No, tooth roots cannot grow back in adults. Once a root is lost or significantly damaged, your body does not regenerate it the way it would heal a cut or even a broken bone. That is the short, direct answer. But there is a lot of nuance worth understanding here, especially if you have recently had a root canal, suffered a dental injury, or are wondering whether something you read online about tooth regeneration actually applies to you. The reality is more interesting than a flat "no" and also more practically useful.
Can Teeth Roots Grow Back After a Root Canal? Facts
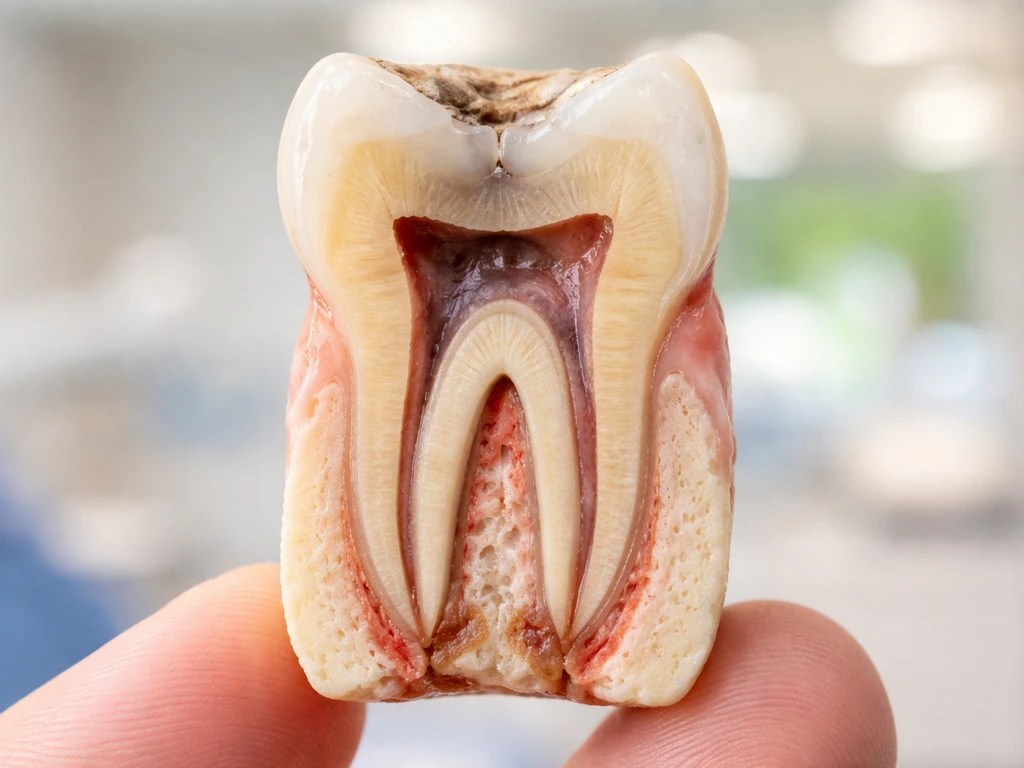
Do tooth roots grow back after loss or injury?
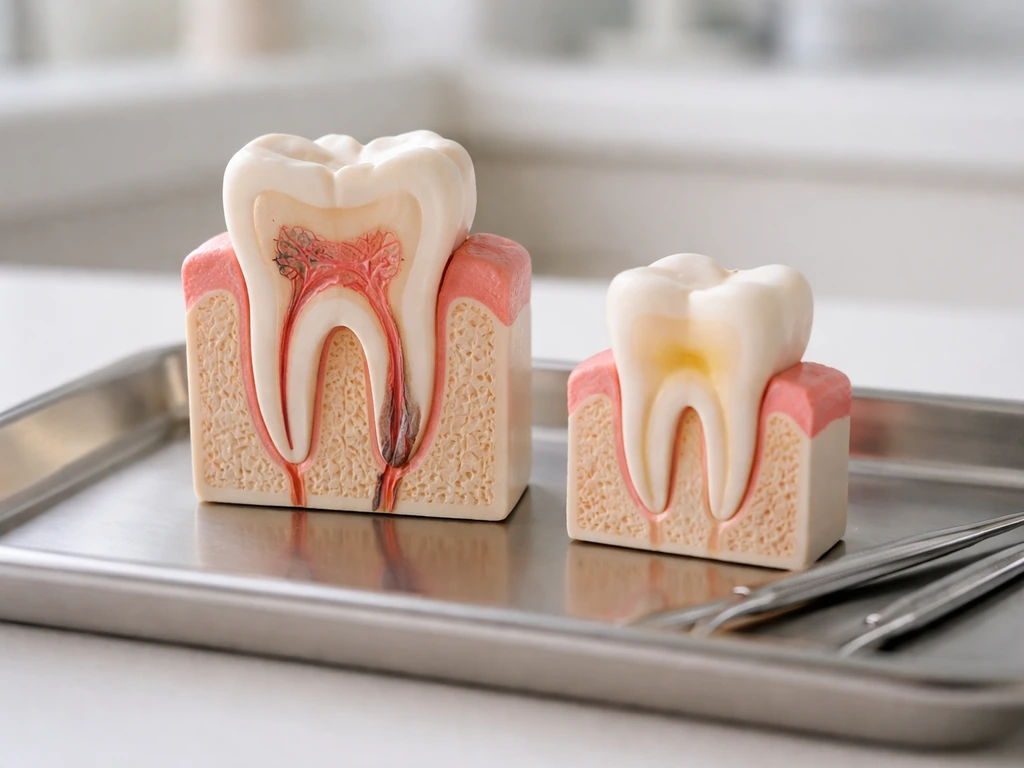
In healthy adult mouths, tooth roots do not grow back. They are not like fingernails or skin. The cells responsible for forming root structure (cementoblasts, which lay down cementum, and the periodontal ligament fibroblasts that anchor the root to the bone) are present in your mouth but they cannot rebuild a root from scratch once it is gone or severely resorbed. Researchers have successfully regrown teeth in mice and ferrets in laboratory settings, but as the American Dental Association has noted, this is experimental work and is nowhere close to being a routine treatment option for human patients right now.
There is one limited exception worth mentioning honestly: children and teenagers with immature teeth that have open root tips (what dentists call "open apices") can sometimes continue root development even after the pulp (the nerve and blood supply inside) has died, but only under specific conditions and with specialized regenerative endodontic treatment. The American Association of Endodontists actually maintains a dedicated regenerative endodontics database focused specifically on these incompletely developed teeth. This is not typical adult root regrowth. It is the continuation of a developmental process that was already underway in a young, biologically favorable environment. Once your roots are fully formed, that window is closed.
What actually happens to the root after a root canal?
This is where a lot of confusion comes from. A root canal does not remove the root. It removes the pulp tissue (the nerve, blood vessels, and soft tissue) from inside the root. The root itself stays in your jaw. After the canal is cleaned, shaped, and sealed, your body begins healing the surrounding tissues, particularly the periapical tissues at the root tip that may have been inflamed or infected.
What that healing actually looks like under a microscope is instructive. In many successful cases, the inflamed or resorbed tissue around the root tip repairs itself. Research has even documented cases where, after 25 years of follow-up, the apical canal was almost completely filled with a cementum-like tissue, which is about as close to "repair" as you can realistically hope for. But this is repair, not regeneration. The original root structure that was resorbed or damaged does not grow back fresh. Instead, the body patches the area, sometimes with cementum-like material, sometimes with fibrous scar tissue, and sometimes with a combination of both. Long-term studies show that most people achieve complete periapical healing with no ongoing inflammatory processes, even when the healing tissue is scar rather than true bone or cementum.
The important takeaway: when your tooth stops hurting after a root canal, that usually means the infection is under control and healing is occurring. It does not mean your root grew back. Feeling better and regenerating tissue are two very different things, and conflating them is one of the most common misconceptions in this space.
Why your body cannot just regrow a root
The biological reasons are worth understanding because they also explain why certain treatments work and others do not. A tooth root is a highly organized structure. The root surface is coated with cementum, a mineralized tissue that anchors the fibers of the periodontal ligament, which in turn connects the root to the surrounding alveolar bone. This whole system (cementum, periodontal ligament, and bone) has to work together in a very coordinated way. Complete cementum regeneration alone is described in recent research as clinically challenging due to multiple biological barriers, and that is just one component of the root attachment system.
When the periodontal ligament is lost or severely damaged, things get even worse. In a process called ankylosis, the cementum fuses directly with the alveolar bone and the periodontal ligament disappears partially or completely. At that point, not only is the root not growing back, but the normal ligament-mediated attachment architecture that would even allow for regenerative healing is gone too. This is part of why teeth don't grow back in adults the way many people hope or assume they might.
It is also worth noting that dentin, the hard tissue that makes up most of the root's internal structure, has very limited self-repair capacity. If you are wondering about that specifically, does dentin grow back is a question with its own nuanced answer, but the short version is: tertiary dentin can form in response to mild irritation, but it does not rebuild a root.
Healing vs. regrowth: the myth-busting section
Let's be direct about the most common myths circulating online about tooth and root regrowth.
| Myth | Reality |
|---|---|
| If my tooth pain went away, the root healed itself | Pain relief means infection is controlled or resolved; it does not mean the root regenerated |
| Oil pulling / supplements / remineralization products can regrow roots | No topical product or supplement can regenerate lost root structure; remineralization applies only to enamel surfaces |
| Regenerative dentistry means adults can regrow roots | Regenerative endodontics is primarily for immature teeth with open apices in younger patients, not for regrowing mature adult roots |
| Root canal damage can be fixed by waiting it out | Without treatment, periapical infection can spread; monitoring is not a substitute for care |
| If bone can grow back around a tooth, the root can too | Bone and root tissue are different structures with different regenerative potential; bone regrowth around teeth is possible in certain scenarios but does not mean the root itself regenerates |
The confusion between healing and regeneration is understandable because they can look similar from the outside. Your tooth stops hurting. Your follow-up X-ray looks better. You feel fine. But what is actually happening is that granulation tissue (a fibro-vascular matrix) is walling off and resolving the inflammatory process, and the body is filling in the periapical area with whatever repair tissue it can produce, often fibrous scar tissue. That is a good outcome. It just is not "root regrowth."
Similarly, people sometimes assume that because enamel has some remineralization capacity, other tooth structures must too. They are different. If you want the full picture on that, can enamel grow back covers what is actually possible there, and how long it takes for enamel to grow back explains the realistic timeline for that surface-level remineralization process. Neither applies to root structure.
What about the nerve inside the root?
After a root canal, the nerve inside the tooth is gone and it does not come back. The tooth becomes what dentists sometimes call "non-vital" because it no longer has its own blood supply or nerve tissue. People often ask whether the nerve can regenerate, and the answer is similarly limited. Can teeth nerves grow back is its own topic, but in brief: in a fully mature, root-canal-treated tooth, the pulp tissue is gone and does not regenerate. In some immature teeth treated with regenerative protocols, revascularization can occur, meaning new tissue grows into the canal space, but even then, that tissue may not fully replicate the original pulp.
Your real options when a root cannot regrow
This is the part that actually matters for solving your problem today. If root regrowth is not on the table, what is? The answer depends on what specific situation you are dealing with, but here is how dentists and endodontists typically think through the options.
Monitoring and follow-up
After a root canal or a dental injury, regular follow-up imaging is not optional, it is essential. The AAE recommends follow-up evaluations for up to five years after traumatic dental injuries to ensure root resorption is not progressing and that surrounding tissues are continuing to heal. This is not just box-ticking. Periapical changes can develop slowly and asymptomatically, meaning you might feel fine while a problem is building. Root resorption that is caught early is much more manageable than root resorption that has been silently progressing for years.
Nonsurgical retreatment
If a previous root canal has failed (meaning infection returned or never fully resolved), retreatment is often the first option to consider before anything more invasive. The canals are re-accessed, the old filling material is removed, the canals are re-cleaned and re-sealed. Long-term data support high success rates when this is done well and when there is adequate tooth structure remaining.
Periapical surgery (apicoectomy)
When nonsurgical options are not practical or have already been tried, an apicoectomy removes the very tip of the root and seals it from the other end. This is a surgical procedure done through the gum tissue, and it can resolve persistent periapical pathology in cases where retreatment alone would not be effective. It is not root regrowth, but it is root preservation.
Extraction and implant or bridge
Some roots are not salvageable. Vertical root fractures, for example, are often an indication for extraction because the fracture pattern makes predictable repair impossible. When a root cannot be saved, extraction followed by an implant (which serves as an artificial root) or a bridge is the standard path forward. Implants in particular function as a structural replacement for the root, integrating with the jawbone over several months. This is not biological regrowth, but it restores function effectively.
Restoration quality matters as much as the root decision
One thing that does not get enough attention: even when a root is saved, the restoration placed on top of it dramatically affects long-term survival. Research shows that endodontically treated teeth need a solid crown with adequate ferrule (ideally 1.5 to 2 mm of sound tooth structure above the gum line) to resist fracture. If there is not enough remaining coronal tooth structure to support a proper restoration, extraction may actually be the better long-term choice even if the root itself is intact. Grinding and bruxism can also complicate this picture significantly, since repeated heavy forces accelerate structural loss. If that is your situation, whether teeth grow back after grinding is worth reading alongside this.
How imaging guides these decisions
You cannot make good decisions about root treatment without good imaging. Standard periapical X-rays are usually the first step and are appropriate for most follow-up evaluations. The ADA published updated guidance in early 2026 emphasizing that dental X-rays should be used when clinically justified, with 2D imaging appropriate for the majority of scenarios. Cone beam CT (CBCT) offers 3D detail that standard X-rays cannot provide, but it delivers more radiation and is recommended specifically for symptomatic patients where 2D imaging has not given a clear answer. If your dentist suspects a complex fracture, unusual anatomy, or has inconclusive 2D findings, asking about CBCT is reasonable. But for routine follow-up after a root canal, a standard periapical X-ray is typically sufficient.
Signs you need to see a dentist now
Some situations are genuinely urgent and should not wait for a scheduled check-up. Dental infections can spread to surrounding tissues, and periapical abscesses in particular can track toward the sinuses or deeper facial spaces if left untreated.
- Swelling of the face, jaw, or neck (especially if it is expanding or affecting your ability to swallow or breathe)
- Fever along with dental pain or swelling
- Persistent bad taste or bad breath that suggests ongoing drainage from an infected tooth
- Pain that is worsening after a root canal rather than gradually improving
- Visible pimple or bump on the gum near a tooth (this is often a draining sinus tract from an abscess)
- A tooth that was previously treated but is now sensitive to pressure or percussion again
- Any traumatic dental injury, even if the tooth looks fine immediately afterward
If you have fever, spreading swelling, or difficulty swallowing, that is an emergency. Go to an urgent dental clinic or an emergency room. Do not wait for a regular appointment.
Questions to ask your dentist at your next visit
Going into a dental appointment with specific questions gets you better information. Here are the most useful ones if you are dealing with a root issue:
- Is there any sign of root resorption on my current X-rays, and if so, how much and how fast is it progressing?
- Is my root canal healing as expected, or is there still periapical pathology present?
- If the root cannot be saved, what are my actual options and what does the timeline look like for each?
- Do I need a CBCT scan, or will standard X-rays give you enough information to make this decision?
- Is my current crown or restoration giving the tooth adequate protection, and is there enough tooth structure above the gum line to support a long-term restoration?
- If retreatment is an option, what is the expected success rate given my specific anatomy and history?
- At what point would you recommend extraction over continued attempts to save this root?
The bottom line
Tooth roots do not grow back in adults. The biology simply does not support it outside of very specific, immature-tooth scenarios that do not apply to most people asking this question. What your body can do is heal the tissues around the root, control infection, and repair (not regenerate) damaged areas with scar-like or cementum-like tissue. That healing is real, it is meaningful, and it can last for decades. But it is not the same as the root growing back. Understanding that distinction helps you make better decisions: stop waiting for something that is not coming, get properly diagnosed with the right imaging, and have an honest conversation with your dentist about whether the goal is saving the root you have or replacing it with something that works just as well.
FAQ
If my root canal tooth feels better, does that mean the root and nerve healed or regenerated?
Feeling better usually means the inflammation and infection around the root tip are settling, not that the nerve inside regenerated or that missing root tissue regrew. The tooth can still be “non-vital,” and what improves is the surrounding periapical area that has been repairing with scar-like or cementum-like tissue.
Can a dentist tell from an X-ray whether the root is completely healed after a root canal?
An X-ray can show whether the periapical area looks stable or improved, but it cannot always prove the exact type of tissue that formed. For unclear cases, your dentist may compare multiple time points or recommend additional imaging (for example, CBCT when symptoms or suspected complex anatomy are present).
What symptoms suggest something is going wrong after a root canal, even if the pain has gone away?
New or recurrent swelling, a persistent pimple on the gum near the tooth, bad taste or drainage, pain when biting after an initial improvement, or symptoms that gradually return over weeks to months can all suggest incomplete healing. These are reasons to get follow-up evaluation rather than assuming you are fully cured.
Does root canal retreatment ever make it look like the root “grew back”?
Retreatment aims to eliminate bacteria and improve the seal, so the periapical tissues can heal better over time. It does not rebuild the original root structure, but improved sealing and canal disinfection can lead to more complete resolution on follow-up imaging.
How do I know whether I am in the rare case where immature teeth can continue root development?
The key factor is whether the tooth had an open root tip (immature root) at the time of treatment. Your dentist can assess this with imaging and the tooth’s developmental stage. This does not apply to typical adult teeth where the root is already fully formed.
If my tooth has ankylosis, is extraction always required?
Not always. Ankylosis changes the prognosis because the ligament space is altered and normal ligament-mediated healing is limited. Treatment decisions depend on symptoms, extent of fusion, adjacent bone health, and whether the tooth can be stabilized or restored. A specialist can help weigh monitoring versus removal.
Can a crown or filling affect whether the root canal heals successfully?
Yes. The restoration influences long-term survival by preventing recontamination and supporting the tooth against fracture. Many clinicians aim for an adequate ferrule (enough sound tooth structure above the gum line) so the tooth resists cracks and chewing forces.
Should I get follow-up X-rays for years after a root canal?
Often you do, but the exact schedule depends on why the treatment was done and your risk level. For traumatic dental injuries, follow-up may be recommended for up to several years because resorption can be slow and initially silent. Ask your dentist what timeline fits your case.
Are there situations where the best plan is not saving the root even if it looks intact?
Yes. Vertical root fractures, inadequate remaining tooth structure to support a durable restoration, or heavy occlusal forces (bruxism, grinding) can make long-term saving unlikely. In those cases, extraction followed by an implant or bridge may offer a more predictable outcome.
What should I do if I think an infection is spreading after a root canal?
Do not wait for a routine appointment. Fever, rapidly spreading swelling, trouble swallowing, or difficulty breathing are emergency signs. Seek urgent care immediately because infections can extend into surrounding facial spaces.
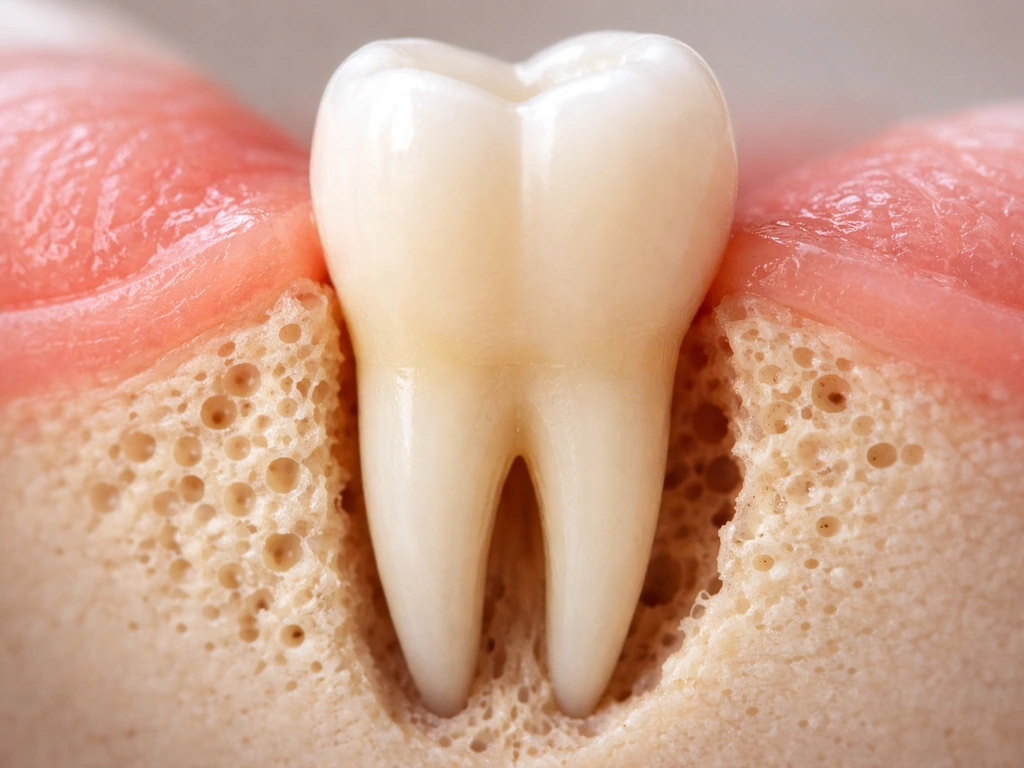
Can bone grow back around teeth? Learn real limits, causes, and what helps periodontal bone loss and gum recession.
Learn why teeth and enamel dont regenerate, what happens after loss, and the practical options for fixing gaps.
Learn if enamel can regrow, why it cannot, and how fluoride and remineralization can repair early damage.

