Yes, you can still get a wisdom tooth erupting at 30, but it is not common and it is not the same thing as growing a brand-new tooth. What is actually happening is that a wisdom tooth that has been sitting in your jaw for years is finally pushing through the gum. That is a very different process from true tooth regeneration, which is not something the human body can do on its own. If you are feeling pressure, pain, or swelling at the back of your mouth at 30, there is a real chance a delayed wisdom tooth is the cause, and it is worth getting checked out.
Can You Grow Wisdom Teeth at 30? What to Expect
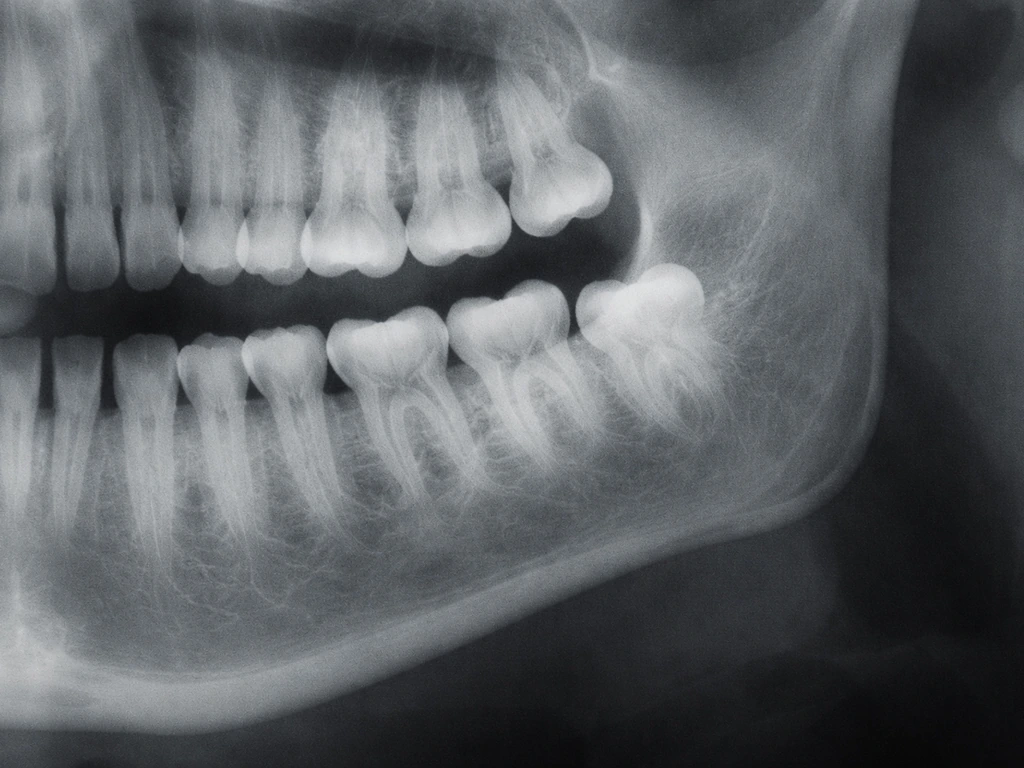
Can wisdom teeth actually erupt after age 30?
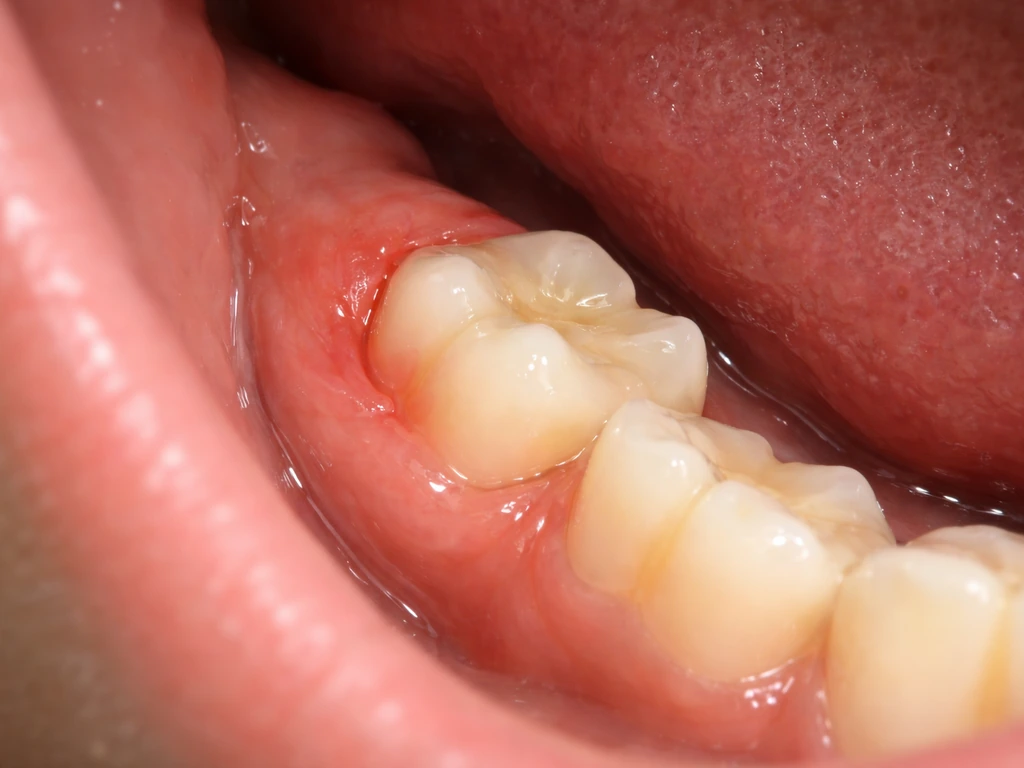
The short biological answer is yes, though it is increasingly rare the older you get. The American Association of Oral and Maxillofacial Surgeons (AAOMS) puts the typical eruption window for third molars between ages 17 and 25. But research on adults aged 25 and older shows that partially impacted wisdom teeth do still exist past that window, and some continue a slow, partial eruption into the early 30s. A retrospective study of adults 25 and older found that the incidence of partially impacted third molars drops notably after age 30, which tells us two things: late eruption is real, but it becomes less and less likely with each passing year.
The key word here is eruption, not regrowth. Tooth eruption is a biological process where a developing tooth moves from inside the jawbone into its functional position in the mouth. If you are experiencing something at 30, the tooth was already there, already formed in the jaw, and is now making its move. Nothing is being generated from scratch.
Typical timing versus what counts as a late eruption
Most people see their wisdom teeth between 17 and 25. For a lot of people, nothing erupts cleanly because there is not enough room, and the tooth becomes impacted. A tooth that is still partially impacted at 25, 28, or even 30 can sometimes continue inching toward the surface, especially if it is only partially blocked. This is different from a tooth suddenly deciding to grow at 35 out of nowhere. By 30, most of the tooth's root development is already complete, and the window for eruption is closing fast. AAOMS notes that it is not always possible to predict eruption of third molars in all cases, which is why imaging is so important. Some teeth that look dormant on an X-ray at 25 can show subtle movement over the following years.
Why some wisdom teeth erupt late
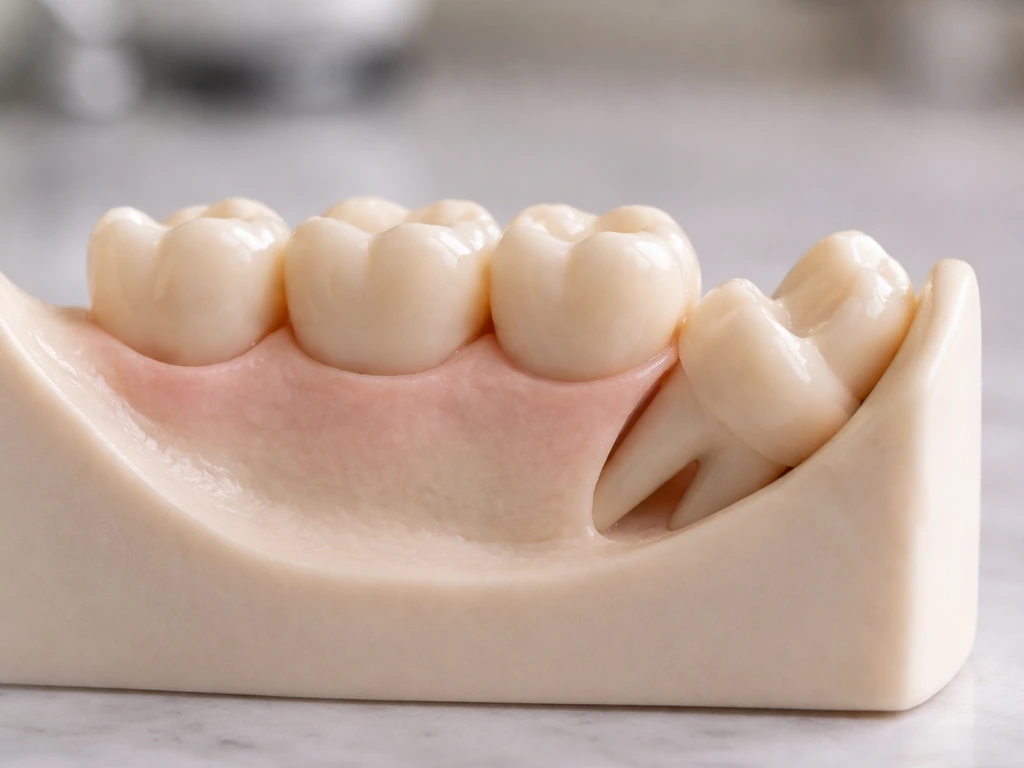
Several factors determine whether a wisdom tooth erupts early, late, or not at all. Genetics plays a huge role. Some people are simply wired to have slower jaw development or third molars that are positioned in ways that make them slower to move. The amount of space at the back of the jaw is probably the most critical factor. If there is a tight arch with little room, the tooth will not push through, or it will only partially do so. Tooth angulation matters too. A wisdom tooth tilted sideways or angled toward the second molar faces a literal physical barrier and is far more likely to stay stuck. AAOMS specifically identifies tooth angulation and degree of root development as key parameters in assessing whether a third molar is likely to erupt.
- Genetics and jaw size: smaller jaws leave less room for third molars to emerge
- Tooth angulation: mesially or horizontally angled teeth are more likely to stay impacted
- Root development stage: eruption is driven partly by how fully the roots have developed
- Available space at the back of the arch: crowding from earlier teeth can block the path
- Partial impaction status: some teeth partially emerge and then stall, sometimes for years
Signs you might have a wisdom tooth coming in at 30
The symptom pattern for a late-erupting wisdom tooth is pretty recognizable once you know what to look for. The most common is a dull, persistent ache or pressure at the back of the jaw, behind your second molars. You might notice swelling or tenderness in the gum tissue back there. If the tooth is only partially through the gum, a flap of tissue called an operculum can form over it, and food and bacteria get trapped underneath. That leads to pericoronitis, an infection of the soft tissue around a partially erupted tooth. Pericoronitis causes pain, swelling, a bad taste in the mouth, and sometimes discharge. The Mayo Clinic and Cleveland Clinic both describe this pattern clearly: bacteria and food debris get caught between the gum flap and the tooth, triggering inflammation that can escalate quickly.
Here is a practical checklist of signs worth paying attention to:
- Dull aching pressure at the very back of the jaw, upper or lower
- Swollen, red, or tender gum tissue behind your last visible molar
- Jaw stiffness or difficulty opening your mouth wide
- A bad taste or smell coming from the back of your mouth
- Visible white tissue or a small bump starting to peek through the gum
- Earache or headache on one side with no other obvious cause
- Pain when chewing that seems centered at the back of the mouth
A note on urgency: if you have swelling that is spreading toward your throat or neck, difficulty swallowing, or a high fever alongside jaw pain, that is not a wait-and-see situation. Get to an emergency dentist or urgent care the same day. Dental infections can escalate into serious medical emergencies faster than most people expect.
What to actually do next: exam and imaging
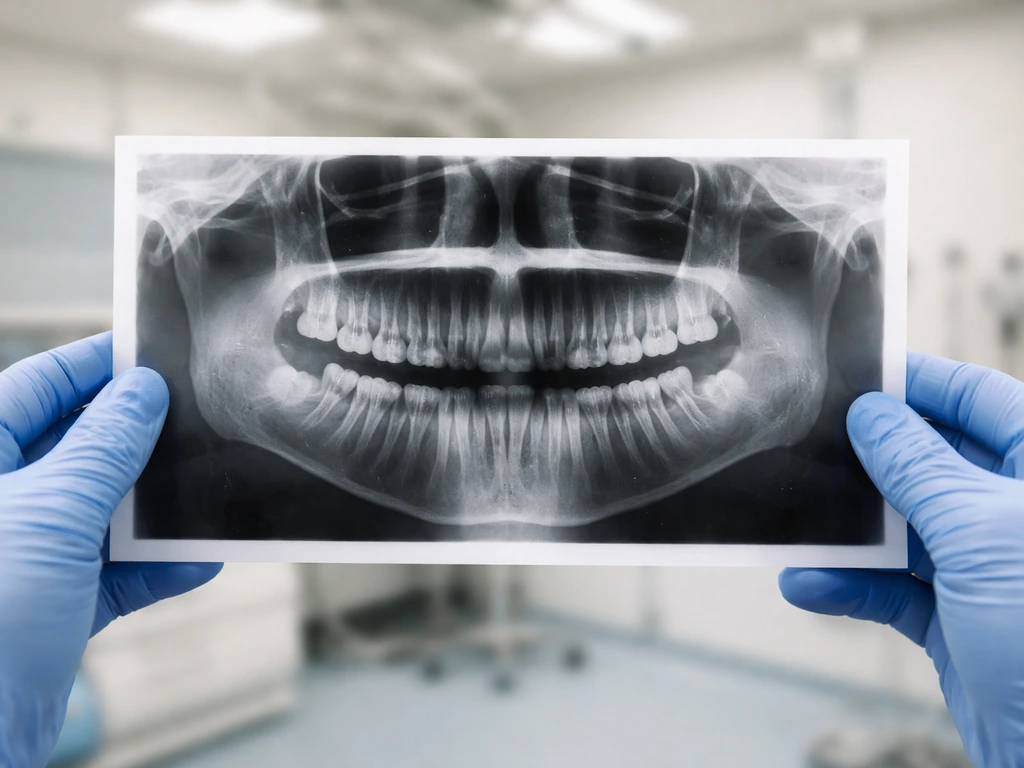
If you suspect a wisdom tooth is trying to come through, the single most useful thing you can do is get a dental exam and a panoramic X-ray. A panoramic radiograph gives the dentist a full picture of all your teeth, including the ones still inside the bone. AAOMS identifies the panoramic radiograph as the standard imaging technique for evaluating third molars, and their 2024 clinical paper on impacted third molars confirms it is the most commonly accepted imaging modality for this assessment. From that image, your dentist can see exactly where the tooth is sitting, what angle it is at, how developed the roots are, and how close it is to nerves or adjacent teeth.
In some cases, particularly when the wisdom tooth's roots appear close to the inferior alveolar nerve in the lower jaw, your dentist or oral surgeon may recommend a cone beam CT scan (CBCT) for more detailed 3D imaging. This is not routine for everyone. The European Academy of Dentomaxillofacial Radiology recommends CBCT only when the panoramic image leaves a specific clinical question unanswered, such as the precise relationship between the tooth root and the nerve. Do not be alarmed if your dentist sticks with just the panoramic to start. That is appropriate for most cases.
Your options if the wisdom tooth is stuck or causing problems
Once you have imaging, the decision usually comes down to two paths: monitor or remove. Neither is automatically right. It depends on what the tooth is doing and how much trouble it is causing.
Watchful monitoring
If your wisdom tooth is fully impacted, not infected, not causing damage to the neighboring tooth, and not showing any cystic changes around it, monitoring is a reasonable approach. NICE (the UK's National Institute for Health and Care Excellence) has specifically stated that there is no reliable evidence supporting the prophylactic removal of healthy, disease-free impacted wisdom teeth. The Cochrane review on this question reached similar conclusions, noting that evidence is uncertain and that routine removal of asymptomatic teeth is not clearly justified. Monitoring means checking the tooth at regular intervals with imaging to make sure nothing is changing for the worse.
Treatment and removal
Removal becomes the more logical choice when the tooth is causing repeated infections (pericoronitis), is damaging the root of the adjacent second molar, has developed a cyst or tumor around it, or cannot be kept clean enough to avoid decay. AAOMS lists pain, acute or chronic infection, periodontal disease, and cystic lesions as common clinical indications for extraction. If you have had two or more bouts of pericoronitis from the same tooth, most oral surgeons will recommend removal rather than continuing to treat each episode as a one-off.
For mild pericoronitis without spreading infection, the first-line approach is usually local debridement, which just means the dentist cleans out the pocket under the gum flap and irrigates it. In some cases, the soft tissue flap (operculum) covering the tooth can be surgically removed, which eliminates the pocket where bacteria were collecting and can allow the tooth to continue erupting if there is enough room. Antibiotics are not the default for mild cases. They are reserved for when the infection shows signs of spreading.
If removal is the path, it is worth knowing the real risks going in. Dry socket is one of the more common post-extraction complications. If your wisdom tooth roots are near the inferior alveolar nerve, nerve injury is a known risk, though it is relatively uncommon in straightforward cases. For high-risk situations where the roots are very close to the nerve, a procedure called coronectomy (removing only the crown of the tooth and leaving the roots in place) can reduce nerve injury risk significantly. A systematic review reported nerve injury rates of around 0.5% for the inferior alveolar nerve with coronectomy in successful cases, compared to higher risks with full extraction in difficult nerve-proximity situations.
| Scenario | Likely Recommendation | Key Consideration |
|---|---|---|
| Fully impacted, no symptoms, no damage to adjacent tooth | Monitor with periodic X-rays | Evidence does not support prophylactic removal |
| Partially erupted with recurring pericoronitis | Removal | Repeated infection episodes outweigh risks of extraction |
| Partially erupted, first episode of pericoronitis | Clean the area, possible operculum removal, reassess | See if tooth can fully erupt or if infection recurs |
| Impacted with cyst or damage to second molar root | Removal | Active pathology requires intervention |
| Roots very close to inferior alveolar nerve | Removal with possible coronectomy | Nerve proximity increases injury risk with full extraction |
Let's clear up the regrowth myth
This comes up a lot, so it is worth addressing directly. A wisdom tooth erupting at 30 is not the same as a tooth regrowing. The tooth already existed inside your jaw. It was always there, sitting in bone, formed during development. Eruption is just the process of it moving into the mouth. It does not mean teeth can regenerate on demand.
True tooth regeneration, meaning the biological restoration of enamel, dentin, pulp, or a whole tooth from scratch, is not something the human body can do once adult teeth are in place. Enamel is the clearest example. Once the cells that produce enamel (ameloblasts) are lost after a tooth erupts, they are gone. Enamel cannot repair or regenerate itself. Research published by RSC Publishing confirms this directly: enamel lacks natural regenerative capacity after eruption. Experimental research is exploring biomaterial-based approaches to tooth regeneration, but nothing that amounts to regrowing a complete functional tooth is available clinically today.
What does happen after an extraction is healing of the socket, which involves bone remodeling and soft tissue closure over weeks and months. Some people misread this as evidence that something tooth-like is regenerating in the space. It is not. The bone remodels, the socket closes, and sometimes bone volume is even lost over time. Nothing grows back in the form of a tooth.
If you are exploring related questions about wisdom tooth timing, the picture is pretty consistent: eruption is developmentally time-limited, and whether it happens at 20, at 25, or into your early 30s depends on individual anatomy and how much room exists in the jaw. The biology of late eruption in your 30s is closely related to what drives delayed eruption through the mid to late 20s, and both are distinct from what happens with eruption in your 40s, which is quite rare. Because wisdom teeth erupting in your 40s is quite rare, symptoms at that age still deserve an exam and imaging to confirm what is going on eruption in your 40s. In all cases, the mechanism is the same: an existing tooth either erupts or it does not, based on physical conditions in the jaw.
The bottom line
If you are 30 and feel like something is happening at the back of your jaw, do not dismiss it. A wisdom tooth that has been quietly sitting in your bone for years can still push through, especially if it was only partially blocked. It is not common past 30, but it happens. Late wisdom tooth eruption can happen, but it is uncommon and becomes less likely with age past 30. Get a dental exam and a panoramic X-ray. That one step tells you everything: whether the tooth is there, where it is positioned, and whether it is something to watch or something to remove. Do not wait on symptoms like recurring infection or spreading pain. Those are clear signals that the tooth is not going to sort itself out.
FAQ
If I’m 30 and I feel pain back there, how can I tell it’s a late wisdom tooth and not something else?
A wisdom-tooth pattern usually centers on a specific location behind the second molar and comes with gum tenderness in that same area. If the pain is accompanied by tooth-cavity symptoms in a nearby molar, recent dental work sensitivity, or pain that worsens strongly when biting on a particular tooth, the cause may be different. A dental exam plus a panoramic X-ray is the practical way to confirm whether there’s an erupting or partially impacted third molar versus another source (like decay or a periodontal pocket).
Can a wisdom tooth at 30 start erupting suddenly, or should it be gradual the whole time?
Most late eruptions are gradual, even if the symptoms start suddenly. The gum and surrounding tissue can become inflamed once the tooth reaches a point where food and bacteria trap under a gum flap, which can make it feel like it began abruptly. If symptoms flare repeatedly in the same spot, that often points to recurring pericoronitis rather than a random new problem.
Is it safe to “wait and see” for a wisdom tooth eruption at 30?
Waiting can be reasonable when the tooth is not causing infections, is not damaging the adjacent second molar, and imaging does not show cystic changes. The key is having a defined monitoring schedule, using repeat imaging if your dentist recommends it. If you already have recurrent pericoronitis, worsening swelling, or evidence of damage to the neighboring tooth, waiting usually increases the odds you will end up needing extraction under less ideal conditions.
How often would I need follow-up if I’m monitoring a partially erupted wisdom tooth?
There is no one universal interval, but many clinicians use follow-ups based on your symptoms plus what imaging shows about space, angulation, and whether the operculum is forming. If you have any intermittent pain or gum flare-ups, the monitoring period is typically shorter. Ask your dentist to set a schedule and to specify triggers for urgent re-evaluation (for example, fever, spreading swelling, or difficulty swallowing).
What treatments can reduce symptoms right now if I can’t get in for an exam immediately?
For suspected mild pericoronitis, rinsing gently with warm salt water can help with comfort, and keeping the area as clean as possible can reduce trapped debris. However, if there is significant swelling, bad taste with discharge, or worsening pain, home care is not a substitute for drainage and cleaning under the gum flap when needed. Antibiotics are not usually the first step for mild cases, so delaying an assessment may mean missing the chance for local debridement.
Do I need a cone beam CT (CBCT) at 30, or is a panoramic X-ray enough?
A panoramic radiograph is usually the starting point because it shows tooth position, angulation, and general root development. CBCT becomes more relevant when there is a specific uncertainty on the panoramic image, such as the precise relationship between lower wisdom tooth roots and the inferior alveolar nerve. If your dentist is considering extraction and nerve proximity is a concern, CBCT may help with planning, but it is not routine for every case.
If my wisdom tooth is close to a nerve, does that mean I must choose coronectomy?
Not necessarily. The choice depends on how close the roots appear to be to the nerve, whether the tooth is infected, and whether the roots are fully formed or positioned in a way that makes full removal riskier. Coronedectomy can reduce nerve injury risk in selected situations, but it is still a procedure with its own considerations, including the need for follow-up of the retained roots. Your oral surgeon can explain which option fits your specific imaging findings.
What signs mean the infection is spreading and I should go the same day?
Go urgently if swelling is spreading toward your neck or under the jaw, you have difficulty swallowing, you cannot open your mouth normally (trismus), or you develop a high fever with increasing jaw pain. These can be early signs of a deeper or spreading infection where waiting could be unsafe.
Will extraction at 30 be more difficult than extraction at 20?
It can be. By the early 30s, many wisdom tooth roots are more developed and the tooth is more likely to be firmly positioned, which can make extraction technically more challenging. That said, difficulty varies widely by tooth angulation, depth, and how close the roots are to nerves and adjacent teeth. Pre-op imaging and an experience-matched surgeon or oral surgeon matter as much as age.
Can my wisdom tooth eruption cause problems with my second molar?
Yes, it can. A partially impacted wisdom tooth can create a hard-to-clean area, increasing risk of decay or gum disease around the neighboring second molar. It can also apply pressure and contribute to periodontal issues at that site. If imaging suggests contact or damage, dentists often recommend extraction sooner rather than later.
Can wisdom teeth erupt in your 40s? Learn late eruption signs, risks, and dentist options to monitor or extract.
Can wisdom teeth erupt in your 20s? Learn signs, diagnosis with X-rays, and when extraction is needed.
Can wisdom teeth erupt in your 30s? Learn symptoms, timing, how dentists confirm, and when extraction is needed.

