Gums do not grow back after Invisalign on their own. If you have true gingival recession (meaning the gum margin has migrated below the cemento-enamel junction and root surface is exposed), that tissue is gone permanently unless a periodontist surgically restores it. What can improve on its own is gum swelling and inflammation that made recession look worse than it really was. Once inflammation settles down, the gum margin can appear to bounce back a little, but that is the tissue returning to its healthy baseline, not actual regrowth over lost root surface.
Will Gums Grow Back After Invisalign? What to Expect
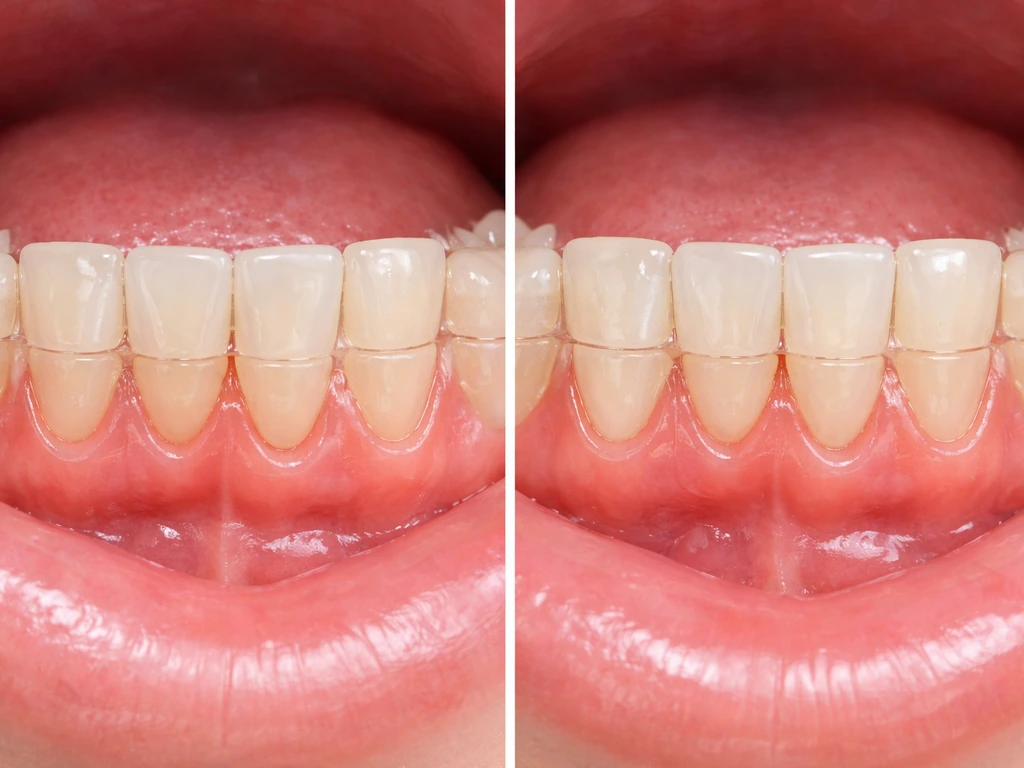
What actually happens to your gums during Invisalign (and braces)
Orthodontic tooth movement, whether with clear aligners or traditional brackets, puts mechanical force on the teeth and the bone and soft tissue surrounding them. When a tooth is pushed or pulled in a direction, the alveolar bone on the leading side gets resorbed and new bone forms on the trailing side. The gum tissue follows the bone, which is why tooth movement can affect the gumline.
There is also a hygiene factor. Invisalign trays trap bacteria against teeth and gums if you are not meticulous about cleaning. Even though research suggests clear aligners are somewhat easier to keep clean than fixed metal braces (since you remove them to eat and brush), any orthodontic treatment increases your risk of plaque accumulation, which drives gingival inflammation. Inflamed gums bleed, swell, and over time can recede. Studies comparing fixed appliances to clear aligners have found that fixed appliances show a more significant increase in gingival recession at around the 3-month mark, while clear aligners tend to show less of that short-term change, partly because of the hygiene advantage.
Your gum biotype matters enormously here. People with thin, scalloped gingival tissue (the tissue looks delicate and you can almost see the teeth through it) are far more vulnerable to recession than people with thick, flat gingival phenotypes. Research consistently identifies thin biotype as one of the strongest predictors of orthodontic-related gum recession. If you have naturally thin gums going into Invisalign, you are at higher risk regardless of how good your hygiene is.
Will gums grow back after Invisalign? The real answer
Here is the honest, myth-busting answer: true gingival recession does not reverse itself. The gum tissue that has migrated apically (toward the root) and the bone that has been lost beneath it do not spontaneously regenerate. Research linking recession to bone loss estimates that 1 mm of gingival recession is associated with roughly 2.8 mm of bone dehiscence underneath. That is a significant structural loss, and the human body has no natural mechanism to rebuild it without intervention.
What many people experience as gums "growing back" after finishing Invisalign is actually the resolution of reversible gingival inflammation. During treatment, gums may be red, swollen, and slightly rolled away from the teeth due to plaque irritation. Once the trays are out, hygiene improves, and inflammation settles, the tissue firms up and sits slightly higher again. Clinically, waiting at least 6 months after active orthodontic treatment before measuring recession is recommended for exactly this reason: you want the reversible inflammatory component to fully resolve before deciding what is permanent and what is not.
Another thing to understand is what "grow back" would even mean clinically. Full root coverage means gum tissue sitting back at or above the cemento-enamel junction (CEJ), covering exposed root. Partial coverage means some improvement but not complete. Stabilization means recession stops getting worse. Spontaneous reversal of true recession (not just reduced inflammation) essentially does not happen in adults. Studies on orthodontic patients confirm this: some post-treatment improvement is seen, but it reflects inflammation resolution, not tissue regeneration.
Why gums sometimes look worse during or right after treatment
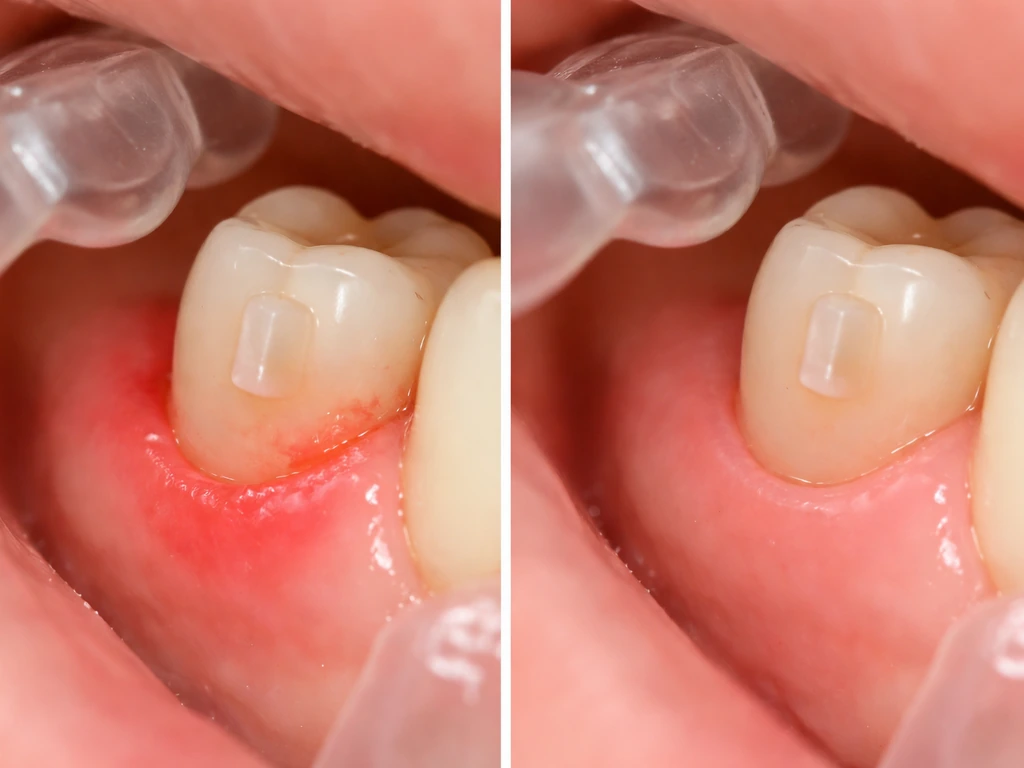
Understanding why recession happens during Invisalign helps you figure out which category your situation falls into. The causes are usually a mix of several factors at once.
- Tooth movement toward thin bone: When teeth are moved labially (forward toward the lips), the thin buccal bone plate can become even thinner or develop a dehiscence, creating the perfect condition for gum recession. Research is clear that moving teeth outside their alveolar bone boundaries dramatically increases recession risk.
- Plaque and gingival inflammation: Poor cleaning around trays leads to bacterial buildup. Gingivitis by itself can cause the gum margin to appear lower, and chronic gingivitis that goes untreated can progress to periodontitis with permanent attachment loss.
- Pre-existing recession: Many people start Invisalign with minor recession they were never told about. Treatment does not cause it, but it may worsen slowly over time, especially with additional mechanical stress.
- Thin gingival biotype: Thin tissue has less collagen density and less resilience. Even minor trauma or plaque irritation can tip thin-biotype gums into recession more easily than thick tissue.
- Aligner trauma: Poorly fitting trays or edges digging into the gumline can mechanically irritate tissue directly.
- Periodontal disease: If you had undetected or inadequately treated periodontal disease when you started treatment, orthodontic forces can accelerate bone and attachment loss significantly.
- Age and tobacco use: Both are known independent risk factors for recession, and they stack on top of orthodontic risk.
When things improve on their own vs when you need intervention
The key is distinguishing between pseudo-recession (swollen, inflamed tissue making the gumline look lower) and true recession (actual apical migration of the gum margin). Here is a practical way to think about the two timelines.
| Situation | Likely outcome | Timeframe |
|---|---|---|
| Gums looked puffy/red during treatment, improving since finishing | Inflammation resolving, gumline may return close to baseline | 4 to 6 months post-treatment |
| Gums appeared to recede gradually during treatment | May have some improvement, but any true recession is likely permanent | Reassess at 6-month mark; consult periodontist |
| Root surface visibly exposed, tooth looks longer than before | True recession, will not reverse without surgical intervention | See a periodontist now, do not wait |
| Recession worsening during retention phase | Common delayed effect; may indicate retainer trauma or ongoing hygiene issues | Reassess immediately, do not attribute to treatment alone |
| Thin biotype with minor recession pre-treatment, now slightly worse | True recession unlikely to self-correct; grafting may be needed | Periodontal evaluation as soon as possible |
It is worth knowing that recession can also progress during the retention phase, not just during active aligner wear. Studies have found a significant increase in recession during the retention period, sometimes appearing as a delayed effect of orthodontic tooth movement. So if you are done with your trays and just wearing retainers, your gums are not necessarily in the clear. Keep monitoring.
One scenario where improvement is genuinely possible: if you had gingival overgrowth or hyperplasia (gums growing over teeth rather than receding), finishing treatment and restoring good hygiene can reduce that overgrowth substantially. That is the opposite problem from recession, but some people confuse the two.
What to do right now: assessing your gums and fixing the problem
Step 1: Get a proper periodontal evaluation
Do not just rely on a visual check in your bathroom mirror or a quick look during a routine cleaning appointment. Ask for a comprehensive periodontal evaluation, ideally with a periodontist if you have visible recession or concerns your general dentist cannot clearly address. The measurements you need are recession depth (how far the gum margin is from the CEJ), probing depth at each site, clinical attachment level, width of keratinized gingiva, and bleeding on probing. Bone levels via X-rays are also important. These numbers tell you whether what you are seeing is shallow recession that may be manageable, or deeper recession with bone loss that needs surgical attention.
Step 2: Ask the right questions
- "What is my recession depth at each affected site and has it changed since my last measurements?"
- "Do I have adequate keratinized gingiva? Is the attached gingiva at least 1 mm and total keratinized tissue at least 2 mm?"
- "What is my gingival biotype, and does it put me at higher risk going forward?"
- "Is there bone dehiscence under the recession, and does that change my surgical options?"
- "Am I a candidate for root coverage surgery, and what procedure would give me the best outcome?"
- "Should my orthodontist be involved in adjusting tooth position before or alongside any gum surgery?"
Step 3: Understand your treatment options
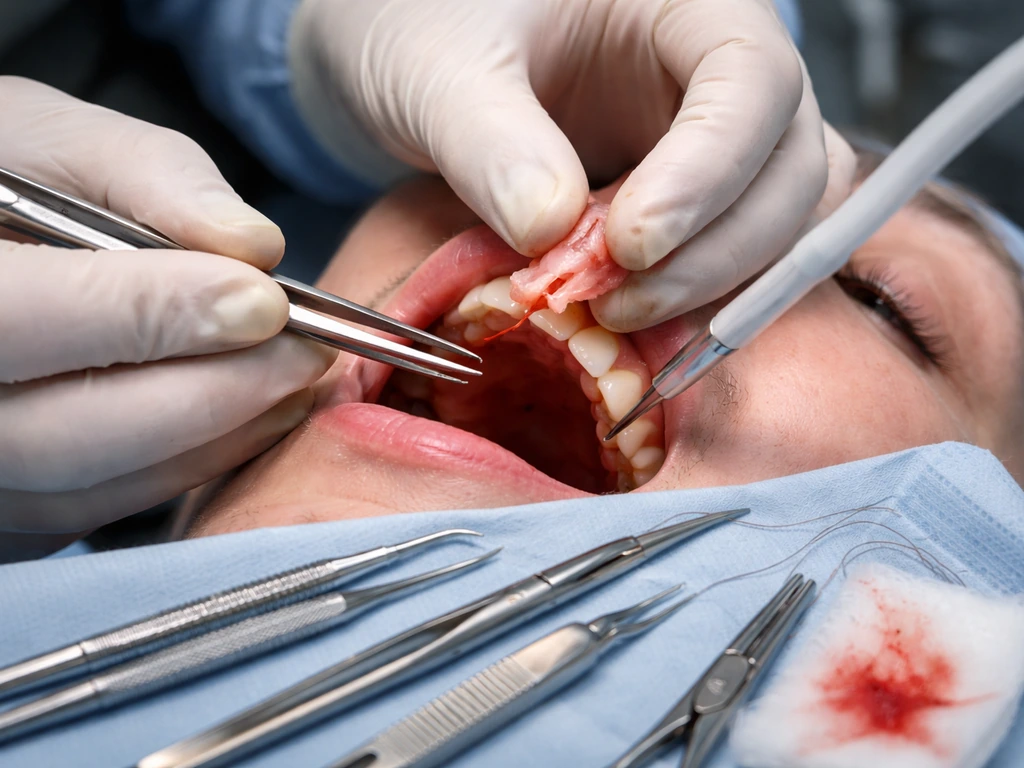
If true recession is confirmed and it is bothering you cosmetically or causing sensitivity, surgery is the main pathway. The gold standard for root coverage is the subepithelial connective tissue graft (SCTG), which AAP research consistently identifies as providing the best root coverage outcomes. A small piece of connective tissue is harvested from the palate and placed under a flap at the recession site. For cases where graft harvesting is difficult (limited palatal tissue, multiple recession sites), a coronally advanced flap (CAF) with acellular dermal matrix can be an alternative with good outcomes. Studies on orthodontic-associated Miller Class III recession (where the bone has already migrated apically) using coronally advanced flap with connective tissue graft report meaningful clinical improvements in recession depth, probing depth, and width of keratinized tissue at one year. Just know that Miller Class III defects are harder to fully cover than Class I or II defects.
Before any gum surgery, your periodontist may want your orthodontist involved. If a tooth is sitting too far forward in the arch or outside the alveolar boundary, repositioning it first (or adjusting planned movement) can create a better bone environment for the graft to succeed. The two specialties should communicate if both are involved in your care.
Preventing further gum loss during and after Invisalign
If you are still in treatment or just finished, you have a real opportunity to prevent further damage. Hygiene is the most controllable variable. Brush twice daily with a soft-bristled brush and a gentle technique (no scrubbing side to side, which is a common cause of mechanical recession in its own right). Floss or use an interdental cleaner every day. Research on orthodontic patients comparing water flossers to traditional floss found both effective, and water flossers can be easier to use consistently during treatment.
Remove your aligners before every meal and clean them before reinserting. Never sleep in dirty trays. Rinse after eating even when you cannot brush immediately. If you develop significant gingival inflammation during treatment, short-term chlorhexidine mouthwash can help bring it under control. Studies support its use for reducing plaque and inflammation in orthodontic patients, though it is meant for short-term use (typically 2 to 4 weeks) because of staining and taste effects.
If your periodontist identifies thin biotype or inadequate keratinized gingiva before or during treatment, a prophylactic free gingival graft (to thicken and widen the keratinized zone before tooth movement begins) is sometimes recommended. This is not about cosmetics: it is about giving the tissue enough resilience to survive orthodontic forces. Some cases of Invisalign use with pre-existing severe recession have been managed with simultaneous periodontal monitoring and even concurrent tissue management, showing that it is possible to move teeth and stabilize gums at the same time with the right oversight.
After finishing Invisalign, schedule periodontal monitoring every 3 to 6 months rather than only yearly cleanings. Recession that starts or worsens during the retention phase can be caught early. Your retainer should also be checked to make sure it is not traumatizing the gum margin at any point. A lingual retainer, in particular, has been linked in longitudinal research to delayed recession at the mandibular anterior teeth, so that area deserves extra attention.
The broader question of whether gums can grow back applies across many dental situations, from tartar removal to scaling to procedures like osseous surgery or crown lengthening. Gums generally do not regrow after crown lengthening because true recession and lost supporting tissue are not spontaneously replaced do gums grow back after crown lengthening. If you are wondering whether gums can grow back after wisdom teeth removal, the answer depends on whether you are dealing with temporary healing or true recession of the gum margin. If you are considering osseous surgery, it helps to set expectations: true gum recession and lost bone typically do not regrow on their own. In nearly every scenario, the biology is the same: inflamed gum tissue can recover and appear to "fill back in" once the irritant is removed, but actual recession with exposed root and lost bone does not reverse without surgical help. Invisalign is no exception to that biological reality. That is why the same answer applies to do gums grow back after veneers: true gum recession typically will not regenerate on its own, though inflammation may improve.
FAQ
How long after Invisalign should I wait before assuming my gums will not improve anymore?
If you are trying to distinguish reversible inflammation from true recession, wait at least 6 months after active aligner treatment before making a final call. During that window, inflammation-related “rollback” of the gumline can happen, but tissue that has genuinely migrated and exposed root generally will not regenerate.
If I notice my gumline is lower after I finish Invisalign, does that mean my gums will never improve?
Not necessarily. Gum appearance can drop during retention if inflammation returns or if a retainer irritates the margin. A periodontal exam with measurements (recession depth, clinical attachment level, and bleeding on probing) is the only way to tell whether it is true recession worsening or temporary swelling.
What should I ask a dentist or periodontist to measure to confirm true recession?
Ask for recession depth relative to the CEJ at specific teeth, probing depth at the same sites, clinical attachment level, width of keratinized gingiva, and bleeding on probing. Also request an assessment of bone levels with X-rays, because visible gum recession can look similar even when bone loss is or is not present.
Can Invisalign trays themselves cause gum recession even if my hygiene is excellent?
Yes, hygiene is only one factor. Tooth position and movement direction matter, and some patients have a thin biotype or limited keratinized tissue, which makes the gum margin more vulnerable to the mechanical effects of moving teeth, even with excellent cleaning.
Is flossing enough, or do I need additional interdental cleaning during Invisalign?
Flossing or interdental brushes are often effective, but consistency matters most. If traditional floss feels difficult with aligners in your routine, an oral irrigator can be a practical backup for daily cleaning, especially for patients who struggle to reach posterior areas consistently.
Could my retainer be contributing to delayed gum recession?
It can. If a retainer edge rubs or presses along the gum margin, it may keep the area chronically inflamed or mechanically traumatized. Have your retainer fit checked if recession appears during retention, particularly at the mandibular anterior teeth.
What are the chances that root coverage surgery will fully cover the recession I have after Invisalign?
Coverage depends heavily on defect classification and site conditions. Miller Class I and II defects tend to respond better than Class III, where prior bone migration apically reduces the predictability of complete coverage even when grafting is done well.
If I have recession after Invisalign, should I treat it immediately or wait?
You usually should stabilize the situation first. Waiting about 6 months after active orthodontics helps ensure inflammation has settled so the periodontist can plan based on the true, measurable recession and bone condition rather than a temporary appearance.
Can gums look thicker after Invisalign, but still be a problem underneath?
Yes. Improved color and firmness can mean inflammation has resolved, which may make the gum margin look more “up.” But if clinical attachment level and recession depth do not improve in a measurable way, it can still represent true tissue loss that may require periodontal treatment.
Does brushing side-to-side or aggressive cleaning during Invisalign affect my gumline?
It can. Mechanical trauma from scrubbing is a common self-inflicted contributor to recession. Use gentle technique with a soft brush, and focus on plaque removal without forcing the gum margin away from the teeth.
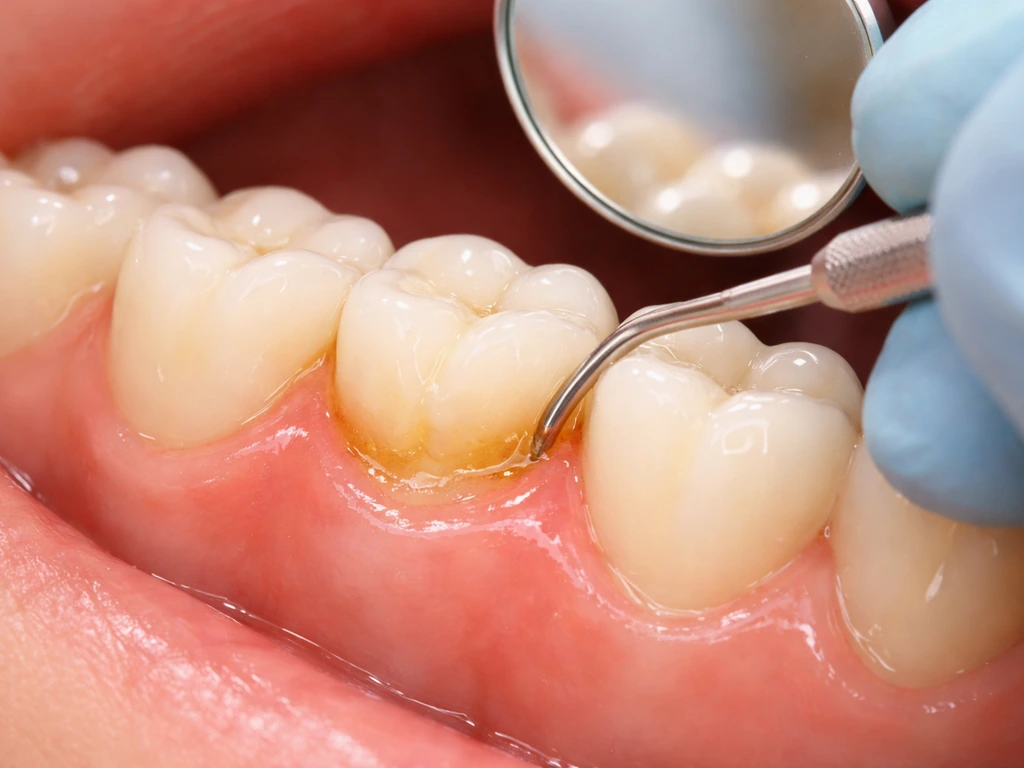
Learn what happens to gums after tartar removal, which changes are reversible, and when recession needs more care.
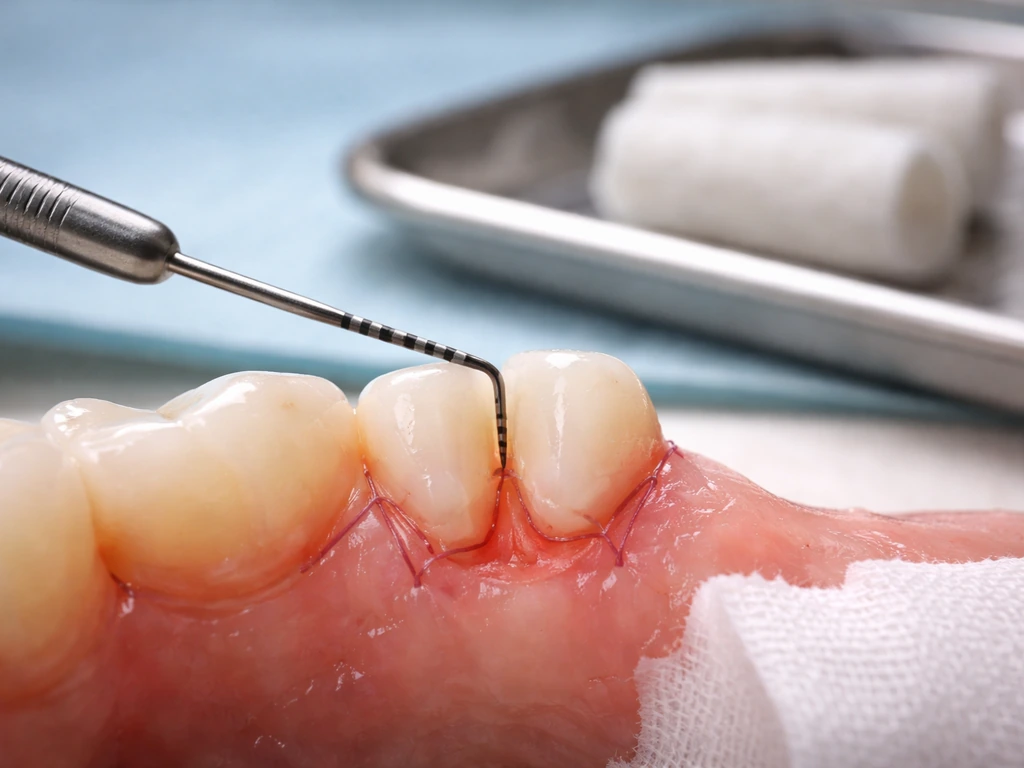
Learn if gums truly regrow after osseous surgery, typical timelines, factors that affect results, and red flags.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

