Here's the honest answer upfront: you cannot grow new enamel on an adult tooth. The cells that build enamel die off once your teeth finish forming, so there's no biological mechanism to produce a fresh layer. But that doesn't mean you're helpless. A process called remineralization can rebuild mineral density in weakened or early-damaged enamel, and it's genuinely effective when you know how to support it. This guide covers exactly what's possible, what's not, and what you should do today.
How to Grow Teeth Enamel: What Works and What Doesn’t
What enamel actually is, and why it can't just "grow back"
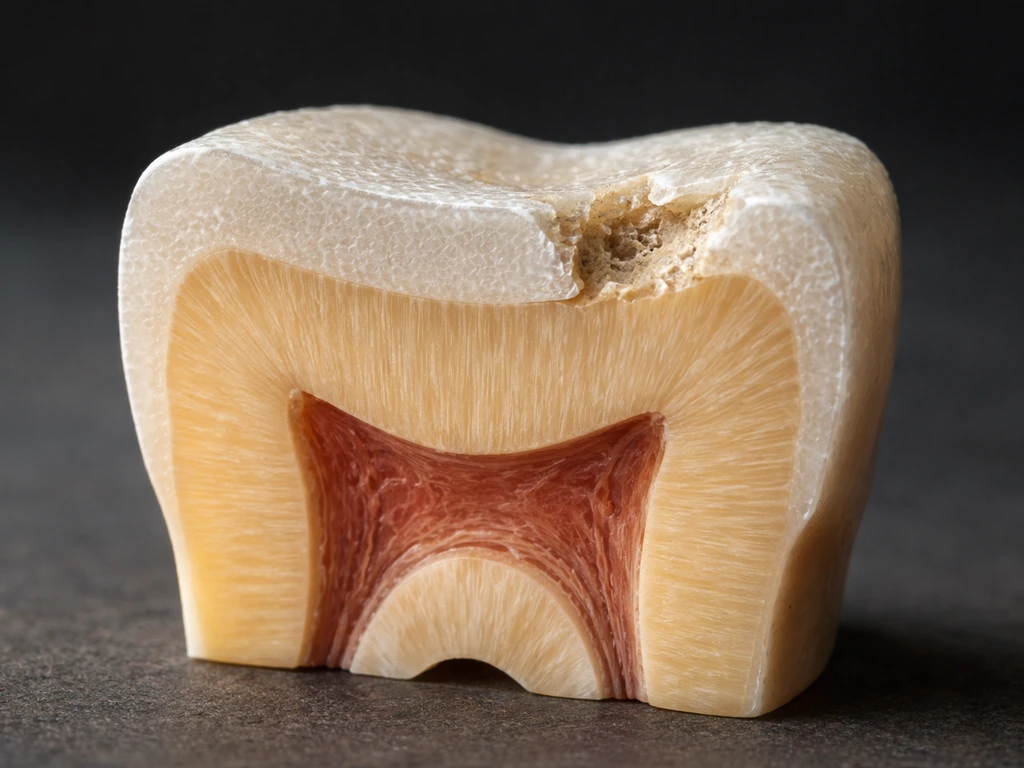
Enamel is the hardest substance in the human body, and that toughness comes from its composition: roughly 96% inorganic mineral, mainly carbonated hydroxyapatite crystals, with the remaining 4% being water and organic material. It's not living tissue in the way your skin or gums are. It has no cells running through it, no blood supply, and no nerve endings of its own.
Enamel is built during tooth development by specialized cells called ameloblasts. Once your tooth crown is fully formed and the tooth erupts into your mouth, those ameloblasts die. They don't hang around waiting to patch up damage later. UCSF researchers have been explicit about this: to replace enamel, you'd need to regenerate the ameloblasts themselves, and right now, that's not something the human body can do on its own. Stem cell research is exploring this territory, but nothing is clinically available yet.
So when you see products or blogs claiming to "regrow" enamel, treat that language skeptically. What they almost always mean is remineralization, which is real and useful, but it's not the same as producing new enamel from scratch. Understanding that distinction is the foundation of everything else in this guide. If you're also wondering about how to grow back enamel in a broader sense, the biology is the same: remineralization is your best realistic tool.
When enamel actually forms: childhood, development, and eruption
Enamel formation happens during a specific developmental window. Baby teeth start forming before birth, and permanent teeth form throughout childhood, with the third molars (wisdom teeth) typically completing their crown formation in the late teens. During this entire period, ameloblasts are actively laying down enamel mineral layer by layer.
This is why childhood nutrition matters so much for dental health. Deficiencies in calcium, phosphorus, or vitamin D during tooth development can result in structural weaknesses baked right into the enamel before the tooth even erupts. Once the tooth is in your mouth, that window is closed. The enamel you have at eruption is the enamel you work with for life. Parents sometimes ask what helps teeth grow in their kids, and the honest answer is: good nutrition during development, fluoride exposure, and avoiding repeated sugar and acid exposure while the enamel is still maturing post-eruption.
There's one partial exception worth mentioning: newly erupted teeth, especially in children and teenagers, have enamel that's not yet fully hardened. This "maturation" phase after eruption is a real window where fluoride and good mineral availability can meaningfully strengthen enamel at a structural level. It's not new enamel production, but the enamel is still integrating minerals, which is why fluoride is especially powerful for kids.
Remineralization: the real way to repair enamel naturally
Remineralization is the process where minerals, mainly calcium and phosphate, are redeposited into areas of enamel that have been partially dissolved by acid. When acids (from food, drinks, or bacteria) attack enamel, they pull minerals out of the crystal structure, creating tiny pores in the enamel. If the surface layer is still intact and the conditions are right, those pores can refill with minerals from your saliva and from topical fluoride treatments. This is what dentists call a "white spot lesion" reversal, and it's genuinely achievable.
The key word is "partially demineralized." Remineralization works on early lesions where the surface enamel is still structurally present. Once the surface breaks down and a cavity forms, you're past the remineralization window. That's why catching enamel loss early is so important.
Fluoride: still the gold standard
Fluoride works by helping form fluorapatite, a harder and more acid-resistant mineral than the carbonated hydroxyapatite that makes up natural enamel. Fluoride toothpaste (with at least 1,000 ppm fluoride for adults, 1,450 ppm is standard in many prescription formulas) used twice daily is your most evidence-backed at-home tool. For people with significant enamel loss, a dentist can prescribe high-fluoride gels or varnishes applied in-office.
Saliva: your built-in repair system
Saliva is genuinely underrated. It's supersaturated with calcium and phosphate ions, and it naturally bathes your teeth in the minerals needed for remineralization. It also buffers acids and clears food debris. Anything that reduces saliva flow (certain medications, mouth breathing, dehydration, medical conditions like Sjogren's syndrome) significantly impairs your enamel's ability to repair itself. Staying well hydrated, chewing sugar-free xylitol gum to stimulate saliva flow, and managing dry mouth are all practical steps.
Calcium, phosphate, and diet

Your diet directly feeds the mineral pool your saliva draws from. Dairy products are a classic source of calcium and phosphate. There's a reason people ask does milk help your teeth grow: calcium from dairy really does contribute to the mineral environment that supports remineralization, especially in children. Non-dairy alternatives include leafy greens, almonds, canned fish with bones, and fortified plant milks. Vitamin D is equally important because it regulates how well your gut absorbs calcium in the first place.
Casein phosphopeptide-amorphous calcium phosphate (CPP-ACP), sold in products like MI Paste, is a clinically studied remineralization agent. It delivers calcium and phosphate directly to the tooth surface in a form that integrates into enamel. It's particularly useful for people with dry mouth, those in orthodontic treatment, or anyone with significant white spot lesions.
Fix the causes of enamel loss first, or nothing else works
Remineralization and fluoride are only helpful if you slow down the rate of enamel destruction. If acid keeps hitting your teeth faster than minerals can redeposit, you'll lose ground regardless of what supplements or toothpastes you use. Here are the main culprits to address.
- Acidic and sugary drinks: Sodas, sports drinks, fruit juices, and energy drinks are some of the most common causes of enamel erosion. It's not just the sugar, it's the pH. Anything below pH 5.5 can start dissolving enamel. Drink these through a straw to reduce contact with teeth, don't sip slowly over hours, and rinse with water immediately after.
- Acid reflux and GERD: Stomach acid reaching your mouth is extremely damaging to enamel, particularly on the back surfaces of upper front teeth. If you have frequent heartburn or regurgitation, managing it medically isn't optional, it's essential for your teeth. Talk to your doctor about treatment if this applies to you.
- Brushing too soon after acid exposure: Enamel is temporarily softened by acid. Brushing within 30 to 60 minutes after consuming acidic food or drinks can physically scrub away softened mineral. Wait, rinse with water first, then brush.
- Brushing too hard or with the wrong technique: Aggressive horizontal scrubbing wears enamel, especially at the gumline. Use a soft-bristled brush with gentle circular or modified bass technique motions.
- Bruxism (teeth grinding): Grinding wears enamel in ways no amount of remineralization can counteract. If you grind your teeth at night, a custom night guard from your dentist is one of the most protective investments you can make for your enamel.
When natural approaches aren't enough: what dentists actually do
Remineralization has a ceiling. Once enamel has broken down to the point where a cavity has formed, or where a significant chunk of enamel is simply gone, topical minerals and fluoride can't rebuild the physical structure. At that point, you need dental treatment. It's worth being clear: these treatments replace or cover lost enamel. They don't regenerate it. But they protect the tooth and restore function effectively.
| Treatment | What it does | Best for | Is it real enamel? |
|---|---|---|---|
| Fluoride varnish / gel | Boosts remineralization of early lesions | White spot lesions, early demineralization | No, enhances existing enamel |
| Dental sealants | Plastic coating seals pits and fissures against acid and bacteria | Kids and teens with cavity-prone molars | No, a protective cover |
| Composite bonding | Tooth-colored resin applied to eroded or chipped enamel surfaces | Moderate erosion, cosmetic enamel loss | No, a synthetic replacement |
| Tooth-colored fillings | Removes decayed area and fills it with composite or ceramic material | Cavities where enamel and dentin are lost | No, a structural repair |
| Porcelain veneers / crowns | Covers the tooth surface or entire crown when enamel loss is severe | Advanced erosion, large structural damage | No, a full surface replacement |
The goal of all these treatments is to stop the progression of damage, protect the underlying dentin and pulp, and restore the tooth's function and appearance. None of them involve growing new biological enamel, but they work. If you're curious about the broader question of how to grow new teeth or regenerate dental structures more fully, current science is exploring stem cell and bioengineering approaches, but nothing is available as a standard clinical treatment yet.
Your daily routine to maximize enamel repair

This is the practical part. Follow this routine consistently and you'll be doing everything within your control to remineralize and protect your enamel.
- Morning: Brush for two full minutes with a fluoride toothpaste (1,000 to 1,450 ppm fluoride). Use a soft-bristled manual or electric toothbrush with light pressure. Don't rinse your mouth out after brushing, just spit. The residual fluoride film continues protecting your enamel.
- After breakfast: If you had anything acidic (orange juice, coffee, fruit), wait at least 30 to 60 minutes before brushing, or skip that second brush and just rinse with water.
- Throughout the day: Stay hydrated with plain water. After any sugary or acidic drink, rinse your mouth with water immediately. Chew sugar-free xylitol gum for 20 minutes after meals if you can't brush, to stimulate saliva and neutralize acids.
- With meals: Eat calcium-rich foods regularly. End meals with cheese or plain milk if possible, both raise oral pH and provide calcium.
- Evening: Floss before brushing to clear food and plaque from between teeth. Brush again with fluoride toothpaste. If your dentist has prescribed a high-fluoride gel or CPP-ACP product (like MI Paste), apply it now after brushing and don't eat or drink afterward.
- Night: If you grind your teeth, wear your night guard every night without exception. Grinding can undo months of remineralization progress in a matter of weeks.
- Ongoing: Schedule dental checkups every six months. X-rays and clinical exams can catch early demineralization that you can't see or feel yet.
Signs you need to see a dentist now, not later
Remineralization is powerful for early, subclinical enamel loss, but there are clear signs that you're past the point where home care alone is the right answer. Don't wait on these.
- Tooth sensitivity to cold, heat, or sweet foods that is new or worsening: This often signals that enamel is thin enough that the underlying dentin is exposed.
- Visible white spots, brown or yellow discoloration, or a chalky appearance on tooth surfaces: These are classic early signs of demineralization and can sometimes be reversed with professional fluoride treatment if caught early.
- Chipping, pitting, or teeth that look shorter or more transparent at the edges: These indicate physical enamel loss that has progressed beyond early-stage demineralization.
- Tooth pain that lingers after eating or drinking, or that wakes you up: This suggests the nerve may be involved, which requires prompt dental evaluation.
- Teeth that feel rough or look dull: Surface texture changes can signal enamel erosion.
- Any visible hole or dark spot on a tooth: This is a cavity and needs to be treated before it grows.
When you go to the dentist, ask specifically for a remineralization assessment if you're trying to avoid restorations on early lesions. Many dentists will monitor white spot lesions over time with fluoride varnish applications rather than immediately filling them. Being proactive about the conversation gets you better, more conservative care.
If you have kids and are worried about their dental development, the questions look a little different. Parents sometimes wonder about things like my teeth are small, will they grow, which touches on normal tooth size variation and development timelines. A pediatric dentist can help distinguish between normal developmental variation and actual structural enamel problems that need attention.
The broader question of how to grow back teeth in a more comprehensive sense, including what's biologically possible and what's currently being researched, is worth understanding if you're facing significant tooth loss alongside enamel damage. But for most people reading this, the priority is protecting what's there and giving your enamel every possible advantage through the remineralization tools that actually work today.
FAQ
Can I regrow enamel if I already have cavities or obvious damage?
In most cases, you cannot truly “grow” enamel again on an adult tooth. The realistic goal is reversing early mineral loss, which shows up as white spot lesions. If the surface has softened or a cavity has formed, at-home products and remineralization agents cannot rebuild the missing enamel structure, and you need a dentist to restore/protect the tooth.
How can I tell if my enamel loss is early enough for remineralization?
Yes, but only for enamel that is still intact enough to accept mineral. A simple decision aid is: if you can scrape off a chalky white area with brushing, it is often not fully remineralized or could be surface breakdown. When symptoms are present (sticky rough spots, catching a toothbrush on a defect, visible pits), request an exam to determine whether you are dealing with reversible demineralization versus a cavitated lesion.
What should I do after drinking soda, juice, or coffee to avoid making enamel worse?
Don’t brush immediately after acidic drinks or foods. Acid can temporarily soften enamel, so wait about 30 to 60 minutes before brushing, then use fluoride toothpaste. If you need to rinse, use water right after and brush later, this helps avoid mechanically wearing away softened enamel.
Should I rinse my mouth after brushing with fluoride toothpaste?
Rinsing right after brushing can reduce the toothpaste’s fluoride contact time. If you use fluoride twice daily, spit out excess but avoid rinsing with water immediately afterward, especially at night. In practice, that small change often improves the benefit of the fluoride treatment.
How often should I use fluoride if I’m trying to reverse white spots or prevent new lesions?
If you have white spot lesions or orthodontic brackets, you can be more aggressive with fluoride scheduling, but do it carefully. Many people benefit from adding an in-office fluoride varnish or prescribed gel during high-risk periods, while maintaining consistent twice-daily brushing at home. Ask your dentist for a plan tailored to your caries risk rather than stacking multiple OTC products at random.
Why isn’t my enamel improving even though I use fluoride toothpaste?
Dry mouth reduces saliva’s mineral supply and acid buffering, which slows remineralization even if you use excellent toothpaste. If you have medication-related dry mouth or mouth breathing, consider saliva substitutes, discuss prescription options with your clinician, and prioritize frequent hydration. If symptoms are persistent, getting evaluated for conditions like Sjogren’s syndrome matters because the fix is not only dental products.
Is MI Paste (CPP-ACP) better than fluoride, or should I combine them?
CPP-ACP can be helpful, especially for people at higher risk, with orthodontics, or with dry mouth, because it delivers calcium and phosphate to the tooth surface. However, it still relies on having enough fluoride exposure and low ongoing acid attacks to work. If you use CPP-ACP, maintain your fluoride routine and don’t use it as a substitute for reducing sugary or acidic exposures.
What brushing technique mistakes can block remineralization progress?
The toothpaste “strength” alone isn’t the only factor. Technique and exposure time matter, use a soft brush, spend enough time, and brush twice daily consistently. Also, ensure you cover the areas that demineralize easily (near the gumline, around brackets, and between teeth), since missed spots can prevent overall improvement.
Does chewing xylitol gum actually help regrow enamel, or is it just preventive?
Xylitol gum can support saliva flow and reduce bacterial acid production, but it is not a one-step replacement for fluoride and diet control. For practical results, choose sugar-free gum with reliable xylitol content and use it around risk times (for example after meals) rather than treating it as a cure for existing enamel loss.
When should I stop trying at-home remineralization and see a dentist urgently?
If you are seeing sensitivity, yellow-brown discoloration, or roughness, it is worth treating it as higher stakes. Ask for a visual and tactile assessment, and if needed, ask whether the lesion is cavitated. The fastest path to success is early classification, because management differs for reversible lesions versus those that need filling or sealing.
How long should I expect before I see improvement?
Lifestyle changes take time, and remineralization is not overnight. Many people notice changes in the appearance of white spots over several weeks, but the speed depends on ongoing acid exposure, saliva status, and lesion depth. If there is no visible improvement within a reasonable monitoring window, it usually means the acid challenge is too high or the lesion is too deep for home care.
What if my enamel loss is related to acid reflux or frequent vomiting?
If you have significant erosion from reflux or frequent vomiting, the enamel problem is being actively attacked by acid from inside the body. Even excellent fluoride routines may fail unless the reflux is treated. Ask your dentist and your physician about evaluation and targeted management, because controlling the source of acid is often the deciding factor for whether enamel can stabilize.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

