The surface gum tissue does grow back after a tooth extraction, but only partially and only in a specific way. The soft tissue closes over the socket within about 3 to 4 weeks. What does not come back on its own is the full volume of gum you had before, especially if bone underneath remodels and shrinks. So the honest answer is: yes, your gums will cover the hole, but the area may look or feel different than it did when the tooth was there.
Does Gum Tissue Grow Back After Extraction? What to Expect
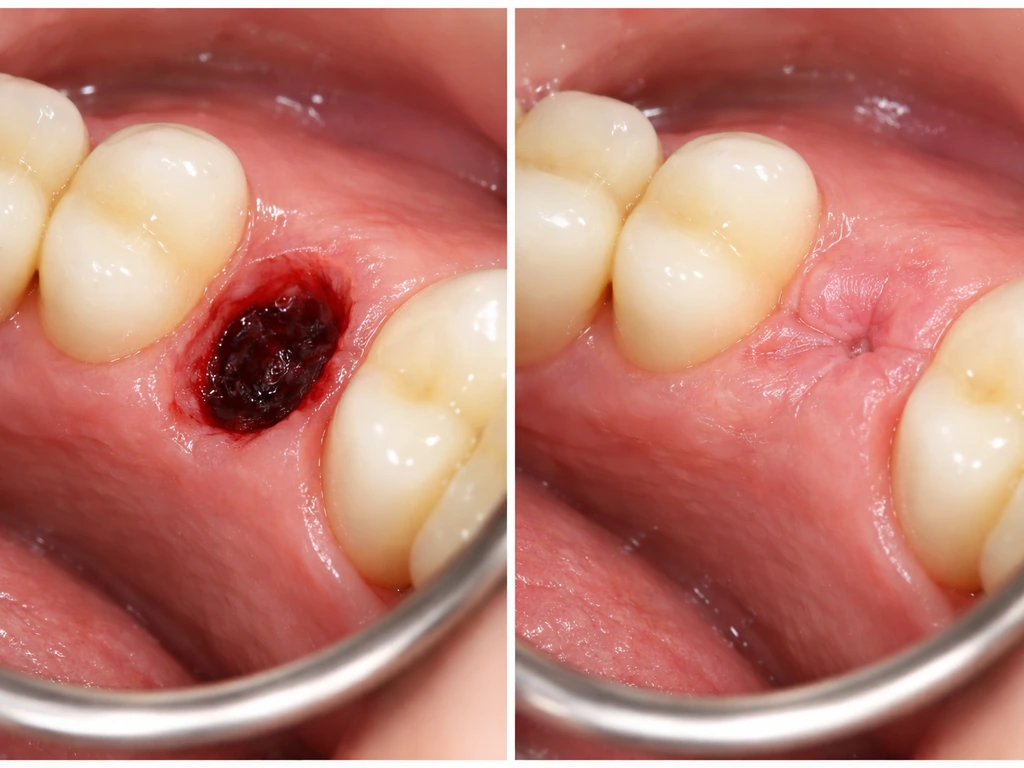
What actually happens to gum tissue after an extraction
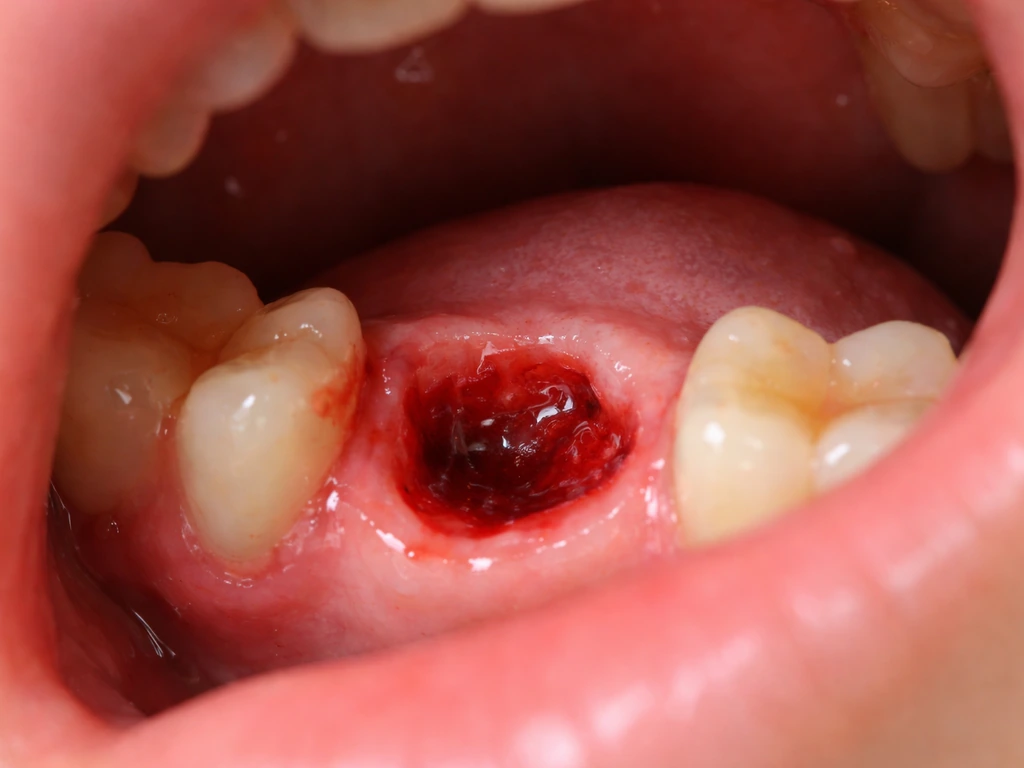
Right after a tooth is pulled, the socket fills with a blood clot. That clot is critical. It is not just plugging a hole, it is the foundation for everything that heals next. Within the first week, the clot is replaced by granulation tissue, which is a soft, vascular tissue that starts the process of filling the socket. Epithelial cells (the cells that make up the surface layer of your gum) begin migrating inward from the edges of the socket around day 4 or 5. By about day 24, research shows this epithelialization is complete and the surface is closed over. Around 4 weeks post-extraction, most people have full soft-tissue closure of the socket.
That sounds reassuring, and it is, but here is where expectations need to be realistic. The gum tissue that covers the socket is new surface tissue, not a full reconstruction of the gum architecture. The height and thickness of the gum depends heavily on what is happening underneath with the bone. After extraction, the alveolar bone (the bone that used to support the tooth root) remodels and partially resorbs. That can reduce the ridge height, which in turn means less gum volume. This is normal biology, not a sign something went wrong.
What affects how well gum heals
The type and complexity of the extraction

A straightforward extraction of an erupted tooth with minimal trauma heals faster and more cleanly than a surgical extraction of an impacted wisdom tooth. When bone needs to be removed or a flap of gum is cut and sutured back, the tissue has more to repair. Sutured sites may look more uneven early on, but the sutures actually help the tissue align better during healing.
The thickness of your bone and gum biotype
People with a thin periodontal biotype (thin gum tissue and thin underlying bone) tend to experience more ridge resorption after extraction than people with a thick biotype. Research confirms that a thin buccal (cheek-side) bone plate leads to greater bone loss after extraction even with careful, flapless technique. Less bone means less support for the overlying gum, which is one reason some people notice a visible dip or concavity in the gum line after a tooth is removed.
Smoking and tobacco use

Smoking is one of the most documented factors that impairs post-extraction healing. It increases the risk of dry socket significantly, and research shows it slows soft-tissue healing measurably in smokers versus non-smokers. This applies to both cigarettes and smokeless tobacco. The CDC links tobacco use directly to greater periodontal disease and alveolar bone loss, both of which compound the problem after an extraction.
Age, medications, and systemic factors
Younger patients generally heal faster because cell turnover is quicker. Older adults, or anyone with diabetes, immune suppression, or who takes medications that affect bone (like certain bisphosphonates), may see slower or less complete tissue repair. For women on oral contraceptives, there is also a documented increased risk of alveolar osteitis (dry socket) after third molar extractions, with research suggesting timing the extraction during days 23 to 28 of the pill cycle may reduce that risk.
Pre-existing gum disease
If the tooth was extracted because of advanced periodontal disease, the surrounding gum and bone were already compromised before the extraction happened. That means there is less healthy tissue available to heal and close the site properly. This is a common reason why some people find healing is slower or the gum coverage looks incomplete.
Is that 'missing gum' actually what you think it is?
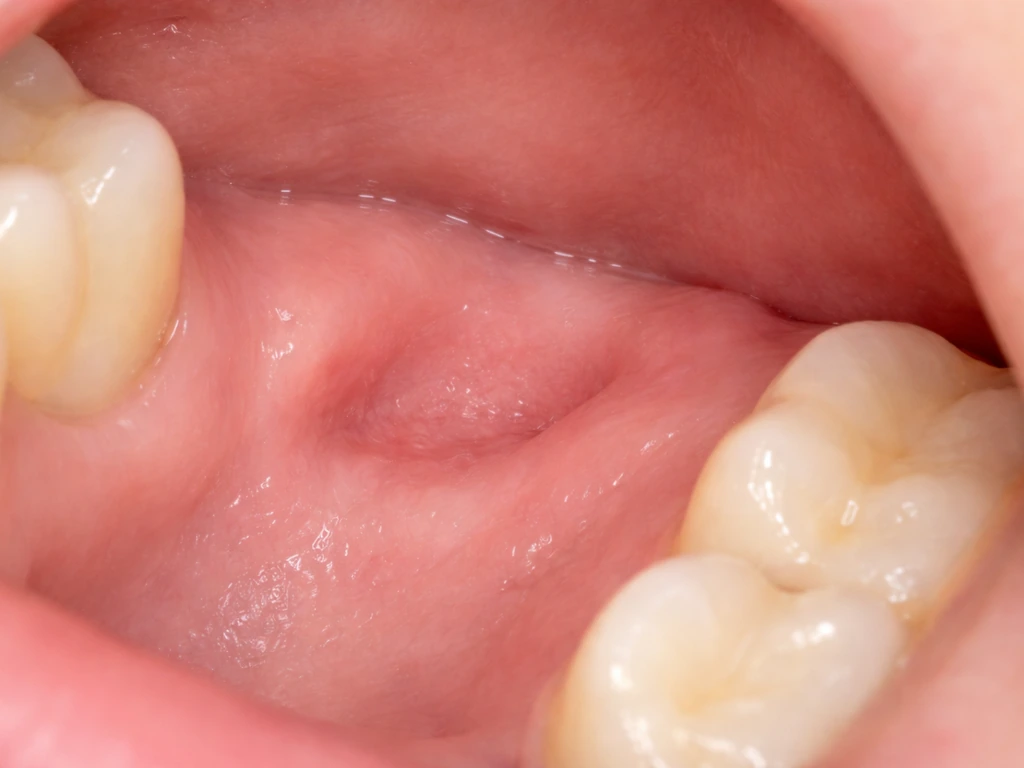
A lot of people look at the extraction site a week or two later and think their gums look wrong or receded. Sometimes they are right, and sometimes what they are seeing is just normal socket healing at a specific stage. Here is how to tell the difference.
| What you see | What it likely is | Is it a concern? |
|---|---|---|
| Sunken, dark red or pink area in first 1-2 weeks | Normal granulation tissue filling the socket | No, this is expected |
| White or yellowish tissue over the socket around day 3-5 | Fibrin (part of normal clot maturation), not infection | Usually no, unless painful and worsening |
| Gum line looks lower than neighboring teeth after 4+ weeks | Ridge resorption reducing bone and gum volume | Cosmetic concern; worth mentioning to dentist |
| Sharp bony edge or hard lump under the gum | Bony spicule or retained socket wall fragment | Yes, see your dentist |
| Gum that never fully covers the socket | Incomplete epithelialization or underlying bone issue | Yes, needs evaluation |
| Gum recession on adjacent teeth (not just the socket) | Pre-existing or new recession, unrelated to healing | Yes, evaluate separately |
The distinction between normal socket healing and true gum recession matters because they have different causes and different solutions. Recession on a neighboring tooth, for example, is unrelated to the extraction healing process and would need its own evaluation. If you are worried about recession in general, the causes are usually quite different from what happens inside a healing extraction socket.
Warning signs that something is wrong
Most extractions heal without drama. But there are specific signs that mean you should not wait and see.
Dry socket (alveolar osteitis)
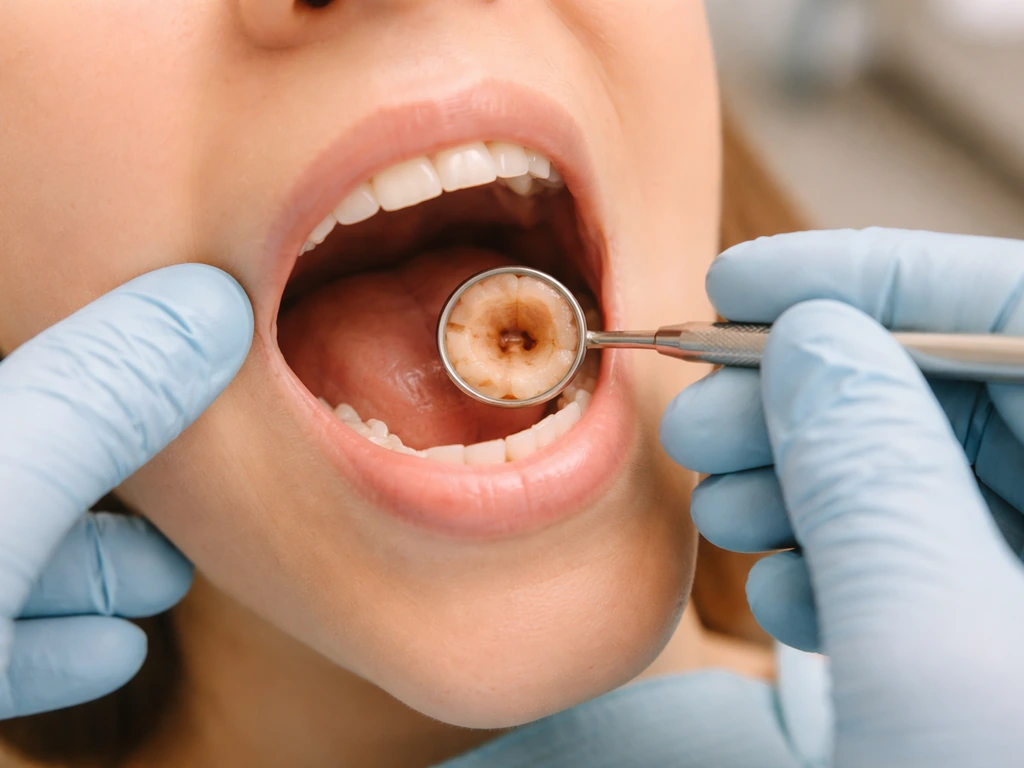
The classic sign of dry socket is pain that starts or significantly worsens 1 to 3 days after the extraction, often radiating to the ear or jaw. You may look at the socket and see an exposed, empty-looking bone rather than a dark clot or pink tissue. Dry socket is not an infection, it is a failure of the clot to form or stay in place, which leaves the bone exposed and hypersensitive. It is more common after lower wisdom tooth extractions, in smokers, and in women on oral contraceptives. Your dentist can pack the socket with a medicated dressing that brings fast relief.
Infection
An infected socket typically shows up at least 7 days after surgery, and usually presents with increasing pain or swelling (not improving), discharge that looks white or yellow (pus), a foul taste, and possibly fever. Swelling that spreads to your cheek, face, or neck is a more serious sign. If you have facial swelling and fever and cannot reach your dentist, go to an emergency room. These are not symptoms to manage at home.
Other red flags worth a call to your dentist
- Pain that is getting worse after the first 3 days instead of gradually improving
- Bleeding that restarts or does not stop after gentle pressure
- Visible bone that is not covered by soft tissue after 2 weeks
- A socket that looks like it is opening back up or not closing after 4 to 6 weeks
- Numbness or tingling in the lip, chin, or tongue that persists beyond the first day or two
- Swelling that returns or increases after it had started improving
What you can do right now to help your gums heal properly
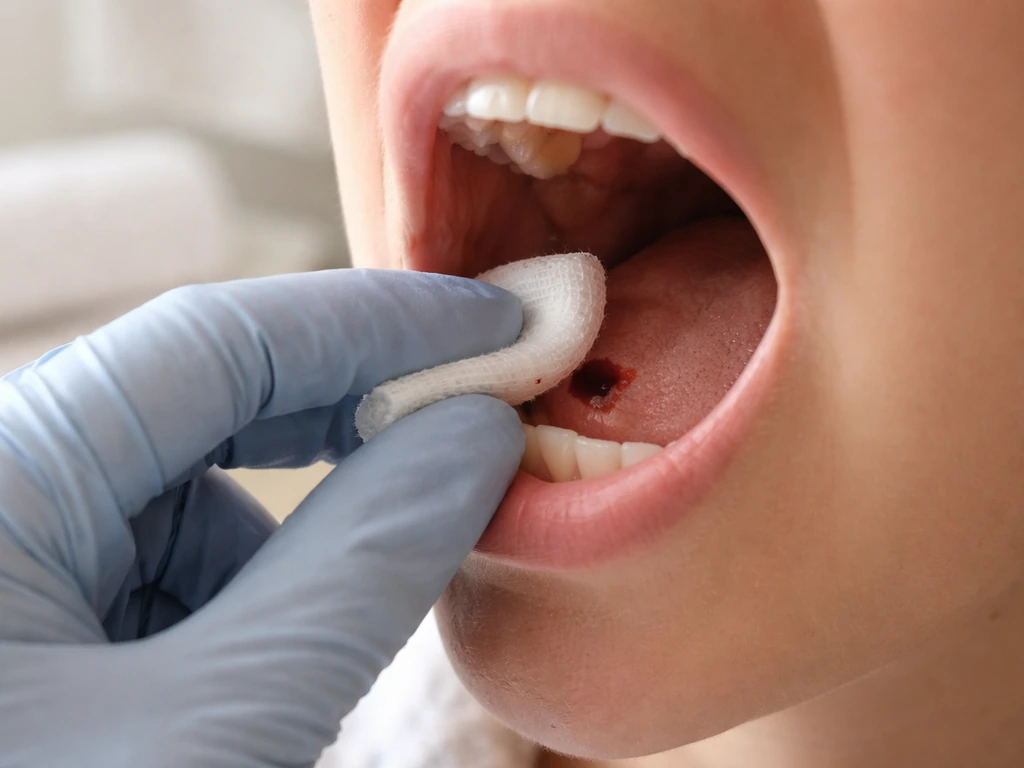
The single most important thing in the first 24 to 48 hours is protecting the blood clot. Almost every aftercare instruction you get from your dentist or oral surgeon is in service of that one goal.
- No straws for at least 72 hours: the suction can physically dislodge the clot. This is not a suggestion you can bend.
- No vigorous rinsing or spitting in the first 24 to 48 hours: again, suction and pressure are the enemy of the clot.
- After the first 24 hours, gentle salt water rinses (a teaspoon of salt in 8 oz of warm water) help keep the site clean without trauma.
- Brush carefully: you can resume brushing after the first day but avoid the extraction site directly for the first 48 hours. Keep the rest of your mouth clean because bacteria elsewhere can migrate.
- Eat soft foods: think yogurt, mashed potatoes, scrambled eggs, soup (not hot). Avoid anything hard, crunchy, or chewy that requires chewing near the site.
- No smoking or tobacco: this is the most impactful thing you can do to prevent dry socket and speed healing. Even a few days without smoking makes a real difference.
- Keep your head elevated when sleeping for the first couple of nights to reduce swelling.
- Take any prescribed medications as directed, including antibiotics if given, and use over-the-counter pain relief as needed to stay comfortable.
Once the socket is past the clot stage (roughly after day 4 to 5), gentle cleaning becomes more important. Food and bacteria that sit in a partially healed socket can slow the process. Most dentists recommend gentle irrigation with a curved-tip syringe after meals once you are a few weeks out, especially for lower molar extraction sites.
What to do if your gums don't fully cover or the area still looks wrong
If you are past the 4 to 6 week mark and the site still does not look right, or if the healed area shows a noticeable loss of gum volume or a visible dip, that is worth a dentist or periodontist evaluation. If you are wondering whether your gums will grow back from dipping, the key takeaway is that soft-tissue closure can happen, but the gum volume may not fully return do your gums grow back from dipping. A chunk of gum that is missing usually refers to a loss of gum volume after healing, so it may not fully grow back without evaluating the gum and underlying bone gum volume or a visible dip. If you are wondering whether gums can grow back, experiences like those discussed on Reddit usually point to the same idea: partial closure happens naturally, but restoring full gum volume may require treatment can gums grow back reddit. Not because something has definitely gone wrong, but because understanding what is happening is the first step to deciding if anything needs to be done.
Ridge and socket preservation
If you are planning an implant or bridge in the future, your dentist may have already discussed socket preservation at the time of extraction. This involves placing bone grafting material into the socket immediately after extraction to slow the natural resorption process. It does not eliminate bone loss entirely, but it significantly reduces the ridge remodeling that otherwise happens and preserves more gum volume for future restorations.
Soft tissue grafting
If you have significant gum recession on adjacent teeth, or if the extraction site healed with inadequate gum tissue coverage for a future restoration, a periodontist may recommend a soft tissue graft. Common options include a connective tissue graft taken from the palate or an allograft (donor tissue). This is a real clinical option, not a last resort, and periodontists do these routinely. The key is getting an evaluation first so you know whether the issue is the gum, the bone, or both, because the treatment differs.
When a bone graft is needed instead
If the problem is primarily volume loss in the underlying bone ridge rather than the gum tissue itself, adding a soft tissue graft alone will not solve it. Bone grafting procedures, either done at the time of extraction or later as a staged approach, can rebuild the ridge before placing an implant. A dentist or oral surgeon will evaluate this with imaging, typically a CBCT scan, to assess what is actually missing and what makes sense to restore.
Realistic timelines for gum healing
Here is what most people can realistically expect, absent complications.
| Timeframe | What is happening | What is normal to see or feel |
|---|---|---|
| Day 1-3 | Blood clot forms and stabilizes | Soreness, minor swelling, blood-tinged saliva, dark clot visible in socket |
| Day 3-7 | Granulation tissue replaces the clot, epithelialization begins | Soreness improving, socket looks pink/red, white film may appear (normal fibrin) |
| Week 2-3 | Epithelial coverage progressing, soft tissue closure underway | Site looks more pink, swelling mostly gone, socket shrinking in appearance |
| Week 4 | Soft tissue closure complete in most cases | Socket surface closed, may still feel tender to pressure, gum may look slightly lower than adjacent teeth |
| 3-6 months | Bone continues to remodel beneath surface tissue | Area feels normal, ridge contour settling, final appearance stabilizes |
| 6+ months | Bone remodeling mostly complete | Final ridge shape visible, implant or restoration planning can proceed if needed |
Most dentists schedule a follow-up at 1 to 2 weeks after extraction, and again around 4 to 6 weeks if there were sutures or a surgical extraction. If your extraction was simple and healing is going normally, you may not be called back in. That does not mean you cannot call with concerns. If anything feels wrong or looks wrong after the first week, contact your dentist rather than waiting. Dry socket and early infections are both much easier to manage when caught within the first week or two.
The bottom line on gum regrowth after extraction is this: the surface heals reliably and relatively quickly, but it does not restore the full tissue architecture that existed before. What you get back is functional closure, not an exact replica. For most people, that is completely fine. For people who need implants, bridges, or who are unhappy with the cosmetic result, there are real options that a dentist or periodontist can walk you through once healing is complete.
FAQ
If my gum looks lower after extraction, does that mean I’m guaranteed to lose more tissue later?
Not usually. The gum closes over the socket in weeks, but the final gum height and thickness are often reduced because the underlying ridge remodels. If you want a more predictable match to the original gum contour, the decision is usually based on what’s missing (gum only versus bone volume), and that requires an in-person exam and often imaging.
How can I tell the difference between normal healing, dry socket, and an infection at home?
You can often tell by timing and symptoms. Normal healing closes the surface by about a few weeks without worsening pain. Dry socket pain typically starts or spikes 1 to 3 days after extraction, while infection tends to increase pain and swelling after about a week. If symptoms do not follow that pattern, ask your dentist to reassess rather than waiting.
Does my medical history change whether gum tissue will cover the extraction site?
Certain people have a higher risk of impaired healing, and that can affect how well the soft tissue covers the socket. Smoking and diabetes, for example, can slow soft-tissue healing. If you fall into higher-risk categories, it’s smart to follow up earlier than the usual 1 to 2 weeks and ask what precautions matter most for you.
What if the extracted tooth was taken out because of gum disease, will it heal differently?
If a tooth was removed due to advanced periodontal disease, the adjacent gum and bone may already be compromised. That means the socket can heal but still end up with less coverage or a different gum line than you expected. In those cases, an evaluation by a periodontist can help decide whether grafting is needed now or only if you later plan for an implant.
My gums look uneven after a surgical extraction, is that normal or should I worry?
Swelling can distort the early look of the gum line. In the first couple of weeks, the tissue may appear uneven or slightly “off” even when the healing is progressing normally, especially after sutures or a more involved surgical approach. Focus on the trend (improving over time) and any worsening pain, rather than a single snapshot.
If I need treatment for a visible dip, will a gum graft fix it or will I also need bone work?
If you’re a few weeks out and the gum surface seems covered but there’s a dip or missing volume at the ridge, it may require treatment planning based on the underlying bone. A soft tissue graft can help when the issue is primarily gum, but it won’t rebuild bone height by itself. Imaging is often used to decide whether staged bone grafting is the better path.
Does socket preservation at extraction time actually help with future implants and gum appearance?
Yes, especially if you’re considering an implant later. Socket preservation at the time of extraction (bone graft placed into the socket) is aimed at reducing the amount of ridge remodeling that later affects gum volume. Even if gum closes, less bone means the implant site may not support the same contour you want.
What signs mean I should call my dentist even if my socket looks mostly healed?
Because the surface closes, many people stop paying attention too early. If you notice food packing, persistent foul taste, worsening sensitivity, or the gum line looks progressively more concave after the first couple of weeks, contact your dentist. Those are clues to a problem with healing or with hygiene that can be easier to manage sooner.
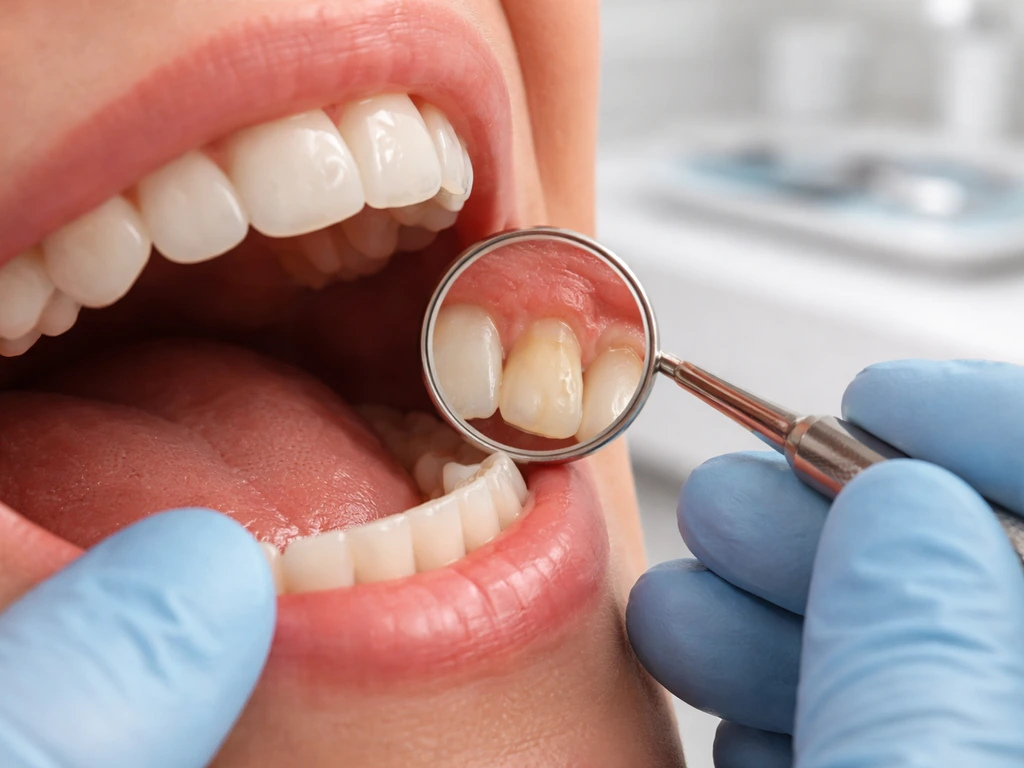
Why receding gums often do not fully grow back, and the real options to stop recession and rebuild tissue.
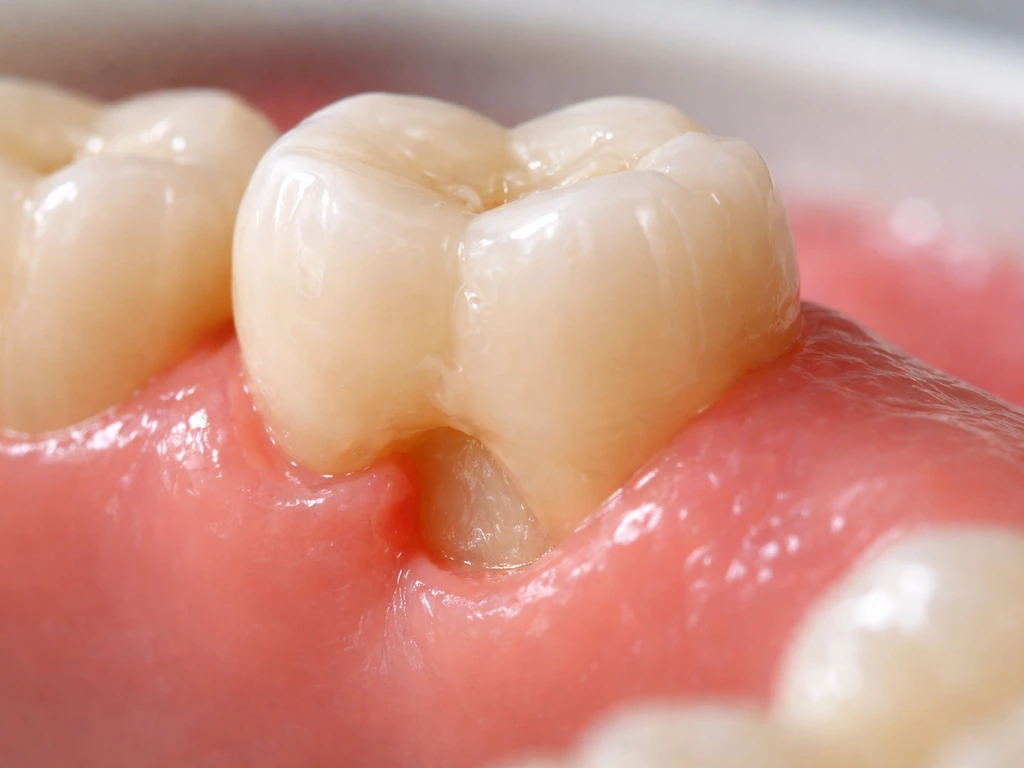
When a chunk of gum is missing, get clear answers on regrowth limits, causes, healing timelines, and next steps.
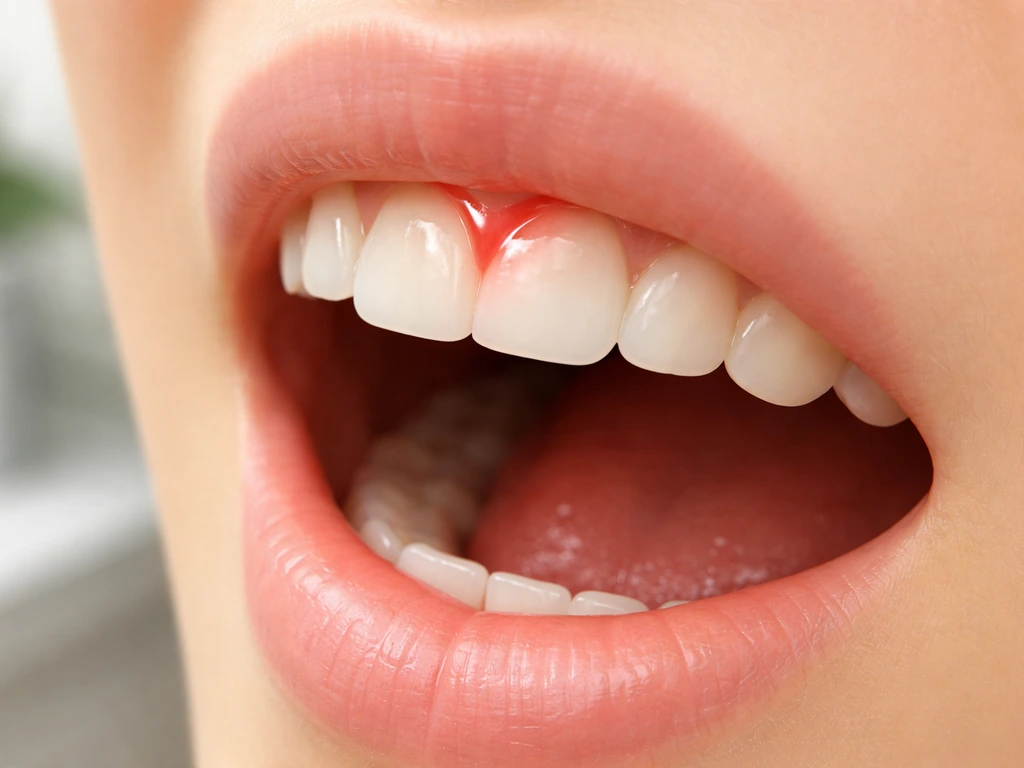
Find out if a torn tooth or gum will regrow, what heals in days, what won’t, and when to see an emergency dentist.

