Yes, certain tumors can grow structures that contain real dental tissues, including enamel, dentin, cementum, and pulp. In some rare cases, those structures look and function very much like actual teeth. But here's the important distinction: this is not the same as a tumor regenerating a tooth for you. These growths are abnormal, often benign, and require medical evaluation. If you've stumbled across alarming claims online about tumors sprouting teeth, the reality is both more nuanced and less scary than the headlines suggest.
Can Tumor Grow Teeth? What Dental-Like Growth Means
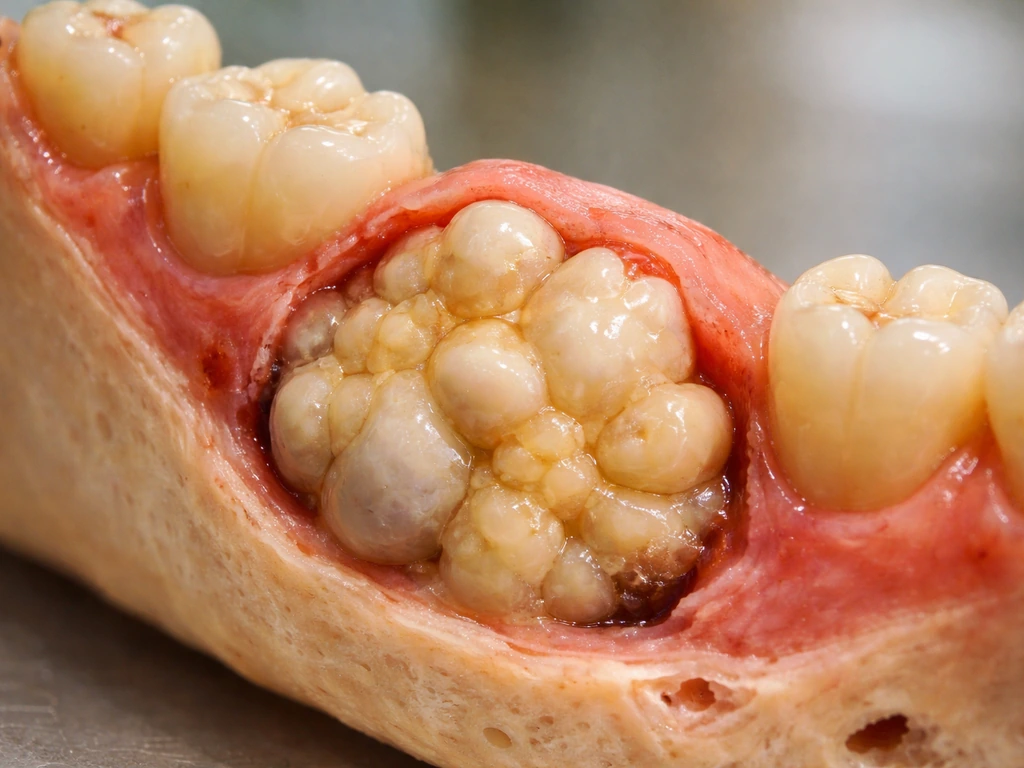
What "growing teeth" actually means in a tumor
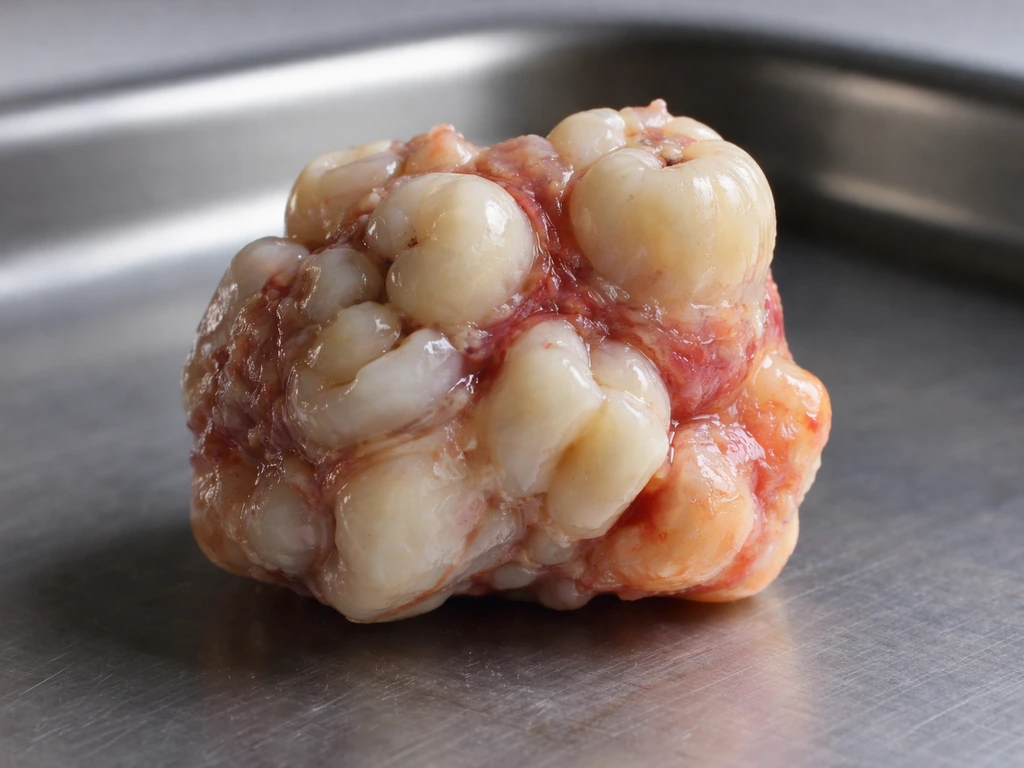
When people ask whether a tumor can grow teeth, they usually mean one of two very different things. The first is whether a tumor can produce fully organized, functional teeth, complete with a crown, root, and all layers of dental tissue in proper arrangement. The second is whether a tumor can produce calcified, tooth-like material that looks like a tooth on an X-ray or under a microscope but isn't a functional tooth in the traditional sense.
Both happen, and it depends entirely on the tumor type. Compound odontomas, for example, are composed of enamel, dentin, cementum, and pulpal tissue organized into small, discrete tooth-like units called denticles. These are arguably the closest a tumor gets to "growing a real tooth." Complex odontomas contain the same dental tissue components but in a disorganized, irregular mass rather than a recognizable tooth shape. Malignant odontogenic tumors, on the other hand, may produce dentin-like material (called dentinoid) without forming anything resembling a tooth at all.
How teeth normally form in the body
To understand why tumors can sometimes produce tooth-like tissues, you need a quick picture of how teeth form during normal development. Tooth development starts with a tightly coordinated conversation between two tissue types: dental epithelium and dental mesenchyme. The process moves through well-defined stages, from a thickened bud of cells, through cap and bell stages, to eventual mineralization and eruption.
Several molecular signaling pathways orchestrate this whole process. Wnt/beta-catenin signaling plays an essential role in activating the odontogenic mesenchyme (the tissue that will become the inner part of the tooth), while BMP, FGF, and Sonic hedgehog (SHH) pathways work in concert to regulate the differentiation of specialized cells: ameloblasts (which form enamel) and odontoblasts (which form dentin). The root itself is shaped by a structure called Hertwig's epithelial root sheath, which extends apically from the enamel organ and controls root formation. When these pathways work together in the right sequence, you get a properly formed tooth. When that signaling is disrupted or ectopically activated in tumor tissue, you can get a partial or disorganized version of the same process.
Why tumors can produce tooth-like structures
The short answer is that some tumor cells retain, or inappropriately reactivate, the same developmental programs that build teeth in embryos. Odontogenic tumors arise from remnants of the dental lamina, enamel organ, or odontogenic ectomesenchyme, which are the exact tissues that drive normal tooth development. Because these cells still carry the genetic machinery for tooth formation, they can, under the right (or wrong) conditions, begin differentiating into odontoblasts and ameloblast-like cells and producing dental hard tissues.
This is also why understanding why teratomas grow teeth is so relevant here. Teratomas are germ cell tumors that can contain tissues from all three embryonic germ layers, including primitive cells capable of differentiating into almost anything, including tooth-forming tissues. A published case report of an oral teratoma in a 9-year-old girl described, on surgical excision, tissues that included structures resembling a developing tooth, which is a striking illustration of how ectopic activation of developmental programs in tumor tissue can produce dental components far outside the jaw's normal development.
For odontogenic tumors specifically, the explanation is even more direct. Benign odontogenic tumors are classified based on which component of the tooth germ gives rise to them: epithelial, mesenchymal/ectomesenchymal, or mixed. A tumor arising from mixed odontogenic tissue has the cellular machinery to produce both enamel and dentin, which is why compound odontoma can generate multiple organized, tooth-like structures. Malignant variants, like odontogenic carcinosarcoma with dentinoid, can also produce dentin-like hard tissue, though in a far less organized way.
Which tumor types are actually linked to tooth-like growth
Not every tumor that grows near your jaw or mouth will produce dental tissues. The ones most strongly associated with tooth-like growth are odontogenic in origin, meaning they arise from the same tissues that build teeth. Here are the main players:
- Compound odontoma: The most organized type. Produces multiple small denticles (tooth-like units) with properly arranged enamel, dentin, cementum, and pulp. These are almost always benign and are among the most common odontogenic tumors found in the jaws.
- Complex odontoma: Contains the same dental tissue components as compound odontoma but in a haphazard, disorganized mass. Radiographically it can appear as a dense, calcified lesion rather than identifiable tooth-like shapes.
- Teratoma (especially oral/head-neck): Can contain tissues resembling developing teeth, depending on which germ layers are represented. This is less predictable than odontomas because teratomas can incorporate any tissue type.
- Calcifying ghost cell odontogenic cyst (Gorlin cyst): Produces ghost cells and calcified/dentinoid material, but this is distinct from organized tooth formation. The calcification here results from a ghost-cell mechanism rather than true odontogenic differentiation.
- Odontogenic carcinosarcoma with dentinoid: A rare, malignant tumor that can produce dentin-like hard tissue (dentinoid) alongside odontogenic epithelium, but without the organized structure of a true tooth.
- Ameloblastoma: A locally aggressive benign tumor of enamel organ origin. It typically does not produce dental hard tissues, but it arises from the same epithelial source as tooth-forming cells.
- Adenomatoid odontogenic tumor and other mixed-origin lesions: Can occasionally show calcified/enamel-like deposits depending on their cellular composition.
It's also worth noting that cysts can grow teeth too, particularly when they're odontogenic in origin or are associated with impacted teeth. The distinction between an odontogenic cyst and an odontogenic tumor matters clinically because their behavior, recurrence risk, and treatment differ significantly.
A side-by-side look at the main tumor types
| Tumor Type | Dental Tissues Produced | Organized Like a Tooth? | Benign or Malignant | Common Location |
|---|---|---|---|---|
| Compound odontoma | Enamel, dentin, cementum, pulp | Yes (multiple denticles) | Benign | Anterior maxilla |
| Complex odontoma | Enamel, dentin, cementum, pulp | No (disorganized mass) | Benign | Posterior mandible |
| Oral teratoma | Variable (teeth/tooth-like tissue possible) | Partially | Can be benign or malignant | Head/neck region |
| Calcifying ghost cell odontogenic cyst | Dentinoid/calcified material | No | Usually benign | Jaw (anterior) |
| Odontogenic carcinosarcoma | Dentinoid (dentin-like) | No | Malignant | Jaw |
| Ameloblastoma | Typically none | No | Benign (locally aggressive) | Posterior mandible |
Symptoms and red flags worth taking seriously
Many odontogenic tumors, especially odontomas, are found incidentally on routine dental X-rays because they don't always cause pain. But there are symptoms that should prompt you to get evaluated sooner rather than later. A sore or lump in your mouth that doesn't improve within two weeks, red or white patches on your gums or oral lining, unexplained bleeding, jaw swelling, loose teeth without an obvious cause, and persistent numbness or pain are all warning signs that warrant a dental or medical visit.
If you notice facial swelling alongside fever or difficulty swallowing, that's an emergency, not a "wait and see" situation. Infections and some aggressive tumors can spread beyond the jaw into the throat and neck, and that kind of spread needs urgent care. Oral and maxillofacial surgeons recommend that if symptoms like persistent mouth sores or swelling have been present for several weeks or longer, you stop waiting and get evaluated. The earlier these lesions are found, the simpler the management typically is.
Also worth mentioning: if you have an impacted tooth that hasn't erupted and your dentist finds a lesion around it on X-ray, that lesion could be a dentigerous cyst or an associated odontoma. These are genuinely common findings, especially around wisdom teeth and unerupted canines in younger patients, and they're very manageable when caught early.
What diagnosis and treatment actually look like
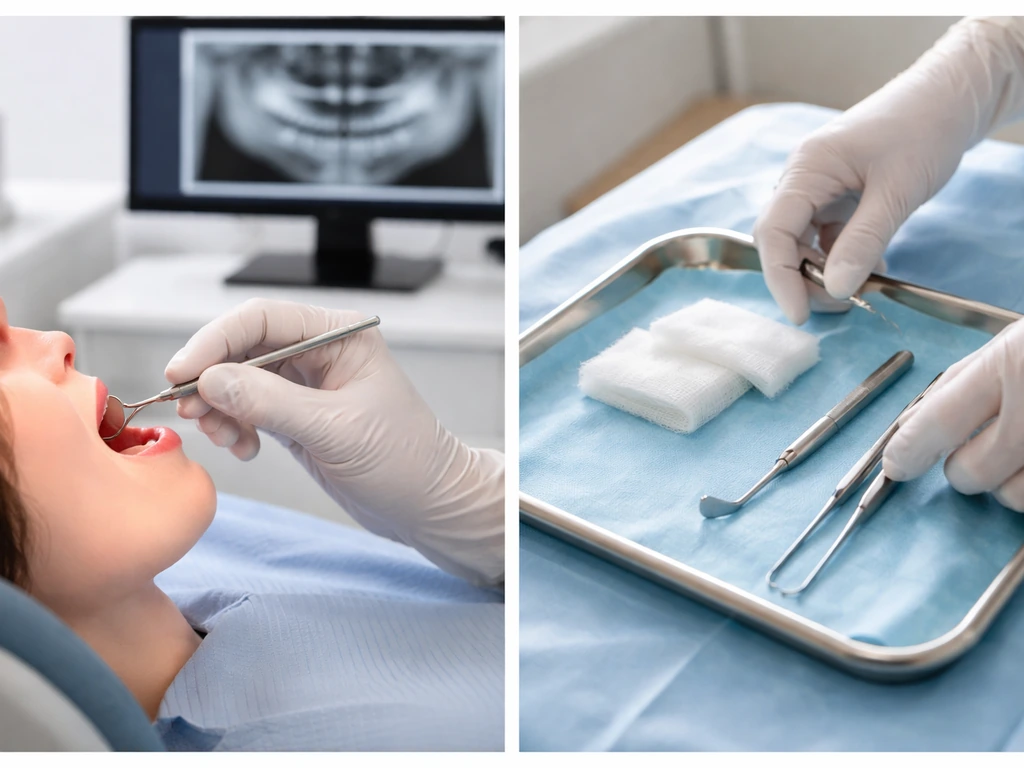
Diagnosis starts with a clinical exam and imaging, usually a periapical X-ray or panoramic radiograph for jaw lesions. If something looks suspicious or unusual on imaging, a CT scan may be ordered for better detail. The definitive diagnosis, however, always requires histopathology, meaning a biopsy specimen examined under a microscope. Radiographic calcifications alone can look like odontoma, cysts with calcified contents, or even foreign bodies, so the microscope is non-negotiable for a reliable diagnosis.
For most benign odontogenic tumors, including odontomas, enucleation (surgical removal of the lesion along with its surrounding tissue) is the standard treatment. The procedure is typically straightforward, and recurrence rates for most benign variants are low. That said, recurrence is possible, which is why radiographic monitoring after enucleation is genuinely important. A published case report with 7-year follow-up illustrates that even after apparently successful removal, radiographic controls catch recurrences that might otherwise go unnoticed.
For malignant odontogenic tumors, treatment is more aggressive and typically involves wider surgical resection, sometimes combined with radiation or chemotherapy depending on histological grade and extent. The prognosis and treatment planning in malignant cases are handled by an oncology team, not a general dentist.
One point people often wonder about is whether mandibular tori can grow and whether they're related to these tumors. They're not the same thing. Tori are benign bony outgrowths that don't contain dental tissues and don't involve odontogenic differentiation the way odontomas do.
The myth: tumors as a tooth regrowth mechanism
Here's where internet speculation gets genuinely misleading. Some people, after reading about tumors that "grow teeth," leap to the idea that this means the body has a hidden capacity to regenerate teeth, that it just needs the right trigger or that tumors are somehow unlocking a dormant regrowth ability. This is not how it works.
The tooth-like structures in odontomas and teratomas are not the body regenerating a lost or missing tooth. They are abnormal growths of disorganized or ectopically organized dental tissue, arising in the wrong place, at the wrong time, from aberrant cell behavior. They don't emerge through your gum and function as a replacement tooth. They're lesions that require removal.
Normal adult teeth cannot regenerate. Enamel, specifically, cannot be regrown because the ameloblasts that produce it are lost by the time the tooth erupts into the mouth. This is a firm biological constraint, not a gap in dental medicine's ambition. Research into whether stem cells can grow teeth is ongoing, but as of today, spontaneous tooth regeneration is not something postnatal human cells naturally accomplish, and a tumor is absolutely not a shortcut to that goal.
The question of whether ovarian dermoid cysts can produce dental tissues is a related one that surprises a lot of people. If you've wondered about whether ovaries can grow teeth, the answer follows the same logic: ovarian teratomas (dermoid cysts) can contain dental tissues because they arise from pluripotent germ cells, not because the ovary has any inherent tooth-forming capability. The biology is fascinating, but the clinical message is the same: these are abnormal growths, not regeneration.
What to do if you're concerned right now
- Book a dental appointment promptly if you have jaw swelling, unexplained loosening of teeth, a lump or sore that hasn't resolved in two weeks, or anything that looked unusual on a previous X-ray and was never followed up.
- Ask for a panoramic radiograph (OPG) if you haven't had one recently. This single image gives your dentist a broad view of both jaws, all teeth including unerupted ones, and surrounding structures where odontogenic lesions commonly appear.
- If your GP or dentist finds something on imaging that looks calcified or unusual within the jaw, ask specifically for a referral to an oral and maxillofacial surgeon. This is their specialty, and they are the right person to decide whether a biopsy is needed.
- Don't ignore systemic symptoms. Fever, difficulty swallowing, or rapid swelling alongside any oral lesion are emergency-level symptoms. Go to an emergency room, not an urgent care clinic.
- Follow up after treatment. If you've had a jaw lesion removed in the past and haven't had a follow-up X-ray in a year or more, schedule one. Recurrence of odontogenic tumors is uncommon but real, and catching it early makes retreatment simpler.
The bottom line is this: tumors can produce tooth-like structures, and in some cases those structures contain genuine dental tissues organized in ways that look remarkably like teeth. But this is abnormal biology, not regeneration. If you're searching this topic because something feels off in your mouth or jaw, the most useful thing you can do today is see a dental professional and get imaging done. Most of these lesions are benign and entirely manageable when found early.
FAQ
If imaging shows calcified tooth-like structures, does that automatically mean it is an odontoma?
No. Tumor-associated “tooth-like” material does not replace missing teeth or restore normal bite function. These lesions are abnormal growths that need evaluation, and any involvement of adjacent structures (roots, nerves, sinuses) can still cause damage even if mineralized tissue is present.
Can a cyst that contains calcifications be mistaken for a tumor that grows teeth?
No. Calcifications can also appear with odontogenic cysts, chronic infections, scar tissue, or other jaw lesions. Because several conditions can mimic the same radiographic pattern, a biopsy with histopathology is what confirms the diagnosis and guides treatment.
What’s the most common mistake people make after noticing a lump or swelling near an impacted tooth?
Yes. One common pitfall is waiting too long when symptoms persist or slowly worsen. Even when lesions are benign, enlargement can erode bone, affect an impacted tooth, or compromise nearby nerves, so “two weeks then checked” for persistent sores, swelling, or lumps is a sensible threshold to avoid delayed diagnosis.
Could a tumor that grows dental tissue be painless and only discovered on dental X-rays?
Often, yes. Some odontogenic tumors, including odontomas, are found incidentally on routine X-rays because they may not cause pain. If you have a known impacted tooth, recurring infections, or changes in tooth eruption, periodic imaging can be important even in the absence of dramatic symptoms.
If an odontoma or similar lesion is found, is surgery always straightforward?
Usually they are removable, but the surgical plan depends on size, location, and proximity to critical structures. For example, lesions near the inferior alveolar nerve or close to the maxillary sinus may require more careful planning and follow-up to reduce the risk of numbness, sensory changes, or oroantral complications.
How likely is it for tooth-like tumors to come back after removal?
Recurrence risk varies by lesion type and completeness of removal. That is why follow-up imaging after enucleation is typically recommended, especially for lesions with irregular borders or those that were hard to separate entirely from surrounding tissue.
Is it possible to inherit a tendency for odontogenic tumors that develop tooth-like tissues?
Genetic factors can play a role in some rare syndromic conditions and in certain tumor tendencies, but most cases occur sporadically without a clear inherited cause. A clinician can assess family history and, if appropriate, discuss whether genetic evaluation is warranted.
Can a dental professional tell whether the lesion is benign or malignant without a biopsy?
Sometimes. Imaging can suggest odontogenic origin, but the definitive diagnosis still requires histopathology from tissue removed or biopsied. Nerve symptoms, rapid expansion, or suspicious imaging features make prompt evaluation more urgent because the differential includes more aggressive conditions.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

