No, tooth nerves cannot grow back in adults once the pulp tissue inside the tooth dies or is removed. The nerve supply to your tooth is part of the dental pulp, a soft tissue living inside the tooth, and mature human pulp has almost no ability to regenerate after it becomes necrotic. There is one meaningful exception: in children and teenagers with immature teeth whose roots haven't fully formed yet, a procedure called revascularization can sometimes encourage new tissue to grow into the empty pulp space. In other words, while bone around tooth roots may remodel somewhat, the pulp nerve tissue itself does not truly regrow once it has died. But for most adults asking this question after a toothache, a crack, or a cavity that went too deep, the honest answer is that the nerve is not coming back on its own, and waiting usually makes things worse.
Can Teeth Nerves Grow Back? What Happens After Damage

What "tooth nerves" actually are (and why it matters)
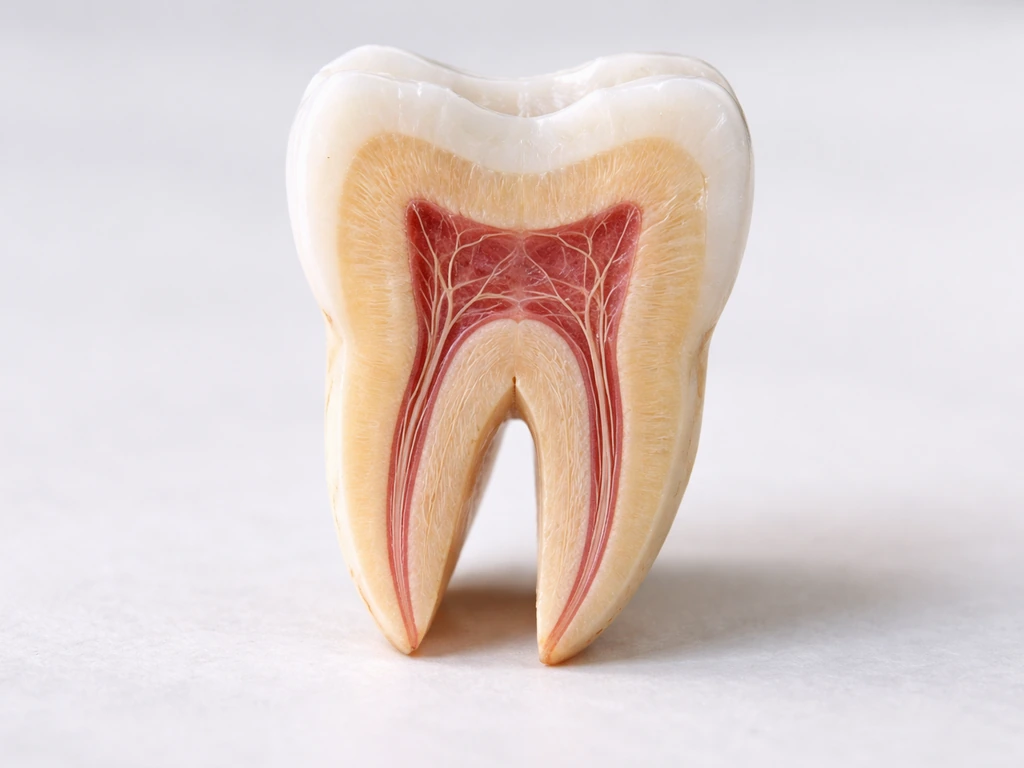
When people say "tooth nerve," they usually mean the dental pulp, the soft connective tissue that fills the pulp chamber in the center of the crown and runs down through the root canals. The pulp is richly stocked with blood vessels and two types of nerve fibers: sensory fibers that fire pain and temperature signals up through the trigeminal nerve to your brain, and autonomic (sympathetic) fibers that regulate blood flow inside the tooth. The pulp's blood supply enters and exits through a tiny opening at the tip of each root called the apical foramen.
This matters because the nerve fibers inside your tooth are not isolated cables you can splice back together. They are part of a living tissue system. When the pulp dies, the entire vascular and nerve supply collapses together. You can't lose the blood supply and keep functioning nerves, or vice versa. Pulp vitality and nerve health are the same thing in practice, which is why dentists talk about "pulp vitality" rather than specifically "nerve health."
It's also worth separating this from related questions about other tooth structures. Enamel, dentin, and the bone around tooth roots are all different tissues with their own regeneration limitations. Dentin has a limited ability to form a secondary protective layer, and bone around teeth can sometimes remodel, but the nerve tissue inside the pulp is on a separate track entirely and has far less repair capacity than any of those.
Can tooth nerves grow back? The honest answer depends on these factors
Whether any recovery is possible hinges on three things: your age, the state of root development, and how far along the pulp damage actually is. These aren't minor details; they completely change the clinical picture.
Reversible pulpitis: the pulp is irritated, not dead
If you have a short, sharp zing when you drink cold water that disappears within a few seconds, you may have reversible pulpitis. The pulp is inflamed but still vital. In this case, removing the irritant, usually sealing a cavity or covering exposed dentin, can allow the pulp to settle back down. The nerve fibers don't technically "regrow," but they were never destroyed in the first place. Treating reversible pulpitis early is one of the best things you can do to protect your tooth long-term.
Irreversible pulpitis: inflamed past the point of no return
When pain lingers for more than a few seconds after a cold stimulus, comes on spontaneously, wakes you up at night, or becomes impossible to pinpoint, the pulp has crossed into irreversible pulpitis territory. The tissue is severely inflamed and heading toward necrosis. At this stage, the pulp cannot heal itself, and nerve regeneration is not on the table. The AAE's clinical diagnostic guidelines are clear that irreversible pulpitis requires endodontic treatment, either a pulpotomy (removing the inflamed coronal portion) or a full root canal. Some case-selected patients with irreversible pulpitis can be managed with pulpotomy if the remaining root-canal pulp is still viable, but that's about preserving what's left, not regrowing what's damaged.
Pulp necrosis: the nerve is gone
Once the pulp is fully necrotic, there is no nerve tissue left to regenerate, and the blood supply that would carry any repair cells is gone too. Because the nerve cannot regrow once the pulp is necrotic, can teeth roots grow back is sometimes only relevant in specific immature-tooth situations. Interestingly, a dead tooth doesn't always hurt; the pain actually stops when all the nerve tissue dies. But the infection risk doesn't stop. Bacteria can colonize the empty pulp space and spread into the surrounding bone, which is why pulp necrosis needs treatment even when it feels like the problem resolved itself.
The exception: immature teeth in kids and teens
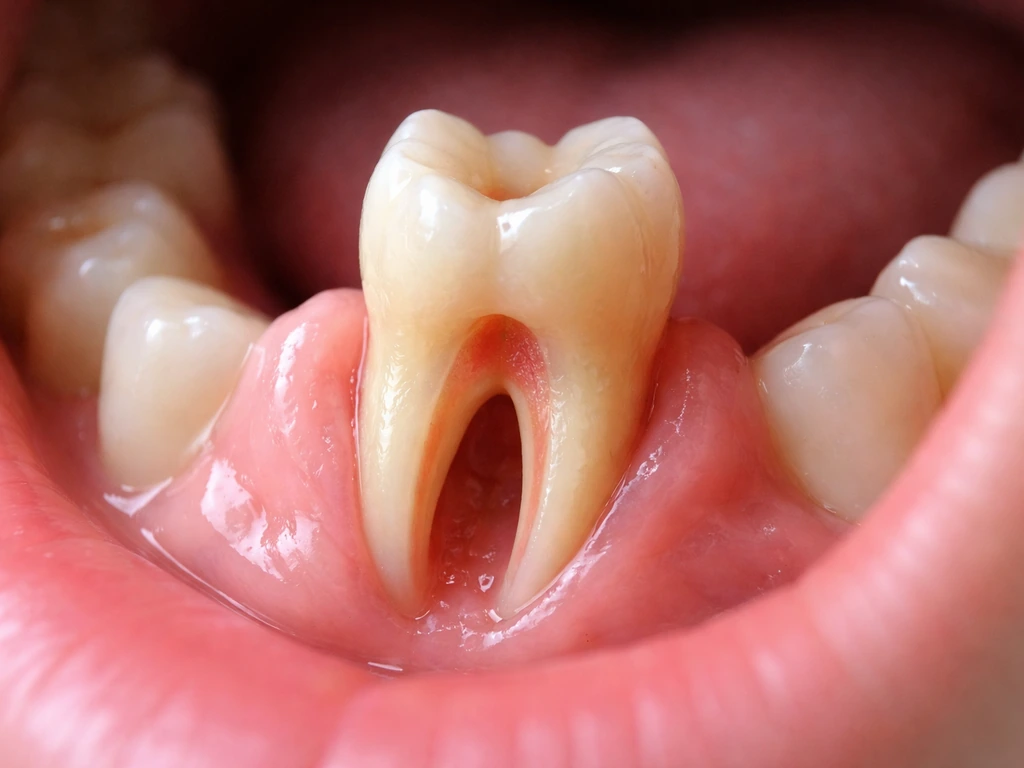
Here's where the answer shifts. In children and adolescents whose permanent teeth haven't finished forming, the root tip (apex) is still wide open. This wide-open apex means a blood clot and stem cells from the surrounding tissues can potentially be guided into the pulp space through a procedure called regenerative endodontics or revascularization. The AAE's current position statement on regenerative endodontics confines this approach specifically to immature permanent teeth with necrotic pulp, because the biology simply doesn't work the same way once roots are fully formed. Studies show the approach has meaningful success rates, though outcomes depend heavily on the protocol used, with delayed induction approaches outperforming immediate ones in some clinical comparisons. What grows back isn't a perfect replica of the original pulp, but new tissue can allow the root to continue developing and the tooth to survive long-term.
Age also matters in a subtler way for adults: pulp innervation naturally decreases over time, and older teeth have less pulp tissue and less nerve density even in healthy mouths. This doesn't mean older adults lose teeth faster, but it does mean a mature tooth with reduced pulp has even less capacity for repair than a young adult's tooth.
Signs you might have a dead or dying nerve
Nerve damage progresses through a fairly recognizable pattern, though not everyone experiences every stage. If you notice any of the following, it's worth getting a dental appointment soon rather than waiting to see if it resolves.
- Lingering tooth pain after hot or cold that lasts more than 30 seconds after the stimulus is removed
- Spontaneous tooth pain that arrives without any obvious trigger, especially at night
- A tooth that used to be sensitive but has suddenly stopped hurting entirely (this can mean the pulp has died, not that the problem fixed itself)
- Visible darkening or graying of a tooth, particularly after an injury
- A pimple-like bump on the gum near a tooth (this is a sinus tract draining an abscess)
- Swelling in the gum, jaw, or face near a specific tooth
- Tenderness when biting or tapping on the tooth
- A persistent bad taste that doesn't go away after brushing
It's worth knowing that pulp necrosis can be completely silent. Some people walk in for a routine checkup and get the news that a tooth is dead, with no pain history at all. Early radiographic changes like a slightly widened periodontal ligament space around the root tip can be the only clue, which is one reason regular X-rays matter even when nothing hurts.
How dentists confirm nerve health today
Dentists use a combination of clinical tests and imaging to figure out exactly what's happening inside the pulp before deciding on treatment. The goal is to match the right diagnosis to the right care, since the treatment for reversible pulpitis looks very different from the treatment for full necrosis.
Pulp sensibility tests
Cold tests (using a refrigerant spray or ice) and electric pulp tests are the most common ways to assess pulp nerve function. Both measure whether the sensory nerve fibers inside the tooth are still responding to stimulation. An electric pulp test has been shown to detect non-vital teeth with very high accuracy, around 100% in some study models, and vital teeth at roughly 96%. The key distinction is that these tests measure nerve fiber activity, not blood flow, so they confirm whether the nerve is still functioning, not whether the pulp tissue is totally healthy.
Vitality tests
True vitality testing measures blood flow rather than nerve response, using technologies like pulse oximetry or laser Doppler flowmetry. These are more specialized and not available in every dental office, but they give a cleaner picture of whether the pulp is still vascularized and alive as a tissue.
X-rays and CBCT
Periapical X-rays look for tell-tale signs of pulp disease around the root tip: a widened periodontal ligament space, loss of the lamina dura (the thin white line of dense bone around the root), or a dark shadow (radiolucency) indicating bone loss from an abscess. These changes often lag behind the actual disease by weeks or months, which means a normal-looking X-ray doesn't guarantee a healthy pulp. Cone-beam CT (CBCT) gives a three-dimensional view and can detect early bone changes that flat X-rays miss entirely.
Treatment options when nerves can't regenerate
If your pulp is past the point where it can recover on its own, the goal shifts from regeneration to either preserving remaining vital tissue or eliminating the damaged tissue and sealing the tooth. Here's how the main options stack up:
| Diagnosis | Typical Treatment | What It Does | Tooth Survival Outlook |
|---|---|---|---|
| Reversible pulpitis | Remove irritant, restore tooth | Lets inflamed but living pulp settle | Good if treated promptly |
| Symptomatic irreversible pulpitis | Pulpotomy or root canal therapy | Removes inflamed/necrotic pulp, seals canals | Good with crown restoration |
| Pulp necrosis (no abscess) | Root canal therapy | Cleans and seals empty pulp space | Good with prompt treatment |
| Pulp necrosis with abscess | Root canal + possible drainage or extraction | Eliminates infection source | Depends on bone/tissue loss |
| Immature tooth with necrotic pulp (child/teen) | Regenerative endodontics (revascularization) | Encourages new tissue growth, continued root development | Good in selected cases |
Root canal therapy and crowns
Root canal therapy removes all pulp tissue from the chamber and canals, shapes and cleans the space, and fills it with a rubber-like material called gutta-percha. The tooth is then sealed and almost always needs a crown afterward, because a tooth without a pulp becomes more brittle over time and is much more likely to crack without protection. Root canal-treated teeth can last decades with the right restoration, and modern techniques make the procedure far less uncomfortable than its reputation suggests.
Pulpotomy as an alternative for some irreversible pulpitis cases
Pulpotomy removes only the pulp in the crown portion of the tooth while leaving the root canal pulp intact (if it's still healthy). Recent evidence and cost-effectiveness analyses show that pulpotomy can be a clinically reasonable alternative to full root canal treatment in carefully selected mature permanent teeth with irreversible pulpitis, offering comparable outcomes in some cases at lower cost and treatment time. However, case selection matters significantly, and it isn't appropriate for every situation.
Vital pulp therapy and direct pulp capping
For teeth with deep cavities where the pulp is just barely exposed, direct pulp capping involves placing a protective biocompatible material (often mineral trioxide aggregate or calcium silicate cement) directly over the exposed pulp to encourage it to wall itself off with a dentin bridge. Dentin does not grow back in the way nerves can be discussed, so protecting remaining tooth structure is key dentin grow back. This works best in true reversible pulpitis, though some research suggests it can be attempted even in borderline irreversible cases with careful patient selection. Vital pulp therapy broadly refers to any approach that tries to keep the pulp alive rather than removing it.
When regeneration actually is possible
Regenerative endodontics is the real-world closest thing we have to regrowing a tooth nerve, and it's genuinely promising for the right patients. The procedure targets immature permanent teeth in children and teenagers where the root apex is still open (this is called an open apex or incomplete root formation). In these cases, the pulp space can be disinfected with antibiotics and irrigants, and then a blood clot is deliberately induced inside the canal by irritating the periapical tissue. This clot, along with stem cells from the surrounding tissues, can organize into new tissue inside the root, allowing the root walls to thicken and the apex to close.
The AAE explicitly frames this as targeting the pulp-dentin complex rather than promising full nerve regeneration, and the new tissue that grows in isn't identical to original pulp. But it works well enough to save teeth that would otherwise need extraction or a static, non-developing root canal filling, which in a growing child is a significant win. If your child's dentist or endodontist mentions revascularization after a traumatic tooth injury or severe infection in a young permanent tooth, this is the procedure they're describing.
Outside of the immature-tooth scenario, there is ongoing research into pulp-like tissue engineering and stem cell-based approaches, but as of today these remain experimental and are not standard clinical practice. Don't let internet enthusiasm about "regrowing tooth nerves" convince you to wait on treatment while hoping for a breakthrough.
What to do right now
Assess your urgency
If you have facial swelling, difficulty swallowing or breathing, fever alongside dental pain, or swelling that's expanding rapidly, go to an emergency room or urgent care dentist today. These are signs that a dental infection is spreading beyond the tooth and can become dangerous quickly. For most other cases, including throbbing pain without swelling, a dead tooth discovered on X-ray, or lingering sensitivity, call your dentist and ask for the first available appointment. Don't book a routine cleaning slot; let them know it's an active concern.
Managing pain while you wait
For adults, ibuprofen is generally the most effective OTC option for dental pain because it addresses both pain and inflammation. The ADA's acute dental pain guidelines support ibuprofen, naproxen, or combinations with acetaminophen as interim measures. Safe daily limits are up to 2,400 mg ibuprofen, 4,000 mg acetaminophen (lower if you drink alcohol or have liver concerns), or 660 mg naproxen sodium twice daily. For children, the ADA guideline specifically recommends ibuprofen alone or naproxen alone as first-line options. Always follow the dosing instructions on the package and check with a pharmacist if you have any health conditions. Pain medication buys you time to get to the dentist; it doesn't treat the underlying problem.
What to expect after treatment
After a root canal, it's normal to have tenderness in the surrounding gum tissue for a few days, especially if there was an abscess. This isn't the nerve coming back; it's normal post-procedure inflammation. That is why teeth typically do not regrow their nerve tissue after it dies, even if symptoms improve why teeth don't grow back. Teeth usually do not regrow the nerve after grinding either, so any deep damage still needs timely dental evaluation why teeth don't grow back. Most people can manage it with the same OTC pain relievers used before treatment. The tooth itself won't feel temperature or pain sensations anymore once the pulp is removed, which can feel strange at first but is completely normal. Get the permanent crown placed promptly after the root canal, because an unrestored root-canal tooth is vulnerable to fracture.
How to protect your tooth nerves and avoid getting here again
Most pulp damage is preventable. Deep cavities and cracks are the two most common routes bacteria and irritants use to reach the pulp, and both are largely controllable with consistent habits and regular dental visits. Catching a cavity when it's still small means it never gets anywhere near the nerve. Catching a crack before it extends into the pulp preserves the tooth. Here's what actually makes a difference:
- Brush twice daily with a fluoride toothpaste and floss once daily to reduce the bacterial load that causes cavities
- Don't skip dental X-rays; they catch decay and early bone changes around roots long before symptoms appear
- If you grind your teeth at night, wear a night guard, because grinding cracks enamel and can traumatize the pulp over time
- Treat tooth sensitivity early rather than waiting; short sharp sensitivity is often reversible pulpitis, which is fixable without a root canal
- After any tooth trauma (a fall, a hit to the mouth, a cracked tooth from biting something hard), see a dentist within 48 hours even if it doesn't hurt, because pulp damage from trauma can take weeks to fully declare itself
- For children, prompt treatment of deep decay in baby and young permanent teeth protects the developing pulp and root; don't assume a baby tooth cavity "doesn't matter" since the pulp infection can affect the permanent tooth underneath
- Limit acidic and sugary foods and drinks, which erode enamel and expose the dentin layer closer to the pulp
The pulp's blood supply and nerve fibers are what keep a tooth alive and responsive. Once that tissue is gone in a mature tooth, no supplement, oil, rinse, or home remedy is going to bring it back. What you can do is protect what you still have, act quickly when something feels wrong, and get a clear diagnosis from a dentist so you know exactly which treatment path makes sense for your specific situation.
FAQ
If a tooth stops hurting after a cavity or crack, does that mean the nerve is healing?
Not necessarily. Pain can fade when the pulp becomes necrotic, meaning the nerve tissue is no longer functioning. The tooth still may have an infection risk in the root area, so you still need an exam and X-rays to confirm vitality and rule out abscess.
Can the dentist save the nerve without doing a root canal?
Sometimes. If symptoms fit reversible pulpitis, treating the cause (like sealing an exposed area or covering dentin) may allow the pulp to settle. For irreversible pulpitis in selected mature teeth, pulpotomy may be an option, but the decision depends on tests showing enough healthy root-canal pulp remains.
Do electric pulp tests and cold tests prove the pulp is healthy?
They show whether nerve fibers are responding to stimulation, which is different from whether the pulp tissue is fully healthy. A tooth can respond to tests yet still have inflammation, or it can fail tests even if the surrounding bone findings have not fully changed. Dentists combine test results with imaging for a better diagnosis.
How urgent is it to treat irreversible pulpitis or a necrotic tooth?
If you have spontaneous pain, pain that wakes you at night, or pain that lingers beyond cold sensitivity, treatment is usually urgent to prevent the infection from spreading into the tissues around the root. Waiting weeks can increase the chance of an abscess and may make the eventual treatment more complex.
What does regenerative endodontics require, and why can’t adults usually get it?
It works best when the tooth is still developing, typically with an open apex and incomplete root formation. The open tip lets a blood clot and stem cell activity from surrounding tissues contribute to continued root development. Once roots are fully formed, the biology is too constrained, so outcomes are not comparable to immature-tooth cases.
After a root canal, can the tooth still get nerve pain or feel temperature later?
Usually no. With the pulp removed and the canals sealed, the tooth is not expected to respond normally to cold or heat. If sensitivity returns later, it often points to issues like a crack, a failed seal, or persistent infection, not nerve regrowth.
Is it ever possible for a root-canal-treated tooth to “feel” pain years later?
Yes. Pain years later can come from inflammation around the root tip, a fracture, or leakage from the crown or filling. A common practical step is to check the restoration and get updated imaging if symptoms recur.
Will antibiotics fix a dead or infected tooth without dental treatment?
Antibiotics can reduce spreading infection in some cases, but they do not remove damaged pulp or eliminate bacteria inside the canal system. Definitive dental treatment (like root canal therapy or extraction depending on the situation) is what actually addresses the source.
Can home remedies, rinses, or supplements bring back a dead tooth nerve?
No. Once pulp tissue is necrotic in a mature tooth, the nerve supply and blood supply are gone. Home products may temporarily change symptoms but cannot restore living pulp. The best “next step” is diagnosis, then choosing the appropriate restorative or endodontic option.
What are signs that dental infection is spreading and needs urgent care?
Facial swelling, trouble swallowing or breathing, fever with dental pain, or rapidly expanding swelling are red flags. These can indicate spread beyond the tooth into deeper spaces, which warrants urgent evaluation rather than waiting for a routine appointment.
Yes or no on dentin regrowth, realistic timelines, and what to do for exposed dentin, cavities, trauma, and repair optio
Can tooth roots grow back after a root canal? Mostly no, with healing explained and next-step options for failing roots.
Can bone grow back around teeth? Learn real limits, causes, and what helps periodontal bone loss and gum recession.

