Yes, it is genuinely possible to never grow wisdom teeth, but probably not in the way you're hoping for. Some people are simply born without them, and others have them form but never erupt. If yours are already developing, you can't stop that biological process, but you can absolutely influence whether they ever break through your gum line. That distinction, between forming, erupting, and being impacted, is what really matters when you're trying to figure out your options.
Is It Possible to Not Grow Wisdom Teeth
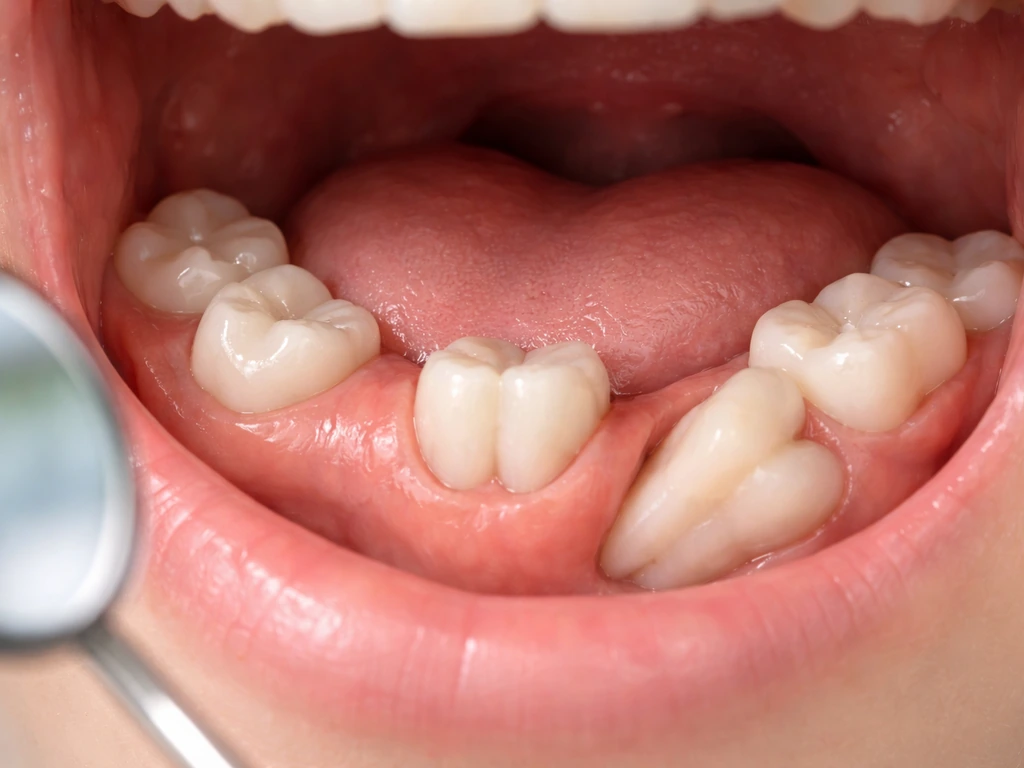
Can you actually prevent wisdom teeth from erupting?
Let's be direct: once a wisdom tooth has started forming in your jaw, you cannot stop it from developing. Tooth development is a biological process controlled by genetics and cellular signals, there's no supplement, diet change, or home remedy that reverses it. What you can prevent, or at least control, is eruption, whether the tooth actually pushes through the gum and into your mouth. That's where dentistry genuinely gives you options.
Some wisdom teeth form completely but never erupt on their own. They stay buried in the jawbone (fully impacted) or get partway out and stop (partially impacted). In fact, a large systematic review and meta-analysis found that roughly 36.9% of people per subject have at least one impacted third molar, so 'not erupting' is actually common, not a fluke. The problem is that staying buried doesn't automatically mean staying harmless. That's where the conversation gets practical.
Why wisdom teeth come in at all (and what changes the odds)
Wisdom teeth, formally called third molars, are the last set of molars to develop. The American Association of Oral and Maxillofacial Surgeons (AAOMS) puts the typical eruption window between ages 17 and 25, though a 2025 clinical consensus paper notes that full maturation may not happen until around age 24 in healthy individuals. They're a leftover from our evolutionary ancestors, who needed extra grinding power for a rougher diet and whose jaws were larger. Modern human jaws are frequently too small to accommodate them comfortably, which is why impaction rates are so high.
Whether your wisdom teeth erupt, and how smoothly, depends on several overlapping factors. Jaw size and shape are the biggest ones: a wider jaw with more available space makes eruption far more likely. The angle at which the tooth is developing also matters enormously. A tooth angled toward the adjacent molar is much more likely to become impacted than one growing straight up. Then there's genetics: if your parents had their wisdom teeth removed due to impaction, your odds of the same outcome are higher.
And then there's the possibility that they simply never form. About 34.1% of people in some studied populations show third molar agenesis, meaning one or more wisdom teeth never develop at all, confirmed on X-ray. This is entirely genetic and not something you can engineer. If you're lucky enough to be in that group, the question answers itself. A panoramic X-ray taken during your teen years will tell you whether wisdom tooth buds are even present.
Timing matters: when can you realistically influence eruption?
This is the part most people miss. There's a window where intervention is most effective, and it doesn't stay open forever. Research on third molar developmental stages (using Nolla staging) shows that by around age 13, third molars are already progressing through defined formation stages, meaning the clock is ticking well before you feel any symptoms. By the mid-teens, a dentist can often see on a panoramic X-ray whether a wisdom tooth is present, what angle it's at, and roughly whether there's enough space for it to erupt cleanly.
Here's a rough breakdown of where timing puts you in terms of options:
| Age Range | What's Happening | Realistic Influence |
|---|---|---|
| 12–15 | Tooth buds forming; roots partially developed | Best time to identify presence and trajectory; early orthodontic planning possible |
| 16–20 | Teeth approaching eruption; roots lengthening | Good window for extraction before roots fully form; impaction risk can be assessed clearly |
| 21–25 | Active eruption or impaction occurring | Intervention still effective but recovery typically harder; monitoring urgently needed |
| 25+ | Roots fully formed; eruption largely complete or locked in | Extraction still possible but more complex; focus shifts to managing complications |
The earlier you get a panoramic X-ray to evaluate your wisdom teeth, the more options you have. This is why many dentists recommend an evaluation in the mid-to-late teen years, not because something is necessarily wrong, but because waiting until you're in pain significantly narrows what can be done comfortably and safely.
Your actual options: watchful waiting, extraction, or orthodontic planning
There's no one-size-fits-all answer here. What's right for you depends on your jaw anatomy, how many wisdom teeth are forming, their angle, your orthodontic situation, and whether you're having symptoms. These are the three main paths dentists consider:
Watchful waiting (monitoring)
If your wisdom teeth appear to be erupting straight, there's enough space, and you're not having any symptoms, monitoring is a completely reasonable approach. This means periodic panoramic X-rays, typically every one to two years, to track whether the situation is changing. The key is that 'watchful waiting' is an active choice with regular check-ins, not just ignoring the issue. Some people watch and wait their entire lives without problems. Others find that what looked fine at 20 becomes problematic at 28. Your dentist can help you understand which direction you're trending.
Extraction (before or after eruption)
Extraction is the most definitive way to prevent eruption. If a wisdom tooth is removed before it fully erupts, ideally in the late teens when roots are less than two-thirds formed, recovery is generally faster, the procedure is simpler, and the risk of complications like nerve involvement is lower. This is why oral surgeons often prefer to act early rather than reactively. That said, extraction isn't automatically necessary for everyone; it should be driven by clear clinical reasons like impaction risk, insufficient space, or early signs of decay or gum problems around the tooth.
Orthodontic planning
If you're already in orthodontic treatment or planning to start, wisdom teeth are very much part of the conversation. Orthodontists often coordinate with oral surgeons because impacted wisdom teeth can put pressure on adjacent teeth and potentially undo alignment work. In some cases, extractions are timed around orthodontic treatment to preserve results. If you're a teenager getting braces, it's worth specifically asking your orthodontist what the plan is for your wisdom teeth, it shouldn't be an afterthought.
Risks and complications that make ignoring them a bad idea
People often assume that if a wisdom tooth isn't hurting, it's not a problem. That's not always true. Partially erupted wisdom teeth create a pocket between the gum and tooth where bacteria collect easily, this leads to pericoronitis, an infection of the gum tissue surrounding the tooth. Pericoronitis can cause significant pain, swelling, and difficulty opening your mouth, and in severe cases it can spread. It also tends to recur until the tooth is removed.
Impacted wisdom teeth pressing against the second molar can cause damage to that tooth's roots, sometimes without any pain at all. Cysts can also form around impacted teeth over time, gradually destroying surrounding bone. And fully buried wisdom teeth can still develop decay if they're partially exposed or if the follicle around them becomes infected. None of these complications announce themselves loudly in the early stages, which is exactly why regular imaging matters.
- Pericoronitis: gum infection around a partially erupted wisdom tooth, often recurring
- Damage to adjacent teeth: impacted teeth can resorb the roots of second molars
- Cyst formation: follicular cysts around impacted teeth can destroy jawbone silently
- Crowding: pressure from erupting wisdom teeth on neighboring teeth (though this is debated as a primary cause of crowding)
- Decay and gum disease: hard-to-clean wisdom teeth are cavity- and gum-disease-prone even when they erupt
The risk profile also changes with age. The same extraction that's relatively straightforward at 19 can involve longer recovery, more bone removal, and higher complication risk at 35, simply because roots are fully formed and denser bone has grown around the tooth. Waiting isn't neutral; it's a choice with increasing costs over time if problems are developing.
How to talk to your dentist and what to ask for
If you're genuinely trying to understand your wisdom tooth situation today, the most useful first step is getting a panoramic X-ray (also called an OPT or orthopantomogram) if you don't already have a recent one. This gives your dentist or oral surgeon a full view of all four potential wisdom tooth sites, their developmental stage, their angle, and their relationship to surrounding structures like nerves and adjacent teeth. A standard small-film X-ray taken at a regular checkup won't give you this full picture.
When you're in the appointment, here are the specific questions worth asking:
- Do I have all four wisdom teeth forming, or are any absent (agenesis)?
- What angle are they at, and is there enough space for them to erupt fully?
- Are any of them impacted, or likely to become impacted based on their current trajectory?
- How close are the roots to the inferior alveolar nerve (for lower teeth)?
- What is your recommendation — monitor, extract now, or refer to an oral surgeon?
- If we wait, what signs should I watch for, and how often do I need follow-up imaging?
If your dentist recommends extraction and you're uncertain, getting a second opinion from an oral and maxillofacial surgeon is completely reasonable. They specialize in this area and can give you a more detailed assessment of complexity and timing. The goal is to make an informed, proactive decision, not to react when you're already in pain.
The regrowth myth: can wisdom teeth grow back after removal?
This comes up more than you'd expect: people worry that removing a wisdom tooth isn't permanent, or conversely, that something can be done to prevent a tooth from 'growing back' after it's been dealt with. To be clear, adult human teeth do not regenerate. Once a permanent wisdom tooth is removed, it does not grow back. There is no second set of wisdom teeth waiting in reserve. Humans have exactly two sets of teeth in their lifetime: primary (baby) teeth and permanent teeth. That's it.
The rare cases where someone feels like a tooth 'grew back' after wisdom tooth removal usually have a straightforward explanation: either a small root fragment was left behind and caused ongoing symptoms, a different tooth shifted position after removal, or (in very rare cases) a supernumerary tooth, an extra tooth that was developing nearby, eventually erupted. These are dental anomalies, not regeneration.
The broader question of whether dental structures can regenerate is a genuinely fascinating area of research, and scientists are actively working on it. But as of today, nothing on the market or in clinical practice can regenerate a removed human adult tooth. What the research community is exploring in terms of tooth germ stimulation and enamel repair is still far from clinical application. So if you've had a wisdom tooth removed, it's gone, and that's actually the point.
The confusion around 'not growing' wisdom teeth often mixes up three different situations: teeth that never form (agenesis), teeth that form but never erupt (impaction), and teeth that have already erupted or been removed. Each of these is biologically distinct. Related questions, like why wisdom teeth develop so late, whether they can grow in on the top arch only, how many typically form, or whether eruption happens in bursts, are all part of the same broader picture of understanding what your third molars are actually doing and what you can realistically do about it. Related to how many wisdom teeth grow, the common scenario is that most people develop four third molars, though some may be missing how many wisdom teeth typically form. Whether eruption happens in bursts is part of how wisdom teeth progress, so it’s useful to understand the timing and stage of development.
The bottom line: you probably can't stop wisdom teeth from forming if they're going to. But you absolutely have options around eruption, timing, and intervention, and the earlier you get a clear picture of what's happening in your jaw, the more those options are available to you.
FAQ
If I already feel or see symptoms, can I still avoid wisdom tooth eruption?
If your tooth buds are already present on a panoramic X-ray, you generally cannot “turn off” development, but you may still prevent eruption by choosing watchful waiting with scheduled imaging or planning early removal if impaction risk is high. If you are getting symptoms (pain, swelling, recurring bad taste), you should be evaluated sooner rather than waiting for your next routine visit.
Do any supplements, mouth rinses, or diet changes prevent wisdom teeth from erupting?
Home remedies, pain gels, special diets, and supplements cannot reverse tooth development. They may temporarily reduce discomfort, but they do not address the underlying cause, often a pocket of bacteria from partial eruption or an unfavorable tooth angle. If symptoms keep returning, the decision usually becomes clinical (monitor versus extract), not home-based.
If my wisdom tooth is fully impacted, is it automatically safe to ignore?
“Not erupting” does not always mean “no risk.” Partially erupted wisdom teeth can trigger pericoronitis because bacteria get trapped under the gum flap. Fully impacted teeth can still cause problems like decay or cyst formation, especially if any portion becomes exposed or the area becomes infected, so periodic imaging still matters even when there is no pain.
How should wisdom teeth planning change if I am already in (or starting) orthodontic treatment?
Yes. If you have braces or plan to start orthodontics, ask for a documented plan that includes whether your third molars will be monitored, removed before or after braces, and how that timing aligns with your tooth movement. Pressures from impacted third molars can interfere with alignment goals, so coordinating with both your orthodontist and an oral surgeon can protect results.
When is it actually worth getting a second opinion before deciding on extraction?
A second opinion is most helpful when the imaging suggests higher complexity, such as proximity to a nerve canal, limited space, deep impaction, or borderline angles. Surgeons can also explain which option best fits your risk tolerance and age, since extraction is often simpler in the late teens than later in adulthood when roots are fully formed.
If I choose watchful waiting, how often should I get X-rays and what would change the plan?
If a wisdom tooth has not erupted and you are choosing monitoring, the key is a specific follow-up schedule based on your imaging findings. Many people need periodic panoramic X-rays (often about every 1 to 2 years), but the interval can be shorter if there is partial eruption, signs of gum inflammation, or changes in angulation over time. “No symptoms” does not replace imaging follow-ups.
What symptoms mean I should stop monitoring and be seen urgently?
During monitoring, you should call promptly if pain and swelling recur, if you notice worsening gum redness around the area, if you get difficulty opening your mouth, or if you see a persistent bad taste or drainage (common with gum pockets). These signs can indicate pericoronitis or infection, which often shifts the recommendation toward intervention.
Is a panoramic X-ray really necessary, or can my dentist just use a smaller dental X-ray?
You typically cannot rely on a standard small in-office X-ray to evaluate third molars well because it often does not show the full position, angle, and nerve relationship. A panoramic X-ray (OPT) is usually the practical first step, especially in the mid-to-late teen window, because it captures all potential wisdom tooth sites at once.
Why would it seem like a wisdom tooth “came back” after extraction?
If wisdom teeth were removed, they do not regenerate as new adult teeth. What sometimes feels like “it came back” is usually a residual root fragment, ongoing symptoms from healing tissue, or a different tooth erupting or shifting that draws attention to the area. True regrowth of an extracted adult tooth is not how human tooth biology works.
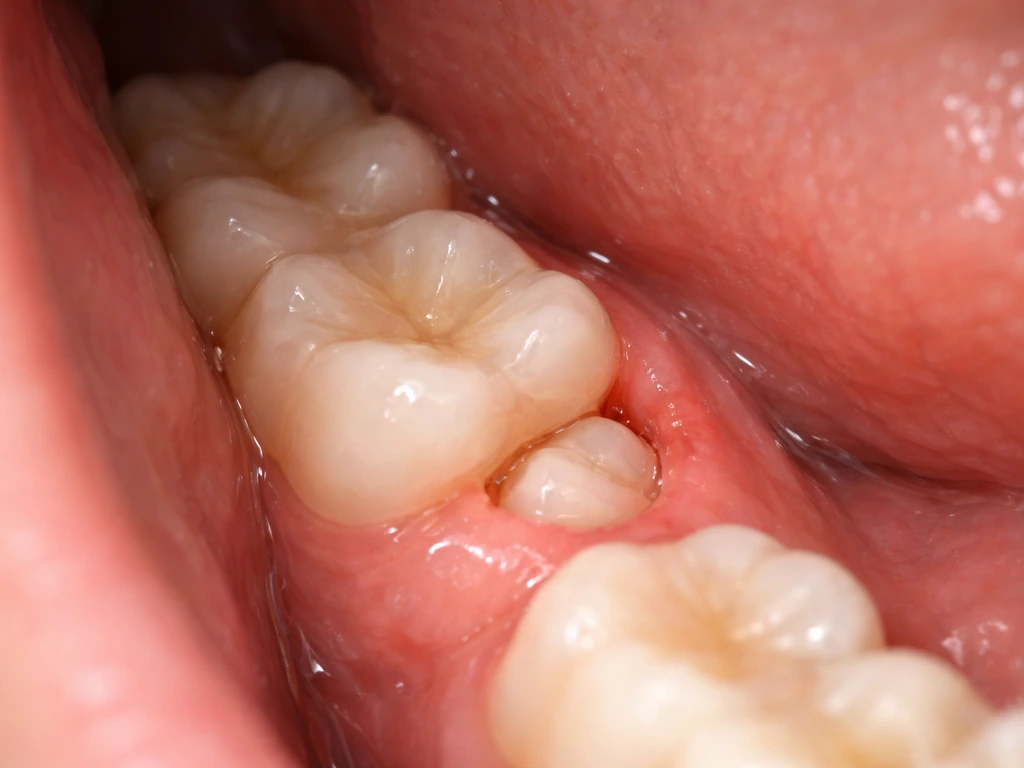
Learn why wisdom teeth erupt late, what “late” really means, and when to seek care for impaction or delayed eruption.
Can wisdom teeth grow on top or the palate? Learn locations, signs, causes, and when to get X-rays and dental care.

Why humans have only baby and permanent teeth: eruption timeline, limits of enamel regrowth, and common exceptions to kn

