Yes, plaque absolutely forms on and around your gums, not just on your teeth. It builds up along the gumline (called supragingival plaque) and can sneak below the gum margin into the tiny crevice between your tooth and gum (subgingival plaque). So if you've noticed a sticky, slightly fuzzy film right where your teeth meet your gums, that's plaque doing exactly what it does. The good news is that early-stage plaque-driven gum inflammation, known as gingivitis, is completely reversible with the right daily routine. The bad news is that if you ignore it long enough, it progresses into periodontitis, which involves bone loss that doesn't grow back on its own.
Can Plaque Grow on Gums? What It Means and What to Do
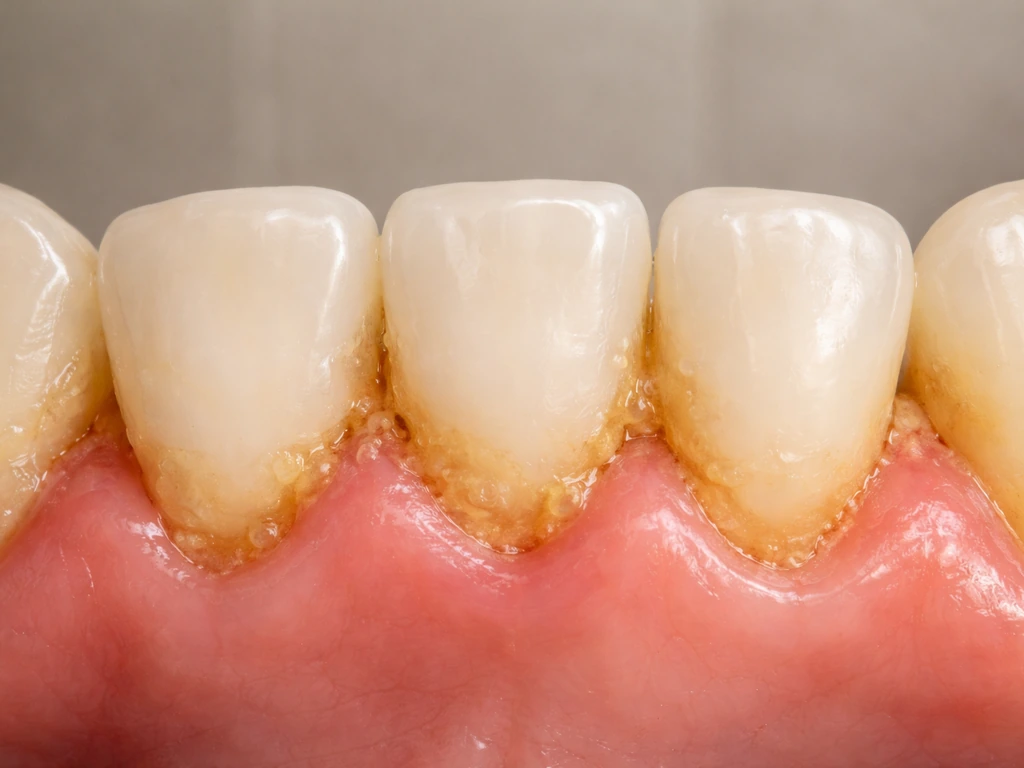
Does plaque actually form on gum tissue itself?
Here's the clarification most people need: plaque is a sticky bacterial biofilm that colonizes tooth surfaces, both above and below the gumline. It doesn't grow on gum tissue the way a plant grows in soil, but it absolutely forms right at the gum margin and extends down into the sulcus (the narrow groove where your gum meets your tooth). Because that boundary is so close, plaque at the gumline directly irritates the gum tissue next to it, causing the inflammation you know as gum disease.
The CDC describes plaque as a sticky, removable film of bacteria that lives on tooth surfaces and, importantly, can extend its effects below the gumline leading to periodontal pockets. Dental hygiene research on biofilms confirms that plaque colonizes tooth surfaces both above and below the gingival margin, which is why the gumline is always ground zero for early gum disease. So when someone says they have plaque on their gums, what they're really describing is plaque sitting right at that tooth-gum junction, which is close enough to cause real damage.
How plaque builds up along your gumline
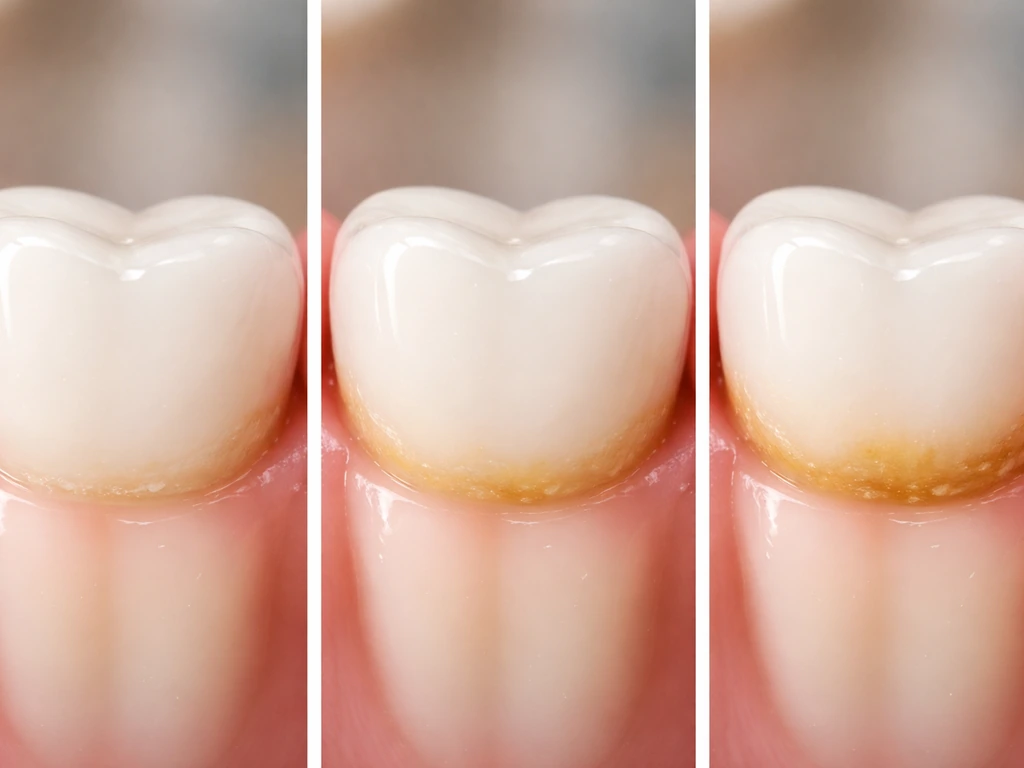
Plaque starts forming on your teeth within minutes of brushing. Bacteria from your saliva attach to a thin protein layer on your tooth surface, and over hours, more bacteria layer on top, forming a structured community called a biofilm. This biofilm matures through what researchers call a succession of microbial colonization, meaning different bacterial species join at different stages, each making the environment more hospitable for the next. Within 24 to 72 hours without cleaning, this biofilm thickens and starts triggering an immune response in the nearby gum tissue.
The gumline is especially vulnerable because it's a hard-to-clean zone where plaque gets a foothold. Interdental spaces (between teeth) and the gum crevice are the spots most people miss with a quick brush. Left alone, plaque at or below the gumline produces waste products that inflame gum tissue, which is why gingivitis is mainly found where the tooth and gum meet. If plaque isn't removed consistently, it hardens into tartar (calculus), which is mineralized and can no longer be brushed away at home, making professional cleaning necessary. The related question of whether tartar can grow on gums follows the same logic: tartar is just old plaque that has calcified in place.
Plaque vs. irritation vs. infection: how to tell the difference
This is where people get confused, and it matters because each condition calls for a different response. Here's a practical breakdown:
| What you notice | Most likely cause | What to do |
|---|---|---|
| Sticky, slightly fuzzy film at gumline, no pain or bleeding | Supragingival plaque | Step up home cleaning routine immediately |
| Gums look pink/firm but feel slightly rough between teeth | Early plaque buildup | Floss daily, brush at 45-degree angle to gumline |
| Gums are red, puffy, or bleed when you brush or floss | Gingivitis (plaque-induced inflammation) | Improve hygiene routine; see dentist if it persists past 2 weeks |
| Gums are swollen, dark red or purplish, tender to touch | More established gingivitis | See a dentist soon for professional cleaning |
| Persistent bad breath, gum pain, pus, or loose teeth | Possible periodontitis or infection | See a dentist urgently |
Healthy gingiva is pink, firm, and doesn't bleed after gentle brushing. Gingivitis shows up as soft, swollen, reddish-purple gums that bleed easily and feel tender. Gingivitis generally doesn't cause significant pain, which is exactly why people miss it for months. The fuzzy or furry sensation on your gums that some people describe is often plaque biofilm sitting right at that tooth-gum junction. A simple gum infection or injury from a food item, by contrast, will usually look more localized, may have a clear trauma point, and won't follow the pattern of bleeding all along the gumline. Food can irritate gums, but true gum overgrowth is usually driven by ongoing plaque buildup and inflammation along the gumline.
What happens when plaque stays put: gingivitis vs. periodontitis
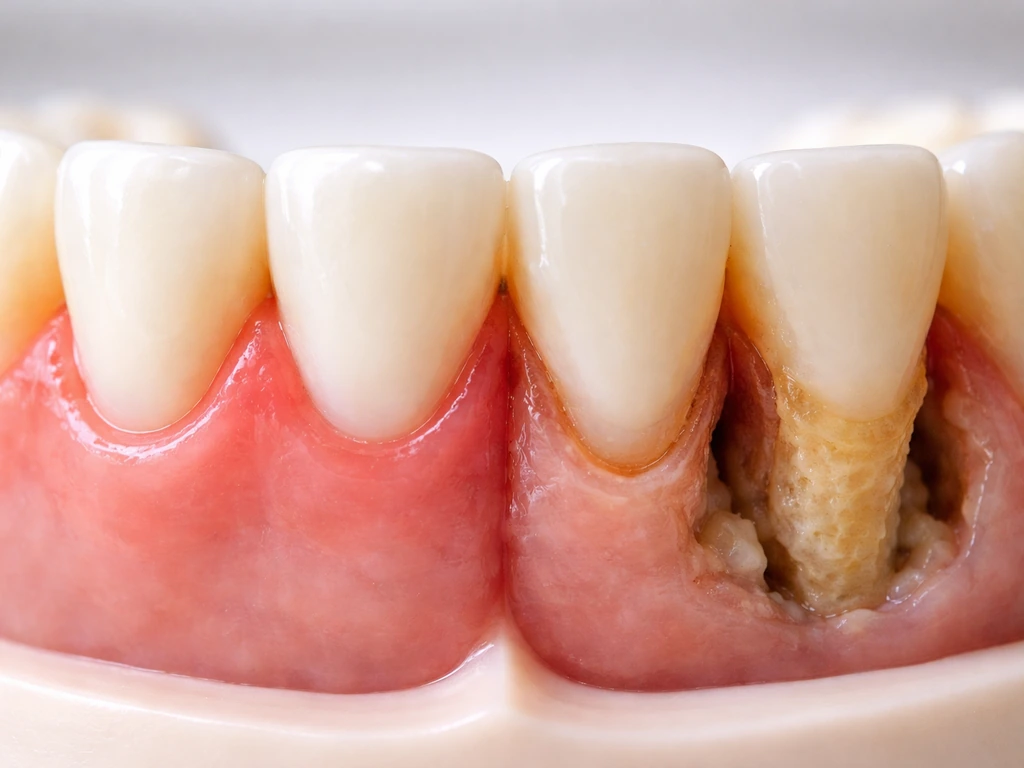
This is the part that really matters. Gingivitis is plaque-induced inflammation confined to the gum tissue, with no bone or attachment loss. It's reversible. Remove the plaque consistently, and the gums can return to normal. The CDC confirms this clearly: gingivitis is milder and preventable, and with good oral hygiene it goes away. The ADA frames it the same way, noting that if plaque isn't cleaned well, it inflames the gums, but the situation can be turned around.
Periodontitis is a different story. When gingivitis is not treated, bacteria in plaque can spread below the gumline, triggering a deeper immune response that destroys the connective tissue and bone supporting your teeth. The gum pulls away from the tooth, forming a periodontal pocket. Once bone is lost to periodontitis, that bone does not grow back on its own. The CDC is explicit: periodontitis is irreversible and can only be slowed or managed, not undone. This is the key biological limit the site's audience often needs to understand: plaque is not a tissue that can regenerate, but the damage it causes to supporting bone and gum attachment is largely permanent without specialized treatment.
The timeline from gingivitis to periodontitis isn't fixed, but untreated gingivitis can progress to periodontitis over months to years, especially with contributing factors like smoking, diabetes, or genetic predisposition. This is why acting at the gingivitis stage is genuinely urgent, even though it doesn't hurt yet.
Remove plaque near your gums today: a step-by-step routine
This is the practical part. The goal is to disrupt the biofilm mechanically, every single day, in the spots where it likes to hide. No single product or rinse can do this for you.
- Use a soft-bristled toothbrush. The ADA recommends soft bristles specifically to avoid gingival abrasion. Electric or manual both work well if you use them correctly.
- Angle the brush at 45 degrees to the gumline. Place the bristles where the tooth meets the gum, tilting the head slightly toward the gum. This lets the bristle tips reach just into the sulcus where plaque hides. Use short, gentle strokes or small circular motions. Scrubbing hard does not remove more plaque and will damage your gums and enamel over time.
- Brush for two full minutes, twice a day. Cover all surfaces: outer, inner, and chewing surfaces of every tooth. Most people spend less than 45 seconds brushing, which leaves a lot of plaque behind.
- Clean between your teeth once daily without skipping. Traditional floss, when applied correctly, can reach into the sulcus between teeth. Curve the floss into a C-shape around each tooth and slide it gently below the gumline before moving up and down against the tooth surface. Interdental brushes work well when they fit the space between teeth and may be easier to use for people with wider gaps or dental work.
- Ask your dentist or hygienist which interdental cleaner suits your anatomy. Toothpicks are not appropriate for cleaning between teeth as they can damage gum tissue.
- Add an antimicrobial rinse as a supplement, not a replacement. Ingredients like chlorhexidine, cetylpyridinium chloride, and essential oils can help reduce plaque and gingivitis when used alongside brushing and flossing. Chlorhexidine is particularly effective but should only be used short-term (typically no more than 14 days at a stretch) because it causes tooth staining and needs professional removal. For ongoing maintenance, an over-the-counter antimicrobial rinse is a useful addition.
- Don't aggressively scrape at plaque with fingernails, toothpicks, or sharp objects near your gums. You will injure the tissue and can introduce bacteria.
- Don't ignore early bleeding. Bleeding when you floss is usually gingivitis, and it is a signal to clean more carefully, not to stop flossing to avoid the bleeding.
If you've been inconsistent with flossing, expect your gums to bleed for the first few days of a consistent routine. That's normal. With daily cleaning and good technique, bleeding and tenderness from gingivitis typically lessen within one to two weeks. If it doesn't, that's your sign to call the dentist.
When to see a dentist urgently
Home care handles early plaque and mild gingivitis well, but there are situations where waiting is genuinely risky. Go to a dentist promptly if you notice any of the following:
- Bleeding that continues or worsens after two weeks of consistent brushing and flossing
- Gums that are visibly pulling away from your teeth or look like they've receded
- Persistent bad breath that doesn't improve with cleaning
- Pus coming from between a tooth and the gum
- Teeth that feel loose or that have shifted position
- Significant pain, swelling, or tenderness in the gum or jaw
- Swelling that extends to the face, neck, or lips (this needs same-day emergency care)
At the appointment, expect the dentist to probe around each tooth with a small instrument to measure pocket depth, look for signs of attachment or bone loss, and take X-rays if periodontitis is suspected. For gingivitis, a professional cleaning (scaling) removes the hardened tartar you can't brush away, and that's often the turning point. For established periodontitis, scaling and root planing is a deeper cleaning procedure done below the gumline, sometimes under local anesthetic, to remove bacterial deposits from the root surface and allow the tissue to heal. The ADA frames periodontal treatment as eliminating the dysbiotic plaque biofilm from tooth surfaces and establishing conditions where health can be maintained.
What actually heals after plaque is removed (and what doesn't)
This is the regeneration reality check this site's readers need most. Plaque itself is not a tissue. It doesn't grow back in any biological sense the way cells regrow. It simply re-forms from bacteria in your mouth within hours of cleaning, which is why daily disruption is non-negotiable, not optional.
Once plaque is removed and gingivitis is treated, gum tissue can heal back to a healthy state. The inflammation resolves, the gums firm up, and the color normalizes, usually within one to two weeks for mild cases. This is genuine, meaningful healing. So yes, in the context of gingivitis, the gums do recover, though they're not truly "regrowing" so much as returning to the healthy state they were in before the inflammation started.
Periodontitis is where the limits become hard and real. Once the bone and connective tissue attachment around your teeth are destroyed by periodontitis, that structure does not regenerate on its own after plaque removal. Advanced gum loss, recession, and bone loss from periodontitis typically do not reverse with home care alone. Some of this damage can be addressed with surgical procedures (like bone grafts or guided tissue regeneration), but those are specialized treatments, not natural healing. This connects to questions people often ask on this site, like whether gums can grow over teeth or how to grow gums back. The honest answer is that gum tissue has limited regenerative capacity, and significant gum loss from chronic periodontitis rarely reverses without clinical intervention.
The bottom line: catch it at the plaque and gingivitis stage, where the damage is still reversible, and your gums can fully recover. If your goal is to improve gum health and restore a healthier gum line, focus on consistent plaque removal and prompt treatment at the gingivitis stage how to grow gums in teeth. Let it progress to periodontitis with bone loss, and you're managing a chronic condition, not reversing it. That's the most important reason to act on plaque near your gums today rather than waiting to see if it gets better on its own.
FAQ
If I brush and still see plaque near my gums, does that mean I have periodontitis already?
Not necessarily. Plaque that remains at the gumline after inconsistent cleaning often reflects technique or missed areas (especially between teeth and along the back molars). Periodontitis is diagnosed by pocket depth and signs of attachment or bone loss, which are determined at an exam and X-rays, not just by what looks “sticky” at home.
Can plaque grow on gums if I never get bleeding when brushing?
Yes. Plaque can form without obvious bleeding, especially early on. Bleeding is a sign of inflammation, not proof that plaque is absent. If you have persistent bad breath, gum puffiness, or a film that returns quickly, plaque may be building even if your gums do not bleed.
How do I tell the difference between plaque buildup at the gumline and tartar that I can’t remove at home?
Tartar (calculus) usually feels hard or rough and tends to persist at the same spots even after careful brushing. Plaque feels more like a removable film that softens or disappears with proper brushing and cleaning. If the area doesn’t improve after several days of consistent technique, a professional cleaning is often needed.
Can plaque “spread” from one tooth to others if I ignore gingivitis?
Yes. As inflammation continues, the bacterial community can extend below the gum margin and create deeper infected sites that affect multiple teeth. This is why gum disease often becomes more widespread over time, rather than staying isolated to one spot.
Does mouthwash remove gumline plaque well enough to skip flossing or interdental cleaning?
Mouthwash alone usually cannot disrupt the biofilm in the gum crevice and between teeth, which are common hiding spots. For best results, pair brushing with floss or interdental brushes to mechanically disrupt plaque where rinses can’t reach.
If my gums bleed when I start flossing, should I stop to avoid making it worse?
Bleeding often happens when gums are inflamed and the routine is just starting. In many people, it decreases within 1 to 2 weeks of consistent, gentle cleaning. Stop and get checked if bleeding is heavy, you have spontaneous bleeding, or it does not improve after improving technique and consistency.
Can diet or specific foods cause “plaque-like” buildup near the gums?
Food debris and irritation can cause localized tenderness, but it doesn’t behave like plaque biofilm that repeatedly reforms and inflames along the gumline. If you notice a pattern of gumline redness or bleeding across multiple teeth, that points more toward plaque-driven inflammation than a one-time food injury.
Do smokers or people with diabetes experience plaque and gum inflammation differently?
They often have a higher risk that mild gingivitis progresses faster and that healing is slower. Even if symptoms seem mild, it’s especially important to maintain daily plaque disruption and not delay a dental exam if bleeding or swelling persists.
How often should I get my teeth cleaned if I’m trying to prevent plaque from hardening into tartar?
Many people need professional cleaning about every 6 months, but the right interval depends on your risk (history of gingivitis or periodontitis, heavy tartar buildup, smoking, diabetes). If you develop tartar quickly or gum inflammation keeps returning, ask your dentist for a personalized schedule rather than relying on a generic timeframe.
If plaque doesn’t “grow back” on gums like plant growth, how fast does it return after cleaning?
Plaque can re-form quickly because bacteria already present in your mouth recolonize tooth surfaces after you remove the biofilm. That’s why the daily routine matters. The aim is ongoing disruption, not a one-time “reset.”
Can gum grow over teeth? Know causes, timelines, and what to do for recession, overgrowth, or broken teeth.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.
Can humans grow new teeth? Evidence on regeneration science, what works today, and realistic replacement options

