Yes and no, and the distinction really matters. After wisdom teeth removal, the gum tissue does close over and heal, but it doesn't regrow in the way most people imagine. You won't get back the exact gum architecture you had before, especially if bone was also removed during the extraction. What you do get is a gradual process where soft tissue fills in the socket, the site closes up, and the gum line stabilizes over several weeks to months. Whether that looks and feels "normal" depends a lot on how the extraction went, how you heal, and whether any complications got in the way.
Will My Gums Grow Back After Wisdom Teeth Removal?
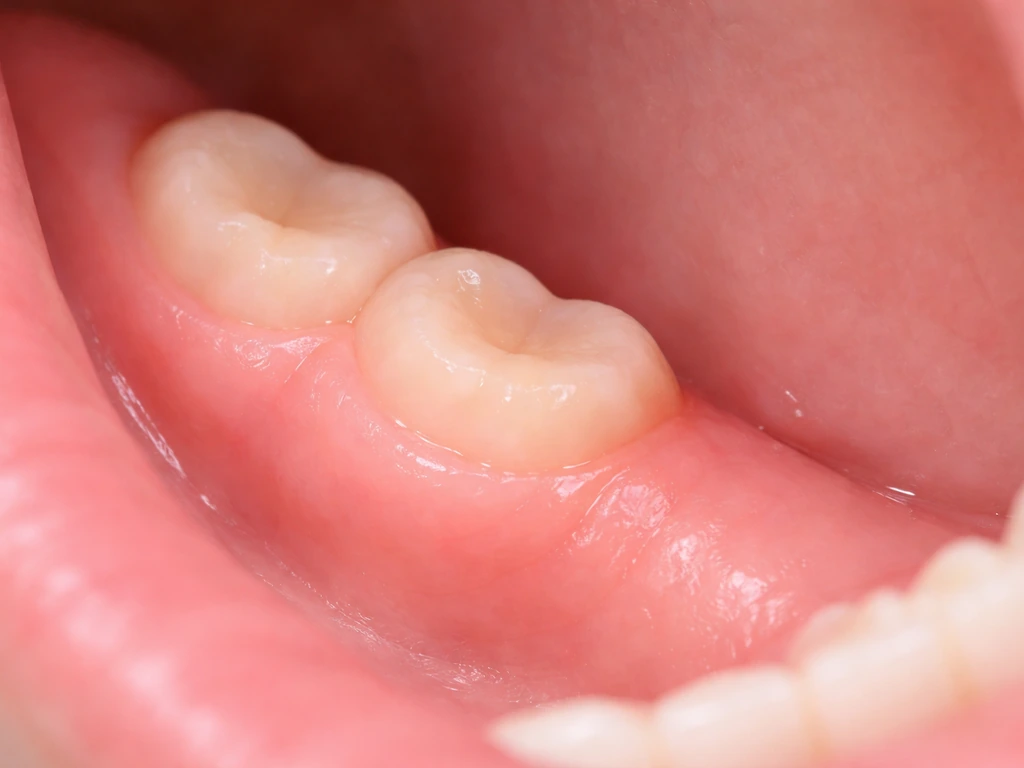
What "gum regrowth" actually means after an extraction
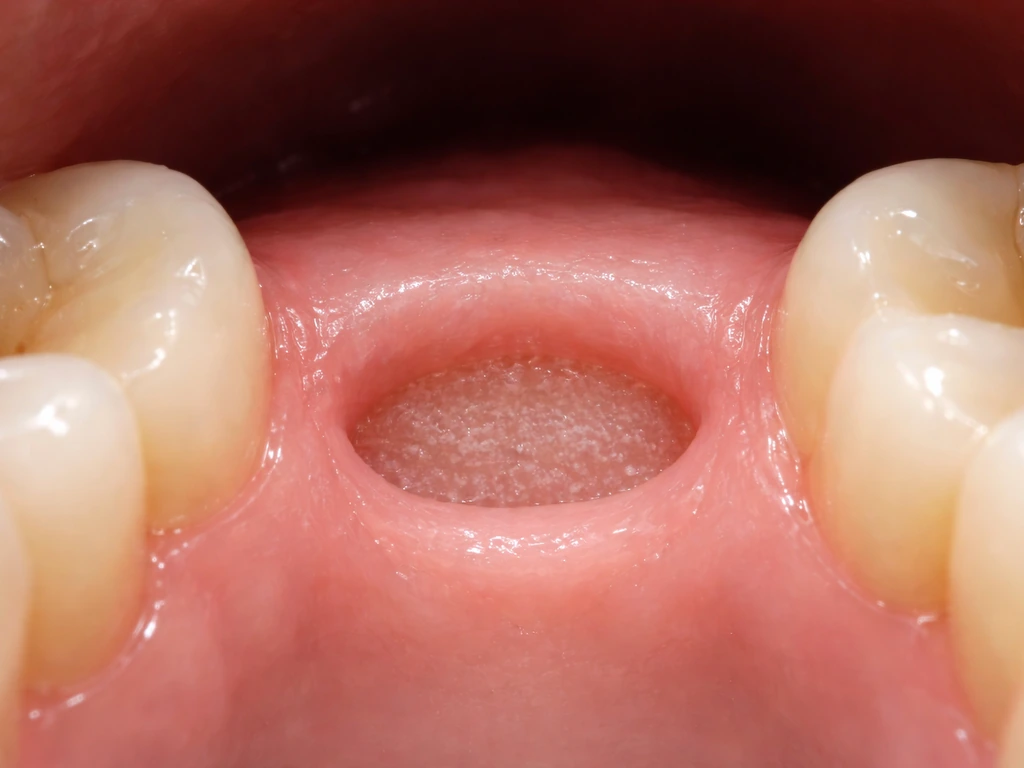
When people worry about their gums growing back, they usually mean one of two things: they either want the socket to close up and stop looking like a hole, or they're concerned about gum recession around neighboring teeth. These are two very different situations, and they have very different answers.
The socket itself fills in through a process called secondary intention healing. A blood clot forms within the first 24 hours, granulation tissue replaces it over the next few days, and then new soft tissue gradually covers the site. This is not the same as your gum regrowing from scratch. It's more like a wound closing. The architecture of the gum, its shape, contour, and the way it hugged the base of the wisdom tooth, doesn't regenerate to its original form.
If the extraction also involved removing some bone (as impacted wisdom teeth often do), the gum tissue that eventually covers that area will be sitting over less structural support. That's why some people notice their gum line looks slightly different or lower near the back of the mouth after healing. This is not necessarily a problem, but it is a normal consequence of removing a tooth that was embedded in bone.
Gum recession around the second molar, the tooth just in front of where the wisdom tooth was, is a separate and more serious concern. This happens when the extraction disturbs the tissue and bone supporting that neighboring tooth. That kind of recession doesn't resolve on its own, and it's worth watching closely during healing.
Normal healing timeline: what to expect week by week
Healing after wisdom tooth extraction happens in overlapping stages, and knowing the rough timeline helps you figure out whether what you're seeing is normal or a red flag.
| Timeframe | What's happening | What it looks like |
|---|---|---|
| Day 1 | Blood clot forms in the socket | Dark red clot, some swelling and bleeding is normal |
| Days 2 to 3 | Clot stabilizes, inflammation peaks | Swelling at its worst, site looks raw, may feel tight |
| Days 4 to 7 | Granulation tissue starts forming | Site starts to look more pale/pink, less raw, pain decreases |
| Week 1 to 2 | New soft tissue begins covering the socket (per AAOMS) | Hole appears smaller, gum edges start closing inward |
| Weeks 3 to 4 | Soft tissue mostly closed over the surface | Site looks mostly healed on the outside, still tender inside |
| Months 1 to 3 | Bone remodeling and full soft tissue maturation | Gum line stabilizes, final contour becomes clear |
| Months 3 to 6 | Full healing for impacted extractions | Bone fills socket, final appearance is set |
Most simple (non-impacted) extractions look visually healed within three to four weeks. Impacted wisdom teeth that required surgical removal with flap incisions can take three to six months before the bone fully fills in and the gum reaches its final shape. The outside may look healed long before the inside is actually done.
Why gums sometimes don't fully recover: risk factors worth knowing
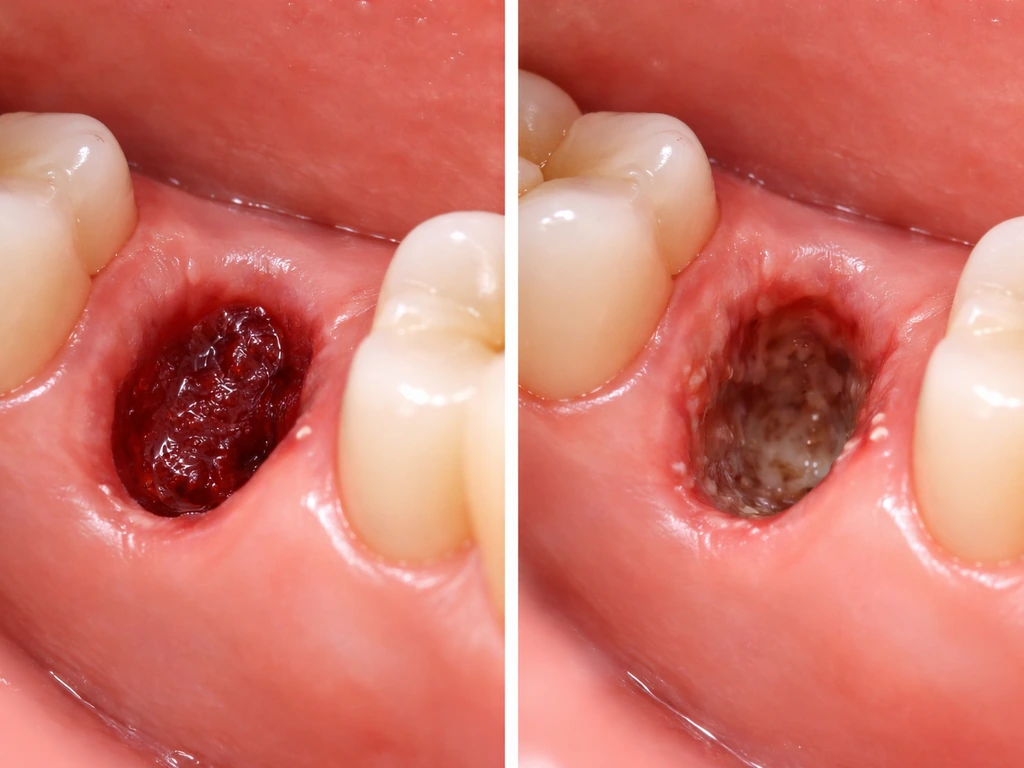
Not every extraction heals cleanly, and several factors can slow things down or prevent the gum from healing as expected.
Dry socket
Dry socket (alveolar osteitis) happens when the blood clot is lost or dissolves before the socket has closed. It's one of the most common complications after wisdom tooth removal, affecting roughly 2 to 5 percent of standard extractions and up to 30 percent of impacted lower wisdom tooth removals. Without that clot, the bone and nerve endings are exposed, healing stalls, and the gum can't close properly. You'll usually notice it three to five days after the extraction as a sudden worsening of pain rather than gradual improvement.
Smoking
Smoking is one of the biggest risk factors for poor healing. Nicotine constricts blood vessels, reducing the oxygen and nutrients that the healing tissue needs. The suction from inhaling can also dislodge the clot. Smokers are significantly more likely to develop dry socket and slower overall gum closure. If you smoke, stopping for at least 72 hours post-op (ideally longer) makes a real difference.
Infection
If bacteria get into the socket before it closes, healing gets derailed. Signs of infection (covered in more detail below) need prompt treatment, because untreated infection doesn't just slow healing, it can cause bone loss that changes the gum's final appearance permanently.
Surgical complexity and technique
The more complex the extraction, the longer and more variable the healing. A fully erupted wisdom tooth that came out cleanly is very different from a deeply impacted tooth that required bone removal, sectioning the tooth into pieces, and suturing the gum flap back. More tissue disturbance means more healing time and a greater chance that the final gum contour will differ from where it started.
Age, bone health, and overall health
Younger patients (late teens to mid-twenties) generally heal faster because bone is denser and tissue regenerates more readily. Older adults, patients with diabetes, those on corticosteroids or blood thinners, and people with existing gum disease all tend to heal more slowly and have a higher risk of complications. Gum disease in particular matters, because if the supporting bone around neighboring teeth is already compromised, an extraction nearby can accelerate recession in a way that won't reverse on its own.
Sutures and whether they were used
Sutures help hold the gum flap in place so the tissue heals in the correct position. If sutures weren't placed, or if they came out too early, the gum edges can heal in a slightly different position than intended. Dissolvable sutures typically last seven to ten days, which is usually long enough to anchor the tissue while initial healing takes hold.
Warning signs that mean you should call your dentist or oral surgeon
A lot of post-extraction discomfort is completely normal. But there are specific signs that mean something is going wrong and you shouldn't wait it out.
- Pain that gets significantly worse three to five days after the extraction instead of gradually improving (classic dry socket sign)
- Visible empty socket with exposed bone, or a foul taste and smell coming from the site
- Swelling that increases after day three rather than subsiding
- Pus or discharge coming from the extraction site
- Fever above 101°F (38.3°C) that develops or persists after the first day
- Numbness or tingling in the tongue, chin, or lip that doesn't improve after the first day or two
- The gum near the neighboring second molar appears to be pulling away from the tooth or the root is becoming visible
- Heavy bleeding that doesn't stop after gentle pressure for 30 to 45 minutes
Don't try to manage these at home. Dry socket needs to be packed by your oral surgeon to relieve pain and allow healing to restart. Infections need antibiotics and possibly drainage. And recession around neighboring teeth needs to be documented and monitored before it gets worse.
At-home care that actually supports healing

How you take care of the site in the first two weeks makes a meaningful difference in how well and how quickly the gum heals. The basics from AAOMS are straightforward but easy to get wrong.
- Keep the clot in place: no straws, no spitting forcefully, and no vigorous rinsing for at least 24 hours. The suction and pressure can pull the clot right out.
- After the first 24 hours, rinse gently with warm salt water (half a teaspoon of salt in eight ounces of warm water) after meals and before bed. Tilt your head rather than swishing hard.
- Brush gently around the area but do not brush directly over the socket until it has closed. Use a soft-bristled brush.
- Eat soft foods for the first several days: yogurt, scrambled eggs, mashed potatoes, smoothies without straws. Avoid anything crunchy, chewy, or sharp that could disturb the clot or get lodged in the socket.
- Don't smoke. Even if you usually smoke, stopping for at least 72 hours post-op is critical. Longer is much better.
- Keep your head elevated, especially when sleeping, for the first few nights to reduce swelling.
- Avoid alcohol and mouthwashes containing alcohol for at least 24 hours, as both can interfere with clot formation and tissue healing.
- Take prescribed medications as directed. If antibiotics were prescribed, finish the full course even if you feel fine.
One thing worth emphasizing: gentle care does not mean no care. If you are wondering whether gums grow back after brushing too hard, the key is that gentle cleaning supports healing and prevents additional gum recession. Keeping the area clean is important for preventing infection, which is itself a major cause of poor healing. The goal is careful, consistent hygiene, not avoiding the area entirely.
Professional options if the gum doesn't recover as expected
If several months have passed and you're still dealing with visible gum recession around neighboring teeth, exposed bone, or an uneven gum line that bothers you functionally or aesthetically, there are legitimate treatment paths available.
Soft tissue grafting
If gum recession occurred around the second molar after the wisdom tooth was removed, a connective tissue graft can restore coverage. A periodontist takes a small amount of tissue, usually from the palate, and grafts it over the receded area. This is the gold standard for treating gum recession that won't resolve on its own, and it works well when there's adequate bone structure underneath.
Socket preservation and bone grafting
Ideally, this happens at the time of extraction: bone graft material is placed in the socket to preserve its volume and shape. If it wasn't done at the time of surgery and you've ended up with significant bone loss that's affecting gum contour, bone grafting after the fact is still possible, though it's more involved.
Dry socket packing and follow-up care
If you're still in the early weeks and dealing with a dry socket, your oral surgeon will place a medicated dressing in the socket to relieve pain and allow healing to restart. This typically needs to be changed every few days until granulation tissue takes over. It's a straightforward procedure but it does require multiple visits.
Monitoring with your periodontist
If you're concerned about gum changes around neighboring teeth but they aren't severe yet, a periodontist can take baseline measurements and track changes over time. Catching recession early, before it becomes significant, gives you more and better treatment options. This is similar to monitoring that happens after other gum-affecting procedures like osseous surgery or crown lengthening. It can be helpful to ask how crown lengthening or related gum contouring might affect your long-term gum appearance. This idea is also important after osseous surgery, where bone and gum position can change during healing.
Myths about gum and tooth regrowth after extractions
There's a lot of wishful thinking floating around online about dental regeneration. Here's where the science and the folklore part ways.
Myth: Gums fully grow back to their original shape after any extraction
The socket closes and soft tissue covers it, but the original gum architecture doesn't regenerate perfectly. The contour of the gum after healing reflects the new bone level underneath, which may be slightly lower than before, especially after a complex impacted extraction. If you are specifically asking, can gums grow back after scaling, remember that gum recession treatment depends on the underlying bone support, similar to how healing after extraction works. Whether that changes your gum line or looks like gum recession, the question do gums grow back after tartar removal is similar but has its own specific answer. Tissue heals, but it doesn't rebuild to a precise original blueprint.
Myth: Oil pulling, vitamin supplements, or special toothpastes can regenerate lost gum tissue
There is no supplement, oil, paste, or rinse that will cause lost gum tissue to grow back. This applies broadly across dental health, not just after extractions. Gum tissue that has permanently receded requires a physical graft to be restored. Good nutrition and vitamin C, for example, support overall healing and immune function, but they don't generate new gum tissue where none exists.
Myth: A new tooth can grow in place of an extracted wisdom tooth
Humans get two sets of teeth, and that's it. Once a permanent tooth is removed, it doesn't grow back. There's no third set waiting in reserve. Research into stem-cell-based tooth regeneration is ongoing, but it is not clinically available. The socket fills with bone and gum tissue over time, but there's no tooth coming.
Myth: If the gum looks healed on the outside, it's fully healed
The surface can close over within three to four weeks while the underlying bone is still in the process of filling in, which can take three to six months for impacted extractions. Looking healed and being fully healed are two different things. This is why biting into hard foods or starting contact sports too soon can still damage the site even when the surface looks fine.
Myth: Recession after wisdom tooth removal only affects the back of the mouth
Wisdom tooth extractions can affect the gum and bone support of the adjacent second molar, which is a tooth you very much need to keep. This is one reason why the timing and technique of wisdom tooth removal matters, and why post-op monitoring isn't just about the extraction site itself. If you've had gum recession after other dental work too, like after scaling, brushing too hard, or Invisalign treatment, you're likely already aware of how interconnected gum health is across the mouth.
What to do right now if you're worried about your gums
If you're in the first two weeks after extraction and things look or feel off, call your oral surgeon's office today. Don't search for workarounds or wait it out if you're experiencing increasing pain, fever, or visible problems. These are exactly the situations they expect calls about.
If you're several months out and unhappy with how the gum looks or worried about recession near a neighboring tooth, book an appointment with a periodontist for an assessment. Take photos now if you can, so you have a baseline to compare as time goes on. The earlier you address gum recession, the more straightforward and successful the treatment options tend to be.
And if you're somewhere in the middle, past the acute healing phase but not quite at the point where you'd call it a problem, just stay consistent with gentle oral hygiene, keep your follow-up appointments, and watch for any of the warning signs listed above. Most people heal without incident. But knowing the difference between normal and not-normal is what gives you the ability to act early if something does go wrong.
FAQ
How long after wisdom tooth removal should I expect the gum to look “closed” versus fully settled?
The surface often looks closed in about three to four weeks for simpler extractions, but the deeper healing and gum line stabilization can keep changing for months, especially after impacted lower teeth. If the gum contour is still shifting or subtly dropping after the first month, that can still fall within a normal impacted-to-final-shape window, but it should be trending steadily rather than worsening.
Is it normal if the gum at the extraction site looks slightly lower or different from the rest of my mouth?
Yes, it can be normal if your gum line appears a bit lower near the back of the mouth after a procedure that involved bone removal. The key is whether it’s stable and painless. If you notice increasing soreness, bad taste or drainage, or a sudden change after initially improving, that points away from normal settling.
Does brushing too soon or too hard cause permanent gum recession after the surgery?
It can, particularly around the neighboring second molar, because aggressive brushing can irritate healing tissue and increase inflammation before the site is strong enough to tolerate pressure. Gentle cleaning plus careful technique (and following your surgeon’s specific instructions for the first days) reduces the risk, but it won’t “undo” recession once bone support is lost.
If I’m not having severe pain, can I still have dry socket?
Dry socket usually presents with pain that gets worse around days three to five rather than gradually improving. If your pain is mild but doesn’t follow the expected pattern, or you have pain that worsens after you thought you were healing normally, contact your oral surgeon. Not all cases feel dramatic, and prompt evaluation matters.
What signs of infection mean I should call immediately after wisdom teeth removal?
Call promptly if you develop fever, spreading facial swelling, pus or a persistent foul taste, or pain that intensifies instead of tapering off. These patterns can suggest infection that may require antibiotics and possibly drainage, and delaying can increase the chance of bone involvement and lasting contour changes.
When should I start flossing near the second molar after the procedure?
Don’t guess, because timing depends on whether you had sutures and how well the tissue has sealed. Many people can resume careful cleaning with floss once your surgeon says the area is safe, typically after early acute healing. If flossing causes bleeding that doesn’t stop quickly, or it worsens pain, pause and ask for guidance rather than forcing it.
Can I smoke or vape during the healing window if I do it carefully?
Smoking and vaping both increase the risk of poor healing because nicotine constricts blood vessels and aerosol use can contribute to clot disruption. Even “careful” use still raises risk. Stopping for at least 72 hours post-op is often the minimum recommendation, longer is better, and follow your surgeon’s instructions if they differ.
What about alcohol, mouthwash, or straws, do they affect gum regrowth?
Alcohol can worsen dehydration and may interfere with medication use, and straws create suction that can dislodge the clot early on. For mouthwash, some antiseptics are helpful later but can irritate healing tissue if used too early. Follow your surgeon’s timeline, especially during the first week when clot protection is most important.
If my gums don’t return to the exact original shape, does that automatically mean permanent gum loss?
Not automatically. The socket can close and the gum line can stabilize, but the architecture may not fully match what you had before, especially after impacted or bone-involved extraction. Permanent issues are more likely if you develop recession around the neighboring teeth, exposed root or bone, or visible contour changes that keep progressing after the initial healing phase.
At what point should I see a periodontist instead of waiting for my oral surgeon follow-ups?
If you are several months out and have persistent gum recession around the second molar, exposed bone, or an uneven gum line that bothers you aesthetically or functionally, a periodontist assessment is appropriate. Bringing baseline photos to your visit helps document whether recession is truly stable or still changing.
If gum recession happens near the adjacent tooth, what treatments are realistic?
A connective tissue graft is commonly used when there is adequate underlying support and the goal is root coverage. If there is significant bone loss, additional procedures such as bone grafting or staged approaches may be needed. A periodontist will decide based on measurements, tissue thickness, and how stable your gum line is over time.
Do vitamins or supplements help the gums grow back after wisdom tooth removal?
They can support overall healing and immune function, but they do not regenerate missing gum tissue or replace lost bone where support is gone. Vitamin C can be beneficial if you’re deficient, but it won’t function like a graft. The most impactful “supplements” after extraction are good follow-up care, clot protection, and controlling risk factors like smoking.
Explains whether gums truly regrow after plaque removal, what can improve, timing, and what to do to heal safely.
See what regrows after Invisalign gum recession, what stays permanent, why it happens, and next-step checks.
Learn what happens to gums after tartar removal, which changes are reversible, and when recession needs more care.

