Common reasons gums cover teeth (and why it happens)
There are several distinct mechanisms behind gum tissue appearing to cover a tooth, and they're worth separating because the treatment for each is completely different.
Gingival hyperplasia (true overgrowth)
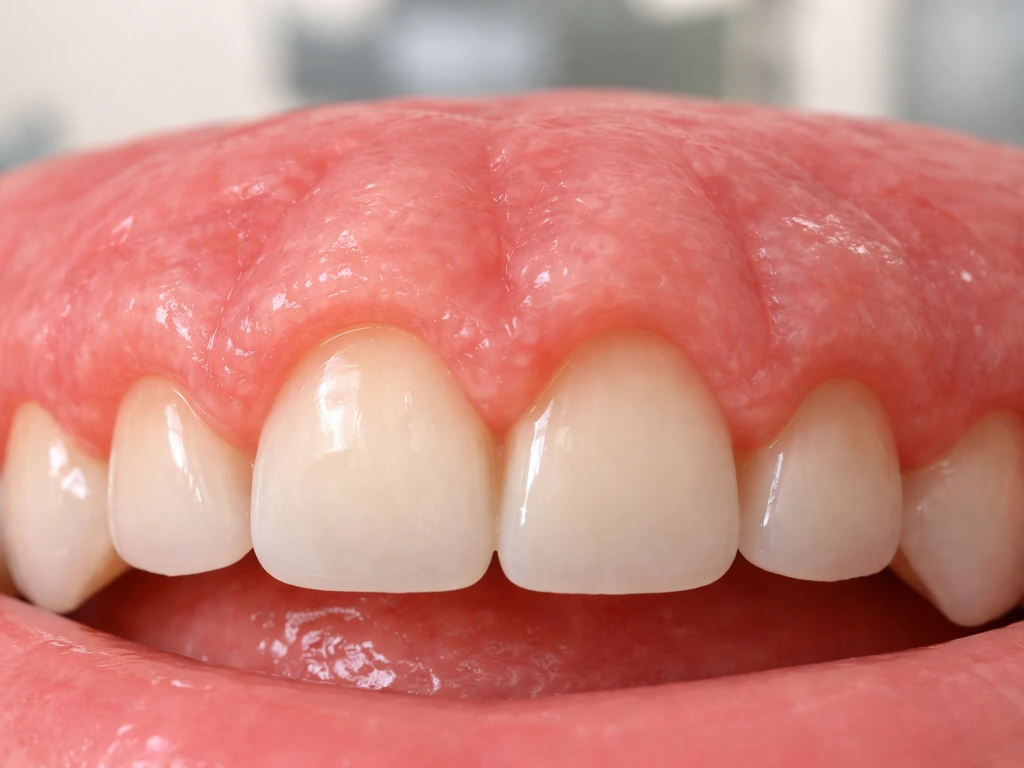
This is the most dramatic version. Gingival hyperplasia, also called gingival enlargement, is a condition where gum tissue proliferates beyond its normal boundaries. According to the Merck Manual, the overgrowth can be nodular or diffuse and may almost completely cover some teeth. It happens for a few reasons: certain medications (anti-seizure drugs like phenytoin, calcium channel blockers for blood pressure, and cyclosporine for organ transplant patients are the classic culprits), some systemic conditions like leukemia, or chronic local irritation. If you or a family member recently started a new medication and notice the gums seem to be taking over, this is the mechanism to ask your dentist about.
Inflammation and pseudopockets
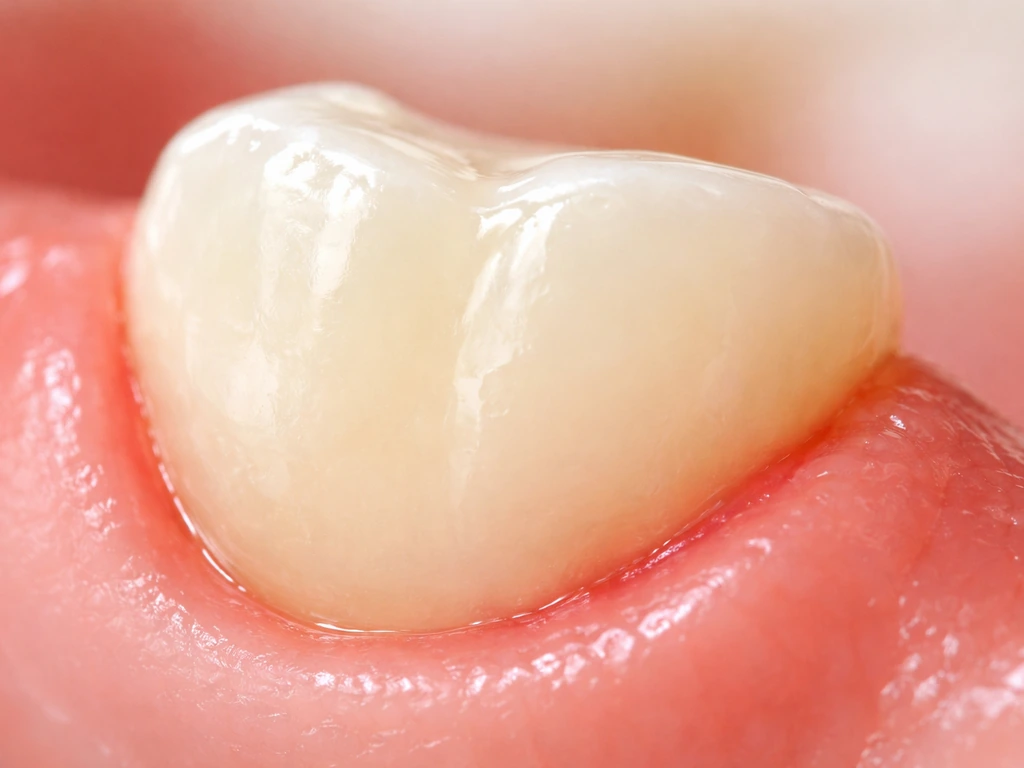
Ordinary gingivitis, the mildest form of gum disease, can make gum tissue swell enough that the gingival margin looks like it has crept up (or down, depending on which teeth) over the tooth. The gums lose their healthy, slightly stippled, knife-edge appearance and become rounded and shiny. This swelling can create what's called a pseudopocket or false pocket: the gum looks deeper around the tooth when probed, but there hasn't been any actual destruction of the attachment holding the gum to the tooth. It looks like the gum has grown, but really the tissue has just puffed outward. Once inflammation is controlled, the margin often returns to normal. If you're worried about buildup making this worse, it's also worth knowing that plaque can grow on gums and drive this kind of ongoing irritation.
Partially erupted teeth (especially wisdom teeth)
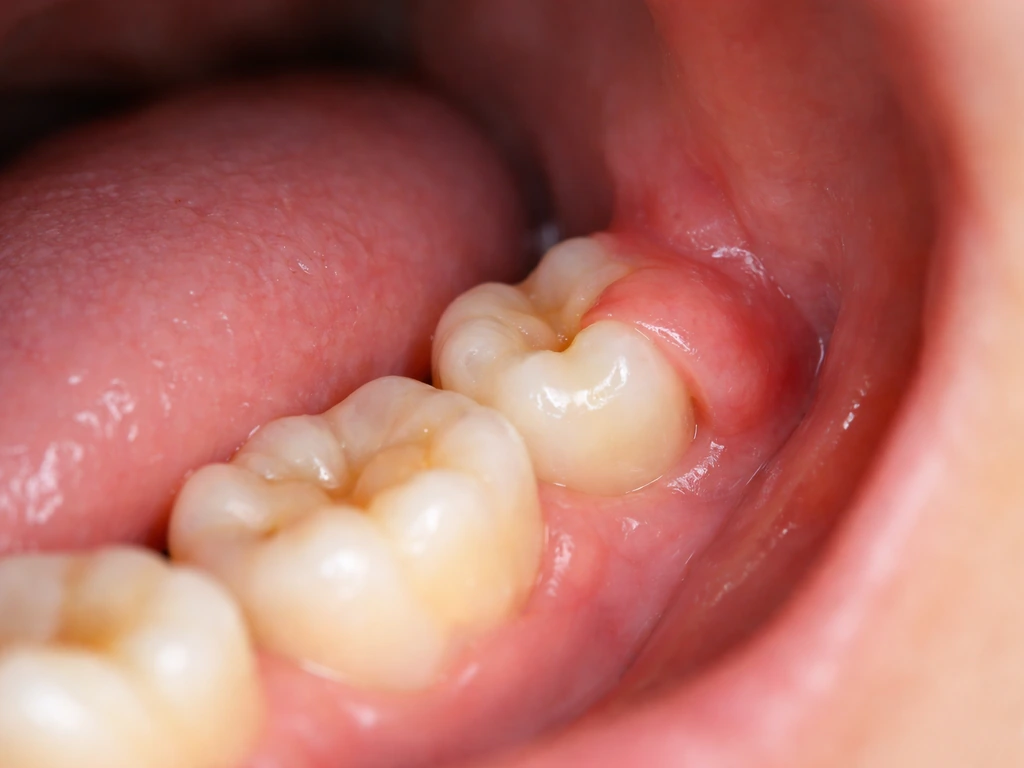
When a tooth is still pushing through the jaw, a flap of gum tissue called an operculum commonly sits over part of the crown. This is extremely normal in children and teenagers as adult teeth erupt, and it's the reason wisdom teeth in young adults so often look "half buried." The gum isn't growing over the tooth in a pathological sense; the tooth just hasn't finished its journey yet. That said, this operculum can trap food and bacteria and become infected (pericoronitis), so "normal eruption" doesn't always mean painless or problem-free.
Tooth drift, crowding, or alignment issues
When teeth are crowded, tipped, or have drifted out of position, the gingival contour around them can look irregular, with some surfaces appearing more covered than others. This isn't the gum growing; it's the tooth that has moved relative to the surrounding tissue. Orthodontic treatment can change this relationship dramatically.
When it happens: timelines for gums covering teeth
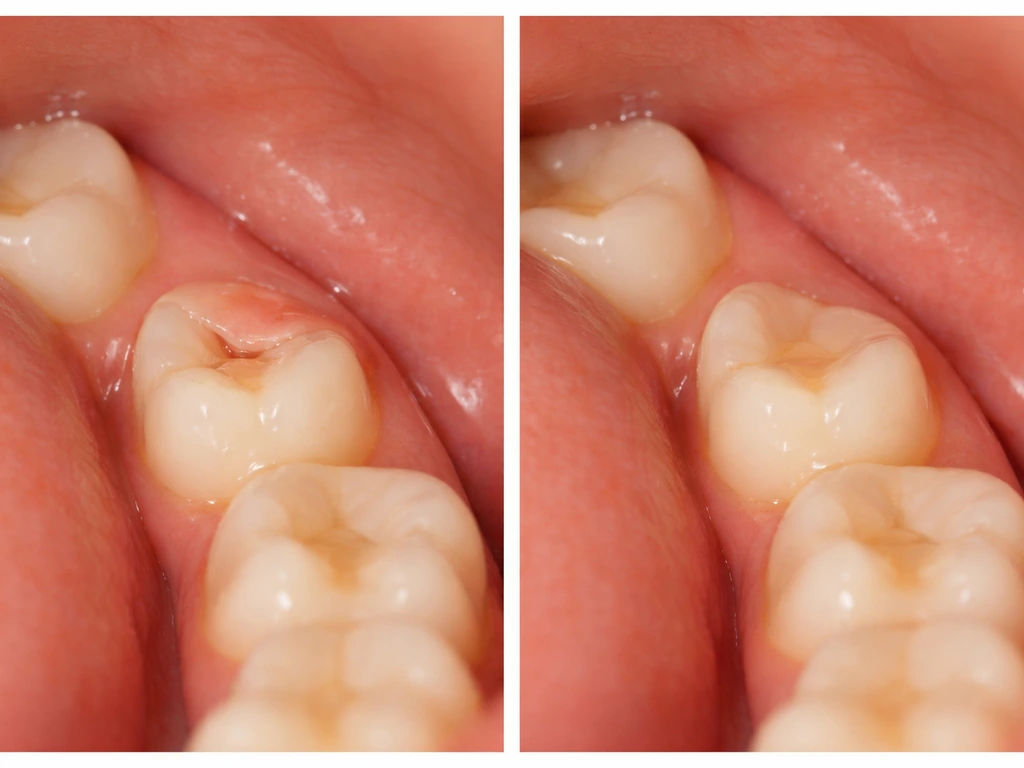
Timing gives you a lot of diagnostic information before you even get to a dentist. Here's how to think about it:
| Situation | Typical timeline | What's usually happening |
|---|
| Child's adult tooth erupting | Weeks to months | Normal eruption; gum flap recedes as tooth pushes through |
| Wisdom tooth partially in | Months to years in young adults | Operculum over partially erupted tooth; watch for pericoronitis |
| After dental cleaning or scaling | Swelling visible within days; resolves in 1–2 weeks with healing | Inflammatory pseudopocket; tissue remodels after treatment |
| After periodontal surgery | Full healing takes 2–3 weeks; probing deferred until healed | Normal healing; early "coverage" is expected, not a problem |
| After a tooth fracture or trauma | Gum may migrate over broken tooth within days to weeks | Biological response to exposed root/crown; needs dental eval |
| Medication-induced overgrowth | Develops over weeks to months after starting medication | True hyperplasia; may need medication change + debridement |
| Gingivitis / infection | Swelling can appear within days of poor hygiene or irritation | Pseudopocket from inflammation; resolves with treatment |
If gum tissue appears to have covered a tooth within a day or two after eating something (like a piece of food got lodged and the tissue swelled), that's a different story. Gums can swell over trapped food, which is a short-term inflammatory response rather than actual tissue migration. It usually settles once the irritant is removed, but if swelling is severe or doesn't go down within a few days, see a dentist.
Broken tooth scenario: will gums grow over a broken tooth?
This is one of the most common situations people search about. If you've broken a tooth and left it untreated, or noticed that the gum seems to be "covering" the broken edge, here's what's actually happening biologically.
Gum tissue does migrate toward and over exposed, broken tooth surfaces over time. The biology is straightforward: the body tries to cover exposed tissue. But this is not healing, and it is not safe to wait it out. A broken tooth, especially one with a fracture that extends below the gumline (a crown-root fracture), creates a very complicated restorative scenario because the margins are now subgingival, meaning your dentist may need to access them surgically. The gum covering doesn't protect the underlying tooth structure from decay or infection; it can actually hide the problem while it gets worse.
Fractures are classified by depth. Enamel-only chips can often be smoothed or monitored. Fractures reaching the dentin or pulp are emergencies: pulp exposure (Ellis Class III) requires prompt pulp therapy, and delays significantly increase the risk of abscess formation. Just because you can no longer see the broken edge doesn't mean the tooth is okay. Always get imaging done; a clinical exam alone isn't enough to rule out internal involvement.
If the tooth also becomes infected, you may develop a dental abscess, which is pus building up beneath the tooth or gum. Signs include throbbing pain, swelling of the face or jaw, a bad taste in your mouth, and sometimes fever. The NHS and Mayo Clinic both describe this as a condition requiring prompt professional drainage, not home treatment. If you have fever and facial swelling and cannot reach your regular dentist, go to an emergency department. A broken tooth with gum tissue growing over it is not a cosmetically managed problem; it needs to be evaluated.
Can gums grow back? What regrows vs. what doesn't
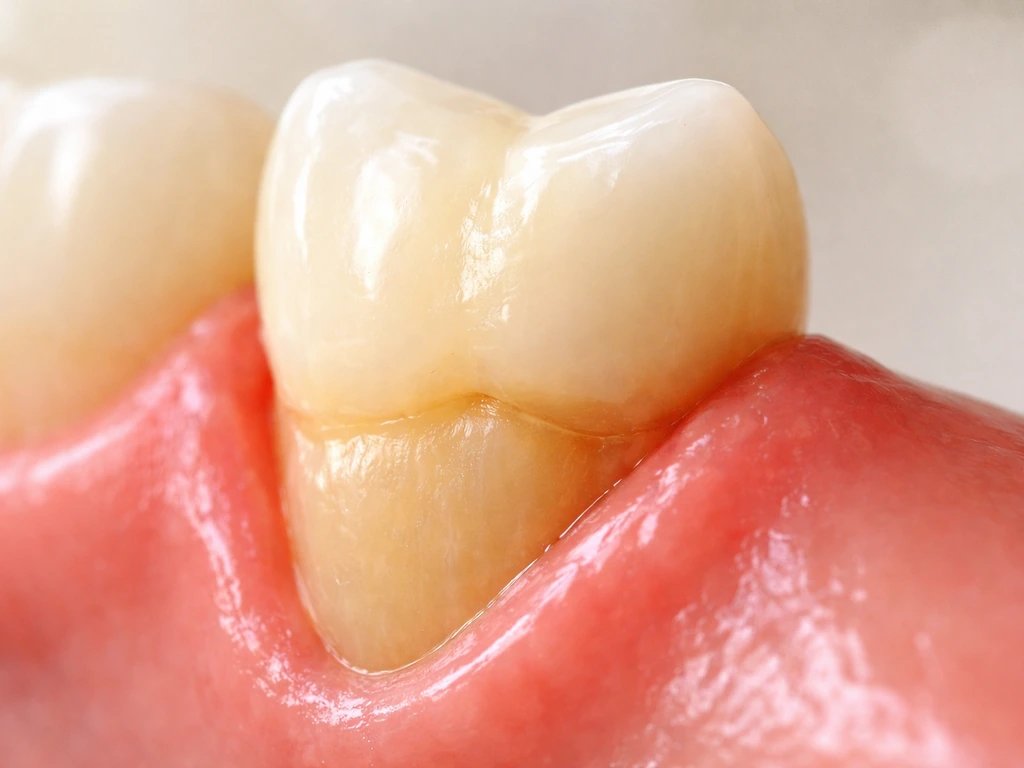
This is where a lot of internet misinformation lives. Let's be direct: once gum tissue has receded due to periodontal disease or chronic recession, it does not grow back on its own. Gingival recession, the process by which gum tissue retreats down the root surface and exposes it, is not reversible through brushing differently or using a special toothpaste. The exposed root is exposed for good unless a dentist physically moves tissue back over it.
What can be done surgically is another matter. Grafting procedures, particularly the subepithelial connective tissue graft, are considered the gold standard for Miller Class I and II recession defects. Clinical studies report mean root coverage outcomes around 84 to 85 percent at 12 months, with the goal of complete root coverage tracked as a defined endpoint rather than just "some improvement." So yes, dentists can re-cover exposed roots, but it involves surgery, not natural regrowth. If you're researching your options after a dentist tells you that recession is present, reading about how to grow gums back over teeth will walk you through what those procedures actually involve.
The same rule applies to the deeper structures. True periodontal regeneration means regenerating cementum, alveolar bone, and the Sharpey fibers that anchor the tooth, all together. That's a specific, biologically constrained target. Procedures like guided tissue regeneration can achieve partial regeneration in the right conditions, but it's not the same as tissue spontaneously regrowing. The body does not automatically rebuild what periodontal disease has destroyed.
One thing that does happen naturally is healing after controlled treatment. After scaling and root planing (a deep cleaning procedure), the gum tissue can tighten, reduce in swelling, and the pseudopockets created by inflammation can resolve. This is sometimes interpreted as "the gums grew back," but what actually happened is that the swollen tissue returned to its healthy, less-puffy state. The distinction matters because if recession was present beforehand, that's still there even after the gums look better.
Can a tooth grow on your gums? What's biologically possible
This is a question that comes up in a few different contexts, and the biological answer is essentially no, not in a healthy adult mouth. What you might actually be seeing if it looks like a tooth is growing on or from the gum tissue includes: a retained baby tooth root that was never fully resorbed, a tooth that erupted in an unusual position (ectopic eruption), a supernumerary tooth (an extra tooth that is actually forming and pushing through), or in rare cases a calcified mass like a torus or a nodule of calcified tissue.
In children, unexpected bumps on the gum can sometimes be eruption cysts (a bluish, fluid-filled swelling over an erupting tooth that usually resolves on its own). In adults, a hard lump on the gum that isn't associated with an erupting tooth should always be evaluated, because gingival enlargement can occasionally signal something more serious, including malignant processes, which is why Merck explicitly notes that differential diagnosis is necessary for any unexplained gum enlargement.
Wisdom teeth erupting in adult patients can look and feel like a "new tooth growing in the gum," and technically that's exactly what it is. That's one of the few times in adulthood when a tooth is literally growing through gum tissue. Outside of wisdom teeth, if something tooth-like appears to grow from your gum, that needs an X-ray and a professional evaluation, not a wait-and-see approach.
What to do today: self-checks, red flags, and next-step dental care
Start with a mirror and good light. Look at the gum tissue around the tooth or teeth you're concerned about and run through these questions before you decide how urgently to act.
Do a basic self-check
- Is the gum swollen, red, shiny, or bleeding when you touch it? These are signs of active inflammation, not normal anatomy.
- Did this change appear after a trauma, a broken tooth, or something getting stuck in the gum? If yes, that's the likely cause.
- Is there a visible flap of tissue (operculum) over a partially erupted tooth, especially a back molar? That's probably normal eruption, but watch for pain, pus, or smell.
- Did you recently start a new medication? Drug-induced gingival overgrowth is real and underdiagnosed.
- Is there pain when you press on the area, a bad taste, or swelling in your jaw or face? These are infection red flags.
- Has the change been there for more than two to three weeks without improving? That needs professional evaluation regardless of cause.
Red flags that mean go today (not next week)
- Fever combined with dental pain or facial swelling: this can indicate that infection has spread beyond the local area and requires emergency care.
- Difficulty swallowing or opening your mouth fully: possible sign of spreading infection.
- A pimple-like bump on the gum that drains and tastes foul: this is likely an abscess, and even if the pain improves when it drains, treatment is still required.
- Visible broken tooth with no pain: counterintuitively, a broken tooth that stops hurting may mean the pulp has died, which doesn't mean it's fine; it means an infection can develop silently.
- Rapid progression of swelling over hours, not days.
Next-step dental care based on what you're seeing
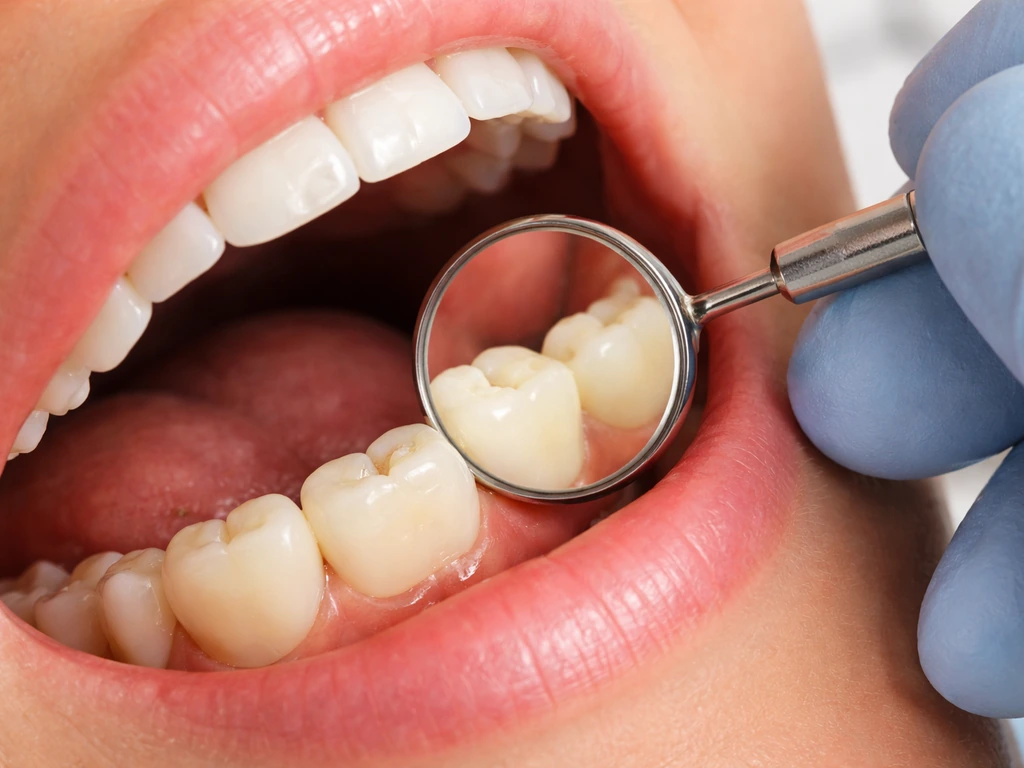
For gum overgrowth or unexplained tissue changes, a periodontal evaluation is the right first step. Your dentist will probe around each tooth to measure pocket depths, check for bleeding on probing, and take X-rays to assess bone levels. This distinguishes a pseudopocket (just inflammation) from true periodontal pocketing with bone loss, and it shapes the entire treatment plan. Addressing tartar buildup is often part of that process, since it's useful to understand that tartar can accumulate on gum tissue and perpetuate exactly the kind of chronic inflammation that produces these tissue changes.
For a broken tooth, get clinical photos and radiographs taken. The treatment depends on fracture depth: enamel chips may just need smoothing, but anything involving dentin or pulp needs restorative work, root canal therapy, or extraction depending on how much tooth structure remains. Don't assume that gum growing over the broken edge means the problem is resolving.
For infection signs, the current standard of care prioritizes definitive dental treatment first, meaning drainage of the infection, pulp therapy, or extraction as needed, over antibiotics as a first move. Antibiotics are reserved for cases with systemic involvement (fever, malaise, spreading swelling). If your dentist can see you today and drain the infection directly, that's more effective than antibiotics alone.
For patients dealing with recession rather than overgrowth, the conversation is about timing and candidacy for grafting. Not every recession site needs surgery immediately, but monitoring is essential because recession from aggressive brushing, crowded teeth, or periodontal disease tends to progress without intervention. Ask your dentist about your Miller classification, which predicts how much root coverage a graft can realistically achieve, and whether the gold-standard connective tissue graft approach is appropriate for your situation.
The bottom line is this: gum tissue can cover teeth through several different mechanisms, most of which are not natural healing and almost none of which are "your gums growing back" in the way people hope. What gum tissue can do surgically, with the right periodontal procedures, is genuinely impressive. But what it won't do on its own is undo periodontal disease, heal a broken tooth, or regenerate structures that have been destroyed. Knowing which situation you're in is the whole game, and that requires a proper examination, not just a mirror check.