Yes, cavities grow. Left alone, a cavity will almost always get bigger over time, spreading deeper into the tooth and eventually reaching the nerve. The only real question is how fast, and whether you can stop or slow that progression before it turns into a bigger problem. This article walks you through exactly what cavity growth looks like, where it happens, how to tell if yours is early or advanced, and what you can do right now to stop things from getting worse.
Do Cavities Grow Over Time? Where Decay Spreads and What to Do
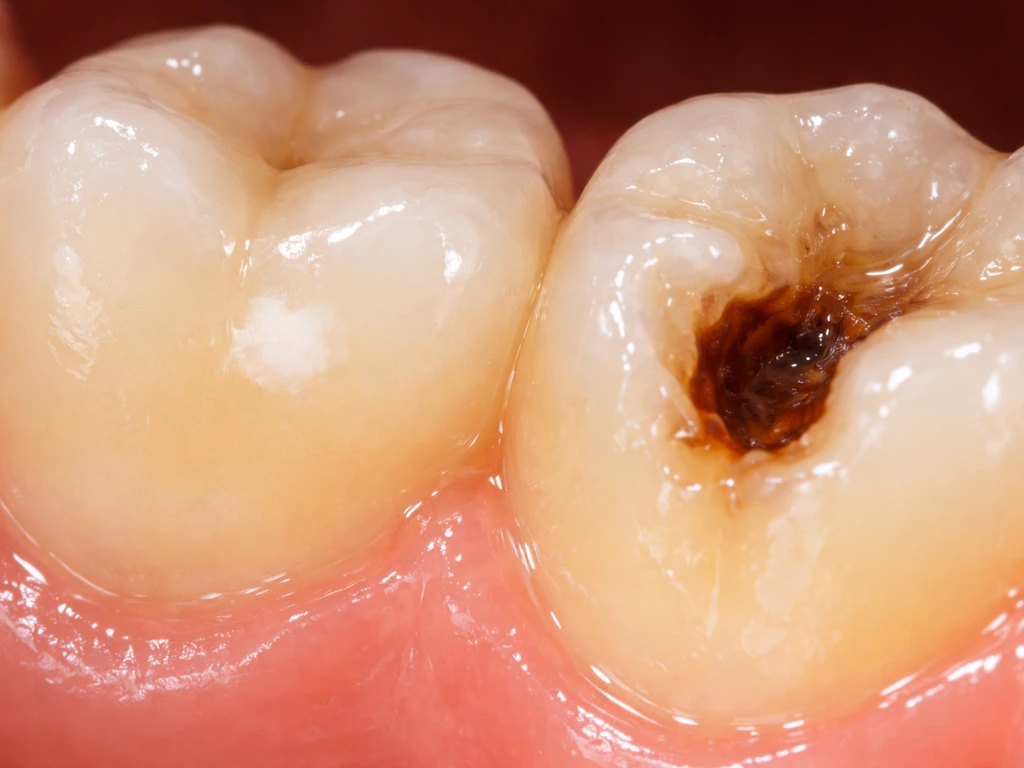
What 'cavity growth' really means: progression vs. regeneration
Here's a misconception worth clearing up immediately: cavities do not heal themselves in the way a cut on your skin does. Once tooth structure is physically lost (meaning there's an actual hole or breakdown in the enamel), your body cannot regenerate that missing material. Teeth are not living tissue that rebuilds itself. The dental classification system known as ICDAS II specifically separates 'noncavitated' lesions (early damage where the surface is still intact) from 'cavitated' lesions (where there's actual breakdown and exposed dentin). That distinction matters enormously when it comes to what can and can't reverse naturally.
So when dentists talk about cavity 'growth,' they mean progression: the decay process advancing from the outer enamel layer inward, dissolving more tooth structure as it goes. This is driven by acid-producing bacteria in your mouth that feed on fermentable carbohydrates (sugars and refined starches). The acid dissolves minerals out of your tooth. If nothing stops that process, the cavity keeps expanding, not because something is growing toward the tooth, but because the tooth itself is being slowly destroyed from the inside out.
Where cavities tend to grow: the usual suspects
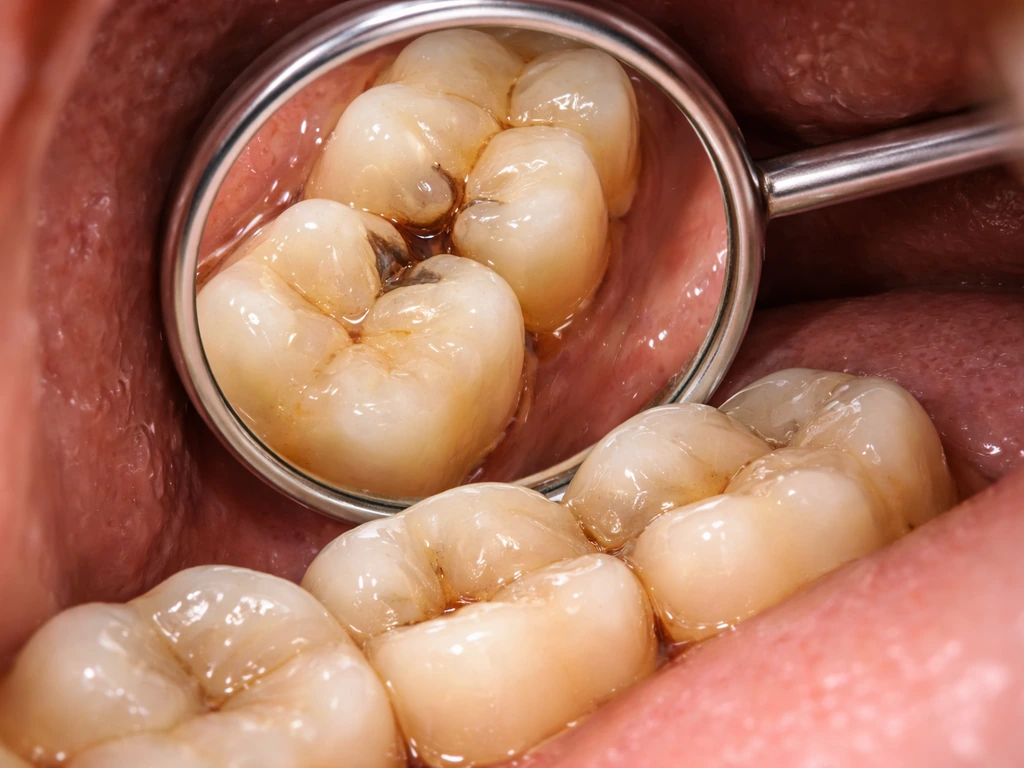
Decay doesn't strike randomly. It clusters in places where bacteria-laden plaque can sit undisturbed and where acid exposure is prolonged. Knowing the most common spots helps you target your brushing and flossing where it matters most.
- Occlusal surfaces (chewing surfaces): The deep pits and fissures on the top of molars are prime real estate for cavities. Food and bacteria get trapped in these grooves, and a toothbrush bristle often can't reach the bottom of them. The ADA specifically notes that anatomical pits and fissures on permanent molars trap food and promote the bacterial biofilm that starts decay.
- Between teeth (interproximal surfaces): Cavities between teeth are extremely common and also the hardest to spot without an X-ray. Flossing is the main defense here, because brushing alone simply doesn't reach these surfaces.
- Near the gumline (cervical/root surfaces): As gums recede with age or gum disease, the root surface (which is covered by cementum, not enamel) becomes exposed. Root surface caries progress faster than enamel caries because cementum is softer and less mineral-dense.
- Around existing fillings and crowns: Decay can start at the margins where a filling or crown meets natural tooth structure, especially if that seal has degraded over time. This is sometimes called secondary or recurrent decay.
- In children: baby teeth and newly erupted permanent teeth have thinner, less mature enamel, making them especially vulnerable. Early childhood caries can progress faster than decay in adult teeth.
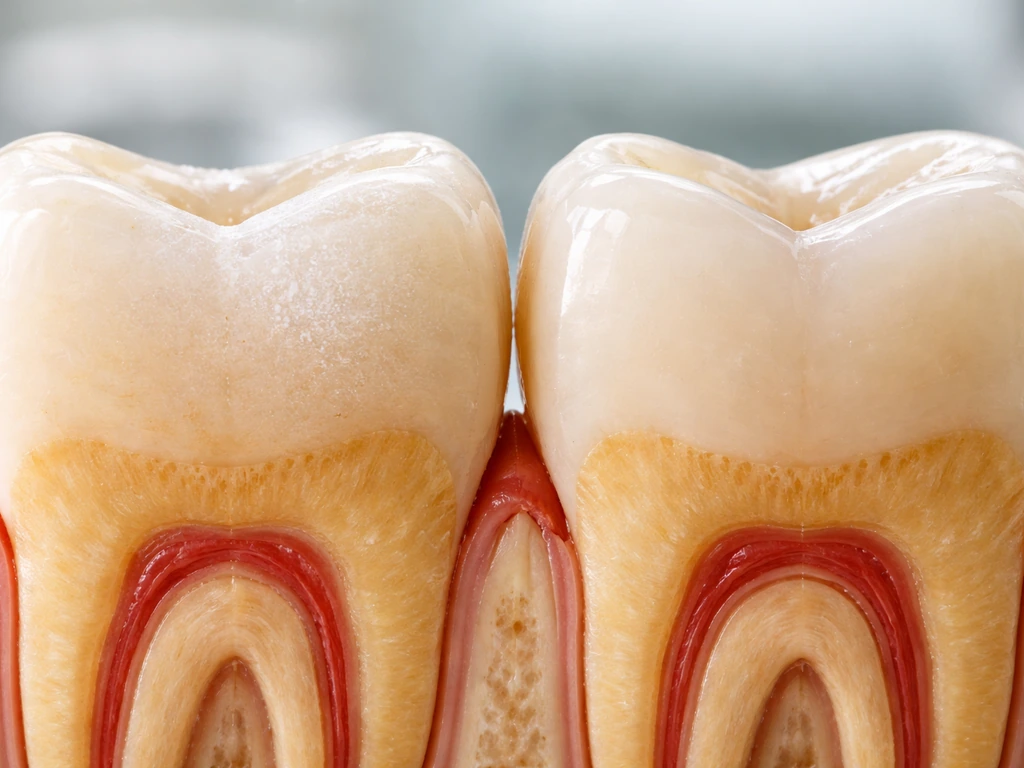
How decay spreads through your tooth: enamel to dentin to pulp
Think of a cavity as moving inward in stages. Each layer it crosses represents a bigger problem and more complex treatment.
- Enamel: The outermost layer. Early decay starts here as mineral loss without visible breakdown. At the very early stage (a 'white spot lesion'), the surface may look chalky or opaque, and it can feel slightly rough when a dental probe passes over it. The enamel is still physically intact, and this is the only stage where natural reversal (remineralization) is genuinely possible.
- Cavitated enamel: Once the enamel surface actually breaks down and a hole or pit forms, the cavity is now 'cavitated.' The structural loss is permanent. Bacteria have a sheltered place to colonize and the destruction accelerates.
- Dentin: Dentin lies just beneath enamel and is significantly softer and more permeable. Once decay reaches dentin, it spreads faster because the material offers less resistance. Dentin also contains microscopic tubules that connect to the nerve, which is why you may start feeling sensitivity or pain at this stage.
- Pulp: The pulp is the soft core of the tooth containing nerves and blood vessels. If decay reaches the pulp, you're looking at significant pain, possible infection, and a root canal or extraction to resolve it. From here, without treatment, infection can form an abscess.
The jump from enamel to dentin is a clinical turning point. A small cavity caught in enamel may need only a minor filling. The same cavity left to grow into dentin or pulp may require a crown, root canal, or tooth removal. That's why the speed of treatment genuinely matters.
Early signs vs. clear warning signs you need to see a dentist
One frustrating thing about cavities is that they're often painless in the early stages. By the time you feel significant pain, the decay has usually progressed well past the enamel. That said, there are symptoms at each stage worth knowing.
Early signs (worth monitoring, but see a dentist soon)
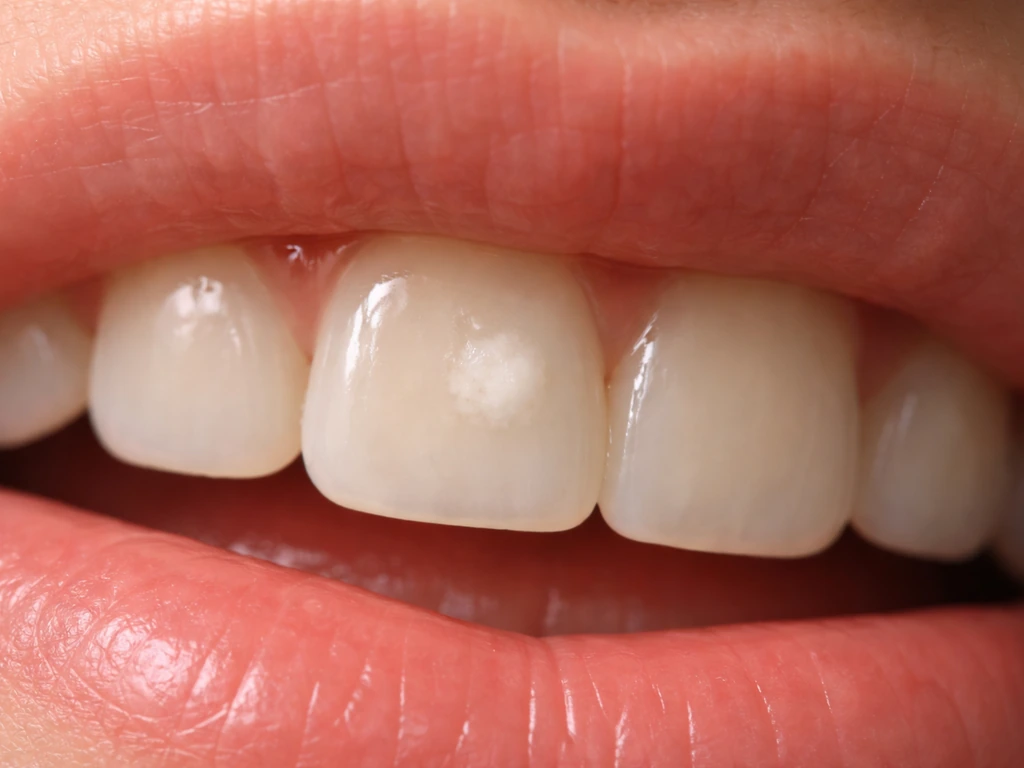
- A white or chalky spot on a tooth surface, especially near the gumline or on a smooth surface
- Mild sensitivity to cold drinks or sweet foods that passes quickly
- A slight rough texture you can feel with your tongue on a tooth surface
- A visible discoloration (white, brown, or tan) in a pit or fissure on a molar
Clear warning signs: don't wait on these
- Persistent or spontaneous toothache, especially pain that wakes you up or lingers after the cause (hot, cold, sweet) is removed
- Visible hole, dark pit, or obvious discoloration in the tooth
- Sharp pain when biting down
- Swelling in the gum near a tooth, a bump that looks like a pimple on the gum (this may indicate an abscess)
- Fever or facial swelling alongside tooth pain: go to an emergency room immediately if you can't reach a dentist. The Mayo Clinic and Cleveland Clinic both list fever and facial swelling with tooth pain as reasons for urgent care, because infection can spread beyond the tooth and become life-threatening.
If you're experiencing fever, swelling in your face or jaw, or difficulty swallowing or breathing along with dental pain, do not wait for a dentist appointment. If an infection from a tooth abscess is spreading, it can worsen quickly, so prompt dental care matters how fast can a tooth abscess grow. Go to an emergency room. These are signs a dental infection may be spreading systemically.
Can cavities stop or reverse? White spot lesions vs. true cavities
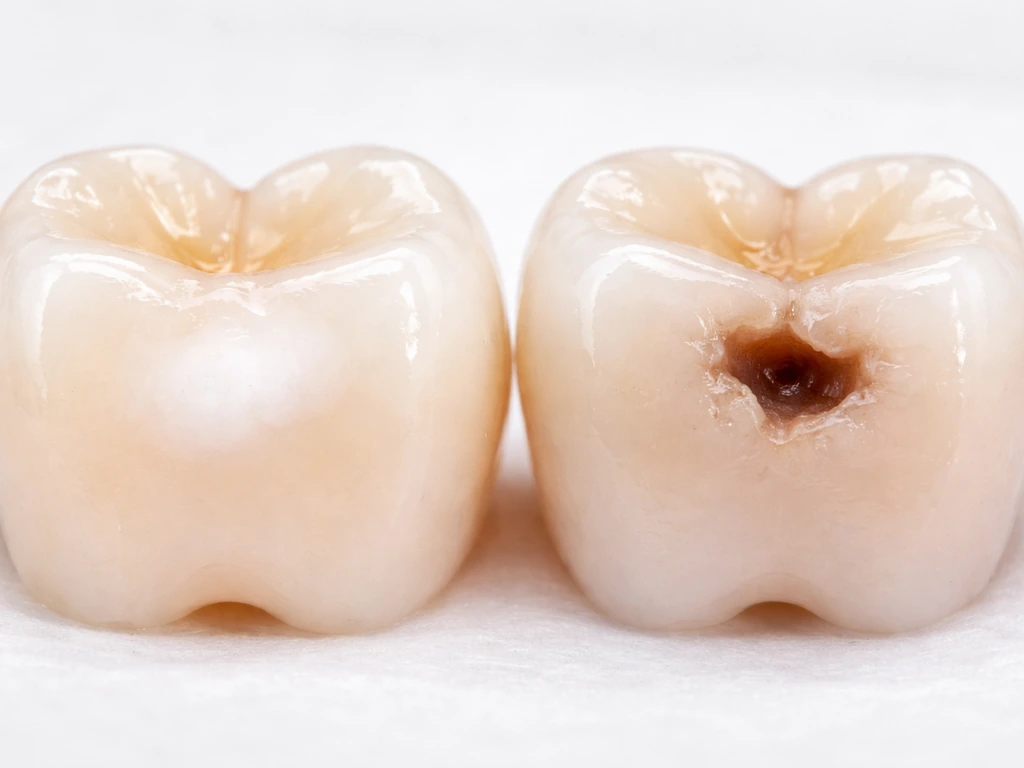
This is probably the most important distinction in this entire article. The answer is: it depends on which stage you're at, and the line between 'can reverse' and 'cannot reverse' is whether the tooth surface has actually broken down.
A white spot lesion is a noncavitated early caries lesion. The enamel has lost minerals and looks chalky or opaque, but the surface is still physically intact. At this stage, remineralization is real and achievable. Fluoride promotes remineralization by helping deposit minerals back into the demineralized enamel and by suppressing the cariogenic bacteria driving the process. A 2024 randomized trial on remineralizing toothpastes found that white spot lesions can improve (partial remineralization or arrest) with consistent use of remineralizing products, though results vary by the individual and adherence to the protocol. Cochrane reviews of fluoride use in patients with fixed braces also found that early demineralized lesions ('white or brown marks') can be prevented and reduced with fluoride strategies.
But once a cavity is cavitated, meaning the surface has broken down and there's an actual hole or exposed dentin, remineralization cannot restore what's physically missing. The architecture of the tooth is gone. You can arrest the decay (stop it from growing), but you cannot regrow the lost tooth structure without a filling. This is why the sibling question about whether a tooth can grow back from a cavity has a clear answer: no, it cannot, at least not with current biology. The same logic applies to the question of whether cavities can grow on fillings: the natural tooth structure at the margins of an existing filling remains vulnerable, and decay there follows the same progression rules.
| Stage | Surface Intact? | Can Reverse Naturally? | What Helps |
|---|---|---|---|
| White spot lesion (early enamel demineralization) | Yes | Yes, with fluoride and risk reduction | Fluoride toothpaste, varnish, diet changes |
| Cavitated enamel lesion | No (surface broken) | No (structural loss is permanent) | Filling required; fluoride prevents further spread |
| Dentin-level cavity | No | No | Filling or crown; urgent if near pulp |
| Pulp involvement / abscess | No | No | Root canal or extraction; may need antibiotics |
What to do today to stop decay from getting worse
If you suspect you have a cavity, or you know you do and haven't treated it yet, here's what you can do right now to slow progression while you get to a dentist.
Fix your brushing routine immediately

Brush twice a day with fluoride toothpaste. The CDC recommends children under 3 use a smear (grain-of-rice-sized) amount, and children aged 3 to 6 use a pea-sized amount. Adults should be using a fluoride toothpaste in the 1,000 to 1,500 ppm fluoride range, which is standard for most over-the-counter products. Brush for a full two minutes and spit, don't rinse with water immediately after, to let the fluoride stay on your teeth longer.
Adjust your diet starting today
Every time you eat or drink something sugary or starchy, bacteria produce acid for roughly 20 to 30 minutes afterward. Frequent snacking throughout the day means your teeth are under near-constant acid attack. Reducing the frequency of sugar exposure, not just the quantity, significantly cuts down on the acid exposure time. Swap constant sipping of sugary drinks for water, and save sweets for mealtimes rather than spreading them across the day.
Floss daily, especially if decay is between teeth
Interproximal (between-teeth) cavities are extremely common and almost entirely preventable with daily flossing. If you're not flossing, plaque sits undisturbed between your teeth 24 hours a day. Start today. There's no point in brushing carefully if the spaces between your teeth remain a constant breeding ground for decay.
Consider a fluoride rinse if you're high risk
For adults with higher cavity risk (dry mouth, gum recession, history of frequent cavities), an over-the-counter fluoride mouthrinse used after brushing adds an additional layer of protection. The AADOCR recommends fluoride rinses for higher-risk individuals but cautions against their use in young children who can't reliably spit, due to swallowing risk.
Book a dentist appointment: sooner is always better
None of the above replaces professional treatment for an existing cavity. If you have a cavitated lesion, you need a filling. Home care can slow the progression and prevent new cavities from forming, but it won't close an existing hole. The longer you wait, the deeper the decay goes, and the more complex (and expensive) the treatment becomes. A small cavity treated early is a 20-minute filling. That same cavity left for 6 to 12 months might be a root canal and crown. That same cavity left for 6 to 12 months might be a root canal and crown, which is why learning how long does it take a small cavity to grow can help you judge urgency. How fast a small cavity can grow depends on your individual risk factors, but waiting is never the right move.
Prevention going forward: fluoride, sealants, and managing your risk
Once you've addressed the immediate problem, the goal is to change the conditions that allowed decay to start in the first place. Cavity progression is not random bad luck. It reflects a balance between the forces that destroy tooth mineral (acid-producing bacteria, sugar, dry mouth) and the forces that protect and rebuild it (saliva, fluoride, good hygiene). Tip that balance in your favor and cavities slow down or stop.
Fluoride: your best daily tool
Fluoride works by inhibiting the acid-producing bacteria in plaque and by enhancing remineralization of early enamel damage. The CDC's review of fluoride's role in caries prevention confirms both mechanisms. For most people, twice-daily brushing with fluoride toothpaste is the foundation. Higher-risk individuals may benefit from prescription-strength fluoride toothpaste (5,000 ppm) prescribed by their dentist, or fluoride varnish applied professionally. The American Academy of Pediatrics notes that the AAPD recommends fluoride varnish every 3 to 6 months for children at elevated caries risk.
Sealants for kids (and some adults)
Dental sealants are thin coatings applied to the pits and fissures of molars, physically blocking bacteria and food from getting into those grooves. The AAPD notes that sealants have been used for nearly 50 years and have strong evidence showing they reduce caries and delay invasive treatment in children and adolescents at elevated risk. If your child has deep grooves in their molars and hasn't had sealants applied, ask about it at their next appointment. For adults with deep fissures and a history of occlusal cavities, sealants are also worth discussing.
Address dry mouth
Saliva is your mouth's natural defense system. It buffers acid, washes away food particles, and delivers minerals that help remineralize enamel. Dry mouth (from medications, mouth breathing, certain medical conditions, or aging) significantly raises your cavity risk. If you have dry mouth, talk to your doctor or dentist about management strategies: staying well hydrated, using saliva substitutes, chewing sugar-free gum to stimulate saliva flow, and adjusting medications if possible.
Age-specific considerations
Children are at high risk because their enamel is thinner and less mature, their teeth are newer, and diet and brushing habits are harder to control. The AAPD's early childhood caries policy emphasizes that frequent sugar exposure and poor fluoride access are the primary drivers of rampant early decay in young children. In contrast, older adults face a different version of the same problem: gum recession exposes root surfaces that decay more easily, and medications that cause dry mouth amplify risk. The prevention strategies are the same in principle (fluoride, diet control, professional care), but the implementation and risk level differ by age.
The bottom line: cavities grow when conditions allow them to. They don't pause on their own, and they don't heal once the enamel surface breaks down. But they're also not inevitable, and they're very stoppable with the right combination of daily habits, professional treatment, and risk management. If you're worried about a cavity right now, make the appointment, start the fluoride routine today, and cut back on sugar frequency. That combination, applied consistently, is genuinely effective.
FAQ
Do cavities grow even if I’m not in pain?
If a cavity is already cavitated, it will not “seal itself” or regrow missing tooth structure. At best, you can stop further progression with professional treatment plus strict home care. If the lesion is only a white spot (surface intact), consistent fluoride and diet changes can arrest it, but you need a dental exam to know which case you have.
Why don’t I feel anything yet, but my dentist says I have decay?
Pain is a late sign for many people. Early decay can be painless because enamel has fewer pain nerves. Common exceptions are when decay is near the surface where you can get sensitivity to cold or sweet, or when inflammation around the nerve has already started. If you have any lingering sensitivity or new bad taste, don’t wait for pain.
Can I have a cavity and not see a hole?
You can have a cavity and still see no obvious hole. Decay often starts as demineralization (chalky or brownish spots) or occurs between teeth where you cannot see it. That’s why dentists use bitewing X-rays and visual probes, and why symptoms can be misleading.
Is it okay to rinse with water after brushing with fluoride toothpaste?
Rinsing right after brushing can wash away fluoride, especially if your brush schedule is rushed. If you want maximum benefit, spit after brushing, avoid eating for 30 minutes, and do not rinse with water immediately. If you use a mouthrinse later, wait until after the fluoride toothpaste time window.
Does cutting sugar help if I still snack on crackers, chips, or bread?
Frequent “healthy” snacks can still drive acid attacks if they are sticky or starchy. The key issue is timing, not just sugar quantity, because bacteria need fermentable carbs. Try to limit grazing, choose water with meals, and consider finishing carbs with a proper meal rather than holding them on the teeth all day.
Can cavities grow around or under existing fillings?
Yes, but the risk is usually highest at the filling margins where plaque can collect and where the interface may not perfectly seal over time. Practically, you should watch for new sensitivity or food trapping, and keep the same fluoride and flossing routine. If you suspect an old filling is failing, get an exam rather than trying to “wait it out.”
What should I do if I have dry mouth or take medications that reduce saliva?
If you have dry mouth, mouth breathing, or frequent reflux, you may need stronger or additional fluoride beyond basic toothpaste. Ask your dentist whether a prescription high-fluoride toothpaste, fluoride varnish, or a saliva plan fits your situation. Dry mouth conditions also change how quickly decay can progress.
When is tooth pain an emergency versus just a regular appointment?
If you get facial swelling, fever, trouble swallowing, or trouble breathing with tooth pain, treat it as an emergency because infection can spread beyond the tooth. Otherwise, persistent sensitivity lasting more than a couple of weeks, bleeding gums plus localized pain, or worsening pain when biting warrants prompt dental evaluation.
If I have a cavity, can I just manage it at home until I can get a filling?
Home care can slow progression, but it cannot physically close a cavitated hole. If a dentist recommends a filling, delaying usually increases the chance the treatment will get larger (more tooth loss and closer to the nerve). If you cannot get treated immediately, focus on strict fluoride use, reduce sugar frequency, and keep flossing so you do not accelerate the process.
Can dental sealants stop an existing cavity from getting bigger?
Sealants work on pits and fissures, mainly to prevent decay in molars, not to treat an existing cavity. If you already have a lesion, the dentist will decide whether sealing is appropriate or whether you need restoration. Still, sealants can be valuable on other at-risk teeth if you have a history of occlusal cavities.
Can teeth regrow from cavities? Learn what can remineralize early, what cannot, warning signs, and next steps.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn
Learn which teeth seem to grow twice: primary replaced by permanent, plus wisdom teeth timing and limits on regrowth

