Yes, gum tissue does grow around a dental implant, and to a meaningful degree it can grow over a cover screw or healing abutment during the early healing phase. What it cannot do is regenerate the way your body heals a cut on your skin. The soft tissue around an implant reattaches and matures, but it forms a slightly different biological seal than the one around a natural tooth, and that distinction matters a lot when you're trying to figure out whether what you're seeing is normal healing or a real problem.
Does Gum Grow Around Implant? What to Expect and Fix
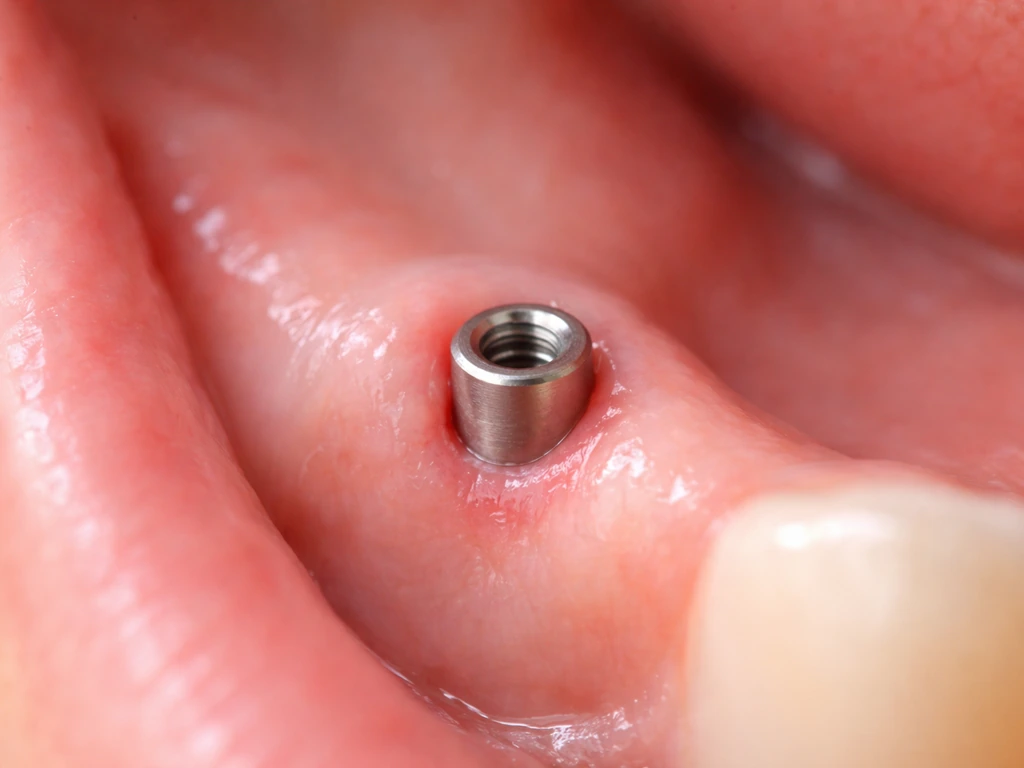
What actually happens to your gums after an implant
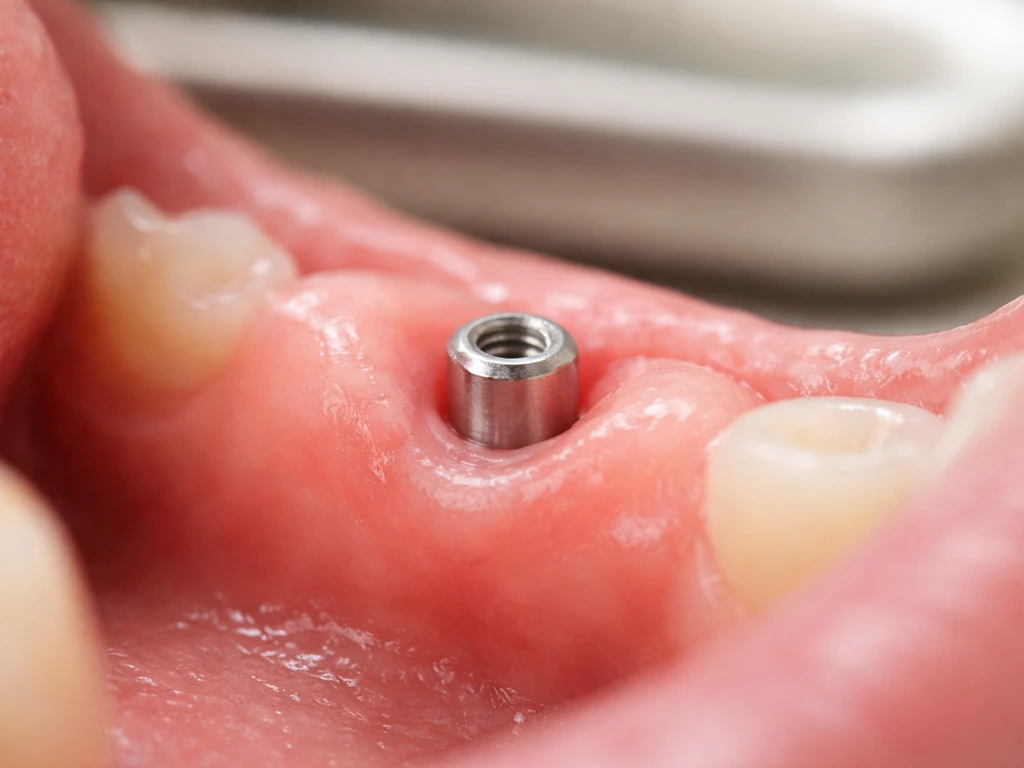
After implant placement, the gum tissue goes through a staged healing process. In the first couple of weeks, swelling and minor recession are completely normal. The tissue is adapting to a foreign surface, the titanium post or the healing cap sitting above the gumline. Over the following weeks, the soft tissue begins to organize around the implant neck and abutment, forming what's called the peri-implant epithelial interface. Histological research shows this interface reaches full biological maturation somewhere between 6 and 12 weeks after surgery. So if your gums still look a little off at week three, that's not panic territory.
The key point is that gum tissue does not fuse to the implant surface the same way it attaches to a natural tooth root. Around a natural tooth, you have a system of connective tissue fibers that actually anchor into the root surface. Around a titanium implant, the soft tissue forms more of a collar or cuff, and the attachment is primarily through a hemidesmosomal seal at the epithelium rather than true fiber insertion. This is why researchers and clinicians describe the healing and regenerative capacity of soft tissue around implants as lower than that around natural teeth.
Healing timeline: what's normal week by week
Longitudinal studies tracking recession and tissue changes after implant placement have followed patients from about one week post-surgery through one month, three months, six months, nine months, and a full year. Here's what that generally looks like in practice:
| Timeframe | What's normal | Possible concern |
|---|---|---|
| Days 1–7 | Swelling, tenderness, mild bleeding, tissue looks puffy or uneven | Heavy bleeding, severe pain, or implant moving |
| Weeks 2–4 | Tissue starting to shrink back to its resting position, possible minor recession | Sudden increase in recession, exposed implant threads |
| Weeks 6–12 | Tissue collar forming around the abutment or healing cap, color evening out | Persistent redness, pus, bleeding when touched lightly |
| 3–6 months | Soft tissue largely stabilized, crown placement period | Grey titanium hue visible through the gum, deepening pockets |
| 6–12 months | Final tissue contour should be stable; check-in with dentist | Continued recession, pain, loosening of the implant |
One thing that surprises a lot of patients: mild recession in the first few months does not mean your implant is failing. It can mean the tissue is just settling. The concern kicks in when recession is progressive, when you can see actual implant surface or threads through the gum, or when there's a grey metallic hue visible beneath thin tissue in the smile zone. These are the signs that something beyond normal healing may be happening.
Can gum grow over the cover screw specifically?
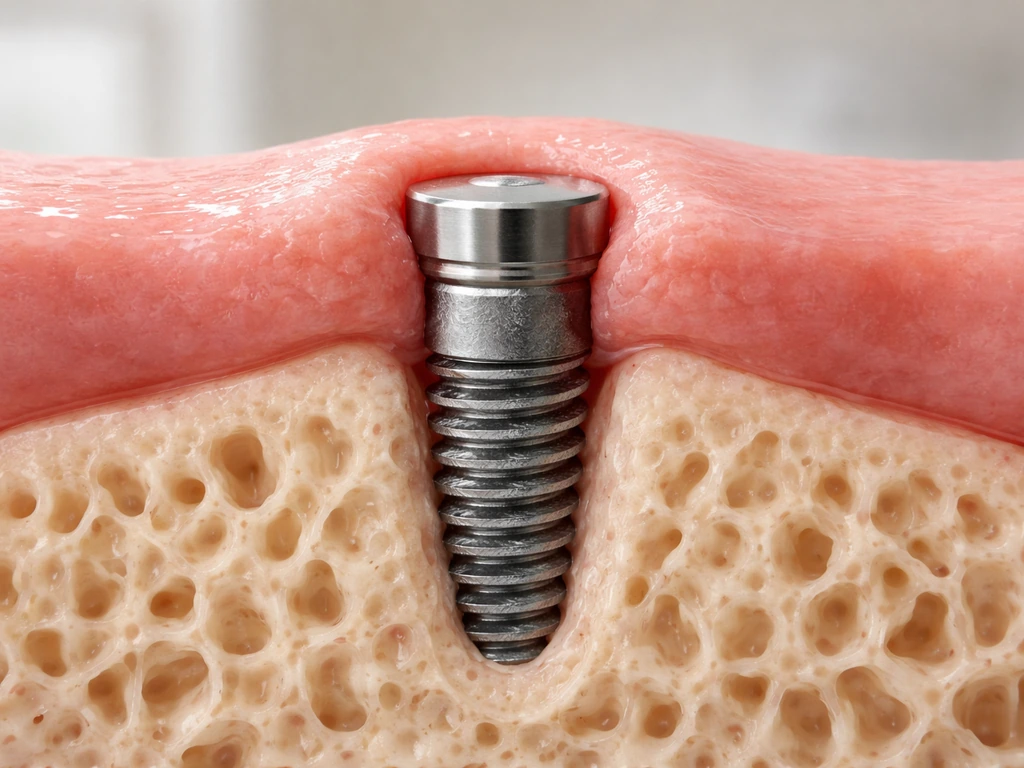
Yes, and this actually happens routinely in two-stage implant protocols. When the implant is placed and then left to integrate with the jawbone over several months, the surgeon places a cover screw flush with or slightly below the gumline, and the tissue grows right over it. That's entirely intentional. When the surgeon re-enters to place the healing abutment, they're cutting through or punching through tissue that has grown over the top of the implant. If you've had a single-stage protocol with a healing abutment sticking up through the gum, the tissue grows around that post rather than over it.
What affects whether gum tissue covers and stays around an implant
Not everyone heals the same way, and a handful of factors significantly affect how well the gum tissue integrates and whether it stays put long-term.
- Gum biotype: people with thick, dense gum tissue (thick biotype) tend to maintain better coverage than people with thin, fragile tissue (thin biotype), which is more prone to recession after any procedure
- Implant depth and position: implants placed too shallow or too far forward in the jaw leave less tissue over the collar; proper three-dimensional positioning is critical for tissue outcomes
- Abutment choice: the shape, height, and material of the abutment affect how the tissue drapes around it; this is a bigger deal in the front of the mouth where aesthetics matter most
- Keratinized mucosa width: having at least 2 mm of keratinized (tough, attached) gum tissue around an implant is associated with better plaque control and lower recession rates long-term
- Inflammation and peri-implantitis: the American Academy of Periodontology describes peri-implantitis as inflammation of the soft tissues combined with bone loss around the implant; this is not just cosmetic recession, it's active disease
- Smoking: research shows smokers have roughly 2.27 times higher odds of developing peri-implantitis compared with non-smokers; smoking impairs blood flow and immune response in the tissue
- Oral hygiene: biofilm buildup around the implant collar is the primary driver of peri-implant mucositis (reversible inflammation without bone loss) that can progress to peri-implantitis if untreated
- Prior gum recession: if you had recession around the natural tooth that was replaced, the tissue architecture in that area is already compromised
What to do right now if you're worried about your gum coverage
If you're in the first few weeks after surgery and the tissue looks uneven or slightly pulled back, take a breath. Monitor it daily and take a photo so you can compare over time. What you're watching for is whether it's improving, staying the same, or getting worse. Tissue that's slowly filling in and looking healthier is reassuring. Tissue that's actively receding week over week is a reason to call.
If you're months out from surgery and something feels off, here are the specific signs that warrant a call to your implant dentist or oral surgeon without delay:
- You can see a grey or metallic color through the gum near the implant site
- The implant shoulder, abutment, or any threaded surface is visibly exposed above the gumline
- The gum bleeds easily when you brush or touch it gently
- There's any discharge or pus around the implant
- The implant itself feels mobile or loose
- Probing depth at your recall appointment is 6 mm or deeper, or you're told there's bone loss on the X-ray beyond what's expected in the first year
When you call, ask specifically whether the recession is within normal healing parameters or whether it meets criteria for a soft-tissue dehiscence. The clinical distinction matters because exposed implant surface is classified as a risk marker for future disease, even if there's no active infection yet.
Treatment options when gums don't cover as expected
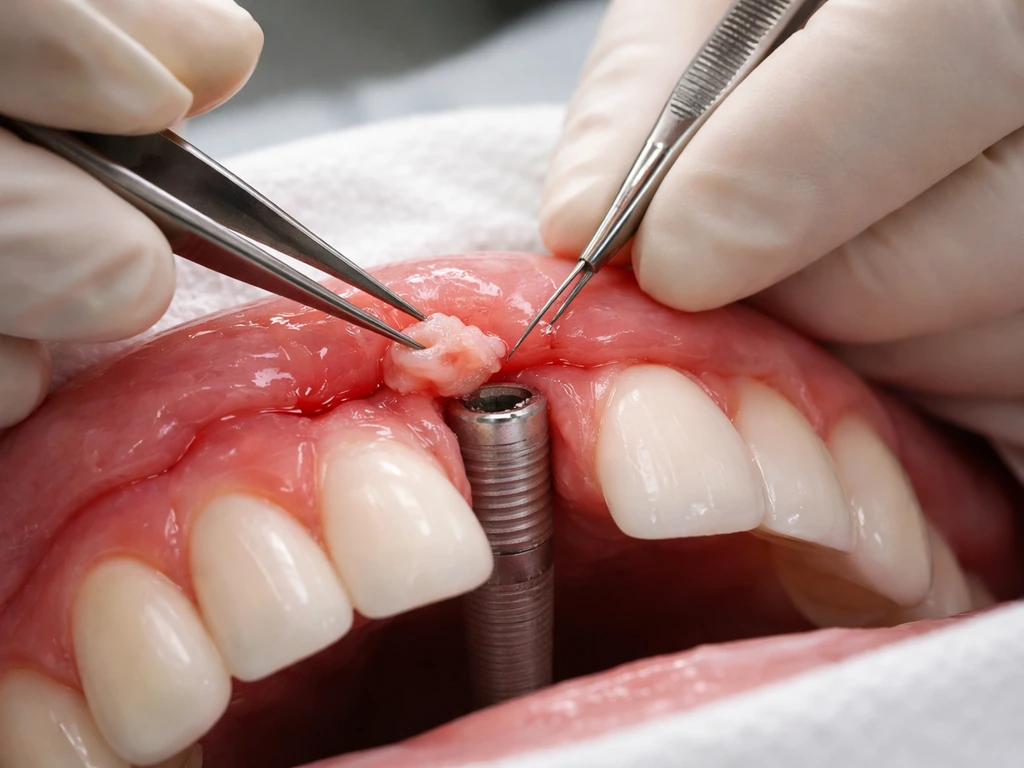
If your gum tissue hasn't grown around the implant the way it should, or if recession has left the implant exposed, there are surgical options that can help. These aren't magic regrowth procedures, they're tissue grafting techniques that physically add or reposition gum tissue around the implant site.
Connective tissue grafts
This is the most common soft-tissue procedure around implants for coverage and thickening. A small piece of connective tissue is taken from the roof of your mouth and placed under the existing gum at the implant site. Research shows connective tissue grafts can reduce mid-buccal recession by around 0.34 mm and increase tissue thickness by roughly 0.66 mm compared with no grafting. Those numbers might sound small, but in the aesthetic zone, a fraction of a millimeter is visible. Evidence also supports that connective tissue grafts yield stable peri-implant soft tissue at medium-term follow-up.
Free gingival grafts
A free gingival graft takes a slightly thicker slice of tissue from the palate and places it directly at the implant site to increase the width of keratinized mucosa. This is particularly useful when an implant has less than 2 mm of tough attached gum around it. Extended follow-up trials show this approach can increase keratinized mucosa width and help stabilize recession and crestal bone levels over 18 months or more. It's especially common in posterior (back) areas of the mouth.
Collagen matrix alternatives
For patients who don't want a second surgical site at the palate, acellular collagen matrix (a processed xenograft material) can be used to augment soft tissue volume. Three-dimensional analysis studies have shown measurable soft-tissue gain with this approach at six-month follow-up, though it's generally considered slightly less predictable than your own palatal tissue.
It's worth noting that there is no single universal protocol for managing facial soft-tissue defects in aesthetic areas. The ITI (International Team for Implantology) has specifically noted that treatment planning here requires case-by-case clinical judgment. So if one surgeon suggests a different approach than another, that doesn't mean someone is wrong.
What gums actually can and can't do after an implant
There's a lot of confusion online about whether gums, bone, and enamel can "grow back" after dental procedures. Here's the honest breakdown specific to implants.
| Claim | Reality |
|---|---|
| Gums grow back after implant surgery | Soft tissue heals and matures around the implant, but it does not regenerate the same fiber-anchored attachment as around natural teeth |
| Gums can cover the cover screw | True. In two-stage protocols this is exactly what happens intentionally |
| Gum tissue can fill in recession on its own over time | Minor recession in the first weeks may partially self-correct; established recession beyond the first couple of months rarely reverses without intervention |
| A gum graft restores 'natural' gum tissue | It provides coverage and thickness but the biological attachment is still different from what surrounds a real tooth |
| Bone lost to peri-implantitis grows back on its own | It does not. Bone loss around implants is largely irreversible without surgical regenerative procedures, and even then outcomes vary |
| Good oral hygiene reverses peri-implant mucositis | Yes, peri-implant mucositis (soft tissue inflammation without bone loss) is considered reversible with improved hygiene and professional cleaning |
| Smoking doesn't affect implant gum healing | It significantly does. Smokers have over twice the risk of developing peri-implantitis |
The broader principle at work here is one this site covers across many dental structures: soft tissue can heal, reattach, and be augmented, but true biological regeneration of specialized dental structures doesn't happen in adults. Enamel doesn't regrow, true periodontal ligament fibers don't re-form around titanium, and established bone loss doesn't reverse spontaneously. What you're working with around an implant is the best approximation your body can create, not a replacement for what was originally there.
This same principle applies whether you're asking about gums growing around a crown, around a bridge, or over a bone graft. The biology is similar: soft tissue adapts and heals, but there are real limits to what it can do without intervention. If you're dealing with a related question about gum changes from orthodontic hardware, or whether gums fill in gaps after tooth loss, the underlying biology follows the same rules. Many people also ask why gums grow over braces, and the same healing and tissue-attachment principles help explain what you’re seeing gum changes from orthodontic hardware.
The bottom line on gum tissue and implants
Gum tissue does grow around dental implants, and it does so predictably during the healing phase. What it can't do is regenerate on demand or reverse established recession without help. If you are asking specifically about gum covering after bone grafting, it follows the same general healing concept: soft tissue can thicken and seal as it matures, but it depends on how the graft site is covered and heals regenerate on demand. If you're in early healing, give it time and monitor closely. If you are wondering, "will my gum grow around my crown," the answer depends on your healing stage and whether enough tissue volume is present to cover the margin. If you're months out and concerned about exposure, grey hue through the gum, or bleeding on gentle touch, that's your sign to call your dentist and ask for a thorough peri-implant evaluation. Catching tissue problems early is always better than waiting, because unlike healing tissue, active disease around an implant doesn't quietly resolve on its own.
FAQ
If gum tissue grows over the cover screw, should I worry if it looks uneven or looks like it is “moving” during the first weeks?
Uneven coverage can happen early as swelling settles and the soft tissue reorganizes, but it should gradually stabilize. A useful check is whether the tissue margin is improving (less visible edges, healthier pink color) rather than steadily pulling back week over week. If you notice persistent bleeding with gentle touch, increasing grey/metal show-through, or worsening recession after the first couple of weeks, contact your implant dentist.
How can I tell normal healing recession from peri-implant tissue problems at home?
Track three things over time using the same lighting and camera angle: the amount of visible implant/abutment (or a grey metallic hue), the trend in bleeding on gentle probing (for example, after rinsing or with a soft brush), and whether the tissue line is progressively lowering. Normal settling tends to slow and then plateau, while concerning patterns continue to worsen despite good hygiene.
Does gum grow around an implant in smokers or people with gum disease, and is the timeline different?
Yes, gum can still heal and form an appropriate soft-tissue seal, but smokers and people with prior periodontal disease have a higher risk of slower, less stable outcomes. In practice, clinicians often monitor more frequently and may recommend earlier soft-tissue procedures if recession starts trending unfavorably, so don’t wait for a “months later” appointment if you see progressive changes.
Will my gum tissue grow back if the implant becomes exposed after healing?
If the implant surface is exposed, it usually cannot be “self-covered” reliably. You generally need a soft-tissue grafting or tissue-repositioning approach to rebuild coverage and reduce the risk marker nature of exposed implant metal. Your dentist will also evaluate for infection or dehiscence, since treatment depends on whether there is underlying peri-implant inflammation.
Is a connective tissue graft always the best option for recession around implants?
Not always. Connective tissue grafts are a common choice for coverage and thickening, but the best plan depends on how much tissue width you have (especially the presence or absence of keratinized mucosa), the location (front versus back), and the defect pattern. For example, if you have less than about 2 mm of attached keratinized tissue, a free gingival graft is often considered because it can increase keratinized mucosa width more directly.
What should I ask my dentist to determine whether my recession meets criteria for soft-tissue dehiscence?
Ask for a peri-implant soft-tissue assessment that includes: whether any implant surface is visible, whether the margin is classified as dehiscence versus “within healing parameters,” and what the clinician sees regarding tissue thickness and keratinized mucosa. Also ask whether probing depth and bleeding are consistent with normal post-healing tissue or suggest ongoing peri-implant inflammation.
If I get a soft-tissue graft, will it grow around the implant the same way it would around a natural tooth?
Grafts can thicken and reposition tissue so you get a more protective seal, but they do not recreate the same specialized fiber attachment pattern found around natural teeth. The goal is improved stability and reduced exposure risk, not true regeneration of the periodontal ligament attachment system.
Can I speed up gum coverage after my surgery, or should I avoid certain actions?
You can’t force biologic attachment to advance faster, but you can avoid setbacks. Common pitfalls include aggressive brushing at the surgical area, using mouthwashes that irritate tissue early on (unless your surgeon directs them), and skipping follow-up visits. Ask your clinician for a specific hygiene and activity plan, since the correct timing and technique can affect soft-tissue stability.
Does the “implant” part matter, like titanium surface finish or implant brand, for whether gum grows around it?
The soft tissue seal behavior is influenced by the overall implant system and how the healing cap or abutment is positioned, but in day-to-day care the bigger drivers are surgical technique, tissue volume, and your biologic risk factors (healing capacity, smoking status, prior periodontal health). Your clinician can explain how your specific implant and connection type influenced the planned soft-tissue coverage.
Is it normal for the gum to look different around an implant versus my natural teeth even after healing?
Yes. Even when healing is successful, the peri-implant interface tends to produce a different soft-tissue architecture than what you have around natural tooth roots. It’s normal for appearance and attachment behavior to differ slightly, but persistent or worsening exposure signs (grey metal show-through, progressive recession, or bleeding on gentle touch) are not something to watch indefinitely.
Learn why gums cover braces and what to do now with hygiene steps, red flags, and orthodontist treatments.
Learn if gums can grow around a dental bridge, what gaps mean, inflammation signs, and next steps to protect abutment te
Find out if gums can regrow over crown margins, what affects recession vs stability, and what steps to take now.

