But here is where the nuance matters: there is a real and useful process called remineralization, and it is not the same thing as growing new enamel. Remineralization means calcium and phosphate ions (from saliva, fluoride products, and diet) are deposited back into the crystal structure of enamel that has been partially dissolved by acid. The American Dental Association describes it as increasing the mineral content of previously damaged enamel, which can restore surface smoothness on early, noncavitated lesions. So you are not building new enamel from scratch. You are re-hardening and strengthening enamel that still exists but has been partially weakened. That distinction matters enormously for deciding what you should actually do.
Age also changes the conversation. In children whose permanent teeth are still developing or recently erupted, enamel is still maturing and mineralizing, making it more responsive to fluoride and remineralization support. For adults and seniors, the window for reversing early damage is narrower, but remineralization is still very real and worth pursuing. If you are wondering about broader tooth development questions, what helps teeth grow covers the development side in more depth.
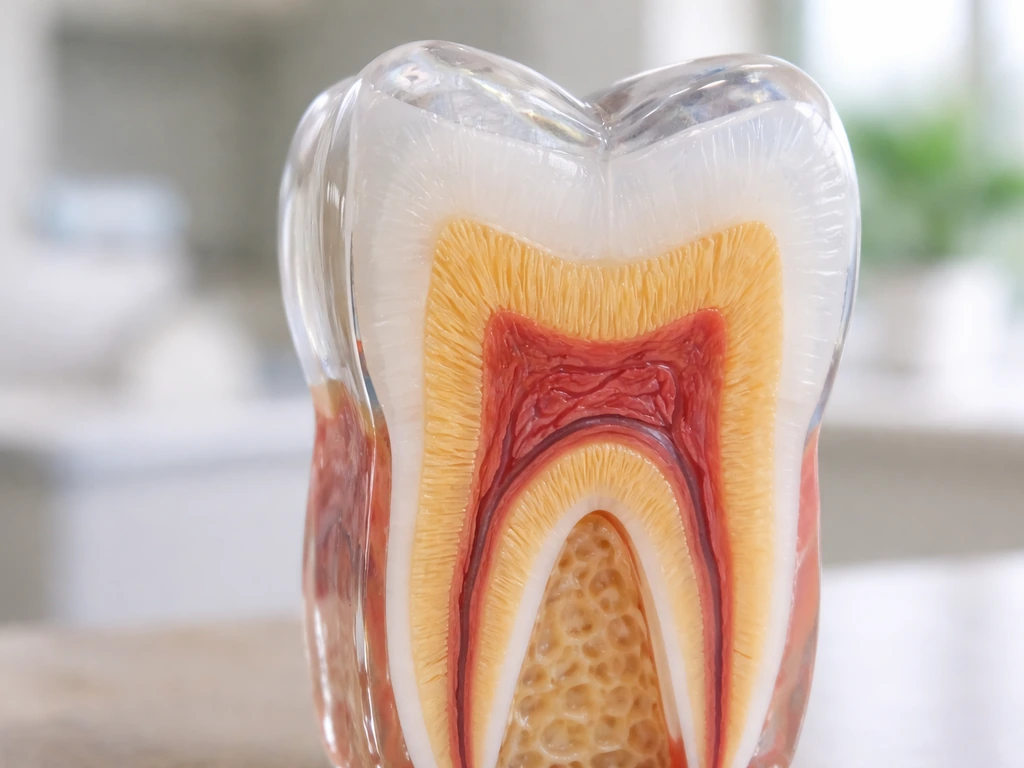
How enamel loss happens: erosion, decay, and exposed surfaces
Enamel loss is not one single thing. It comes from several different mechanisms, and knowing which one is affecting you changes how you address it.
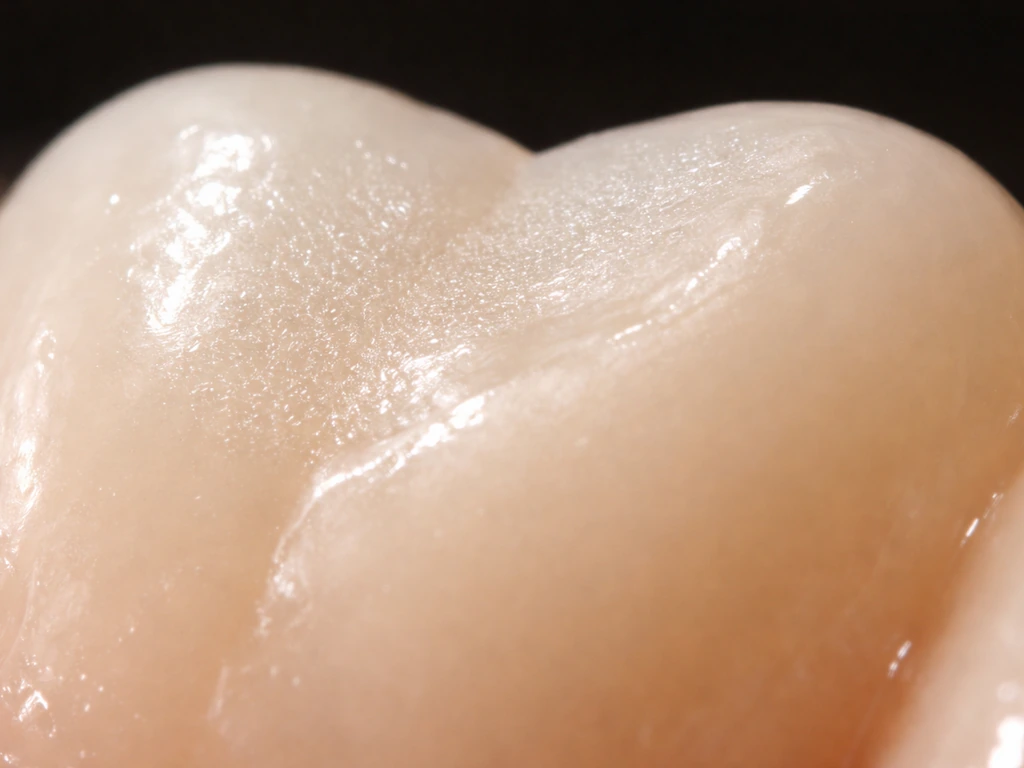
- Acid erosion: Dietary acids from citrus, sodas, sports drinks, and vinegar-based foods dissolve the mineral crystals in enamel directly. Acid reflux (GERD) does the same thing from the inside. This type of erosion tends to appear as smooth, scooped-out surfaces and generalized thinning.
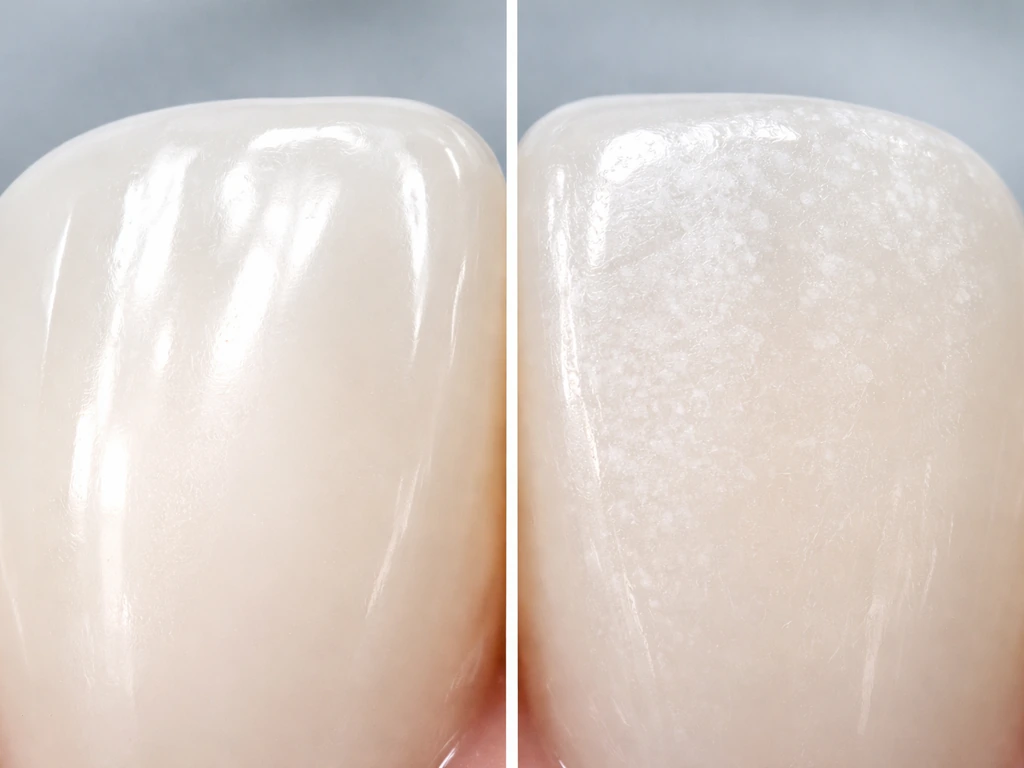
- Demineralization from bacterial acids: When plaque bacteria metabolize sugar, they produce lactic acid right against the tooth surface. This is the precursor to cavities. Early lesions appear as white or chalky spots (white spot lesions) before a hole forms.
- Mechanical wear: Aggressive brushing with a hard-bristled toothbrush, bruxism (tooth grinding), and abrasive toothpastes physically scrape away enamel over time.
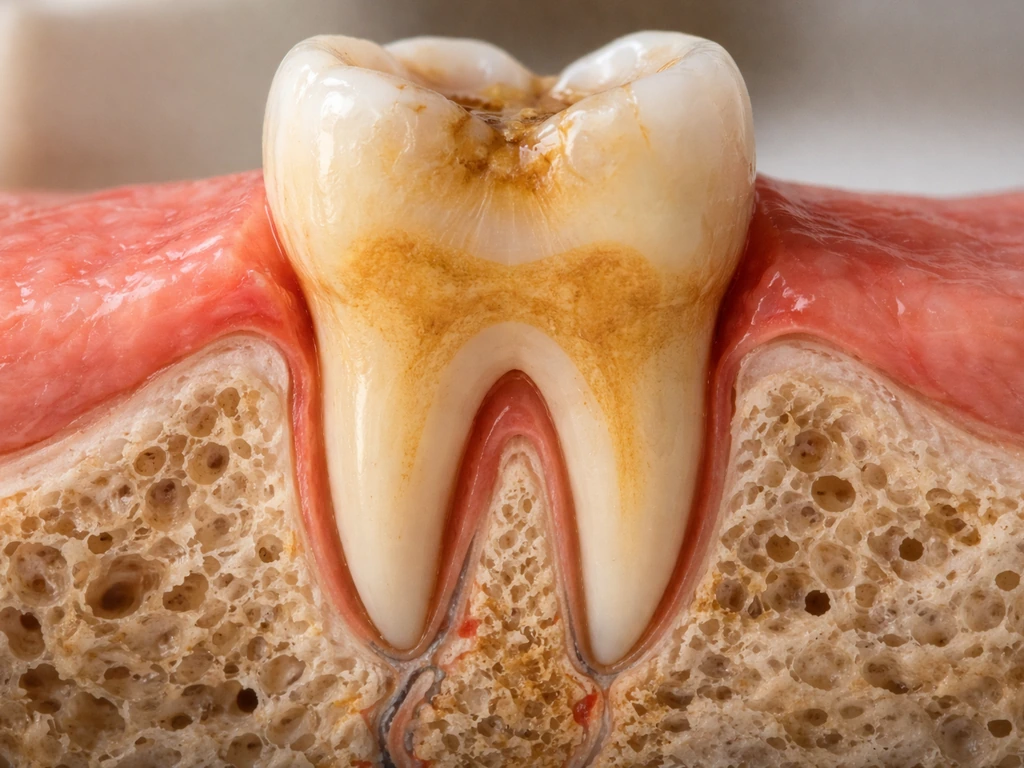
- Gum recession exposing root surfaces: Root surfaces are covered by cementum, not enamel. When gums recede and roots are exposed, those surfaces are softer and more vulnerable to acid and abrasion than enamel ever was.
- Age-related thinning: Enamel naturally thins over decades of use, making older teeth more susceptible to sensitivity and further damage.
One important myth to bust here: whitening products do not cause enamel to "disappear," but overuse of highly abrasive whitening products or acidic whitening strips can temporarily demineralize the surface, increasing sensitivity and roughness. That is not the same as permanent structural loss in most cases, but it is a reason to use whitening products as directed and not to stack multiple aggressive treatments at once.
How to restore enamel naturally at home (remineralization basics)
Remineralization is real, it works for early-stage enamel damage, and it is something you can actively support every day. The key ingredients are fluoride, calcium, phosphate, and a healthy saliva flow. Here is how they each work.
Fluoride works by incorporating into the enamel crystal lattice and forming fluorapatite, which is harder and more acid-resistant than the original hydroxyapatite. Standard fluoride toothpaste (1,000 to 1,500 ppm) is effective for most adults. People with a history of frequent cavities or active enamel erosion often benefit from a higher-concentration fluoride toothpaste (up to 5,000 ppm), which is available by prescription. The critical thing most people get wrong: do not rinse your mouth with water immediately after brushing. Spit, but do not rinse. Leaving the fluoride on your teeth for longer after brushing significantly increases its effectiveness.
Calcium and phosphate support
Products containing casein phosphopeptide-amorphous calcium phosphate (CPP-ACP), sold under the brand name MI Paste in many countries, deliver calcium and phosphate directly to the tooth surface and have solid research behind them for remineralizing early white spot lesions. They are not magic, but they are genuinely useful, especially when used after fluoride treatment (apply fluoride first, then CPP-ACP later in the day). Hydroxyapatite toothpastes are another option with emerging evidence, particularly relevant for people who prefer fluoride-free products.
Diet changes that actually move the needle

Reducing the frequency of acid and sugar exposure matters more than the total amount. Sipping a soda over two hours is far worse for your enamel than drinking one in ten minutes, because you are keeping the pH in your mouth low for a sustained period. Dairy products like cheese and milk raise salivary calcium levels and can buffer oral pH after a meal. Does milk help your teeth grow goes into detail on what dairy actually does for dental health. Crunchy, fibrous vegetables stimulate saliva flow, which is your mouth's natural remineralizing agent. Water, particularly fluoridated tap water, is the best between-meal drink.
What does not work (the myth-busting part)
Activated charcoal toothpaste is highly abrasive and has no evidence of remineralization benefit. It can actually remove surface enamel through mechanical abrasion. Oil pulling has not been shown in quality research to remineralize enamel. Apple cider vinegar used topically is acidic and directly erodes enamel. Calcium supplements taken orally do not translate directly into more calcium in your enamel. None of these address the actual mechanism of remineralization, which requires fluoride or calcium/phosphate delivery directly to the tooth surface at the right pH. Skip the hacks and focus on the ingredients with real mechanisms.
Your daily routine: brushing, fluoride timing, diet, and saliva support
A consistent daily routine is what actually prevents further enamel loss and keeps remineralization working in your favor. Here is what a practical evidence-based routine looks like.
- Brush twice daily with a soft-bristled toothbrush and fluoride toothpaste. Use gentle, circular motions. Scrubbing hard does not clean better; it just wears enamel and damages gums.
- Wait 30 to 60 minutes after eating acidic food or drinking soda before brushing. Acid temporarily softens enamel, and brushing immediately can accelerate abrasion.
- After brushing at night, spit but do not rinse. This leaves a thin fluoride film on your teeth overnight when saliva flow is lower and remineralization can work undisturbed.
- Use a fluoride mouthwash at a different time of day from brushing (mid-afternoon or after lunch works well) to add another fluoride exposure window.
- Drink water throughout the day, especially after meals. Rinsing with water after acidic food or drink raises oral pH quickly.
- Chew sugar-free gum (xylitol-containing options are ideal) after meals when brushing is not possible. This stimulates saliva flow and raises pH within minutes.
- If you have dry mouth from medication, medical conditions, or just age, talk to your dentist. Reduced saliva flow dramatically increases enamel demineralization risk because saliva is your body's main remineralizing agent.
- If you grind your teeth at night, get a custom night guard. Bruxism is one of the fastest ways to mechanically destroy enamel and no amount of remineralization product offsets active grinding.
For children, the routine is similar but with age-appropriate fluoride levels. Kids under 3 use a smear of fluoride toothpaste; kids 3 to 6 use a pea-sized amount. Parents often ask whether their child's teeth are developing properly or whether small teeth will keep growing. If that is on your mind, the article on my teeth are small, will they grow addresses exactly that question.
How to tell if it's reversible vs needs dental treatment
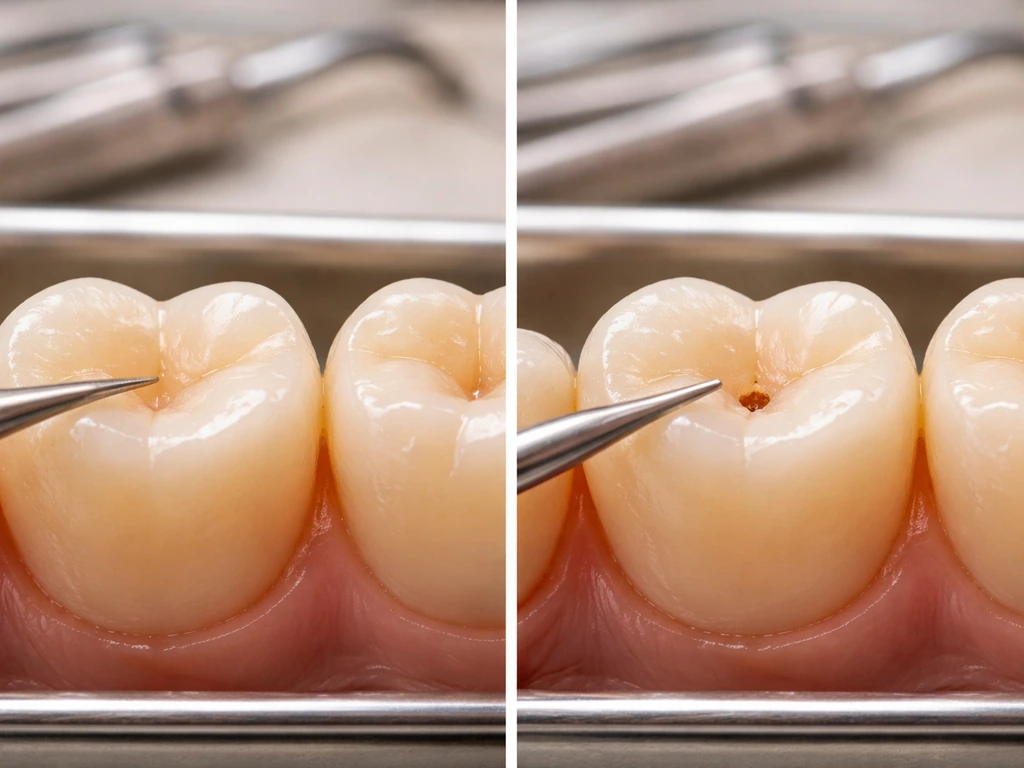
This is the most important judgment call you need to make, because remineralization only works on early, noncavitated lesions. Once there is a hole in the tooth (a cavity), the mineral structure has been broken through and remineralization cannot fill that gap. You need a filling.
Early, potentially reversible enamel damage typically looks or feels like: chalky white or milky spots on the tooth surface (especially near the gumline), mild sensitivity to cold or sweet foods that passes quickly, a slightly rough texture you can feel with your tongue, or a dull appearance compared to surrounding enamel. These are white spot lesions and they represent demineralization that has not yet broken through the surface. With consistent remineralization effort and possibly a fluoride varnish treatment from your dentist, these can stabilize and often partially reverse.
Signs you are past the reversible stage and need professional treatment: a visible pit or hole you can see or feel, brown or black discoloration in a specific spot (not just generalized staining), persistent toothache or sensitivity that does not go away quickly, pain when you bite down, or visible cracks. At this point, remineralization products are not going to close a hole. You need restorative treatment.
For erosion specifically (the smooth, scooped-out look), the reversibility question depends on how much enamel is left. If erosion has reached dentine (the yellowish layer underneath enamel), remineralization cannot restore what is missing. A dentist can assess this with an exam and, in some cases, X-rays or other imaging.
| Sign or Symptom | Likely Stage | What To Do |
|---|
| Chalky white spot, no rough edge or cavity | Early demineralization (reversible) | Start remineralization routine, see dentist for fluoride varnish |
| Mild cold/sweet sensitivity that resolves fast | Early-to-moderate enamel thinning | Remineralize, use sensitivity toothpaste, get dental eval |
| Rough or pitted surface you can feel | Surface breakdown beginning | Dentist exam needed; may still be treatable with sealant or varnish |
| Visible hole, brown/black spot, or persistent pain | Established cavity or severe erosion | Restorative treatment required (filling, bonding, or crown) |
| Generalized thinning, yellowing, sensitivity throughout | Significant erosion, possibly to dentine | Dentist exam, address underlying cause (diet, GERD, etc.) |
Professional treatments that replace or repair lost enamel
When enamel damage is beyond what remineralization can address, dentistry has a solid toolkit. The right option depends on how much enamel is lost and where.
Fluoride varnish and prescription fluoride
Applied in-office, fluoride varnish delivers a high-concentration fluoride dose directly to the tooth surface and is one of the most evidence-backed tools for arresting early enamel lesions and remineralizing white spots. Your dentist may also prescribe a 5,000 ppm fluoride toothpaste for home use if your enamel is at elevated risk. These are not cosmetic treatments; they are genuinely functional and should be the first step for anyone with active early enamel loss.
Dental sealants
For pits and fissures in back teeth that are at high risk of decay but have not yet formed cavities, sealants are a thin resin coating applied to the chewing surface. They are especially common in children and teenagers but can be applied to adults too. They do not replace lost enamel, but they protect the remaining enamel from further acid and bacterial attack.
Composite bonding and white fillings
For established cavities or small areas of significant enamel loss, tooth-colored composite resin is bonded directly to the tooth. This is the standard "filling" most people are familiar with. It restores the shape and function of the tooth and seals the area from further decay. Composite bonding can also be used cosmetically to cover areas where erosion has left teeth looking shorter, thinner, or discolored.
Veneers and crowns for significant enamel loss
When enamel loss is severe enough to affect the whole tooth surface (common in people with long-term GERD, eating disorders, or heavy erosion), porcelain veneers or full crowns may be the appropriate solution. These cover the remaining tooth structure entirely and restore function, appearance, and protection. They are not a first resort but are the right call when structural integrity is genuinely compromised.
Treating the underlying cause
No restorative treatment holds up long-term if the cause of enamel loss is still active. If acid reflux is eroding your enamel from the inside, managing your GERD with your physician is just as important as any dental work. If dry mouth from medication is your issue, your doctor may be able to adjust your prescription or recommend saliva substitutes. If diet is the driver, changes there are non-negotiable. Treating enamel loss without addressing the cause is like patching a leak without turning off the water.
People researching enamel recovery often wonder whether the tooth itself could regrow under the right conditions. If that broader question interests you, how to grow new teeth covers what science currently says about tooth regeneration research. For those focused specifically on enamel-building strategies, how to grow teeth enamel digs deeper into the remineralization science.
What to ask your dentist and how to move forward today
If you suspect enamel damage, the most useful thing you can do right now is book a dental exam and go in with specific questions. Ask your dentist whether your enamel loss is noncavitated (meaning remineralization is still on the table) or whether you have active cavities that need restoration. Ask whether you are a candidate for fluoride varnish. Ask whether there is an underlying cause (like reflux or bruxism) that needs to be addressed. Ask whether prescription-strength fluoride toothpaste makes sense for your situation.
In the meantime, start the daily routine described above. Switch to a soft-bristled brush if you have not already. Stop rinsing after you brush at night. Cut the frequency of acidic drinks. These steps cost nothing and begin shifting the balance toward remineralization immediately. The biology is clear that you cannot grow enamel back from scratch, but you absolutely can stop losing more of it and strengthen what remains. That is a realistic and worthwhile goal, and it starts today.
If you have children and are thinking about how all of this applies to their developing teeth, how to grow back teeth addresses the specific context of children's dental development and what parents can do at each stage. And if you want a broader overview of what supports healthy dental development from the beginning, what helps teeth grow is worth a read too.