No, gums do not grow back once they recede. This is one of the most persistent misconceptions in dental health, and it shows up constantly in Reddit threads because people desperately want a different answer. The honest truth is that gum tissue lost to recession is gone for good unless a dentist or periodontist physically replaces it. What you can do, though, is stop it from getting worse, improve how the tissue looks and feels by reducing inflammation, and in some cases use clinical procedures to physically restore coverage over exposed roots. That distinction between true regrowth and stabilization or repair is the whole ballgame when it comes to gum recession. If you're wondering, "if your smiley rips will it grow back," the answer is that true gum regrowth is unlikely, but preventing further recession and getting the right care can help restore coverage and appearance.
Can Gums Grow Back? Reddit Answers and What to Do Now
What "grow back" actually means (and why gums can't do it)
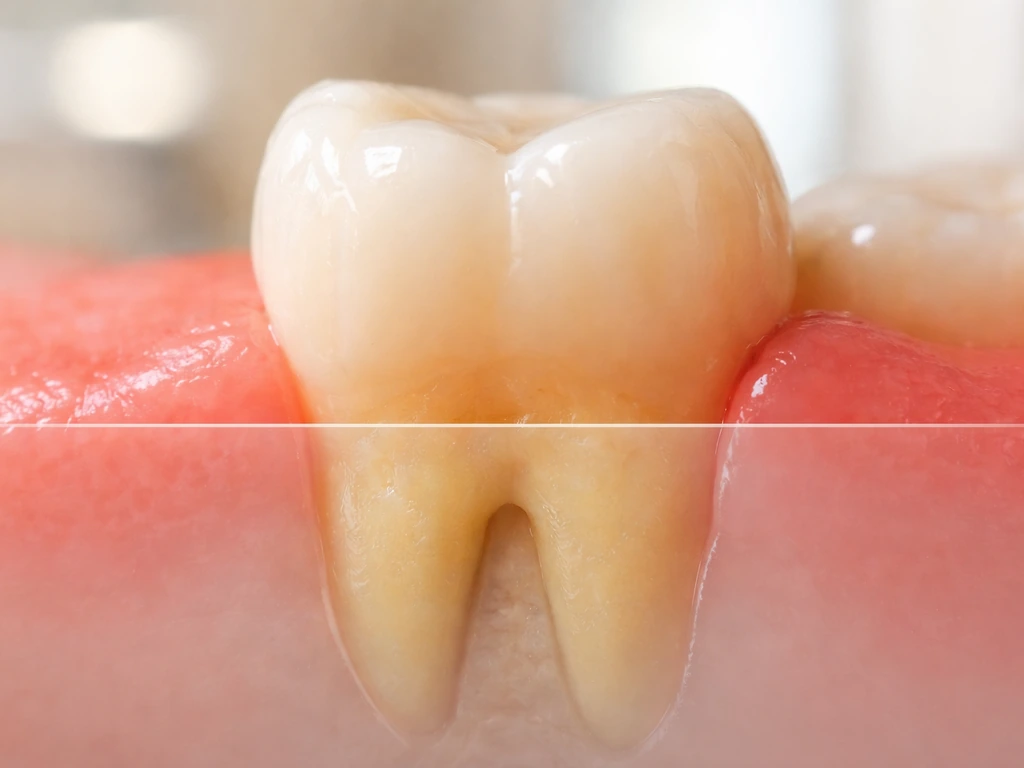
When people say they want their gums to grow back, they usually mean one of two things: they want the tissue to creep back up and cover the exposed root surface, or they want the jawbone and attachment structures underneath to rebuild themselves. Neither happens naturally. Gingival tissue is not like skin that heals a scrape. The periodontal attachment apparatus, which includes cementum on the tooth root, the periodontal ligament, and the alveolar bone, is a highly specialized structure. Once it's destroyed by disease, trauma, or mechanical damage, it does not regenerate on its own.
The science here is well established. Periodontitis is defined as a destructive, chronic inflammatory disease involving loss of attachment and alveolar bone resorption. The key word is destructive: this isn't just inflammation you can dial back. The tissue is gone. Gingivitis, on the other hand, is inflammation of the gingiva without bone or attachment loss, and that is reversible with good oral hygiene. This difference matters enormously. If your gums look slightly puffy and swollen from gingivitis, treating the inflammation can make them appear to "return to normal." But if you have actual recession where the gum margin has migrated down the tooth, that margin is not coming back on its own.
Why receding gums usually don't fully come back
The biology is straightforward but unforgiving. Gum tissue that has receded has lost its attachment to the underlying bone and root surface. The cells responsible for maintaining that attachment, the periodontal ligament fibroblasts, cementoblasts, and osteoblasts, don't spontaneously repopulate and rebuild the lost structure. Even with modern regenerative techniques, true regeneration, meaning new cementum, new periodontal ligament insertion, and new alveolar bone, is difficult to achieve and is never guaranteed. Research into guided tissue regeneration, bone grafting, and enamel matrix derivatives confirms that outcomes vary widely and full restoration is not a reliable expectation.
Bone loss compounds the problem. Once the bone that supports the gum tissue has resorbed, the gum has nothing to sit on. Horizontal bone loss in particular is notoriously resistant to regeneration. The gingiva reflects the level of the underlying bone, so even if you control all the inflammation perfectly, the tissue can't sit higher than the bone supports it. This is why periodontists focus so heavily on staging and grading using clinical attachment loss (CAL), because the amount of destroyed tissue determines what's realistically salvageable.
What you might notice that feels like regrowth (but isn't)

Here's where Reddit threads get confusing. A lot of people report that their gums "came back" after they started flossing or switched to a gentler toothbrush, and sometimes that's partially true. Inflamed gum tissue is swollen and puffy. When you treat the inflammation through better oral hygiene, the tissue tightens up and looks healthier. This can make gums appear less receded because the swelling is gone and the tissue looks more defined. But the actual gum margin, the level where the gum attaches to the tooth, has not moved. What improved is gingival health, not gingival position.
Stabilization is the other thing people notice and interpret as regrowth. If recession stops progressing, which it can with proper care, the teeth no longer look like they're getting longer month by month. That stability feels like improvement, and it is, but the lost tissue is still gone. Partial improvement in appearance can also occur after treatment like scaling and root planing, because removing calculus buildup and controlling infection allows the tissue to become less inflamed and sit more naturally. Again, this is health improvement, not regeneration.
Common causes of gum recession, and how to figure out yours
Knowing your specific cause matters because it determines what you do next. The most common drivers of recession include gum disease (periodontitis), aggressive or improper toothbrushing technique, thin gum tissue biotype (some people are just born with less gum tissue), smoking and tobacco use, tooth malposition or crowding, and trauma to the gum tissue. If dipping is one of your habits, it can contribute to gum recession and make it less likely to improve on its own. Orthodontic treatment can also contribute depending on the direction teeth are moved and the thickness of supporting bone. Some people have a genetic predisposition to thin tissue that recedes more easily regardless of how carefully they brush.
To figure out your cause, think about where the recession is happening. Recession that's localized to one or two teeth and appears on the outer (cheek-side) surface, especially on a tooth that sticks out slightly, often points to brushing trauma or tooth malposition. Recession that's generalized across multiple teeth and accompanied by bleeding, bad breath, and deep pockets is more likely periodontal disease. If you're a tobacco user, that's almost certainly a contributing factor regardless of other causes. A periodontist can measure probing depth, clinical attachment loss, and recession at each tooth to give you a precise picture.
| Cause | Typical recession pattern | Key sign |
|---|---|---|
| Aggressive brushing | Localized, outer surface, often canines/premolars | Notching or wedge-shaped wear at gumline |
| Periodontal disease | Generalized, multiple teeth, between teeth too | Bleeding, bad breath, deep pockets |
| Thin tissue biotype | Often localized, minimal inflammation | Naturally thin, fragile gum tissue |
| Smoking/tobacco | Can be generalized, often masked inflammation | Reduced bleeding despite disease activity |
| Tooth malposition | Single tooth, labial surface | Tooth visibly outside arch or rotated |
| Orthodontic treatment | Along moved teeth | Recession developed or worsened during/after treatment |
| Trauma/injury | Localized to injury site | History of impact, lip/cheek piercing, or habits |
What you can do at home right now

The goal at home is to stop the recession from progressing while you arrange professional evaluation. You can't grow tissue back on your own, but you can absolutely prevent further loss, and that matters enormously for your long-term outcome.
- Switch to a soft-bristle toothbrush immediately and use a gentle circular or Bass technique, not horizontal scrubbing. Research on brushing force links excessive pressure and bristle stiffness to gingival recession and tooth wear, so this change is not optional.
- If you use a power toothbrush, let the brush do the work and don't press it into the gum. Studies comparing manual and oscillating-rotating brushes found no significant difference in recession outcomes when technique is controlled, so it's technique and force that matter more than the type of brush.
- Floss daily. Inflammation between the teeth from plaque buildup contributes to attachment loss. Consistent flossing removes biofilm that your brush can't reach.
- Stop smoking or using any tobacco products. Tobacco impairs healing, masks gum disease symptoms by suppressing bleeding, and is one of the most direct contributors to recession and periodontitis progression.
- Avoid mouthwashes with high alcohol content that irritate tissue. If your dentist recommends it, a chlorhexidine rinse can help control gingivitis, though it's a short-term tool and should be used exactly as directed (don't rinse with water immediately afterward, and don't use it indefinitely).
- Don't use whitening or abrasive products aggressively on already-exposed root surfaces. Exposed root dentin is softer than enamel and wears more easily.
These steps will help control inflammation and prevent further mechanical damage, but they are not a substitute for professional evaluation. Gum recession is progressive when left unmanaged, and the longer structural loss continues, the fewer options you have. Book an appointment soon, not someday.
When you need a dentist or periodontist, not just home care
If your recession is already visible, meaning you can see the root surface or your teeth look noticeably longer than they used to, you need a professional assessment. A general dentist can do an initial evaluation, but a periodontist is the specialist for this. They will measure probing depths and clinical attachment levels at multiple points on each tooth, check for bleeding on probing and any pocketing, take radiographs to assess bone levels, and determine whether your recession is stable or actively progressing.
If periodontitis is involved, the first step before any surgical or cosmetic consideration is non-surgical therapy: scaling and root planing (deep cleaning). This removes calculus, bacterial biofilm, and infected tissue from below the gumline, providing a biologically clean root surface that allows the gum tissue to reattach or at least stabilize. This is not optional if disease is present. No graft or cosmetic procedure will succeed long-term on a mouth with active periodontal infection.
Clinical options when gums won't come back on their own
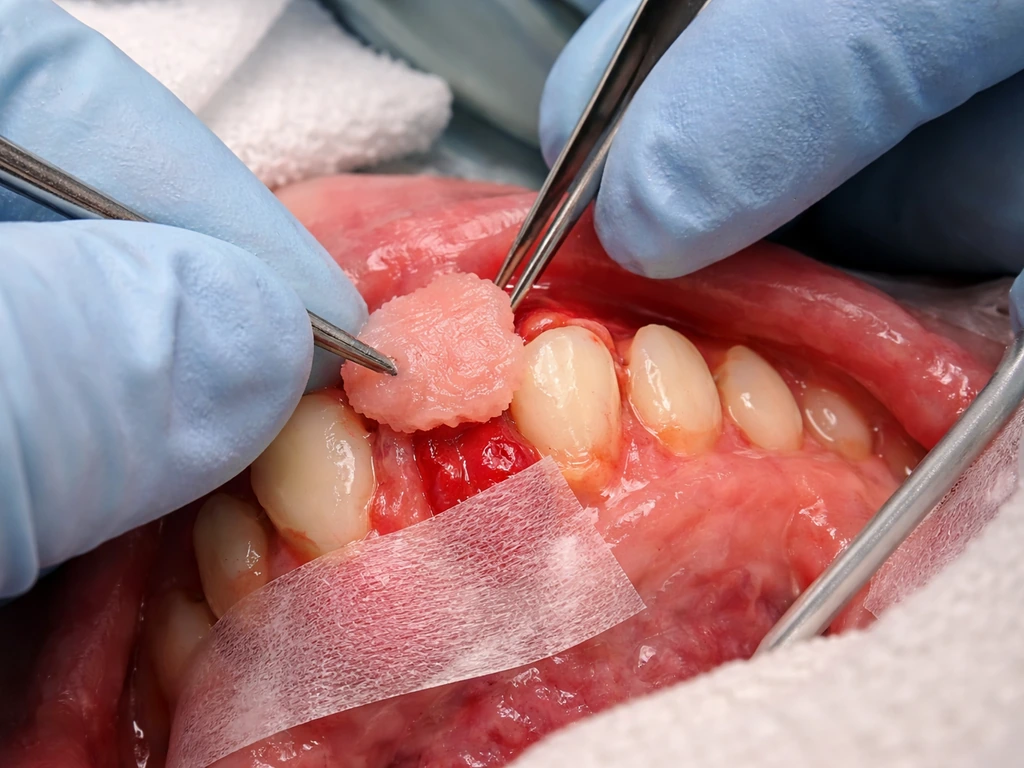
Once disease is controlled and recession is stable, several procedures can physically restore gum coverage over exposed roots. These don't make the body regrow tissue, they transplant or reposition existing tissue to cover what's missing.
Subepithelial connective tissue graft (SCTG)
This is considered the gold standard for root coverage. Tissue is taken from the roof of your mouth (the palate) and placed under a flap at the recession site. AAP consensus data confirms SCTG provides the best root coverage outcomes among periodontal soft tissue procedures. It's proven, predictable in the right candidates, and can significantly improve both function and aesthetics.
Coronally advanced flap (CAF)
This procedure repositions your existing gum tissue upward to cover exposed roots without taking tissue from the palate. It works best for Miller Class I and II recession defects where there's adequate tissue height nearby. When combined with adjuncts like enamel matrix derivative, research shows an enhanced probability of complete root coverage for localized recession.
Guided tissue regeneration (GTR) and bone grafting
When bone loss is involved, periodontists may use barrier membranes and/or bone grafts to encourage the body to regenerate lost supporting structures. These approaches aim to restore the periodontal ligament, cementum, and alveolar bone, though outcomes vary. True regeneration of the full attachment apparatus is achievable in some defect types (particularly vertical or angular bone loss) but not reliably in all situations.
Enamel matrix derivatives (Emdogain)
Emdogain is a protein-based gel derived from developing tooth tissue that is applied to the root surface during surgery to stimulate regeneration of periodontal structures. It is often used in combination with grafting or CAF procedures. Research confirms it can improve outcomes, particularly in intrabony defects, though it's not a standalone fix and works best as part of a comprehensive surgical plan.
Realistic outcomes, timelines, and keeping what you have
After non-surgical treatment like scaling and root planing, tissue often looks and feels better within a few weeks as inflammation resolves. A re-evaluation usually happens 4 to 8 weeks after deep cleaning to assess whether pockets have reduced and whether surgical intervention is needed. If you have a graft or a CAF procedure, initial healing takes 2 to 4 weeks, but full maturation of the tissue can take 6 to 12 months. If you are dealing with gum recession, the most important timing question is whether it is stabilizing or progressing, because true regrowth is typically not expected. You won't see the final result immediately.
Root coverage procedures don't always achieve 100 percent coverage, and outcomes depend heavily on the severity and class of the recession defect, the thickness of available tissue, your overall periodontal health, and whether you stop contributing factors like smoking. Predictable complete coverage is most realistic for shallow, localized recession without significant bone loss. Deeper, generalized recession with bone involvement is harder to fully correct.
After treatment, periodontal maintenance visits are critical. For patients with a history of periodontitis, the AAP has recommended visits at roughly three-month intervals initially, with schedules adjusted based on individual risk over time. Skipping maintenance is the most common way people lose the gains they made. Your periodontist will set a specific interval for you based on how your tissue responds.
Preventing further recession is genuinely achievable. Fix your brushing technique, manage gum disease aggressively, attend your maintenance visits, stop tobacco use, and address any bite or tooth position issues your dentist identifies. Recession that is caught and stabilized early leaves far more options on the table than recession that has progressed for years. If you're reading this and wondering whether your situation is urgent: if you can see exposed root surface, feel sensitivity to cold or touch on the root, or notice your teeth look longer than they did a year ago, that's your signal to get evaluated now, not later. A chunk of gum that is missing due to recession typically will not grow back by itself, but early evaluation can help stop further loss chunk of gum missing will it grow back.
Related situations like gum tissue loss after a tooth extraction, recession from dipping tobacco, or trauma to oral tissue like a torn frenulum all follow the same core principle: the gum body itself does not regenerate on its own, but professional options exist for each scenario depending on the cause and severity. Whatever the trigger for your recession, the path forward starts with an accurate diagnosis from someone who can actually measure what's happening below the gumline.
FAQ
If my gums look like they “came back” after switching to a softer toothbrush, does that mean they regrew?
Not necessarily. Often this is reduced swelling from inflammation and better tissue tone, so the gum margin can appear higher. True regrowth would require the attachment apparatus to rebuild, which is uncommon. A periodontist can confirm by measuring recession height and probing depths over time.
How can I tell whether my recession is stable versus still getting worse?
Ask your dentist to document baseline measurements (recession height, probing depth, and clinical attachment loss) and then compare them at a follow-up. Visual checks and photos can help, but only repeated clinical measurements show whether the gum margin and attachment level are actually changing.
Does flossing alone reverse gum recession?
Flossing can improve gingival health and reduce bleeding, but it usually cannot move the gum margin back if recession already occurred. If recession is driven by periodontitis or brushing trauma, flossing is supportive, but you still need a plan to control disease and stop mechanical damage.
Can gums grow back naturally if I stop smoking or quit tobacco dips?
Quitting tobacco can slow or halt further recession and improve healing potential, but it does not typically recreate lost gum tissue on its own. Expect stabilization and better response to treatment, not guaranteed regrowth.
Is it safe to use whitening strips or sensitive toothpaste if I have exposed roots?
Sensitive toothpaste is generally helpful for root sensitivity, but avoid aggressive “gum regrowth” products or anything that irritates inflamed tissue. Whitening products can increase sensitivity on exposed roots, so consider discussing options with your dentist, especially if you have active bleeding or pockets.
What brushing technique actually prevents further recession?
Use a soft-bristled brush, light pressure, and a technique that avoids scrubbing the gumline. If recession is localized to the outer surfaces, that pattern can suggest brushing trauma or tooth positioning issues, and a clinician may recommend a specific method and possibly an evaluation for orthodontic factors.
If I already have gum recession, should I still get deep cleaning (scaling and root planing)?
If there is periodontitis, deep cleaning is usually the first priority before any cosmetic root coverage attempts. Without controlling infection and inflammation, grafts and flap procedures are less likely to last long-term.
What’s the difference between “root coverage” and “gums growing back”?
Root coverage procedures reposition or transplant existing tissue to cover exposed root surfaces, they do not reliably rebuild the original periodontal attachment in a way that equals true biological regrowth. The realistic goal is improved coverage, comfort, and appearance, with stabilization as the priority.
Are there situations where true regeneration is more realistic?
Regeneration of the deeper supporting structures can be more achievable in selected defect types, especially certain intrabony scenarios, but it is not guaranteed for every recession case. Your periodontist’s measurements and imaging determine whether the defect has the conditions needed for better regenerative outcomes.
How long will it take to see results after gum grafting or CAF?
Inflammation usually improves within a few weeks, but tissue maturation can take months. Commonly, initial healing is about 2 to 4 weeks, with longer consolidation and final appearance often taking 6 to 12 months depending on the procedure and healing response.
Will my gums “re-recede” after surgery if I stop maintenance visits?
Yes, risk is high. Periodontal maintenance is what protects the gains from both non-surgical and surgical care. Many people lose improvement when they skip scheduled cleanings and re-evaluations, especially if they had periodontitis.
Should I be worried if recession is only on one or two teeth?
It depends on the cause. Localized recession is often related to brushing trauma, tooth position, or anatomy, and it can still be managed effectively, but you still need measurements to rule out disease. Ask for assessment of probing depth and clinical attachment loss at those specific teeth.
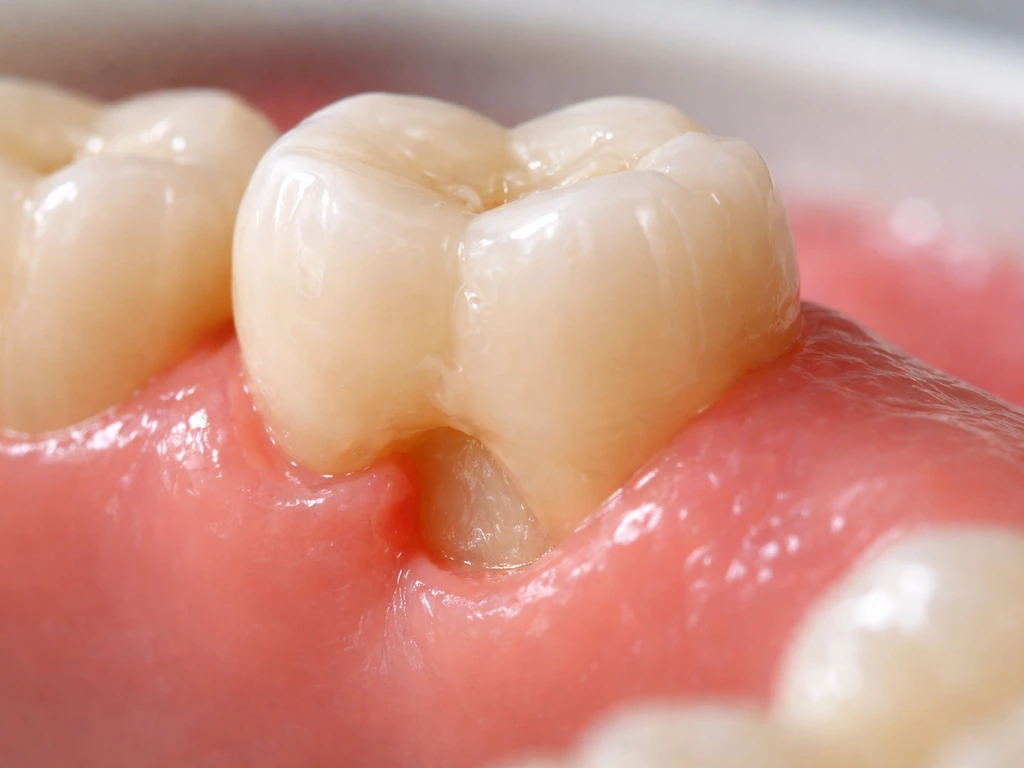
When a chunk of gum is missing, get clear answers on regrowth limits, causes, healing timelines, and next steps.
Find out if a torn tooth or gum will regrow, what heals in days, what won’t, and when to see an emergency dentist.
Timeline for gum healing after recession or injury, factors affecting regrowth, and when you need dental care

