If a chunk of your gum is missing, whether it grows back depends almost entirely on what caused the loss and how deep the damage goes. Small surface wounds, post-extraction tissue, and minor trauma ulcers can close on their own within one to three weeks. But gum that has receded from periodontal disease, aggressive brushing, or significant trauma does not simply grow back the way skin does. Once the deeper, attached gum tissue is lost, your body cannot rebuild it without help. Knowing which situation you're in makes all the difference.
Chunk of Gum Missing: Will It Grow Back?
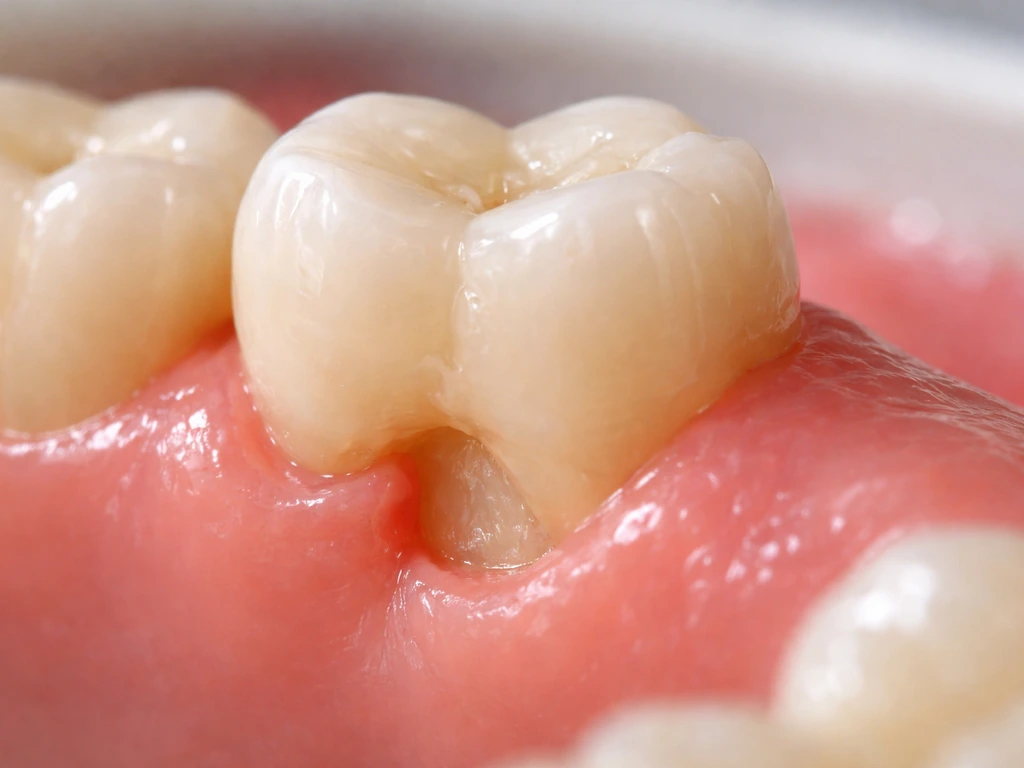
What 'missing gum' usually means
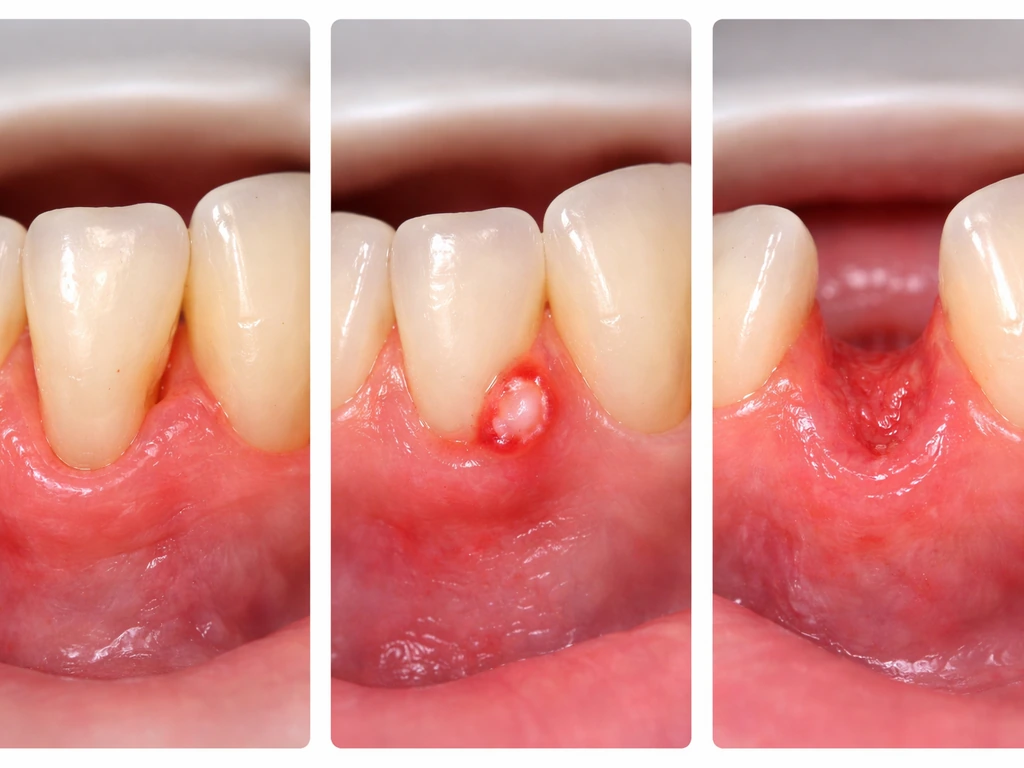
People use this phrase to describe several very different things, and the cause matters a lot for what happens next. Here are the most common scenarios you might actually be dealing with:
- Gum recession: The gumline has gradually crept down (or up on lower teeth), exposing part of the tooth root. The tooth looks longer than it used to. This is the most common meaning of 'missing gum.'
- Trauma or laceration: A blow to the mouth, a sharp food item, or a dental procedure tore or cut soft tissue, leaving a raw, open area.
- Post-extraction tissue loss: After a tooth is pulled, the socket area looks hollow or gum tissue appears to be 'missing' around the healing wound.
- Burn or chemical irritation: Hot food, aspirin held against the gum, or a harsh mouthwash can destroy the surface layer of tissue, making it look and feel like something is gone.
- A canker sore or ulcer: These look like craters in the gum and feel like missing tissue, but they are shallow surface ulcers that almost always heal on their own.
- Periodontal disease-related loss: Chronic gum disease destroys the attachment between gum and tooth over time, pulling the gumline away from the crown.
- Wisdom tooth area tissue: Partially erupted wisdom teeth often have a flap of gum tissue (the operculum) that tears or becomes inflamed, making the area look abnormal.
The single biggest clue to your situation: can you see the root of the tooth? If the tooth looks noticeably longer than its neighbors, or if you can see a yellowish surface below where the gumline should be, you are dealing with root exposure, and that needs professional attention. If the area just looks raw, red, or ulcerated but the tooth looks normal length, you are more likely dealing with a surface wound that may close on its own.
Will gum grow back on its own?
Here is where a lot of people get misled. Gum tissue is not like the skin on your arm. When you cut your arm, skin cells migrate in from the edges and rebuild the surface relatively quickly. Oral mucosa does actually re-epithelialize (close over the surface) faster than skin in many cases, which is why small mouth wounds often feel better within days. But that surface closure is not the same as true gum regeneration. Gum recession can look minor at first, but if your smiley areas are impacted, it is worth getting checked to see whether the tissue can be restored true gum regeneration.
True gum consists of keratinized, attached tissue firmly anchored to the bone and tooth root. When that tissue is lost, your body cannot spontaneously rebuild the full architecture of fibers, attachment, and keratinized tissue that was there before. This is one of the most important biological limits in dentistry: epithelium can close a wound, but it cannot regenerate lost periodontal attachment on its own.
What this looks like in practice:
| Scenario | Can it close/heal on its own? | Does it fully regenerate? |
|---|---|---|
| Canker sore / surface ulcer | Yes, usually within 1–2 weeks | Yes, surface heals completely |
| Minor burn or chemical irritation | Yes, re-epithelialization happens within days to a couple of weeks | Surface closes, but severe burns may scar |
| Post-extraction socket | Soft tissue closes by weeks 2–3; full healing takes months | Socket fills, but gum contour may change |
| Trauma laceration (small) | Often heals on its own if clean and uninfected | Surface heals; deep tears may need stitches |
| Gum recession from brushing | No, receded gum does not grow back | No spontaneous regeneration of attachment |
| Gum recession from periodontal disease | No, and it may worsen without treatment | Requires professional treatment for any coverage |
| Root exposed after trauma | Unlikely to recover without professional care | Needs treatment; exposed root won't self-resolve |
Age plays a role too. Younger people and children tend to heal faster and may have more resilient tissue. But even a teenager with recession from aggressive brushing is not going to grow that gum back without treatment. The biology just doesn't work that way at any age.
Normal healing vs. something that needs urgent care
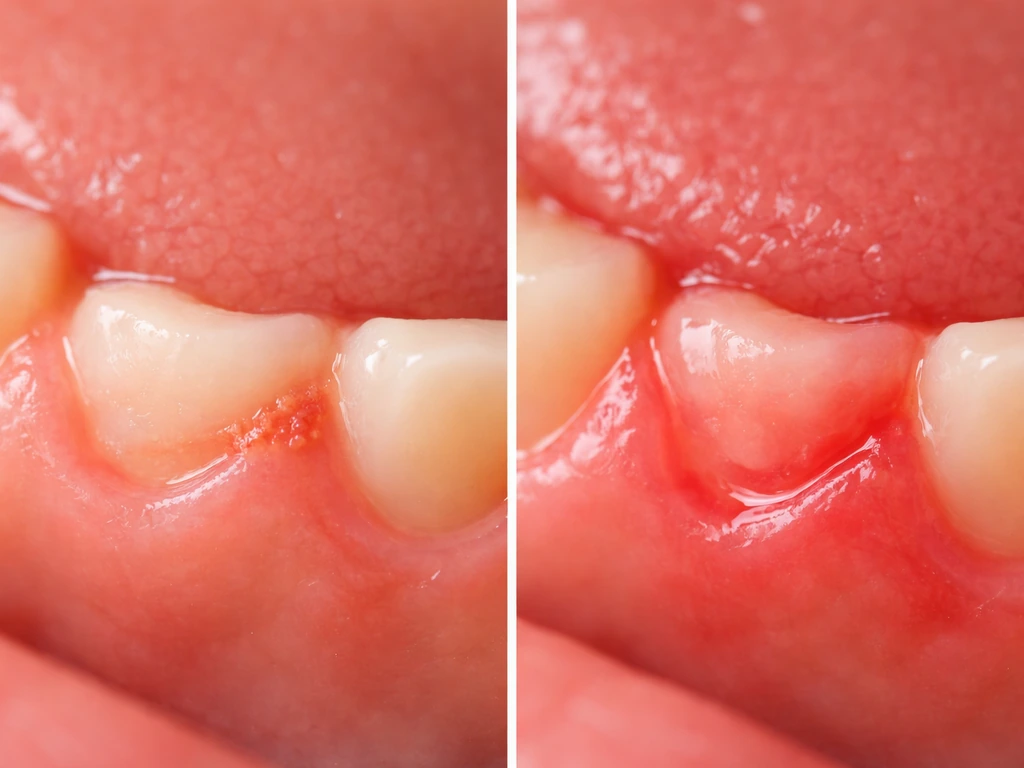
If you have an acute wound or a post-extraction site, your body should follow a predictable pattern. Inflammation peaks in the first 24 to 48 hours, meaning swelling, redness, and some pain are expected in that window. Over the following week, the inflammatory phase winds down and tissue starts closing over. By the end of the second or third week, soft tissue over an extraction socket or minor wound should be mostly closed. Gum tissue after an extraction can also be limited by how much attachment was lost, and it is not usually considered true regeneration extraction socket.
Signs that healing is on track:
- Steady improvement in pain and swelling after the first 48 hours
- The wound area looks smaller and less raw each day
- No significant discharge or smell
- Mild sensitivity that is improving, not getting worse
- After an extraction, the socket feels protected and there is no intense pain after day 3
Warning signs that need prompt dental attention:
- Intense, throbbing pain that gets dramatically worse around 2 to 3 days after an extraction (classic dry socket pattern)
- Spreading redness, swelling, or warmth in the jaw, face, or neck
- Pus, green or yellow discharge, or a foul taste you cannot explain
- Fever above 101°F (38.3°C)
- Visible tooth root that wasn't there before, or the tooth suddenly looking longer
- A wound that is not improving or is actively getting larger after a week
- Significant bleeding that doesn't slow down after 20 to 30 minutes of gentle pressure
If you can see the root of the tooth at all, that is not a 'wait and see' situation. Exposed roots don't resolve on their own. The research is clear on this: an exposed root won't get better unless it's professionally treated. Get to a dentist.
What you can safely do today at home
If you have just noticed the issue and you are not in one of the urgent-care categories above, here is what actually helps and what you should avoid.
Safe steps to take now
- Rinse gently with warm salt water: After the first 24 hours from any fresh wound or extraction, gentle warm salt-water rinses help keep the area clean without disrupting healing tissue. Mix about half a teaspoon of salt in a glass of warm water and swish gently — don't spit forcefully.
- Manage pain with appropriate medication: NSAIDs like ibuprofen (if you can take them) are well-supported for managing acute oral pain. Ibuprofen alone, or combined with acetaminophen, is the dentist-recommended first line for post-extraction and acute gum pain in adults and teens over 12.
- Keep the area clean but gently: Use a soft-bristled toothbrush and be very gentle around the affected site. Skipping hygiene altogether lets bacteria accumulate, which makes things worse.
- Protect a clot if you just had an extraction: Don't rinse at all for the first 24 hours. After that, start the gentle salt-water rinse routine. Avoid sucking motions (straws, smoking) that create negative pressure in the mouth.
- Monitor the size of the wound: Take a look each day. If it's getting smaller, you're heading in the right direction.
What to avoid
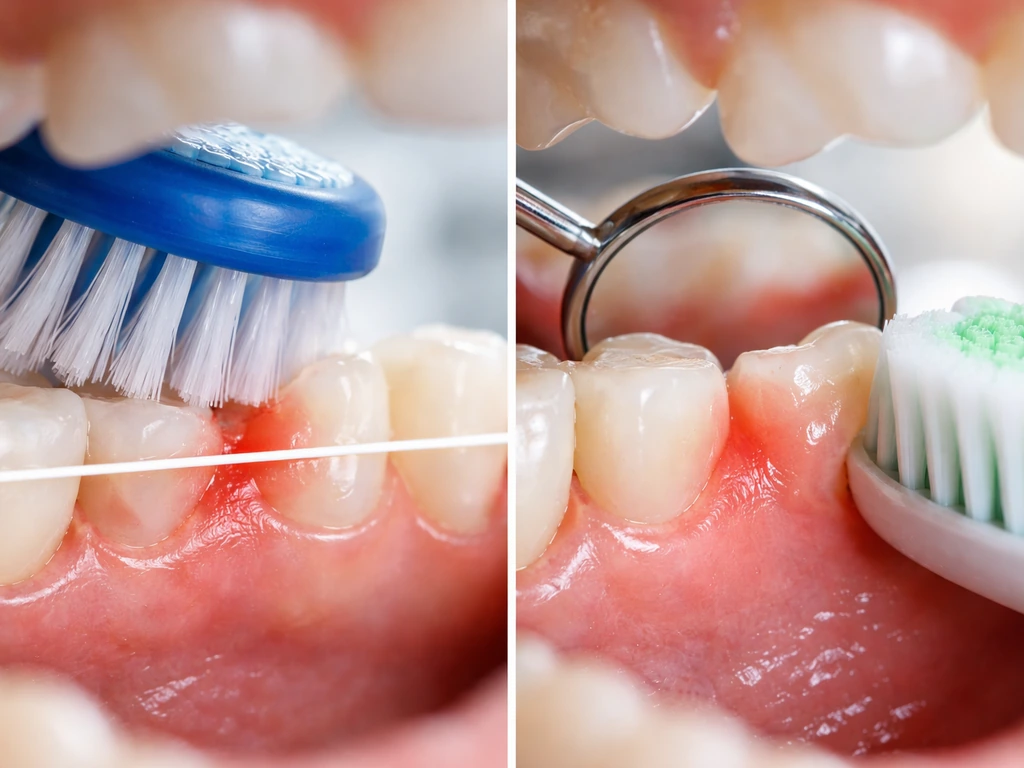
- Aggressive brushing or flossing directly over the wound — this tears healing tissue
- Holding aspirin against sore gum tissue — this causes a chemical burn and makes things worse
- Hot, spicy, or sharp-edged foods near the area
- Alcohol-based mouthwashes on fresh wounds — these are too harsh for healing tissue
- Poking, pressing, or picking at the area out of curiosity
- Smoking or vaping, which significantly impairs oral wound healing
- Waiting indefinitely if symptoms aren't improving
One important myth to kill here: rubbing vitamin E oil, aloe vera, or any other home remedy directly on a recession defect will not make the gum grow back. These things won't hurt you, but they have no meaningful effect on lost keratinized tissue or gum attachment. Don't let them substitute for getting real treatment.
Professional options when gum won't grow back enough on its own
If you have true gum recession, significant tissue loss, or a root that's exposed, this is where dentistry can actually help. The goal of professional treatment isn't always to perfectly recreate what was there before, it's to restore enough coverage, protection, and healthy attachment to function well and stop getting worse.
Treating the underlying cause first
Before any graft or surgery, a periodontist or dentist needs to address what caused the loss. If gum disease is the driver, that means scaling and root planing (a deep cleaning below the gumline), infection control, and getting inflammation under control. Operating on inflamed tissue doesn't work well. A thorough periodontal exam measuring probing depth, recession, attachment levels, and bleeding on probing tells the clinician what they're actually dealing with.
Gum grafting procedures
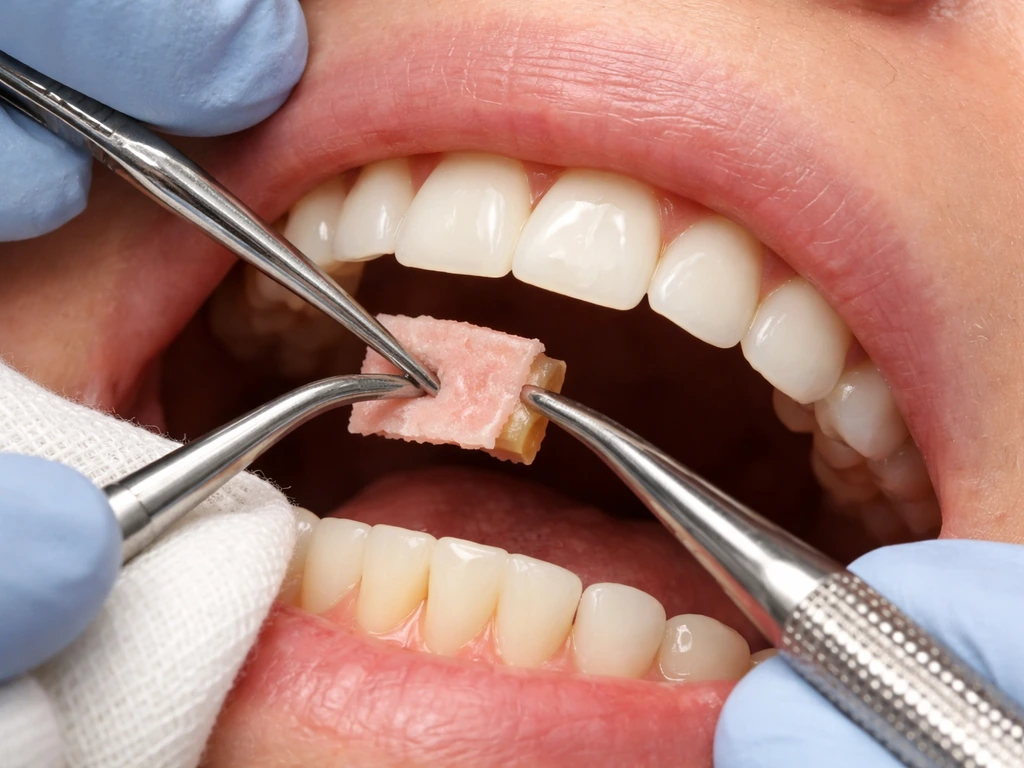
Gum grafting is the main surgical approach for restoring lost tissue. There are several techniques, and the right one depends on your specific defect:
- Connective tissue graft (CTG): The gold standard for root coverage. A small piece of connective tissue is taken from the roof of your mouth (palate) and placed under a flap of existing gum tissue at the recession site. Often combined with a coronally advanced flap (CAF), where the existing gum is carefully repositioned up over the root. Studies consistently show this combination achieves the best root coverage outcomes.
- Free gingival graft (FGG): A strip of tissue including the surface epithelium is taken from the palate and placed directly at the defect site. This is the standard choice when the goal is to increase the width of keratinized (firm, attached) gum tissue rather than cover a root. Less cosmetically ideal but very effective for building a stable tissue band.
- Pedicle graft: Uses existing gum tissue from next to the recession site, rotated or slid over the defect. Works well when there is enough adjacent tissue and no need for donor tissue from the palate.
- Acellular dermal matrix (ADM): A processed donor tissue alternative that avoids a second surgical site at the palate. Used alone or with CAF; outcomes are generally good but may be slightly less predictable than CTG in some studies.
- Guided tissue regeneration (GTR): Uses barrier membranes to encourage the body's own cells to rebuild attachment. More complex and typically reserved for specific defect types.
An important honest note: how much coverage is achievable depends heavily on the severity of the recession and how much interproximal (between the teeth) tissue is still present. Dentists use classification systems like Miller's classification to predict outcomes. Mild to moderate recession cases often achieve complete or near-complete root coverage. Severe cases, especially those with significant bone and tissue loss between the teeth, may only achieve partial coverage even with surgery.
If you have health conditions like uncontrolled diabetes or take immunosuppressive medications, healing after grafting is more unpredictable and your periodontist needs to know this upfront.
Healing timelines, what to realistically expect, and stopping it from getting worse
Healing time varies a lot by what you're dealing with, but here are realistic windows to plan around:
| Situation | Surface closure | Full healing |
|---|---|---|
| Minor ulcer or surface wound | 5–14 days | 2–3 weeks |
| Post-extraction socket (simple) | 2–3 weeks for soft tissue | Several months for complete resolution |
| Burn or chemical irritation | Days to 2 weeks | 2–4 weeks depending on depth |
| Gum graft surgery | 1–2 weeks for initial healing | 3–6 months for full maturation |
| Gum recession without treatment | Does not resolve | Likely to worsen over time without care |
The most important thing you can do to prevent the situation from getting worse is to fix whatever caused it. If recession came from brushing too hard, switch to a soft-bristled brush and use a gentle, circular technique. If gum disease is the driver, professional cleaning and a consistent home care routine are non-negotiable. If a habit like dipping tobacco or vaping is involved, those directly cause and accelerate tissue loss, and continuing them guarantees things get worse regardless of any other treatment. If you dip tobacco, it can also accelerate gum tissue damage and make recession worse over time dipping tobacco.
After gum graft surgery, the first two weeks are the most critical. The graft needs to stay still to establish blood supply, so you will be on a soft diet, avoiding brushing at the surgical site, and using prescribed rinses (often chlorhexidine) to control bacteria. Your periodontist will give you specific instructions, and following them closely is what separates good outcomes from poor ones.
The bottom line is this: small, surface-level gum wounds have a genuinely good chance of healing on their own if you keep the area clean and don't irritate it further. But lost, attached gum tissue from recession or disease doesn't just grow back. If you are wondering can gums grow back reddit-style, the key point is that lost, attached gum tissue from recession or disease does not simply grow back without treatment. If your tooth looks longer, if you're having sensitivity to temperature or touch on a root surface, or if a wound isn't improving after a week or two, get to a dentist or periodontist. The longer true recession sits untreated, the more tissue is lost and the harder it becomes to restore adequate coverage.
FAQ
If a small chunk of gum is missing, how long should I wait before seeing a dentist?
If the area is clearly a surface ulcer or minor trauma spot, it usually improves within 1 to 2 weeks. If you do not see clear shrinkage of the raw area by about 10 to 14 days, or symptoms are worsening (pain, bleeding, sensitivity), you should book a dental exam rather than waiting longer.
What is the fastest way to tell if this is just irritation or true gum recession?
Look for tooth length change. If the tooth appears longer than nearby teeth or you can see a yellowish root surface where the gumline should be, that points to recession or root exposure. Pure irritation tends to look raw without a visible shift in the gumline or tooth length.
Will gum grow back if I stop brushing hard and switch to a soft toothbrush?
Stopping trauma can prevent further loss, and minor surface wounds can heal. But if the missing tissue is attached, keratinized gum and the root is exposed, switching brushes alone rarely rebuilds the lost attachment, you usually need professional treatment to restore coverage.
Can sensitivity be a sign that the missing gum is not going to heal on its own?
Yes. Temperature or touch sensitivity often suggests the root surface is exposed, which typically will not resolve without treatment. Sensitivity that persists beyond a couple of weeks is a strong reason to get a periodontal evaluation.
Does chlorhexidine mouthwash help gum recession grow back?
Chlorhexidine can reduce bacteria and help healing of inflamed tissue, especially around wounds or after procedures. It does not regenerate attached gum or rebuild periodontal attachment on its own, so it should be viewed as supportive care, not a replacement for grafting when recession is present.
I pulled out a food stuck to my gum and now there is a sore spot. Should I worry about long-term missing gum?
A sore spot after minor trauma can heal, particularly if the gumline did not move and you cannot see the root. Still, if the area bleeds easily, looks like a persistent ulcer, or does not start improving within 1 to 2 weeks, an exam is warranted to rule out deeper attachment loss.
If gum grafting is needed, will it work better if I wait for it to heal first?
Your clinician usually treats the cause first and measures the defect after inflammation settles. In many cases they can graft after controlling infection or periodontal inflammation, but the exact timing depends on probing depth, bleeding on probing, and overall gum health, so waiting too long without evaluation can reduce options.
Can vitamin E oil, aloe, or salt water help a recession defect heal?
They may soothe irritation and support general oral comfort, but they do not meaningfully recreate keratinized, attached gum or periodontal attachment. For true recession, the decision point is whether you have root exposure or lost attachment, and those usually require dental treatment.
Does age change whether gum can regrow?
You may heal faster when younger, but the biological limitation is about tissue type. Even if a wound closes, that is not the same as regrowing attached gum and fiber attachment, so age does not eliminate the need for grafting when true recession is present.
Will bleeding gums automatically mean my missing gum will grow back?
Bleeding often indicates active inflammation, not spontaneous regeneration. If bleeding is present with recession or root exposure, you generally need periodontal therapy (deep cleaning, infection control, and improved home care) rather than waiting for the bleeding to stop on its own.
How do diabetes or immunosuppressive medications affect healing if I get a graft?
They can make healing less predictable and increase the risk of delayed recovery or complications. Tell your periodontist about medication doses and blood sugar control upfront, because your timeline, infection-prevention plan, and post-op instructions may need to be adjusted.
Is there anything I should do immediately if I think the missing gum is from brushing injury?
Switch to a soft-bristled brush and gentle technique right away, avoid picking at the area, and keep the area clean. If the gumline looks lower, the tooth looks longer, or you can see root, treat it as recession and schedule an evaluation rather than assuming it will fully reverse.

Find out if a torn tooth or gum will regrow, what heals in days, what won’t, and when to see an emergency dentist.
Timeline for gum healing after recession or injury, factors affecting regrowth, and when you need dental care
Can milk teeth grow twice? Learn why baby teeth usually only get replaced, not regrown, and what to do if one falls out

