Yes, wisdom teeth do grow out of the gum, but they do it slowly, sometimes over months or even years, and they don't always make it all the way through. The process is called eruption, and it's not a sudden event. Your wisdom tooth starts deep in the jawbone and gradually pushes upward through bone and gum tissue until it either emerges fully, partially, or gets stuck (impacted). So if you're feeling pressure, tenderness, or noticing a tooth slowly peeking through, you're likely watching a normal developmental process, or, in some cases, one that needs a dentist's attention.
Do Wisdom Teeth Grow Out of the Gum? What’s Normal
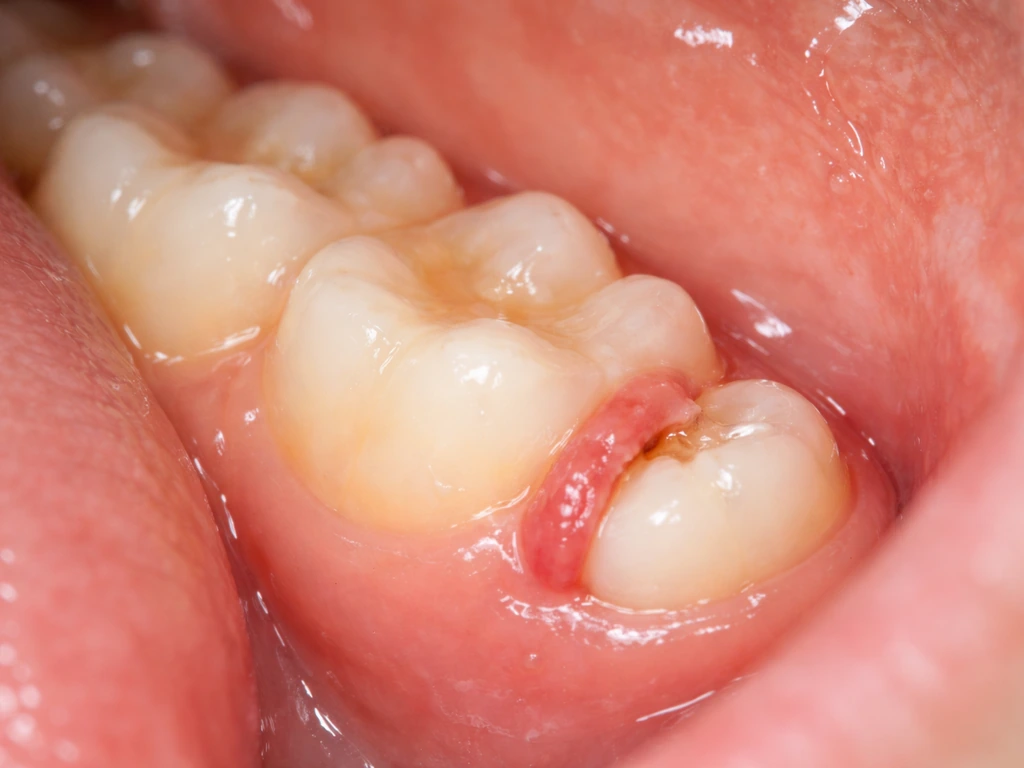
What 'growing through the gum' actually means for wisdom teeth
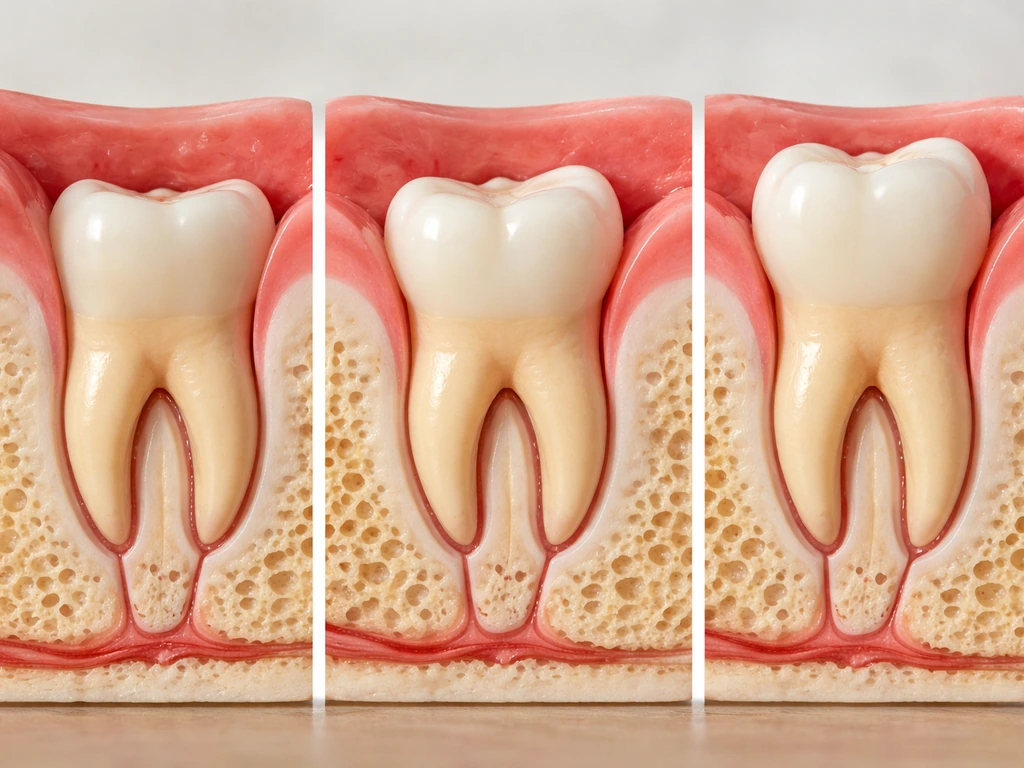
The technical term for a tooth coming through the gum is eruption. It's not like a tooth just suddenly pops up one day. Eruption is a coordinated biological process where the tooth moves vertically from its developmental position deep in the jaw, through alveolar bone, and finally through the gum tissue into your mouth where it can eventually meet its opposing tooth. Bone and soft tissue actively remodel to create a pathway for the tooth, it's quite a production happening beneath the surface before you ever see or feel anything.
For wisdom teeth specifically, this process starts years before you ever notice it. The tooth forms, the roots begin developing, and slowly the whole structure migrates upward. When people say a wisdom tooth is 'growing in,' they mean this eruption process is underway. The gum doesn't just move out of the way cleanly, the tooth has to break through the tissue, which is part of why it can feel sore and swollen when it's happening.
Normal eruption timeline and what it can look like
Wisdom teeth typically begin erupting between ages 17 and 25, though the AAPD notes the range can extend to age 30 for both the upper and lower sets. Peak activity tends to fall in the early-to-mid 20s. So if you're 19 and just starting to feel them, that's completely normal. If you're 27 and one is just now making an appearance, that's also within range.
Partial eruption is extremely common. Many wisdom teeth poke through the gum just enough to be visible, a small white tip, a slight bump, or a flap of gum tissue half-covering the tooth's biting surface. Full eruption, where the tooth comes all the way in and sits in a clean, usable position, is actually less common for wisdom teeth than for other molars. The tooth may stay partially exposed for months while the gum slowly recedes around it, or it may never fully emerge. In some cases, a wisdom tooth's position or partial eruption can seem like it is affecting nearby soft tissue, so you may wonder whether it can grow into your cheek can wisdom teeth grow into your cheek.
Early signs that eruption is underway include mild pressure or aching at the back of the jaw, tenderness in the gum behind your last visible molar, occasional jaw soreness, and sometimes a slight swelling of the gum tissue back there. These are normal signs that something is moving. They tend to come and go rather than stay constant, especially early on.
Why wisdom teeth can seem stuck, delayed, or like they 'grow in and out'
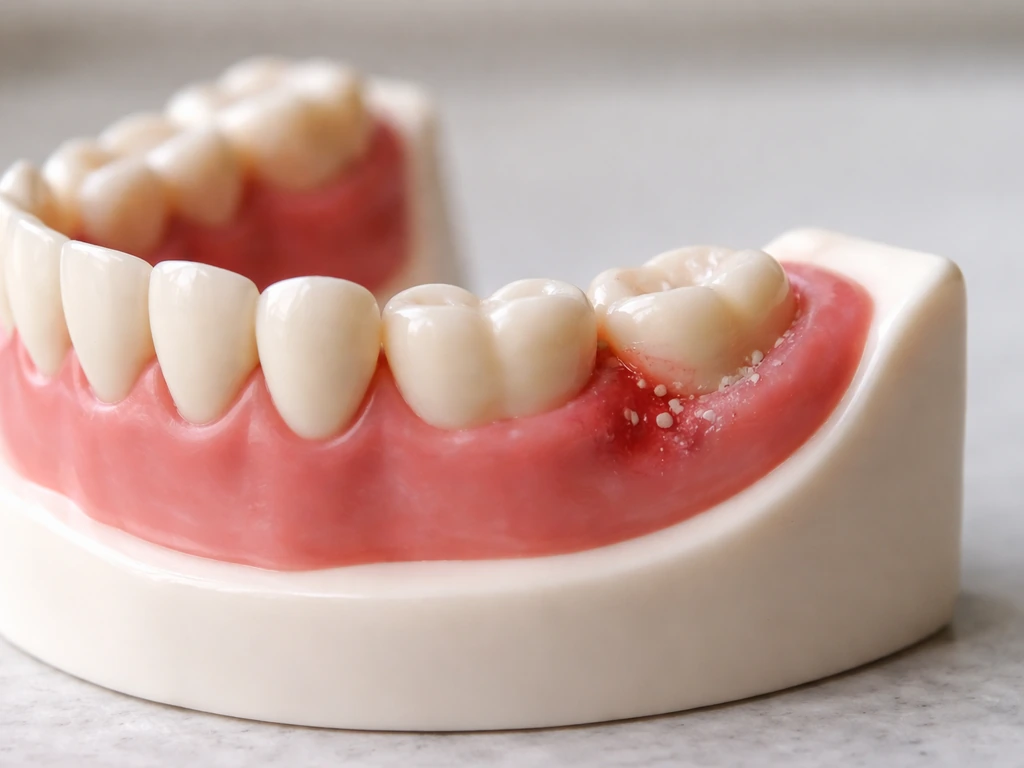
This is one of the most confusing things about wisdom teeth. You might feel pressure and soreness for a week, then nothing for months, then the whole cycle starts again. It genuinely can feel like the tooth is coming and going. What's actually happening is that eruption is not a continuous process, it moves in fits and starts, and the soreness correlates with active movement phases.
Some wisdom teeth get truly stuck, a state called impaction. There are two main reasons this happens: the tooth never rotates from a sideways or angled position into a more vertical one, or there simply isn't enough space in the jaw for the tooth to emerge. Modern human jaws tend to be smaller than our ancestors' jaws, which is a widely cited reason wisdom teeth cause so many problems, there's just no room at the inn. Impaction can be partial (tooth is stuck but some of it breaks through the gum) or complete (the tooth never makes it through the gum at all and stays entirely within bone).
Impacted wisdom teeth are classified by their angle and depth. Winter's classification describes positions like vertical, horizontal, mesioangular, and distoangular based on how the tooth is tilted relative to the second molar next to it. Pell and Gregory classification further describes depth, whether the tooth is level with or below the neighboring tooth's chewing surface, and how much of the jawbone's ramus is covering it. These classifications matter when your dentist is deciding how complex a potential extraction might be.
It's also worth knowing that what looks like a wisdom tooth 'going back in' is actually the gum tissue swelling over a partially erupted tooth during inflammation, then calming down. The tooth itself doesn't move backward, your perception of it changes based on how much gum tissue is covering it at any given time.
Normal discomfort vs. red flags you shouldn't ignore
Mild, intermittent soreness and pressure at the back of the jaw are normal parts of wisdom tooth eruption. What you want to watch out for is when symptoms shift from 'a bit annoying' to 'something is actually wrong.' The most common problematic condition associated with partially erupted wisdom teeth is pericoronitis, inflammation of the gum tissue surrounding the partially emerged tooth. It affects the operculum, which is the flap of gum tissue sitting over the tooth, and it's driven by bacteria and food debris getting trapped under that flap where a toothbrush can't reach. Pericoronitis is most common in people aged 20 to 29.
The distinction between normal eruption discomfort and pericoronitis matters a lot. Here's a practical way to think about it:
| Symptom | Likely Normal Eruption | Possible Pericoronitis / Red Flag |
|---|---|---|
| Jaw pressure or mild aching | Yes, common | Not specific on its own |
| Gum tenderness behind last molar | Yes, expected | More intense and localized |
| Swelling of the gum at the back | Mild and temporary | Persistent, spreading, or worsening |
| Bad taste or smell from the area | No | Yes — sign of infection under the operculum |
| Pus or discharge | No | Yes — see a dentist promptly |
| Fever or general feeling unwell | No | Yes — urgent dental/medical attention needed |
| Difficulty opening your mouth (trismus) | No | Yes — this is a red flag, seek care today |
| Difficulty swallowing or breathing | No | Yes — emergency, go immediately |
The most serious pericoronitis warning signs are trismus (limited mouth opening), fever and malaise, visible facial swelling that creates asymmetry, difficulty swallowing, and in severe cases, any change in your voice or breathing. These suggest the infection may be spreading beyond the local area, which can become dangerous quickly. Don't wait those out at home with saltwater rinses.
What a dentist will check and what treatment can look like
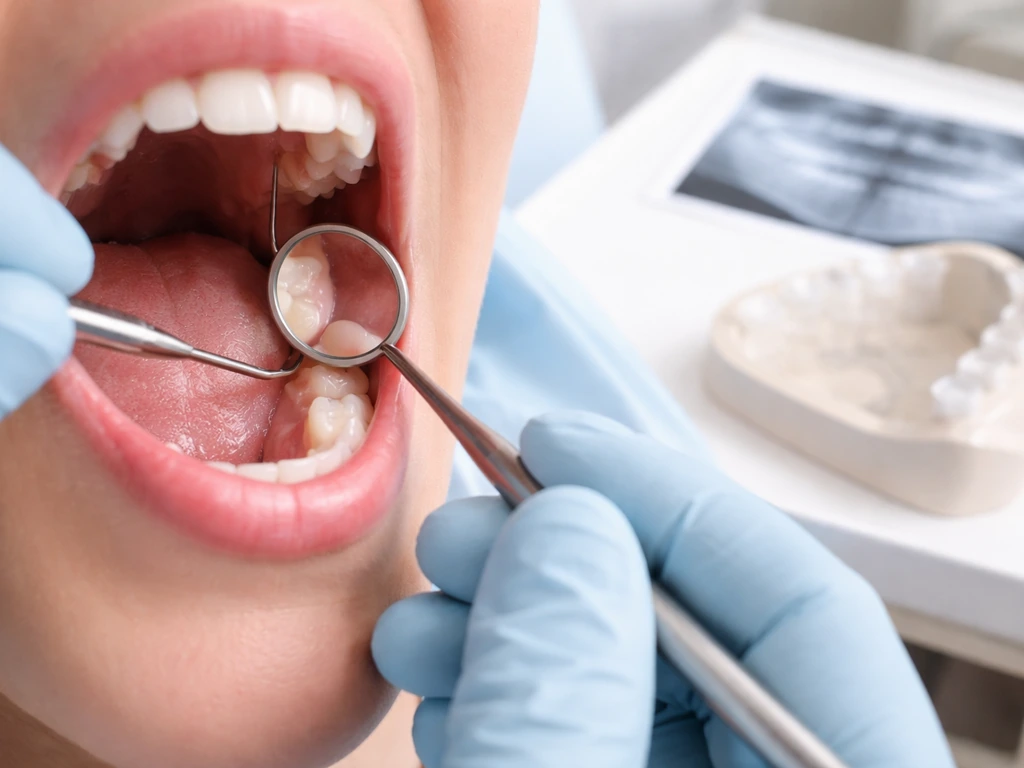
At a dental visit for a wisdom tooth concern, your dentist will do a clinical exam of the area, probing the gum, checking the operculum, looking for swelling, redness, or discharge, and assessing whether there's pus. They'll ask about your symptoms: how long, how severe, any fever? Then they'll take X-rays. Panoramic radiographs (the wide film that images all your teeth at once) and periapical X-rays are typically the starting point. These show the tooth's position, angle, root development, and its relationship to surrounding bone.
For complex cases, particularly when the lower wisdom tooth appears close to the inferior alveolar nerve (the main nerve running through your lower jaw), a CBCT (cone beam CT) scan may be recommended. This gives a 3D view that a standard X-ray can't provide and helps plan extraction in a way that minimizes nerve risk. CBCT isn't routine for every wisdom tooth evaluation, but it's valuable when standard imaging raises concerns.
Treatment paths depend heavily on what's found. If a tooth is erupting normally with mild pericoronitis, the dentist may clean and irrigate under the operculum, have you rinse with an antiseptic mouthwash, and monitor. Antibiotics are not the default, current guidelines reserve them for specific situations: fever, spreading infection, persistent swelling that doesn't respond to local treatment, or trismus. Routine pericoronitis without those features is managed locally, not with antibiotics.
If the operculum keeps causing recurrent infections, operculectomy (surgically removing that flap of gum tissue) is sometimes performed to expose the tooth and eliminate the trap. And if the wisdom tooth is impacted, repeatedly infected, causing crowding, or damaging the adjacent second molar, extraction is often the recommended path. Whether you need a general dentist or an oral surgeon depends on the tooth's position and complexity.
Can a wisdom tooth 'grow back' or regenerate?
This question comes up a lot, and the answer is no, not in any meaningful biological sense. Wisdom teeth are not a 'bonus set' that grows on demand later in life. They form as part of normal dental development, and the eruption process is a one-way journey: the tooth either makes it through the gum or it doesn't. Eruption is driven by bone remodeling and the forces of root development, not by any regenerative capacity.
If a wisdom tooth gets extracted, it does not grow back. Humans have two sets of teeth, baby teeth and permanent teeth, and wisdom teeth are simply the last permanent molars to develop. There is no third set waiting in reserve. Once a wisdom tooth is gone, it's gone permanently, just like any other adult tooth.
What sometimes gets mistaken for 'regrowth' is a tooth that was impacted and partially hidden in bone becoming more visible over time, or a small piece of root left after an extraction slowly working its way toward the surface. Neither of these is regeneration. Similarly, if eruption stalls entirely without a physical obstruction, a condition called primary failure of eruption, the tooth doesn't eventually try again. The eruption mechanism has simply stopped, and that requires clinical management, not waiting for nature to restart the process.
The biology of wisdom tooth eruption is fascinating, but it has hard limits. The tooth moves through bone and gum in a carefully coordinated process involving bone resorption and remodeling. That process doesn't reset after extraction, and it can't be triggered from scratch once development is complete. Understanding this is important because it means impacted or problematic wisdom teeth need to be managed proactively, not passively hoped away.
Practical next steps based on where you are right now
If you're feeling mild pressure and soreness at the back of your jaw and you're in your late teens or 20s, it's worth booking a dental check-up so your dentist can take baseline X-rays and confirm the eruption is progressing normally. You don't need to be in pain to go, catching an impaction early makes management much simpler.
If you have swelling, a bad taste, or pain that's been building for more than a few days, don't put it off. That combination points toward pericoronitis and it won't sort itself out without some intervention. Rinse with warm salt water in the meantime, but get seen.
And if you have fever, difficulty opening your mouth, or swelling spreading toward your neck or face, treat it as urgent. Go to a dentist today or head to an emergency clinic. These are not symptoms to manage at home.
One more thing worth knowing: wisdom teeth don't always all come in at the same time, and it's quite common for only one or two to erupt while others stay impacted or never develop at all. The exact pattern varies from person to person. So if one side is acting up and the other isn't, that's normal, everyone's eruption timeline is a little different. Wisdom teeth can also erupt at different times, so it may be normal for one tooth to come in while the other lags behind come in at the same time. Wisdom teeth can erupt on either side of your mouth, and symptoms may appear more on one side than the other.
FAQ
How long should a wisdom tooth be sore before it settles?
Eruption discomfort often comes and goes, but if soreness consistently worsens over several days or you start seeing increasing swelling around the partially erupted area, that is a sign to contact your dentist to rule out pericoronitis.
Is it normal for a wisdom tooth to only show a small white tip for months?
Yes, partial eruption is common. The key caveat is whether the gum flap starts trapping food and causing repeated inflammation, which can lead to recurring pain, bad taste, or gum discharge.
What can I do at home if my gum is tender around a partially erupted wisdom tooth?
You can rinse gently with warm salt water and keep the area clean, but avoid aggressive poking under the gum flap. If symptoms persist beyond a few days, keep appointments, because pericoronitis usually needs local cleaning or other treatment.
Does a “bad taste” mean I definitely have an infection?
Not always, but a foul or persistent taste along with gum tenderness behind the last molar raises suspicion for inflammation under the operculum. If you also notice swelling, worsening pain, or any fever, get evaluated promptly.
Can wisdom tooth pain be confused with an earache or jaw joint pain?
Yes. Back-of-mouth tooth pain can feel like it radiates to the ear or makes chewing feel off. However, if you have limited mouth opening, fever, or facial swelling, treat it as more than simple eruption discomfort and seek care.
If one wisdom tooth is erupting, should both sides start at the same time?
No. It is common for only one side or only one tooth to become symptomatic first, while others stay fully impacted or erupt later. Asymmetry in timing and symptoms is usually expected.
What should I do if I feel like the tooth is “going back in” when my gum swells?
That perception is often due to changes in gum inflammation, not the tooth moving backward. Still, if the episode repeats or becomes more frequent, ask your dentist about recurrent pericoronitis and whether local management or operculectomy is appropriate.
Are antibiotics always needed for wisdom tooth gum flap inflammation?
No. Antibiotics are usually reserved for red flags such as fever, spreading swelling, trismus, or infection that does not improve with local cleaning and antiseptic rinses. Ask your dentist what criteria apply to your case.
When is it urgent enough to go to emergency care?
Go urgently if you have fever, trouble swallowing, difficulty opening your mouth (trismus), swelling that is rapidly spreading, or any breathing or voice changes. These can indicate infection beyond the local gum area.
Can I delay treatment if the pain improves on its own?
Short-term improvement can happen when swelling calms down, but repeated flare-ups suggest ongoing issues. If you have recurrent symptoms, get an exam and imaging so the dentist can confirm whether the problem is impaction-related or pericoronitis.
Will an X-ray always be enough, or might I need a CBCT?
Many cases can be planned with panoramic or periapical X-rays. CBCT is more likely when the lower tooth appears close to the inferior alveolar nerve or when standard images create uncertainty about depth and nerve proximity.
If I had a wisdom tooth removed, can it regrow later?
No. A removed wisdom tooth does not regenerate. What can happen instead is that the area continues to have issues during healing, or a small remaining root fragment becomes less visible over time, which is not true regrowth.
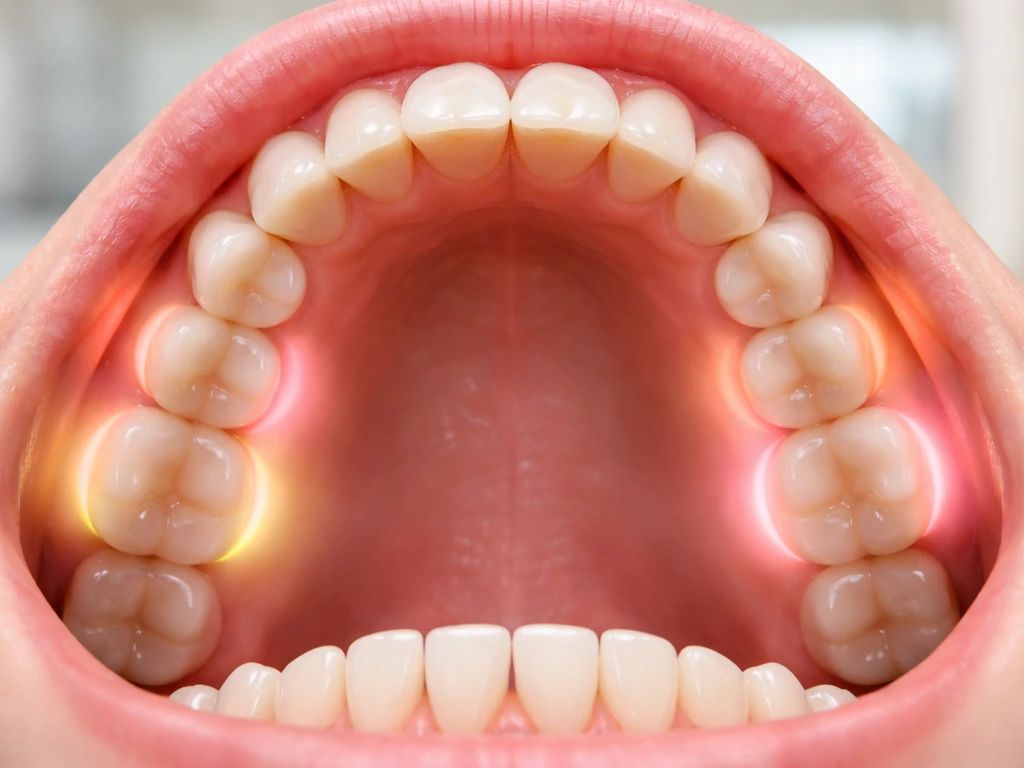
Do wisdom teeth grow at the same time? Learn typical eruption timeline, staggered patterns, and when to see a dentist.
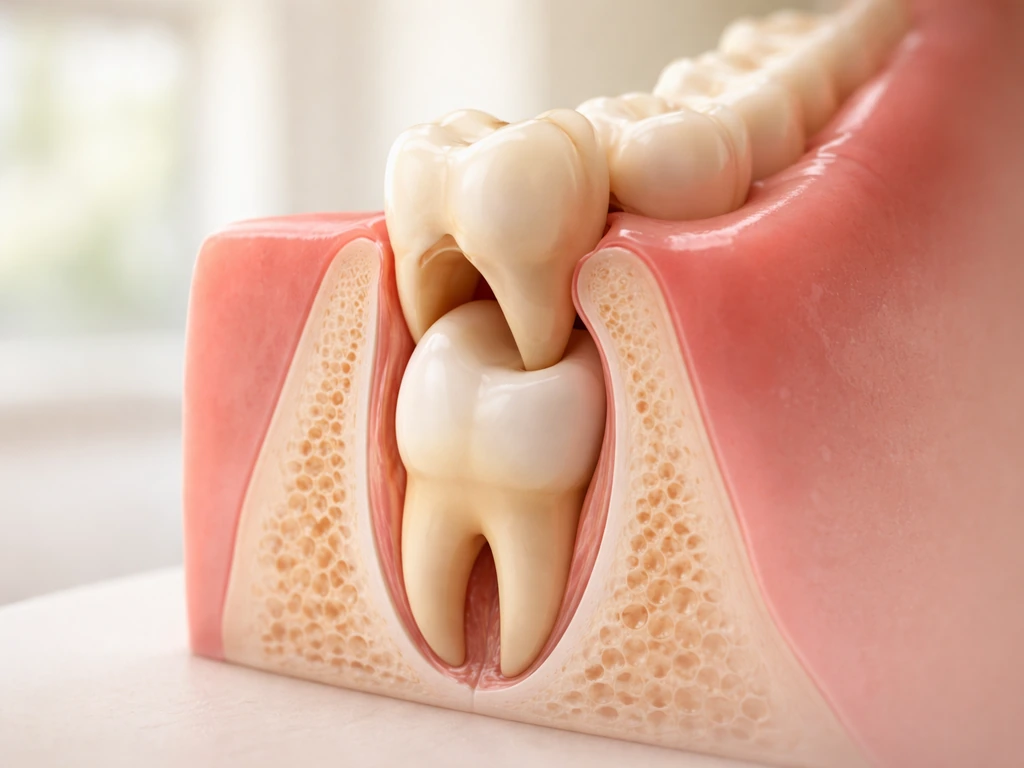
Can milk teeth grow twice? Learn why baby teeth usually only get replaced, not regrown, and what to do if one falls out

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn

