Yes, wisdom teeth can erupt in your 40s. It sounds unlikely, but it happens more often than most people expect. The key thing to understand is that this isn't new tooth growth. Your wisdom teeth formed decades ago. What's happening is that a tooth that has been sitting dormant or partially impacted in your jaw is finally pushing through, sometimes triggered by changes in jaw space, shifting of adjacent teeth, or just the unpredictable nature of third molar development. True regrowth of a completely unformed tooth is not something the human body can do, but a tooth that was already there quietly waiting? That one can absolutely still make its move.
Can Wisdom Teeth Grow in Your 40s? Late Eruption Guide
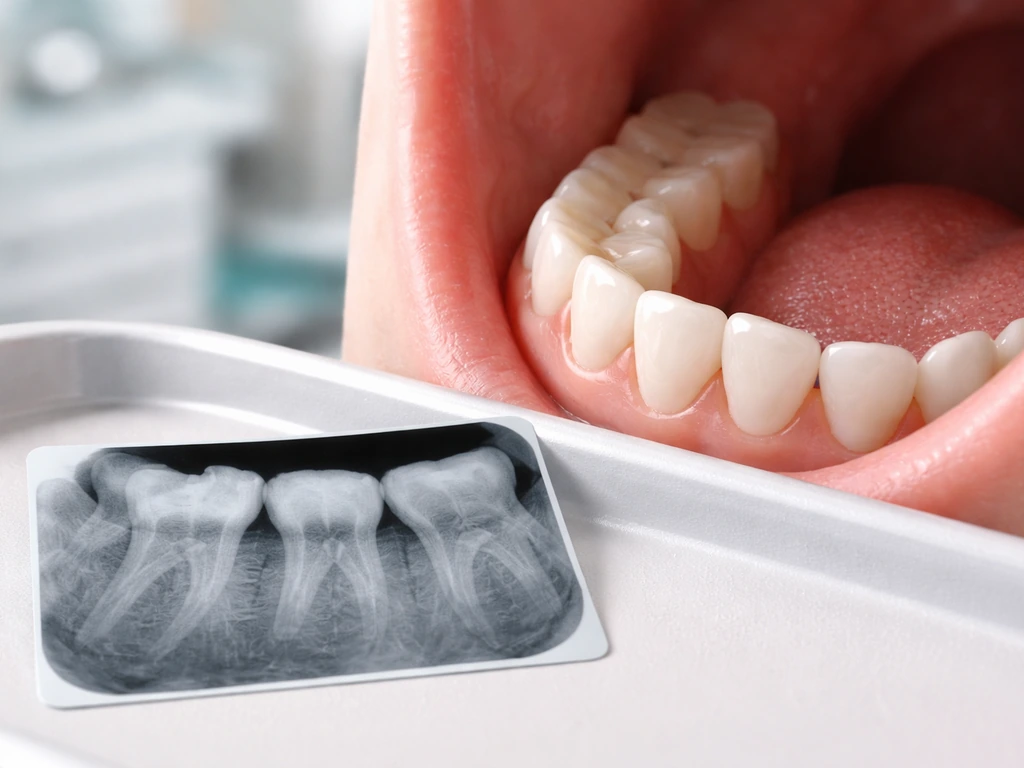
Can wisdom teeth actually erupt after 40?
The short biology lesson here: wisdom teeth, also called third molars, are the last teeth to develop. The American Association of Oral and Maxillofacial Surgeons (AAOMS) puts the typical eruption window between ages 17 and 25, and the American Dental Association puts it even tighter, between 17 and 21. But those are averages, not hard cutoffs. The AAOMS has documented in its third molar data research that there is a real and notable increase in patients over 40 requiring third molar removal, and that eruption of third molars in older patients is more frequent than was once believed.
Longitudinal studies back this up. In one 18-year follow-up, researchers tracked adults and found that third molar eruption status continued to change well past the early-20s window, with teeth that had been impacted or unerupted showing new eruption or position changes as participants moved into their 30s and beyond. Another 10-year longitudinal study found the same pattern: unerupted third molars in adults did erupt during the follow-up period, some well outside the textbook timeline. So if you're in your 40s and suddenly feeling pressure and soreness at the very back of your jaw, your body is not doing something impossible. It's doing something uncommon, but documented.
The normal timeline vs. what actually happens later
Most wisdom teeth make their move between 17 and 25. But yes, wisdom teeth can also erupt in your 20s within the typical eruption window for third molars wisdom teeth in your 20s. During this window, the jaw is still maturing, which gives third molars the best mechanical environment to push through. By the mid-20s, most dentists expect a fairly clear picture of whether your wisdom teeth will erupt, stay impacted, or need removal. For people wondering about eruption in their 30s or beyond, there's a related continuum here, whether eruption after 25 is realistic, or specifically whether it happens in the 30s, and the answer in both cases is yes, occasionally. In other words, yes, wisdom teeth can sometimes erupt after 25, even if it is less common than the typical timeline eruption after 25. If you’re asking, can you grow wisdom teeth at 30, the answer is usually no, but you can still have third molars that finally erupt that were already present. If you’re asking, can wisdom teeth grow in your 30s, the short answer is yes, it can happen occasionally. The 40s just represent a later point on that same continuum.
What the research shows is that in a 12-year observational study of adults, 22% of third molars erupted during the study period, with some erupting even after age 26. That's still a younger cohort, but it illustrates that the process doesn't always follow the textbook. AAOMS explicitly notes that retained third molars frequently and unpredictably change position, eruption status, and periodontal condition over time. That unpredictability is exactly why late eruption in midlife is possible.
Why a wisdom tooth would start erupting in your 40s
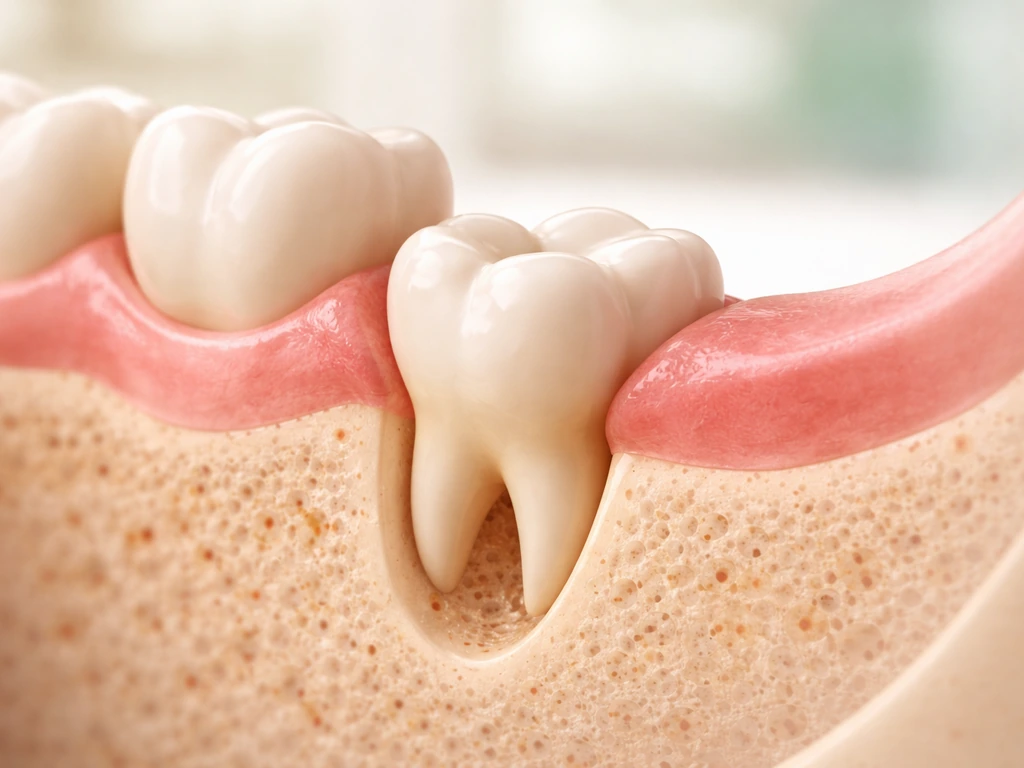
This is where anatomy, genetics, and timing all intersect. A wisdom tooth that erupts at 43 didn't just suddenly form. It was there all along, likely sitting in a partially impacted position, held back by bone density, adjacent tooth pressure, or simple lack of space. Several things can shift that equation decades later.
- Jaw space changes: If adjacent teeth have shifted, been extracted, or worn down over the years, space that previously didn't exist can open up and allow the wisdom tooth a path forward.
- Bone remodeling: The jaw bone changes gradually throughout life. Subtle remodeling can alter the position of an impacted tooth relative to the bone around it.
- Genetics: Some people are simply predisposed to late third molar eruption patterns. If your parents or siblings had wisdom teeth surface late, your own timeline may follow a similar track.
- Partial impaction becoming full eruption: A tooth that was horizontally or angularly impacted and never fully broke through the gum may slowly work its way into a more vertical position over years, eventually reaching a point where it can erupt.
- Reduced resistance from gum tissue: Gum tissue changes with age and can, in some cases, offer less mechanical resistance to a pushing tooth.
What isn't happening is spontaneous tooth formation. Humans don't regenerate teeth as adults. If you never had a wisdom tooth bud to begin with, no new one is forming at 42. An X-ray from years ago would have shown the absence of that tooth bud, and nothing has changed that biological reality. What's erupting in midlife is always a tooth that was already structurally present.
Signs that a wisdom tooth might be erupting right now
The tricky part is that late wisdom tooth eruption can feel almost identical to other dental problems that become more common in midlife, like gum disease, a cracked tooth, or a periodontal abscess. Here's what to look for specifically at the back of your mouth.
- Persistent dull aching or pressure at the very back of the upper or lower jaw, often behind your last visible molar
- Swollen, tender, or reddish gum tissue at the back of your mouth, sometimes covering a small visible piece of emerging tooth
- A flap of gum tissue (called an operculum) overlying the back of the jaw that feels raised or inflamed
- Pain that radiates toward the ear, jaw joint, or throat on one side
- Difficulty opening your mouth fully, or discomfort when chewing
- A bad taste or mild odor coming from the back of the mouth even with good brushing
- Swelling along the jaw line or in the cheek on one side
A key warning: these symptoms can genuinely mimic periodontal disease or a dental abscess. A study in StatPearls notes that pericoronal abscesses from partially erupted teeth often mimic periodontal abscesses in presentation, including increased gum pocket depth and swelling. You can't reliably tell which one you're dealing with from symptoms alone. That's exactly why getting an X-ray is non-negotiable at this stage.
Risks that come with wisdom tooth eruption at this age
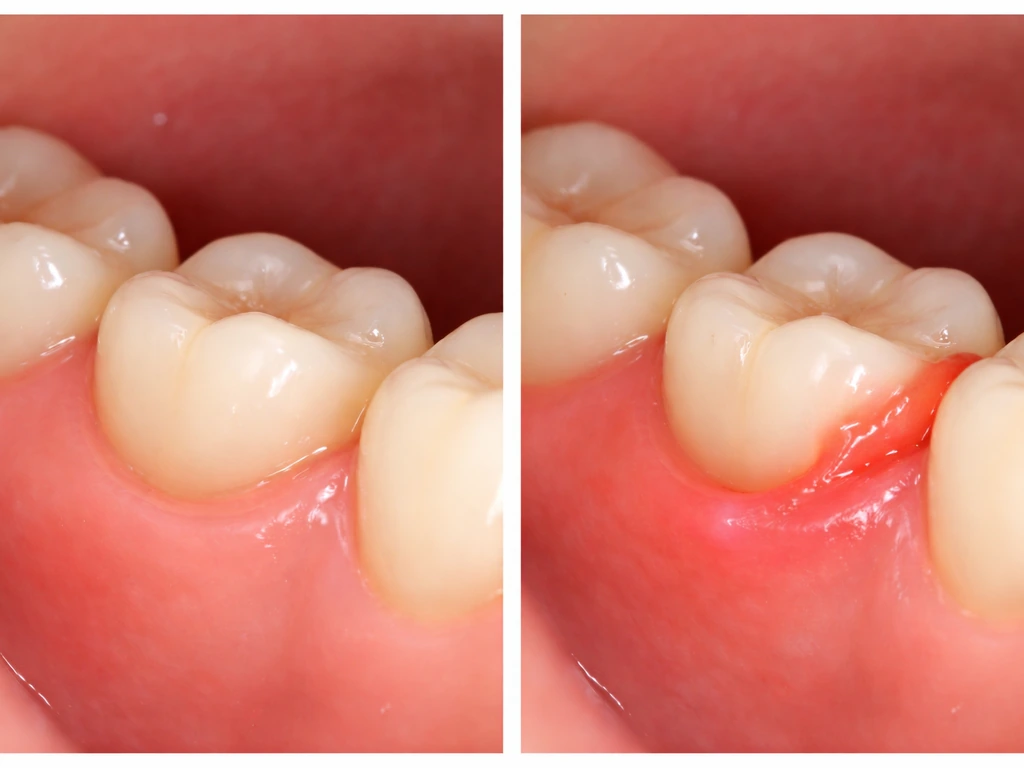
Late eruption isn't just inconvenient. The older you are when a wisdom tooth starts breaking through, the more complicated the situation tends to get. Here are the main risks worth understanding before you assume it'll just sort itself out.
Pericoronitis
This is the most common immediate problem. Pericoronitis is inflammation and sometimes infection of the gum tissue surrounding a partially erupted tooth. That flap of tissue over the tooth (the operculum) traps food and bacteria, and the result is pain, swelling, and sometimes a serious infection. StatPearls defines it clearly: it starts as localized pain and swelling at the back of the mouth and can radiate to the ear, jaw, and throat. If the infection spreads into deeper tissues, you can develop trismus (difficulty opening the mouth), difficulty swallowing, and systemic signs like fever. That's a dental emergency.
Damage to the tooth next door
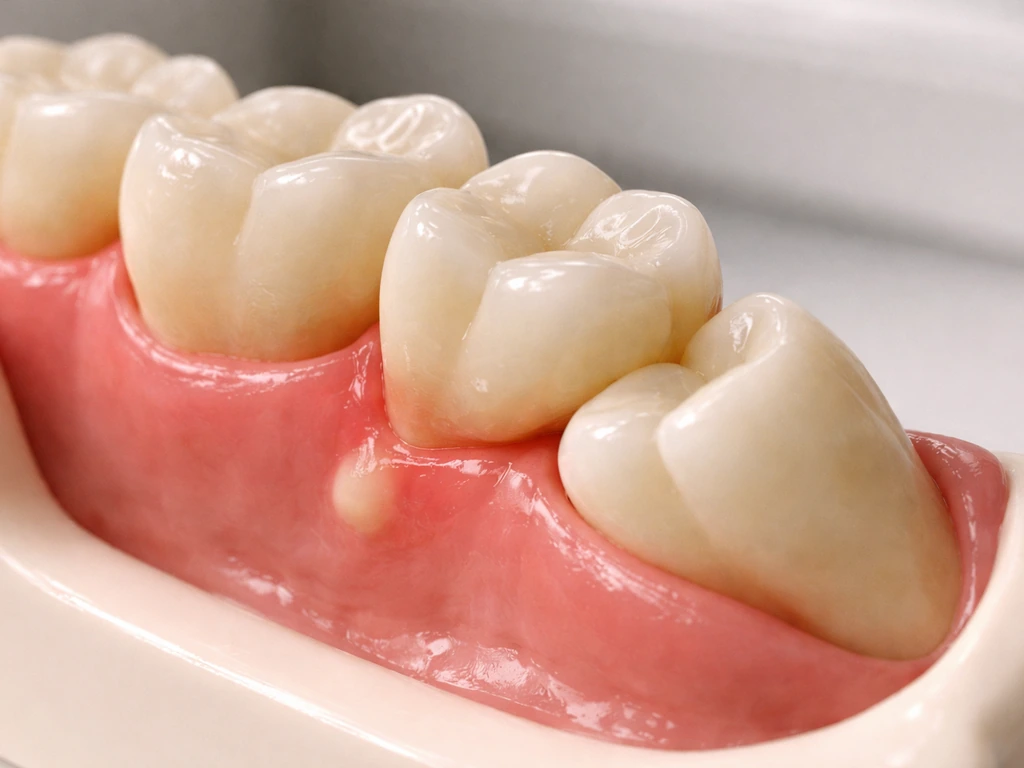
A wisdom tooth pushing through at an angle (which is common with late-erupting, long-impacted teeth) puts direct mechanical pressure on the second molar in front of it. This can cause root resorption on that second molar, meaning it gradually destroys the root of an otherwise healthy tooth. The 2024 expert consensus on third molar management specifically flags increased risk of periodontitis and decay on adjacent teeth as a documented complication of erupting or impacted third molars.
Crowding and bite changes
If you had orthodontic work years ago or your teeth have settled into a stable alignment, a newly erupting wisdom tooth can push things out of position. This is more of a long-term concern than an acute one, but it's worth factoring into the decision about whether to monitor or intervene.
Cysts and (rarely) tumors
Impacted wisdom teeth that have been sitting unerupted for decades can develop a dentigerous cyst around the crown. These cysts can quietly expand and destroy surrounding bone before causing symptoms. Rarely, these develop into more serious pathology. This is one reason why retained impacted wisdom teeth in older adults deserve periodic monitoring even if they've been symptom-free for years.
Higher surgical risk if removal becomes necessary
This one matters a lot. A 10-year comparative study on third molar removal in aging populations found explicitly that morbidity increases after age 40, with a significant portion of older patients requiring removal being over 60. A separate case series titled 'Hazards of retained third molars in older persons' documented 15 cases in people over 40 and described both the complications of retaining those teeth and the increased surgical difficulty when extraction was eventually needed. Bone is denser, healing is slower, and the roots of long-impacted teeth can be closely positioned near nerves. Removing a wisdom tooth at 45 is simply a harder procedure than removing it at 22.
When to see a dentist and what to expect
If you're feeling any of the symptoms described above, book an appointment soon rather than watching and waiting on your own. There's no good reason to delay. If you're having swelling that's spreading, difficulty swallowing, fever, or inability to open your mouth normally, treat that as urgent and get seen the same day.
At your appointment, the dentist will do a clinical exam to assess the gum tissue at the back of your mouth, check for any visible tooth structure, and probe for pocketing or infection. The essential next step is imaging. Standard periapical or panoramic X-rays give a two-dimensional view of the tooth's position and root structure. For a more complex impaction, especially one near the inferior alveolar nerve, AAOMS has published guidance supporting the use of cone beam computed tomography (CBCT) imaging, which gives a three-dimensional map of exactly where the tooth sits relative to nerves, adjacent roots, and bone. This matters enormously for surgical planning.
From that exam and imaging, the dentist or oral surgeon will typically lay out a decision pathway that falls into one of three directions.
| Path | When it applies | What it involves |
|---|---|---|
| Monitoring | Tooth is erupting without symptoms or significant pathology; patient is a higher surgical risk | Regular X-rays to watch for cyst formation, position changes, or emerging problems |
| Local management | Pericoronitis present but mild and localized; tooth has potential to erupt favorably | Irrigation and debridement of the pericoronal space, possible operculum removal, antibiotics only if infection is spreading or systemic signs are present |
| Extraction or coronectomy | Significant impaction, unfavorable angulation, recurrent infection, adjacent tooth damage, or cyst development | Surgical extraction; coronectomy (crown removal, roots left in place) considered when roots are dangerously close to the inferior alveolar nerve |
Can anything actually regrow or regenerate a wisdom tooth?
This is the myth worth busting directly: no. Adult humans do not regenerate teeth. Once a tooth or tooth bud is gone, it's gone. What's described throughout this article is the eruption of a tooth that was already biologically present but hadn't yet broken through the gum. That's fundamentally different from regrowth. If you had a wisdom tooth extracted years ago, that socket is not going to produce a new one. If you were born without wisdom tooth buds (a condition called third molar agenesis, which affects a significant portion of the population), no amount of time or intervention will cause new ones to form.
Dental research into stem cell-based tooth regeneration is ongoing, but it remains experimental and is not a clinical reality for patients today. The only scenario where a wisdom tooth 'appears' in your 40s is the one this article covers: a long-present, previously dormant or impacted tooth finally reaching the surface. That's biology being slow and unpredictable, not biology being regenerative.
Practical next steps if you think this is happening to you
- Book a dental appointment now, especially if you're having pain, swelling, or pressure at the back of your jaw. Don't wait to see if it resolves on its own for more than a few days.
- Be specific about your symptoms when you call: mention the location (back of upper or lower jaw), how long it's been happening, and any radiating pain or swelling.
- Ask for imaging at the appointment. If your dentist only does a visual exam, ask whether an X-ray or panoramic film is warranted given your symptoms and age.
- If you're referred to an oral and maxillofacial surgeon, that's routine for complex third molar cases, not a sign that something is catastrophically wrong.
- Keep the area as clean as possible in the meantime: gentle rinsing with warm salt water can help reduce inflammation around an operculum and dislodge debris.
- Avoid taking antibiotics you happen to have on hand without a current prescription. Pericoronitis management guidelines are clear that antibiotics are warranted when infection is spreading systemically, not as a first line for mild local inflammation.
- Ask about your options explicitly: monitoring, local management, extraction, and where applicable, coronectomy. Get a clear picture of the pros and cons given your tooth's position before agreeing to any procedure.
The bottom line is that wisdom teeth in your 40s are surprising but not impossible. The biology behind it is straightforward once you understand that these teeth have been there all along. What matters most now is getting an accurate picture of what's happening in your jaw and making a decision based on real imaging and a clinician who knows third molar management. The risks of late eruption are real, and so is the increased complexity of any surgical intervention at this stage. Acting sooner rather than later almost always leads to better outcomes.
FAQ
How can I tell if my back-of-jaw pain is a late wisdom tooth problem versus gum disease or an abscess?
Usually, you cannot tell by symptoms alone. Late third molar issues can mimic periodontal disease, a cracked tooth, or a periodontal abscess, and both pericoronal and periodontal infections can cause swelling and pocket-like inflammation. An exam plus imaging is the deciding step, not how it feels day to day.
If my wisdom tooth might be erupting, how quickly do I need to be seen?
Because many wisdom teeth in the 30s to 40s are partially impacted, their gum flap can trap bacteria and food, so it often worsens without improving. If you have swelling, fever, pus, trouble swallowing, or you cannot open your mouth normally, you should be seen the same day rather than waiting for a routine appointment.
Can a dentist confirm that a tooth truly “grew” versus already being present but hidden?
No. Wisdom teeth do not regenerate in adults. A “new” tooth in your 40s implies the tooth existed earlier, but was blocked (partially impacted), positioned deeper in the bone, or still undetected. If you truly lacked third molar buds (third molar agenesis), time will not create them.
What symptoms are warning signs that late wisdom tooth eruption might be more than local gum inflammation?
If you cannot open your mouth normally (trismus), have fever, feel ill, or have swelling spreading toward the jaw or neck, treat it as urgent. Those can be signs that inflammation or infection is moving beyond the gum flap around a partially erupted tooth.
Can a late-erupting wisdom tooth damage the second molar in front of it?
If a wisdom tooth is erupting at an angle, it can mechanically irritate the second molar and contribute to root or gum problems over time. Ask your clinician to check the second molar for periodontal probing depth changes and signs of damage, because late eruption problems are not limited to the wisdom tooth itself.
When do dentists recommend monitoring a late wisdom tooth eruption instead of removing it?
Often, monitoring is considered only after baseline imaging and a clear risk assessment. If your tooth is fully or mostly impacted, symptom-free, and not threatening adjacent roots or nerves, a clinician may choose observation. If there is recurrent pericoronitis, progressive bone loss, significant pocketing, or proximity to key structures, the plan tends to shift toward extraction.
What should I do at home while I’m waiting to be seen for possible late wisdom tooth eruption?
Start with gentle oral hygiene and avoid digging at the gum flap, which can worsen irritation. Rinse with warm salt water can help with comfort, but it is not a substitute for diagnosis. If you already have swelling, drainage, or worsening pain, you still need an exam and imaging before relying on home care.
Do I always need CBCT, or are regular X-rays usually enough for a wisdom tooth in the 40s?
Cone beam CT is typically used when the imaging needs more detail for surgical planning, such as when the tooth is close to the inferior alveolar nerve or the impaction pattern is complex. If your panoramic or periapical X-rays suggest nerve proximity, curved roots, or complicated angles, ask whether CBCT is warranted for your case.
If I get antibiotics, does that mean the wisdom tooth issue is solved, or might I still need extraction?
Antibiotics are not a cure for the underlying cause if the gum flap is trapping bacteria or if the tooth is driving recurring inflammation. In many cases, antibiotics may be used to control infection temporarily, but definitive management depends on the tooth’s position, symptoms, and imaging findings.
If the pain improved for a few days, should I still follow up for late wisdom tooth evaluation?
Pain can peak and fluctuate, but “getting better” does not reliably mean the eruption risk has passed. The gum flap may repeatedly inflame as the tooth continues to push through, so if symptoms recur over weeks or keep returning, it is a strong reason to get re-evaluated rather than assuming it resolved.
Can wisdom teeth erupt in your 20s? Learn signs, diagnosis with X-rays, and when extraction is needed.
Can wisdom teeth erupt in your 30s? Learn symptoms, timing, how dentists confirm, and when extraction is needed.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

