Yes, wisdom teeth can and usually do grow on both sides. Most people have four wisdom teeth total, one in each corner of the mouth, and studies show that when impaction occurs, it's bilateral (both sides) in roughly 74 to 83 percent of cases. That said, it's genuinely possible for wisdom teeth to develop on only one side, or to appear that way because one side is erupting faster, more visibly, or with more symptoms than the other. So if you're feeling pressure or pain on just one side right now, that doesn't automatically mean the other side is fine or missing. It just means one side got your attention first.
Do Wisdom Teeth Grow on Both Sides? One-Side Eruption Explained
The normal eruption pattern: both sides, but not always in sync
Wisdom teeth are your third molars, and there are typically four of them: upper left, upper right, lower left, and lower right. According to the Merck Manual, they normally erupt between ages 17 and 25, though eruption timing can vary by about six months in either direction and still fall within normal range. Because each tooth follows its own developmental timeline, it's completely normal for them to erupt at different rates. Because each wisdom tooth follows its own developmental timeline, they do not always grow at the same time do wisdom teeth grow at the same time. You might feel your lower right wisdom tooth pushing through at 19 while the upper left doesn't cause a peep until you're 23.
The bilateral pattern is the norm. Research on mandibular (lower jaw) wisdom teeth shows that bilateral impaction accounts for 73 to 83 percent of cases. Unilateral (one-sided) impaction happens, but it's the minority. And when it is one-sided, studies suggest the right side is slightly more often affected than the left. The takeaway: symmetric development is expected, but asymmetric symptoms are common and don't mean something is wrong by default.
Why wisdom teeth sometimes seem to grow on only one side
This is one of the most common sources of confusion, and there are several real reasons behind it.
- Timing differences: One tooth simply erupts earlier. The other side may be developing perfectly normally but hasn't broken through the gum yet. You're not seeing the full picture without an X-ray.
- Impaction on one side: A tooth blocked by bone, soft tissue, or an adjacent molar can get stuck while the other side erupts freely. The most common angulation patterns seen on X-rays are vertical (53%), mesioangular (22%), horizontal (20%), and distoangular (4%), and each affects how the tooth moves (or doesn't).
- Partial eruption: One tooth may be only partially through the gum, creating a flap of tissue called an operculum. This is one of the most symptom-heavy stages and can make it feel like that side is the only side doing anything.
- Congenitally missing teeth: Some people simply don't develop all four wisdom teeth. Dental agenesis (a missing tooth bud entirely) is not rare, and without a panoramic X-ray, you'd never know.
- Different upper vs. lower timelines: Upper and lower wisdom teeth don't always erupt at the same time. Your lower jaw teeth often cause more noticeable symptoms because of their angle and the density of the surrounding bone.
- Asymmetric space: If there's more room on one side of your jaw, that tooth may erupt without much drama while the other side stays impacted due to crowding.
Upper vs. lower, left vs. right: which side to actually check
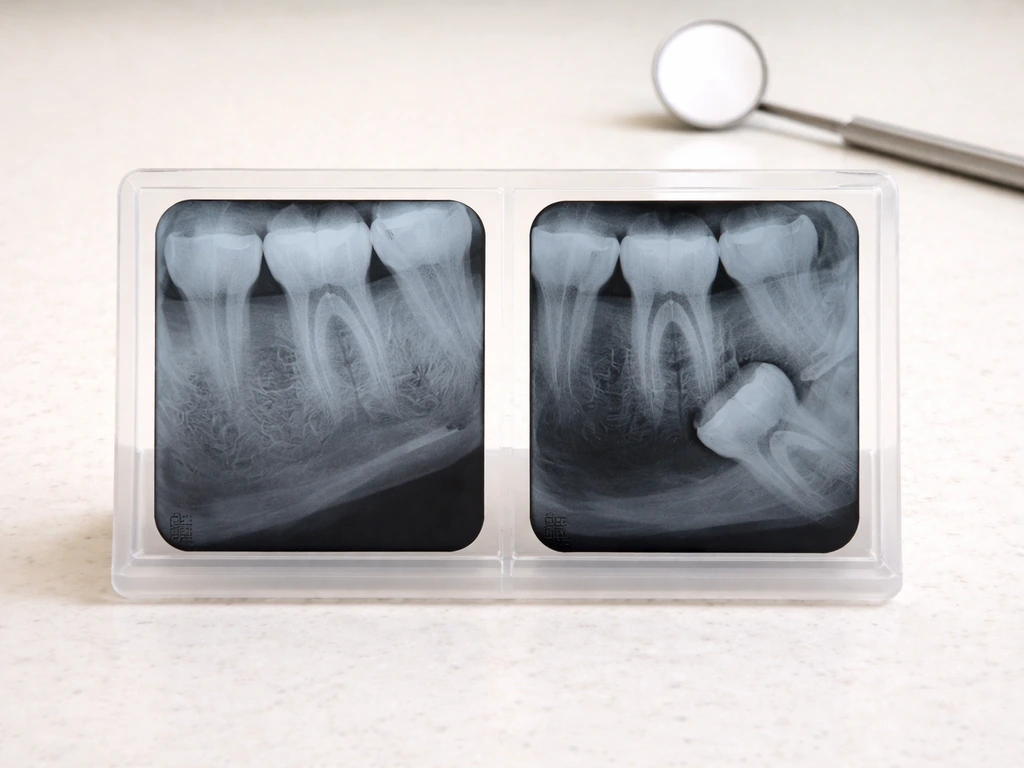
When people ask about "one side," they usually mean left versus right, but the upper versus lower distinction matters just as much. Lower wisdom teeth are generally more problematic because the mandible is denser, the available eruption space tends to be tighter, and the angle of the tooth is more likely to cause it to lean into the second molar. Lower wisdom teeth are also more closely associated with pericoronitis (the gum infection that happens around a partially erupted tooth) and more likely to be the ones flagged on an X-ray for potential removal.
Upper wisdom teeth often erupt more quietly. They tend to have a more forgiving angulation and slightly more space, so they can come through without causing the kind of dramatic jaw pain or swelling that makes you call a dentist. This asymmetry in symptom intensity can make it seem like you only have wisdom teeth on the bottom, or only on one side. If you're not sure which teeth you actually have, a panoramic X-ray will map all four corners at once and immediately answer the question.
For a left-versus-right check, don't rely on symptoms alone. Impacted teeth can sit silently in the jaw for years before causing trouble. Serial panoramic X-rays are actually studied specifically for their ability to predict whether a lower wisdom tooth will erupt on its own or stay impacted, which tells you that clinical observation alone isn't enough to know what's happening on the quieter side.
Signs a wisdom tooth is actually coming in
There's a difference between normal back-of-mouth changes and a tooth genuinely erupting. This is why people often wonder whether wisdom teeth grow out of the gum on their own versus staying impacted genuinely erupting. Here's what to look for.
- Gum swelling or tenderness at the very back of the jaw, behind the last visible molar
- A dull, pressure-like ache that comes and goes, sometimes radiating toward the ear or jaw joint
- A visible white edge or cusp tip breaking through the gum surface
- A gum flap (operculum) covering part of a tooth, which can trap food and cause a bad taste or bad breath
- Difficulty fully opening your mouth (trismus), which is a more serious sign and warrants a prompt dentist visit
- Pain that worsens when biting down on that side
- In more serious cases: facial swelling, pus, or fever (fever is unusual with routine dental issues and suggests infection has spread)
Pericoronitis is the specific condition to know about here. It happens when plaque and food collect under the operculum around a partially erupted wisdom tooth. Symptoms range from mild soreness and a bad taste all the way to swelling, fever, and trouble opening your jaw. If the tooth fully erupts into a position where you can clean it properly, pericoronitis often resolves on its own as the gum flap recedes. If the tooth is horizontally impacted or there simply isn't enough space, that infected pocket can't be properly cleaned and the problem tends to recur. That's when extraction becomes the practical answer.
What to do today: self-checks and when to get an X-ray

Start with a simple self-check. With clean hands and good lighting (a flashlight helps), open your mouth as wide as you comfortably can and look at the very back of each side of your upper and lower jaw. You're looking for any gum swelling, redness, a visible tooth edge, or a tissue flap. Run your tongue along that area too; you can often feel a hard edge under the gum before you can see anything. Do this for all four corners, not just the one that's bothering you.
If you see swelling, feel significant pain, notice a bad taste or smell, or have any difficulty opening your jaw, contact a dentist today. Don't wait. If you have fever, facial swelling that's spreading, trouble swallowing, drooling, or any change in your voice alongside jaw symptoms, those are red-flag signs that need urgent or emergency assessment. These can indicate infection spreading beyond the tooth, and that's not a situation to manage at home.
If symptoms are mild or you're simply curious about what's happening on both sides, book a routine dental appointment and ask specifically for a panoramic X-ray (OPG). A panoramic radiograph is the standard first-line imaging for wisdom tooth evaluation. It shows all four wisdom teeth at once, their angulation, their relationship to adjacent teeth and nerves (particularly the inferior alveolar nerve in the lower jaw), and whether any are impacted. The American Association of Oral and Maxillofacial Surgeons (AAOMS) recognizes the panoramic radiograph as the most commonly accepted imaging for third molar management. In situations where a lower wisdom tooth appears close to the inferior alveolar nerve canal, your dentist or oral surgeon may also recommend a CBCT (3D scan) to better assess the risk before any procedure.
Treatment and planning when one or both sides are affected
Once you have a clear picture from imaging, your dentist or oral surgeon can give you real options rather than guesswork. Here's how decisions generally get made.
| Situation | Typical approach |
|---|---|
| Fully erupted, healthy, cleanable wisdom tooth | Monitor; no action needed unless problems develop |
| Partially erupted with mild pericoronitis (first episode) | Irrigation, oral hygiene instruction, possibly antibiotics; monitor for full eruption |
| Recurrent pericoronitis or horizontal/deep impaction | Extraction is usually recommended |
| Asymptomatic impaction, no adjacent damage | Monitor with periodic X-rays; NICE guidelines advise against prophylactic removal if symptom-free |
| Impaction causing root resorption of second molar, cyst, or abscess | Extraction indicated |
| Only one side impacted, other erupted normally | Manage each tooth on its own merits; bilateral symptoms don't require bilateral extraction |
For lower wisdom teeth near the inferior alveolar nerve, the risk of temporary nerve injury (numbness or tingling) after extraction is generally in the range of 0.4 to 8.4 percent, and permanent injury is rare, estimated at under 1 to 3.6 percent in most reviews, with higher risk in specific high-risk anatomical situations. Your oral surgeon will discuss this during consultation. The point is that risks are real but manageable, and proper imaging before any procedure significantly reduces uncertainty.
If both sides are symptomatic, it's common for patients to have both lower wisdom teeth removed in one session under local anesthesia or sedation. Related: if you're also asking can 2 wisdom teeth grow at the same time, that typically depends on your individual eruption timelines and whether they are independently impacted on each side. Upper and lower, or all four, can also be addressed together. Your surgeon will factor in your anatomy, health history, and the complexity of each tooth when planning the approach. Related to timing, if you're wondering whether both wisdom teeth grow at the same time or whether two can come in simultaneously, the answer is that they often develop in parallel even if symptoms appear at different times, which is exactly why a panoramic X-ray showing all four teeth at once is so useful.
Can a wisdom tooth 'grow back' if it never erupts? The regeneration reality
This question comes up more often than you'd think, especially when someone is told their wisdom tooth is impacted or when it seems like a tooth that was removed has started causing symptoms again. The honest answer: no, a wisdom tooth cannot grow back or re-erupt once its developmental window has passed or once it's been extracted.
Humans are diphyodonts, meaning we get exactly two sets of teeth (baby and adult) and that's it. Mammals largely lost the capacity for tooth regeneration over evolutionary time. While stem cells do exist in dental pulp and the tooth follicle, and they can contribute to the repair of existing dental hard tissue, there is no evidence that these cells have the competence to form an entirely new tooth from scratch. A wisdom tooth bud either develops and erupts (or partially erupts) during the normal window of ages 17 to 25, or it stays impacted. It doesn't disappear and reappear later.
What can happen is that an impacted or partially erupted wisdom tooth that has been asymptomatic for years suddenly becomes symptomatic, which can feel like the tooth is newly "growing." What's actually happening is that the tooth's position has shifted slightly, the surrounding bone has changed, or an infection has developed in tissue that was previously quiet. Research on serial panoramic X-rays confirms that some impacted lower third molars do eventually erupt spontaneously, but this is movement of a tooth that was already present and developing, not regrowth of a tooth that wasn't there. If a wisdom tooth has been surgically removed, there is no tooth bud remaining to regenerate it. The socket heals with bone and soft tissue, and that's the end of the story for that corner of your mouth.
Dental regeneration research is an active and genuinely exciting field, but as of today, the science of regrowing an entirely new human tooth is still experimental and not clinically available. If someone tells you a wisdom tooth "grew back" after extraction, what they almost certainly experienced was a retained root tip that was missed during surgery, a developing fourth molar that was present but unnoticed, or simply a different tooth causing symptoms in the same area. An X-ray will sort it out immediately.
FAQ
If I have symptoms on only one side, does that mean only one wisdom tooth is present?
Not necessarily. One side can hurt first because a lower tooth is more likely to trigger pericoronitis, and the other side may be impacted but quiet. The only reliable way to confirm what teeth are there is imaging, usually a panoramic X-ray (OPG) that shows all four corners at once.
Can wisdom teeth erupt on both sides at different times, even if they are coming in parallel?
Yes. Teeth often develop on similar schedules but symptoms can lag. For example, one lower tooth may partially erupt and start collecting food under the gum flap weeks or months before the corresponding tooth on the other side becomes symptomatic.
How long should I wait before contacting a dentist if I suspect a one-sided problem?
If there is noticeable swelling, bad taste, increasing pain, or any trouble opening your jaw, contact a dentist promptly rather than waiting for it to settle. Mild, occasional discomfort can sometimes be monitored briefly, but persistent or worsening symptoms should be assessed because pericoronitis can recur.
What is the difference between a tooth partially erupting and an impacted tooth that is staying stuck?
A partially erupting tooth has a visible edge or gum flap area you can sometimes clean, and symptoms may improve once the gum tissue settles. An impacted tooth is more likely to sit horizontally or at a blocking angle, where you cannot reach and clean under the operculum, leading to repeated flare-ups.
Is pericoronitis always an infection, or can it start as something less serious?
It often begins with inflammation from trapped debris, but it can progress to infection around the partially erupted tooth. Red flags that suggest more than mild irritation include fever, spreading facial swelling, difficulty swallowing, drooling, or voice changes.
If my panoramic X-ray shows both sides, why might only one side need extraction?
Some teeth are positioned in a way that causes symptoms or clear risk to adjacent teeth or nerves, while others may be present but relatively stable and easier to monitor. Extraction decisions are based on angulation, space, proximity to nerve structures, and whether the tooth is causing repeated inflammation.
Could a missing or “quiet” wisdom tooth be the upper side instead of the lower side?
Yes. Upper wisdom teeth can be less dramatic because they often have more space and may erupt with fewer noticeable symptoms. If you only checked based on pain, you could be missing an upper tooth that is present but not bothering you yet.
Do wisdom teeth on both sides always come out at the same time if both are problematic?
No. Even when both sides are symptomatic, clinicians may stage treatment depending on your anatomy, health factors, and which teeth are closer to nerves. Some people have both lower teeth addressed in one visit, but the safest plan is individualized after imaging and consultation.
Can a wisdom tooth “grow back” after it was extracted on one side?
A removed wisdom tooth cannot reappear because there is no remaining bud to develop. If symptoms return in the same area, common explanations are a missed root tip, another developing tooth (such as a retained or unnoticed fourth-molar variant), or a different source of pain, and X-rays can usually clarify which one it is.
What symptoms suggest the other side might be getting worse even before pain starts?
Watch for changes in smell or taste from the gum area, recurrent soreness around the back molars, or a sensation of a hard edge under the gum that becomes more noticeable over time. Because some impacted teeth are silent for years, periodic evaluation is useful if you have one active flare and worry about the remaining corners.
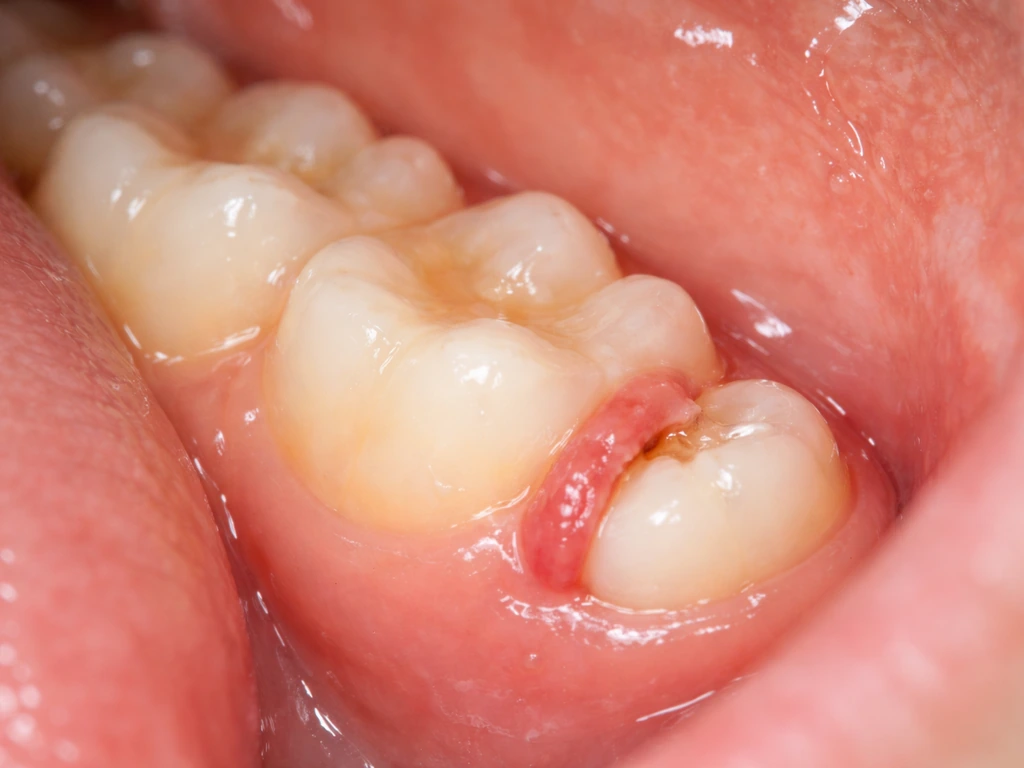
Learn if wisdom teeth truly grow out, normal eruption signs and timelines, red flags, and what to do next.
Do wisdom teeth grow at the same time? Learn typical eruption timeline, staggered patterns, and when to see a dentist.
Can milk teeth grow twice? Learn why baby teeth usually only get replaced, not regrown, and what to do if one falls out

