No, a tooth does not grow back after a filling. The enamel and dentin your dentist drilled away to remove the decay are gone permanently. The filling material (composite resin, amalgam, glass ionomer, or similar) replaces that lost structure mechanically, like a patch, but it does not trigger any biological regrowth. Once a tooth is past its baby-tooth stage, human teeth simply do not regenerate lost hard tissue the way skin heals a cut. That is the plain truth, and no supplement, product, or technique currently changes it for a filled adult tooth.
Does Your Tooth Grow Back After a Filling? What’s True
What a dental filling does (and what it doesn't repair)
A filling has one job: restore the shape and function of a tooth after decay has been removed. Your dentist drills out the damaged, bacteria-riddled tissue, then packs the cavity with a restorative material. The ADA recognizes four main categories of direct filling materials: amalgam (the silver-colored classic), resin-based composites (tooth-colored), glass ionomer, and resin-modified glass ionomer. Each works differently in terms of durability, bonding, and aesthetics, but all of them are inert patches. They are not biologically active. They do not bond to your tooth the way your own dentin would, and they have no ability to signal your body to produce new enamel or new dentin in their place.
What a filling does do well is seal the cavity, stop the decay process in that specific spot (by removing the decayed tissue and cutting off bacteria's food supply), and restore your ability to chew normally. That is genuinely useful, but it is purely mechanical. Think of it like patching a hole in drywall: the wall is intact again, but new wall material did not actually grow there.
Can tooth structure regenerate after a filling? (enamel, dentin, pulp)
This is the core biology question, and the answer differs slightly depending on which layer of the tooth you are asking about.
Enamel: no regeneration
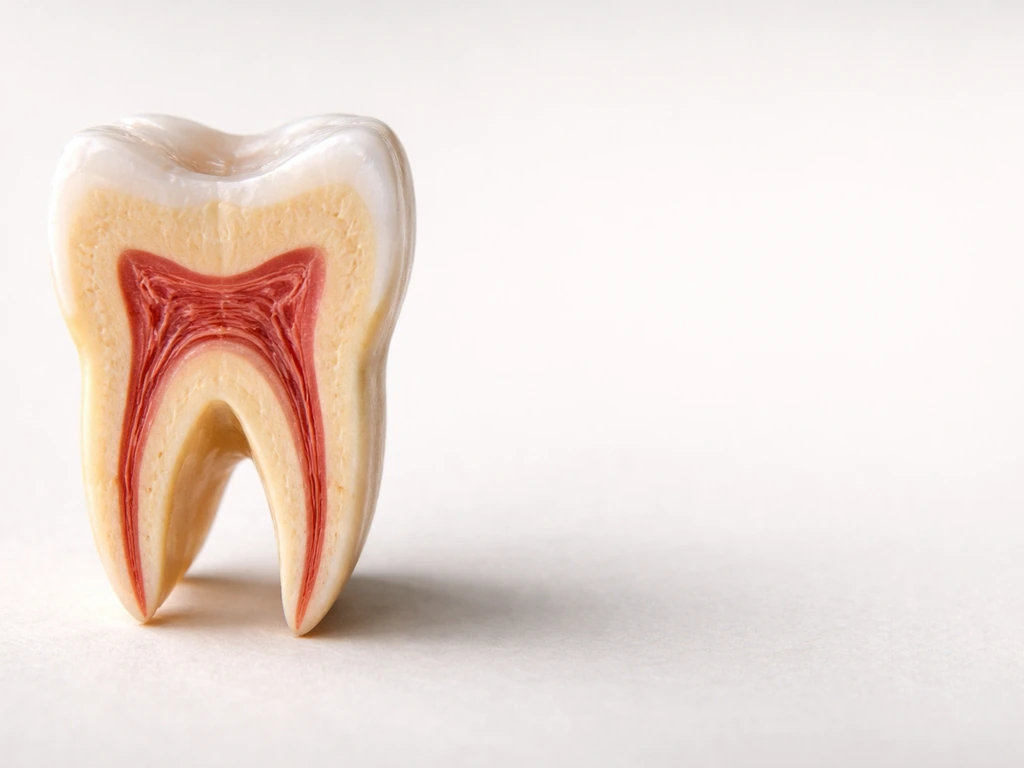
Enamel is the hardest substance in the human body, but the cells that produced it (ameloblasts) are destroyed as soon as a tooth finishes forming. Once a tooth erupts, there are no enamel-producing cells left. Enamel that is drilled away is gone. Full stop. Fluoride can remineralize very early-stage enamel lesions, where minerals have started to leach out but the physical structure is still intact, but that is fundamentally different from regrowing enamel that has been physically removed. If you are curious about whether early-stage enamel damage can be reversed before it becomes a cavity, that is a real phenomenon, but it does not apply once drilling has already happened.
Dentin: limited, and not after a filling
Dentin is slightly more forgiving. The pulp tissue inside your tooth contains odontoblasts, cells that can deposit small amounts of "tertiary" or "reparative" dentin in response to mild irritation or slow-moving decay. Dentists now actively try to preserve as much healthy dentin as possible during cavity prep, partly to protect the pulp and partly because of this limited self-defense response. However, this reparative dentin forms inward (toward the pulp), not outward to fill a drilled cavity, and it certainly is not restoring the tooth structure that was removed. After a filling is placed, you are not getting your dentin back.
Pulp and nerve: no practical regrowth
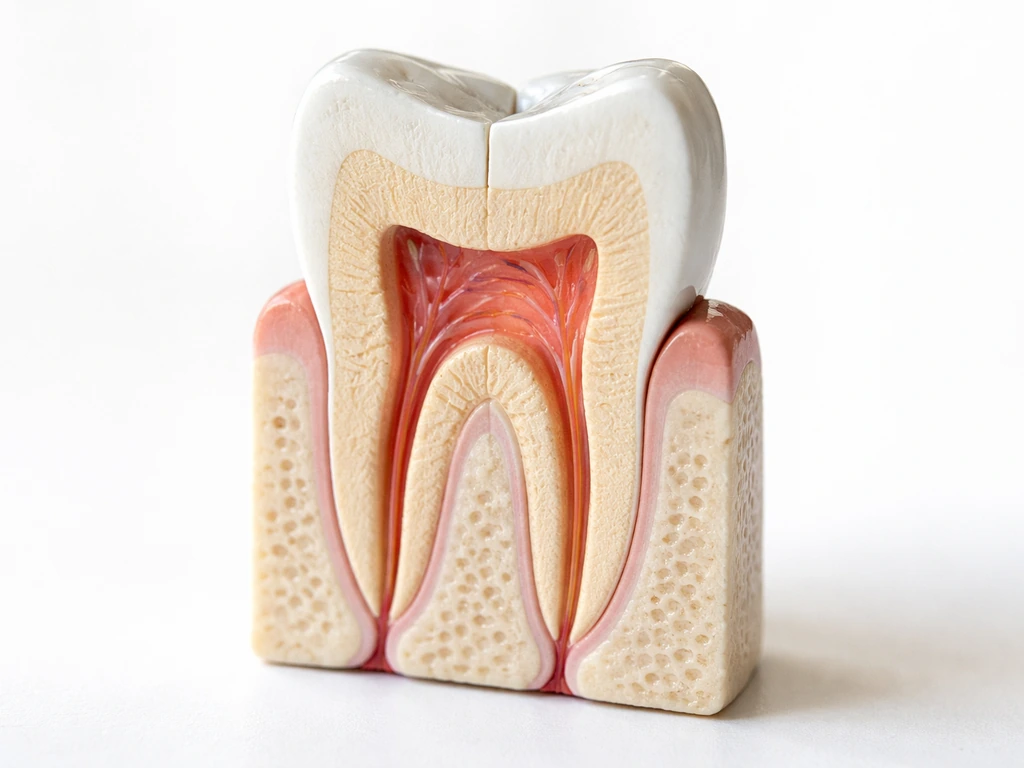
The dental pulp (the soft tissue containing blood vessels and nerves) does not regenerate in any meaningful clinical sense after a standard filling. There is an exciting research area called regenerative endodontics, which uses biologic techniques to encourage continued root development in young teeth with immature roots and dead pulps. The American Association of Endodontists has reported outcomes including continued root development and thickening of dentinal walls in these cases. But this is a specialized procedure for specific clinical situations, not something that happens on its own after a routine cavity filling. If your pulp is damaged enough to need a root canal, it is not going to heal itself and grow back. After an extraction, your teeth do not regrow or grow back into the empty space will teeth grow back after extraction.
What can actually change after a filling (it's not regrowth, but it can feel like it)
Even though the tooth itself is not regenerating, several real changes happen after a filling that people sometimes interpret as the tooth "healing" or "growing back." None of these are true tooth regrowth, but they are worth understanding.
- Gum tissue healing: If your gums were irritated during the procedure, they will visibly recover over the following days. Gum tissue heals well, and this is sometimes noticed as the area looking healthier or feeling less raw. This is gum healing, not tooth regeneration.
- Sensitivity improving: Post-filling sensitivity is your nerve calming down after the trauma of the procedure. As the pulp recovers from mild inflammation, sensitivity to hot, cold, and pressure typically decreases over days to a few weeks. This feels like the tooth is getting better, and in a functional sense it is, but nothing structural has grown.
- Remineralization at margins: Around the edge of a glass ionomer filling in particular, fluoride released from the material can remineralize tiny areas of early demineralization. This is a genuine benefit of glass ionomer materials, but it is restoring mineral to tooth structure that still existed, not replacing structure that was drilled away.
- Bite settling: A filling that was placed slightly high will cause the tooth to feel prominent and sore when you bite. Over a few days, the filling often wears in slightly and the soreness goes away. This is not the tooth remodeling itself; it is just mechanical adjustment of the restoration.
When the tooth feels worse after a filling: causes and warning signs
Some post-filling discomfort is completely normal. Your tooth went through a procedure. But there is a difference between normal settling-in soreness and signs that something is actually wrong.
Normal after a filling
- Sensitivity to hot, cold, or sweet foods for up to a few weeks
- Mild soreness when biting, especially in the first few days
- A slight awareness of the tooth that fades over time
- Minor gum tenderness around the tooth
Warning signs that need attention
If sensitivity lasts beyond about four weeks without improving, that is a signal to call your dentist. More urgently, certain symptoms suggest the problem has moved beyond routine post-filling sensitivity and into something that requires prompt evaluation.
- Spontaneous pain that wakes you up or throbs without any stimulus (hot, cold, or pressure) — this can indicate pulpitis, meaning the nerve is inflamed and potentially dying
- Pain that lingers for 30 seconds or more after a cold stimulus is removed, which is a classic sign of irreversible pulpitis
- Swelling in the gum, jaw, or face near the tooth
- A pimple-like bump on the gum (a sinus tract or fistula, which means an abscess is draining)
- Fever of 100.4°F (38°C) or higher, difficulty swallowing, or trouble opening your mouth fully — these are red flags for a spreading infection that requires same-day or emergency evaluation
- A constant, worsening ache in the jaw or around the tooth that does not respond to over-the-counter pain relief
The ADA's guidance on urgent dental pain is clear: when deeper infection or spreading swelling is suspected, the priority is getting definitive dental treatment, not waiting it out. A spreading dental infection can move through tissue planes quickly and become a medical emergency, not just a dental one.
How to tell if more tooth is being lost: symptoms of failure or progressing decay
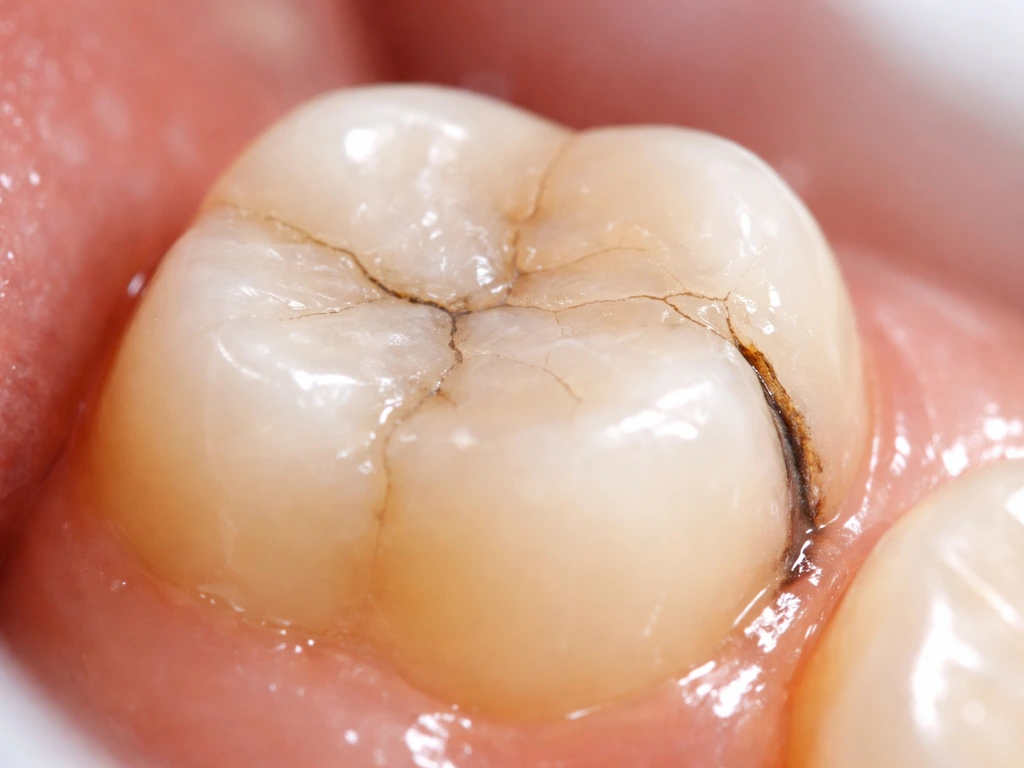
A filling can fail in a few ways: it can crack, a margin can open up (called microleakage), or decay can develop around or under it (recurrent or secondary decay). When this happens, the tooth is losing more structure, not gaining it back.
Symptoms that suggest a filling may be failing or that new decay is developing include:
- New sensitivity in a tooth that had been comfortable for months or years after a filling
- Pain or discomfort when biting down on that specific tooth
- A visible crack line in the filling material or a feeling that part of it has chipped
- Food consistently packing between that tooth and its neighbor (suggesting a margin has opened)
- A new cavity showing up on dental X-rays at or near the edge of an existing filling
- Discoloration (dark line or stain) visible at the filling margin
Your dentist evaluates these concerns with a combination of tools: visual and tactile examination, bitewing and periapical X-rays (which can detect decay on surfaces between teeth and bone changes near the roots), and assessing how the tooth responds to probing and bite testing. X-rays are especially important because decay forming under a filling or at a contact point is invisible to the naked eye. The ADA recognizes that radiographic imaging is a core part of diagnosing caries and monitoring existing restorations, and that visual exam alone misses a significant number of interproximal lesions.
Realistic next steps: what to do today and when to call your dentist
If you just had a filling placed and are wondering if the tooth is healing or regrowing, the direct answer is: no regrowth is happening, but if you are within the first two to four weeks and experiencing only sensitivity and mild soreness, that is within the range of normal recovery. If you are asking a similar question about what happens when a permanent tooth falls out, the key point is that teeth generally do not grow back after being lost if permanent tooth falls out will it grow back. Here is how to triage where you stand:
- Less than 2 weeks post-filling with only cold/sweet sensitivity and no spontaneous pain: this is normal. Use a sensitivity toothpaste, avoid extreme temperatures, and give it more time. Over-the-counter NSAIDs (ibuprofen) can help with soreness if needed.
- Bite feels high or the tooth feels prominent when you close your mouth: call your dentist for a quick bite adjustment. This is a very easy fix and is not a sign of anything serious.
- Sensitivity still present and not improving after 4 weeks: schedule an appointment. Do not keep waiting indefinitely. Your dentist needs to assess whether the pulp is inflamed beyond what it can recover from.
- Any of the urgent warning signs listed above (spontaneous throbbing pain, swelling, fever, trouble swallowing): call your dentist today or go to an urgent dental clinic. Do not wait for a routine appointment.
- You suspect the filling cracked or a chunk came off: call your dentist to schedule repair. Leaving an open margin exposes the tooth to rapid new decay.
- It has been over a year and the tooth has started bothering you again: schedule an exam and request updated X-rays to check the margins and the area around the filling.
One thing worth knowing: if a filling does fail and decay progresses further, the next interventions (crown, root canal, or extraction) involve removing even more tooth structure. The tooth does not get easier to save the longer you wait. This is true for chipped teeth, broken teeth, and teeth lost to extraction as well: once structure is gone, modern dentistry has no way to regrow it, only to replace it with prosthetics or restorations. If you are dealing with a chipped tooth, the key point is the same: the missing structure does not regrow, but your dentist can restore it with the right treatment chipped teeth.
Prevention and protection after fillings: stopping new decay and managing sensitivity

Getting a filling is not the end of the story for that tooth. The bacteria that caused the original cavity are still in your mouth, and the margins of a filling (where filling material meets tooth) are slightly more vulnerable to new decay than intact enamel. Here is what actually makes a difference:
Daily habits that protect filled teeth
- Brush at least twice a day with a fluoride toothpaste. Fluoride remineralizes early enamel lesions and strengthens the tooth surface around filling margins, reducing the risk of recurrent decay.
- Floss once a day. The contact points between teeth are where decay most commonly starts around filling margins, and flossing is the only effective way to clean those surfaces.
- Drink fluoridated water when available. The CDC recommends this as part of a caries-prevention approach, and it provides a steady low-level fluoride exposure throughout the day.
- Use a sensitivity toothpaste if you have post-filling sensitivity. Potassium nitrate-based toothpastes can calm nerve responses over time with consistent use.
Professional steps that extend filling life
- Keep your regular check-up and cleaning schedule. X-rays taken at appropriate intervals catch recurrent decay and failing margins before they become big problems.
- Ask your dentist about in-office fluoride varnish if you are at higher cavity risk (dry mouth, history of frequent cavities, or low fluoride exposure). NIDCR specifically notes fluoride varnish for high-risk patients.
- If you grind your teeth at night (bruxism), talk to your dentist about a night guard. Grinding puts extreme stress on fillings and can crack or dislodge them, particularly composite restorations.
- Report any new sensitivity in a previously comfortable filled tooth at your next visit, even if it is mild. Early interception is always easier than treating a failed restoration.
The bottom line is straightforward: fillings fix teeth, they do not regrow them. The tooth you have after a filling is sealed and restored, but the biology of that tooth is still yours to protect. Good daily hygiene, fluoride, and consistent dental care are the closest things to "protecting" a filled tooth from needing more work down the road. The tooth will not do the regenerating for you, but you can absolutely stop new damage from happening.
FAQ
If my tooth feels “better” after a filling, does that mean it’s growing back?
No. After a standard cavity filling, the drilled enamel and dentin are not replaced by new tooth material. If you notice the area feels different weeks later, it is usually swelling settling down, nerves calming after prep, or the bite and margins adjusting, not new enamel growth.
How long is normal sensitivity after a filling, and when should I worry?
It can be, especially for deeper cavities. If the filling is on a tooth with a near-pulp area, irritation can cause temporary sensitivity. A useful rule is that improvement should trend upward over 2 to 4 weeks, otherwise call your dentist for reassessment.
Why does a filling hurt when I bite down?
Tooth growth back is not the cause. Pain can come from high bite (the filling feels “high”), cracks, or microleakage leading to secondary decay. If the pain is triggered by biting or chewing, ask your dentist to check bite contacts and the integrity of margins.
Can fluoride make the tooth enamel regrow after a filling?
Yes, but it is not regrowth. Fluoride can help early enamel lesions by rebalancing minerals when the surface structure is still intact. Once a dentist drills and places a filling, any future improvement you see is stabilization of the area, not reversal of removed tooth.
Why does cold sensitivity keep coming back months after my filling?
Some people get sensitivity because of bonding and sealing changes at the edges, especially if the margin is near exposed dentin. If cold sensitivity keeps returning in the same spot, it can point to marginal leakage or incomplete seal, which needs a clinical check and possibly replacement.
What symptoms suggest my filling problem is more than normal healing?
It should not. Persistent or worsening pain, swelling, a bad taste or drainage, or pain that wakes you at night are red flags for infection or a failing restoration. Seek prompt evaluation rather than waiting for it to “heal.”
Can a filling hide a cracked tooth, and what does that feel like?
A cracked tooth can cause delayed symptoms, and it often shows up as pain with chewing or temperature changes. When a filling is present, cracks around the tooth can make the filling look like the issue, but the underlying tooth structure may be breaking down.
If my filling looks fine, can new decay still develop under it?
Yes. One common misconception is that a filling “protects everything inside.” If decay continues under a restoration or between teeth, the filling may stay in place while the disease progresses, which is why bitewing and periapical X-rays matter.
Does the tooth ever make reparative dentin after a filling to replace what was removed?
Usually, no. Reparative dentin response is limited and occurs toward the pulp, not outward to fill missing structure. In mature teeth, that self-defense response is not enough to regenerate the cavity that was removed and filled.
Is regenerative dentistry the answer if my pulp was damaged by the cavity?
In certain cases, regenerative endodontic procedures can encourage continued root development, mainly in young teeth with specific conditions (like immature roots) rather than routine cavity fillings. If you had a root canal or the pulp was removed, spontaneous regrowth is not expected.
Does waiting after a filling starts failing make the final treatment harder?
When a filling fails and decay progresses, later treatments often require more removal, such as a crown or root canal, and in some cases extraction. Delaying can make the tooth harder to save, because there is no reliable way to regenerate lost hard tissue.
Could tooth whitening or new habits make it feel like my filling is growing back?
Bleaching or temperature sensitivity can make teeth feel “different,” but those sensations are not tooth regrowth. If you have new darkening, increasing roughness at the margin, or ongoing pain, you should still have the restoration evaluated rather than assuming it is cosmetic or temporary.
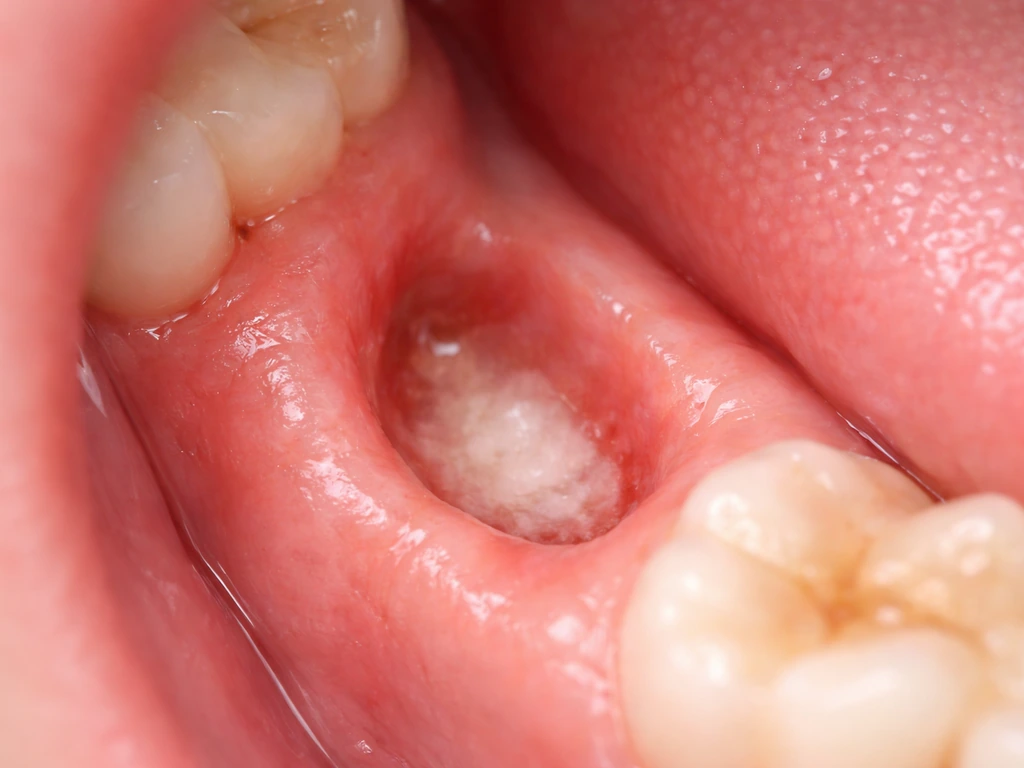
Explains if extracted teeth can regrow, how jaw bone heals, and what options help missing teeth after removal.
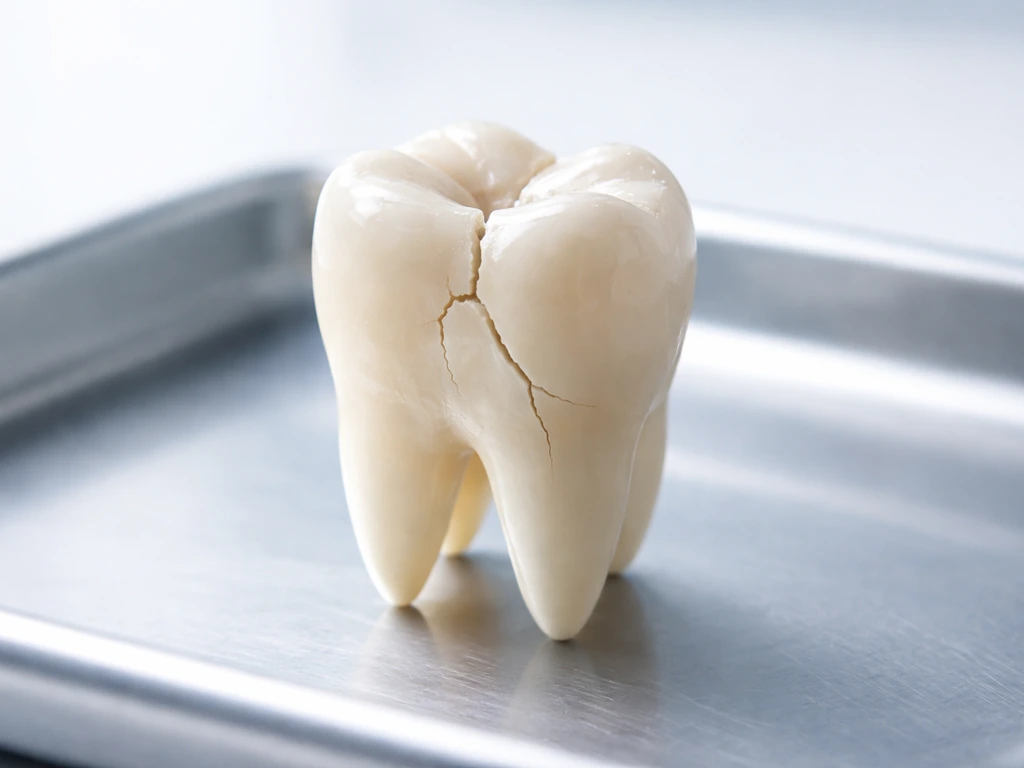
Broken or cracked tooth rarely regrows; learn what can heal, what needs bonding, crowns, root canal, or extraction.
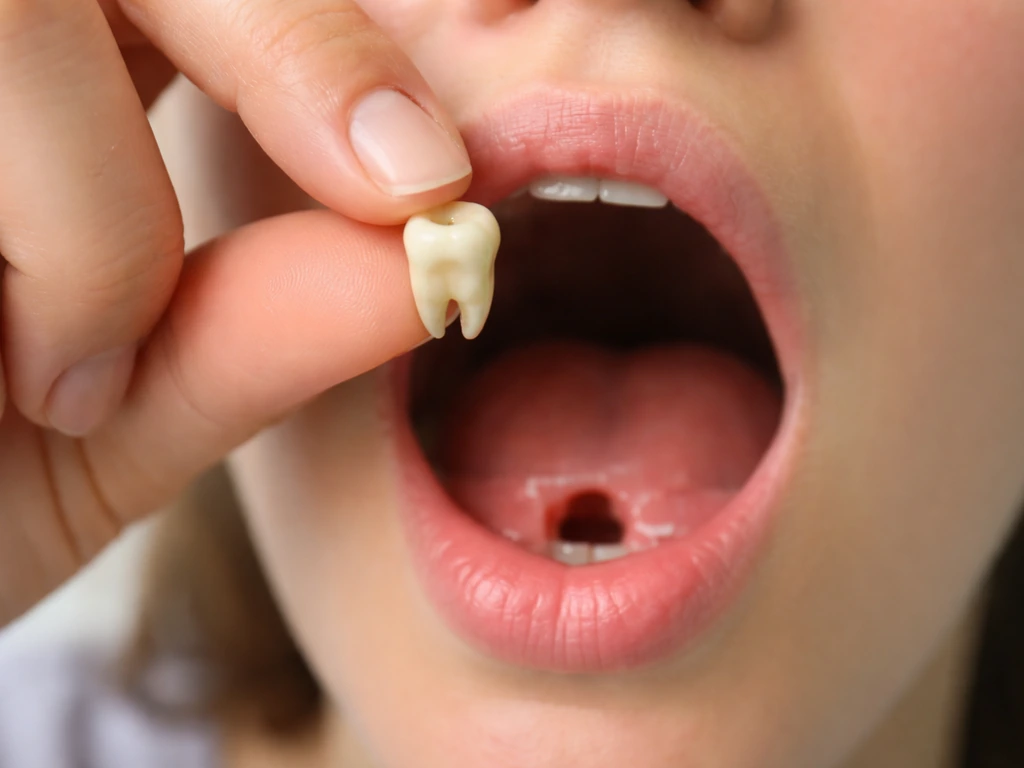
Know if a permanent tooth regrows after it falls out, why it usually won’t, and what to do immediately and next.

