Yes, gums can genuinely appear to grow over your braces, and it happens to a lot of people wearing fixed appliances. Most of the time it is not a sign that something is seriously wrong, but it is your mouth telling you that something needs to change, usually around hygiene, irritation, or both. The tissue is not sprouting new cells from nowhere; it is swelling, becoming inflamed, or in some cases producing excess fibrous tissue in direct response to plaque buildup and mechanical irritation from the brackets and wires. The good news is that this is almost always fixable, and in many cases the gums can return to a healthier state once the underlying cause is addressed.
Why Do Gums Grow Over Braces? Causes and What to Do
Can gums actually grow over braces, and how does it happen?
Here is a common misconception worth clearing up immediately: gums do not simply "grow" over braces the way a vine grows over a fence. What you are actually seeing is either inflammation-driven swelling that makes existing gum tissue look larger and higher, or in more persistent cases, a condition called gingival enlargement or hyperplasia, where the gum tissue genuinely proliferates and begins to engulf the brackets. Both are real and both are related to what fixed appliances do to the environment inside your mouth.
Brackets and wires are essentially plaque magnets. Research consistently shows that fixed orthodontic appliances cause increased plaque retention around the appliance sites, which triggers moderate to significant gingivitis in many patients. That inflammation causes the gum tissue, especially the little triangular peaks between your teeth called the interdental papillae, to swell, redden, and creep upward or outward toward the brackets. In some patients this progresses to true gingival overgrowth, where excess tissue physically covers part of the bracket. Studies on orthodontic patients also describe something called pseudo pocketing, where swollen tissue creates an artificially deep crevice around the tooth that looks alarming on probing but resolves once the inflammation clears.
This is a distinctly different process from what happens when gums grow around a crown, bridge, or implant, where the tissue is adapting to a fixed restoration. With braces, the mechanism is almost always about inflammation and local irritation, not biologic integration. That distinction matters because it shapes exactly what you need to do about it.
Why it happens: the main culprits
Plaque and inflammation
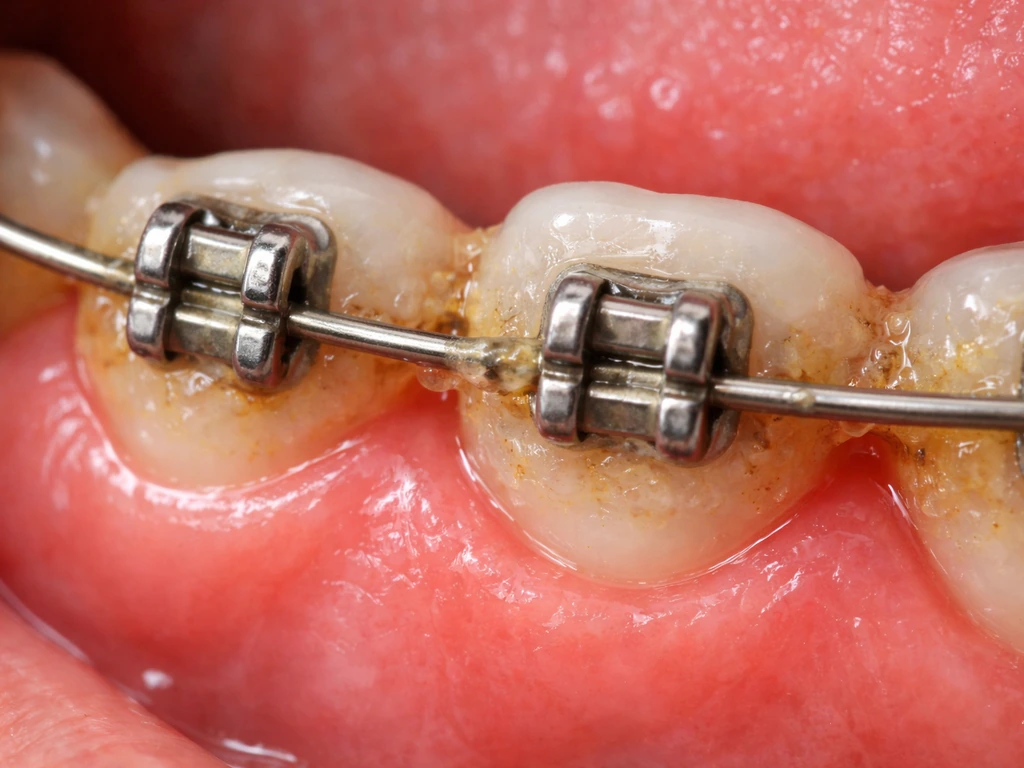
Plaque buildup is the number one driver. Brackets, elastic modules, and wire ties all create surfaces and crevices where bacteria hide and thrive. Even patients who brush regularly often miss the areas just under the wire and along the gum line because conventional brushing technique does not account for the obstacle course braces create. The bacteria in that biofilm trigger an inflammatory response in the gum tissue, and the tissue responds by swelling, bleeding, and in some cases overgrowth. Research specifically notes that altered periodontal tissue homeostasis and the interaction between plaque biofilm and mechanical stress from the appliance combine to drive gingival overgrowth in orthodontic patients.
Mechanical irritation from the appliance
Wire ends that poke out, bracket edges that dig into the cheek or gum, and constant pressure from certain parts of the appliance can all directly injure soft tissue. Clinical research identifies wire-poke injuries and appliance-related trauma as common causes of ulceration in orthodontic patients, and that repeated local trauma can trigger a localized tissue response. Think of it like any repetitive injury: the body sends resources to the area, and sometimes the healing response overshoots.
Mouth breathing and dry mouth
If you or your child tends to breathe through the mouth, especially at night, that dryness significantly accelerates the problem. Saliva is a natural defense against plaque buildup; it rinses, buffers acids, and has antimicrobial properties. Studies show mouth breathing reduces that salivary defense and self-cleaning effect, leading to faster plaque accumulation and a higher risk of gingival disease. Dry mouth from any cause, including certain medications, compounds this risk further.
Medications and other less common causes
In a smaller number of cases, gingival overgrowth has nothing to do with plaque at all, or plaque is only part of the story. Certain systemic medications, including some anti-seizure drugs, calcium channel blockers used for blood pressure, and some immunosuppressants, can cause drug-induced gingival overgrowth that typically starts one to three months after beginning the medication. If you are on any of these and also wearing braces, the two factors can compound each other significantly. This is one reason why your orthodontist needs a full medication history. Other rare systemic conditions can also cause gingival enlargement, so if the overgrowth is rapid, unusual, or does not respond to improved hygiene, a broader evaluation is warranted.
What to look for: normal vs. concerning
Some degree of gum puffiness early in orthodontic treatment is genuinely common. Your gums are adjusting to foreign hardware in your mouth. The question is whether what you are seeing is within the expected range or a sign that something needs more attention.
| Sign | Likely normal or manageable | Call your orthodontist |
|---|---|---|
| Gum color | Slight redness near brackets, especially early in treatment | Deep red, purple, or white patches; widespread discoloration |
| Swelling | Mild puffiness around brackets that improves with better brushing | Swelling that grows, spreads, or does not improve after 1-2 weeks of diligent hygiene |
| Bleeding | Light bleeding when brushing that reduces as hygiene improves | Bleeding that is heavy, spontaneous, or persists despite good hygiene |
| Tissue coverage | Gum that looks slightly raised around a bracket | Bracket partially or fully buried under tissue; tissue growing rapidly |
| Pain | Mild tenderness, especially after adjustments | Throbbing pain, pain at rest, pain when not eating or touching the area |
| Taste or odor | Slight metallic taste after brushing/flossing | Persistent bad taste, pus, or foul odor from the gum area |
| Ulcers | Small sore from a wire poke that heals within a week | Ulcers that do not heal, spread, or are associated with fever |
| Fever or facial swelling | Not expected at any stage | Any fever or spreading facial swelling: treat as urgent, call same day |
A key red flag to act on immediately is any combination of swelling, pain, and fever, or swelling that seems to be spreading from the mouth toward your face or neck. That can signal a dental infection that needs same-day professional attention, not a wait-and-see approach.
What to do right now: home care steps
If you have caught this early or you are dealing with moderate swelling without the red flags above, there is a lot you can do today before your next orthodontic appointment. The goal right now is to reduce plaque burden and protect irritated tissue from further mechanical injury.
Brushing technique for braces
- Use a soft-bristle toothbrush or an electric toothbrush with a small round head. Medium or hard bristles will further irritate already inflamed gum tissue.
- Angle the brush at 45 degrees toward the gum line, not straight across the brackets. You want the bristles working into the gum margin where plaque hides.
- Brush above the wire (between the bracket and the gum), directly over each bracket, and below the wire as three separate zones. Do not rush through them as one sweep.
- Spend at least two full minutes brushing, ideally closer to three when you have braces. Use a timer if needed.
- Rinse your mouth with water before brushing to dislodge loose food debris first.
Interdental cleaning: floss, threaders, and interdental brushes
Brushing alone does not cut it, especially with braces. Evidence consistently shows that adding interdental cleaning to brushing reduces plaque and gingivitis more effectively than brushing alone, and orthodontic patients particularly benefit. Use a floss threader or orthodontic floss to thread regular floss under the wire so you can clean between each pair of teeth. Alternatively, small interdental brushes (sometimes called proxy brushes) are excellent for getting into the space between brackets and under the wire in one motion. A water flosser is another useful tool, particularly good for flushing out debris from around brackets, though it works best as a complement to mechanical cleaning rather than a replacement for it.
Rinses and soothing options
A chlorhexidine mouthrinse used in addition to brushing and flossing has solid clinical backing for reducing plaque and gingival inflammation in orthodontic patients. Multiple systematic reviews confirm its effectiveness specifically in this population. Use it as directed, typically once or twice daily, but not as a substitute for mechanical cleaning. If chlorhexidine is not available or you want a gentler daily option, a warm salt water rinse (about half a teaspoon of salt in eight ounces of warm water) can help soothe inflamed tissue without disrupting the oral microbiome. Avoid alcohol-based mouthwashes on already irritated gums as they tend to cause more burning and dryness.
Protecting irritated areas from further trauma
If a wire end or bracket edge is actively poking your gum or cheek, roll a small piece of orthodontic relief wax into a ball and press it over the offending part. This is a short-term protective measure only; it does not heal the tissue, but it stops the mechanical injury while you wait for your appointment. Do not eat sticky or hard foods that could knock the wax off or further irritate the area. If you cannot get wax immediately, a small piece of sugarless gum works in a pinch. Schedule an orthodontic appointment as soon as you can to have the wire trimmed or the bracket repositioned properly.
How orthodontists manage gum overgrowth during treatment
When you go in, your orthodontist or a collaborating periodontist will first assess whether the overgrowth is inflammatory, mechanical, medication-related, or something else. Do not be surprised if they ask about your medications, systemic health history, and your hygiene routine in detail. The exam usually includes periodontal probing to measure pocket depths and distinguish true overgrowth from pseudo pocketing.
Immediate appliance fixes
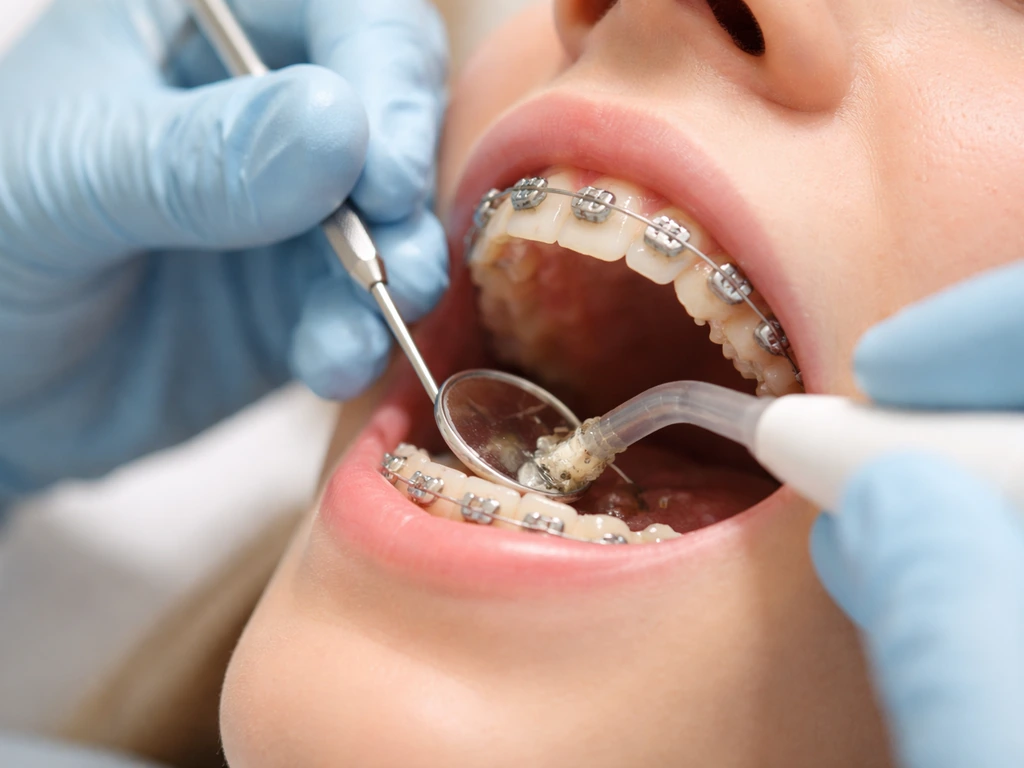
Protruding wire ends will be trimmed or bent back. Brackets causing persistent soft tissue trauma may be repositioned or temporarily debonded if they are doing more harm than good. Sharp bracket edges can sometimes be smoothed. These adjustments alone can dramatically reduce the local irritation driving overgrowth in a specific area.
Professional cleaning and hygiene restructuring
A professional cleaning to remove calculus (tartar) and subgingival plaque that you cannot reach at home is often part of the plan. Your orthodontist or hygienist will also likely walk through your brushing and flossing technique with you and prescribe a specific hygiene protocol going forward. This is not a lecture; it is a genuinely necessary step because the technique that works fine without braces is usually not adequate with them.
When medication changes or specialist referral are needed
If a medication is identified as contributing, your orthodontist will likely communicate with your prescribing physician about whether a substitute is appropriate. Stopping or changing a medication is not always possible, but even in drug-induced cases, controlling plaque aggressively can significantly reduce the severity of overgrowth.
Surgical options for persistent overgrowth
In cases where the gingival overgrowth does not respond to improved hygiene and plaque control, or where excess tissue is physically interfering with treatment, a gingivectomy may be recommended. This is a minor surgical procedure to remove the excess tissue. Case report evidence and clinical guidelines both support it as an effective option for orthodontic-induced gingival overgrowth that persists despite conservative management. Surgery is generally not considered the first step; it is reserved for situations where less invasive approaches have not been enough.
What to expect going forward: healing timelines and preventing recurrence
It is worth being honest about what "healing" means here, because this connects directly to the bigger picture of how gum tissue actually behaves. The gums are not regenerating from scratch when they improve. What you are seeing resolve is inflammation and swelling going down as the bacterial trigger is removed and the mechanical irritation is controlled. If you are wondering whether gums grow around a bridge, the key idea is similar: inflammation and irritation can make gum tissue look like it is enlarging until the trigger is controlled do gums grow around bridge. Research confirms that pseudo pocketing, one of the most alarming-looking effects of orthodontic-induced gingival enlargement, tends to resolve once the hyperplasia and inflammation clear. True new gum tissue generation is not what is happening. If your case involves actual gum overgrowth over a graft site, healing and treatment depend on the surgeon’s assessment and whether the area is still inflamed or infected does gum grow over bone graft.
With consistent improved hygiene and any necessary appliance adjustments, you can typically expect to see noticeable improvement in gum appearance and bleeding within two to four weeks. Full resolution of inflammatory swelling may take six to eight weeks of sustained effort. If there was true gingival overgrowth (as opposed to just swelling), the timeline depends on severity and whether any surgical intervention was needed. In some cases, issues like gingival overgrowth can make it look like gum is growing around an implant, so it helps to know what to expect with both situations true gingival overgrowth. After a gingivectomy, most soft tissue healing is visible within a few weeks, though complete tissue maturation takes longer.
The real challenge with braces is that prevention requires consistency across the entire time you are wearing them, not just a burst of effort when things look bad. Your risk of inflammation does not disappear between appointments. Every day that plaque sits undisturbed around a bracket is a day your gums are being challenged. Building the three-zone brushing habit and interdental cleaning into your routine from day one is far easier than trying to reverse established gingival overgrowth later in treatment.
Key ongoing habits that actually make a difference
- Brush after every meal, not just morning and night. Food debris sitting against brackets between meals significantly increases plaque accumulation.
- Use interdental brushes or floss threaders daily, ideally at night before bed when your mouth is most vulnerable to bacterial overgrowth during sleep.
- Stay well hydrated and address mouth breathing if it is a habit. Dry mouth accelerates every gingival problem braces create.
- Keep all scheduled orthodontic appointments and mention any gum changes at the start of each visit, even if you think it is minor.
- Get professional cleanings on whatever schedule your orthodontist or dentist recommends, which is often more frequent than the standard twice-yearly schedule during active orthodontic treatment.
- If you are on a medication that carries gingival overgrowth risk, talk to both your orthodontist and prescribing doctor before symptoms escalate.
The broader truth here, consistent with everything this site covers about what dental structures can and cannot do biologically, is that gums do not regenerate lost tissue the way we might hope. What they can do is recover from inflammation remarkably well when the cause is removed and they are given the right environment. That distinction should shape your expectations: the goal of treatment is controlling the cause, not banking on your body regrowing what was affected. Get ahead of it early, stay consistent, and your gums can absolutely get back to a healthy state during and after orthodontic treatment.
FAQ
Can gums really shrink back if they look like they are growing over my braces?
Yes, if the swelling is caused by gingivitis or pseudo pocketing, gums can look larger and still improve once plaque control and appliance irritation are addressed. However, if the tissue is true gingival enlargement, it may not fully reverse without periodontal treatment, orthodontic adjustments, or sometimes a gingivectomy.
How can I tell if my “gum growth” is just swelling or true gingival enlargement?
A big difference is symptoms and probing behavior. Inflammation-related swelling often comes with redness and bleeding that improves as hygiene improves, and pseudo pocketing can look like deep pockets but resolves when the gum inflammation settles. True overgrowth is more persistent and can physically cover bracket parts even after plaque is controlled.
When is gum overgrowth with braces an emergency versus something to schedule?
If there is fever, worsening swelling, facial or neck spreading, pus, or significant tooth pain, do not wait for the next orthodontic visit. Those signs can indicate infection and need same-day dental assessment. If symptoms are mild and localized, contact your orthodontist promptly and aim for a visit within days rather than weeks.
How long should I use chlorhexidine mouthwash, and can I rely on it instead of flossing?
Chlorhexidine can help reduce inflammation, but it can also stain teeth or alter taste in some people, especially with longer use. Use it only for the duration and frequency your dentist recommends, and continue mechanical cleaning since mouthrinse alone usually does not clear plaque from around brackets.
What’s the right brushing technique if my gums are enlarging over my braces?
Do not aggressively scrub with hard bristles. With braces, gums usually respond better to gentle technique plus targeted interdental cleaning (floss threader, orthodontic floss, or small interdental brushes) rather than over-brushing, which can worsen irritation.
Is relief wax enough to stop the gums from growing over braces?
If a wire is digging in, relief wax is useful short-term, but you should still arrange an adjustment. Wax can slip off with eating and does not remove plaque or eliminate the mechanical trauma that can perpetuate overgrowth.
I brush daily, so why do my gums still get puffy around the brackets?
Yes. Even if you brush, people often miss the gumline under the wire and around tie areas, so inflammation persists. Consider adding interdental brushes or flossing under the archwire, and ask your orthodontist or hygienist to check your technique during your next visit.
Can mouth breathing at night make gum overgrowth around braces worse?
Mouth breathing can increase dryness and reduce the protective effect of saliva, which can make plaque-related inflammation worse. If you notice chronic mouth breathing, it can be worth mentioning to your dentist and orthodontist, since addressing allergies or nasal blockage may indirectly improve gum health.
What if my gums started changing after I began a new medication?
Yes, drug-induced gingival overgrowth can start relatively soon after starting certain medications, and braces can compound the irritation. If your gum changes began after a medication change, tell your orthodontist and confirm with your prescribing clinician rather than stopping medication on your own.
Should I keep my braces on and start home care, or do I need my orthodontist to adjust things right away?
You can start immediately with safe, gentle interdental cleaning and rinses, but if the overgrowth is covering bracket parts, interfering with tooth movement, or feels rapidly worsening, prioritize orthodontic assessment. Treatment planning often needs an exam and possibly professional cleaning to remove calculus and to distinguish swelling from actual enlargement.
When do dentists consider a gingivectomy instead of more cleaning or brace changes?
If you are on the verge of tissue removal, imaging is not usually the first decision point, but a periodontal evaluation with probing helps determine severity. A gingivectomy is generally considered when the overgrowth does not improve with plaque control and appliance adjustments, or when it physically blocks progress.
Learn if gums can grow around a dental bridge, what gaps mean, inflammation signs, and next steps to protect abutment te
Find out if gums can regrow over crown margins, what affects recession vs stability, and what steps to take now.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

