose a molar near it, there are rare cases where the wisdom tooth drifts forward to partially fill the space, though this is not something you can rely on. The more practical exception involves children in the window between losing a baby tooth and the adult tooth erupting, which is normal dental development, not regrowth. That's not a cavity growing back, it's just the permanent tooth doing what it's supposed to do.
What about dental regeneration research
You may have seen headlines about scientists regrowing teeth or regenerating dental pulp. This is real research. There are pilot clinical studies using dental pulp stem cells to regenerate pulp-like tissue inside teeth, and there are regenerative endodontic procedures used in immature permanent teeth (mainly in children and teenagers) where the root hasn't finished forming. In those cases, certain procedures can help the root continue developing and may regenerate some pulp tissue. But these are specialized clinical scenarios. They are not treatments available at your regular dentist for a standard cavity in a fully formed adult tooth. For everyday cavities in grown adults, the biological limits described above still apply completely.
How to stop a cavity from progressing further, starting today
If you suspect you have an early cavity or you've just had one confirmed, here's what to actually do. First, book a dental appointment if you haven't already. Don't delay hoping it will improve on its own. If it's already cavitated, it will only get worse. If it's still a white spot, early professional intervention makes a real difference.
- Brush with fluoride toothpaste twice a day, and don't rinse with water immediately after brushing. Let the fluoride sit on your teeth.
- Cut back on sugar frequency, not just amount. Every time you eat or drink something sugary or acidic, your enamel spends about 20 to 30 minutes in an acid attack. Five small sugary snacks cause more damage than one large one.
- Drink fluoridated tap water when possible. It provides consistent low-level fluoride exposure throughout the day.
- Ask your dentist about fluoride varnish at your next visit, especially if you've had recent cavities.
- Consider dental sealants for children and teenagers. Sealants physically block bacteria from accessing the pits and fissures of back teeth, where most cavities start.
- Don't skip checkups. Catching a lesion at the noncavitated stage is the only point where you have a real chance to avoid a filling.
The bottom line is that teeth don't grow back from cavities, but early decay doesn't have to become a filling. The biology gives you a small but real window to intervene before a cavity becomes permanent damage. Use that window, see your dentist, and don't let internet folklore about teeth regenerating stop you from getting treatment that actually works.
FAQ
If a cavity is small, can it heal itself without a filling?
Not in the way people usually mean it. A dentist can sometimes arrest early decay (noncavitated white spot lesions) with fluoride and other measures, but that does not close a hole that has already formed. If you see a true pit, shadow, or catch your tongue on a spot, it is very likely cavitated and will not self-heal.
How do I tell if my cavity is still at the early stage or already too deep?
If you have severe sensitivity or pain that wakes you up, or the tooth feels “high” when you bite, that can indicate deeper involvement, not just surface damage. Those scenarios often need exam-based decisions like a filling with deeper work, a root canal, or urgent evaluation, so waiting for home remedies is risky.
Will whitening toothpaste or teeth-whitening strips make a cavity disappear?
Whitening products can sometimes make sensitivity worse, but they do not reverse cavity formation. Also, after professional cleaning, you may notice spots that look new or darker, which can mimic cavities. A dentist can distinguish demineralization from staining with focused inspection and, if needed, imaging.
If I cut sugar and improve brushing, will that stop a cavity from getting worse?
Diet changes alone can slow acid attacks, but they rarely work fast enough to stop established decay. The highest-impact combo is consistent fluoride exposure (like twice-daily fluoride toothpaste) plus reducing frequent sugar or sipping exposure. If you have active lesions, ask your dentist whether you should shorten your recall interval.
Can fluoride varnish or high-fluoride toothpaste reverse a cavity I can feel with my tongue?
Yes, but only when the tooth already has a surface that can be remineralized. If the enamel surface is intact, professional varnish and high-fluoride products can rebuild mineral density. If the tooth surface is already broken, those products can only help manage surrounding risk, not repair the cavity.
Can aggressive brushing or charcoal toothpaste help or hurt cavity healing?
Over-brushing with abrasive techniques can wear enamel and make sensitivity worse, which can create confusion when a cavity is developing. Aim for gentle, thorough technique with a soft brush, and if you are using whitening or charcoal products, ask your dentist whether they increase abrasion for your specific enamel condition.
What role do mouthwash and flossing play if teeth cannot grow back from cavities?
Mouth rinses and flossing are supportive, but they are not a substitute for fluoride. If you use mouthwash, choose an option that does not replace brushing with fluoride toothpaste. Also, if you are skipping floss because of bleeding, that is a sign to floss gently and consistently, since plaque between teeth is a common cavity starting point.
Could my toothache be from a cracked tooth or a failing filling instead of a new cavity?
If a tooth has a visible crack, a filling may not be the whole issue, since decay can occur at margins and along crack lines. A dentist will check the margins, look for secondary decay, and determine whether the problem is a failing restoration, a new cavity, or both, which affects treatment.
When should I treat symptoms like fever or swelling as an emergency, not a dental appointment problem?
The safest rule is to treat worsening symptoms as urgent. If you have fever, facial swelling, or trouble breathing or swallowing, seek emergency care, even if the pain seems to be “going down.” For persistent pain, call your dentist promptly rather than waiting for symptoms to fully resolve.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

