Enamel does not grow back, full stop. Once the enamel on an adult tooth is gone, your body has no way to replace it. For a deeper explanation of why teeth do not regrow enamel once it is gone, keep reading. But that is not the whole story, because what most people are actually asking about is whether early, surface-level enamel damage can be reversed or repaired, and the answer there is a qualified yes. Early demineralization, the kind that shows up as chalky white spots or mild sensitivity, can be largely reversed through a process called remineralization. That takes anywhere from a few weeks to several months depending on how deep the damage is, what products you use, and how consistent you are. Beyond that early-damage window, the answer shifts back to no, at least for now, and what you need is a dentist and a restoration rather than a home remedy.
How Long Does It Take for Enamel to Grow Back?
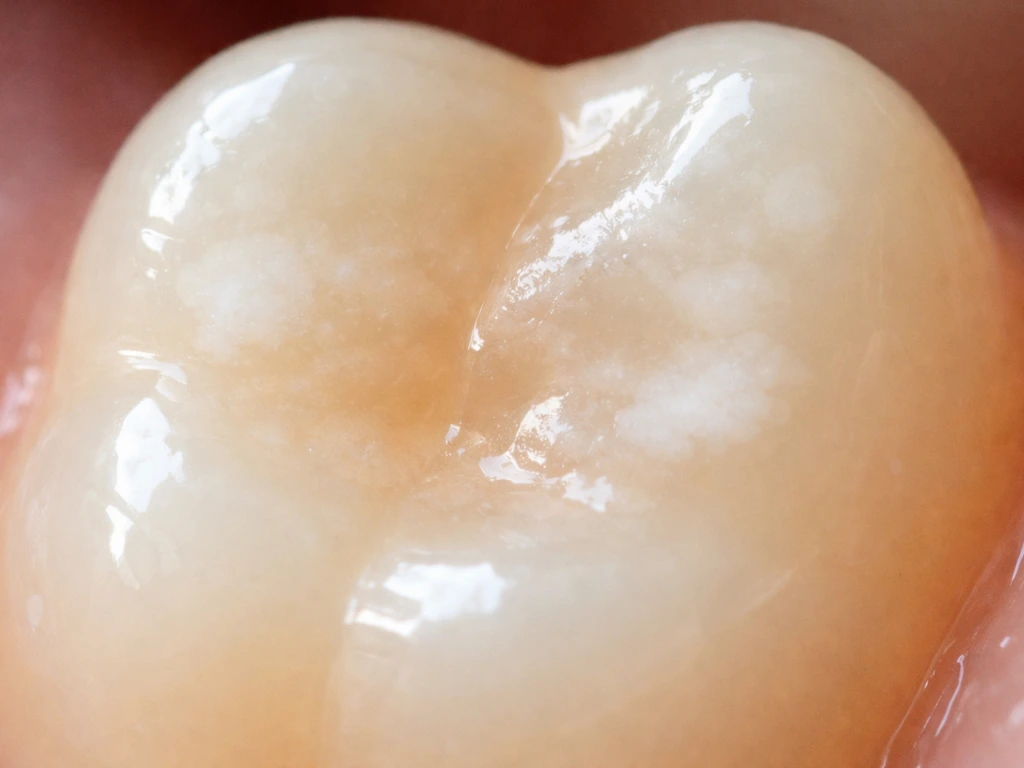
What enamel actually is (and why it can't just grow back)
Enamel is the hard, translucent outer shell of your tooth. It is made mostly of a crystalline mineral called hydroxyapatite, and it is the hardest substance your body produces. Here is the catch: enamel is also completely acellular, meaning once it is fully formed, there are no living cells inside it. The cells that built it, called ameloblasts, do their job while the tooth is still developing, and then they die off through a process called apoptosis right around the time the tooth erupts. No ameloblasts left means no biological machinery to make new enamel. Ever.
This is what makes enamel fundamentally different from something like bone or even dentin (the layer just beneath enamel). Bone has cells that constantly remodel it. Dentin has odontoblasts that can lay down small amounts of new protective dentin in response to damage. Enamel has none of that. Once it is gone in an adult, it is gone. The reason this matters so much is that a lot of popular advice online implies you can "rebuild" or "restore" enamel with the right toothpaste or diet change, and while you can absolutely support its mineral content in the very early stages of damage, you cannot generate a new enamel layer from scratch.
How enamel loss happens and what "regrowth" really means in practice
Enamel loss happens in several ways, and the cause matters a lot for what you can realistically do about it. Acid erosion from soft drinks, citrus, acid reflux, or frequent vomiting slowly dissolves the mineral surface. Cavities (dental caries) begin as acid from bacteria eating sugar, which demineralizes enamel from the outside in. Abrasion from aggressive brushing, hard bristles, or teeth grinding wears enamel down mechanically. Teeth grinding can also wear enamel down, so it is important to address the underlying cause and protect your teeth. After whitening treatments, temporary surface sensitivity happens because the process opens up enamel pores, though this usually stabilizes within days to weeks with proper care.
When people talk about enamel "growing back," they are almost always describing one specific scenario: a non-cavitated white spot lesion. This is enamel that has been partially demineralized (lost mineral) but has not yet broken through into a full cavity. The surface layer is still intact, just less dense underneath. In this state, remineralization is genuinely possible. Minerals from saliva and fluoride can reprecipitate into the subsurface of the lesion, making it denser and functionally stronger again. The white spot may fade, harden, and stop progressing. That is the real-world version of enamel "coming back." It is mineral repair, not tissue regrowth, but it is meaningful and it works.
Realistic timelines: how long remineralization actually takes
The timeline depends almost entirely on how early you catch the damage and how aggressively you treat it. Here is how to think about the different windows:
Early, superficial changes (days to weeks)
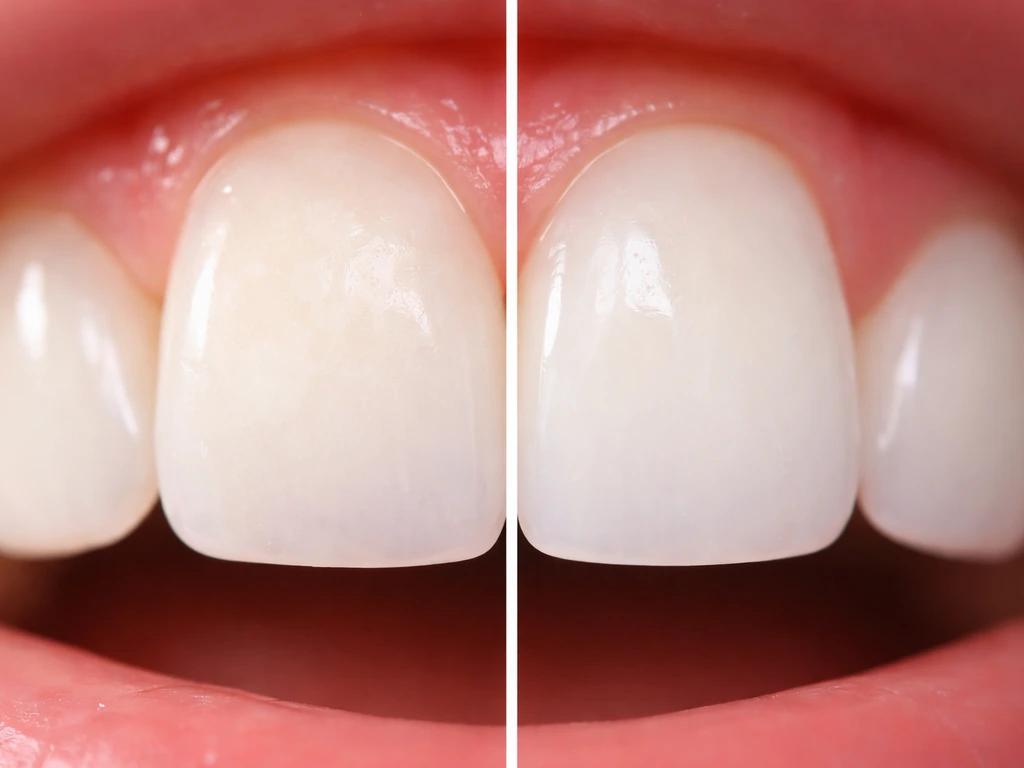
For very early demineralization, like mild sensitivity after whitening or the very earliest stage of a white spot, visible optical changes can appear within two to four weeks under ideal conditions. One experimental study saw lesion glossiness returning after just two weeks of treatment. In practice, ex vivo research using remineralizing rinses four times daily showed measurable mineral gain within about 35 days. So if you catch something very early and start fluoride use and acid reduction immediately, you can see real improvement in about a month.
Non-cavitated white spot lesions (weeks to months)
Clinically, the standard monitoring window for remineralizing a white spot lesion is six to twelve weeks at minimum, with many dentists tracking progress over three to six months. Clinical trials evaluating products like CPP-ACP (a casein-based remineralizing paste) and fluoride varnish routinely use six-month endpoints to measure outcomes. A randomized controlled trial applying fluoride varnish monthly for six months after orthodontic treatment showed meaningful lesion area reduction over that time frame. Resin infiltration (a microinvasive treatment available at the dentist) achieved roughly 47 percent lesion-area reduction compared to about 27 to 30 percent for fluoride varnish and CPP-ACP groups over the same period. So six months of consistent effort is a realistic planning window for visible improvement in white spots.
Cavitated or structural enamel loss (no timeline applies)
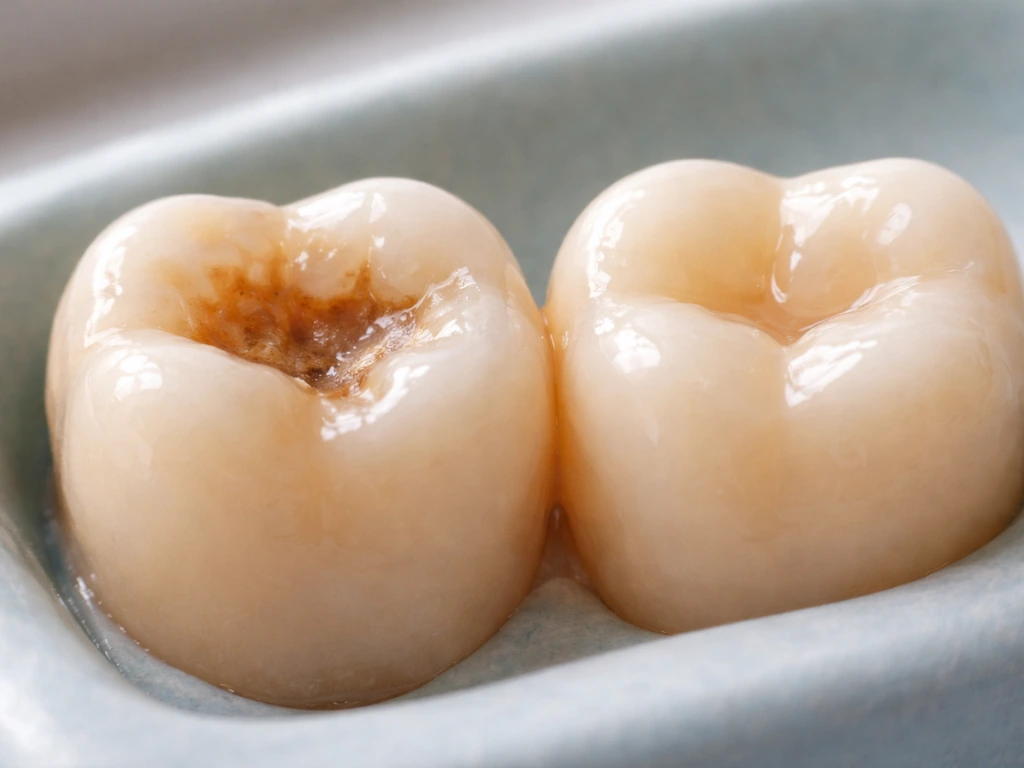
Once enamel has broken through into a cavity, or once erosion and abrasion have physically removed enamel thickness, no amount of fluoride or remineralizing toothpaste will replace what is lost. Similarly, dental enamel cannot regrow once it is fully gone, but early white-spot damage may still improve with remineralization can enamel grow back. In the same way, tooth roots do not regrow once they are lost to periodontal disease or other damage <a data-article-id="2C1BDF66-C52D-4FAD-ADBA-D5DCC4CA69E9">can teeth roots grow back</a>. There is no biological timeline for this because it simply does not happen. At that stage, treatment means a restoration, a filling, a crown, a veneer, or another dental procedure depending on the extent of damage.
Children vs. adults: a genuinely different situation
Children's teeth are a unique case. Primary (baby) teeth and developing permanent teeth are actively being mineralized during childhood, which means enamel quality can be influenced during that window in ways it simply cannot be in adults. Disruptions during development, like illness, high fevers, or nutritional deficiencies, can leave permanent marks in the form of hypomineralized or chalky enamel that is weaker than normal. Once those teeth erupt, the structural record is set. That said, children's newly erupted permanent teeth do benefit significantly from fluoride exposure early on because the enamel is still maturing at the surface level for a period after eruption and is more receptive to incorporating fluoride into its crystal structure. This is also why fluoride varnish is recommended for all children every six months (or every three months for high-risk kids), starting when the first tooth comes in. For context on tooth development timelines in kids, wisdom teeth are the last permanent teeth to form and typically erupt between ages 17 and 25, so tooth development and enamel formation continues into early adulthood in that specific case.
What can actually regenerate vs. what is permanently gone
It helps to have a clear-eyed picture of what dental tissues can and cannot do on their own:
| Tissue | Can it regenerate? | Notes |
|---|---|---|
| Enamel (adults) | No | Acellular, no ameloblasts present after eruption; lost enamel cannot be replaced biologically |
| Enamel (early demineralization) | Partially | Mineral can be reprecipitated into subsurface lesions via remineralization; not true tissue regrowth |
| Dentin | Limited yes | Odontoblasts can form reparative dentin in response to injury; not the same as full dentin replacement |
| Bone around teeth | Partially | With appropriate treatment, some bone regeneration is possible; depends on cause and extent |
| Tooth roots / pulp / nerves | No (in most cases) | Pulp removed in root canal does not regrow; nerve regrowth in dental contexts is limited and context-specific |
| Baby teeth | No (replaced by adult teeth) | Primary teeth are lost and replaced naturally; the permanent tooth underneath is the "replacement" |
Dentin is worth calling out specifically because it is often confused with enamel. Dentin sits beneath enamel and is produced by odontoblasts, which remain alive in the tooth. When enamel thins and dentin is exposed or threatened, odontoblasts can respond by secreting new reparative dentin to protect the pulp. That is a real biological process, unlike enamel regeneration. Unlike enamel, dentin can sometimes form new reparative dentin in response to damage, but it does not mean it fully grows back like an entire tissue replacement dentin grow back. Similarly, dental pulp and nerve tissue have their own regeneration limitations that are separate from the enamel question entirely. Similarly, dental pulp and nerve tissue have their own regeneration limitations that are separate from the enamel question entirely can teeth nerves grow back.
How to speed up repair safely: what actually works
If you are in that early-damage window where remineralization is possible, here is what the evidence supports:
Fluoride: the most important tool you have
Fluoride is the single most evidence-backed tool for supporting enamel remineralization. It works by shifting the balance from mineral loss to mineral gain, and it directly inhibits the acid-producing bacteria that cause demineralization. Use a fluoride toothpaste (1,000 to 1,500 ppm fluoride for adults) twice daily without rinsing immediately after, so the fluoride stays on your teeth longer. If you have active white spots or high cavity risk, a fluoride rinse used separately from brushing adds another exposure. For kids, toothpaste fluoride levels should be age-appropriate and match current pediatric guidelines.
CPP-ACP products (MI Paste and similar)

CPP-ACP, found in products like GC MI Paste, releases bioavailable calcium and phosphate directly onto the enamel surface, giving the remineralization process more raw material to work with. Research suggests it supports mineral gain in early lesions, particularly when combined with fluoride. It is especially useful after orthodontic treatment, when white spots around brackets are common, or during periods of high acid exposure.
Diet and acid management
Remineralization only wins when the acid attacks stop or slow down. Reduce the frequency of acidic food and drink (sodas, sports drinks, citrus juice, vinegar-based foods) rather than eliminating them entirely, since frequency matters more than total amount. Drink water after acidic foods, chew xylitol gum (which reduces the bacteria that produce acid), and do not brush immediately after an acid exposure, since enamel is temporarily softened and more vulnerable to abrasion for about 30 minutes afterward. If you have acid reflux, managing that medically is also a direct intervention for your enamel.
Saliva: your built-in remineralizer
Saliva buffers acids and delivers the calcium and phosphate your enamel needs to remineralize naturally. Anything that reduces saliva flow, like certain medications, mouth breathing, or dehydration, slows remineralization and increases damage risk. Staying well hydrated, chewing sugar-free gum to stimulate saliva production, and addressing dry mouth causes can meaningfully affect your outcomes.
Professional treatments worth asking about
- Fluoride varnish: Applied in-office, typically every three to six months depending on your risk level; provides a concentrated topical fluoride dose that supports remineralization of early lesions
- Resin infiltration (Icon): A microinvasive in-office procedure that fills the porous subsurface of a white spot lesion with resin, stabilizing it and improving its appearance; best for lesions that are cosmetically bothersome or at risk of progressing
- Silver diamine fluoride (SDF): Used to arrest active carious lesions, particularly in children or in situations where traditional restorations are not yet practical
- Custom fluoride trays: For high-risk patients, dentists sometimes prescribe prescription-strength fluoride gel used in custom trays at home for more intensive remineralization support
When to see a dentist: signs you are past the DIY window
Some enamel situations genuinely require professional input, and waiting too long only means more damage and more expensive treatment. See a dentist if you notice any of the following:
- Persistent tooth sensitivity that does not improve within two to four weeks of starting a fluoride routine
- Visible white, chalky, or opaque spots on teeth that you did not notice before, especially around where brackets were if you recently finished orthodontic treatment
- Visible pitting, chipping, notching at the gumline, or a translucent or rounded appearance to tooth edges (signs of acid erosion that has gone beyond surface level)
- Discoloration, darkening, or rough texture on a tooth surface, which can signal an arrested or active cavity rather than a remineralizable white spot
- Pain when biting, temperature sensitivity that lingers, or spontaneous toothache, all of which indicate the damage may have reached dentin or pulp
- Known risk factors that you have not addressed yet, including frequent reflux, an eating disorder history, very frequent consumption of acidic foods or drinks, or chronic dry mouth from medications
A good rule of thumb: if you can see or feel something wrong, book an appointment rather than waiting to see if remineralization handles it. Non-cavitated lesions can often be managed non-invasively with fluoride and monitoring alone. But cavitated lesions, active erosion, and structurally compromised enamel need restorative treatment, and the earlier that treatment happens, the more tooth structure can be preserved.
Your action plan starting today
Here is the practical bottom line. If you have early, non-cavitated enamel damage (sensitivity, white spots, post-whitening softness), you have a real window to improve things with consistent effort over four to twelve weeks. Start fluoride toothpaste twice daily without rinsing immediately after, reduce acid frequency in your diet, stay hydrated, and consider CPP-ACP paste if white spots are present. Book a dental checkup to confirm the lesions are non-cavitated and get professional fluoride varnish applied. Track progress over six months. If you have visible structural damage, pitting, chips, or pain, skip the home remedies and go straight to the dentist because no amount of fluoride toothpaste repairs lost tooth structure. And if you are a parent wondering about your child's enamel, get them on fluoride toothpaste as soon as the first tooth erupts and establish dental care early, because the window for influencing developing enamel is real and it closes.
FAQ
What if I’ve been using fluoride for a month, but my white spot or sensitivity isn’t improving?
If you do not see improvement, it usually means one of two things: the lesion is more advanced than you thought (it may be cavitated), or the demineralization trigger is still happening frequently (for example, frequent sips of soda, reflux, or dry mouth). In practice, reassess with a dentist if nothing changes after about 6 to 12 weeks of consistent fluoride and acid control.
How do I know if my enamel damage is reversible (non-cavitated) or already a cavity?
A dentist can confirm whether a white spot is still non-cavitated using visual exam and sometimes staining, transillumination, or radiographs depending on the case. This matters because once there is a break-through cavitation, remineralization can’t rebuild the missing enamel surface and you may need infiltration or a restoration.
Does it matter how much acidic food or drinks I have, or is frequency what matters for enamel repair?
For remineralization to work, the critical factor is how often the pH drops below the protective threshold, not just how much acid you consume. Even small, frequent exposures (like sipping citrus drinks or having sour snacks often) can keep preventing mineral gain.
How can I tell whether my sensitivity after whitening is temporary, versus true enamel remineralization progress?
You may see “quicker” changes after whitening or during early treatment, but that is not the same as durable enamel repair. Whitening can cause temporary sensitivity from surface changes, which often settles within days to weeks, while true white-spot mineral gain typically needs several weeks to months of fluoride plus trigger control.
Is there a best time to use fluoride toothpaste to help enamel remineralize faster?
Yes. You can strengthen remineralization by timing fluoride correctly: brush with fluoride toothpaste twice daily and avoid rinsing immediately afterward, and do not eat or drink for about 30 minutes after brushing so fluoride stays on the enamel surface longer.
Should I brush immediately after eating something acidic, or will that slow down enamel repair?
If you brush right after an acidic exposure, the softened enamel is more vulnerable to abrasion. A practical rule is to wait about 30 minutes after acids before brushing, use water to rinse in the meantime, and then brush when the enamel has re-hardened.
How does dry mouth or medications affect how long enamel repair takes?
Dry mouth and saliva changes can noticeably slow remineralization and increase ongoing risk. If you have mouth breathing, dehydration, medication-related dry mouth, or reflux, address that issue medically or with your dentist, because without adequate saliva buffering the lesion may not stabilize.
If my white spot still looks visible, does that mean remineralization failed?
Not necessarily. Enamel mineral repair can take place without making the white spot completely disappear, and some lesions leave a lasting optical difference even after they stabilize. Your dentist may judge success by whether the lesion is no longer progressing and by changes in hardness or surface appearance during follow-up.
Can I speed things up by using fluoride rinse and fluoride toothpaste together, or will that be redundant?
Using two fluoride products at the same time can increase irritation in some people and does not always add meaningful benefit if you are already following a strong routine. Instead of stacking multiple products blindly, ask your dentist whether a separate fluoride rinse or varnish schedule is appropriate based on your cavity risk.
I have enamel white spots from orthodontic treatment, how long should I wait before seeking professional options?
If you have braces or recent orthodontic work, white spots are common and tracking matters. Dentist-directed options like fluoride varnish and professional infiltration can change the timeline, and home care alone may be slower, so it is reasonable to schedule follow-up within the first few months of noticing lesions.
Is there any situation where enamel can regrow after erosion or abrasion wears it down?
If the enamel has physically been removed (erosion/abrasion with pitting or chips) or you suspect a cavity, the “growth back” timeline is effectively none, because fluoride cannot regenerate lost thickness. At that point, the right timeline is scheduling evaluation promptly for restoration, sealants, or microinvasive options depending on depth.
Do kids heal enamel faster, and should fluoride be adjusted if my child has high cavity risk?
For children’s newly erupted permanent teeth, the window for incorporating fluoride while the surface matures is real, but you still need consistent brushing and fluoride exposure over time. If a child has high risk, many clinicians adjust the schedule (for example, more frequent varnish) rather than expecting a one-time change to reverse enamel damage.
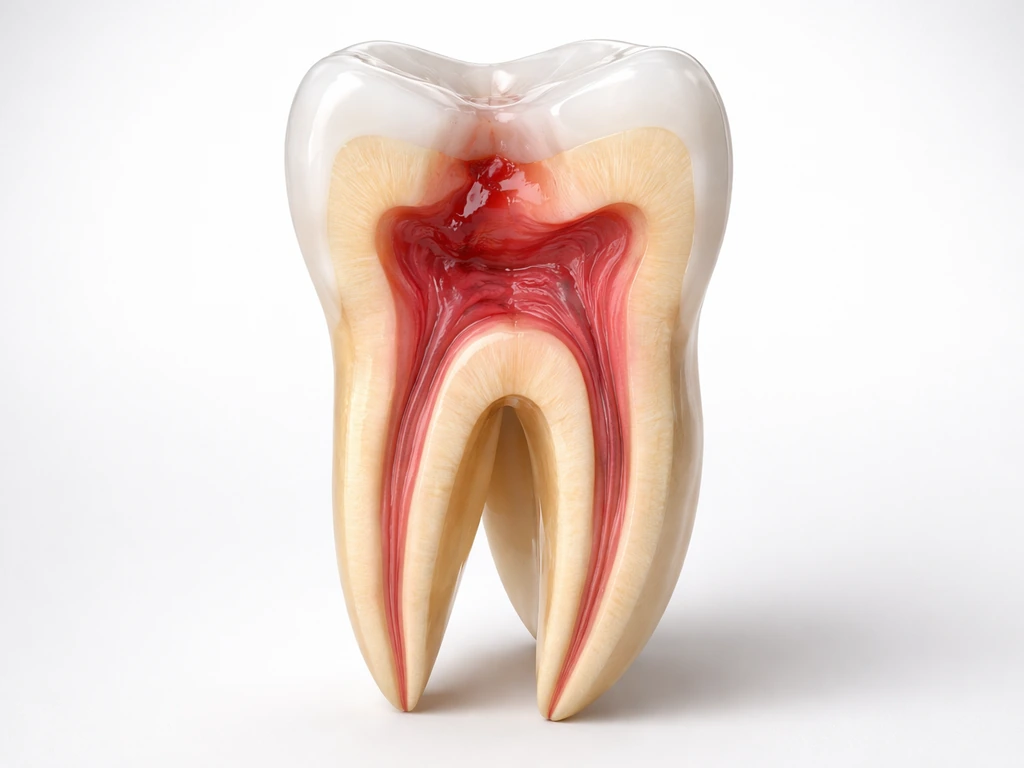
Can tooth nerves regrow? Learn if pulp can recover by age and damage stage, and what treatments you need.
Yes or no on dentin regrowth, realistic timelines, and what to do for exposed dentin, cavities, trauma, and repair optio
Can tooth roots grow back after a root canal? Mostly no, with healing explained and next-step options for failing roots.

