Yes, mandibular tori can grow larger over time, but it happens slowly and the process is more like gradual bone remodeling than a tumor suddenly expanding. These benign bony bumps on the inner surface of your lower jaw tend to increase in size across decades, driven by a mix of genetics, chewing forces, and age-related bone changes. They are not cancerous, they are not regrowing tooth tissue, and for many people they never cause a single problem. But they can get big enough to interfere with speech, swallowing, denture fit, or oral hygiene, and that is when they need attention.
Can Mandibular Tori Grow? What Changes Size Over Time
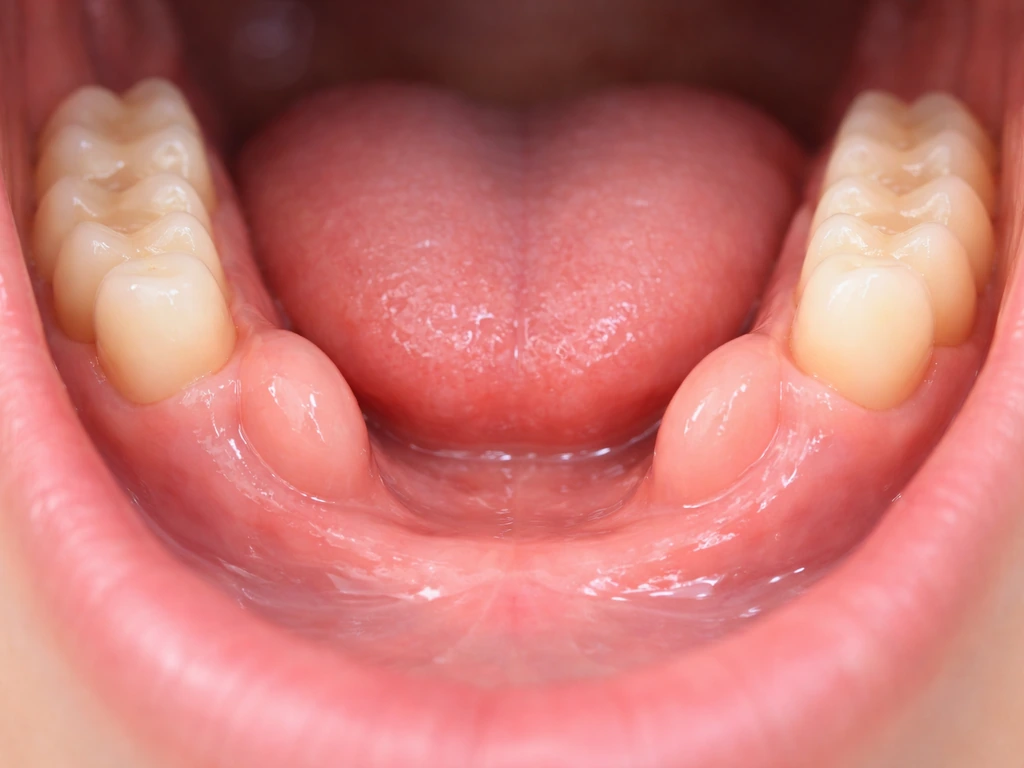
What mandibular tori actually are (and what they are not)
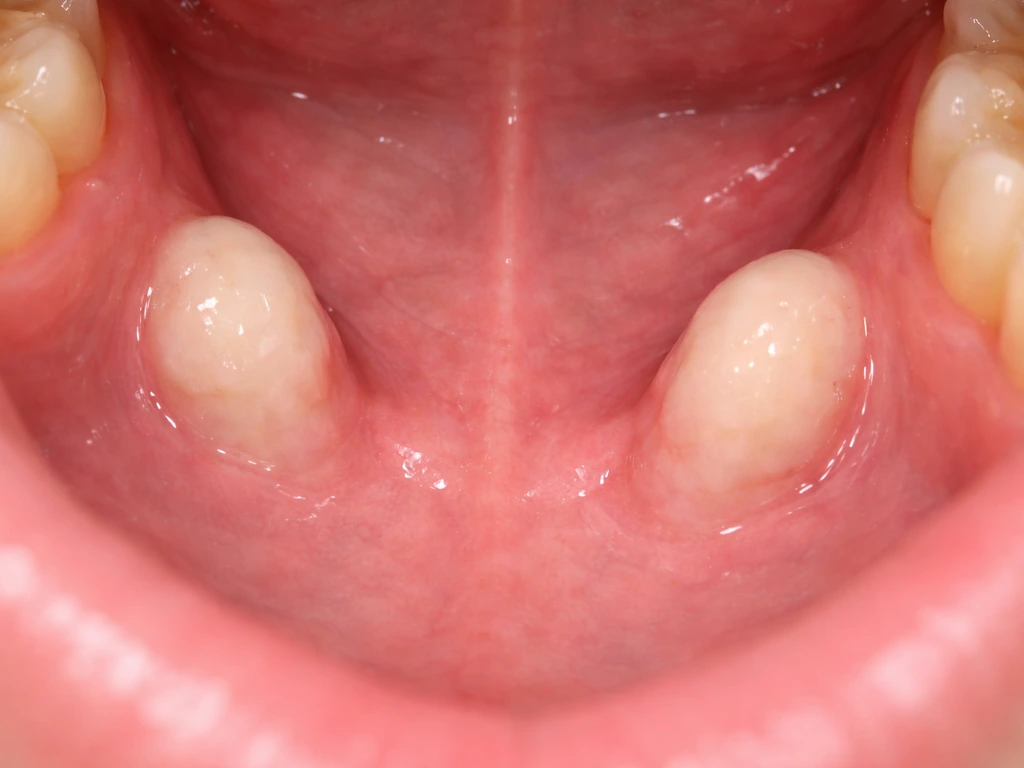
Mandibular tori (singular: torus mandibularis) are benign bony outgrowths that form on the lingual side of the lower jaw, the surface that faces your tongue. Clinically they are classified as exostoses, meaning localized outgrowths of cortical bone that are continuous with the normal jawbone underneath. They are hard, fixed, covered by a thin layer of oral mucosa, and completely noncancerous.
Here is where the confusion with 'regrowth' usually comes in. Because this site covers what dental structures can and cannot regenerate, it is worth being direct: mandibular tori are not a regeneration phenomenon. They are not enamel growing back, not tooth tissue sprouting from the gum, and not anything like the bizarre but fascinating cases where cysts or tumors elsewhere in the body develop dental tissue. Tori are bone, plain and simple. They form from the existing mandible and expand through the same bone-remodeling mechanisms your skeleton uses throughout life. That is a fundamentally different process from what happens when a child loses a baby tooth and a permanent one erupts, or from the experimental stem cell research aimed at regrowing teeth from scratch.
Distinguishing tori from other jaw lesions matters clinically too. Osteomas, ossifying fibromas, and osteochondromas can all look similar on a quick exam but behave differently. What separates a torus from these is that it shows clear continuity with the cortical bone on imaging, has a predictable location, and stays benign. That is why a dentist who is unsure will order a CT or CBCT rather than just watching: the imaging confirms the diagnosis and rules out anything more concerning.
Why mandibular tori grow: the real drivers
Genetics is the biggest factor

The single strongest predictor of whether you will develop mandibular tori is your family history. Twin studies have estimated the heritability of oral bony outgrowths including torus mandibularis at around 0.658, meaning roughly two-thirds of the variation in who gets them is explained by genetics. If a parent or sibling has tori, your odds of developing them are meaningfully higher. This genetic influence also partly explains why tori appear across ethnic and geographic populations at very different rates, with prevalence varying widely between studied groups.
Age and biology
Tori rarely show up in young children. They typically emerge in adolescence or early adulthood and then grow slowly across decades. CBCT and postmortem CT studies have found measurable age-related increases in torus thickness, which aligns with the idea that cumulative bone remodeling and sustained mechanical loading over years contribute to gradual enlargement. There is also evidence of sex-related differences in when and how prominently tori develop, with some research pointing to hormonal influences on timing, including observations in populations with chromosomal differences like Turner syndrome. The biology here is not fully mapped out, but the bottom line is that tori tend to grow most actively during periods of significant occlusal loading and then continue to change, slowly, throughout adulthood.
Chewing habits, bite stress, and other mechanical triggers
Beyond genetics and age, what you do with your jaw matters. Mechanical stress on the mandible appears to stimulate bone apposition in torus-prone individuals. The clearest evidence for this comes from research on bruxism: a systematic review found that signs of abnormal tooth wear significantly increased the odds of having torus mandibularis, and studies on temporomandibular disorders also flag occlusal stress as a contributing factor. In practical terms, if you grind or clench your teeth, you may be continuously feeding the mechanical stimulus that encourages tori to enlarge.
CBCT population data adds more detail here. Torus thickness showed a stronger age-related increase in males who maintained full occlusal contact, which is consistent with bite force being a direct driver of bone remodeling at the torus site. Other factors implicated in the research include trauma, nutritional influences, and infections, though these are less consistently documented than the occlusal stress connection.
Denture wearers face a specific mechanical problem. After tooth loss, the mandible and alveolar ridge undergo resorption and remodeling, which can make an existing torus look and feel dramatically more prominent even if the torus itself has not changed much. The surrounding bone shrinks while the torus remains, so the relative protrusion increases. This is one of the most common reasons patients come in convinced their tori have 'suddenly grown,' when what has really changed is the landscape around them.
How to tell if your tori are actually getting bigger
This is genuinely tricky to assess on your own, because tori change so slowly that year-to-year differences are usually imperceptible. The most reliable approach is serial documentation: intraoral photographs taken at regular dental visits give you a visual baseline that is far more useful than trying to remember what something felt like two years ago. Some research protocols use CBCT imaging with direct thickness measurements to track change over time, which is what would be used if your dentist or oral surgeon wanted to formally monitor progression.
Practically speaking, here are the signs that something has changed and deserves attention rather than passive monitoring:
- A hard lump under your tongue that you previously could not feel or barely noticed has become noticeably larger or more prominent
- The overlying tissue looks white, raw, or ulcerated, especially after eating crunchy or hard foods
- Your denture or partial no longer fits the way it used to and rocks or causes sore spots near the inner lower jaw
- You notice speech changes, a lispy quality, or difficulty positioning your tongue comfortably
- Swallowing feels different or you notice increased saliva pooling
- You feel discomfort or pressure in the area that was not there before
- The area feels suddenly tender or swollen rather than the usual hard and painless texture
That last point is worth emphasizing. Tori themselves do not hurt under normal circumstances. Pain, rapid apparent enlargement, swelling of the surrounding soft tissue, or difficulty with salivary flow are not typical torus behavior and need to be evaluated promptly. There are documented cases of very large mandibular tori causing submandibular duct obstruction and secondary sialadenitis, which is a situation that requires urgent assessment, not watchful waiting.
When to see a dentist or oral surgeon
If your tori are small, asymptomatic, and your dentist has already confirmed they are tori at a previous visit, you do not need to rush in. Keep your regular checkups and mention any changes you have noticed. Your dentist will examine the site visually and by palpation at each visit and note any changes.
You should make an appointment sooner rather than later if any of the following apply:
- You have never had the bumps formally diagnosed and are not certain what they are
- The area has ulcerated or developed a sore that is not healing within two weeks
- You are getting a new denture or existing denture no longer fits and tori may be the reason
- You have pain, swelling, or difficulty opening your mouth, swallowing, or speaking
- The growth feels different in texture (softer, irregular) than the smooth hard nodule you are used to
- You have noticed rapid change over weeks rather than gradual change over years
At the appointment, the dentist or oral surgeon will examine the tori directly, assess the overlying mucosa, and check your bite and any appliances. If there is any uncertainty about what the lesion is, or if the tori are large enough that imaging would guide treatment planning, they will order a panoramic radiograph or CBCT. CT imaging is particularly useful for ruling out other radiopaque jaw lesions that can mimic tori and for measuring torus dimensions before any planned surgery.
Treatment options: monitoring vs. surgical removal
The standard approach for asymptomatic mandibular tori is observation. No treatment is needed if the tori are not interfering with function, oral hygiene, or prosthetic fit. Your dentist documents their size, checks them at regular intervals, and that is that. Most people with tori go their entire lives without needing anything done.
Surgical removal, sometimes called torsectomy, torus reduction, or surgical osteoplasty, becomes the recommendation when tori are causing real problems. The specific indications that typically push a case from monitoring to surgery include:
- Interference with denture fabrication or fit that cannot be accommodated by adjusting the appliance
- Recurrent traumatic ulceration from the thin mucosa over the torus being repeatedly injured by food or appliances
- Significant interference with speech or tongue positioning
- Difficulty maintaining adequate oral hygiene around the tori
- Obstruction of salivary gland ducts or other adjacent structures in rare large-torus cases
- Prosthetic rehabilitation planning where the torus volume makes a functional restoration impossible without reduction
The surgery itself is typically done under local anesthesia as an outpatient procedure. The oral surgeon makes an incision in the overlying mucosa, removes or reduces the bony prominence using a bur or osteotome, and closes the site. Recovery involves soft diet, oral rinses, and follow-up to confirm healing. The procedure is well-established and generally has a predictable outcome, though there is a documented possibility of recurrence, particularly if the mechanical stresses that drove the original growth persist. One published case report describes early torus recurrence following surgical resection and proposes that continued mechanical stress was the likely mechanism, which is a useful reminder that bruxism management and occlusal factors should be addressed alongside any surgical treatment.
| Scenario | Recommended approach | Urgency |
|---|---|---|
| Small, asymptomatic, already diagnosed | Routine monitoring at dental checkups | Low, continue regular visits |
| Undiagnosed hard lump on inner lower jaw | Dental evaluation for formal diagnosis | Schedule soon |
| Ulceration or sore over torus not healing | Dental or oral surgery evaluation | Within 1-2 weeks |
| Denture no longer fitting due to tori | Oral surgery consultation for possible reduction | Schedule soon |
| Pain, swelling, or salivary gland symptoms | Prompt evaluation, possible imaging | Urgent, within days |
| Rapid apparent enlargement over weeks | Oral surgery or dental evaluation with imaging | Urgent, rule out other lesions |
One thing worth keeping in mind as you navigate this: the question of whether a bony jaw growth can enlarge is genuinely different from questions about whether dental tissue can regenerate. For example, even though stem cell research explores whether can stem cells grow teeth, mandibular tori themselves are not evidence of tooth regeneration. Tori grow because bone remodels in response to stress and genetic programming, not because of any regenerative biological process. There is no evidence that ovaries can grow teeth, and dental tissue does not form that way in the body can ovaries grow teeth. That puts them in a completely different category from the experimental frontier of stem cell-driven tooth regrowth or the curious biology behind why some tumors or cysts in other parts of the body end up containing tooth-like structures. In rare cases, people wonder <a data-article-id="BBEF992E-C56C-4A2A-8E34-11435BDBF061">can tumor grow teeth</a>, but mandibular tori themselves are not tumors and they do not regenerate tooth tissue tumors or cysts. In rare cases, people wonder why do teratomas grow teeth, but mandibular tori themselves are not tumors and they do not regenerate tooth tissue. Mandibular tori are your own jawbone adapting to decades of use, and understanding that makes the management approach much clearer: track them, address functional problems when they arise, and work with a dentist or oral surgeon who can actually measure and document what is happening over time.
FAQ
How can I tell whether my tori are truly growing versus my mouth “changing around them”?
If the bony bump seems more prominent but you have no change in firmness or shape at the torus surface, the difference may be from shifting landmarks (especially after tooth loss, gum recession, or denture adjustments). The most reliable way to sort this out is to compare serial intraoral photos and, when needed, measured CBCT thickness rather than relying on how it “feels” day to day.
Can tori go away on their own or stop growing completely?
They usually do not fully disappear. Growth tends to be gradual, and activity often slows after decades of remodeling, but the torus can still look more prominent as nearby tissues change (for example, with age-related ridge resorption or denture wear). If your tori appear to be shrinking, it can also reflect weight loss or prosthesis changes rather than true bone reduction.
Do mandibular tori mean I will need dentures or major dental work later?
Not automatically. Many people with tori never require removal. The main issues are prosthetic fit and oral hygiene access, so the risk depends on size and location relative to your planned appliance. A dentist can plan early, such as adjusting denture borders or considering torus reduction only if it interferes with function.
If I have tori and I get an implant or fixed bridge, will the presence of tori make treatment impossible?
Often it does not make it impossible, but it changes planning. The concern is mainly space and alignment in the lower jaw, plus ensuring the overlying mucosa can be managed during impressions and restorations. Your dentist or oral surgeon may use panoramic imaging or CBCT to map exact bone contours before committing to implant positioning or substructure design.
Is it safe to try to remove or grind down tori at home?
No. Because they are continuous with the underlying cortical bone, attempting to file, shave, or burn them yourself can cause mucosal injury, infection, and uncontrolled bleeding. If reduction is needed, it should be done surgically by an oral surgeon under appropriate anesthesia with a plan for protecting the mucosa and achieving clean edges.
What symptoms are most concerning for something other than a benign torus?
Pain is a key red flag, especially new or worsening pain localized to the torus, ulceration of the overlying mucosa, rapid apparent enlargement over weeks to months, soft tissue swelling, bleeding that does not heal, or trouble with saliva-related symptoms. These warrant prompt evaluation to rule out other jaw lesions that can mimic exostoses.
How often should I have my tori checked if they are not causing problems?
A reasonable approach is to follow your routine dental visit schedule and specifically ask for documentation of torus size at each exam. If they are large, if you are using dentures, or if you have occlusal issues like bruxism, your dentist may recommend more frequent assessment or additional imaging to guide prosthetic planning.
Will treating bruxism stop torus growth, or is surgery still likely later?
Treating bruxism can reduce ongoing mechanical loading, which may slow further remodeling, but it does not guarantee the torus will stop enlarging. Surgery is considered based on functional impact, not just the presence of stress. If you reduce clenching or grinding (night guard, bite management, stress control), it may also lower the risk of recurrence after torus reduction.
If I had torus reduction before, can the torus come back?
Recurrence is possible, particularly if the factors that promoted growth, such as heavy bite force or persistent bruxism, continue afterward. Discuss long-term bite management during follow-up, because controlling mechanical stress is one of the few modifiable factors that can influence whether regrowth occurs.
Does CT or CBCT monitoring mean radiation exposure is a concern?
It can be, which is why routine torus monitoring often relies on clinical exams and photos, reserving CBCT for cases where diagnosis is uncertain, size measurement will change treatment planning, or symptoms are present. Ask your clinician to use the lowest practical imaging needed to answer a specific question.
Yes, ovaries can show teeth in dermoid cysts due to teratomas; learn symptoms, diagnosis, and realistic treatment outcom
See what stem cells can truly do for teeth today, what is still impossible, and how to spot safe real trials.
Learn how teratomas form tooth structures from embryologic tissue, whether teeth can develop or reappear, and real clini

