Here's the short answer: human teeth do not grow back once they're gone. Enamel cannot regenerate on its own. Gums that have receded don't spontaneously regrow. And no home remedy, oil pulling routine, or supplement changes any of that. What CAN happen, and what this guide covers in detail, is a nuanced picture of eruption (teeth moving into position), tissue remodeling, limited biological repair, and the modern dental treatments that can genuinely replace what nature won't rebuild. Whether you're a parent watching your child lose baby teeth, an adult dealing with a cavity or receding gums, or someone wondering why a wisdom tooth is taking forever to come in, this guide gives you straight answers based on actual dental biology.
Good to Grow Dental: What Can Grow Back and What Can’t
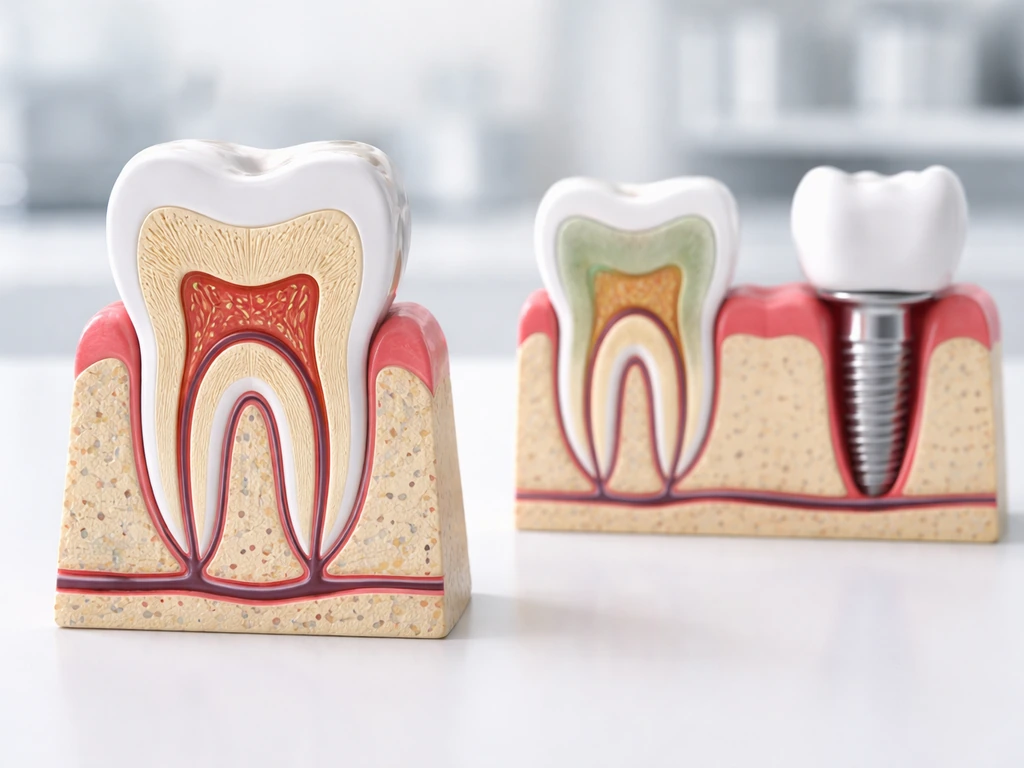
What "growing dental" really means: regrow vs erupt vs remodel
People use the phrase "grow back" loosely, but in dentistry it covers three completely different things. It's worth separating them clearly before anything else.
- Eruption: A tooth that already exists moves through the jaw and breaks through the gum line. This is what's happening when a kid's adult teeth come in, or when a wisdom tooth appears in your late teens. The tooth was always there, developing inside the bone. It didn't "grow back" from nothing.
- Remodeling: The jaw bone and surrounding tissues adjust and shift in response to forces, age, or treatment. This is real but limited. Bone can lay down new mineral around implants, for example. Pulp tissue can form a thin layer of secondary or tertiary dentin in response to mild irritation. These are genuine biological events, but they are not the same as regrowing a lost tooth.
- Regeneration: True regrowth of lost tissue from scratch. This is what most people wish for and what most "natural remedy" claims promise. In the strict biological sense, human adults cannot regenerate tooth enamel, cannot regrow a lost tooth, and cannot fully restore lost periodontal attachment without clinical intervention.
The field of regenerative endodontics, as defined by the American Association of Endodontists, is developing biologically based procedures intended to replace damaged dentin-pulp complex structures, but this is a highly specialized clinical discipline, not something that happens naturally at home. Knowing which of the three processes you're actually asking about is step one, because the answer and your next steps depend entirely on it.
What can actually regrow in humans, and what can't
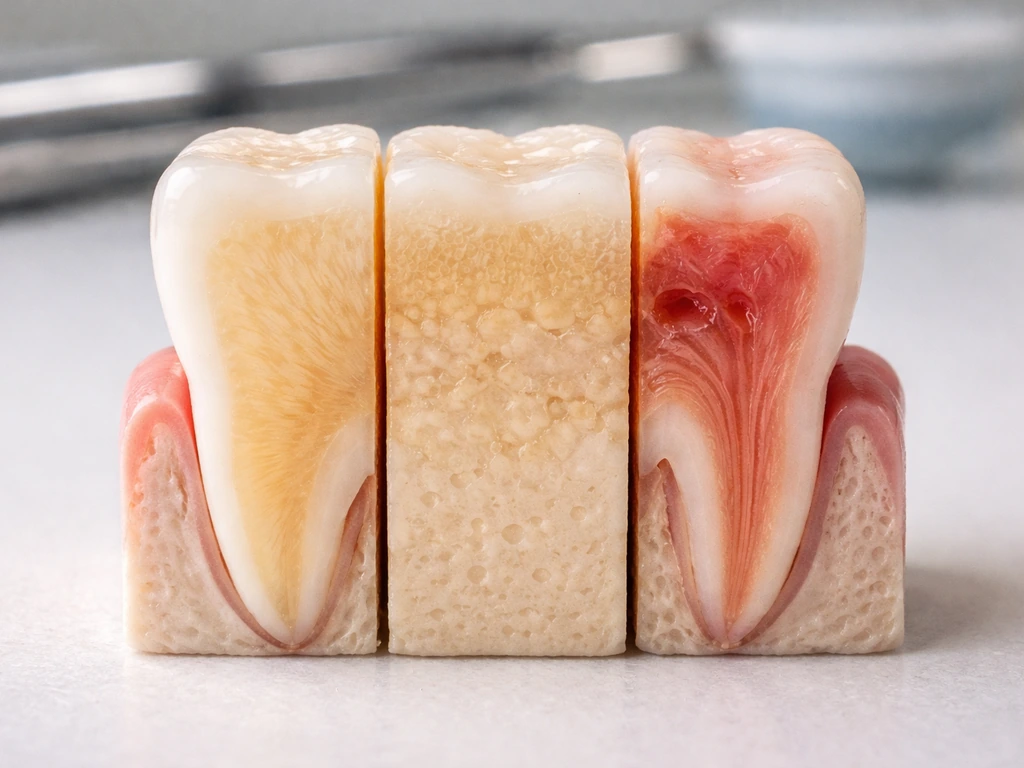
Let's go tissue by tissue, because they are not all the same.
Enamel
Enamel is the hardest substance in the human body, and once the cells that produce it (ameloblasts) are gone after a tooth finishes developing, they're gone for good. There are no replacement cells waiting to rebuild enamel after acid erosion, grinding, or decay. Fluoride can remineralize early-stage lesions (small, not yet cavitated areas where minerals have leached out) but this is mineral redeposition into existing enamel structure, not the formation of new enamel tissue. Once a cavity has broken through the enamel surface, no amount of fluoride or remineralization will close it. That requires a dentist.
Dentin
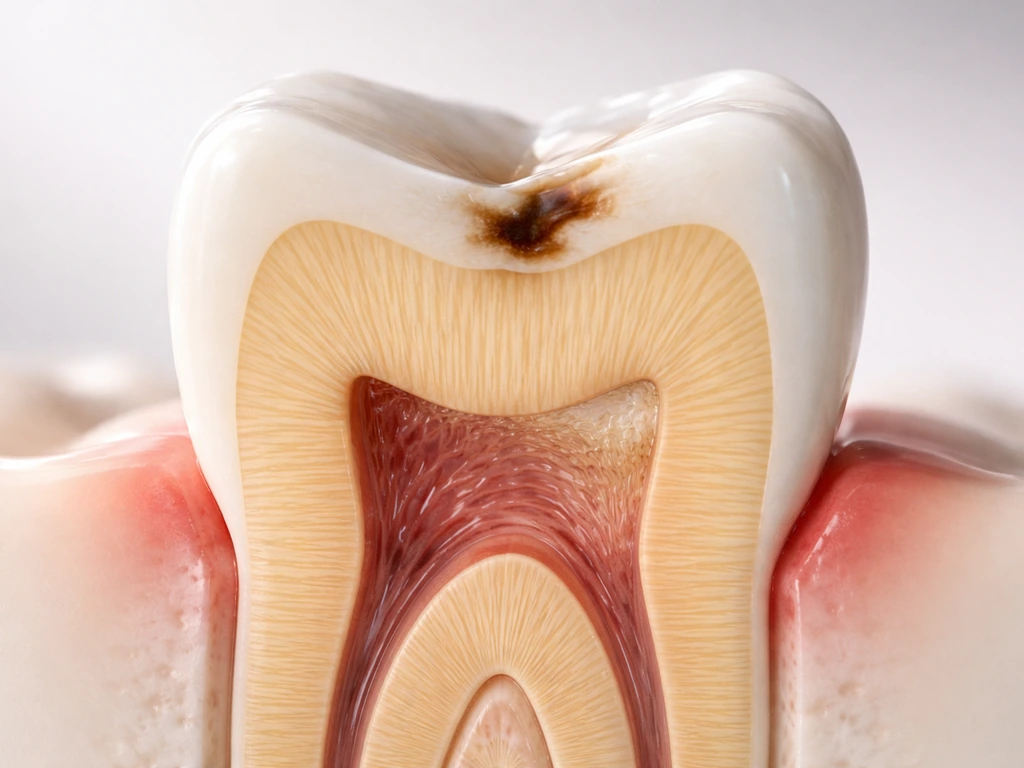
Unlike enamel, dentin does have some capacity for limited repair. When a tooth experiences mild irritation (early decay, a shallow cavity preparation, light grinding), the pulp can deposit reparative or tertiary dentin as a defensive layer. The American Academy of Pediatric Dentistry's guidelines on vital pulp therapy describe this as one of the treatment goals: preserving pulp vitality and promoting tertiary dentin formation to protect the pulp. But this is a thin, defensive response to mild insult, not a restoration of lost tooth structure. Deep decay that has destroyed significant dentin does not get repaired this way.
Pulp
The pulp (the soft tissue at the center of the tooth containing nerves and blood vessels) has some regenerative potential in young, developing teeth with open root tips (immature apexes). This is the specific focus of regenerative endodontic procedures. In mature, fully developed teeth with closed apexes, the capacity for meaningful pulp regeneration is far more limited, and the standard treatment for a severely infected or necrotic pulp remains root canal therapy followed by restoration.
Gums and periodontal bone
Gum tissue that has receded due to aggressive brushing, gum disease, or aging does not grow back on its own. The attachment between gum, periodontal ligament, and bone is a specialized structure, and once that attachment is lost to periodontitis, it does not regenerate spontaneously. The ADA notes that when significant bone destruction is present, surgical regenerative procedures can be used clinically, but this requires a periodontist working with grafting materials and membranes. It is not a natural process, and no mouthwash reverses true periodontal bone loss.
Whole teeth
Adults get one set of permanent teeth. Lose one to decay, injury, or extraction, and nothing biological replaces it. There are researchers investigating tooth regeneration in animal models and even early-stage human trials (particularly around gene pathways that control tooth bud development), but as of 2026, no such treatment is clinically available. If you've seen social media posts claiming otherwise, those are not based on approved, available therapy.
Age-based expectations: kids, adults, and older adults
Age matters enormously in this conversation. What's normal and expected at 7 is a crisis at 40.
Children (roughly ages 5 to 12)
Kids have two sets of teeth: 20 primary (baby) teeth and 32 permanent teeth developing beneath them. When a baby tooth falls out, the permanent tooth beneath it erupts into position. This is the closest thing to "growing back" that humans experience, and it's not regrowth at all: it's a second set that was always there. Parents sometimes panic when a permanent tooth looks different from the baby tooth it replaced (it's more yellow, larger, more ridged). That's completely normal. If a baby tooth is lost too early due to decay or injury, a space maintainer may be needed to prevent crowding for the permanent tooth that's coming. pediatric dental care for growing kids is especially important in this window because what you protect now determines the permanent-tooth environment the child carries for life.
Adolescents and young adults (roughly ages 12 to 25)
By the early teens, most permanent teeth are in place. The major eruption event still on the horizon is wisdom teeth. Root development in some teeth is still completing through the mid-teens. Pulp chambers are larger in young teeth, which is why young patients often experience more sensitivity and why regenerative endodontic approaches are more viable in this age group. Cavity prevention through sealants is particularly evidence-supported here: the American Academy of Pediatric Dentistry specifically identifies pit and fissure sealants as a strategy to prevent occlusal caries in permanent molars, noting that these approaches prevent or delay lesion progression rather than regenerating any structure that's already been lost.
Adults (roughly ages 25 to 60)
For most adults, the biological "growth" window is closed. Pulp chambers have narrowed, root apexes are fully closed, and the body's capacity for dental tissue repair is at its lowest. Enamel erosion from years of acidic food and drink, grinding, or gum recession becomes more prominent. The focus here shifts entirely to protecting what remains and replacing what's lost. Any social media content telling adults their enamel or receded gums can grow back naturally is folklore, not science.
Older adults (60 and beyond)
Root exposure increases with gum recession, which is more common with age. Dry mouth (often medication-related) raises cavity risk dramatically because saliva is a key natural buffer against acid and bacterial plaque. Bone density changes can affect how implants integrate. The restorative goals in this group lean toward preserving existing teeth as long as possible and using implants, bridges, or dentures when teeth are lost. If you're managing dental care for an older parent or yourself, connecting with a practice that understands age-related factors (similar to specialized pediatric and family dental practices focused on lifelong oral growth) makes a real difference in outcomes.
Wisdom teeth: the eruption timeline and what to expect
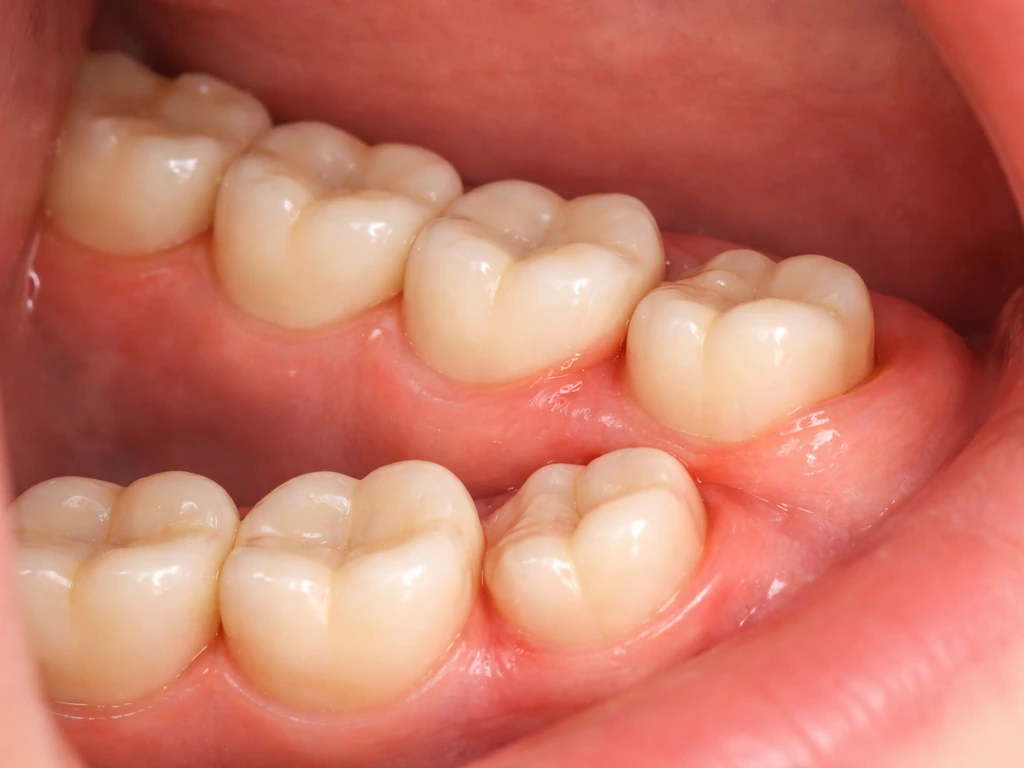
Wisdom teeth (third molars) are the last permanent teeth to erupt, and they are the one significant "growing" dental event most adults experience. According to a Cochrane systematic review, third molars generally erupt between ages 17 and 24. Some erupt fully and function normally. Others partially erupt and get stuck (impacted), either because there isn't enough space in the jaw or because they're angled incorrectly.
What you can expect during this window: mild pressure or discomfort in the back of the jaw, occasional swelling of the gum flap over a partially erupted tooth (called pericoronitis), and sometimes referred pain to the ear or adjacent teeth. What you should not expect: that a wisdom tooth appearing in your 20s means you're "getting a new tooth" in any significant sense. These teeth were already developing in your jaw. They're just finally moving into (or failing to move into) position.
Impacted wisdom teeth that cause pain, crowd nearby teeth, trap food, or develop cysts typically require extraction. Asymptomatic impacted wisdom teeth are sometimes monitored rather than immediately removed, but the decision depends on their position, your age, and your dental history. If you're past 30 and a wisdom tooth hasn't fully erupted yet, it's unlikely to do so and more likely to create problems over time.
When teeth and gums are damaged: understanding your specific situation
Not all damage is the same, and the options differ significantly depending on the cause and extent. Here's a quick breakdown by situation:
| Type of Damage | Can it regrow naturally? | What's realistic |
|---|---|---|
| Early enamel lesion (no cavity yet) | Partial remineralization possible with fluoride | Fluoride treatment, dietary changes, monitoring |
| Cavitated cavity (hole in tooth) | No | Filling or restoration required |
| Cracked or chipped tooth | No | Bonding, crown, or veneer depending on severity |
| Tooth knocked out (avulsion) | No (adult tooth) | Reimplantation within 30-60 minutes if possible; otherwise implant or bridge |
| Gum recession | No (spontaneous regrowth) | Soft tissue graft (surgical), improved oral hygiene to slow progression |
| Periodontal bone loss | Not spontaneously | Scaling/root planing, possibly surgical regenerative procedures |
| Tooth loss (extracted or fallen out) | No | Implant, bridge, or partial denture |
| Infected pulp in young tooth (open apex) | Possible with regenerative endodontic procedure | Specialist referral for regenerative endodontic treatment |
| Infected pulp in adult tooth (closed apex) | No | Root canal therapy and crown |
One thing many patients get wrong about decay specifically: a cavity doesn't stop on its own. The bacterial process that causes decay is ongoing, and without treatment, a small cavity progresses into the dentin, then the pulp, potentially causing an abscess. The ADA's restorative caries guidelines make it clear that once structural loss occurs from caries, the replacement comes from restorative materials, not from any biological repair mechanism.
Evidence-based options that replace what won't regrow
Because so much of dental tissue cannot regenerate, modern dentistry has developed reliable ways to replace or restore lost structure. Here's what the evidence actually supports:
Fillings and direct restorations
Composite resin (tooth-colored) and amalgam fillings are used to restore cavities after decay is removed. They don't replicate the original enamel or dentin biologically, but they restore function and seal the tooth from further bacterial invasion. Composite materials have improved significantly and can be matched to tooth color with excellent durability.
Crowns and veneers
When a tooth has lost significant structure (from a large cavity, fracture, or root canal treatment), a crown caps the remaining tooth structure and protects it. Veneers are thin porcelain or composite shells bonded to the front surfaces of teeth, most often used for cosmetic correction of chipped, discolored, or slightly misaligned teeth. Neither is "regrowth," but both are highly effective replacements.
Implants and bridges
A dental implant is a titanium post placed into the jaw bone that acts as a tooth root, topped with a crown. It is the closest modern dentistry gets to replacing a full tooth, and it performs extremely well in terms of bone preservation and function. A bridge fills the gap from a missing tooth by anchoring to adjacent teeth. Neither grows back your tooth, but implants in particular prevent the bone resorption that accelerates when a tooth is missing.
Periodontal and bone regeneration procedures
Scaling and root planing (deep cleaning) is the first-line treatment for gum disease. When bone loss is significant, a periodontist may perform grafting procedures using bone graft material and membrane barriers to encourage bone regeneration around affected roots. Soft tissue grafts can cover exposed roots from recession and reduce sensitivity, though they do not fully restore the original gum architecture. If you're exploring what comprehensive dental care looks like across these levels, a full-service dental center that offers both general and periodontal treatment under one roof can simplify the process considerably.
Remineralization therapies
Prescription-strength fluoride (5000 ppm), silver diamine fluoride (SDF), and casein phosphopeptide-amorphous calcium phosphate (CPP-ACP) products are used to halt or slow early enamel lesion progression. These work best on white spot lesions (early demineralization) before a cavity has physically formed. They are evidence-supported preventive tools, not treatments for established cavities.
A quick comparison: which restoration fits your situation?
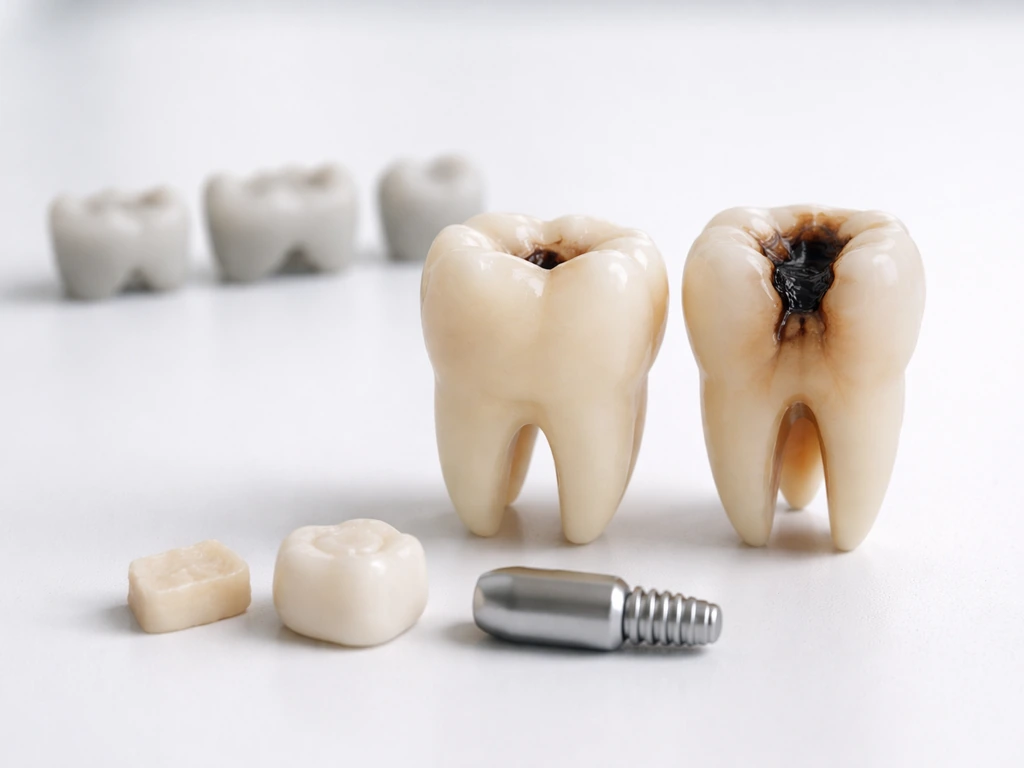
| Situation | Best-evidence option | Considerations |
|---|---|---|
| Small to medium cavity, one surface | Composite or amalgam filling | Durable, preserves tooth structure, fast |
| Large cavity or cracked tooth | Crown | Protects remaining structure; may need root canal first if pulp is involved |
| Minor chip or cosmetic issue | Bonding or veneer | Veneer is more durable; bonding is faster and less invasive |
| Single missing tooth with healthy adjacent teeth | Implant (preferred) | Preserves bone; doesn't involve adjacent teeth |
| Missing tooth, adjacent teeth need crowns anyway | Bridge | Faster than implant; removes tooth structure from adjacent teeth |
| Multiple missing teeth | Implant-supported bridge or partial denture | Depends on bone volume and budget |
| Gum recession with root exposure | Soft tissue graft | Reduces sensitivity and further recession risk |
| Moderate gum disease (no bone loss) | Scaling and root planing | Highly effective when followed with maintenance |
| Significant periodontal bone loss | Surgical regenerative procedure | Requires periodontist; results depend on defect type |
Prevention and when to get help: your next steps
The most useful thing you can do after reading this is decide which category your situation falls into and act accordingly. Here are concrete next steps:
- If you have tooth pain, sensitivity to hot or cold that lingers, a visible hole or chip, or bleeding gums that don't resolve: see a dentist within the week. These are not watch-and-wait situations. Delay turns small problems into large (and expensive) ones.
- If you have noticed gum recession or pockets around your teeth: ask your dentist for a periodontal evaluation specifically, not just a standard cleaning. The treatment path differs significantly from general dental care.
- If your child has a loose baby tooth that's been hanging for more than a few weeks or an adult tooth growing in before the baby tooth has fallen: get a pediatric dental evaluation. Retained baby teeth can push permanent teeth into poor positions.
- If you're in the wisdom tooth eruption window (17 to 24): ask your dentist to take a panoramic X-ray to evaluate the angle and position of third molars. This determines whether to monitor or act.
- For prevention, the basics genuinely work: brush twice daily with fluoride toothpaste, floss once daily, limit acidic and sugary drinks (especially between meals), wear a night guard if you grind, and attend cleanings at least twice a year. For practices focused on building lasting oral health, understanding how a strong dental practice grows through patient education and prevention helps you identify providers who prioritize long-term outcomes over quick fixes.
- If you're uninsured or cost-sensitive: ask about dental membership plans. Many practices offer in-house plans that cover preventive care at a flat annual rate. Understanding how dental membership plans work and grow can help you find affordable coverage that keeps preventive visits accessible year-round.
The bottom line is this: teeth are not like skin or bone in terms of their regenerative capacity. They are more limited, and the myths that suggest otherwise (oil pulling restoring enamel, special toothpastes regrowing lost gum tissue, supplements rebuilding missing teeth) have no clinical evidence behind them. What does work is catching problems early, restoring what's been lost before it cascades further, and consistently maintaining the teeth and gum tissue you have. The biology sets the limits; good dentistry and smart prevention define what's possible within them.
FAQ
If my enamel is worn down, can fluoride or remineralizing toothpaste rebuild it?
Usually no. Fluoride can help strengthen early, mineral-depleted areas (white spot lesions), but it does not create new enamel tissue once enamel is genuinely missing or eroded. For significant wear, dentists more often address it with bonding, sealants, crowns, or bite adjustments to stop further loss (for example from grinding).
My gum line looks lower. Does deep cleaning or “natural” treatment make my gums grow back?
Non-surgical cleaning can reduce inflammation and improve gum health, but recession itself typically does not spontaneously reverse. If root coverage is desired, soft tissue graft procedures are the usual option, and outcomes depend on how much keratinized tissue remains, the thickness of existing gum tissue, and the cause (periodontitis vs trauma from brushing).
Can regenerative endodontics work for adults the way it can for children?
It may be limited. Regenerative endodontics is most predictable in young teeth with immature roots because the pulp environment is still capable of continued development. In adults with closed apexes and established mature anatomy, the standard approach for a necrotic pulp is root canal treatment and restoration, because true pulp “regrowth” is much less reliable.
If a tooth has a “starting” cavity, what should I do to prevent it from turning into a filling?
Act on it early with an in-person exam, because “starting” can mean different lesion types. Clinically, the best next step is often fluoride at the correct strength (sometimes prescription fluoride) and a dietary and plaque control plan, but once a lesion has cavitated (roughness or an opening), it generally needs restorative treatment to remove the decay and seal the tooth.
How do I know whether my wisdom tooth is just erupting normally or becoming a problem?
Normal eruption is usually mild discomfort without recurrent swelling. Concerning signs include repeated flare-ups around the gum flap (pericoronitis), persistent pain, trapped food with bad taste or odor, progressive crowding, or findings of cysts or significant bone changes on imaging. If any of those are present, it is usually worth discussing removal rather than waiting indefinitely.
If a tooth was extracted long ago, is an implant still possible?
Often yes, but it depends on the amount of bone loss and your health factors. Longer time since extraction can mean more ridge resorption, so you may need bone grafting before implant placement. Your dentist or oral surgeon will evaluate bone volume with imaging and check healing and risk factors like smoking, diabetes control, and periodontal history.
Does tooth decay ever stop progressing if I stop sugar or start using fluoride?
Stopping progression is possible for early, non-cavitated lesions, but an already established cavity does not “self-seal” just by improving hygiene. Decay is a continuing process, and once structural loss has formed, the bacteria are underneath the surface and restorative removal plus sealing is typically what prevents further spread.
I had root canal treatment. Does that mean my tooth can no longer “heal” or protect itself?
Root canal treatment removes diseased pulp tissue, but it does not regenerate the pulp. The tooth can still be strong, especially with a well-fitting crown when a lot of structure was lost, but the focus becomes mechanical protection and sealing. A common mistake is delaying the crown after a large root canal, which can increase fracture risk.
Is oil pulling or supplements a substitute for dental visits and preventive care?
No. These may affect mouth feel or saliva temporarily for some people, but they are not evidence-based treatments for enamel loss, recession from periodontitis, or cavities that are already structural. If you are trying to prevent problems, the higher-impact steps are consistent brushing with fluoride, floss or interdental cleaning, professional cleanings, and targeted interventions like sealants when appropriate.
What is the single best time to intervene if I’m worried about “not growing back”?
The best time is before structural loss happens. Early symptoms like sensitivity in young people, white spot lesions, or bleeding and inflammation in gums are windows where stopping the process is more realistic than trying to rebuild. If you have pain, swelling, or a suspected cavity, schedule an exam promptly rather than waiting for it to “settle”.

Find Where Smiles Grow in Delmar fast: pediatric dentist address, hours, booking tips, and dental regrowth facts for par
Teeth grow in two natural sets: baby then permanent. Regrowth after loss is rare; wisdom teeth are the exception.
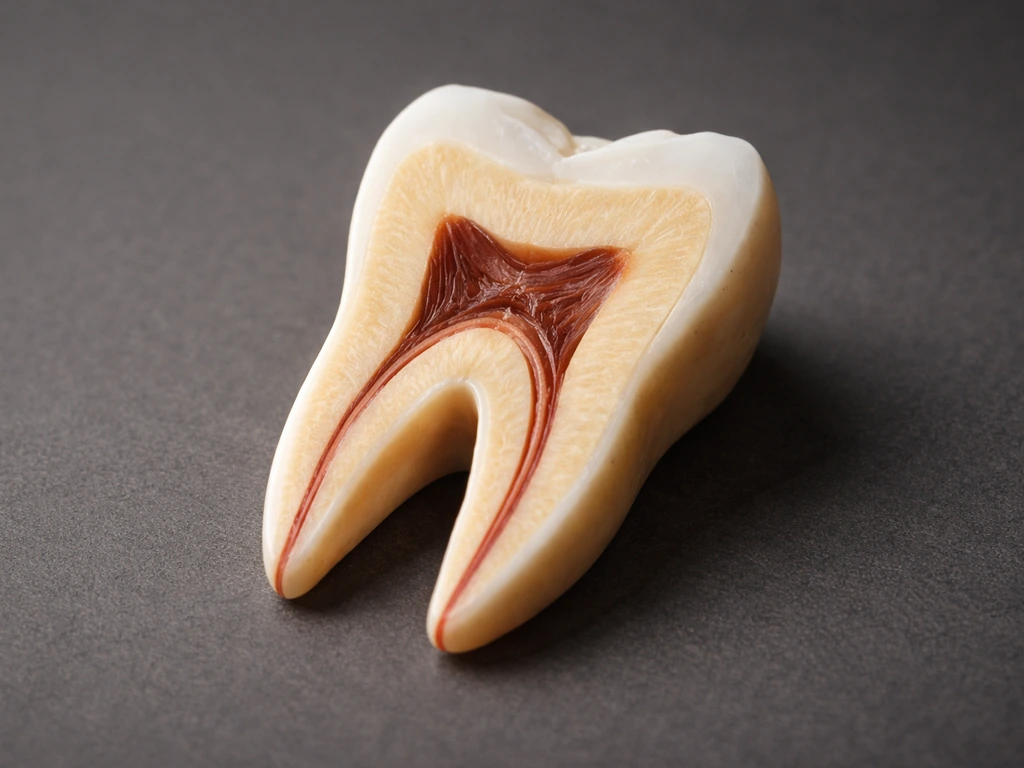
Debunks can teeth grow back 3 times. Explains natural tooth replacement once, enamel remineralization, and real treatmen

