Human teeth don't grow back. Once a permanent tooth is lost, damaged beyond repair, or fails to erupt, your body has no built-in mechanism to replace it. That's not a myth or a scare tactic, it's simply how human biology works. Unlike sharks, which cycle through thousands of teeth in a lifetime, humans get exactly two sets: baby teeth and permanent teeth. When the second set is gone, it's gone. But understanding why that happens, what goes wrong when a tooth doesn't appear on schedule, and what you can actually do about it today, that's where the real, practical value is.
Why Teeth Don’t Grow Back: Causes and Next Steps
What 'not growing back' really means
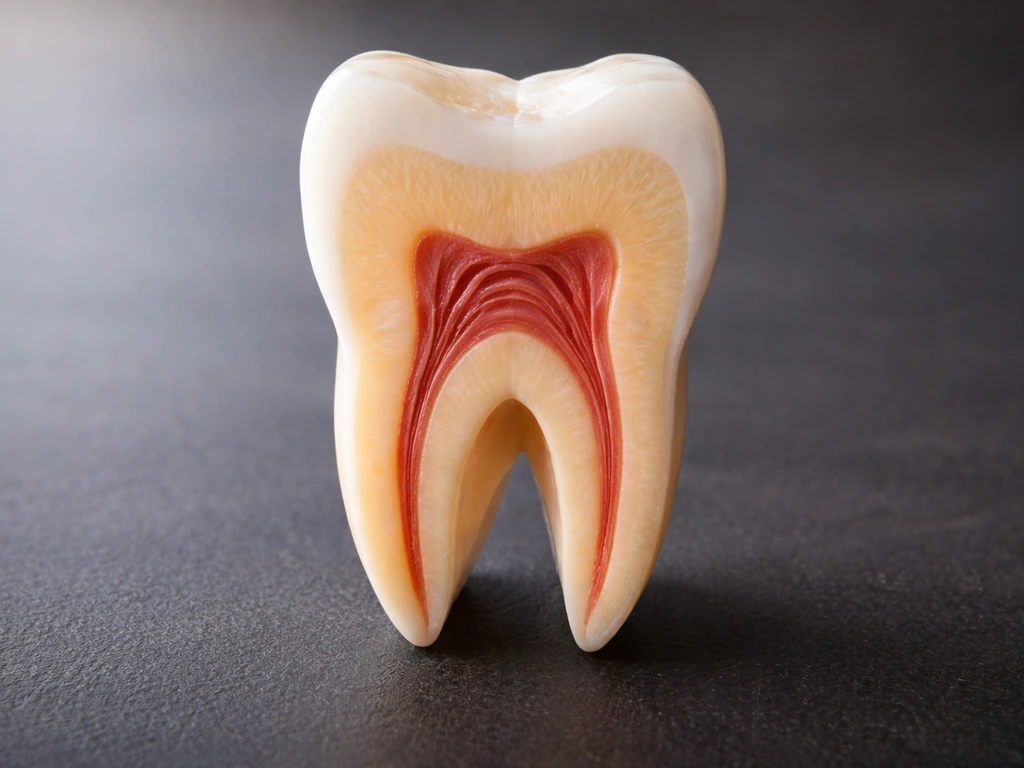
When people say a tooth 'won't grow back,' they're usually talking about one of a few very different situations: a permanent tooth that was knocked out or extracted, a tooth that cracked or decayed past saving, or a tooth that simply never erupted. These are all real scenarios, but they involve different biology and have different solutions. It's also worth separating the tooth as a whole from its individual components, because the layers of a tooth have very different regenerative abilities (or lack thereof).
The outermost layer, enamel, cannot grow back at all once it's lost. The layer beneath it, dentin, has a very limited and imperfect ability to lay down new hard tissue in response to injury, but it's not true regeneration. The pulp (the living tissue inside the tooth containing nerves and blood vessels) and the roots have essentially no capacity to regrow once destroyed or removed. The gap where a tooth used to be won't fill itself in. That's the honest summary, and the sections below explain exactly why.
The biology behind why teeth don't regrow
Tooth development is a one-time event driven by specialized cells that disappear after they finish their job. Enamel, for example, is built by cells called ameloblasts. These cells form part of what's called the enamel organ during tooth development, secreting enamel proteins and building the hardest substance in your body. The catch: once a tooth erupts, ameloblasts undergo programmed cell death (apoptosis). They're simply gone. There are no ameloblasts left in an adult mouth, no stem-cell niche to restart them, and no signal that could coax new ones into existence. Research using single-cell analysis of human tooth development has confirmed there is no active enamel-secreting population remaining after eruption. This is exactly why enamel cannot grow back on its own, no matter what a supplement ad tells you.
Dentin is slightly more interesting. Odontoblasts, the cells that build dentin, can persist inside a living tooth and respond to injury by laying down what's called tertiary dentin, a kind of patch job. But research is clear that this is largely a reparative or protective process, not true regeneration. When the original odontoblasts die from severe injury or infection, any new hard tissue formed afterward may actually be calcified scar tissue rather than a properly structured pulp-dentin complex. You can learn more about exactly how dentin grows back (and its limits) if you want the full breakdown. The short version: it's not reliable, it's incomplete, and it stops nowhere near replacing a whole tooth.
Roots are equally fixed. Once a root is lost, whether from extraction, advanced gum disease, or trauma, there's no restart. The periodontal ligament (which anchors the root to bone) and the cementum covering the root surface don't regenerate in any meaningful way on their own. Curious about whether teeth roots can grow back? The answer is essentially no, though bone and soft tissue can partially remodel around an area, which matters for implant planning. Similarly, teeth nerves don't grow back once the pulp is removed or destroyed, which is why root canal treatment replaces rather than restores the living pulp.
What actually happens when a tooth is missing
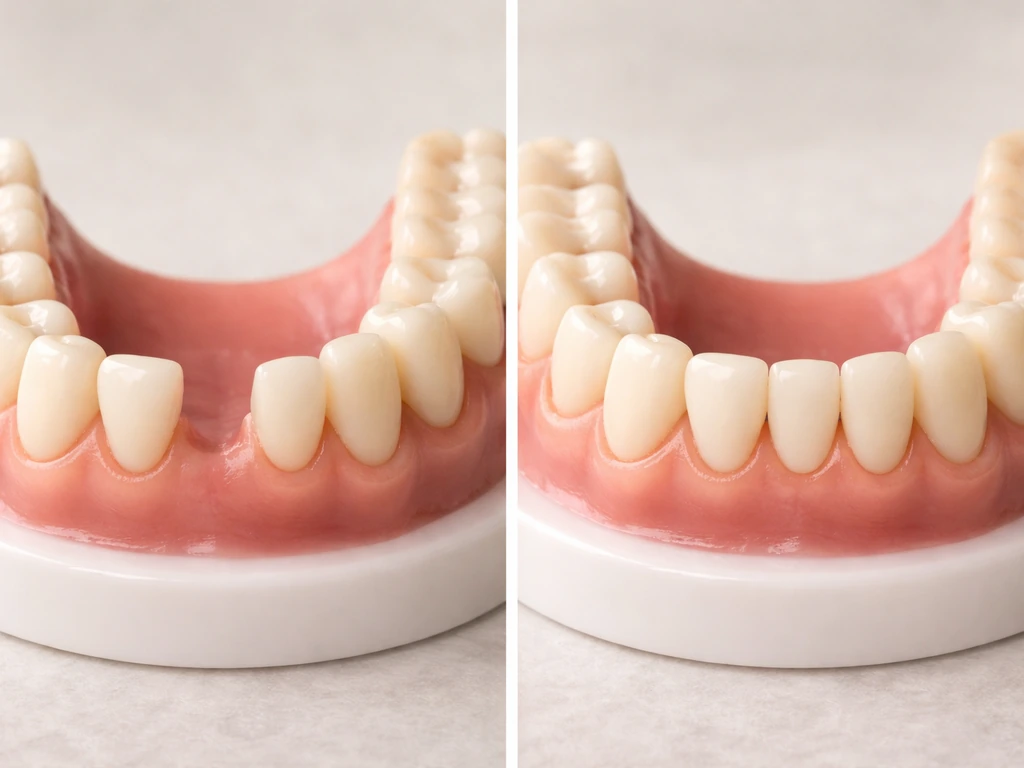
Losing a tooth isn't just a cosmetic issue, and the consequences don't wait. Within weeks of a tooth being lost, adjacent teeth begin to drift into the empty space. The tooth above or below (the opposing tooth) starts to over-erupt because there's nothing to bite against. Your bite shifts, which can put abnormal stress on the jaw joint (TMJ) and remaining teeth, causing wear, cracking, and jaw pain over time.
Underneath the gumline, the jawbone starts to resorb, meaning it shrinks and loses density because there's no tooth root stimulating it. This process begins within the first few months and continues over years. If you ever want a dental implant later, significant bone loss may mean you need a bone graft first, which adds time, cost, and complexity. Bone can grow back around teeth to some extent with the right intervention, but it won't happen on its own.
Beyond the structural issues, a missing tooth affects chewing efficiency, which influences digestion and nutrition. Speech can change depending on which tooth is missing. And for many people, missing teeth create real anxiety around smiling or social situations, which affects quality of life in ways that are hard to quantify but very real.
Common reasons teeth don't grow or won't come back
Not all 'missing tooth' situations are the same. Here are the most common scenarios and what's actually going on:
- Tooth decay and extraction: Severe cavities destroy enamel and dentin, and if infection reaches the pulp or root, the tooth often has to be removed. This is the most common cause of permanent tooth loss in adults.
- Trauma and injury: A knocked-out tooth (avulsion) is a dental emergency. The tooth genuinely cannot reattach and regrow its own, though if you act within 30 to 60 minutes, a dentist may be able to reimplant it.
- Congenitally missing teeth (hypodontia): Some people are simply born without the genetic blueprint for certain teeth, most commonly the upper lateral incisors, second premolars, or wisdom teeth. No amount of waiting will make them appear.
- Impacted or unerupted teeth: A tooth exists in the jaw but is blocked from erupting by bone, another tooth, or abnormal positioning. This is different from a missing tooth, and treatment options differ accordingly.
- Gum disease (periodontitis): Advanced gum disease destroys the bone and soft tissue supporting teeth, causing them to loosen and eventually be lost. This is the leading cause of tooth loss in adults over 35.
- Bruxism (grinding): Chronic grinding wears enamel down significantly over time. Since enamel can't regenerate, this loss is permanent. If you're wondering whether teeth grow back after grinding, they don't, but you can protect what remains.
- Age-related changes: Enamel thins naturally over decades of use. Older adults also face more gum recession, root exposure, and dry mouth, all of which increase cavity and loss risk.
Wisdom teeth and eruption timing: when 'not growing' is normal
A lot of people panic that their wisdom teeth haven't come in yet, or that something is wrong because a tooth seems to be taking forever. Wisdom teeth (third molars) are genuinely the most variable teeth in the human mouth. Most people see them begin to erupt between ages 17 and 25, but it's not unusual for them to appear as late as the early 30s, or not at all. About 20 to 25 percent of people are missing at least one wisdom tooth entirely due to genetics.
If a wisdom tooth is partially erupted, stuck at an angle, or causing pain and swelling in the gum, that's a different story. Partially erupted wisdom teeth create a pocket where bacteria accumulate, leading to a localized infection called pericoronitis. Impacted wisdom teeth can press against neighboring molars, causing pain, crowding, or even root damage to the adjacent tooth. These situations do require a dentist or oral surgeon, not watchful waiting.
For other permanent teeth in younger patients, eruption can also be delayed by overcrowding, a retained baby tooth that won't fall out, or an ectopic tooth (one growing in the wrong direction). A dentist can take an X-ray and tell you within minutes whether a tooth is present, blocked, or genuinely absent. That's always the right first step rather than guessing based on timeline alone.
What to do right now, starting today
If you're reading this because you're worried about a specific tooth, here's how to triage your situation:
- If you just had a tooth knocked out in the last hour: this is a genuine dental emergency. Keep the tooth moist (in milk or between your cheek and gum, never in water), call a dentist immediately, and get there as fast as possible. The window for reimplantation closes fast.
- If you have pain, swelling, or signs of infection (throbbing pain, fever, facial swelling): don't wait. An untreated dental abscess can spread and become serious. Call a dentist today, or go to an urgent care dental clinic or emergency room if you can't reach one.
- If a tooth has been missing for weeks or months but there's no pain: you still need to act, just not in a panic. Book a dental appointment within the next few weeks. Bone loss is already underway, and sooner is better for your options.
- If a tooth hasn't erupted and you're concerned: an X-ray (panoramic or periapical) will show whether the tooth is present, where it sits, and whether it's impacted. Ask specifically for this at your appointment.
- If you're dealing with sensitivity or enamel wear: ask about how quickly enamel is being lost and whether a nightguard, fluoride treatment, or dietary changes can slow the damage.
When you get to the dentist, come prepared with a few direct questions: Is the tooth present or permanently missing? What is causing the loss or delay? How quickly do I need to act before my options get worse? What are my replacement or treatment options and what do they cost? These questions will move the appointment beyond a general look-around into an actual plan.
Your real options: what restores teeth today (and what science is working toward)
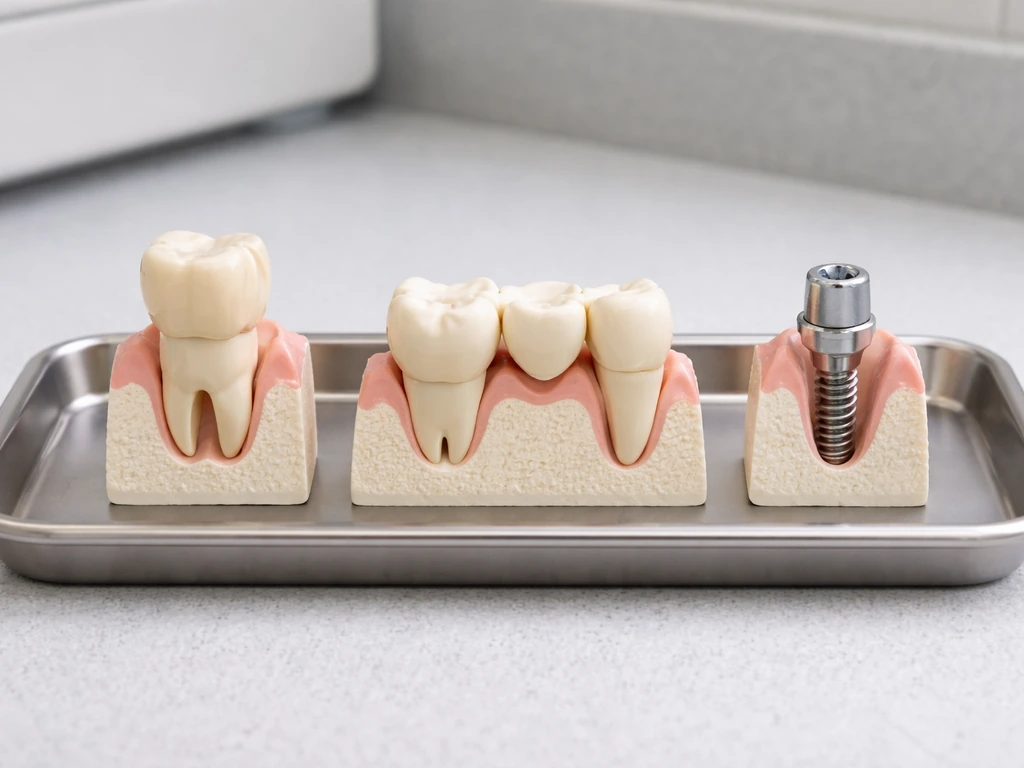
Since natural regrowth isn't on the table, the question becomes: what can dentistry actually do? The good news is that modern dentistry has multiple well-tested options that restore both function and appearance, with very different trade-offs in terms of cost, timeline, and invasiveness.
| Option | Best For | Approximate Longevity | Key Consideration |
|---|---|---|---|
| Dental implant | Single missing tooth with adequate bone | 15–25+ years (often lifetime with care) | Requires surgery and bone; highest upfront cost but best long-term outcome |
| Crown | Damaged or decayed tooth with intact root | 10–15 years | Tooth must still be saveable; protects remaining structure |
| Bridge | One or two missing teeth between healthy teeth | 10–15 years | Adjacent teeth must be filed down to anchor the bridge |
| Partial denture | Multiple missing teeth, not adjacent | 5–10 years (with adjustments) | Removable; least invasive but least stable option |
| Full denture | Full arch tooth loss | 7–10 years | Requires adjustment over time as bone resorbs |
| Orthodontics | Eruption failure or impacted teeth in younger patients | Permanent (with retainer) | Can guide impacted teeth into position in some cases |
| Bone graft | Preparation for implant after significant bone loss | Permanent support for implant | Adds 3–6 months to treatment timeline before implant placement |
For enamel that hasn't been lost entirely but is thinning or damaged, dental options include composite bonding, veneers, and fluoride-based remineralization treatments. It's worth understanding how long enamel remineralization actually takes versus what's marketing, because there are a lot of products claiming to 'restore' enamel that simply can't do what they promise.
What about tooth regeneration research?
This is worth addressing honestly because there's real science here, but it's not ready for your dentist's office yet. Researchers are working on using stem cells, growth factors, and bioengineered tooth buds to potentially grow new teeth in the jaw. Some approaches have shown promise in animal models. As of 2026, human clinical trials are still in early stages, and no commercially available treatment can grow a new tooth in a human patient. If you see a product or clinic claiming otherwise, that's a red flag. The science is genuinely exciting, but it's years away from being a practical option for most people.
For now, the most important thing you can do is not wait. Bone loss, tooth shifting, and infection don't pause while you think it over. Every month without treatment makes your options slightly narrower and slightly more expensive. The biology is fixed, but the window to act is still open, and that's exactly where your focus should go today.
FAQ
If teeth do not grow back, can enamel or “weakened enamel” regrow at all?
Enamel does not truly regenerate once it is worn through. What can happen is remineralization, which replaces lost minerals at the surface when damage is limited, but it cannot rebuild the original enamel thickness, structure, or bonds the way a new tooth layer would.
Can a tooth hole or gap fill in naturally after a permanent tooth is lost?
The empty space typically does not “grow back” into a tooth. Instead, surrounding teeth and gums can shift or change, and the underlying bone can resorb. That means the longer you wait, the harder it can be to place an implant later without additional bone grafting.
What is the difference between a tooth that “never erupted” versus one that erupted then broke?
If a tooth never erupted, the issue is usually developmental or positional (for example, impaction, retained baby tooth, or crowding), and treatment may involve orthodontics or surgical exposure. If a tooth erupted then failed, the cause is often decay, trauma, or infection, and the treatment plan can change dramatically depending on how much root and pulp are still salvageable.
Is it ever possible for a new tooth to appear in place of an extracted tooth naturally?
In typical human biology, no. The only exceptions you might hear about are mistaken diagnosis (for example, a tooth that was not actually missing) or rare developmental anomalies. If something new “appears,” an X-ray is needed to confirm whether it is a different tooth, bone remodeling, or a misread earlier imaging.
What should I do immediately after a permanent tooth is knocked out?
Time matters. If the tooth is truly knocked out, keep it moist (for example, in milk or saline) and seek emergency dental care right away. Reimplantation or other urgent options are time-sensitive and depend on root condition and storage time.
How does a delayed eruption get evaluated, and how quickly should I act?
A dentist typically starts with bitewing or panoramic X-rays, sometimes a cone-beam scan, to check whether the tooth exists, is impacted, or is blocked by another tooth. If you are missing or delayed by more than expected for your age, ask specifically whether it is present but impacted, because that changes urgency and treatment options.
If my wisdom tooth isn’t fully through, when is it safe to watch and wait?
Watchful waiting is usually only reasonable when there is no significant pain, swelling, fever, or recurring infection. If it is partially erupted and you get repeated gum inflammation or foul taste, that often signals bacterial pocketing (pericoronitis) and you should be evaluated promptly.
Can root canal treatment “save” a tooth so it feels natural afterward?
Root canal therapy replaces the removed pulp and cleans and seals the canal system, so the tooth can remain functional. It does not regrow nerves or pulp, so sensation may be altered, and many patients still need a crown or strong restoration to prevent fracture of a weakened tooth structure.
Do supplements help teeth grow back once enamel or dentin is lost?
Most supplements cannot trigger enamel regeneration. If you have mineral loss, dentists can recommend targeted remineralization strategies and fluoride use, but they cannot rebuild lost enamel surfaces to the original state once fully destroyed.
How long should I wait before considering replacement options like implants or bridges?
There is no single timeline for everyone, but waiting months to years can increase bone loss and tooth shifting. A practical next step is to ask what replacement is feasible now, what you might need later if bone volume decreases, and how long bone remodeling or grafting would take in your specific case.
Why does missing a tooth affect the jaw joint and other teeth?
When a tooth is missing, bite forces redistribute, the opposing tooth can over-erupt, and adjacent teeth can drift toward the empty space. Over time this can change occlusion and increase stress on the TMJ and remaining teeth, leading to wear or pain in some people.
Learn if enamel can regrow, why it cannot, and how fluoride and remineralization can repair early damage.
Learn what helps receding gums, real vs possible regrowth, causes, step-by-step care, and when to see a periodontist.
Know if a permanent tooth regrows after it falls out, why it usually won’t, and what to do immediately and next.

