Here's the short answer: gums can heal and recover, but whether they truly "grow back" depends entirely on what happened to them in the first place. If your gums are swollen, irritated, or inflamed from gingivitis or minor trauma, yes, they can return to normal relatively quickly, often within one to three weeks of better oral hygiene. But if you have actual gum recession, where the gum tissue has pulled away from the tooth and attachment has been lost, that tissue does not simply regrow on its own. Understanding which situation you're in changes everything about your timeline and your next steps.
How Long Does It Take for Gum to Grow Back?
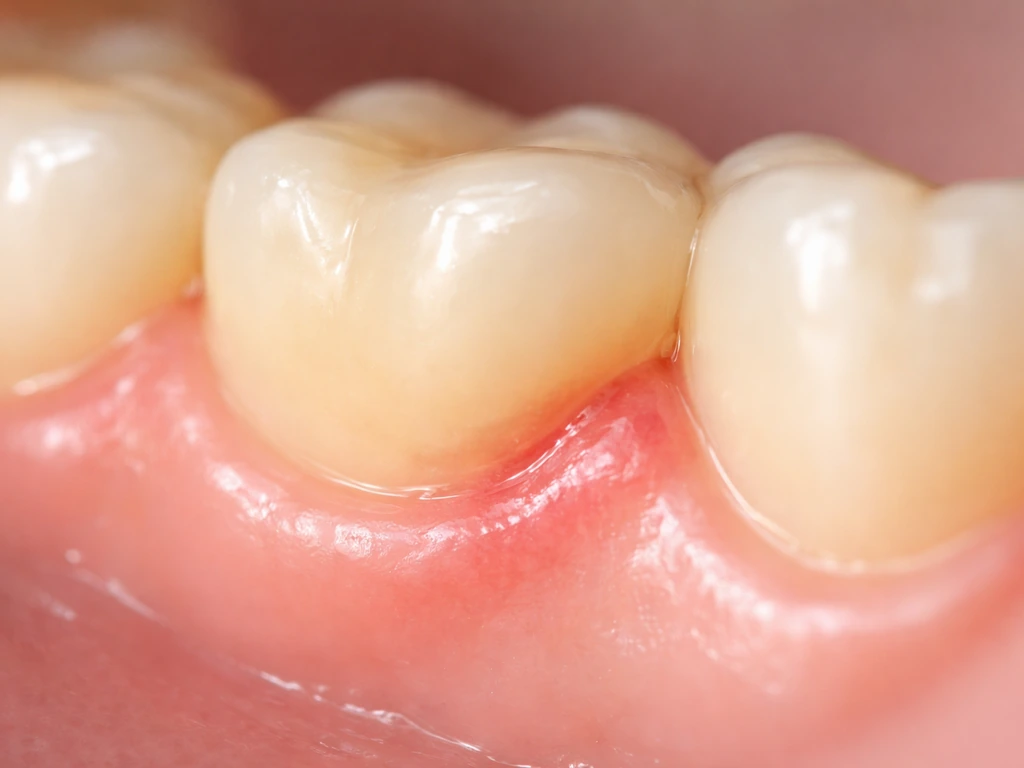
What "gum regrowth" really means
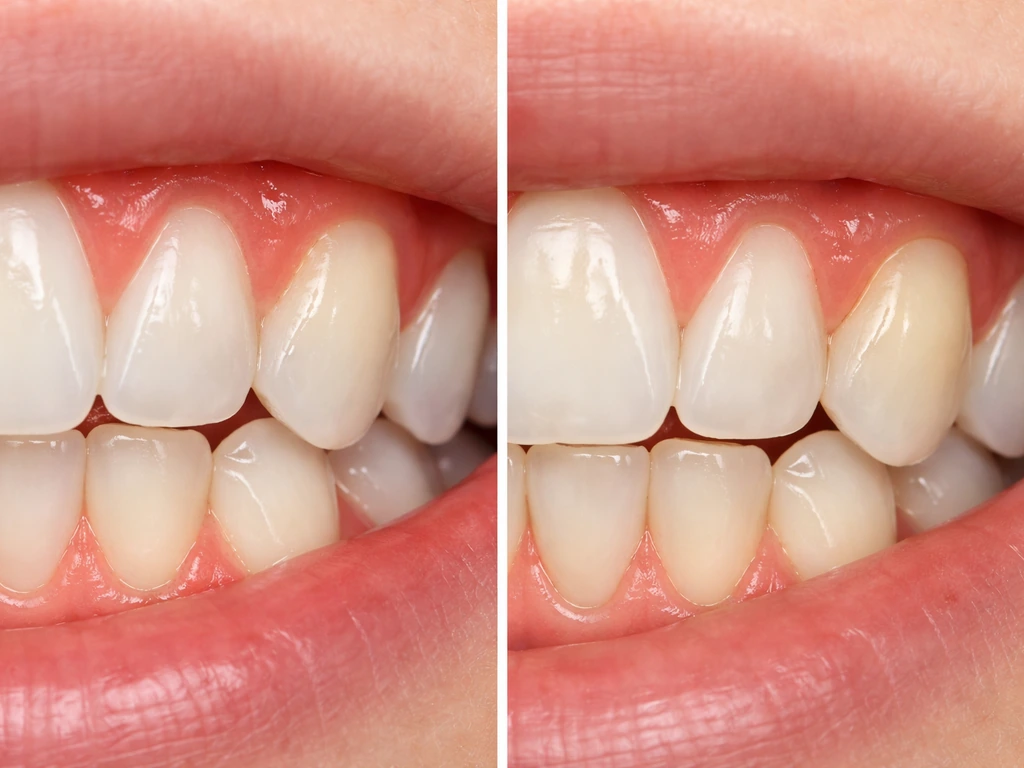
Most people searching this question are picturing one of two very different things. The first is gum tissue that's swollen, red, or puffy from inflammation, basically gums that have expanded or look different because of irritation. When that inflammation goes away, the gums "shrink back" to their normal position, and it can feel like they've grown back or returned to normal. The second scenario is true gum recession, where the gum margin has migrated downward (or upward on upper teeth), exposing more of the tooth root. That's a structural loss of tissue, not just swelling.
These two situations have completely different answers. Inflamed gums can recover well with good home care. Receded gums generally cannot regenerate on their own because the body doesn't replace lost gum tissue the way it heals a cut on your skin. This is the core biological reality this whole article is built around, and it's the most important thing to understand before anything else.
Typical healing timelines by cause
Gingivitis and general gum inflammation
Gingivitis is the most reversible gum condition there is, and the timeline for improvement is actually pretty encouraging. In clinical studies using experimental gingivitis models, where researchers have people stop brushing and flossing for three weeks (to induce gingivitis), and then resume normal oral hygiene, bleeding indices begin to reverse within about a week of resuming care. Most clinical signs, including bleeding on probing, reduce measurably within two to three weeks of consistent oral hygiene. So if you've been slacking on brushing and flossing and your gums are red, swollen, and bleeding, you can expect to see real improvement within one to two weeks, and noticeable recovery within three weeks, if you're genuinely consistent.
After scaling and root planing (deep cleaning)
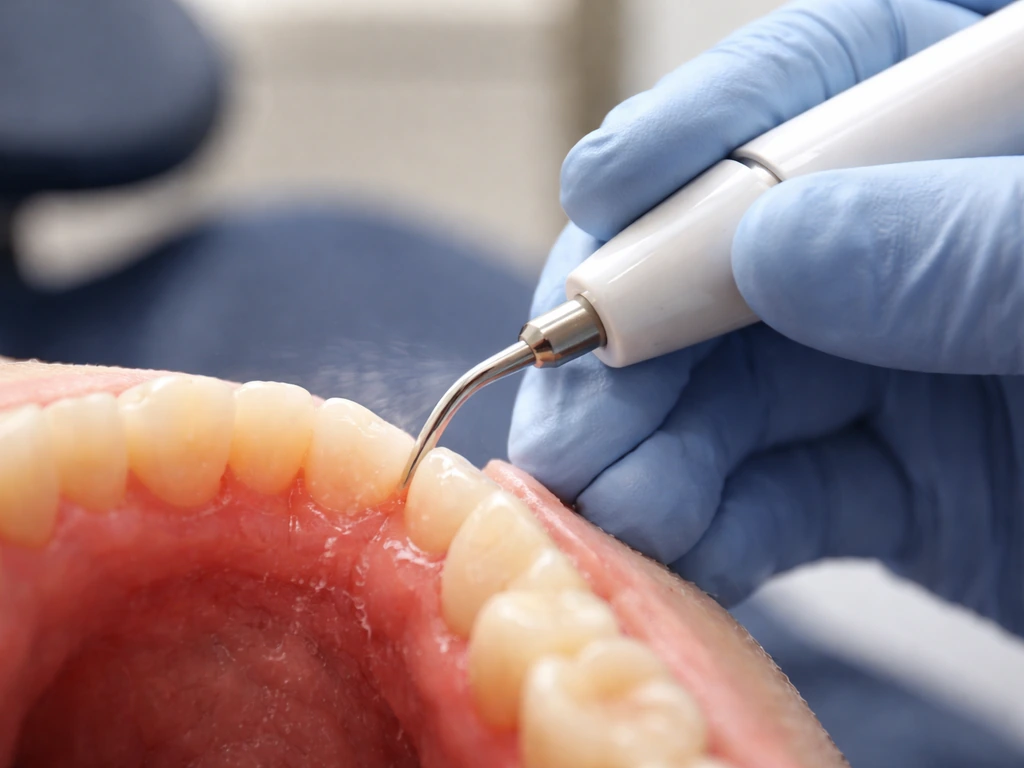
If your dentist or periodontist has done non-surgical periodontal therapy like scaling and root planing, the ADA notes that periodontal tissues require approximately four weeks to show the optimal effects of that treatment. Your dentist will typically schedule a re-evaluation around that four-week mark to check pocket depths and see how the tissue has responded. Don't be discouraged if you're still tender in the first week or two; that's normal.
Minor gum trauma (biting yourself, sharp food, etc.)
Small cuts or abrasions to the gum tissue, from biting your cheek, a sharp chip, or a rogue popcorn kernel, typically heal within seven to fourteen days. The oral mucosa is actually one of the fastest-healing tissues in the body due to its blood supply and the presence of saliva, which contains healing compounds. You'll notice the sharp pain fading in two to three days and the area looking more normal within a week to ten days. If something isn't healing in that window, that's a signal to get it checked.
After a tooth extraction
Gum tissue closure over an extraction socket typically takes around seven to twenty-one days, though this varies significantly based on the size of the extraction and whether it involved any surgical component. If you've ever wondered specifically about whether gum tissue grows back after a tooth is pulled, the answer is that the soft tissue seals over the socket, but the bone and deeper structures underneath take months to fully remodel. The gum surface closing is not the same as full healing beneath it.
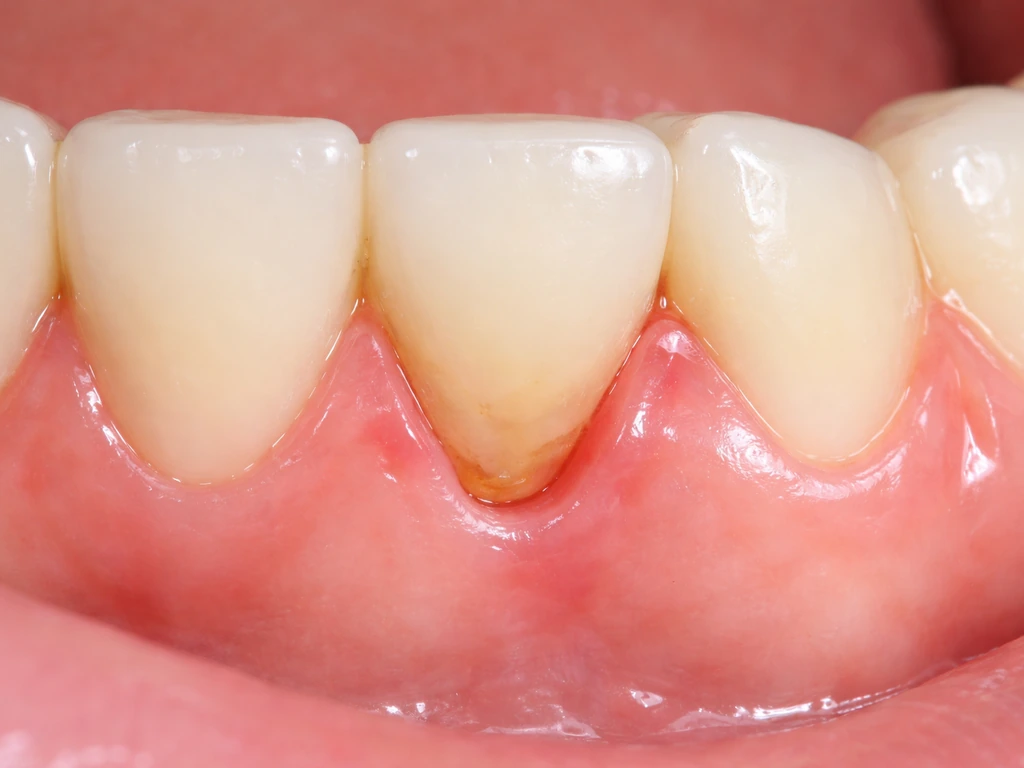
Gum recession from periodontal disease
This is where timelines get more sobering. Once recession has occurred from periodontitis or long-term attachment loss, it does not reverse on its own, period. Treatment can stop it from getting worse, and professional procedures (discussed below) can restore coverage, but there's no at-home regimen that will bring receded gum tissue back. If someone told you that brushing gently for a few months will regrow your gums, that's a myth worth busting clearly and early.
| Cause | First Signs of Improvement | Meaningful Recovery Timeline |
|---|---|---|
| Gingivitis (mild) | 3–7 days | 1–3 weeks with consistent home care |
| Gingivitis (established) | 1–2 weeks | 3–6 weeks with professional cleaning + home care |
| Minor gum trauma | 2–4 days | 7–14 days |
| Post-extraction gum closure | 3–5 days (clot) | 7–21 days (surface closure); months for full healing |
| Post-scaling and root planing | 1–2 weeks (symptom relief) | ~4 weeks for optimal tissue response |
| Gum recession (mild) | Does not reverse on its own | Requires professional treatment; outcomes tracked at 3–6 months |
| Gum recession (moderate/severe) | Does not reverse on its own | Graft surgery outcomes tracked at 3–6 months and beyond |
Factors that affect how fast gums heal
Not everyone heals on the same schedule, and several factors push the timeline one way or the other. Smoking is one of the biggest. Research using NHANES III data found that smoking may account for more than half of periodontitis cases among U.S. adults, and tobacco use consistently impairs the immune and vascular responses that gum healing depends on. If you smoke and are asking whether your gums will grow back, the honest answer is: your timeline is significantly longer, and your outcomes are worse across the board.
Diabetes is another major factor. The American Diabetes Association has long documented that people with diabetes are more likely to develop serious gum disease, and that the relationship runs both ways: poor glycemic control makes gum disease worse, and gum infections can affect blood sugar. If your diabetes is poorly managed, gum healing will be slower and less complete.
Age matters too, though it's not a dealbreaker. Tissue repair generally slows with age, which means a 60-year-old may need more time to see the same improvement a 30-year-old sees. Medications are another consideration: anticoagulants, for example, can increase gingival bleeding tendency, which can complicate your perception of whether things are improving or worsening.
- Smoking: significantly impairs gum healing and increases recession and attachment loss risk
- Poorly controlled diabetes: slows healing and worsens inflammation
- Age: older adults typically heal more slowly
- Oral hygiene consistency: the single most controllable factor for inflammation-based gum issues
- Severity of recession or disease: deeper pockets and more attachment loss mean longer or incomplete recovery without professional help
- Medications: blood thinners, certain antihypertensives, and immunosuppressants can all affect gum health and healing
- Orthodontic history: tooth movement can be associated with recession in some cases, which affects the tissue you're starting with
What you can do right now at home
If your issue is inflammation-based (swollen, red, or bleeding gums), you actually have a lot of control. Start with the basics: brush gently twice a day with a soft-bristled toothbrush and add daily flossing if you're not doing it already. The ADA notes that adding interdental cleaning to brushing produces a statistically significant reduction in gingivitis measures, even in short-term studies. The catch: flossing only works if you actually do it. If you skip it, you're leaving the plaque between your teeth untouched, and that's exactly where gingivitis tends to get its foothold.
A warm salt-water rinse is genuinely useful in the early healing phase, especially after minor trauma or after a procedure. Research comparing salt-water rinses to chlorhexidine mouth rinse after minimal-invasive periodontal surgery found similar anti-inflammatory effects between the two, which says a lot about how effective something as simple as warm salt water can be. Mix about half a teaspoon of salt in a cup of warm water and rinse gently for thirty seconds, two or three times a day.
Avoid anything that irritates the tissue further during healing. That means no aggressive brushing (more pressure does not equal more clean), no picking at the area with your fingernail or a sharp object, and if you use tobacco, stopping or reducing will have a meaningful impact on your healing speed. People who chew tobacco or dip specifically should know that gum recession from dipping is a real and documented problem, and the tissue that's already gone won't come back on its own.
If you have a piercing in or near your mouth and notice gum changes, it's worth knowing that oral piercings can cause direct trauma to gum tissue over time. Whether a torn smiley piercing area will heal depends on the extent of the tissue damage and how the area is managed afterward.
When to see a dentist or periodontist
For mild gingivitis, improved home care often handles it, but you should still see a dentist if things don't improve within two to three weeks, or sooner if you notice any red flags. A professional cleaning removes calculus (hardened plaque) that brushing and flossing simply cannot touch, and that calculus is often the barrier preventing gum healing.
Go sooner rather than later if you notice any of the following:
- Gums that bleed every time you brush, even after two or more weeks of better oral hygiene
- Swelling, pus, or a bump on the gum that looks like a blister (this could be a periodontal abscess, which needs prompt treatment)
- Gums that are visibly pulling away from your teeth or teeth that look longer than they used to
- Persistent pain or sensitivity along the gumline
- Loose teeth or a change in how your bite feels
- Fever or significant facial swelling, which may signal a spreading infection requiring urgent care
When you see a periodontist, they'll measure your pocket depths and clinical attachment level (CAL), which combines pocket depth and any recession to give a full picture of where your attachment actually sits. They'll also check for bone loss on X-rays and assess whether you're dealing with gingivitis (reversible) or periodontitis (requires active management). The distinction between the two is critical for understanding your realistic timeline and what treatment is appropriate.
Some people first start researching their gum situation based on threads they've read online. If you've been scrolling through what people say about gum regrowth on Reddit, you'll find a wide range of personal experiences, but the pattern that holds up consistently is this: mild cases improve with care, and established recession doesn't reverse without professional intervention. User anecdotes can be reassuring or alarming depending on the thread, but they're not a substitute for a clinical evaluation.
If gums don't fully grow back: what dentists can actually do
When true recession is present and won't resolve on its own (which, again, is the norm rather than the exception), there are evidence-based treatments that can restore gum coverage. These are not experimental, they're well-established procedures with tracked outcomes.
Non-surgical periodontal therapy
Scaling and root planing is often the first line of treatment for periodontitis. It removes plaque and calculus from below the gumline and smooths the root surface to help the tissue reattach. This won't reverse recession, but it stops disease progression and reduces pocket depths. After this treatment, the ADA recommends life-long supportive periodontal care to prevent recurrence, which means regular follow-up cleanings (often every three to four months instead of every six).
Gum grafting
For actual recession, the gold standard is a connective tissue graft, where tissue (usually taken from the roof of the mouth) is placed over the exposed root to restore coverage. Long-term studies have followed patients for up to twenty years after connective tissue grafts and guided tissue regeneration procedures, and the outcomes show durable results when the underlying periodontal disease is well-controlled. Clinical outcomes from graft procedures are typically assessed at three and six months post-surgery, with further stability checks over the following year.
One interesting post-graft phenomenon is called creeping attachment, where the gum margin continues to move coronally (toward the crown of the tooth) in the months after surgery, sometimes adding additional coverage beyond what was immediately apparent at the three-month check. This is a real and documented occurrence, not just wishful thinking, but it's unpredictable and not guaranteed.
There are also alternatives to autogenous (your own tissue) grafts, including porcine-derived acellular dermal matrix and collagen matrix materials. Randomized trials have compared these to connective tissue grafts with outcomes measured at three and six months. They tend to produce slightly less root coverage on average but spare the patient a second surgical site (the palate), which affects recovery comfort significantly.
It's also worth knowing that if you've lost a chunk of gum tissue from trauma or another cause, the biological limits are the same: whether a missing piece of gum will grow back on its own depends on how much was lost and whether the underlying attachment is intact. A small superficial loss may heal; a larger or deeper loss may need grafting to fully restore.
Guided tissue regeneration
Guided tissue regeneration (GTR) uses a barrier membrane placed during surgery to encourage the right tissues to repopulate the root surface. It's used in specific situations, particularly where bone loss has also occurred, and its outcomes have been tracked at six months and up to thirty-six months in published case series. It's a more complex procedure typically reserved for patients with specific anatomic situations.
Myth-busting: what gums can and cannot do
Let's be direct about the most common misconceptions floating around online and in dental waiting rooms.
Myth: "If I brush and floss consistently for a few months, my receded gums will grow back." This is false. Good oral hygiene can stop recession from worsening and can resolve gingivitis-related swelling, but it cannot regenerate tissue that has structurally receded. The fibers that attach gum tissue to the tooth (the periodontal ligament) and the cells that maintain them do not spontaneously regenerate a new gum margin once recession has occurred. You're not going to brush your way back from a 3mm recession.
Myth: "Oil pulling, aloe vera, or special toothpastes will regrow my gums." There is no clinical evidence that any over-the-counter product or home remedy reverses true gum recession. These products may support gum health generally or reduce inflammation, but they are not substitutes for professional evaluation and treatment.
Myth: "My gums grew back after I started flossing, so recession is reversible." What most people experience in this case is the resolution of inflammation-related swelling. Inflamed gums are puffy and may partially cover the tooth differently than healthy gums. When the inflammation resolves, gums look and feel healthier, and teeth may appear less exposed. This is a good outcome, but it's not the same as growing back receded tissue.
Myth: "Stem cell treatments will soon let gums regrow naturally." This is an area of active research, but the current evidence is cautious. A systematic review and meta-analysis on stem-cell-based periodontal regeneration therapies found improved clinical attachment level and probing depth outcomes compared to cell-free controls, but reported no statistically significant effect on gingival recession itself. The science is promising but not yet a practical solution you can access today.
The truth is that gum tissue sits in a unique biological category: it can heal from inflammation and minor trauma remarkably well, but it doesn't regenerate structural tissue the way, say, your liver does. The sooner you accept that distinction, the sooner you can stop waiting for something that won't happen on its own and take steps that actually work, whether that's locking in your home care routine, scheduling a periodontal evaluation, or exploring graft options with a specialist.
FAQ
If my gums look better after a couple weeks, does that mean recession is reversing?
Not necessarily. Improvement in color, bleeding, and tenderness often reflects reduced inflammation and less swelling, or better gum positioning. True recession means attachment has shifted and root exposure remains, which usually will not “undo” with hygiene alone, so ask your dentist to measure recession depth or document it with periodontal charting.
How long should I wait after starting better brushing and flossing before I see results?
For inflammation-based problems, you should usually notice reduced bleeding and less puffiness within 1 to 3 weeks of consistent care. If bleeding does not improve by about the 2 to 3 week mark, or if symptoms worsen, that is a sign you likely need professional cleaning and an assessment for periodontitis.
What is the difference between gum tissue healing and gum regrowth?
Healing means the tissue settles, swelling goes down, and minor wounds close. Regrowth, in the true recession sense, would mean rebuilding lost attachment and root coverage, which generally requires periodontal procedures. If the gum margin has permanently migrated, home care cannot rebuild that missing structure by itself.
Can a dentist tell in one visit whether my gums will regrow on their own?
They can often estimate reversibility quickly using measurements like pocket depth, clinical attachment level, and the pattern of gum migration. However, deciding the right timeline and treatment typically depends on whether inflammation versus true attachment loss is driving your symptoms, which may require a re-evaluation after initial therapy or cleaning.
Does scaling and root planing make receded gums grow back?
It usually does not regenerate lost gum tissue, but it can reduce pocket depth and stop progression by removing plaque and calculus and smoothing the root. Many patients notice less bleeding and inflammation, but recession itself generally needs targeted gum coverage procedures if root is truly exposed.
How long does it take to know whether a gum graft or regeneration procedure “worked”?
Clinicians usually check early healing around 3 and 6 months, because initial coverage can continue to improve later in some cases. If creeping attachment occurs, additional coverage can appear after the first few follow-ups, but results are not guaranteed and depend on disease control.
If I smoke, how much longer will gum healing take, and will treatment still work?
Smoking commonly slows healing because it impairs blood flow and immune responses. That can mean slower symptom improvement and higher risk of persistent disease. Treatment can still help, but outcomes are generally less predictable, so cessation improves both speed and durability.
Can diabetes change the timeline for gum repair?
Yes. Poor glycemic control is linked with higher risk of periodontitis and can slow healing and tissue response. If you have diabetes, coordinating with your clinician to improve blood sugar control can make periodontal treatment outcomes more complete and reduce recurrence risk.
Is gentle brushing always safe, or can aggressive brushing cause recession?
Aggressive brushing can contribute to trauma and worsen gum recession, especially if you use hard bristles or scrub horizontally. Switching to a soft brush and improving technique helps prevent further damage, but it will not rebuild established recession without periodontal intervention.
If my gums bleed when I floss, should I stop flossing?
Usually no. Bleeding often reflects inflammation, and stopping flossing can leave plaque behind and prolong gingivitis. The better approach is gentle daily interdental cleaning, using a technique that does not snap into the gumline, and getting a professional cleaning if bleeding persists.
Are there situations where gum changes after a cut or burn do not heal normally?
Yes. If pain or tissue appearance is not improving within about a week or two for minor trauma, or if there is spreading swelling, pus, fever, or worsening odor, you should get checked. Delayed healing can indicate infection, ongoing irritation, or an issue that needs targeted care.
How soon after an extraction should I expect the gum to cover the socket?
Soft tissue closure commonly takes about 1 to 3 weeks, but deeper remodeling continues much longer. If you have increasing pain after initial improvement, foul taste, or visible bone exposure that persists beyond expected healing, contact your dentist because complications like delayed healing or infection may be involved.
Can a mouth piercing cause recession, and does it heal if I remove the jewelry?
Piercings can chronically irritate or traumatize gum tissue. Removing or adjusting the jewelry may improve inflammation, but the amount of recovery depends on how much attachment has been disrupted. A periodontist can measure recession and determine whether grafting is needed for lasting coverage.
Do any supplements, oil pulling, or special toothpastes regrow receded gums?
They have not been shown to regenerate true recession. Some may reduce inflammation or support oral health, but they are not substitutes for diagnosing whether you have gingivitis versus periodontitis and for using evidence-based treatment when attachment loss is present.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

