What a cyst actually is and which types can hold tooth or hair tissue
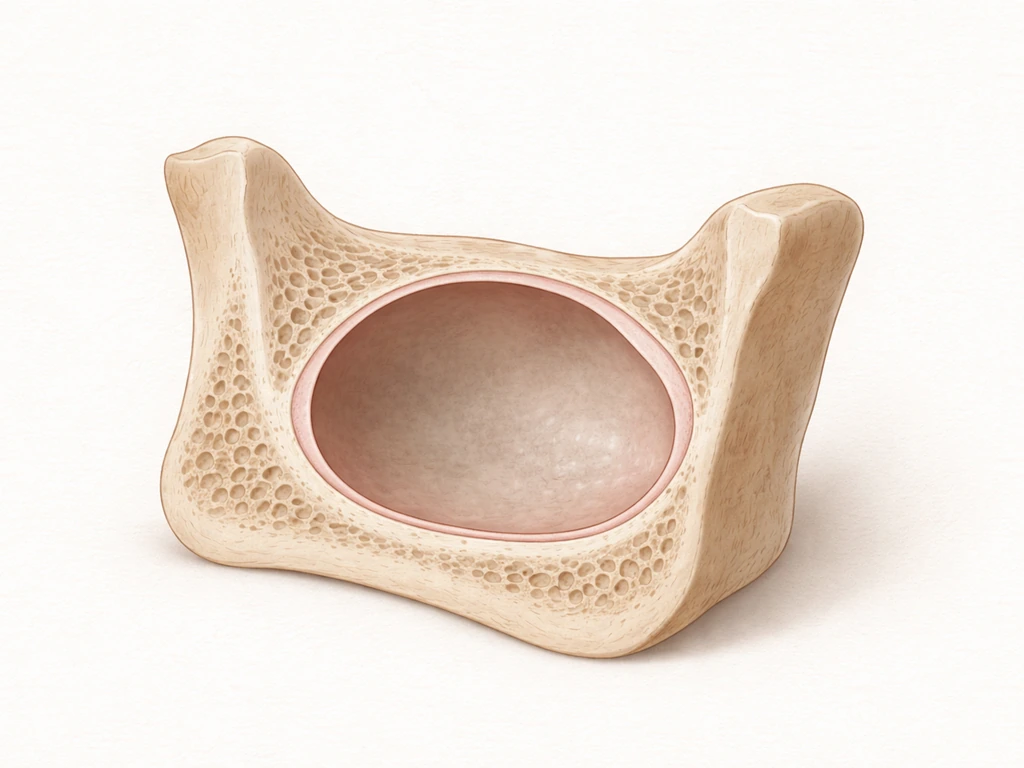
A cyst is a closed sac made of connective tissue lined on the inside by epithelium (a layer of cells), and it contains fluid, gas, or semi-solid material. Think of it like a biological bubble with walls. That epithelial lining is actually the key detail here, because the type of epithelium and how the cyst originally formed determines what can end up inside it.
In the jaws and oral cavity specifically, most cysts are odontogenic, meaning they arise from the epithelial remnants of tooth development. These are incredibly common. The mandible and maxilla (your lower and upper jawbones) are the only bones in the body that carry leftover odontogenic epithelium from when your teeth formed, which is exactly why jaw cysts show up so much more often than cysts in other bones. Odontogenic cysts form closed sacs that can contain air, fluid, or soft debris, and they can push on tooth roots, displace teeth, or expand the jawbone over time. But they don't grow new teeth inside them.
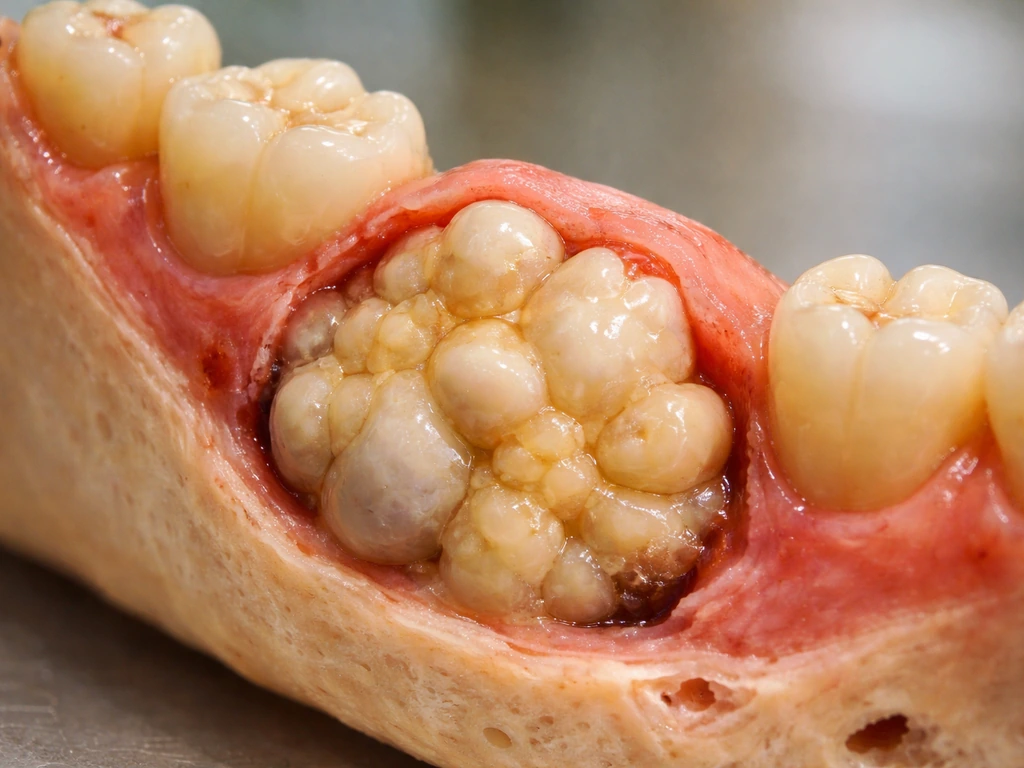
The cysts that actually can contain teeth and hair are dermoid cysts. According to the NCI definition, a dermoid cyst is a benign cyst filled with tissues normally found in the outer skin layers, and it may contain elements of hair and teeth. The Cleveland Clinic adds that these cysts may even contain nerves. They form when skin cells, tissues, and glands get trapped inside a pocket during early fetal development. So the "teeth" and "hair" inside a dermoid cyst aren't growing from scratch inside the cyst later in life. They were essentially folded in during embryonic development and have been sitting there since before you were born. A teratoid cyst is a rare variant that takes this even further, potentially containing derivatives from all three embryonic germ layers (ectoderm, mesoderm, and endoderm), making it the most complex of this category. If you're curious about why teratomas grow teeth, the developmental biology behind that is closely related to what drives dermoid and teratoid cysts to contain these same structures.
| Cyst Type | Where It Forms | Can It Contain Teeth? | Can It Contain Hair? | How Common in the Mouth/Jaw? |
|---|
| Odontogenic cyst (e.g., radicular, dentigerous, keratocyst) | Jaws and oral cavity | No (may be associated with a tooth, not contain one) | No | Very common |
| Dermoid cyst | Floor of mouth, face, ovaries, skin | Yes (tooth-like structures possible) | Yes (hair follicles, sebaceous glands) | Uncommon in oral cavity |
| Teratoid cyst | Head/neck, oral cavity | Yes (complex tissues from all germ layers) | Yes | Rare |
| Epidermoid cyst | Skin, occasionally oral soft tissue | No | No | Uncommon in oral cavity |
| Nasopalatine duct cyst | Anterior hard palate | No | No | Relatively common |
Why most cysts don't grow teeth: the real limits of dental regeneration
Here's where we need to separate two very different questions: can a cyst contain tooth-like tissue (yes, in rare cases), and can a cyst grow new teeth the way your body grows teeth during development (no, not really). These sound similar but they're biologically very different things.
Human teeth form through a tightly controlled developmental process that requires specific signaling between two tissue types: the oral epithelium and the underlying mesenchyme. This process happens during embryonic and early childhood development and doesn't restart in adults. Once your second set of teeth is done forming, the biological machinery for tooth development largely shuts down. There are no tooth buds left sitting around in your jaw waiting to be activated by a cyst. This is also why whether stem cells can grow teeth is such an active area of research right now: scientists are trying to figure out how to switch that developmental program back on, because the body simply doesn't do it on its own.
The tooth-like structures found in dermoid cysts aren't the result of a cyst "growing" teeth. They're developmental remnants that got trapped during fetal growth. It's a completely different mechanism from tooth regeneration, enamel repair, or anything related to how new teeth normally form. So if you read somewhere that a cyst can grow teeth and hair inside your body, the accurate version of that statement is: certain cysts can contain developmental tissue that was already there from early fetal life, including structures resembling teeth and hair follicles. That's fascinating, but it's not regeneration.
Signs that make people think something unusual is happening
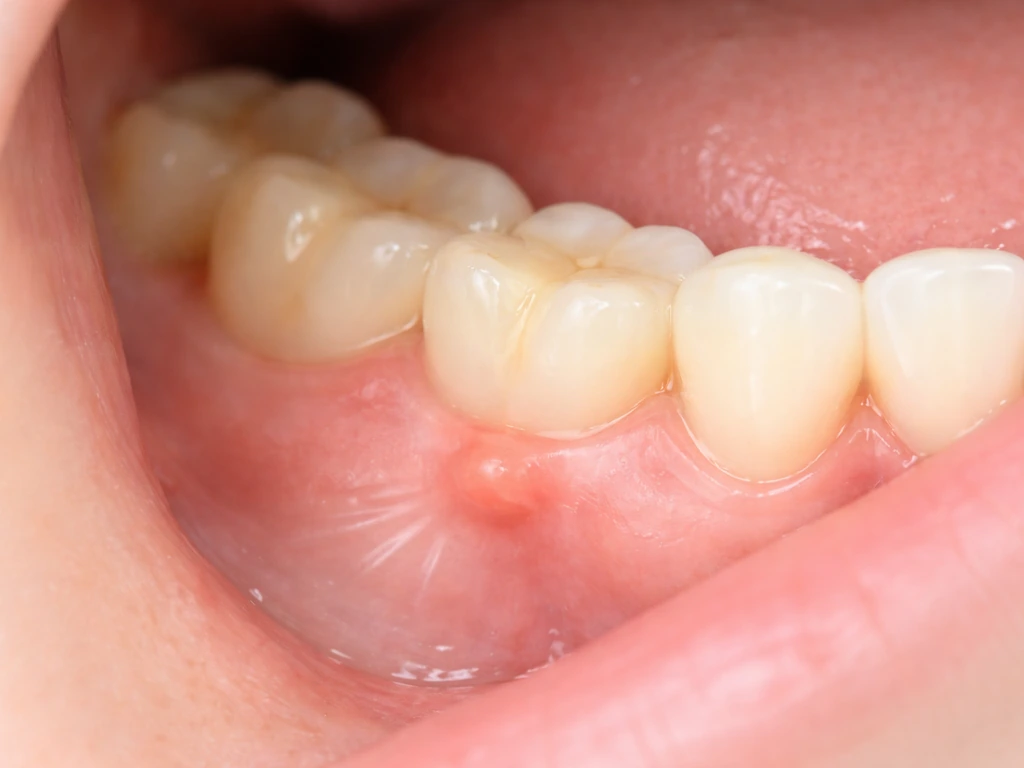
Most people searching this question aren't doing it out of idle curiosity. They've noticed something. Here are the most common real-world situations that send people down this search path, and what those signs actually tend to mean.
- A hard lump in the jaw or along the gumline that doesn't go away: This is often an odontogenic cyst, a bony overgrowth like a torus, an impacted tooth, or a benign tumor. It's not growing teeth, but it does need evaluation. People sometimes wonder if mandibular tori can grow larger over time, and the answer is that they can, slowly, which makes monitoring important.
- A soft, doughy swelling in the floor of the mouth or under the chin: This is a classic presentation location for oral dermoid cysts, which are the type that can contain hair follicles and skin glands. These are uncommon, but they do occur.
- A wisdom tooth that seems to be erupting very late or in an unusual position: Sometimes what feels like "something new growing" is a third molar finally pushing through. This is tooth movement, not a cyst forming teeth.
- An X-ray showing a dark shadow around a tooth root: This is typically a periapical cyst (radicular cyst) that formed from chronic infection. It contains inflammatory fluid and dead tissue, not ectopic structures.
- A pea-sized bump on the skin near the eye, scalp, or face: Skin-surface dermoid cysts are among the most common benign cysts of the face. They rarely contain visible teeth but can contain hair and oily material.
The important thing to understand is that none of these situations means your body is spontaneously generating new teeth inside a cyst. Even in the rare case of an oral dermoid cyst, any tooth-like material inside it has been there since development. The cyst itself may just now be making itself known because it's grown large enough to feel or see.
How doctors and dentists actually diagnose these cysts
If you show up at a dentist's office with a jaw lump or swelling and you're worried it might be a cyst, here's roughly what the diagnostic process looks like in 2026.
- Clinical exam: The dentist will palpate (press on) the area to assess size, firmness, tenderness, and whether it moves. They'll also look at your gums, check for any sinus tracts (small pimple-like openings that drain fluid), and assess the health of nearby teeth.
- Dental X-rays (periapical and panoramic): These are almost always the first imaging step for jaw cysts. Odontogenic cysts appear as radiolucent (dark) areas on X-ray. The size, shape, borders, and relationship to tooth roots or the nerve canal all give important diagnostic clues.
- CBCT (cone beam computed tomography): For larger or more complex lesions, a 3D CBCT scan gives a much clearer picture of how far the cyst extends, whether it's eroded bone, and what structures are nearby. This is increasingly standard for jaw cysts in oral surgery workups.
- MRI or CT (for soft tissue cysts): If the suspected cyst is in the floor of the mouth, neck, or involves soft tissue rather than bone, an MRI or conventional CT scan is more useful than a dental X-ray. Dermoid cysts often have a characteristic appearance on MRI that helps distinguish them from other soft tissue masses.
- Aspiration: Sometimes the clinician will use a needle to draw out a small sample of the cyst's contents. The character of the fluid (clear, straw-colored, cheesy, or bloody) gives a clue to the type of cyst.
- Biopsy and histopathology: The definitive diagnosis for any cyst comes from examining the tissue under a microscope after it's been removed or sampled. This is how pathologists confirm whether the cyst lining is dermoid (keratinizing squamous epithelium with skin appendages like sebaceous glands and hair follicles) versus odontogenic or something else entirely.
It's worth noting that not every cyst needs a biopsy immediately. Your dentist or oral surgeon will use the clinical and imaging findings to decide how urgently to act. Some small, asymptomatic cysts are monitored with periodic X-rays if they show no growth or worrying features. Others warrant prompt excision.
Red flags and what to do before your appointment
Most cysts are benign and slow-moving, but some need faster attention. Here's how to triage your own situation before you can get in to see someone.
Seek prompt evaluation (within days, not weeks) if you notice any of the following: rapid increase in swelling over a few days, pain that's getting significantly worse, difficulty swallowing or breathing, numbness or tingling in your lip or chin (which can indicate nerve involvement), a draining sore in the mouth that won't heal, or fever alongside facial swelling. These signs don't automatically mean something is seriously wrong, but they do mean you shouldn't wait for a routine appointment.
For most people, the situation is less urgent: a lump that's been there for a while, a vague soreness near a tooth, or something spotted on a routine X-ray. In those cases, call your dentist to get it on the schedule within a few weeks. Do not try to pop, drain, or squeeze any oral cyst yourself. The oral cavity is a bacteria-rich environment, and introducing an infection into a cyst cavity is a real and painful risk. There's also the issue that some things that look like cysts are not (benign fibroma, salivary gland issues, bony abnormalities), so you need someone who can actually look and image the area.
Questions worth asking at your appointment: Is this an odontogenic cyst, and which type? Does it need to come out now or can we watch it? Is the associated tooth salvageable? Will I need a referral to an oral surgeon? Do we need a 3D scan? What are the chances this is something other than a cyst?
Treatment options: from watchful waiting to surgery
The right treatment depends entirely on the cyst type, size, location, and what it's doing to surrounding structures. Here's a practical overview.
Observation
Small, incidentally discovered cysts with clear, benign imaging features and no symptoms are sometimes managed with observation alone. This means periodic X-rays (typically every 6 to 12 months) to confirm the cyst isn't growing. This approach is more common for very small periapical lesions after successful root canal treatment, where the body may resolve the lesion on its own over time.
Enucleation and curettage
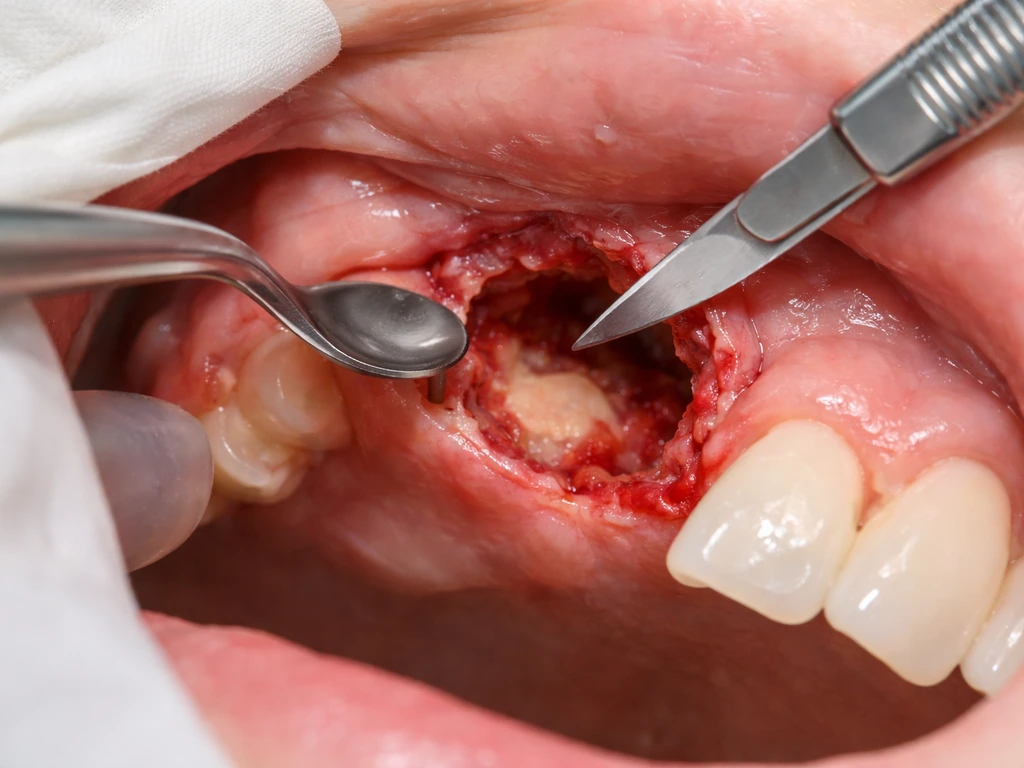
This is the most common surgical approach for odontogenic cysts. The surgeon removes the entire cyst lining (enucleation) and scrapes the bony cavity clean (curettage). The removed tissue goes to pathology for confirmation of the diagnosis. Most patients recover well, though healing of the bone cavity can take several months. Smaller cysts often heal without the need for bone grafting; larger ones may require it.
Marsupialization (decompression)
For very large cysts, especially in the mandible where complete removal might risk fracturing the jaw or damaging the inferior alveolar nerve, surgeons sometimes use marsupialization first. This involves surgically opening the cyst and creating a permanent opening so it drains and decompresses over months, shrinking before final removal. It's a staged approach that reduces risk.
Excision of dermoid and teratoid cysts
Oral dermoid cysts are treated by complete surgical excision. Because they contain skin gland components and hair follicles, they tend to recur if the lining isn't fully removed. The surgical approach depends on location: floor-of-mouth dermoids may be removed through an intraoral approach or, for deeper lesions, through an external incision under the chin. Outcomes are generally excellent when the cyst is completely excised. Whether ovaries can grow teeth involves the same cyst type (dermoid/teratoma), just in a different body location, and surgical excision is similarly the standard treatment there.
What about the tooth associated with the cyst?
Many odontogenic cysts are associated with a specific tooth, often a non-vital (dead) tooth with a chronic infection at its root, or an impacted tooth surrounded by a dentigerous cyst. In these cases, the treatment plan has to address both the cyst and the tooth. Sometimes the tooth can be saved with root canal treatment and the cyst resolves or is removed alongside. Other times, extraction is necessary, especially if the tooth is impacted, has no functional value, or the cyst has compromised too much of the root. Your oral surgeon or endodontist will make this call based on imaging and the specific situation.
The bigger picture: cysts vs. tumors vs. true tooth growth
It's easy to blur the lines between these things when you're worried and reading online. A cyst is not a tumor, though some benign tumors can behave similarly or appear in the same jaw regions. The question of whether tumors can grow teeth overlaps with the dermoid/teratoma biology we've discussed, because odontomas (benign odontogenic tumors) can contain enamel, dentin, and tooth-like structures. These are distinct from cysts but worth knowing about, since they're another reason a jaw X-ray might reveal something that looks unexpectedly tooth-like.
None of this is the same as actual tooth regeneration, which would mean your body producing a new functional tooth from scratch. Human adults cannot do that. Children can only do it once (replacing baby teeth with permanent ones), and that process is complete by the late teens for most people, with wisdom teeth sometimes finishing into the early twenties. If you've ever wondered about the science behind why we can't just grow more, the biology of dental stem cells and what researchers are working on to change that is genuinely fascinating, even if it's not clinically available yet.
The bottom line: if you have a lump, bump, or swelling in your mouth or jaw, get it looked at. Most of these turn out to be benign and very manageable. The rare case of a dermoid cyst containing hair or tooth-like material is surgically treatable with excellent outcomes. What matters most is not guessing at the diagnosis based on what something looks or feels like, but getting proper imaging and a clinical evaluation so you know exactly what you're dealing with.