Quick answer: can dentin grow back (and when)?
Here is the straight answer: dentin does not grow back the way a cut on your skin heals. Once a meaningful amount of dentin is lost to a cavity, grinding, or trauma, your body cannot replace it with a fresh, identical layer. That said, your tooth is not completely passive either. Under the right conditions, specifically when the pulp (the living inner tissue of the tooth) is still vital, the body can deposit a limited amount of new hard tissue called tertiary or reparative dentin. This acts as a defensive barrier, not a full rebuild. So the honest answer is: partial repair is sometimes possible in a living tooth, but true, complete dentin regrowth is not something you can count on in humans.
What 'dentin regrowth' really means vs. exposed dentin
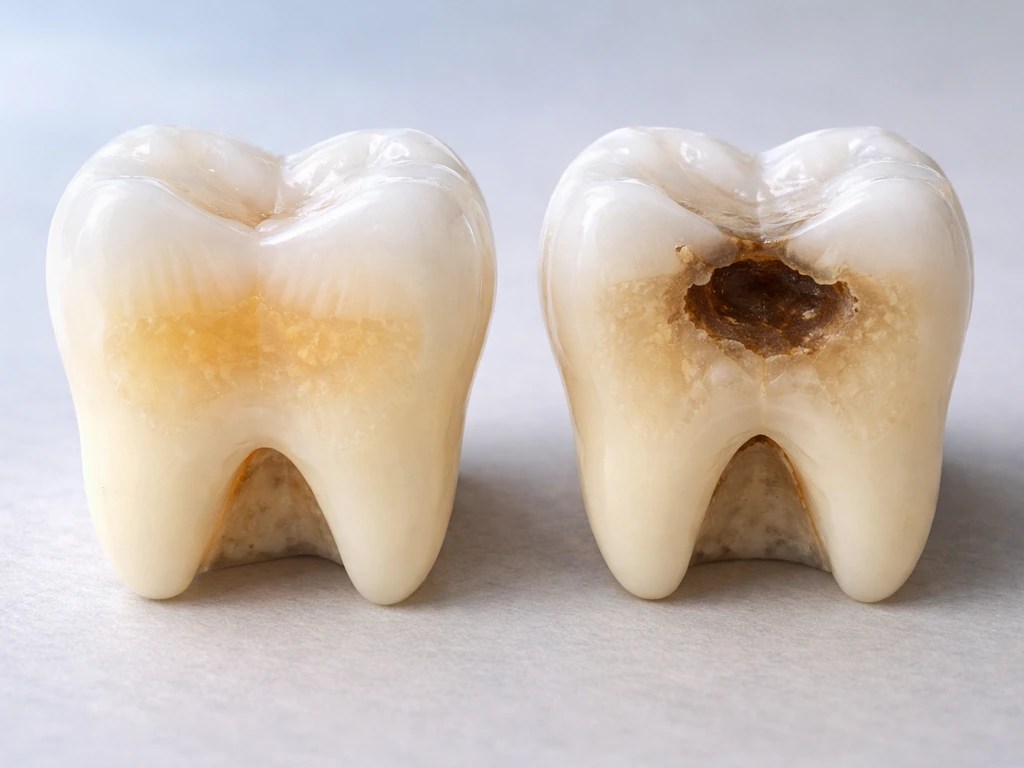
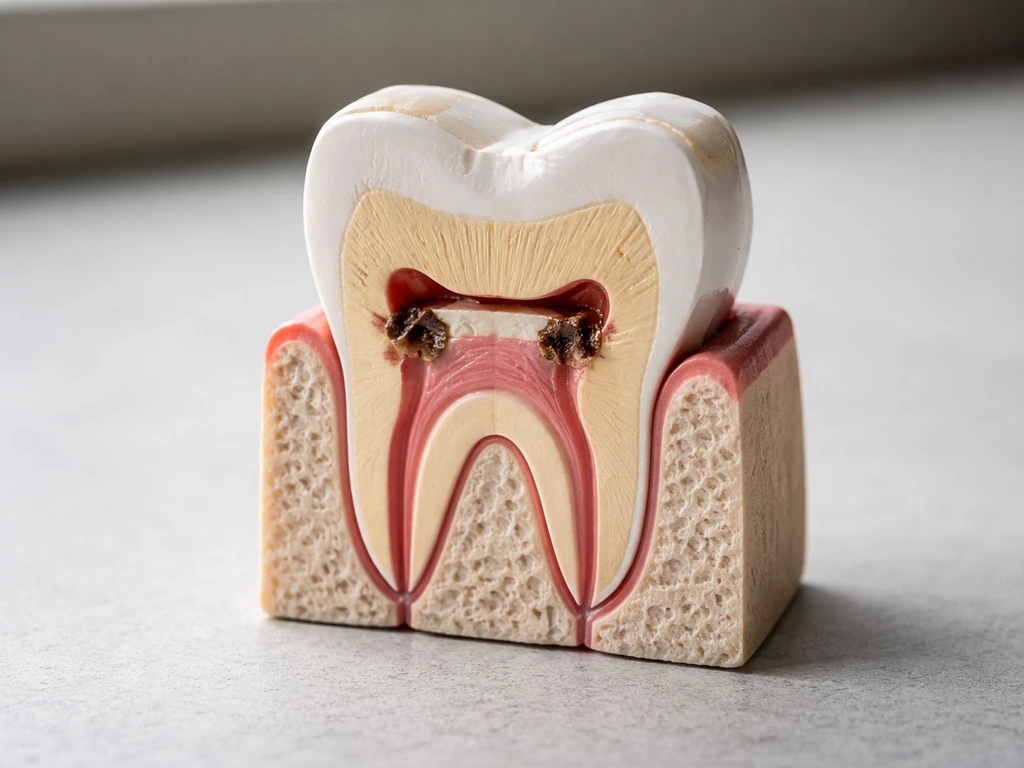
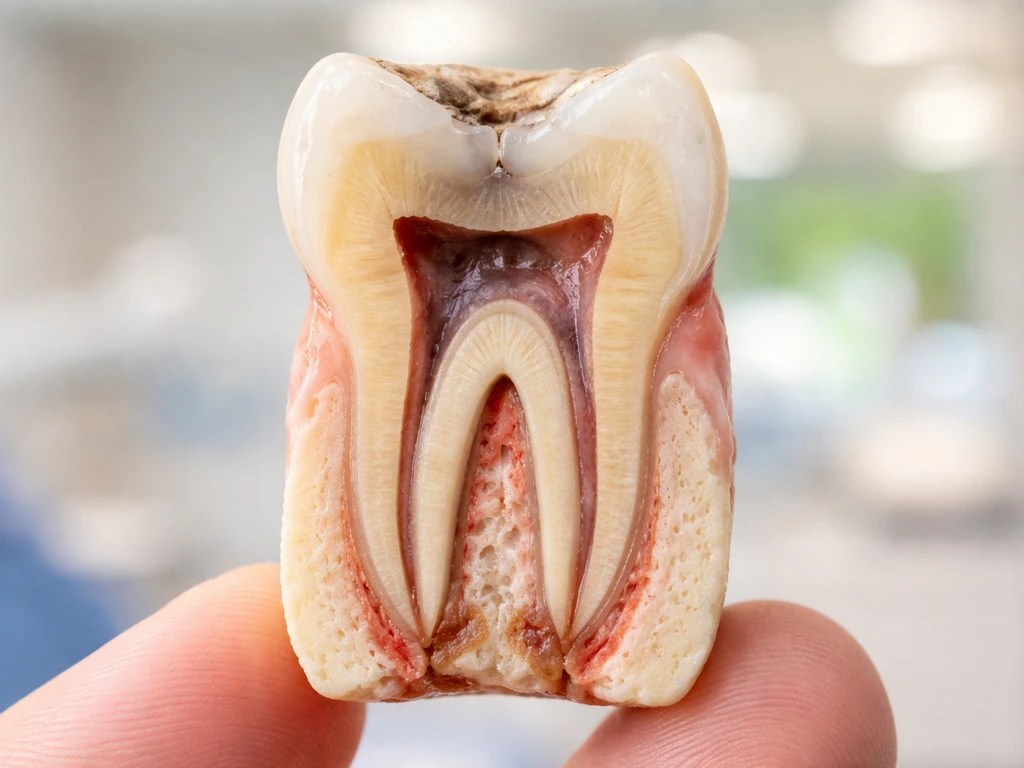
There is a lot of confusion online between two very different problems: having exposed dentin and actually losing dentin thickness. Dentin is the hard, yellowish layer that sits beneath tooth enamel and surrounds the pulp. When enamel wears away, gums recede, or a cavity eats through the outer surface, dentin becomes exposed to the oral environment. That exposure is what causes the sharp, quick sensitivity you feel when you drink something cold or breathe in cold air. The pain happens because exposed dentin has tiny open channels called dentinal tubules, and fluid movement inside those tubules triggers nerve signals.
The key distinction is this: sensitivity from exposed dentin is not the same as losing the dentin itself. You can have exposed dentin with the full thickness still intact underneath, or you can have genuine structural loss where the dentin layer has been eaten away by a cavity or worn down by grinding. These two situations require very different responses, and conflating them leads people to believe that because their sensitivity improved, their dentin somehow 'grew back.' It did not. What often changes is that dentinal tubules become partially blocked, either naturally through mineral deposits or with the help of desensitizing products, reducing fluid movement and therefore pain. The structure underneath stays the same.
Actual dentin regrowth refers to the body forming new mineralized tissue, and this only happens in a very specific biological scenario: the pulp is alive, the stimulus (a cavity, mild trauma) is not too severe, and certain cells called odontoblasts (or newly recruited odontoblast-like cells) respond to the threat by depositing a protective layer of tertiary dentin. This is the body trying to wall off the pulp from danger, not replenishing what was lost on the surface.
How long dentin repair actually takes in real life
If the conditions are right for reparative dentin to form, the timeline is measured in weeks to months, not days. Human histologic studies have found early signs of dentin bridge formation as quickly as 7 to 14 days in some specimens after direct pulp capping with certain materials, though that is far from universal. Clinically, a dentin bridge that is substantial enough to be meaningful is generally documented within approximately 75 to 90 days when vital pulp therapy goes well. A full clinical picture, including radiographic evidence of stability and absence of symptoms, is typically assessed at 1 month, 3 months, 6 months, and 1 year after treatment.
The important caveat is that this kind of repair happens inside a clinical setting, after a dentist has placed a protective capping material (usually a calcium silicate cement like MTA or Biodentine, or calcium hydroxide) over an exposed pulp. This is not something that happens on its own while you wait at home. Without treatment, bacteria and continued damage will overwhelm any repair attempt. And even with treatment, dentin bridge formation is not guaranteed. Research using adhesive systems for pulp capping, for example, has shown incomplete bridge formation in some human specimens even when inflammation appeared controlled.
What affects whether your tooth can repair itself
Pulp vitality: the single biggest factor
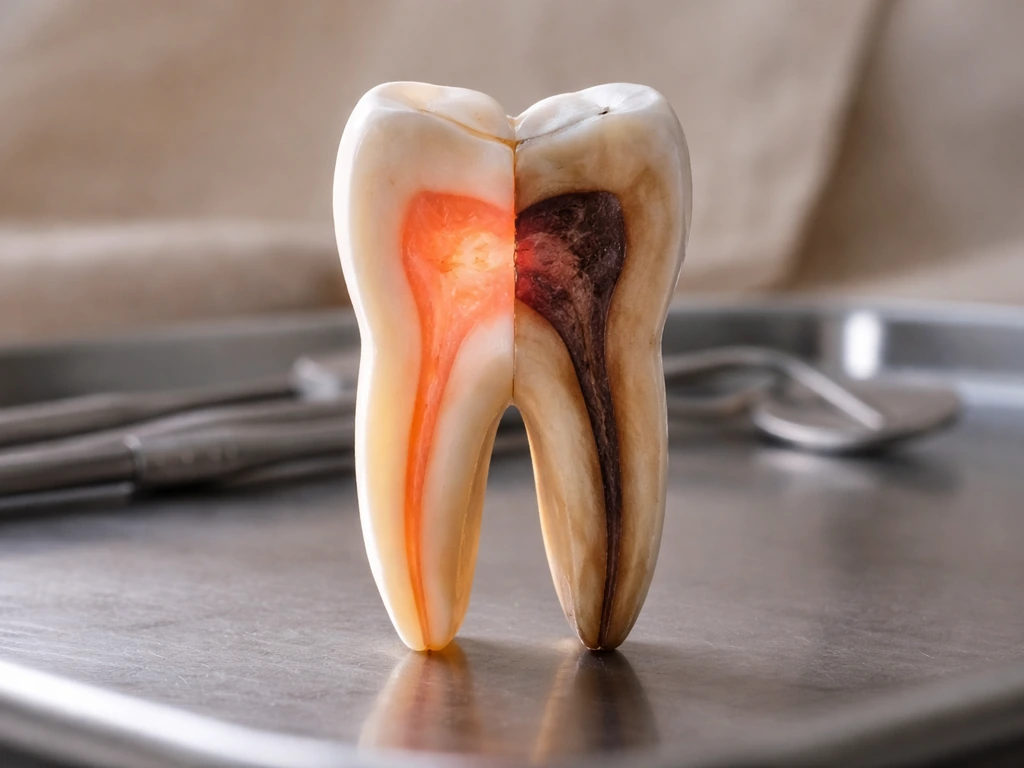
Whether any reparative dentin can form at all comes down almost entirely to whether the pulp is still alive. If the pulp is vital and the inflammation is classified as reversible pulpitis (meaning the pulp can recover once the irritant is removed), there is a biological window for repair. If the pulp has reached irreversible pulpitis, where the pain is spontaneous, lingers well after the stimulus is removed, and is hard to localize, the repair window is essentially closed. A necrotic pulp has no living cells to form dentin at all. Your dentist assesses this using cold tests, percussion testing, and X-rays, not just your description of symptoms.
Cause and severity of the damage
What caused the dentin loss matters enormously. A small, slow-growing cavity that has not yet reached the pulp is a very different situation from a deep cavity with bacterial exposure at the pulp, a cracked tooth, or severe tooth grinding (bruxism). With deep caries, removing the bacterial stimulus and sealing the area can allow pulp stem cells to differentiate into odontoblast-like cells and begin forming a calcific bridge. With trauma, there are cases in the literature of spontaneous dentin bridge formation after injury, but these are rare and depend on whether at least part of the pulp (often the apical portion) remained vital. Heavy grinding wears dentin progressively, and no reparative response can keep pace with ongoing mechanical damage.
Age and tooth type
Age plays a real role, though it is more nuanced than 'younger is always better.' Young permanent teeth have larger pulp chambers, richer blood supply, and more robust stem cell populations, which gives them better reparative potential. For children and adolescents, preserving pulp vitality is a central goal in dental guidelines, including those from the American Academy of Pediatric Dentistry, because the biological response in young teeth is more reliable. In older adults, pulp chambers narrow over time as the body naturally deposits secondary dentin throughout life, the blood supply becomes less robust, and reparative responses tend to be slower and less complete.
The presence of infection
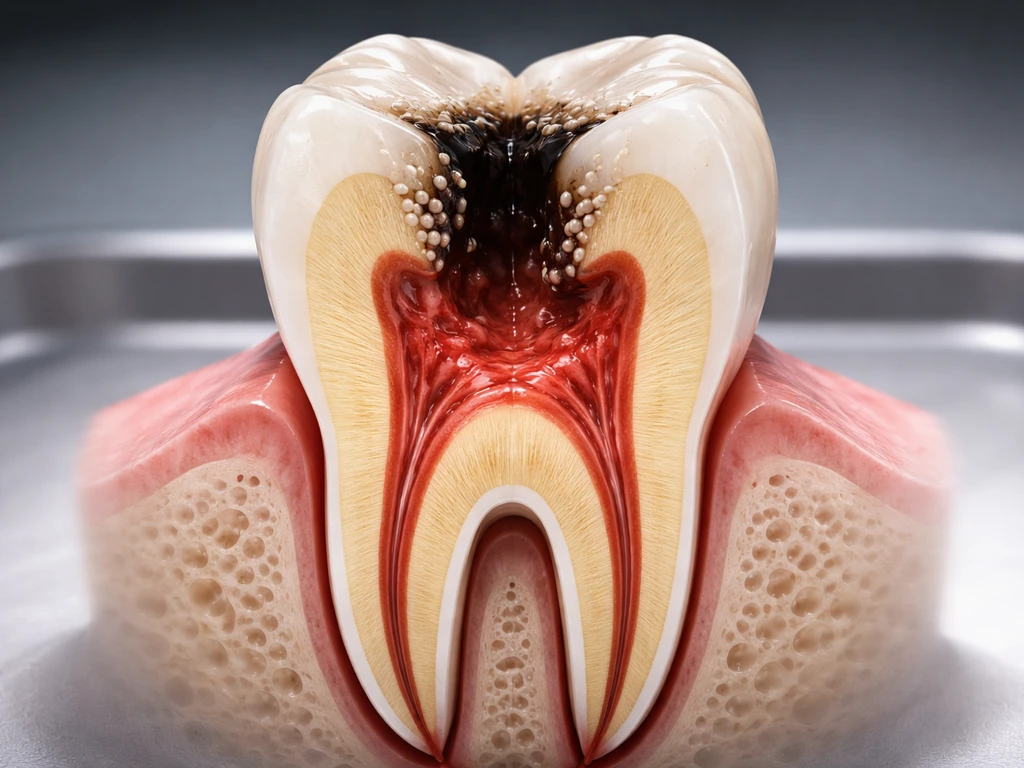
Infection changes everything. When bacteria are involved, the inflammatory mediators and bacterial byproducts can disorganize or kill odontoblasts, the very cells needed to initiate repair. Research in teeth with apical periodontitis (infection around the root tip) shows that while some reparative dentin deposition does occur on root canal walls in these infected teeth, the quality and organization of that mineralization is compromised compared to what forms in response to non-infectious stimuli. The bottom line: infection kills the conditions needed for repair, which is exactly why getting prompt treatment to control infection is so critical.
Signs you need to see a dentist urgently
Some symptoms are a genuine warning that your pulp is in serious trouble and no amount of waiting, desensitizing toothpaste, or home remedies is going to help. If you are experiencing any of the following, treat it as urgent:
- Spontaneous toothache that does not need a trigger, especially at night
- Pain that lingers for more than a few seconds after the cold or hot stimulus is removed
- Swelling in the gum, jaw, or face near the affected tooth
- A pimple-like bump on the gum (a dental abscess draining)
- Fever or difficulty opening your mouth or swallowing
- Tooth pain after trauma, especially if the tooth changed color or feels loose
- Deep, throbbing pain that is hard to pinpoint to a single tooth
The first few symptoms on that list are classic signs of irreversible pulpitis or pulp necrosis. At that point, the reparative window is gone, and the relevant question is no longer 'will dentin grow back' but 'how do we save the tooth or manage the infection.' Swelling, fever, and difficulty swallowing in particular indicate that infection may be spreading beyond the tooth, which is a medical emergency. The American Academy of Family Physicians notes that periapical abscess can progress to serious cellulitis if not treated promptly.
What you can do right now, today
If you are reading this because you have tooth sensitivity or a known cavity and are wondering whether things might sort themselves out, here is the practical reality: the most useful thing you can do immediately is stop the source of ongoing damage. That means:
- Book a dental appointment now, not when it hurts more. The earlier dentin damage is caught, the better the chance that pulp vitality can be preserved and repair encouraged.
- If you grind your teeth, talk to your dentist about a night guard. No repair is possible if the mechanical damage continues.
- Switch to a soft-bristled toothbrush and a desensitizing toothpaste containing fluoride or potassium nitrate. These do not regrow dentin, but they help occlude open dentinal tubules and reduce sensitivity while you wait for your appointment.
- Avoid highly acidic food and drinks (citrus, soda, vinegar-based foods), which can accelerate enamel and dentin erosion.
- Do not poke at or apply pressure to a tooth you suspect has exposed dentin or a deep cavity. You can inadvertently push bacteria deeper.
- If you had a recent dental trauma (impact, crack, chip), see a dentist even if the tooth is not painful yet. Pulp damage from trauma can be slow and silent at first.
It is worth noting that sensitivity improving on its own is not proof that dentin repaired itself. Tubule occlusion can happen with mineral deposits from saliva or from desensitizing products, making you feel better without any structural regrowth. That is a useful symptom improvement, but it is not the same as addressing the underlying cause. If a cavity is present, it will keep growing regardless of whether sensitivity decreases.
Treatment options when dentin cannot regrow on its own
For most cases of meaningful dentin loss, whether from cavities, grinding, or erosion, the goal of dental treatment shifts from encouraging regrowth to protecting what remains and replacing what is gone with restorative materials. Here is how that looks in practice:
| Situation | Treatment approach | Goal |
|---|
| Small to moderate cavity (pulp not exposed) | Composite or ceramic filling after decay removal | Restore shape and protect remaining dentin |
| Deep cavity, pulp still vital (reversible pulpitis) | Vital pulp therapy: indirect or direct pulp capping with calcium silicate cement (MTA, Biodentine) | Preserve pulp vitality and encourage reparative dentin bridge formation |
| Pulp exposed, irreversible pulpitis or necrosis | Root canal treatment (pulpectomy) and crown | Remove infected tissue, seal the canal, restore the tooth |
| Dentin hypersensitivity from exposed root or enamel loss | Desensitizing agents, fluoride varnish, bonding agents, or gum grafting if recession is the cause | Occlude dentinal tubules and eliminate the sensitivity trigger |
| Severe tooth wear from grinding or erosion | Night guard, dietary modification, and restorations (onlays, crowns) to rebuild lost structure | Stop ongoing loss and replace what cannot regrow |
| Traumatic dentin loss (chipped or fractured tooth) | Bonding, veneer, or crown depending on extent | Protect exposed dentin and restore function immediately |
Vital pulp therapy is the treatment most directly aimed at encouraging the body's own reparative response. When a dentist places a calcium silicate material over an exposed vital pulp, they are creating the best possible biological environment for new odontoblast-like cells to differentiate and begin forming a dentin bridge. Calcium silicate cements have largely replaced calcium hydroxide in modern practice because they produce a better inflammatory response and more reliable bridge formation. But it only works if the pulp is genuinely vital and the exposure is caught before irreversible damage sets in.
When the pulp is no longer salvageable, root canal treatment removes the inflamed or necrotic tissue, cleans the canal system, and seals it. The tooth loses its biological reparative capacity at that point, which is one more reason why enamel and dentin protection matter so much before things escalate. The question of whether enamel can grow back follows a very similar logic to dentin: it cannot, and the same urgency around catching damage early applies to both tissues. The question of whether enamel can grow back follows a very similar logic to dentin: it cannot, and the same urgency around catching damage early applies to both tissues. how long does it take for enamel to grow back is typically discussed alongside this enamel non-regrowth point. The same goes for understanding why teeth do not regrow lost structure in the way we might hope, a pattern that extends even to roots and nerves in the pulp. The same goes for understanding why teeth do not regrow lost structure in the way we might hope, a pattern that extends even to roots and nerves in the pulp can bone grow back around teeth. In that same way, questions like can teeth nerves grow back depend on whether the pulp is still vital and whether the damage is reversible. The same limits apply to can teeth roots grow back, so early evaluation and treatment matter.
The practical takeaway is this: if you want the best shot at your tooth doing any self-repair at all, time is your most valuable resource. Reparative dentin formation, where it happens, occurs over weeks to months inside a tooth that still has a living, recoverable pulp. Every week of delay on a symptomatic or visibly damaged tooth reduces that biological window. The same issue of lost hard tissue and delayed treatment is explored in why teeth don't grow back. See your dentist, stop the source of damage, and let the treatment create the conditions for whatever repair is biologically possible.