Here is the short answer: human teeth do not grow back once a permanent tooth is lost. But the process of how teeth actually form and erupt in the first place is fascinating, and understanding it helps explain why that limitation exists, what limited repair is possible, and what your real options are when something goes wrong. Whether you are a parent watching your child's first tooth push through, an adult dealing with a lost molar, or just genuinely curious about dental biology, this guide walks through all of it.
How Do Teeth Grow Back: Primary to Adult Tooth Timeline
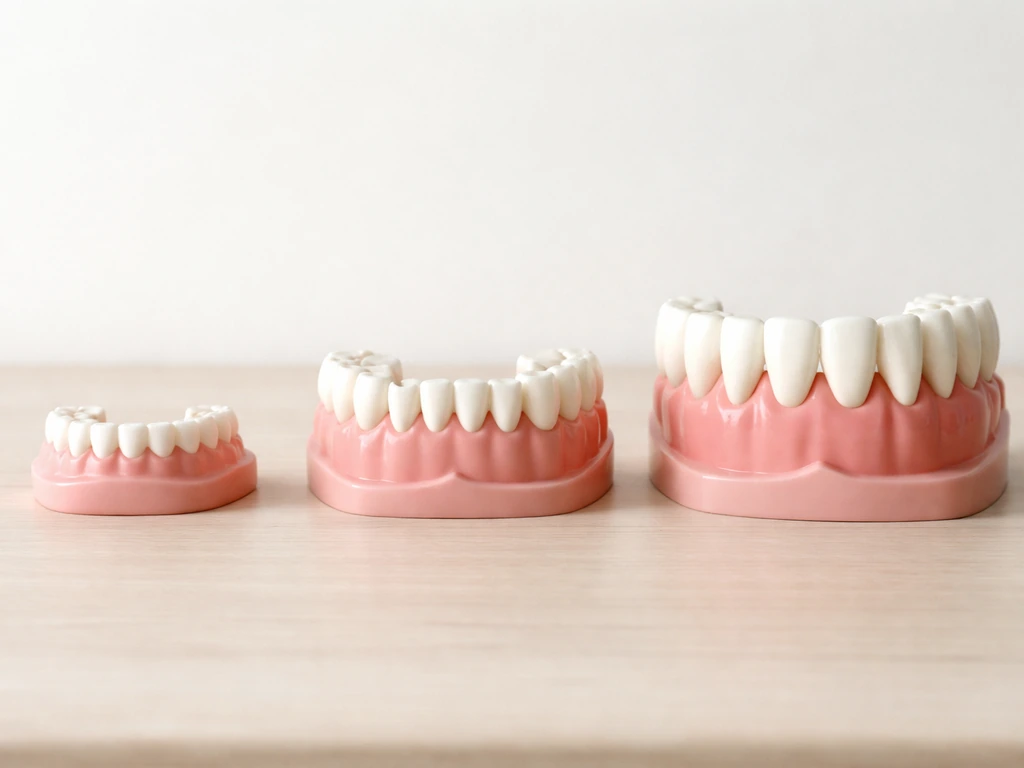
How teeth actually start forming
Tooth development begins long before you ever see a tooth. The whole process, called odontogenesis, starts in the embryo and follows a reliable sequence of five stages: initiation, the bud stage, the cap stage, the bell stage, and maturation. During initiation, a strip of tissue called the dental lamina forms along the future gum line. Epithelial cells in that lamina then cluster into a tooth bud, which is the very first physical sign of a tooth taking shape.
By the cap stage, three distinct structures have appeared: the enamel organ (which will eventually produce enamel), the dental papilla (which will become dentin and pulp), and the dental follicle (which surrounds the whole structure and gives rise to the supporting tissues). Together these three form what is called the tooth germ. If you have ever wondered where teeth grow from, this is the answer: every tooth in your head started as a microscopic cluster of cells in your embryonic jaw tissue.
The bell stage is when the tooth germ really takes on its final shape, with the enamel organ folding in ways that define the eventual crown form. After that comes maturation, where hard tissue actually mineralizes. Researchers have pinpointed specific intrauterine timepoints for these transitions: human incisor tooth germs are already at the late cap stage by around the 12th week of gestation, and reach the late bell stage by about the 20th week. In other words, your teeth were forming months before you were even born.
Baby teeth vs. adult teeth: how the swap works
Humans are diphyodont, meaning we get exactly two sets of teeth across our lifetime: the primary (baby or deciduous) set and the permanent (adult) set. Both sets develop from tooth germs within the jaws, but they do so at different times and have distinct structural differences. Primary teeth have thinner enamel and dentin, and their pulp chambers are proportionally larger relative to the crown size compared to permanent teeth. That is partly why cavities in baby teeth can progress faster and why dentists treat them somewhat differently.
The replacement process is not simply a baby tooth falling out and an adult tooth popping in. The permanent tooth germ develops beneath the primary tooth and, as it matures, triggers root resorption in the baby tooth above it. Osteoclasts (the same bone-dissolving cells active in bone remodeling) break down the primary tooth's root through a process driven by signaling molecules including RANKL. As the root dissolves, the baby tooth loosens and eventually falls out, clearing the path for the permanent tooth to erupt. Understanding how teeth grow through gums during this eruption phase helps clarify why the process can be uncomfortable and take weeks.
One clinically important rule: if a baby tooth is knocked out early, it should NOT be replanted. Replanting a primary tooth risks damaging the permanent tooth germ developing just beneath it. The same is not true for permanent teeth, where prompt replantation can make the difference between saving or losing the tooth.
Tooth eruption timelines from infancy to wisdom teeth
Knowing roughly when teeth should appear helps parents and adults recognize what is normal and what might need a dentist's attention.
| Teeth | Set | Approximate Eruption Age |
|---|---|---|
| Central incisors (lower) | Primary | 6–10 months |
| Central incisors (upper) | Primary | 8–12 months |
| Lateral incisors | Primary | 9–16 months |
| First molars | Primary | 13–19 months |
| Canines (cuspids) | Primary | 16–23 months |
| Second molars | Primary | 23–33 months |
| Full primary set complete | Primary | By about age 3 |
| First permanent molars | Permanent | Around age 6 |
| Central incisors (permanent) | Permanent | 6–8 years |
| Lateral incisors (permanent) | Permanent | 7–9 years |
| Canines and premolars | Permanent | 9–13 years |
| Second molars | Permanent | 11–13 years |
| Third molars (wisdom teeth) | Permanent | 17–25 years (or never fully) |
Most children start teething around 6 months, and the full set of 20 primary teeth is usually in place by age 3. The transition to permanent teeth begins around age 6, when the first permanent molars erupt (these often go unnoticed because they come in behind the baby teeth rather than replacing one). By ages 12 to 13, most permanent teeth excluding wisdom teeth are in place. Wisdom teeth, or third molars, arrive much later, typically between ages 17 and 25, and in many people they either erupt partially, come in at an angle, or never fully emerge. If you are in that window and still waiting, the article on why your teeth haven't grown in yet covers the common reasons for delayed eruption.
Can teeth actually grow back? The honest biological answer
No. Once a permanent tooth is lost, your body cannot grow a new one. Unlike bone, which retains meaningful regenerative capacity throughout life, permanent teeth have no replacement mechanism once they are gone. The dental lamina, that strip of epithelial tissue that generates tooth germs during development, becomes largely inactive after the permanent teeth have formed. There is no hidden reserve of tooth germs waiting to be activated.
This is in stark contrast to many animals. Sharks, for example, maintain an active dental lamina throughout their lives, which continuously produces new tooth rows. Geckos are polyphyodont and can replace each of their teeth roughly every three to four months through odontogenic stem cells in their dental lamina. Researchers studying why extra teeth grow in humans (a condition called hyperdontia) have found some echoes of those embryonic pathways reactivating, but these are aberrations, not a usable regenerative system. The shared stem cell characteristics between human rested lamina and shark regenerative lamina are real and being actively researched, but they have not translated into clinical tooth regeneration for humans yet.
The dental follicle does contain progenitor stem cell populations that contribute to tooth formation during development, and subpopulations of dental epithelial-mesenchymal stem cells are found in pulp and the periodontium in both deciduous and permanent teeth. Scientists are studying whether these could be harnessed for regenerative therapies, but as of today those approaches remain experimental.
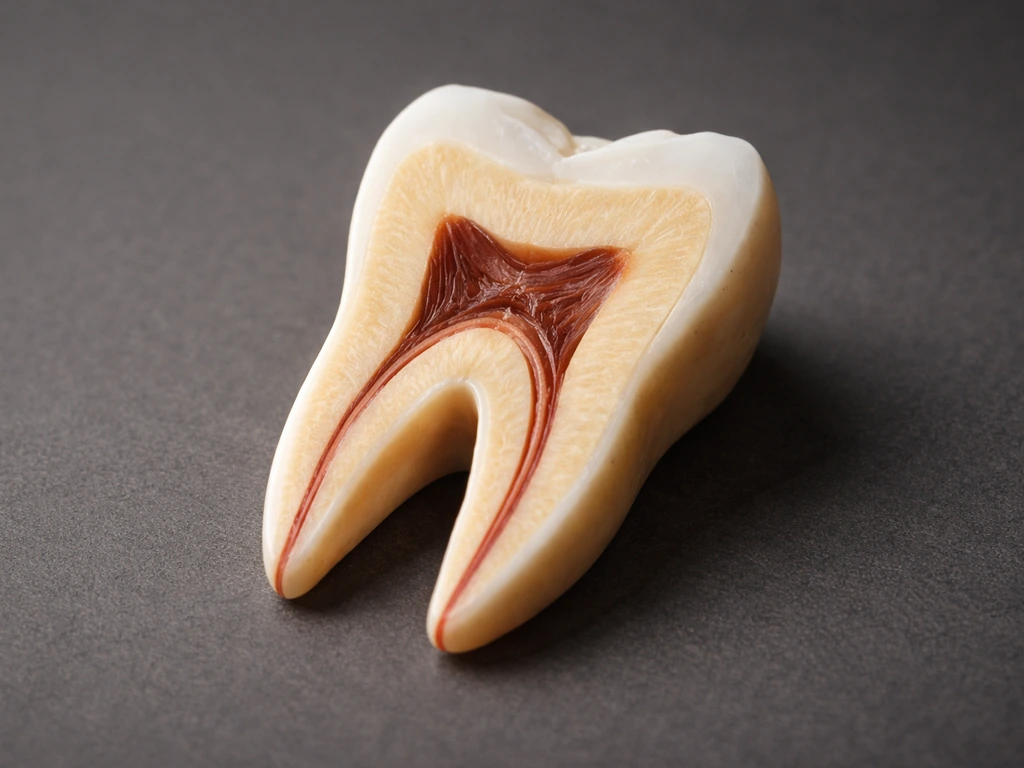
Enamel, dentin, and pulp: what can repair itself and what can't
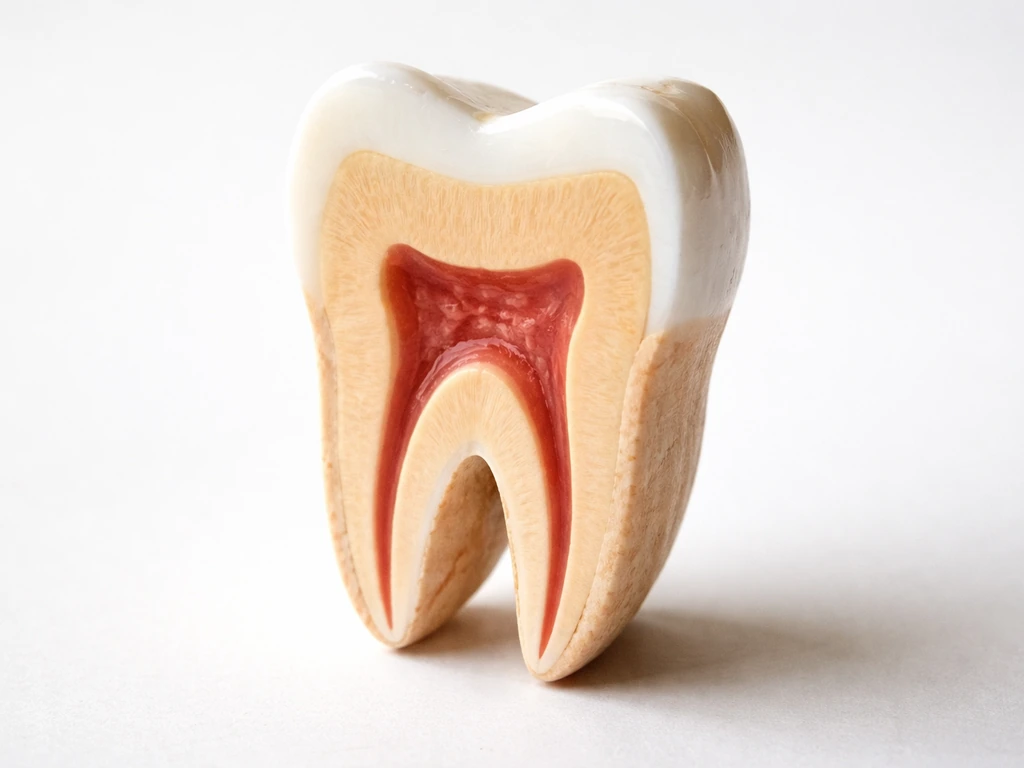
Not all tooth structures are equal when it comes to repair. The differences matter a lot for understanding what is possible after damage or decay.
Enamel
Enamel is the hardest substance in the human body, but it cannot regenerate. The cells that produce enamel, called ameloblasts, die off after the tooth fully erupts. Once enamel is gone, whether through acid erosion, decay, or physical damage, your body cannot replace it. Fluoride and remineralization can slow early-stage demineralization and partially harden weakened enamel, but that is a far cry from growing new enamel. If you have ever wondered why your teeth grew in yellow, one common reason is enamel that formed thinner or with less mineral density, which reveals the yellowish dentin beneath.
Dentin
Dentin is derived from the dental papilla during tooth development and, unlike enamel, does have some limited repair capacity. Odontoblasts, the cells lining the pulp chamber, can produce new dentin in response to injury. This is called reactionary or reparative dentin. However, research is clear that this is not true regeneration: hard tissue formed after the death of primary odontoblasts lacks the tubule structure characteristic of genuine dentin and should be classified as reparative, not regenerative. Pulp capping procedures using bioactive materials like mineral trioxide aggregate work by triggering this dentin bridge formation, which is clinically useful but not the same as regrowing original tooth structure.
Pulp
The pulp is the living core of the tooth containing nerves, blood vessels, and connective tissue. Pulp can mount an inflammatory response to injury and, under the right conditions, can survive mild irritation. But once the pulp becomes necrotic (dead), it does not regenerate. Root canal treatment removes the dead pulp and seals the space. Regenerative endodontics, an emerging clinical area, uses stem cell approaches to try to revascularize and repopulate pulp space, particularly in immature permanent teeth in younger patients, but it is not yet a routine option for most adults.
What to do if you've lost or broken a tooth right now
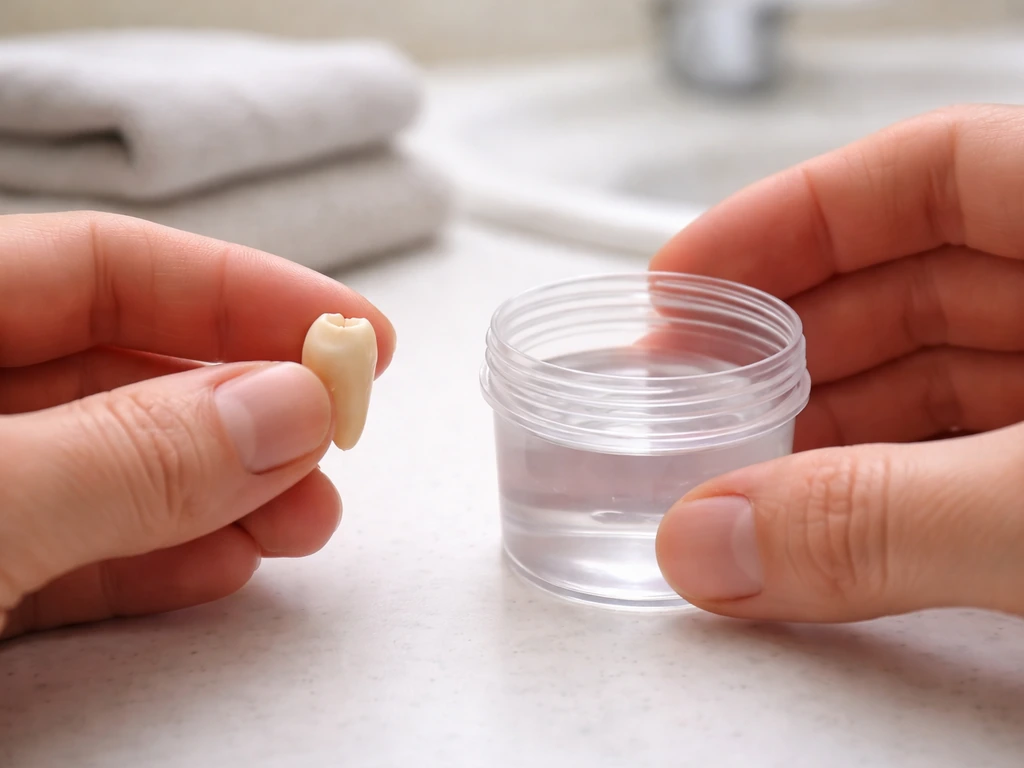
If a permanent tooth has been knocked out completely (avulsed), time is the single most important factor. The goal is to keep the periodontal ligament cells on the root alive until a dentist can replant and splint the tooth. Here is what to do, in order:
- Pick up the tooth by the crown, not the root. Touching the root damages the periodontal ligament cells.
- If the tooth is dirty, rinse it gently with saline or milk. Do not scrub it.
- Try to replant it immediately into the socket and hold it in place. Bite down gently on a clean cloth.
- If replanting on the spot is not possible, store the tooth in milk, Hank's Balanced Salt Solution (HBSS), or between your cheek and gum. Do not use tap water or let it dry out.
- Get to a dentist or emergency room within 30 minutes. Outcomes drop sharply when the tooth has been outside the mouth for more than one hour in dry conditions.
- Once replanted, the tooth is typically splinted for about two weeks according to current IADT guidelines, and follow-up monitoring for root resorption and pulp health is essential.
For a broken or chipped tooth that has not been knocked out entirely, rinse your mouth with warm water, apply a cold pack to reduce swelling if needed, and see a dentist within 24 hours. Even a small chip can expose dentin or pulp and leave you vulnerable to pain and infection.
When a permanent tooth cannot be saved or was lost long ago, the evidence-based replacement options are dental implants (a titanium post placed into the jawbone that acts as an artificial root, topped with a crown), a fixed dental bridge (anchored to adjacent teeth), or a partial denture. Implants are generally considered the closest functional replacement, but they require adequate bone volume and a healing period. Your dentist can assess which option makes the most sense given your specific situation.
Myths about growing teeth back, sorted by what science actually says
There is a lot of noise online about regrowing teeth naturally. Let's go through the most common claims directly.
- Myth: Oil pulling, diet changes, or supplements can regrow lost teeth. Reality: None of these can regenerate a tooth structure that no longer exists. They may support gum health or slow enamel erosion in minor ways, but they cannot produce new enamel, dentin, or a whole tooth.
- Myth: Stem cell treatments are available now to regrow teeth. Reality: Stem cell-based tooth regeneration is an active research area, and the biological building blocks (dental stem cells, shared signaling pathways with polyphyodont animals) are genuinely interesting. But as of today, no proven clinical therapy can regrow a complete human tooth from scratch. Trials are ongoing, but this is not something you can book an appointment for.
- Myth: Third molars are 'extra' teeth and prove the body can grow new ones later. Reality: Wisdom teeth are part of the original permanent tooth set and form from tooth germs laid down in childhood. Their late eruption is just a developmental timing quirk, not evidence of new tooth generation. Issues like teeth growing in the wrong position are explained in detail in the article on why teeth grow behind teeth.
- Myth: Humans used to have more sets of teeth. Reality: There is no credible evidence that ancient humans were more polyphyodont than modern humans. The diphyodont pattern (two sets only) is consistent across the fossil and anthropological record.
- Myth: Enamel can fully remineralize with the right toothpaste. Reality: Fluoride and hydroxyapatite toothpastes can support remineralization of early, subsurface lesions and help harden weakened enamel, but they cannot rebuild enamel that has been fully lost or restore original enamel thickness.
- Myth: Crooked or misaligned permanent teeth are just a genetic fluke and can't be explained. Reality: There are well-documented developmental and environmental reasons why adult teeth come in misaligned, all grounded in jaw development and eruption sequence biology. The full explanation is covered in the article on why teeth grow crooked.
The bottom line on all of these: if someone is selling you a product or protocol that claims to regrow a tooth, the biology does not support it. What does exist is genuinely effective restorative dentistry, and the earlier you see a dentist after losing or damaging a tooth, the better your outcomes. That is not a myth, it is the most consistent finding across all the clinical research.
FAQ
If enamel is the hardest tissue, why can’t it grow back after a cavity or erosion?
No. Once the enamel has fully formed and the ameloblasts have died, enamel cannot regrow. After enamel is lost to cavities, acid erosion, or chips, treatments focus on stopping further loss (fluoride, remineralization) and restoring the missing surface with fillings or crowns.
Is it ever okay to wait with a cavity in a baby tooth since it will fall out anyway?
Baby teeth can show pain or infection, but the treatment priority is different because preserving the space and protecting the developing permanent tooth matter. Even so, a dentist may still remove a badly decayed baby tooth if it is causing an abscess or can’t be restored safely.
How do I know whether a small chip in a permanent tooth is urgent?
Chipping or a small crack can expose dentin, increasing sensitivity and infection risk even if the tooth looks minor. If there is pain when biting, lingering cold sensitivity, visible discoloration, or a rough edge, you should be evaluated promptly, ideally within 24 hours for chips.
What makes a knocked-out (avulsed) permanent tooth different from other injuries, and why does timing matter so much?
The most time-sensitive injuries are complete avulsions of permanent teeth. For a knocked-out permanent tooth, keeping the periodontal ligament cells alive is critical, so you should seek emergency dental care, follow tooth-safe storage guidance (for example, certain liquids recommended by clinicians), and avoid scrubbing the root.
What should I do if my child’s baby tooth is knocked out, can I replant it at home?
No, replanting a primary (baby) tooth is generally discouraged because it can injure the permanent tooth germ beneath it. If a primary tooth is knocked out, dental advice should focus on evaluation of the injury and monitoring rather than trying to put the baby tooth back.
If a permanent tooth hasn’t erupted yet, does that always mean something went wrong with tooth development?
Yes, permanent teeth can be delayed even when the tooth germs are developing normally. Common causes include missing or impacted teeth (especially wisdom teeth), genetic variation in timing, insufficient space from crowding, or hormonal and medical factors. A dentist can use an exam and X-rays to distinguish normal delay from obstruction.
Does “late eruption” for wisdom teeth count as teeth growing back, and when should I worry?
Wisdom teeth are the main teeth with common late or incomplete eruption, but they are not the same as “not growing back.” If third molars are impacted or only partially erupt, symptoms can require evaluation, because partially erupted teeth are more prone to gum inflammation and infection.
How does waiting after a lost permanent tooth affect implant options?
Bone loss around a lost tooth can progress over time, which affects whether an implant will be possible and how complex it becomes. If you are considering an implant, earlier evaluation matters so the site can be assessed for bone volume and whether bone grafting is needed.
If a tooth seems “stuck” behind another one, is it usually a space problem or an impaction problem?
Often, but not always. Some apparent crowding is related to tooth position or jaw size, and the correct approach may be orthodontic rather than extracting. A dentist or orthodontist can determine whether delayed eruption is due to space constraints or impaction using imaging.
What can I do to maximize my chances of saving a tooth, even if I can’t regrow it?
You cannot reliably regenerate a tooth at home, but you can protect what remains. Good targets are preventing new demineralization (fluoride toothpaste, address dry mouth), managing sensitivity, and getting early dental treatment for cracks or early decay before pulp damage occurs.
If reparative dentin can form after injury, why might I still end up needing a root canal?
Reparative dentin may form after some injuries, but it does not restore normal dentin tubule structure, and it does not bring back dead pulp. That is why a tooth can still need procedures like pulp treatment, even if symptoms improve temporarily.
If I replant a permanent tooth quickly, does it always stay healthy long term?
No. Replanted permanent teeth can sometimes be saved, but the prognosis depends on factors like how long the tooth was out, storage conditions, patient age, and contamination level. Splinting and follow-up are required because complications such as infection or root resorption can occur.
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

