Yes, wisdom teeth can absolutely erupt in your 30s. It's not common, but it's not rare either, and if you're suddenly feeling pressure, swelling, or pain in the back of your jaw, there's a real chance a third molar is finally making its move. The standard eruption window is ages 17 to 25, but that range has always had a wide tail. Some people's third molars simply take longer to push through, and a subset of adults don't notice symptoms until their late 20s or 30s when a previously dormant tooth starts shifting position or becomes impacted against neighboring structures.
Can Wisdom Teeth Grow in Your 30s? Symptoms, Timing, Options
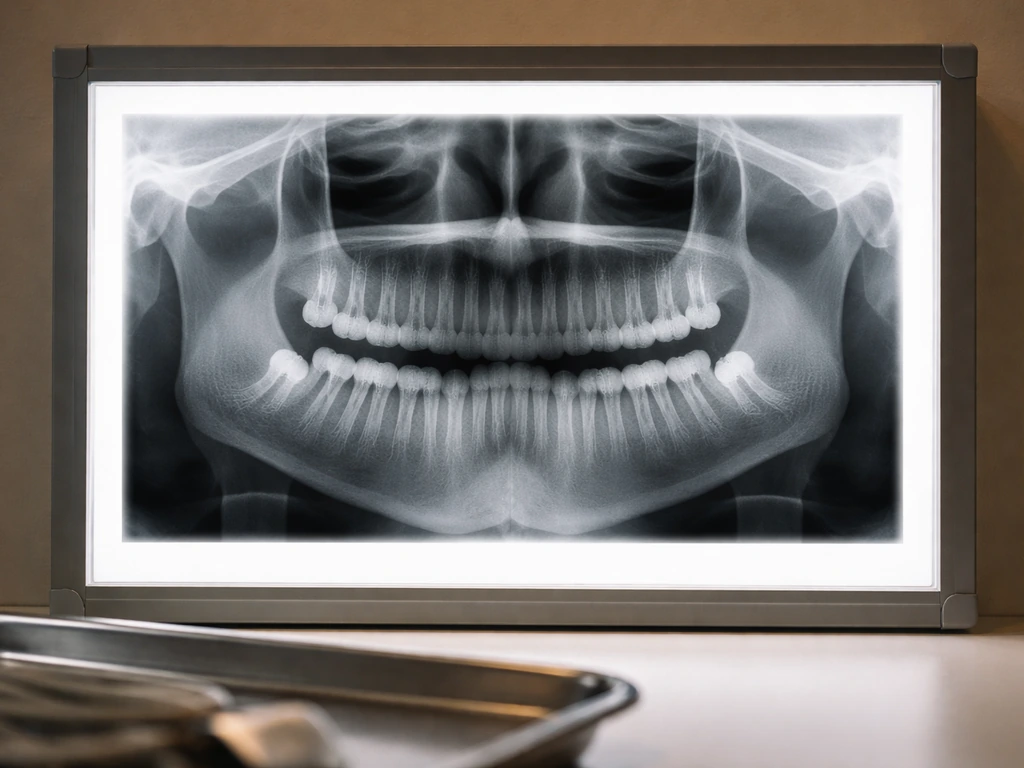
The typical wisdom tooth timeline (and why some people run late)

Wisdom teeth are the last teeth to develop and erupt, generally appearing somewhere between ages 17 and 25. That window exists because third molar root development starts in the early teens and finishes later than every other tooth in the mouth. But "typical" doesn't mean universal. Jaw anatomy, the angle at which the tooth is sitting, and how much space exists all influence whether and when a wisdom tooth breaks through the gum.
A 10-year longitudinal study of adults found that unerupted third molars at baseline could remain unerupted or become clinically apparent later, meaning eruption or position change is something that can actually be observed during adulthood, not just in teenagers. Research also shows that partially impacted third molars are still being newly diagnosed well into the 30s, though the incidence of late partial eruptions does decline as age increases after 30. In other words: the older you are, the less likely a stuck wisdom tooth will spontaneously complete its journey, but it can still happen.
Genetics play a big role here. Some families simply have more crowded jaws or third molars that sit at unusual angles. If one of your parents had a wisdom tooth extracted in their 30s, that's relevant history worth mentioning to your dentist.
What "growing in your 30s" actually means
This is where I want to clear something up, because this site gets a lot of questions about whether teeth can regrow or regenerate. When people ask "can wisdom teeth grow in your 30s," they're usually asking one of two different things, and the answers are very different.
The first meaning is eruption: a wisdom tooth that already exists in your jawbone, formed years ago, finally pushes through the gum tissue. That is absolutely possible in your 30s. The tooth has been there the whole time, buried under bone and gum, and it's only now becoming visible or symptomatic. This is not regrowth. It's an existing tooth completing a delayed journey.
The second meaning is regeneration: a brand-new tooth growing where one never existed or was lost. That does not happen in adult humans. Once a tooth is removed or never developed in the first place, your body cannot grow a replacement. Lost enamel, lost dentin, and missing teeth do not regenerate naturally. So if someone tells you their "wisdom tooth grew back" after extraction, what's more likely is that they had a second unerupted tooth nearby that then became visible, or the original tooth was not fully removed. Just as wisdom teeth erupting after age 25 involves a tooth that already existed rather than a new one forming, any "late" eruption in your 30s follows the same biological logic.
Signs that a wisdom tooth might be erupting or causing trouble
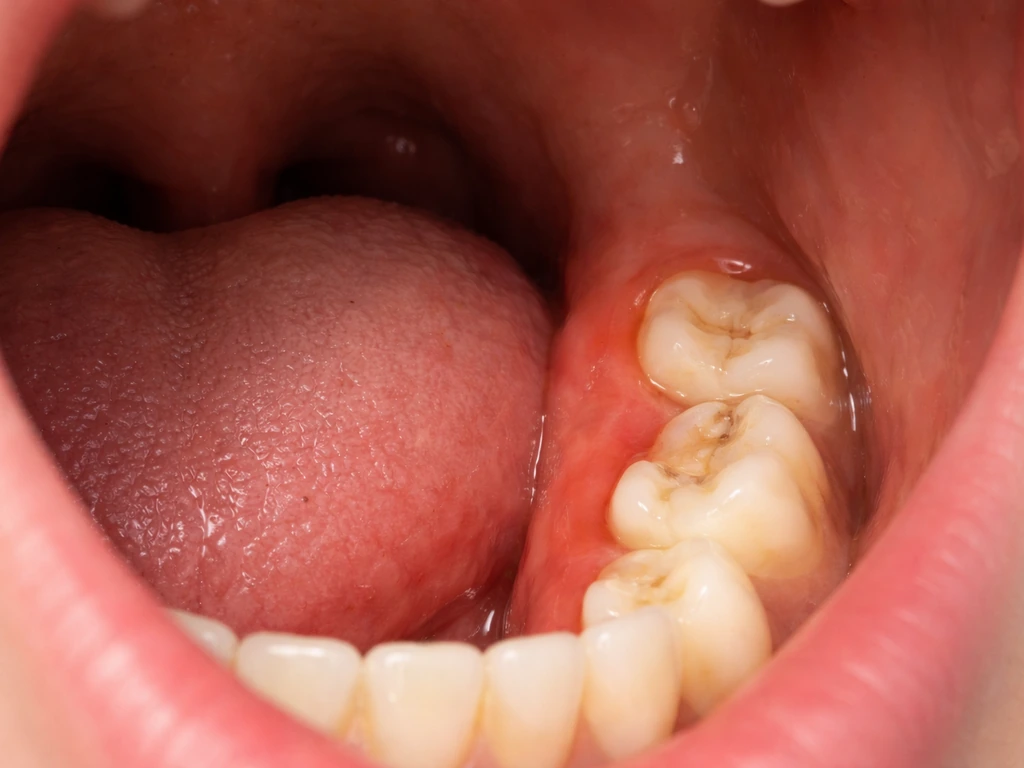
The symptoms of a late-erupting or impacted wisdom tooth in your 30s can range from subtle to seriously uncomfortable. Because bone density increases with age, eruption at this stage tends to be slower and more resistant, which means symptoms often drag on longer than they would in a teenager.
- Dull, persistent aching at the back of the jaw, often on one or both sides
- Swollen, red, or tender gum tissue directly behind your last visible molar
- A feeling of pressure or fullness deep in the jaw
- Pain that radiates up toward the ear or down along the jawline
- Difficulty opening your mouth fully (trismus), especially in the morning
- Bad taste or bad breath from the area even after brushing
- Visible gum tissue partially covering a tooth that is trying to push through (called pericoronitis when it gets infected)
Pericoronitis is especially common in partially erupted wisdom teeth. The gum flap (operculum) that sits over the tooth traps food and bacteria underneath it, causing localized infection. It's uncomfortable, it can spread if untreated, and it's one of the most common reasons adults in their 30s end up needing wisdom tooth extraction they didn't expect.
Not all wisdom tooth symptoms are dramatic, though. Some people notice nothing at all until a dentist spots an issue on X-ray. That's why routine imaging matters even when you feel fine.
How your dentist figures out what's going on
If you come in with back-of-jaw pain, your dentist will start with a clinical exam: probing the gum tissue, checking for swelling or infection, and looking for any visible sign of eruption or operculum. But the real picture comes from imaging.
A panoramic X-ray (OPG) is the most common first step. It gives a full view of both jaws and shows the position, angle, and root development of all four wisdom teeth at once. From this, your dentist can tell whether a tooth is impacted, which direction it's angled, how close the roots are to the inferior alveolar nerve, and whether it has any realistic path to eruption.
For more complex cases, particularly when the tooth is deeply impacted or the roots are in a tricky position relative to the nerve, a cone-beam CT (CBCT) scan gives a 3D view that a flat X-ray simply can't provide. CBCT is increasingly common before surgical extractions in adults because the extra detail reduces risk. Radiologic studies confirm that impaction patterns continue to be diagnosed into the 30s, and the specific class of impaction (angle, depth, relationship to adjacent teeth) shifts with age, which is exactly why a current image matters more than any taken years ago.
What happens next: watch it or remove it
Not every wisdom tooth in your 30s needs to come out immediately. Treatment decisions depend on whether the tooth is causing symptoms, whether it's fully or partially impacted, and whether it creates a hygiene or structural risk to the adjacent second molar.
| Situation | Likely recommendation | Reasoning |
|---|---|---|
| Fully impacted, no symptoms, no pathology on X-ray | Monitor with periodic imaging | Low immediate risk; extraction carries more risk than benefit if the tooth is stable and buried |
| Partially erupted with recurring pericoronitis or infection | Extraction | Repeated infections signal the tooth won't fully clear; risk of spread increases over time |
| Impacted and pressing against the second molar | Extraction | Continued pressure causes root resorption and damage to an otherwise healthy tooth |
| Erupting with enough space and correct angle | Monitor; may fully erupt | If the path is clear and the patient is asymptomatic, watchful waiting is reasonable |
| Partially erupted causing gum disease or cavities | Extraction | Cleaning access is compromised; ongoing decay risk to adjacent teeth |
The "watchful waiting" approach works better when the tooth is truly buried and stable, not when it's partially through the gum. A partially erupted tooth that sits open to bacteria but can't fully emerge is the worst of both worlds. If you're in your 30s and a dentist is telling you to monitor a partially erupted wisdom tooth, it's worth asking specifically why extraction isn't being recommended, because the professional consensus leans toward intervention when partial eruption is causing recurring problems.
If you've wondered whether growing a wisdom tooth at 30 changes which option your dentist will lean toward, the answer is yes, slightly. Older bone is denser, so a tooth that might have erupted on its own at 19 is less likely to complete that journey at 32. That shifts the math toward earlier extraction rather than waiting.
Risks, complications, and what recovery looks like in your 30s
Here's the honest truth about wisdom tooth extraction in your 30s versus your late teens: it's generally more involved. Denser bone means the tooth may require more force or sectioning to remove. Root development is typically complete by this age, which can make roots longer and more curved. Healing also tends to be a bit slower than it is for a 19-year-old, though most healthy adults in their 30s recover well within a week to ten days for routine extractions.
- Dry socket (alveolar osteitis): the most common post-extraction complication, where the blood clot dislodges before healing is complete; it's painful and requires a follow-up appointment for treatment
- Nerve proximity: the inferior alveolar nerve sits close to mandibular (lower) wisdom tooth roots; pre-surgical CBCT is particularly important for adults with fully developed roots
- Infection risk: pericoronitis before extraction increases the chance of post-operative infection; dentists often prescribe antibiotics before surgery if active infection is present
- Prolonged swelling: facial swelling after wisdom tooth surgery in adults can last three to five days; plan for it
- Sinus involvement: upper wisdom teeth occasionally sit close to the maxillary sinus; this is usually visible on imaging and affects surgical planning
The experience in your 30s is meaningfully different from what someone in their early 20s goes through, which is part of why many oral surgeons historically recommended removing wisdom teeth prophylactically in the late teens. That blanket approach is no longer universally endorsed, but the underlying logic, that age makes extraction harder, still holds. If you're curious how the 30s timeline compares to what happens even later, the considerations around wisdom teeth erupting in your 40s take those complications further in the same direction.
Recovery at this age usually involves three to five days of soft foods, ice packs for the first 24 to 48 hours, and prescription or over-the-counter pain management. Smoking significantly increases dry socket risk. Avoiding straws, spitting, and any sucking motion in the first 48 hours is essential for clot preservation.
When to stop waiting and get care now
Some symptoms are uncomfortable but manageable until your next scheduled appointment. Others need same-day or next-day attention. Don't wait if you notice any of the following:
- Swelling that is spreading toward your throat, floor of your mouth, or eye area
- Difficulty swallowing or breathing, even mild
- Fever above 101°F alongside jaw or gum pain
- Inability to open your mouth more than a finger-width or two
- Pus or discharge visible near the back gum tissue
- Pain that's not responding to over-the-counter ibuprofen or acetaminophen after 24 to 48 hours
Spreading infection from a wisdom tooth can become a medical emergency, not just a dental one. Ludwig's angina, a rapidly spreading floor-of-mouth infection, is rare but life-threatening and often starts from a dental source. If swelling is tracking downward toward your neck or upward around your eye, go to an emergency room, not just an urgent dental clinic.
While you're waiting for your appointment or for the discomfort to subside enough to be seen, warm salt water rinses (half a teaspoon of salt in eight ounces of warm water, rinsed gently several times a day) can reduce bacteria under the gum flap. Ibuprofen works better than acetaminophen for dental inflammation because it targets the inflammatory process directly. Avoid poking at the area, and don't try to "clear" a gum flap yourself.
The bigger picture: eruption vs. regrowth, and why it matters
The reason this question matters so much on a site focused on dental regeneration is that people often confuse two things that are biologically completely different. A wisdom tooth that erupts in your 30s is not a tooth regrowing. It's a tooth that has been sitting in your jaw since adolescence finally completing (or failing to complete) its eruption path. That's a development event, not a regeneration event.
True tooth regeneration, where lost enamel, dentin, or a missing tooth grows back naturally, does not happen in humans. Enamel cannot be rebuilt by the body once it's gone. A tooth that was extracted does not regrow. This is fundamentally different from a buried third molar finally erupting. Understanding how wisdom teeth behave in your 20s makes this clearer: the biology is consistent across the late eruption range, whether that's at 22 or 34.
So yes, if you're in your 30s and feeling something happening at the back of your jaw, it can genuinely be a wisdom tooth making a late appearance. Get imaging done, understand where the tooth sits and what it's doing, and work with your dentist or oral surgeon to decide whether monitoring or extraction is the right call for your specific situation. The one thing that won't happen is your body spontaneously growing a new tooth where one never existed. What can happen, and does happen, is a third molar you've had your whole life finally becoming a problem worth addressing.
FAQ
If a wisdom tooth “grew in” after I already had one removed, is that possible?
Not typically. In your 30s, what usually happens is that an existing but buried third molar finally becomes visible or changes position, causing pain or swelling. If someone says their tooth “grew back” after extraction, the more likely explanation is either an unerupted second molar or another tooth that was not fully recognized/removed the first time, or retained tooth structure that later became symptomatic.
Can a partially erupted wisdom tooth cause symptoms on and off in your 30s?
Yes, even if the gum flap looks small. A partially erupted wisdom tooth can trap bacteria and cause recurring pericoronitis, so symptoms may flare and settle repeatedly. If you keep getting the same back-of-jaw discomfort, bad taste, or intermittent swelling, ask whether the tooth is partially erupted and prone to operculum infections, because that pattern often favors definitive treatment rather than waiting.
Will orthodontic treatment or braces make late wisdom tooth symptoms more likely?
Braces or orthodontic work can change the timing and symptoms. If your dentist moves other teeth, they may also increase pressure or alter space conditions near the back of the arch, making a previously quiet third molar more likely to become symptomatic. Tell your orthodontist and oral surgeon that you have late-appearing wisdom tooth symptoms so they can coordinate imaging and timing.
Do I need a dentist visit even if my wisdom tooth pain is mild?
Not always, and delayed diagnosis is common. Some people have minimal pain until the first flare of pericoronitis, or the issue is only seen on an X-ray. If you have persistent or recurrent discomfort in the back of your jaw, schedule an exam rather than relying on whether symptoms feel “severe.”
When would a cone-beam CT be necessary instead of a simple panoramic X-ray?
A panoramic X-ray can miss details when the roots are close to the nerve or when the tooth is angled deeply. If your dentist sees complex angulation, unusual root proximity, or plans surgery, a cone-beam CT (CBCT) is often used to reduce uncertainty about nerve risk and to map how to remove the tooth in sections if needed.
How do I know my back-of-jaw pain is truly from a wisdom tooth, not something else?
It depends on the reason you’re hurting. Pain from a wisdom tooth can mimic sinus issues, TMJ problems, or a cavity in the adjacent second molar. Ask for a full exam that includes checking the neighboring molar and assessing gum inflammation, then review X-ray findings together so you know which structure is driving the symptoms.
If I’m told to monitor it, what criteria should make extraction more likely later?
If the dentist recommends monitoring, it should be based on stability, lack of repeated infection, and low risk to the second molar (for example, no gum pocketing or damage). If you have recurring pericoronitis or signs that the tooth is harming the adjacent tooth, “watchful waiting” becomes less appropriate. Ask what specific risk factors they are watching and how often they want follow-up imaging.
What symptoms mean I should seek urgent care rather than waiting for my dental appointment?
You should contact urgent care or emergency services if swelling is spreading beyond the jaw, you have trouble swallowing, breathing difficulty, fever, or swelling that tracks toward the neck. Those red flags can indicate a rapidly spreading infection, which is not something to manage at home until a routine dental appointment.
If antibiotics help my wisdom tooth infection, does that mean I can avoid extraction?
Antibiotics do not fix the underlying mechanical problem of a partially erupted gum flap. They may calm an acute infection, but if the operculum keeps trapping bacteria, pericoronitis often returns. Ask whether you’re treating an active infection short-term, or whether the longer-term plan is extraction once the swelling settles.
What’s safe to do at home while I wait for a wisdom tooth appointment in my 30s?
You can usually manage mild discomfort at home, but avoid “digging” at the gum flap or using aggressive rinses that irritate tissue. Warm salt water rinses and anti-inflammatories are commonly used for comfort, and you should still follow up promptly because symptoms can worsen quickly if the tooth is partially erupted and repeatedly infected.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn
Learn which teeth seem to grow twice: primary replaced by permanent, plus wisdom teeth timing and limits on regrowth
Milk teeth eruption timeline by age: first tooth, full primary set, what’s normal, and when to see a pediatric dentist.

