Here's the honest answer: bone around your teeth can partially regenerate, but it almost never does so on its own, and it rarely comes back completely. If you've been told you have bone loss around your teeth, that's a serious situation that needs professional treatment, not just better brushing. The good news is that modern periodontal treatments can genuinely rebuild some of that lost bone in the right circumstances. The less good news is that the biology is complicated, and not every case qualifies. This guide will walk you through exactly what's possible, what's not, and what you should do today.
Can Bone Grow Back Around Teeth? What’s Real and What Helps
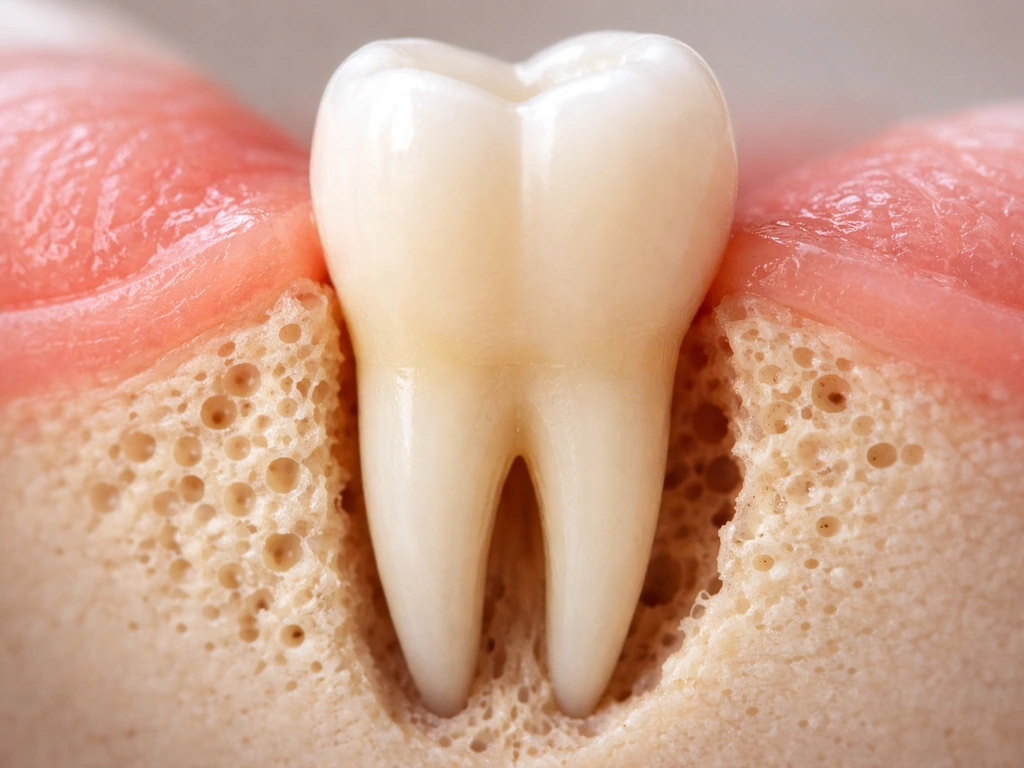
What "bone growing back" actually means in your mouth
When dentists and researchers talk about bone regeneration around teeth, they're referring to something very specific. The tissues that support your teeth make up a system called the periodontium, which includes the gingiva (gum tissue), alveolar bone (the jawbone that holds the teeth), the periodontal ligament (a tiny shock-absorbing structure connecting bone to tooth root), and the cementum (the thin calcified layer covering the root surface). True periodontal regeneration, as defined by the American Academy of Periodontology, means restoring all of these components: new bone, new periodontal ligament, and new cementum. That's the gold standard.
In practice, what most treatments achieve is something called "bone fill" or clinical improvement, which is measurable on X-rays and through probing depth measurements, but doesn't necessarily confirm that every component of the periodontium was perfectly rebuilt. This distinction between repair and regeneration matters a lot. Repair might involve the defect filling in with tissue and the pocket shrinking, but the new attachment apparatus might not be identical to what was originally there. Clinicians measure outcomes like clinical attachment level (CAL) gain and radiographic defect fill because those are the real-world tools available. Histological confirmation (actually looking at the cells under a microscope) isn't something you can do on a living patient routinely. So when your periodontist says bone has "grown back," they usually mean the evidence strongly suggests significant healing occurred, even if it's not a pixel-perfect replacement of every original structure.
It's also worth separating alveolar bone loss from gum recession. People often use these interchangeably, but they're related problems that don't always move at the same pace. You can have gum recession with relatively intact bone underneath, or you can have significant bone loss beneath gums that look fairly normal from the outside. Both are problems, but the treatment paths differ.
Why bone loss happens around teeth in the first place
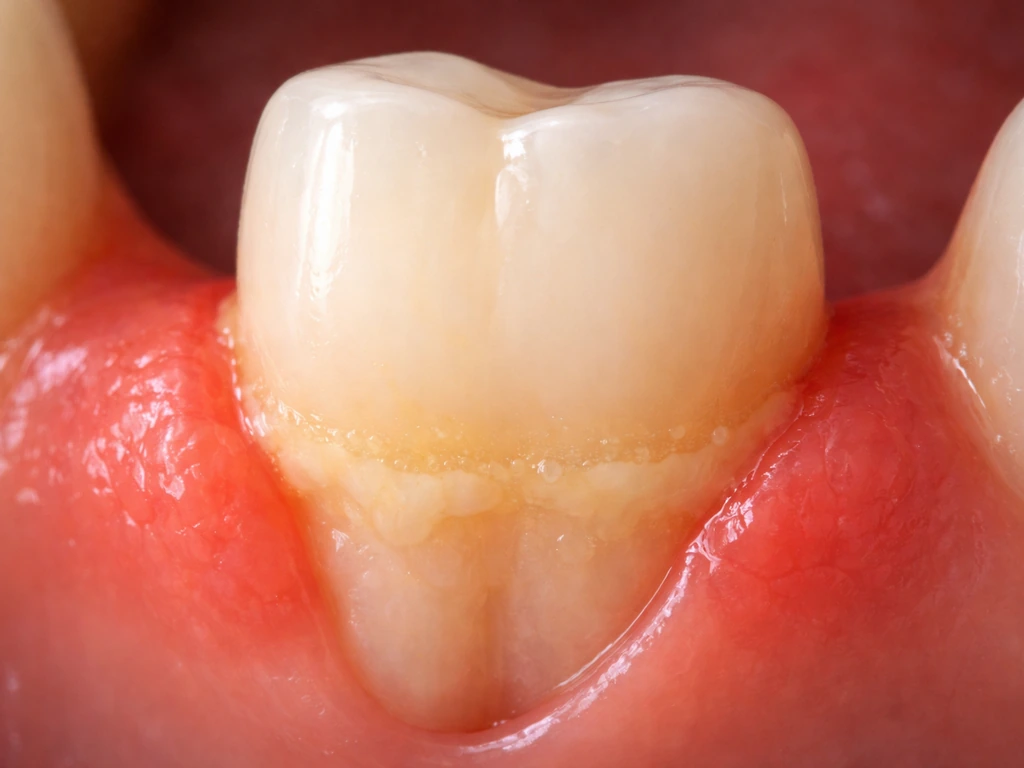
The most common culprit is periodontitis, the advanced form of gum disease. It starts as gingivitis (inflamed gums from plaque buildup), but when that inflammation goes unaddressed, the bacteria and the body's own immune response begin destroying the supporting structures around teeth. The bone doesn't just disappear overnight. It gets resorbed gradually as the infection creates pockets between the gum and the tooth root, where more bacteria accumulate, creating a worsening cycle.
Beyond gum disease, there are other causes worth knowing about. Bruxism (teeth grinding) creates mechanical stress on the bone and supporting ligament. If you've ever wondered whether that grinding habit is causing lasting damage, do teeth grow back after grinding explores that question in more detail, but the short version is that the structural damage from chronic grinding can accelerate bone loss when combined with gum disease. Trauma to the jaw or a single tooth can also cause localized bone loss. Poorly fitting dental appliances, certain medications (especially long-term steroids or some seizure medications), and systemic diseases like uncontrolled diabetes all contribute. Even tooth extraction creates bone loss at the site because the bone that held the tooth no longer has a reason to stay.
The reason so many people are caught off guard by bone loss is that it's largely painless until it's significant. Bone doesn't have nerve endings the way pulp tissue does, so you don't feel it dissolving. By the time teeth feel loose or you notice a change in your bite, a meaningful amount of support may already be gone.
Can dental bone actually regenerate? What's real and what isn't
Yes, bone around teeth can regenerate, but only under specific conditions, and almost never by itself without treatment. The body does have some limited capacity to heal periodontal bone defects after the infection is controlled and inflammation is resolved. Research published through the AAP's regeneration workshops confirms that periodontal regeneration in intrabony defects (vertical bone losses between teeth) is biologically possible on previously diseased root surfaces, evidenced by gains in clinical attachment level, decreased probing depth, and radiographic bone height gain. The key phrase there is "after the infection is controlled."
Here's the honest limit though: horizontal bone loss (where bone has receded evenly across a broad area) is far less amenable to regeneration than isolated vertical or intrabony defects. If your bone loss is widespread and shallow, the regenerative procedures that work well for deep, narrow defects may not be the right tool. A periodontist will assess the architecture of the defect before recommending surgery, because throwing a regenerative procedure at the wrong defect type is both expensive and unlikely to succeed.
It's also useful to understand this alongside what other dental structures can and can't do. For instance, why teeth don't grow back explains the broader biological picture of why adult dental tissues have such limited self-repair capacity. Bone is actually more regeneratively capable than most dental tissues, but it still needs the right environment and usually professional help to do it.
The factors that determine whether your bone can come back
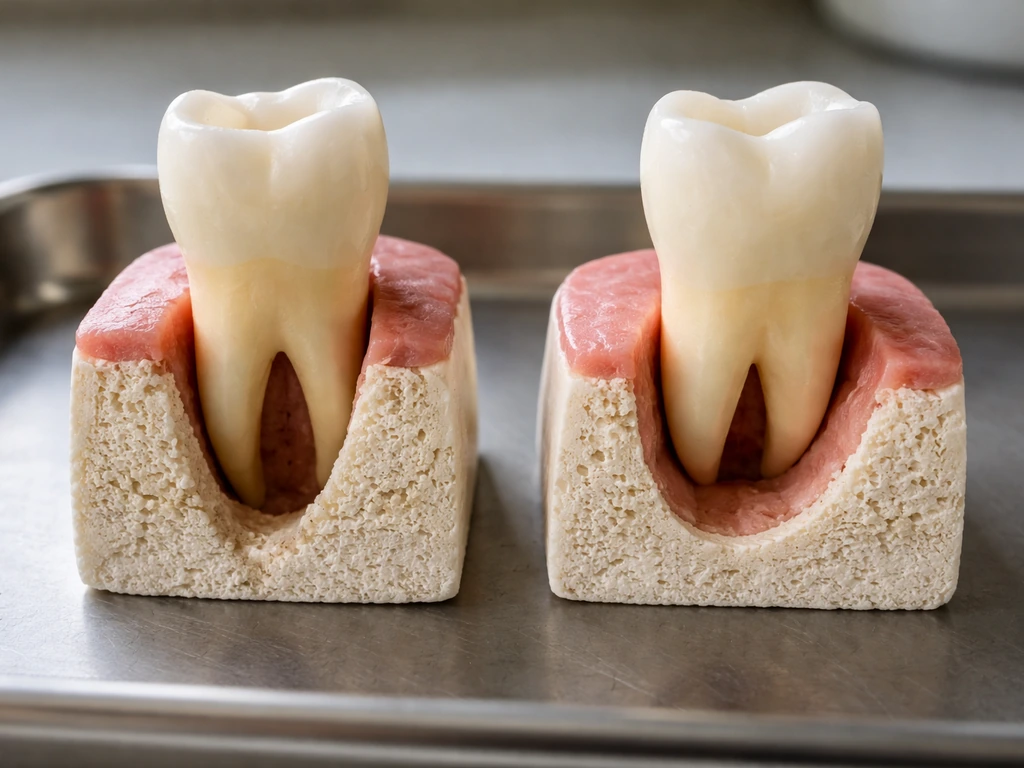
Not all bone loss situations are equal. Several factors heavily influence whether regeneration is realistic in your specific case:
- Defect type and depth: Narrow, deep intrabony defects (especially three-wall defects surrounded by bone on multiple sides) respond best to regenerative procedures. Wide, shallow, or one-wall defects have much less regenerative potential.
- How long the bone loss has been there: Recent, acute bone loss during an active infection that gets controlled quickly gives the bone better odds than decades of slow, chronic destruction.
- Severity: Mild to moderate bone loss has far better outcomes than advanced loss where the tooth is already mobile or has lost most of its root support.
- Smoking: This is a big one. Smokers have significantly worse outcomes from periodontal regeneration procedures. Smoking impairs blood supply, healing, and immune response in a way that directly undermines the regeneration process.
- Diabetes control: Uncontrolled blood sugar worsens periodontal disease and impairs healing. Well-controlled diabetics can still be good candidates for treatment, but it changes the risk profile.
- Age: Younger patients generally have better healing capacity, though periodontitis in younger people can sometimes be more aggressive. Age alone is rarely a hard barrier to treatment.
- Oral hygiene: If the bacterial cause of the disease isn't eliminated through excellent daily hygiene and professional cleaning, any bone that does regenerate is at risk of being lost again.
- Remaining root structure: If the root of the tooth is intact and the tooth is not mobile or is only slightly mobile, that's a much better starting point than a severely compromised tooth.
There's also the matter of what's happening at the root level. The root surface itself plays a role in whether new attachment can form. Can teeth roots grow back is a related question worth understanding because the health and integrity of the root surface directly affects how well regenerative procedures work.
Practical treatments to rebuild bone around teeth right now
The European Federation of Periodontology's S3-level clinical practice guideline emphasizes a staged approach: you don't jump to surgery first. Initial periodontal therapy, including scaling and root planing (deep cleaning), is the foundation. This removes the bacterial deposits and biofilm driving inflammation. For many patients with moderate disease, this alone can result in significant pocket reduction and some bone stabilization. But for cases with residual deep pockets and intrabony defects after initial therapy, that's when regenerative surgery becomes the appropriate next conversation.
Scaling and root planing (deep cleaning)
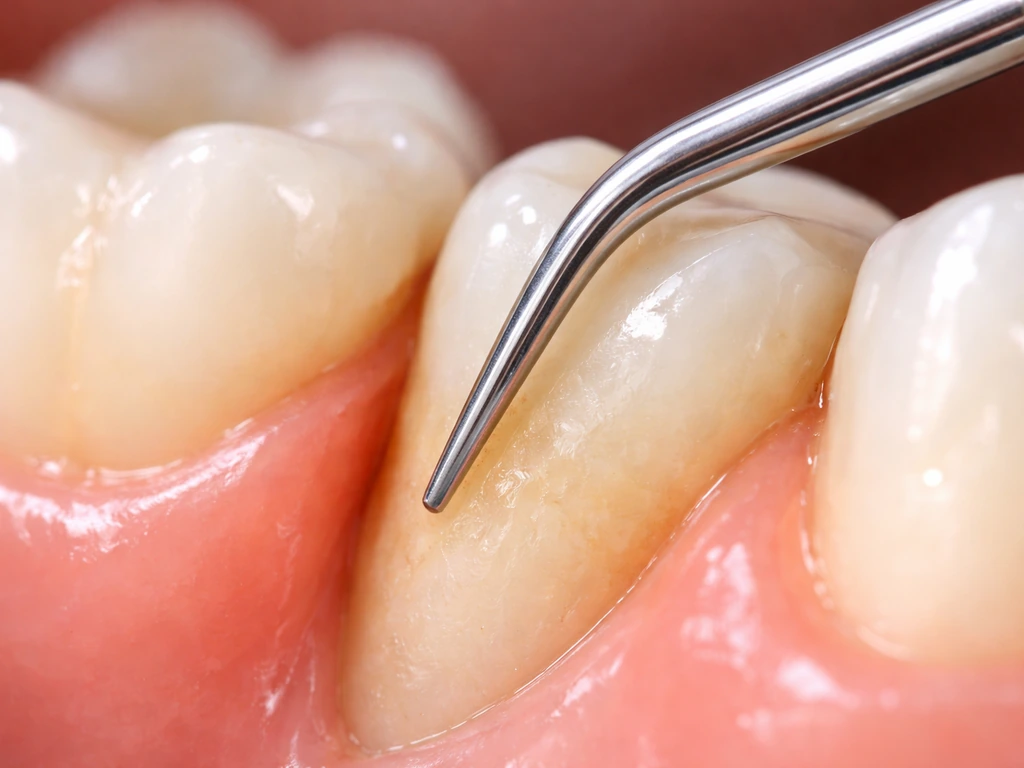
This is step one for virtually everyone with periodontitis. Done under local anesthetic, it cleans bacterial deposits from below the gumline and smooths the root surface so the gum tissue can reattach. It doesn't rebuild lost bone directly, but it stops the active destruction and creates the conditions where some healing can occur. Research supports roughly 1.2 to 1.3 mm of additional clinical attachment gain when this is combined with other adjunctive approaches.
Bone grafting
Bone grafts place material (from your own body, a donor, an animal source, or synthetic material) into the defect to provide a scaffold for new bone to grow into. The graft itself may or may not stay permanently. Some materials are resorbed and replaced by your own bone; others act as a permanent filler. Either way, bone grafts are one of the most widely used tools in periodontal regeneration and have strong evidence for improving radiographic defect fill and clinical attachment in appropriately selected cases.
Guided tissue regeneration (GTR)
GTR uses barrier membranes placed over the defect to physically block faster-growing tissues (like gingival epithelium) from filling the space before the slower-growing bone and periodontal ligament progenitor cells can repopulate it. The concept is simple: give the right cells time and space to do their job. This technique, which Cochrane has reviewed extensively, consistently shows improvements in clinical attachment and radiographic bone fill for infrabony defects. Membranes may be resorbable (dissolve on their own) or non-resorbable (requiring a second procedure to remove).
Biologic agents and growth factors
Enamel matrix derivative (EMD, sold as Emdogain) is a protein preparation that mimics the signals involved in tooth root development and helps stimulate regeneration. It's often combined with bone grafts. Studies comparing EMD plus autogenous bone grafting to controls have shown greater tissue formation with the combination approach. Platelet-rich fibrin (PRF), derived from the patient's own blood, is another biologic adjunct with a growing evidence base. A 2024 network meta-analysis evaluated PRF for periodontal intrabony defects, showing it contributes meaningfully to probing depth reduction and radiographic bone fill outcomes. Recombinant human bone morphogenetic protein-2 (rhBMP-2) is another option studied for intrabony defects, compared against open flap debridement and other biomaterials, with radiographic outcomes supporting its use in select cases.
Comparing the main treatment approaches
| Treatment | Best suited for | Expected outcome | Invasiveness |
|---|---|---|---|
| Scaling and root planing | Mild to moderate periodontitis; all cases as first step | Pocket reduction, some healing; not direct bone regrowth | Non-surgical |
| Bone graft | Intrabony defects, post-extraction sites | Radiographic bone fill; scaffold for new bone | Surgical |
| Guided tissue regeneration (GTR) | Narrow, deep intrabony and furcation defects | CAL gain, pocket reduction, defect fill | Surgical |
| EMD (Emdogain) | Intrabony defects, often combined with graft | Stimulates new attachment; comparable to GTR | Surgical |
| PRF / growth factors | Adjunct to surgery for enhanced healing | Improved defect fill and attachment gain | Surgical |
| rhBMP-2 | Selected complex intrabony cases | Radiographic bone gain vs. debridement alone | Surgical |
How to decide what to do next
If you've been diagnosed with bone loss around your teeth, or you suspect something is wrong, the first move is straightforward: see a periodontist, not just a general dentist. General dentists are great for many things, but a periodontist has specialized training specifically in the bone and gum structures at stake here. They can take a full-mouth series of X-rays and do a comprehensive periodontal charting to map exactly how much bone you've lost, where, and what kind of defect it is. That information determines which treatment path makes sense.
Before or during that appointment, here are the questions worth asking:
- How much bone have I lost, and is it horizontal or vertical (intrabony) loss?
- Is my disease currently active or has the infection been controlled?
- Am I a candidate for regenerative surgery, and if not, why not?
- Which regenerative approach would you recommend for my defect type, and what outcomes can I realistically expect?
- What does my X-ray show now, and what would a successful outcome look like on a follow-up X-ray in 12 months?
- What happens if I only do the deep cleaning and skip surgery?
- Are there any systemic factors in my case (like diabetes or smoking history) that change the prognosis?
- How will we know if the treatment worked?
There are also some red flags that mean you should get in to see someone promptly rather than waiting for a routine appointment. Loose teeth that weren't loose before, teeth that have visibly shifted or drifted, a bad taste in your mouth that doesn't go away, gums that bleed consistently when you brush or eat, and visible lengthening of your teeth (which signals gum recession exposing more root) are all warning signs that bone loss may be actively progressing. Don't wait on these.
It's also worth knowing that the surrounding dental structures matter too. Bone loss doesn't happen in isolation. The nerves, the dentin, the enamel, and the root surface all interact. For instance, exposed root surfaces from bone loss are vulnerable to sensitivity and decay because root dentin isn't as hard as enamel. If you're dealing with sensitivity alongside your gum issues, understanding does dentin grow back can help you understand what's happening to the root surfaces as they become exposed. Similarly, can teeth nerves grow back addresses what happens to pulp tissue and nerve function when the supporting structure around a tooth is compromised.
One more practical point: if your bone loss is the result of periodontitis, treatment is not a one-time fix. Even after successful regenerative surgery, you'll need maintenance visits every three to four months indefinitely to keep the disease from returning. The biology that allowed the bone to be lost in the first place doesn't disappear. The bacteria in your mouth that cause periodontitis are always present; the goal is to keep them at levels your body can manage. Patients who do well long-term are the ones who stay committed to maintenance.
Enamel, as a completely different tissue, is often discussed alongside bone loss because gum recession and bone loss frequently expose root surfaces and damage protective layers. If you're wondering about the harder outer layers of your teeth in parallel, can enamel grow back and how long does it take for enamel to grow back will give you the full picture on what's happening to your tooth surfaces while you're dealing with the bone and gum situation below.
The bottom line: bone can come back around teeth, partially and with professional help, in the right cases. It does not happen on its own, it does not happen quickly, and it requires controlling the cause of the loss before any regeneration is attempted. If you're sitting with a diagnosis of bone loss right now, that's your cue to get to a periodontist, understand your defect type, complete the initial therapy first, and then have a real conversation about whether surgical regeneration makes sense for your situation. That's the practical path forward.
FAQ
If I start better brushing and flossing today, will bone naturally grow back around my teeth?
Yes, but only after the disease is controlled. If inflammation and infection are still active, any regenerative attempt is less likely to “stick,” so the typical sequence is deep cleaning first, then reassessment of pockets and defect shape before surgery.
How can I tell whether the treatment will truly regenerate bone, or just fill the defect?
You might see improvement on X-rays without full periodontal regeneration. “Bone fill” and “true regeneration” are different outcomes, so it helps to ask your periodontist whether your defect is intrabony or horizontal, because intrabony defects have the best chance for meaningful regeneration.
Does regeneration work the same for shallow bone loss versus deep vertical bone loss?
Large, shallow horizontal bone loss across many teeth is usually harder to regenerate than a deep, narrow vertical (intrabony) defect. This is why the diagnosis should include probing depth pattern and bone architecture, not just the fact that bone is “low.”
What if my bone doesn’t come back completely after treatment?
Not always. Even after successful surgery, you can still have residual pocketing, gum recession, or partial attachment gain, and those outcomes still count as progress. Ask what outcomes are realistic for your measurements (CAL gain, probing depth reduction, and expected stability over time).
Which regeneration option is best for me, graft, membrane, EMD, PRF, or something else?
Platelet-rich fibrin, EMD, membranes, and graft materials can be helpful, but they are chosen based on defect type, tooth/root conditions, and your risk factors. A common mistake is asking which material is “best” without understanding whether your defect is the right match for that approach.
Do lifestyle factors like smoking or diabetes affect whether bone can regrow?
Smoking and uncontrolled diabetes are major risk modifiers for periodontal healing. If you use nicotine, ask your periodontist about a cessation plan before surgery, and if you have diabetes ask for coordination with your clinician to optimize glucose because regeneration success drops when healing conditions are poor.
If my teeth are loose, can regeneration still help?
Yes. When teeth become mobile, the supporting ligament and bone support may be too compromised for full regeneration to solve the problem. Your periodontist may discuss splinting, occlusal management, or a stabilization plan alongside any regenerative procedure.
How often will I need follow-up after regeneration treatment?
After active periodontal therapy and any regenerative surgery, maintenance visits are essential, often every 3 to 4 months. Skipping maintenance increases the chance of recurrence, which can reverse the gains and gradually reintroduce pocketing and further bone loss.
Will I need another procedure to remove the membrane or graft?
A second surgery is sometimes required if you use a non-resorbable membrane. If your plan includes membranes or certain graft types, ask whether the material is expected to dissolve and whether you should anticipate an additional procedure for removal.
When should I expect to know whether bone has actually improved after treatment?
You should expect a period of healing and stabilization, and the assessment is usually based on updated probing measurements and imaging after healing time, not immediately. Ask your periodontist when your “re-evaluation” scan and charting will be scheduled so you know what timeline to use for decision-making.
Learn why teeth and enamel dont regenerate, what happens after loss, and the practical options for fixing gaps.
Learn if enamel can regrow, why it cannot, and how fluoride and remineralization can repair early damage.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn

