Plaque removal can absolutely make your gums look and feel healthier, but it depends on what kind of damage has already happened. If your gums are inflamed from plaque buildup (red, puffy, bleeding when you brush), removing that plaque lets the inflammation settle down and the tissue can bounce back to normal within days to a few weeks. That is not the same thing as growing back lost gum tissue. Once gum recession has actually occurred and tissue has pulled away from the tooth, that physical loss does not reverse itself just because plaque is gone. So the honest answer is: yes, your gums can return to normal after plaque removal, but only if what you are seeing is inflammation, not true recession.
Do Your Gums Grow Back After Plaque Removal? What to Expect
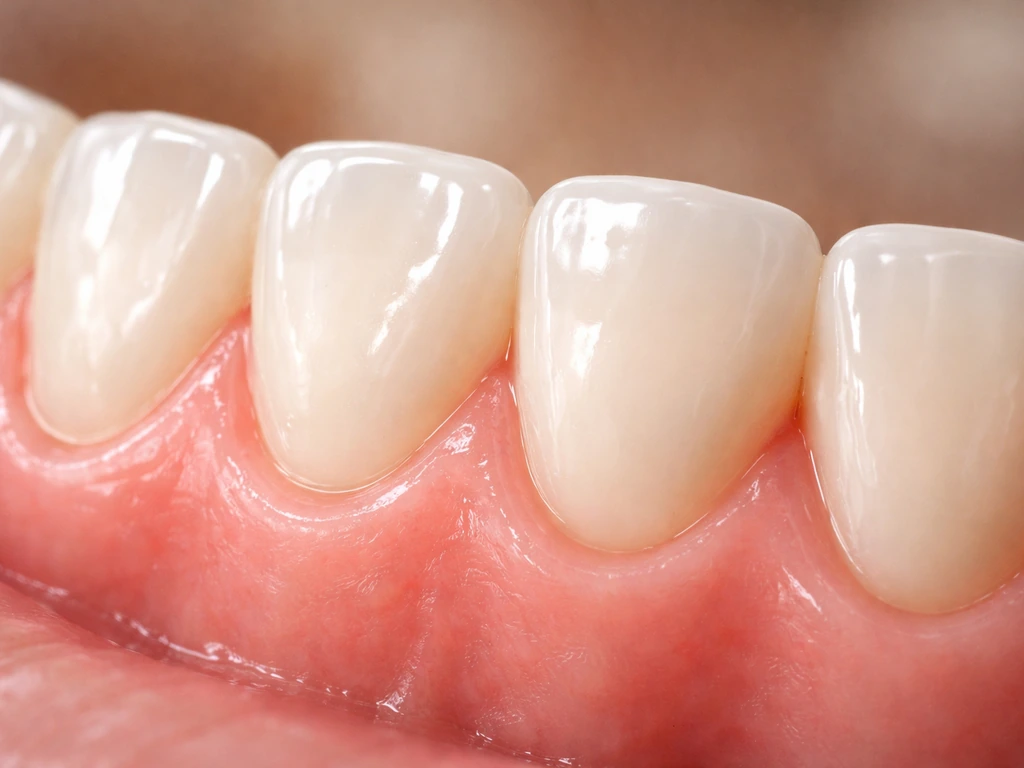
What plaque removal can change in the gums (and what it can't)
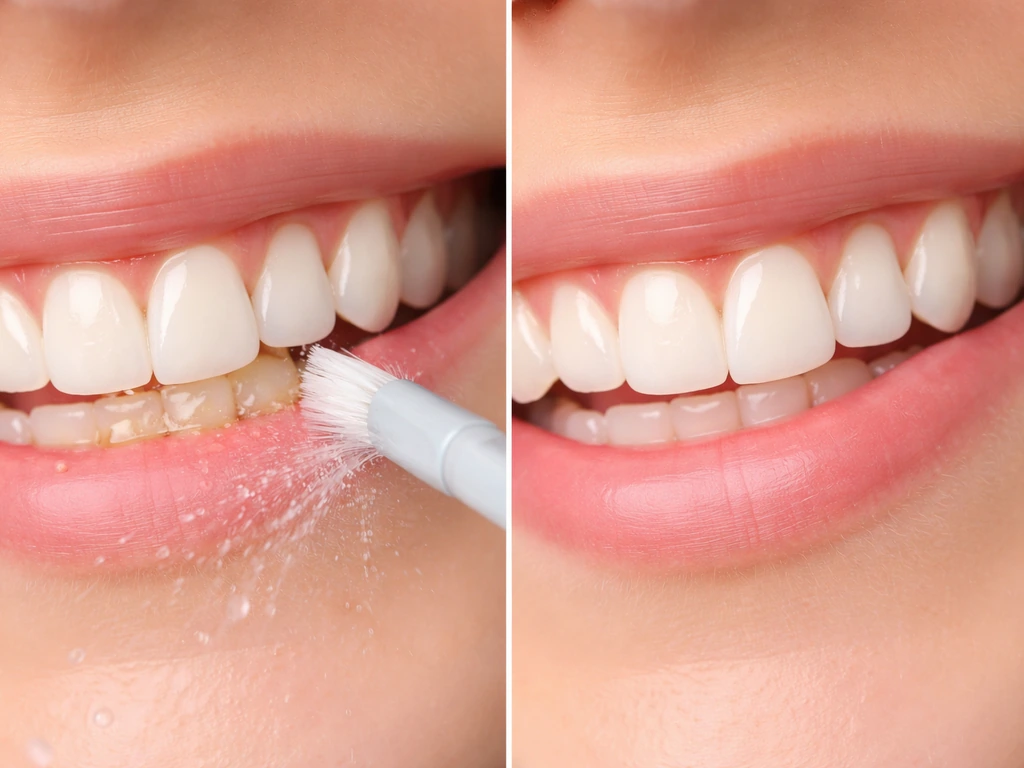
Plaque is a sticky film of bacteria that, when left on your teeth and along the gumline, triggers an inflammatory response in the surrounding tissue. Your immune system reacts to those bacteria, and the result is gums that swell up, turn red or purple, and bleed easily. That swelling is your body trying to fight infection, and it can actually make your gums look larger or more prominent than they normally would.
When you remove plaque consistently (through brushing, flossing, and professional cleaning), you take away the source of that irritation. The inflammation calms down, the swelling reduces, and the gum tissue firms up again. For a lot of people, this looks and feels like the gums "grew back" or returned to normal. In the case of gingivitis, that is basically accurate.
What plaque removal cannot do is regenerate tissue that is structurally gone. If your gums have receded because of periodontitis (advanced gum disease), aggressive brushing, or other causes, the gum tissue that moved away from the tooth does not just come back once the plaque is cleared. The underlying bone and connective tissue attachment that supports the gum margin has been lost, and no amount of home cleaning will rebuild it. That requires professional intervention, and even then, complete regrowth is not always achievable.
Gum "growing back" vs. inflammation going down: key differences
This is probably the most important distinction to understand, because these two things look similar but are biologically very different.
When plaque inflames the gums, the tissue becomes edematous (swollen with fluid) and can even enlarge slightly, making it appear to creep further up the tooth. When you clean the plaque away, that swelling recedes. The gums look smaller and tighter against the tooth, which is actually a good thing. But some people interpret this tightening as the gums "shrinking" and then worry they have lost tissue. In reality, the gum margin is now sitting where it is supposed to sit.
True gum recession is the opposite situation: the tissue actually moves apically (toward the root of the tooth), exposing more of the tooth surface than normal. You will typically notice this as increased tooth sensitivity, teeth that look longer than before, or a visible notch or gap at the gumline. Plaque removal alone will not push that tissue back up the tooth. Once attachment is lost, it is lost unless surgically addressed.
| Feature | Gum Inflammation (Gingivitis) | True Gum Recession |
|---|---|---|
| Cause | Plaque bacteria irritating the gum tissue | Tissue/bone loss from periodontitis, brushing trauma, or other damage |
| Appearance | Red, puffy, swollen gums that may bleed | Gums pulling away from teeth, teeth looking longer |
| Reversible? | Yes, with plaque removal and good hygiene | No, not without surgical treatment |
| Bone involvement | None (soft tissue only) | Often yes (bone loss in periodontitis) |
| What helps | Brushing, flossing, professional cleaning | Gum grafting, regenerative procedures, or scaling/root planing to halt progression |
How fast you might see improvement after cleaning
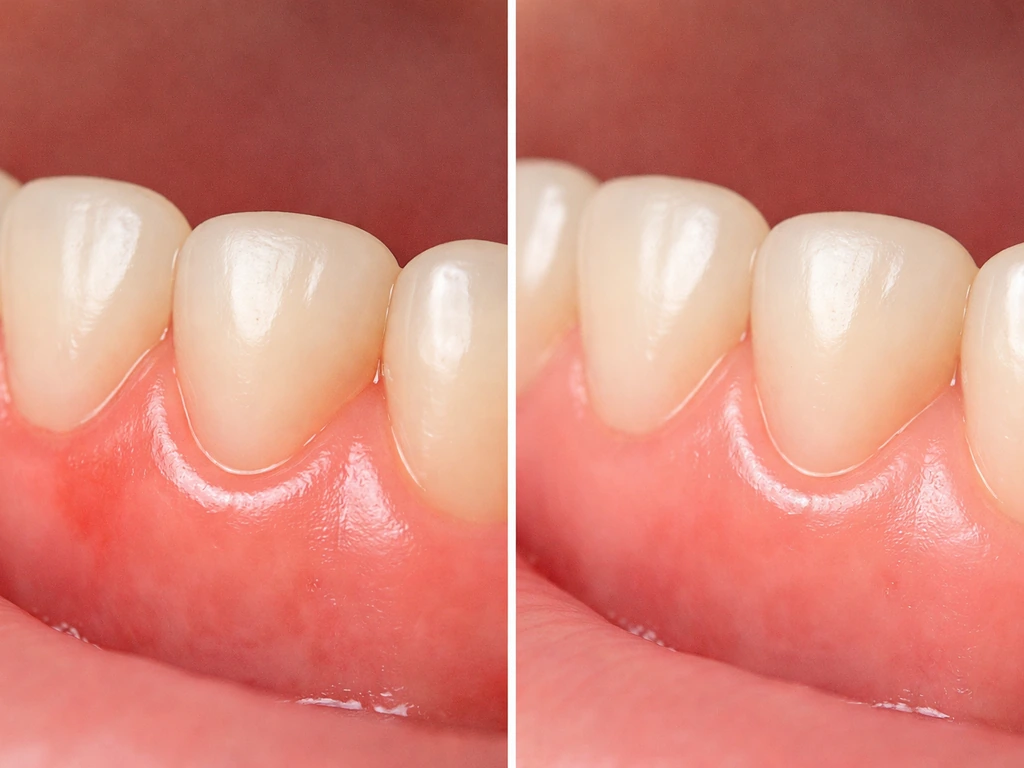
If you have gingivitis and you start properly removing plaque every day, you can expect to see noticeable changes within about one to two weeks. The gums will bleed less, feel less tender, and start to return to a healthy pink color. Mayo Clinic notes that with treatment and continued home care, healthy gum tissue should return within days to weeks. The CDC classifies gingivitis as the mildest and most reversible form of gum disease, meaning it responds well to consistent plaque control.
The key word there is consistent. A one-time cleaning at the dentist will reduce your bacterial load, but if you go home and skip flossing, plaque starts rebuilding within 24 hours and the inflammation cycle starts again. Research from a Cochrane review found that routine professional scale and polish procedures showed little benefit for mild gum issues when patients were not also doing effective plaque control at home. The cleaning itself is not a cure, it is a reset that buys time for good habits to take over.
For more advanced cases (periodontitis, deep pockets, significant bone loss), improvement timelines are longer and the outcome is different. You are not reversing the damage at that point, you are halting it and managing it. Healing around deeper gum pockets after procedures like scaling and root planing can take four to six weeks or longer, and follow-up assessments are needed to gauge response.
When gums can improve: early gingivitis vs. recession and periodontitis
Think of gum disease as a spectrum. On one end is early gingivitis, which involves inflammation only in the gum tissue itself, with no structural destruction to the bone or connective tissue fibers that anchor the tooth. StatPearls (from the NCBI) is clear on this: gingivitis is reversible precisely because it stays confined to the soft tissue and does not involve attachment loss. At this stage, diligent plaque removal can fully restore gum health.
Once gingivitis progresses to periodontitis, the nature of the disease changes. Pockets deepen around the teeth, bacteria migrate below the gumline, and the body's inflammatory response starts destroying the bone and connective tissue that hold the tooth in place. InformedHealth.org describes periodontitis as involving episodes of tissue destruction with deeper gum pockets, bone loss, and eventually loose teeth if untreated. This stage is not reversible through plaque removal alone. You can stop the progression, but you cannot rebuild what has been lost without clinical intervention.
Recession caused by brushing too hard sits in a different category. That is a mechanical injury to the tissue rather than an infection-driven one. Removing plaque properly will prevent further bacterial inflammation, but it will not regenerate the gum tissue displaced by the physical trauma of hard scrubbing. The approach there involves correcting the brushing technique, switching to a soft-bristled brush, and potentially discussing a gum graft with a periodontist if the recession is significant.
For parents wondering about children: kids with healthy baby teeth and early gingivitis respond the same way adults do in the early stages. Their gum tissue can fully recover once plaque is controlled. Children are not more regeneratively capable than adults when it comes to the gum tissue itself.
What to do today: at-home cleaning steps that protect gum tissue
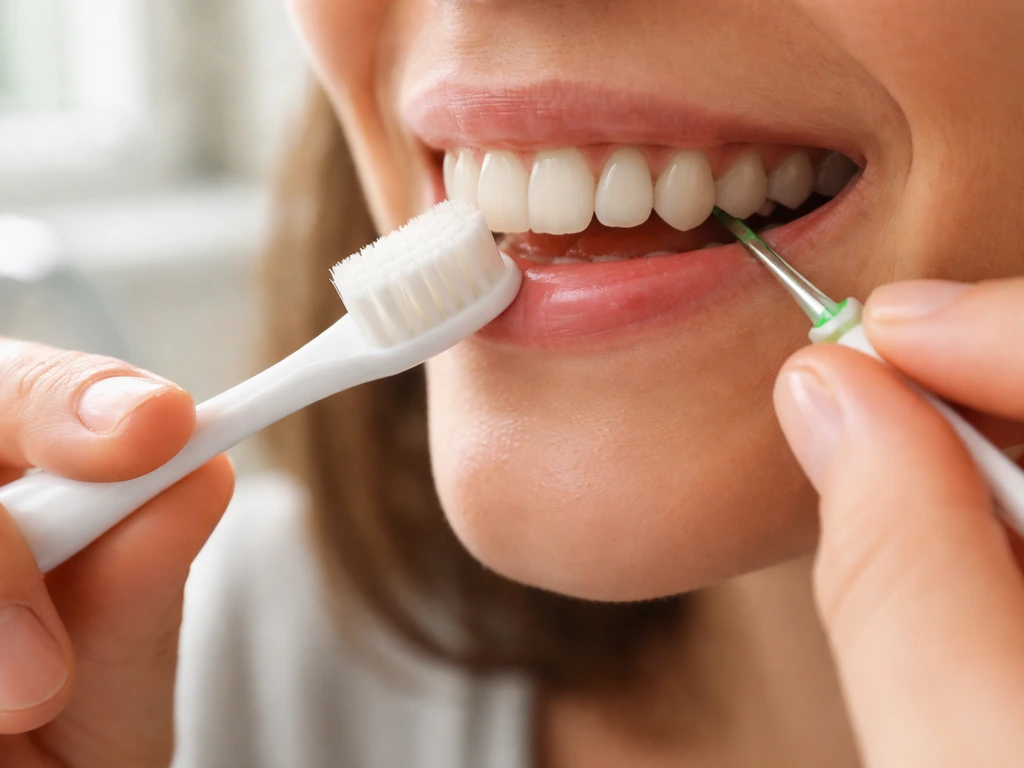
The most important thing you can do right now is get consistent about plaque removal without damaging the gum tissue in the process. Here is what that looks like practically:
- Brush twice a day for two minutes using a soft-bristled toothbrush. Medium and hard bristles cause more harm than good for gum tissue, especially if you already have inflammation or recession.
- Use gentle circular or modified Bass technique strokes at a 45-degree angle to the gumline. Aggressive back-and-forth scrubbing is one of the main causes of mechanical gum damage.
- Floss once a day, sliding the floss in a C-shape around each tooth and gently going below the gumline. This is the only way to remove plaque from the areas a brush cannot reach.
- Consider an antiseptic mouthwash like chlorhexidine (short-term, dentist-directed) or an over-the-counter antibacterial rinse to reduce bacterial load if your gums are actively inflamed.
- Avoid tobacco in any form. Smoking dramatically slows gum healing and masks bleeding, making disease harder to detect early.
- Stay hydrated and manage dry mouth, since reduced saliva flow accelerates plaque buildup.
- Do not skip flossing because your gums bleed. Bleeding is usually a sign of inflammation, and consistent flossing will reduce that bleeding over one to two weeks as the tissue heals.
Also worth saying plainly: do not go harder on your gums to try to speed things up. More pressure does not mean faster healing. It often means more damage, which is the opposite of what you need.
When you need the dentist: signs of deeper gum disease and professional options
Some situations genuinely require professional treatment, and waiting or relying on home care alone will make things worse. See a dentist (or ideally a periodontist) sooner rather than later if you notice any of these:
- Gums that bleed heavily during brushing or flossing, or bleed spontaneously
- Persistent gum soreness, tenderness, or pain that does not improve after a week or two of better hygiene
- Gums that are visibly pulling away from the teeth or teeth that look noticeably longer than before
- Loose or shifting teeth, which indicates bone loss
- Pus between the teeth and gums, or a persistent bad taste or smell
- Gum changes that are worsening rapidly over days rather than weeks
- Any recession that is significant enough to expose root surfaces, which increases cavity risk and sensitivity
Professional options at this stage go beyond a standard cleaning. Scaling and root planing (sometimes called a deep cleaning) involves removing plaque and tartar from below the gumline and smoothing the root surfaces to discourage bacterial reattachment. For more advanced recession or bone loss, a periodontist may discuss procedures like gum grafting (where donor tissue is placed to cover exposed roots) or guided tissue regeneration (where membranes and bone grafting materials help stimulate regrowth of the supporting structures). These are meaningful interventions, but they are not magic resets. The outcome depends heavily on the severity of the disease and your ongoing maintenance.
The topic of what happens to gums after specific dental procedures like osseous surgery, scaling, or tartar removal follows similar biological rules, the treatment goal is always to eliminate the bacterial source and allow the tissue to stabilize, not to regenerate tissue from scratch. The topic of what happens to gums after specific dental procedures like osseous surgery, scaling, or tartar removal follows similar biological rules, the treatment goal is always to eliminate the bacterial source and allow the tissue to stabilize, not to regenerate tissue from scratch.
Myths about gum regrowth and the real limits of regeneration
Let's address the internet claims directly, because there is a lot of misinformation floating around about gum tissue "growing back naturally."
Myth: Once you clean your teeth properly, receded gums will grow back on their own. This is false. After wisdom teeth removal, gum irritation can improve as the area heals, but true gum recession will not regrow on its own without proper dental treatment. Once gum tissue has receded and the underlying bone attachment is lost, it does not regenerate without surgical intervention. Crown lengthening may be one option your dentist considers if you have true gum recession and need more tooth structure exposed. The human body does not spontaneously rebuild lost periodontium (the system of tissues that surround and support the teeth) through hygiene alone. Plaque removal prevents further damage, it does not reverse existing structural loss.
Myth: Natural remedies like oil pulling, turmeric, or aloe vera can regenerate receded gums. There is no credible clinical evidence that any of these approaches regenerate lost gum tissue. Some may have mild anti-inflammatory properties that help with early gingivitis symptoms, but none of them grow new tissue where physical loss has occurred.
Myth: Children regenerate gum tissue faster because they are still growing. Not true. Children's gum tissue has the same biological rules as adults when it comes to gingival regeneration. What children do have is the potential to develop healthy new tissue around erupting permanent teeth, but that is normal tooth eruption, not gum regeneration from damage.
Myth: If your gums stop bleeding after treatment, they have grown back. Bleeding stopping is a sign that inflammation has reduced, not that tissue has regenerated. Healthy gums are firm, pink, and do not bleed on probing. If yours reach that state after improving your hygiene, it means gingivitis has resolved, which is great, but it is not evidence of any new tissue forming.
The biological reality is this: human gum tissue (the gingiva) can heal from inflammation and return to its normal position and health when the cause (plaque and bacteria) is removed early enough. But it is not a regenerating tissue in the way that, say, skin can partially regenerate after a minor cut. Once the fibrous attachment and bone support are gone, that loss is permanent without surgical correction. This is why catching gum disease early, at the gingivitis stage, makes such a dramatic difference in outcomes.
The bottom line: do not wait and hope your gums will grow back on their own if you are seeing visible recession or worsening symptoms. Start the right home care habits today, and get a professional assessment if things do not improve within two to four weeks of consistent effort. Early action is the most powerful tool you have.
FAQ
I have bleeding gums. Should I stop brushing until it heals?
If your gums are bleeding, you should still keep cleaning, but reduce trauma: use a soft-bristled brush, gentle pressure, and daily floss or interdental cleaning. Bleeding that rapidly improves usually signals inflammation settling down, not tissue regrowth.
If I get a scale and polish, will my gums stay healthy without changing my at-home routine?
A “reset” can happen after professional cleaning, but plaque begins reforming quickly. Without daily home plaque control, the inflammation cycle returns, so the visible change you get from one visit often fades within weeks.
How can I tell if what I’m seeing is recession, not just gum swelling?
Sensitivity and “longer-looking teeth” are warning signs for true recession or attachment loss, especially if the gum margin is stable and the tooth looks permanently longer. If that pattern is present, you generally cannot fix it with plaque removal alone.
Could my recession be from brushing too hard rather than gum disease?
If you recently increased brushing intensity or switched to firmer brushes, you can trigger or worsen recession from mechanical trauma. The right next step is to scale down pressure and use a soft brush, then reassess after several weeks.
How long should I wait to see improvement after starting better plaque removal?
If recession or gum margin changes are due to inflammation, you typically notice improvement within about 1 to 2 weeks of consistent plaque control. If nothing improves by 2 to 4 weeks, or it worsens, you likely need an in-person periodontal evaluation.
Can gums really regrow if I’ve had periodontitis or bone loss?
Not usually. Once connective tissue attachment and bone support are lost, regrowth is limited and often requires periodontal procedures. Home care can stabilize conditions, but it usually cannot rebuild lost support by itself.
Do smoking or diabetes affect whether my gums can recover after plaque removal?
Smoking and poorly controlled diabetes commonly slow gum healing and worsen periodontal outcomes. If you smoke or have diabetes, it can change timelines and the likelihood of improvement, so coordinating care with a dentist and medical clinician matters.
I have dry mouth. Will that make it harder for my gums to improve?
Dry mouth reduces saliva’s protective effects, making it easier for plaque to accumulate and for inflammation to persist. Addressing hydration, mouth dryness triggers, and any medications with your clinician can support gum recovery alongside cleaning.
Can mouthwash or toothpaste alone reverse inflamed gums?
Toothpastes and mouthwashes may reduce inflammation or bacterial load, but they do not replace mechanical plaque removal. For example, an antiseptic rinse can help as an add-on, but it cannot fix recession caused by lost attachment.
When should I stop self-treating and see a periodontist?
If you have deep pockets, persistent bad breath, pus, loose teeth, or swelling that does not settle, you should not wait. Ask for a periodontal assessment, because deep infection below the gumline often requires scaling and root planing or other staged treatment.
See what regrows after Invisalign gum recession, what stays permanent, why it happens, and next-step checks.
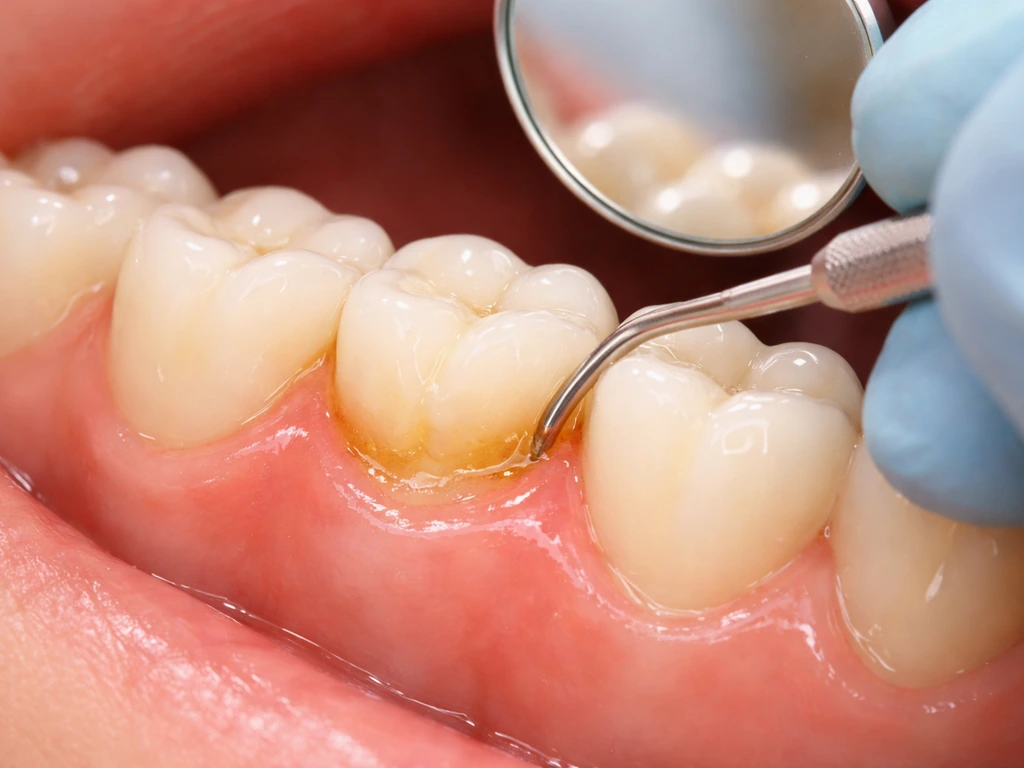
Learn what happens to gums after tartar removal, which changes are reversible, and when recession needs more care.
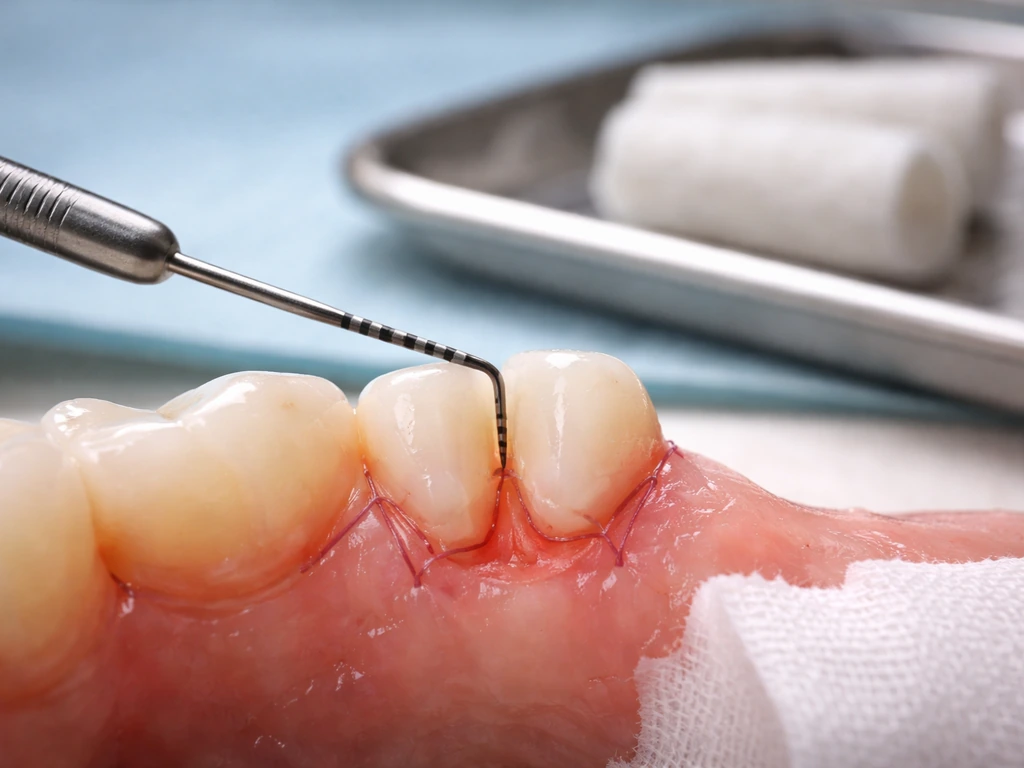
Learn if gums truly regrow after osseous surgery, typical timelines, factors that affect results, and red flags.

