Yes, wisdom teeth can absolutely start growing (erupting) at 15. While the textbook average is 17 to 25, some teens see their first signs of wisdom tooth activity in their mid-teens. It is earlier than typical, but it is not abnormal. What matters is what is happening under the gum, and a quick dental X-ray can tell you exactly where things stand.
Can Wisdom Teeth Grow at 15? Timeline, Signs, and Next Steps
"Growing" vs. "regrowing": an important distinction
Before anything else, let's clear up a confusion that trips a lot of people up. When most teens or parents ask whether wisdom teeth can "grow" at 15, they mean eruption: the tooth that has been developing under the gum for years is finally pushing through the surface. That is completely different from regeneration, which would mean forming a brand-new tooth from scratch. Human adults cannot regenerate teeth. If a tooth never formed, or if it is removed, it does not grow back. Research into dental stem cells is ongoing and genuinely exciting, but it is nowhere near a clinical reality for patients right now. So when your 15-year-old says their wisdom tooth is "growing in," they are describing eruption, not magic.
This distinction matters on this site because a common internet rumor suggests wisdom teeth can somehow appear late as a kind of "regrowth" if they did not come in earlier. That is not how it works biologically. The tooth either formed during childhood development or it did not. Agenesis (when a wisdom tooth simply never develops) affects a significant portion of the population, and there is no natural process that creates a new third molar later in life.
How wisdom teeth actually develop, and where age 15 fits
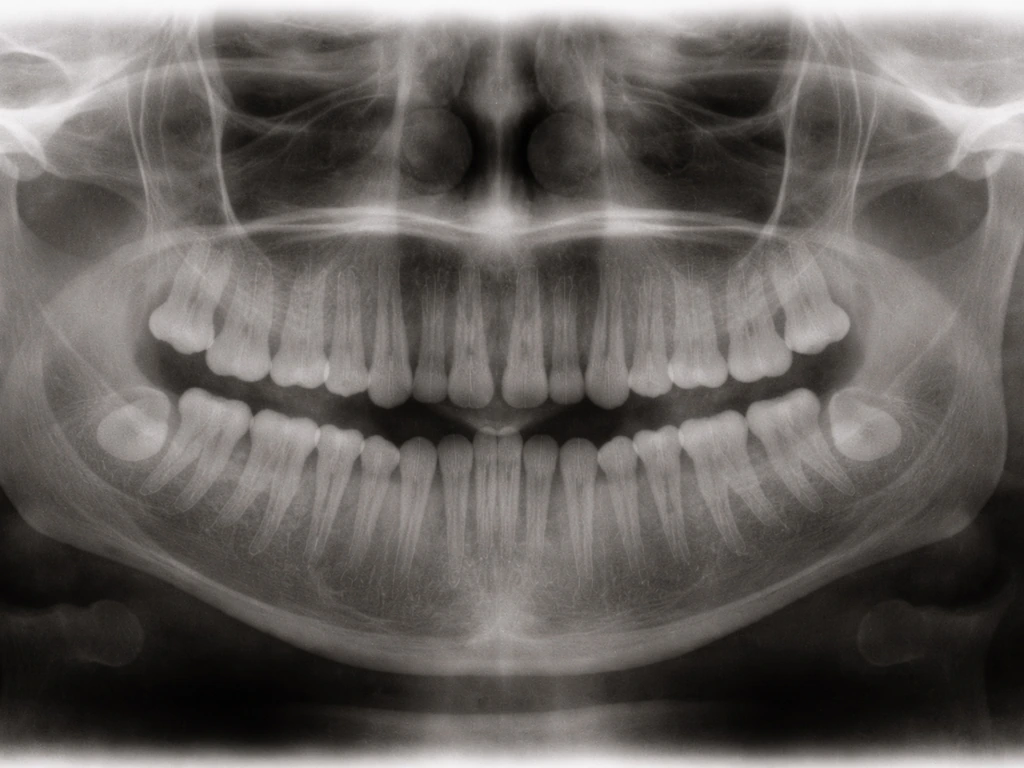
Wisdom tooth development starts much earlier than most people realize. Radiographic evidence shows crypt formation (the very beginning of tooth development) can appear as early as age 5. By the time a teen is 12 to 16, crown mineralization is typically complete and the roots are actively developing while the tooth sits behind the second molar, still below the gumline. The ADA eruption chart places wisdom tooth eruption at roughly 17 to 21 years, and the AAOMS puts the range at 17 to 25. But these are averages, not rules. If you are asking can wisdom teeth grow at 12, the short answer is yes, the underlying development can start much earlier than people think.
Eruption timing varies significantly from person to person, driven by genetics, jaw size, the position of the tooth, and how much room exists behind the second molar. Some people erupt wisdom teeth at 14 or 15. Some do not see movement until their mid-twenties. A 15-year-old with early signs of eruption is simply on the earlier end of a wide and normal biological range, not an outlier who needs to panic.
Siblings of this topic like wisdom teeth at 14 or at 16 follow the same underlying biology. The difference in age is minor; what changes the story is the tooth's position and whether there is enough space for it to come in cleanly.
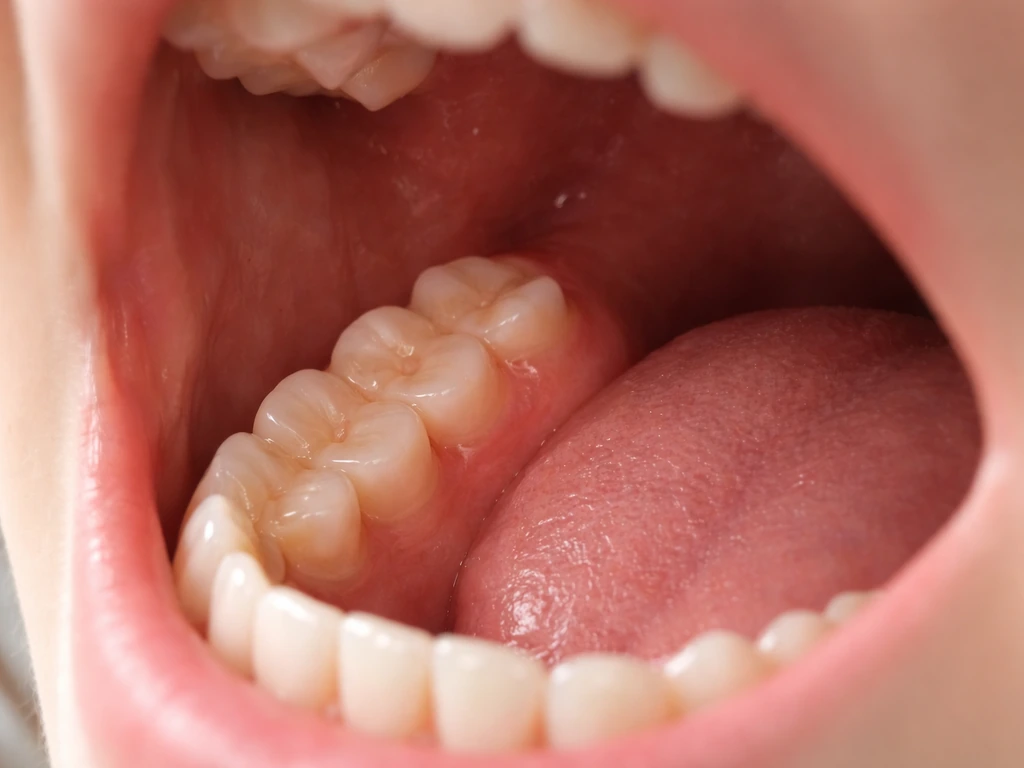
Signs that point to wisdom teeth coming in at 15
The most reliable sign is noticing a new molar appearing at the very back of the mouth. But that is often the final stage. Earlier warning signs are subtler and easy to confuse with other dental issues.
- Aching or pressure at the back of the jaw, usually behind the second molar
- Soreness or tenderness in the gum at the back of the mouth that comes and goes
- A flap of gum tissue (called an operculum) that feels raised or irritated over a barely visible tooth
- Mild swelling along the back of the lower or upper jaw
- A bad taste or bad breath that does not go away with brushing, which can signal bacteria trapped under gum tissue
- Jaw stiffness or mild difficulty opening the mouth wide, in more significant cases
That operculum situation has a clinical name: pericoronitis. It happens when a wisdom tooth only partially erupts and leaves a flap of gum tissue that traps bacteria and food. It is genuinely common in teenagers and young adults, and a 2026 study in Frontiers in Dental Medicine found that for many people, their first painful episode started before age 18. Mild pericoronitis can resolve as the tooth continues to erupt into a position that can be cleaned. But it can also escalate, which is why it needs attention.
How a dentist confirms what is happening
A visual exam can catch a tooth that has already broken through the gum, but the real information comes from imaging. A panoramic X-ray (an OPG) is the standard first step. It shows all four wisdom teeth at once, their angle, their depth below the gumline, how much root has formed, and whether the tooth has a clear path to erupt. Dental guidelines recommend panoramic imaging as the baseline assessment for third molar evaluation.
If the panoramic view suggests a lower wisdom tooth is sitting very close to the inferior alveolar nerve, the dentist or oral surgeon may order a CBCT scan (cone beam computed tomography). This gives a three-dimensional picture that quantifies exactly how close the tooth root is to the nerve, which is critical information for anyone considering extraction. For most 15-year-olds whose roots are not fully formed yet, the panoramic X-ray is usually enough to make a plan.
Dentists and oral surgeons also use standardized classification systems like Winter's classification and the Pell-Gregory classification to describe a wisdom tooth's angle (vertical, horizontal, mesioangular, distoangular) and its depth relative to the second molar and the jawbone. This is not just academic: these classifications directly predict how difficult extraction would be if it becomes necessary, and they guide the conversation about monitoring versus acting now.
Monitor or remove? What the dentist is weighing
This is the question most parents want answered first, and it genuinely depends on what the X-ray shows. There is no universal answer. Both the AAOMS and NICE (the UK's clinical guidance body) emphasize evidence-based decision-making rather than automatic removal of any wisdom tooth that causes any discomfort.
| Scenario | Likely recommendation | Why |
|---|---|---|
| Tooth is erupting vertically with adequate space, no symptoms | Monitor with periodic X-rays | Good chance it comes in without problems |
| Tooth is partially erupted with mild pericoronitis | Monitor or treat pericoronitis first, reassess | Inflammation may resolve as tooth moves into a cleanable position |
| Tooth is horizontally or severely angularly impacted | Extraction often recommended | Unlikely to erupt properly and can damage adjacent tooth |
| Recurrent pericoronitis, cyst formation, or damage to second molar | Extraction recommended | Active disease is present and unlikely to self-resolve |
| Roots less than two-thirds formed (common at 15) | Often monitor unless clear problems | Earlier extraction is technically easier and recovery is faster |
One thing the AAOMS is clear about: extraction gets more complicated as roots fully develop and the jawbone gets denser with age. At 15, roots are often still partially formed, which can actually make the procedure technically simpler if removal is eventually needed. This is why some oral surgeons discuss early germectomy (removal of the tooth germ before the roots fully develop) in teenagers between 12 and 16, particularly for teeth that appear clearly impacted. It is not automatic, but it is a real option worth discussing.
What to do right now if you're 15 (or the parent of a 15-year-old)
- Book a dental appointment soon, ideally within the next few weeks. Do not wait until the pain becomes severe.
- Ask for a panoramic X-ray if one has not been taken in the last year or two. This gives the full picture of all four wisdom teeth at once.
- Tell the dentist exactly where the discomfort is, how long it has been happening, and whether there is swelling, bad taste, or difficulty opening your mouth.
- Ask whether the dentist wants to refer to an oral surgeon, especially if the teeth appear impacted or there are nerve proximity concerns.
- If you wear braces or have had orthodontic treatment, mention this. Emerging wisdom teeth can influence alignment and your orthodontist should be in the loop.
Managing discomfort while you wait for your appointment
If there is mild aching or pressure while you wait, over-the-counter NSAIDs like ibuprofen are the first-line option for dental pain, according to ADA evidence-based guidelines. Ibuprofen reduces both pain and inflammation, which is particularly helpful when gum tissue is the source of discomfort. Acetaminophen can be used alone or combined with ibuprofen for additional relief. Always use the dose appropriate for the teen's age and weight, and follow package instructions.
Rinsing with warm salt water a couple of times a day helps reduce bacteria around the eruption site and can soothe irritated gum tissue. Gentle brushing around the back teeth, even if it is a little uncomfortable, is important because bacterial plaque under the gum flap is what drives pericoronitis. Keeping that area as clean as possible is one of the most useful things you can do at home.
Red flags that mean go sooner, not later

Mild soreness is manageable while you wait a week for an appointment. These symptoms are not manageable and need same-day or emergency dental care:
- Significant swelling that extends outside the mouth or toward the neck
- Difficulty swallowing or opening your mouth more than a couple of centimeters
- Fever combined with mouth or jaw pain
- A bad taste or pus coming from around the back tooth
- Pain that is rapidly worsening despite pain medication
These can indicate a spreading infection from pericoronitis into the deeper spaces of the head and neck, which is genuinely serious. It is rare, but it can happen quickly and it needs professional treatment right away, not home remedies.
The bottom line
Wisdom teeth at 15 are not a myth or a problem by default. If you are wondering whether wisdom teeth can grow at 16, the same rules about eruption timing and dental X-rays apply Wisdom teeth at 15. If you are wondering can wisdom teeth grow at 13, the same eruption biology can apply, just on an earlier end of the normal range Wisdom teeth at 15. Eruption at this age is biologically possible and happens for some teens, even though the average timeline runs a few years later. What you are dealing with is a tooth that has been developing since childhood finally making its move. Get a panoramic X-ray, find out where the tooth is and what angle it is coming in at, and then have a real conversation with your dentist or oral surgeon about whether to watch and wait or act early. The earlier you have that conversation, the more options you have.
FAQ
If my 15-year-old has back-of-mouth pain, does that automatically mean a wisdom tooth is erupting?
In most cases, yes, pain and swelling at 15 can be linked to an erupting wisdom tooth, especially if discomfort is localized behind the second molar or comes and goes as the gum flap changes. However, similar symptoms can also come from a cavity in the second molar, a gum infection unrelated to the third molar, or a dental abscess, which is why an exam and usually a panoramic X-ray matter.
How long is it safe to wait before seeing a dentist if wisdom teeth symptoms start at 15?
You should not try to “wait it out” if there are red flags such as fever, rapidly spreading swelling, trouble swallowing, difficulty opening the mouth, or facial redness. If none of those are present and symptoms are mild, a short wait for a dental appointment is reasonable, but the appointment should not be weeks away because pericoronitis can flare up unpredictably.
When do dentists move from an OPG to a CBCT scan for a wisdom tooth at 15?
A panoramic X-ray (OPG) typically shows tooth position, angulation, and general depth. A CBCT is usually reserved for cases where the tooth is near the inferior alveolar nerve or when extra 3D detail is needed for a safe plan, such as extraction complexity. For many 15-year-olds, the OPG is enough to decide whether to monitor or refer.
If a wisdom tooth is only partly out at 15, what determines whether we monitor or treat?
Partial eruption can create a gum flap that traps food, but the key detail is whether it is cleanable and whether the tooth is trending toward a healthy, fully erupted position. If the flap keeps re-inflaming or the tooth is angulated toward the second molar, monitoring may be less favorable. Your dentist can score this using clinical findings and imaging-based classifications to decide between watchful waiting and intervention.
Does having no wisdom-tooth symptoms at 15 mean they will never erupt?
Yes, even if wisdom teeth are “developing” early under the gum, the first eruption signs may not happen until later. That means a lack of symptoms at 15 does not prove there are no wisdom teeth, and a scan can clarify whether teeth are present, impacted, and how much space exists.
What makes someone a candidate for early germectomy at age 15?
Early germectomy is sometimes discussed for specific cases, usually when a developing tooth is clearly impacted and timing matters for risk reduction. It is not for every situation, and decisions depend on tooth position, root stage, and the teen’s overall dental development. Ask your oral surgeon how they determine eligibility and what the expected outcome is for that exact tooth.
Are NSAIDs like ibuprofen safe for wisdom-tooth pain in teens, and what dosing mistakes should we avoid?
Ibuprofen is commonly used for dental pain, but teens should avoid doubling up on other NSAIDs and should follow the labeled dose based on age and weight. If there is a history of stomach ulcers, kidney issues, or medication conflicts, the dentist or pediatrician should guide the choice. Also, do not apply topical numbing gels excessively to the gum flap, since they can irritate tissue if used incorrectly.
If salt-water rinses help briefly, should we still get it checked?
Warm salt-water rinses can reduce bacteria around the eruption site and soothe inflamed gum tissue, but they do not remove trapped debris under the flap if the tooth is angled or food keeps getting stuck. If home care helps temporarily but symptoms keep returning, it usually means professional cleaning, targeted evaluation, or a longer-term plan is needed.
Can wisdom teeth at 15 cause crowding, and how do we tell if it is actually the third molars?
Wisdom teeth can contribute to crowding symptoms, but crowding at 15 can also come from eruption of other teeth, orthodontic shifts, or habits. Imaging helps separate “space issues” from “tooth position issues.” If your dentist suspects wisdom teeth are pushing adjacent teeth, ask what to monitor and how often you should re-check with X-rays or orthodontic visits.
Learn if wisdom teeth can erupt at 16, what true regrowth means, eruption timeline, and next steps for evaluation.
Can wisdom teeth erupt at 14? Learn eruption vs development, signs, timelines, and when to see a dentist.

Teeth rarely regrow after permanent set: most people get one replacement only. Learn limits, myths, and what to do next.

